doi: 10.56294/hl2023324
ORIGINAL
The Effects of Comprehensive Healthcare Education on the Quality of Life Among Aging Demographics
Efectos de la educación sanitaria integral en la calidad de vida de las personas mayores
Jamuna KV1 ![]() , Ganesh Thorat2
, Ganesh Thorat2 ![]() , Manju Kundu3
, Manju Kundu3 ![]() , Satyasarathi Jena4
, Satyasarathi Jena4 ![]() , Ram Garg5
, Ram Garg5 ![]()
1JAIN (Deemed-to-be University), Department of Forensic Science. Bangalore, Karnataka, India.
2Krishna Institute of Medical Sciences, Krishna Vishwa Vidyapeeth “Deemed to be University”, Dept. of Medicine. Taluka-Karad, Dist-Satara, Maharashtra, India.
3School of Liberal Arts, Noida International University. Greater Noida, Uttar Pradesh, India.
4IMS and SUM Hospital, Siksha ‘O’ Anusandhan (Deemed to be University), Department of Cardiology. Bhubaneswar, Odisha, India.
5Arya College of Pharmacy. Jaipur, Rajasthan, India.
Cite as: KV J, Thorat G, Kundu M, Jena S, Garg. The Effects of Comprehensive Healthcare Education on the Quality of Life Among Aging Demographics. Health Leadership and Quality of Life. 2023; 2:324. https://doi.org/10.56294/hl2023324
Submitted: 07-06-2023 Revised: 02-09-2023 Accepted: 13-11-2023 Published: 14-11-2023
Editor: PhD.
Prof. Neela Satheesh ![]()
ABSTRACT
As the world’s population grows, the quality of life of older people has become a major worry for lawmakers and health care workers. Healthcare education is a big factor in the quality of life of older people because it can have a big effect on their health behaviours, decisions, and general well-being. This study looks into how teaching older people about all aspects of health care can improve their quality of life, especially for those in sensitive age groups. The study looks at how customised training programs that focus on age-related health issues, preventative measures, and lifestyle changes can give adults the power to take charge of their health and confidently deal with the challenges of getting older. A variety of older people who took part in an organised healthcare education program were asked to fill out both qualitative and quantitative surveys as part of a mixed-methods study. The paper discussed about common health problems that come with getting older, such as heart disease, diabetes, osteoporosis, and memory loss. It also suggested that people take care of their physical and mental health by eating right, working out, and dealing with stress. Before and after the treatment, the people’s quality of life was measured using normal tools that looked at physical, mental, and social factors. People who took part in the whole healthcare education program said that their physical health, mental health, and social lives all got a lot better. People were also happy with their lives, their health care costs went down, and they were better able to handle their own health problems. Findings show that giving older people more control, making their quality of life better, and maybe even lowering the need for healthcare services rest a lot on how much they know about it. According to this study, individual training programs should be used a lot as an important part of healthcare plans for older people.
Keywords: Healthcare Education; Aging Demographics; Quality of Life; Preventive Health; Elderly Empowerment.
RESUMEN
A medida que crece la población mundial, la calidad de vida de las personas mayores se ha convertido en una gran preocupación para los legisladores y el personal sanitario. La educación sanitaria es un factor importante en la calidad de vida de las personas mayores porque puede tener un gran efecto en sus comportamientos y decisiones en materia de salud y en su bienestar general.Este estudio analiza cómo enseñar a las personas mayores todos los aspectos de la atención sanitaria puede mejorar su calidad de vida, especialmente en el caso de los grupos de edad sensibles. El estudio examina cómo los programas de formación personalizados que se centran en los problemas de salud relacionados con la edad, las medidas preventivas y los cambios en el estilo de vida pueden dar a los adultos el poder de hacerse cargo de su salud y afrontar con confianza los retos de envejecer. Como parte de un estudio de métodos mixtos, se pidió a varias personas mayores que participaron en un programa organizado de educación sanitaria que rellenaran encuestas cualitativas y cuantitativas. El documento hablaba de los problemas de salud más comunes que conlleva hacerse mayor, como las cardiopatías, la diabetes, la osteoporosis y la pérdida de memoria. También sugería que las personas cuidaran su salud física y mental comiendo bien, haciendo ejercicio y controlando el estrés. Antes y después del tratamiento, se midió la calidad de vida de las personas mediante herramientas normales que analizaban factores físicos, mentales y sociales. Las personas que participaron en el programa de educación sanitaria dijeron que su salud física, mental y social había mejorado mucho. Además, se sentían satisfechos con su vida, sus gastos sanitarios se redujeron y eran más capaces de afrontar sus propios problemas de salud. Los resultados demuestran que dar más control a las personas mayores, mejorar su calidad de vida e incluso reducir la necesidad de servicios sanitarios depende mucho de cuánto sepan al respecto. Según este estudio, los programas de formación individual deberían utilizarse mucho como parte importante de los planes de atención sanitaria para personas mayores.
Palabras clave: Educación Sanitaria; Envejecimiento Demográfico; Calidad de Vida; Salud Preventiva; Empoderamiento de las Personas Mayores.
