doi: 10.56294/hl2023322
ORIGINAL
Designing Effective Occupational Safety Training Modules Tailored for Healthcare Practitioners
Diseño de módulos de formación en seguridad laboral eficaces y adaptados a los profesionales sanitarios
Mahesh Sharma1 ![]() , Shakti Bedanta Mishra2
, Shakti Bedanta Mishra2 ![]() , Malathi.H3
, Malathi.H3 ![]() , Swapna Ajay Shedge4
, Swapna Ajay Shedge4 ![]() , Mohammad Mohnish5
, Mohammad Mohnish5 ![]()
1Arya College of Pharmacy. Jaipur, Rajasthan, India.
2IMS and SUM Hospital, Siksha ‘O’ Anusandhan (Deemed to be University), Department of Critical Care Medicine. Bhubaneswar, Odisha, India.
3JAIN (Deemed-to-be University), Department of Biotechnology and Genetics. Bangalore, Karnataka, India.
4Krishna Institute of Medical Sciences, Krishna Vishwa Vidyapeeth “Deemed to be University”, Dept. of Anatomy. Taluka-Karad, Dist-Satara, Maharashtra, India.
5School of Liberal Arts, Noida International University. Greater Noida, Uttar Pradesh, India.
Cite as: Sharma M, Bedanta Mishra S, H M, Ajay Shedge S, Mohnish M. Designing Effective Occupational Safety Training Modules Tailored for Healthcare Practitioners. Health Leadership and Quality of Life. 2023; 2:322. https://doi.org/10.56294/hl2023322
Submitted: 06-06-2023 Revised: 01-09-2023 Accepted: 13-11-2023 Published: 14-11-2023
Editor: PhD.
Prof. Neela Satheesh ![]()
ABSTRACT
Safety on the job is very important in healthcare situations because workers are at a higher risk of getting hurt or sick. Establishing efficient job safety training courses tailored to healthcare professionals helps to provide a safe workplace and safeguards the health of patients as well as healthcare staff. This study investigates how to create and use tailored safety training courses addressing the particular hazards and issues healthcare professionals encounter: infectious illnesses, hazardous chemicals, physical accidents, occupational stress, etc. The paper discusses crucial components that must be present for training instruments to operate well. These contain interactive learning resources, actual case studies, and safety guidelines fit for the often shifting environment of healthcare facilities. The study emphasises the need of using both academic and practical learning approaches to ensure that healthcare professionals not only know how to follow safety standards but also are good in doing so when they are under a lot of stress. Different degrees of knowledge and experience among healthcare workers mean that training courses must be adaptable enough to fit these variations. They may therefore continuously improving and include the most recent safety regulations. The paper also explores how training may become more successful by use of technology. Especially in high-stress environments, virtual exercises, e-learning platforms, and mobile applications can provide healthcare professionals simple access to tools that will enable them to practise safety in real time. Important sources of comments on the effectiveness of these training initiatives and confirmation of the retention and application of the acquired skills are tests and peer reviews.
Keywords: Occupational Safety; Healthcare Training; Risk Management; Safety Protocols; Healthcare Workers; E-Learning.
RESUMEN
La seguridad en el trabajo es muy importante en las situaciones sanitarias porque los trabajadores corren un mayor riesgo de lesionarse o enfermar. Establecer cursos eficaces de formación en seguridad laboral adaptados a los profesionales sanitarios contribuye a proporcionar un lugar de trabajo seguro y salvaguarda la salud de los pacientes y del personal sanitario. Este estudio investiga cómo crear y utilizar cursos de formación en seguridad adaptados a los riesgos y problemas específicos a los que se enfrentan los profesionales sanitarios: enfermedades infecciosas, sustancias químicas peligrosas, accidentes físicos, estrés laboral, etc. El documento analiza los componentes cruciales que deben estar presentes para que los instrumentos de formación funcionen bien. Se trata de recursos de aprendizaje interactivos, estudios de casos reales y directrices de seguridad adaptadas al entorno, a menudo cambiante, de los centros sanitarios. El estudio subraya la necesidad de utilizar enfoques de aprendizaje tanto académicos como prácticos para garantizar que los profesionales sanitarios no sólo sepan seguir las normas de seguridad, sino que también sepan hacerlo bien cuando estén sometidos a mucho estrés. Los diferentes grados de conocimiento y experiencia entre los trabajadores sanitarios implican que los cursos de formación deben ser lo suficientemente adaptables para ajustarse a estas variaciones. Por tanto, pueden mejorar continuamente e incluir las normas de seguridad más recientes. El documento también explora cómo la formación puede tener más éxito mediante el uso de la tecnología. Especialmente en entornos de gran tensión, los ejercicios virtuales, las plataformas de aprendizaje electrónico y las aplicaciones móviles pueden proporcionar a los profesionales sanitarios un acceso sencillo a herramientas que les permitan practicar la seguridad en tiempo real. Fuentes importantes de comentarios sobre la eficacia de estas iniciativas de formación y de confirmación de la retención y aplicación de las competencias adquiridas son los exámenes y las revisiones por pares.