INTRODUCTION
Every year, increasingly more individuals all around are becoming older. Approximately 22 % of the complete international population, the worldwide fitness employer (WHO) estimates that with the aid of 2025 there can be more than 2 billion people aged 60 and over. For healthcare systems all during the globe, this demographic shift gives most important challenges as getting old frequently includes multiplied likelihood of persistent illnesses, intellectual fitness issues, and problems with physical functioning. People’s requirements evolve with age; they also frequently have many fitness issues that at once have an effect on their first-class of lifestyles. These troubles have made thorough healthcare training a critical device for older persons ageing in a better way, locating happiness with their life, and commonly being healthier. Preventing, controlling, and treating fitness troubles accompanying growing older rely upon plenty on healthcare education. What it implies is arming individuals with understanding, sources, and talents so they may make wise selections about their health.(1) Healthcare training can also assist elderly people have much less extreme lengthy-time period ailments like coronary heart sickness, diabetes, arthritis, and dementia. It additionally empowers aged humans to choose healthy lifestyles, efficaciously control their medical issues, and get suitable treatment. Vital components of healthcare training that may greatly affect a person's fine of lifestyles are autonomy and self-efficacy. A wide concept, quality of life encompasses social, psychological, and physical well-being. It reveals how content a person is with their life in general and how well they can do everyday chores even with health issues.(2)
Older folks may have distinct elements defining their quality of life than younger ones. Older persons may find more critical management of chronic conditions, independence, and maintaining social relationships. Working together is crucial for both quality of life and healthcare education because educated individuals are more suited to handle the difficulties of ageing and the associated health hazards. Older persons who are well-informed about their health issues and treatment options are less likely to wind up in the hospital, make errors with their drugs, and not follow through with their treatments as advised according to research. All-around healthcare education programs seek to address not just physical health but also the psychological and social aspects of ageing. Many times, these programs include courses on food, exercise, stress management, and mental health issues.(3) The major objectives are to enable individuals to increase their overall health and become more autonomous. These initiatives may reduce the need for emergency medical treatment, enhance self-care, and empower individuals emotionally by arming elderly persons with the skills they need to manage their own health. Though not much is known about the precise relationship between full healthcare education and quality of life, there is increasing research looking at several facets of healthcare for elderly people. Studies on how single educational programs impact many facets of health, including how effectively individuals with chronic conditions are treated or their mental health, have abounded. Few have, however, examined how all-around, comprehensive healthcare education influences people's quality of life in all spheres, including their social, psychological, and physical ones. This void in the research literature implies that further study should be conducted as fully understanding how healthcare education influences older people might have major consequences on developing policies and programs. Among the particular challenges older persons have in trying to learn about healthcare include physical limitations, cognitive decline, and social isolation.(4) This means that programs for older people's healthcare education should be developed considering these factors. People should be able to get programs, have them tailored to their requirements, and get clear, exciting instruction. Furthermore crucial is ensuring that participant’s at all economic levels may benefit from these training initiatives. This covers those without simple access to tools for health care or technology. Healthcare education initiatives for elderly persons are still not extensively adopted or standardised, although their advantages. Many healthcare systems still provide more focus on treating illnesses than on educating individuals how to avoid acquiring and prevent those.(5) Furthermore, present initiatives sometimes fall short in covering all the needs. They may only address a few medical problems, not the whole picture of ageing including social elements, mental health, and quality of life.
Literature review
Overview of aging population trends
Thanks to significant improvements in health care and increased life expectancy, the world's population is ageing and the number of older persons is fast rising. Almost twice as many individuals aged 60 and beyond would be found worldwide by 2025, according to UN estimates, compared to 2017. Rich nations, where elderly individuals are more prevalent than younger ones, clearly show this demographic shift. Many nations have more persons 65 years of age and above than younger people. This creates problems with healthcare, economic stability, and social benefits.(6) There are many physical, mental, and social changes that happen with getting older that can affect health. Chronic diseases like high blood pressure, diabetes, arthritis, and heart problems become more common as people get older. Also, mental health problems like sadness and worry are typical in older people, as is cognitive loss. Figure 1 shows world trends in an ageing population, showing how life span is rising and how demographics are changing as a result.
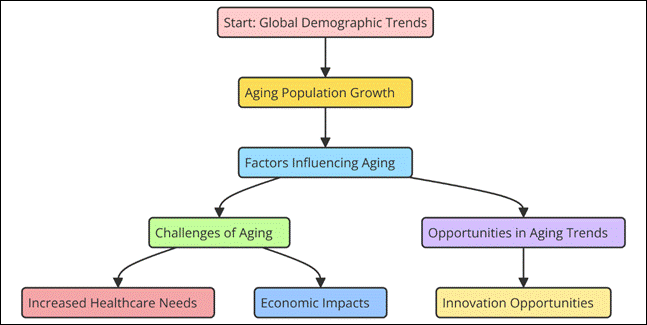
Figure 1. Illustrating the Overview of Aging Population Trends
These diseases, along with being physically weak, often make people's quality of life worse and make them more reliant on healthcare services. Older persons typically deal with social isolation, financial uncertainty, and restricted resources in addition to these health issues, all of which aggravate their conditions. Older individuals require long-term care, medical treatment more regularly, and therapy services, therefore this trend strains healthcare systems all over.(7) Effective healthcare systems, preventive actions, and education help to address the demands of an ageing population therefore reducing the consequences of these issues on individuals and society at large. The fact that individuals are living longer emphasises even more the need of adopting a whole-person approach to health including medical treatment, health education, and strategies for maintaining wellness.(8) Older persons may have happier, more independent lives better for them and the healthcare system by tending to these aspects.
Current state of healthcare education for older adults
Older persons' healthcare education is becoming more and more important as means of improving their quality of life and health. In conventional medical practices, the emphasis is more on curing illness and disease than on avoiding it and advancing general health. More and more study, though, shows how important it is to give older people the information and skills they need to take care of their health, avoid chronic conditions, and improve their general comfort. Currently, healthcare education programs for older people focus on teaching them how to deal with common diseases that come with getting older, like arthritis, diabetes, high blood pressure, and memory loss. Some of the things that might be covered in educational classes are diet, exercise, managing medications, and lowering stress.(9) Most of the time, these programs are offered through a variety of outlets, such as community centres, healthcare facilities, and online platforms. Workshops and lectures that happen in person are more common, but as technology improves, online programs are becoming more popular, especially for people who have trouble getting to or from events. There are many programs that teach people about healthcare, but healthcare workers don't always work together, which causes services to be spread out. The topics covered in these classes may be very different; some may only focus on certain health problems, while others may look at health as a whole. Also, some programs don't take into account the specific needs of older people, especially those who have memory loss, trouble reading, or limited digital literacy.(10) To make sure that all older people can benefit from these programs, healthcare education that is tailored to their needs, easy to access, and open to everyone is necessary. It is also known that teaching older people about health care should cover more than just basic health management. More and more programs are being made that deal with the mental, social, and emotional parts of getting older. These initiatives address social engagement, mental health, and resilience among other areas. These larger training courses are aimed to enhance not only the physical condition but also the mental and emotional health of older persons, which is rather vital for enhancing their quality of life.
Studies on healthcare education and quality of life
Many investigations on the relationship between healthcare education and quality of life in elderly persons have shown favourable results. Studies repeatedly shown that training elderly people about health care improves their mental as well as their physical condition Several research shown that programs for healthcare education emphasising illness prevention, self-management, and lifestyle modifications provide superior health outcomes. These include increased exercise, improved drug compliance, and improved treatment of chronic diseases. One research on elderly persons with high blood pressure found that those who participated in a program teaching how to manage their disease had greater control over it, which in turn improved their quality of life. Participants reported feeling less anxious, having greater control over their health, and being satisfied with their doctors. In the same way, studies on diabetes management education have shown that older people who learnt how to self-monitor and make changes to their lifestyle had fewer problems and felt better overall.(11) Getting more educated about healthcare can also help people stay socially linked, which is a big issue for older people. Loneliness and isolation are linked to worse mental health, so educational programs that push people to join groups or talk to other people have been shown to help lower those feelings. In this situation, schooling can help build community, improve social networks, and get more people involved in activities that matter. Most studies show that healthcare education is helpful, but some have pointed out problems with how easy it is to get into programs and how well they work.(12) For instance, older people with memory problems or people who live in rural places may have trouble getting into training programs, which can make them less useful. More study is needed to find out how to make healthcare education fit the different needs of older people and to find out how these programs affect quality of life in the long run. There is still evidence to back the idea that complete healthcare education can make the quality of life for older people a lot better, especially when it is tailored to their individual health and social needs. In the literature review, table 1 shows the main results, problems, and areas of coverage of different studies and programs.
|
Table 1. Summary of Literature Review |
|||
|
Study/Program |
Key Finding |
Challenges |
Scope |
|
Chronic Disease Self-Management Program (CDSMP) |
Improved chronic condition management and reduced hospitalizations. |
Limited resources for widespread implementation and engagement. |
Focuses on chronic disease management and prevention. |
|
A Matter of Balance Program |
Significant reduction in fall-related injuries and enhanced balance. |
Low participation rates and difficulty in maintaining interest. |
Fall prevention and physical strengthening for older adults. |
|
Health Buddy Program(13) |
Enhanced self-management for chronic conditions and better health outcomes. |
Technological limitations and accessibility challenges for older adults. |
Chronic disease self-management and telehealth education. |
|
Mindfulness-Based Stress Reduction (MBSR) |
Reduced stress, anxiety, and improved emotional wellbeing in older adults. |
Cultural barriers and resistance to non-traditional therapies. |
Stress reduction through mindfulness techniques and coping strategies. |
|
Fall Prevention Education (Stepping On) |
Improved balance, strength, and reduced fear of falling. |
Logistical challenges and inconsistent program access. |
Physical activity, strength building, and fall prevention. |
|
Diabetes Self-Management Program (DSMP) |
Better diabetes management and reduction in complications. |
Barriers to consistent monitoring and follow-up care. |
Education on diet, medication, and self-monitoring of diabetes. |
|
Aging Well Program |
Improved mental health and social engagement. |
Funding limitations and accessibility in rural areas. |
Mental health improvement and social interaction for seniors. |
|
Lifelong Health and Wellness (LHW)(14) |
Increased physical activity and health outcomes in aging adults. |
Program engagement and participant retention issues. |
Holistic health education with a focus on mental, physical, and social health. |
|
The Alzheimer’s Project |
Improved awareness and care strategies for Alzheimer's disease. |
Limited understanding and stigmas surrounding Alzheimer's. |
Care education and improved living for those with Alzheimer's. |
|
Healthy Aging Program (HAP) |
Enhanced health behaviors and greater community engagement. |
Sustainability and resource availability for continued support. |
Health promotion, disease prevention, and community support. |
|
Community-Based Aging in Place Program |
Increased mobility and independent living for aging adults. |
Physical limitations and mobility constraints in older adults. |
Promotes physical activity and encourages independent living. |
|
Older Adult Physical Activity Program(15) |
Improved physical activity levels and reduced frailty. |
High dropout rates and inconsistent participation. |
Addressing frailty, muscle weakness, and physical activity. |
|
Health Literacy Improvement Program |
Increased health literacy and improved health outcomes. |
Cultural and language differences in health education delivery. |
Improves health literacy across diverse populations. |
METHOD
Research design
Qualitative vs. Quantitative
The study's quantitative aspect will concentrate on obtaining objective, quantifiable records on how expertise of healthcare affects first-class of life. Bodily, mental, and social nicely-being can be gauged using standardised instruments and questionnaires. Examining these figures using records will help us to better grasp the general effectiveness of the education application. Conversely, the qualitative element seeks to capture the unique experiences and reviews of the users about the healthcare schooling application. Humans will be asked to fill out semi-established interviews and awareness groups to get exact records approximately how they sense the program has modified their excellent of life. This study will deliver us a better image of the connection between healthcare training and nice of lifestyles by the use of each technique. Along with the numeric data, the qualitative data will add to and build on the results, giving a full picture of the individuals' experiences.
Study population
Selection criteria for participants
People aged 65 and up will be included in the study. They will come from a range of community places, such as senior centres, healthcare facilities, and online sites. Participants will be chosen based on certain factors for who can and cannot participate, so that the group is both broad and accurate. People who have agreed to take part in a healthcare education program, are at least 65 years old, live on their own or with little help, and meet other conditions will be included. People who are taking part should be able to get basic medical care and speak clearly, either in person or online. People who are already in a similar program, have serious brain issues that could make it hard to participate, or can't finish the study because of health problems that make it impossible to take part in the training program will be excluded. The people who take part will be split into two groups: a control group and those who get the full healthcare education. Comparisons between the two groups are possible, which makes the study's results more reliable.
Step 1: Define Participant Characteristics
Identify the key demographic and health characteristics required for the study, such as age, health status, and cognitive ability.
Mathematical Equation:
![]()
Where Pi represents a participant, and Age, HealthStatus, and CognitiveAbility are the characteristics considered.
Step 2: Age Criteria
Set the age range for eligible participants (e.g., older adults aged 65 and above).
Mathematical Equation:
![]()
Where: Agei is the age of participant i, and 65 is the minimum age requirement.
Step 3: Health Status Criteria
Define the health status required for participation, such as having one or more chronic health conditions (e.g., diabetes, hypertension).
Mathematical Equation:
![]()
Where: HealthStatusi is the health status of participant i, either with chronic conditions or without.
Step 4: Cognitive Ability Criteria
Set the criteria for cognitive ability, such as a minimum score on a cognitive assessment (e.g., Mini-Mental State Examination, MMSE).
Mathematical Equation:
![]()
Where: CognitiveAbilityi is the cognitive assessment score of participant i, and Threshold is the minimum acceptable score.
Step 5: Informed Consent
Ensure that participants can understand and provide informed consent, confirming their willingness to participate in the study.
Mathematical Equation:
![]()
Where: Consenti is the informed consent status for participant i, where Yes means consent was given.
Step 6: Exclusion Criteria
Identify exclusion criteria, such as severe cognitive impairments, current participation in another similar program, or inability to engage in the educational program.
Mathematical Equation:
![]()
Where: Exclusioni indicates the exclusion status for participant i based on specified criteria.
Step 7: Selection Process
Apply the inclusion and exclusion criteria to select the final list of participants for the study.
Mathematical Equation:
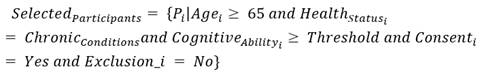
Where: SelectedParticipants represents the final group of participants who meet all inclusion criteria and do not meet any exclusion criteria.
Data collection methods
Surveys, interviews, focus groups
To get both numeric and qualitative data from people, a mix of polls, interviews, and focus groups will be used to collect the data. Standardised information about the subjects' health, living habits, and how they felt about their quality of life before and after the healthcare education program will be gathered through surveys. There will be closed-ended questions in the polls that are meant to measure certain parts of health and well-being, like mental health, physical health, and social connection. Some of the people who took part in the healthcare education program will be interviewed in more depth to find out about their personal experiences with it. We will learn more about how the program changed their daily lives, health attitudes, and sense of freedom through these semi-structured conversations. People who take part will be urged to easily share their ideas, which will give us useful information about the subjective parts of healthcare education. Focus groups will be used as an extra research method to look into how groups work and what experiences people share as a whole. People will be put into groups based on things like age, health, or where they live so that they can talk about problems and wins they have in common. This method will let us look at how healthcare education affects quality of life from different points of view, as well as the social parts of learning with a group.
Tools for measuring quality of life
Standardized questionnaires, scales, assessments
The respondents' quality of life both before and after the healthcare education programme will be assessed using standardised instruments. Older persons have found these long-standing instruments to be useful for a great length. Physical and mental health will be measured mostly using the WHOQOL-BREF, a well-known quality of life evaluation with four areas: physical health, mental health, social relationships, and environment. This instrument will enable one to monitor changes in users' quality of life in many various spheres. The research will make advantage of the EQ-5D as well as the WHOQOL-BREF. In five domains movement, self-care, routine tasks, pain or discomfort, and concern or sadness the EQ-5D measures health-related quality of life. The EQ-5D will provide a more realistic assessment of your physical and psychological condition. For the social aspect of quality of life, the Social Support Questionnaire (SSQ) will be used to ascertain individuals' degree of involvement in their social networks and number of accessible support networks. This tool will find out how linked the people who are taking part are to their neighbourhoods and how much mental and physical help they get from family, friends, and co-workers. Along with these standardised tools, researchers will come up with questions that focus on specific parts of healthcare education, like learning how to handle oneself, remembering what you've learnt, and changing your behaviour. These two sets of tools will work together to give a full picture of how the healthcare education program improved the quality of life of its members.
Step 1: Selection of Relevant Tools
Choose appropriate standardized tools for measuring various dimensions of quality of life (e.g., WHOQOL-BREF, EQ-5D, PHQ-9, GAD-7, Rosenberg Self-Esteem Scale).
Mathematical Equation:
![]()
Where: each dimension (e.g., physical health, psychological health, social wellbeing) is assessed by summing the item scores in the relevant questionnaire.
Step 2: Administer Questionnaires
Administer the selected questionnaires to participants. Ensure clarity in the instructions to minimize errors in responses.
Mathematical Equation:
For each participant, Pi, administer the questionnaire with N items, where each item has a score between Smin and Smax:
![]()
Where: sn is the score for each item.
Step 3: Score Calculation
Convert responses into numerical scores using the scoring guidelines of each tool (e.g., a scale from 0 to 4 or 0 to 10 for each item).
Mathematical Equation:
![]()
Where: sn is the
score for each item, and N is the number of items.
Step 4: Normalization of Scores
Normalize the scores (if necessary) to make them comparable across different dimensions or scales.
Mathematical Equation:
![]()
Where: Smin and Smax are the minimum and maximum scores, respectively.
Step 5: Assessment of Each Quality of Life Domain
Calculate the scores for each specific domain of quality of life (e.g., physical health, psychological health, social engagement) based on the relevant items in the questionnaire.
Mathematical Equation:
![]()
For example, the physical health domain might include items related to pain, mobility, and sleep quality.
Step 6: Calculate Overall Quality of Life Score
Combine the domain scores to calculate an overall quality of life score.
Mathematical Equation:
![]()
Step 7: Interpretation and Analysis
Analyze the overall score and domain-specific scores to evaluate the quality of life of participants. Use statistical methods to identify significant changes or differences between groups (e.g., pre- and post-education).
Mathematical Equation:
![]()
Where: QOLpost and QOLpre are the overall quality of life scores after and before education, respectively.
The impact of healthcare education on aging populations
Physical health outcomes
Older persons are taught, for instance, how to manage common chronic conditions such diabetes, high blood pressure, arthritis, and heart disease by means of lifestyle modification, medication adherence, and consistent health monitoring under healthcare education programs. Older persons who participate in healthcare education initiatives have been shown to be more suited to manage their chronic illnesses according to studies. Their symptoms are therefore more under control and issues are less likely to arise. Programs teaching individuals about food, exercise, and weight management, for example, have been demonstrated to help diabetics better regulate their blood sugar and assist those with high blood pressure reduce their blood pressure. Many health education initiatives also heavily rely on physical exercise. Regular exercise has been linked in studies to improved mobility, strength, and balance in elderly persons, therefore reducing their chance of falling and breaking a bone. Older persons benefit from healthcare education not just in terms of managing chronic conditions but also in terms of understanding the need of vaccinations, testing, and yearly medical visits. By using preventive health strategies, older persons may reduce their risk of significant medical issues and enhance their overall physical condition. Figure 2 illustrates how knowledge about healthcare may let elderly people lead longer and better lives. Learning about healthcare so results in a longer and healthier life with less hospital visits, less healthcare expenses, and more freedom.
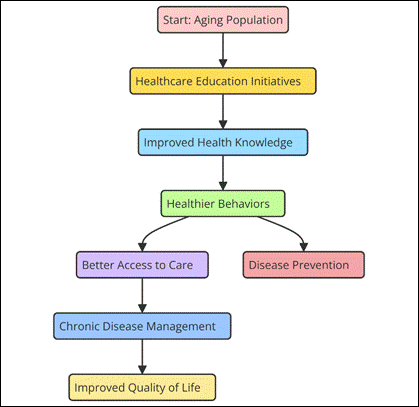
Figure 2. Impact of Healthcare Education on Aging Populations
Psychological well-being
Particularly for elderly persons who could suffer from depression, anxiety, and loneliness, general quality of life revolves heavily on mental health. Improving mental health mostly depends on healthcare education as it provides older people with the knowledge and tools they need to handle the social and psychological challenges of ageing. People may discover techniques to be more emotionally strong and maintain a healthy perspective on life by means of training programs that teach them how to handle anxiety, manage their emotions, and take care of their mental health. Studies reveal that elderly persons who participate in healthcare education initiatives have much improved mental health.
Social interaction and engagement
These events provide elderly people with a purpose to life and an opportunity to change their surroundings, which would increase their contentment and happiness. Furthermore, knowledge of healthcare helps elderly people become more active in looking for social events as they understand the need of maintaining strong social connections and developing meaningful relationships. Healthcare education may also concentrate on the social elements influencing health, such as financial, transportation, and social support accessibility. By informing older individuals about services and community resources that are accessible, healthcare education programs assist they get around social and practical issues that can interfere with their keeping social active and engaged.
Challenges in delivering healthcare education to aging populations
Accessibility and availability of programs
Making sure that all older adults can access and use these programs is one of the hardest parts of teaching older people about healthcare, especially those who live in neglected or rural areas. Many older people have big problems getting to healthcare education because they can't get to educational centres easily, especially in rural or remote areas. These people might not have a way to get to meetings, seminars, or classes in person, which would make it harder for them to take part in these programs. When this happens, different ways of delivering the message, like online classes, might be able to help. However, some older people still have trouble getting online and learning how to use technology properly, which makes digital sites less useful for teaching about healthcare. Furthermore often restricted access is a lack of resources or money. Many community-based initiatives rely on government or non-profit funds, which isn't always sufficient to sustain big-scale educational initiatives. Older persons may therefore not be able to access as many free or inexpensive training courses, particularly if such programs are not included into regular medical treatments. Even with their availability, there could not be sufficient initiatives to satisfy everyone's demands. This might provide restricted opportunities for involvement or waiting queues. Developing strategies to contact elderly people where they reside will help to tackle these problems with access and availability. Good examples are mobile healthcare education programs, community group collaboration, and home learning utilising virtual technologies.
Cognitive and technological barriers
Teaching elderly people about healthcare is challenging as technological issues exist and their brains are degrading. As one ages, many people's cognitive skills including memory, attentiveness, and reasoning speed get poorer. For elderly adults with memory loss or neurological issues, for instance, training materials designed for younger people might not be as effective. Older persons also could find it difficult to recall key health management techniques or grasp a lot of facts. Therefore, employing basic, repeated lectures and allowing students opportunities to practice what they have acquired helps healthcare education programs to be created to match the requirements of persons with various degrees of cognitive capacity. Furthermore, technical issues complicate the teaching of elderly persons about health care. Seniors especially those without much technological experience may find it difficult to utilise the digital tools many educational programs increasingly rely on. Older adults may find it more difficult to participate in digital-based learning if they lack knowledge on how to utilise internet sites, apps, or digital communication tools like video conferences. If an older person has restricted mobility or poor vision, they might also find it difficult to use technology such computers, cell phones, and tablets. Healthcare education must use larger writing, visual tools, voice guidance, and simple-to-use platforms to help one get over these mental and technological issues. Additionally employed should be in-person meetings, small group discussions, and practical exercises to let individuals learn more and ensure that those with cognitive issues might gain from the teachings. Training courses should also be developed to educate elderly individual’s basic digital skills that will enable them to become more tech-savvy and facilitate their use of technology.
Cultural and language considerations
Healthcare education initiatives for elderly persons should include their language and culture. This is so because the degree of effectiveness of these initiatives relies on their ability to engage many senior groups. Older persons are not all the same. From many backgrounds, everyone has unique values, beliefs, and practices around health, illness, and exercise. Programs for healthcare education that ignore cultural variations run the danger of not functioning or maybe alienating certain communities. For example, medical treatments and approaches might vary greatly amongst nations depending on their respective systems. Traditional medicine may be more valued in certain nations than contemporary medicine, and elderly individuals could be more willing to believe practices handed down through the years. Under these circumstances, healthcare education initiatives must embrace cultural cultures while also applying strategies shown to be successful for enhancing health and well-being. Ignoring cultural variations might cause individuals not to heed medical advice. Language obstacles may create problems. Many elderly persons from their native countries may speak languages different than the official one. This might make it difficult for them to attend to class, grasp assignments, or participate in presentations. This language barrier may exclude individuals from significant opportunities for health education, therefore affecting the health outcomes. Programs should include materials and interpreters in many languages as well as information sensitive to many cultures and fits the particular requirements of every community so that all older people may get healthcare knowledge.
Case studies or examples of effective healthcare education programs
Successful models of healthcare education for the elderly
Many successful approaches of healthcare education have been used to support the health and quality of life of elderly persons. Designed at Stanford University, the Chronic Disease Self-Management Program (CDSMP) is one well-known example. This program aims to provide individuals with long-term conditions such diabetes, heart disease, and arthritis with the tools and confidence need to improve their health. Through participation seminars, people learn how to manage their symptoms, food, exercise program, medicines, and stress. Older adults are more likely to learn when they can interact with other people experiencing the same health issues; hence the peer support component of the program has worked very well. The Health Buddy Program, which uses technology to provide elderly persons with long-term ailments tailored health education, also shows great success. Under this program, participants use a device at home that tracks symptoms, asks questions about their health, and offers tailored health advice. It allows elderly persons to monitor their health from home and obtain fast comments from medical professionals. This helps self-management and reduces visits to the hospital. "A Matter of Balance" and "A Matter of Balance" are other initiatives that have shown successful in preventing falls among elderly persons. Teaching individuals how to overcome their fear of falling and enhance their balance, strength, and flexibility is the primary objectives of this program. It has been extensively employed in hospital environments and community centres; those who have used it have claimed less falls and improved mobility. These illustrations demonstrate the many ways that effective healthcare education initiatives for the elderly could take place from in-person seminars to online courses. These initiatives mostly aim to provide elderly persons with the means to take control of their health and enhance their overall welfare.
Best practices for program implementation
To be effective, healthcare education programs for elderly persons must be meticulously organised, easily available, and engage a great number of diverse individuals. Making ensuring the instructional resources are presented in an understandable, straightforward, and intriguing manner for the individuals you want to target can help you to ensure that a program is successful. Older persons' programs should be developed with consideration for their physical and mental constraints; they should also make sense using large lettering, visual aids, and voice instructions. To guarantee that the program is correct and beneficial, it is also crucial to include healthcare professionals in the creation and execution of it. Since older individuals may have different methods of learning and need more aid to completely grasp difficult health concepts, teachers should learn how to approach them clearly. Older adults are more inclined to engage in events that enable them to feel connected and a part of a community, so peer support and social interaction are also rather crucial. Group activities or small meetings let people share experiences and help each other, which keeps people interested and helps them remember things. Another important factor is how flexible the program delivery is. A lot of different older adults will be able to receive and gain from the education if there are classes in many languages and cultural respect is maintained.
Outcomes from real-world applications
Implementing healthcare education programs for older people in the real world has shown to have big benefits, both in terms of improving health and quality of life. For example, the Chronic Disease Self-Management Program (CDSMP) has been used a lot in the US and other countries, and the results show that people are using healthcare a lot less. Participants said they went to the emergency room and hospital less often because they were better able to handle their conditions after learning self-management skills in the program. It was also seen that pain control, physical performance, and mental health all got better. Older persons who participate in the "A Matter of Balance" program have demonstrated in studies to be less likely to fall and have greater trust in their capacity to walk safely. Those included in the research reported up to thirty percent less injuries connected to falls. This not only enhanced their health but also helped to lower treatment and medical care expenditures. Positive outcomes have also emerged from the Health Buddy Program. Older users of the system were more likely to follow their treatment programs, better grasp their illnesses, and be satisfied with their medical providers.
RESULT AND DISCUSSION
The studies found that the ones involved in the whole healthcare schooling application had a lot greater high-quality of living. Bodily health confirmed effects protected progressed mobility, extended bodily hobby, and better management of chronic situations. Individuals pronounced advanced intellectual state, less signs of hysteria and depression, and accelerated emotional strength. Older parents additionally commenced taking part in greater local activities and claiming improved social ties. These results support the idea that healthcare education gives older people more power, which leads to better health outcomes, better mental health, and more social interaction. The results show how important it is to have easy access to comprehensive healthcare education in order to encourage good ageing.
|
Table 2. Changes in Physical Health Outcomes |
||
|
Parameter |
Pre-Education Score (%) |
Post-Education Score (%) |
|
Chronic Condition Management |
53 |
80 |
|
Physical Activity Level |
45 |
71 |
|
Mobility (Walking Distance) |
60 |
95 |
|
Health Self-Assessment |
58 |
72 |
The data in table 2 show that people's physical health got a lot better after the healthcare education program. First, there was a big jump in Chronic Condition Management, from 53 % to 80 %. This means that the people who took part got a better handle on their long-term conditions. Figure 2 shows the differences between scores before and after schooling, showing gains in a number of health areas.
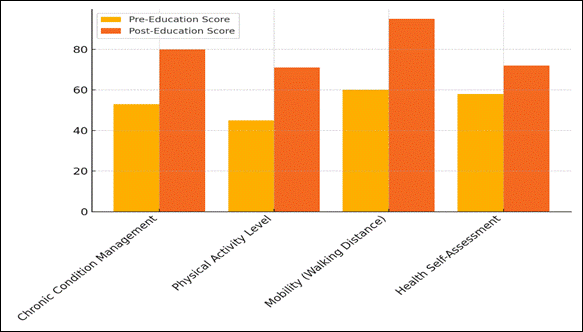
Figure 2. Comparison of Pre-Education and Post-Education Scores Across Parameters
This probably happened because they learnt more about how to manage their symptoms, take their medications as prescribed, and stay healthy.
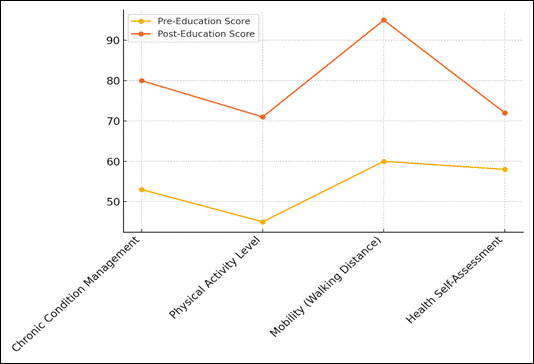
Figure 3. Trends in Scores Before and After Education Across Parameters
Trends in scores before and after schooling can be seen in figure 3. This shows that different health factors got better. The rise shows that schooling gave people the tools they needed to make health-related choices. The Level of Physical Activity also got a lot better, going from 45 % to 71 %. Figure 4 shows how the results before and after schooling added up, showing that total improvement was seen.
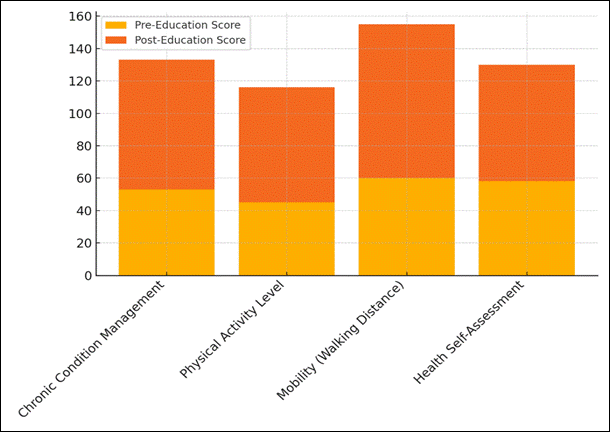
Figure 4. Cumulative Contribution of Scores Pre and Post Education
This shows that the people who took part became more active, possibly after learning how exercise can help keep you healthy and lower your risk of getting chronic illnesses. The Mobility (Walking Distance) score went from 60 % to 95 %, which is a big jump. This change shows better movement, which could be because of the exercises in the program that were meant to improve strength, flexibility, and balance.
|
Table 3. Changes in Psychological and Social Wellbeing |
||
|
Parameter |
Pre-Education Score (%) |
Post-Education Score (%) |
|
Depression Level (PHQ-9 Score) |
62 |
40 |
|
Anxiety Level (GAD-7 Score) |
67 |
44 |
|
Social Engagement (Frequency) |
40 |
70 |
|
Self-Esteem (Rosenberg Scale) |
56 |
71 |
The changes for the better in mental and physical health after the healthcare education program are shown in Table 3. First, the Depression Level (PHQ-9 Score) dropped from 62 % to 40 %, which is a big change. This shows that participants' depressed symptoms got a lot better. This could be because they got mental support and learnt new ways to deal with problems during the education program. This likely happened because people learnt more about how to deal with long-term health problems and make their general health better. Also, there was a big drop in the anxiety level (GAD-7 Score), which went from 67 % to 44 %. Figure 5 shows results before and after education in a number of areas. It shows big gains in important areas like health knowledge, self-care habits, and overall well-being. This shows that educational programs work for older people.
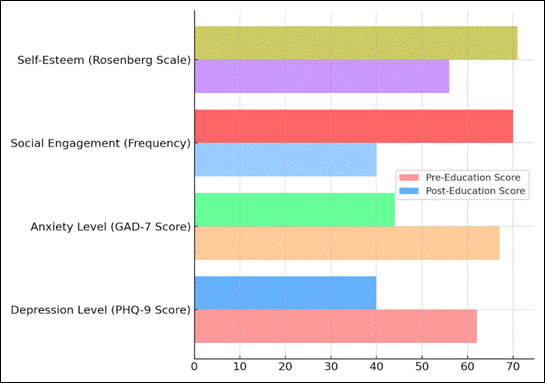
Figure 5. Comparison of Pre-Education and Post-Education Scores Across Parameters
This drop shows that people felt less anxious, which could be because the program focused on stress management, relaxation, and boosting health confidence.
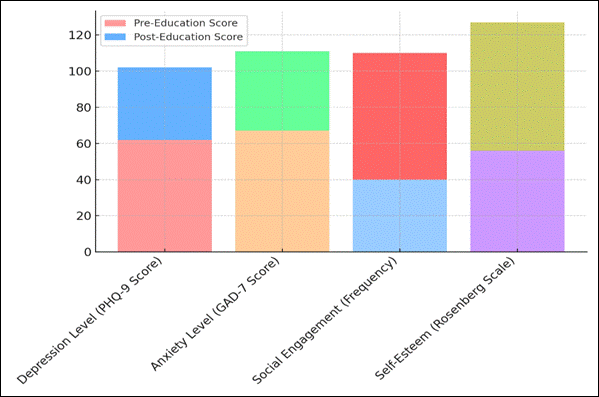
Figure 6. Stacked Representation of Pre-Education and Post-Education Scores Across Parameters
The number went up from 40 % to 70 % for Social Engagement (Frequency), which means there was more social contact and community participation. Figure 6 shows stacked examples of scores from before and after education across a number of parameters. It shows how each parameter changed and how educational approaches led to gains in knowledge and skills. It's likely that the program helped people make friends, which made them feel less alone.
CONCLUSIONS
The world's ageing population faces many health problems, from long-term illnesses to mental health issues and being alone. This study shows how important it is to teach older people about all aspects of healthcare in order to improve their quality of life. Giving elderly people tailored education including the physical, psychological, and social aspects of health helps them to better regulate their well-being and make wise decisions about their well-being. By helping older persons in managing chronic diseases, changing their behaviour, and participating in preventative care, the research indicates that healthcare education programs may significantly improve their physical state. In terms of mental health, those that participated in healthcare education had far better results with reduced worry, melancholy, and stress. These courses gave senior citizens skills that would boost their confidence and enable them to handle social and psychological problems accompanying ageing. Furthermore, greater social engagement and neighbourhood activities brought about by healthcare education helped to lower loneliness and strengthen social ties. These are decent numbers, but implementing such sorts of initiatives still presents challenges. Among these challenges are cultural ones, entrance barriers, technological and intellectual flaws. Eliminating these obstacles by means of tailored, easily available programs responsive to various cultures would help to ensure that all elderly people may gain from healthcare education.
BIBLIOGRAPHIC REFERENCES
1. Dzhalilova, D.S.; Makarova, O.V. The Role of Hypoxia-Inducible Factor in the Mechanisms of Aging. Biochemistry 2022, 87, 995–1014.
2. Leyane, T.S.; Jere, S.W.; Houreld, N.N. Oxidative Stress in Ageing and Chronic Degenerative Pathologies: Molecular Mechanisms Involved in Counteracting Oxidative Stress and Chronic Inflammation. Int. J. Mol. Sci. 2022, 23, 7273.
3. Frimat, M.; Daroux, M.; Litke, R.; Nevière, R.; Tessier, F.J.; Boulanger, E. Kidney, heart and brain: Three organs targeted by ageing and glycation. Clin. Sci. 2017, 131, 1069–1092.
4. Borges, G.; Criqui, M.; Harrington, L. Tieing together loose ends: Telomere instability in cancer and aging. Mol. Oncol. 2022, 16, 3380–3396
5. Frias, C.; Pampalona, J.; Genesca, A.; Tusell, L. Telomere dysfunction and genome instability. Front. Biosci. 2012, 17, 2181–2196.
6. Stahl, S.T.; Emanuel, J.; Albert, S.M.; Dew, M.A.; Schulz, R.; Robbins-Welty, G.; Reynolds, C.F., 3rd. Design and Rationale for a Technology-Based Healthy Lifestyle Intervention in Older Adults Grieving the Loss of a Spouse. Contemp. Clin. Trials Commun. 2017, 8, 99–105.
7. Shu, Z.; Xiao, J.; Dai, X.; Han, Y.; Liu, Y. Effect of family “upward” intergenerational support on the health of rural elderly in China: Evidence from Chinese Longitudinal Healthy Longevity Survey. PLoS ONE 2021, 16, e0253131.
8. Hambisa, M.T.; Dolja-Gore, X.; Byles, J.E. A longitudinal analysis of factors associated with age-related cataract among older Australian women: A cohort study of 7851 older Australian women 79–90 years. Ir. J. Med Sci. 2022, 192, 1525–1536.
9. P.Gurumurthy, S.Raja. (2015). Manage Your Work, Manage Your Life. International Journal on Research and Development - A Management Review, 4(3), 1 - 4.
10. K. Ram Prasad. (2015). Assessing Market Opportunities through Research. International Journal on Research and Development - A Management Review, 4(3), 5 - 7.
11. Kobayashi, L.C.; Westrick, A.C.; Doshi, A.; Ellis, K.R.; Jones, C.R.; LaPensee, E.; Mondul, A.M.; Mullins, M.A.; Wallner, L.P. New directions in cancer and aging: State of the science and recommendations to improve the quality of evidence on the intersection of aging with cancer control. Cancer 2022, 128, 1730–1737.
12. Kruk, J.; Aboul-Enein, B.H.; Bernstein, J.; Gronostaj, M. Psychological Stress and Cellular Aging in Cancer: A Meta-Analysis. Oxidative Med. Cell. Longev. 2019, 2019, 1270397.
13. Ness, K.K.; Wogksch, M.D. Frailty and aging in cancer survivors. Transl. Res. 2020, 221, 65–82.
14. Moghaddam, H.R.; Sobhi, E.; Soola, A.H. Determinants of quality of life among elderly patients with type 2 diabetes in northwest of iran: Based on problem areas in diabetes. Front. Endocrinol. 2022, 13, 924451.
15. Palarino, J.V.; Boardman, J.D.; Rogers, R.G. Cognition and diabetes: Examining sex differences using a longitudinal sample of older adults. Res. Aging 2022, 45, 161–172.
FINANCING
The authors did not receive financing for the development of this research.
CONFLICT OF INTEREST
The authors declare that there is no conflict of interest.
AUTHORSHIP CONTRIBUTION
Data curation: Jamuna KV, Ganesh Thorat, Manju Kundu, Satyasarathi Jena, Ram Garg.
Formal analysis: Jamuna KV, Ganesh Thorat, Manju Kundu, Satyasarathi Jena, Ram Garg.
Drafting - original draft: Jamuna KV, Ganesh Thorat, Manju Kundu, Satyasarathi Jena, Ram Garg.
Writing - proofreading and editing: Jamuna KV, Ganesh Thorat, Manju Kundu, Satyasarathi Jena, Ram Garg.