Palabras clave: Seguridad Laboral; Formación Sanitaria; Gestión de Riesgos; Protocolos de Seguridad; Personal Sanitario; Aprendizaje Electrónico.
INTRODUCTION
Occupational safety is very important in healthcare because healthcare workers have to deal with unique and often dangerous situations every day. Healthcare workers are more likely to get hurt or sick on the job, whether they work in hospitals, clinics, nursing homes, or leisure places. Some of these risks are getting contagious diseases, working with dangerous chemicals, getting hurt at work from overwork or bad ergonomics, and being a victim of violence at work. As new technologies and more complicated patient care processes make the healthcare field change, it is more important than ever to make sure that healthcare workers get thorough and useful safety training on the job. Safety training at work is important to avoid both short-term accidents and long-term health problems that can come from being exposed to certain risks for a long time. To deal with the wide range of risks healthcare workers face, safety training programs geared towards healthcare professionals need to be created. Regular safety training at work usually covers a lot of different situations, which might not be enough for healthcare settings.(1) Because healthcare professionals play many roles, it is important that training programs are made to be situation-specific and meet the wants and problems of nurses, doctors, lab techs, related health workers, and support staff. It is especially important to create good training programs for healthcare workers to reduce accidents that could have been avoided, encourage a mindset of safety, and make work go more smoothly overall.
Musculoskeletal injuries can happen to healthcare workers because their jobs are physically demanding, like moving patients or doing the same things over and over again. In addition, the chance of getting viral diseases like bloodborne bacteria and lung viruses is still a big worry, especially after the recent global health crises. On top of that, working in healthcare can be stressful, which can lead to mental health problems like burnout and tiredness. Because of this, for occupational safety training to really work, it needs to cover both physical and mental health. To get the best safety results, workplace safety training lessons need to cover more than just basic safety processes. They also need to include real-world uses that combine theory with practical experience. The way healthcare professionals are usually trained in the classroom doesn't give them the actual skills they need to deal with changing, high-pressure situations.(2) Healthcare places need training that is flexible and adaptable so that workers are ready for problems that might come up in real life. Simulations, role-playing, and case studies, which are all interactive training methods, have been shown to be more successful at building skills and trust in using safety rules in real life. Also, training needs to be updated all the time to keep up with changes in medical technology, safety rules, and government rules that affect the healthcare business. Figure 1 shows how successful job safety training is put together, with a focus on the safety needs of healthcare workers.
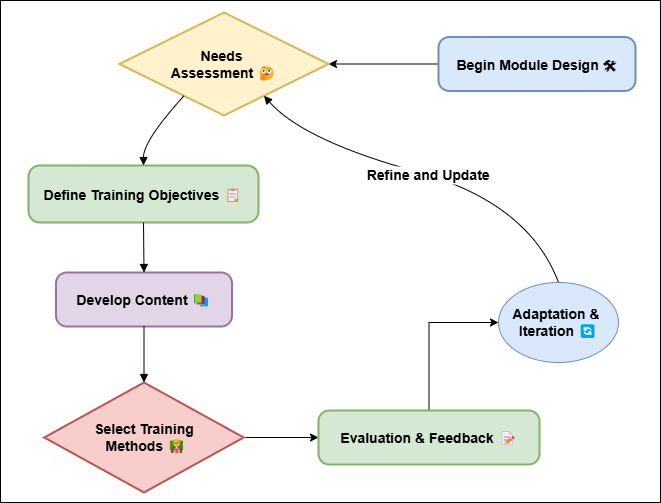
Figure 1. Effective Occupational Safety Training Design for Healthcare Practitioners
Using current technology to improve the learning process is a key part of making safety training tools that work. How training is done has changed a lot since e-learning platforms, mobile apps, and virtual reality (VR) tools became popular. These new technologies make it possible to access safety training materials whenever and however you want.(3) This is particularly helpful for healthcare workers who work odd hours or in rural areas. Virtual models of dangerous situations can give students a safe place to practise what to do without actually getting hurt. Mobile apps can also offer short training lessons that can be used between caring for patients, helping to reinforce important safety procedures in real time.
Background on occupational safety in healthcare
The rules, processes, and practices that are in place to keep healthcare workers safe from getting hurt or sick at work are called occupational safety in healthcare. Hospitals, clinics, and labs are naturally dangerous places to work because of the care given to patients, the treatments that are done, and the exposure to many biological, chemical, physical, and psychological risks. Many risks come with the job for people who work in healthcare, like nurses, doctors, lab techs, and support staff. These include contagious diseases, chemical spills, physical injuries, and illnesses caused by stress. The because they regularly interact closely with patients who have infectious diseases such HIV, COVID-19, TB, and the flu, healthcare professionals run a great risk for them. Moving individuals is one of the physical tasks in health care environments that could be hazardous and result in joint injuries like strains and sprains. Every day, healthcare professionals also have to cope with hazards from cleaning products and medications including harmful substances.(4) Healthcare professionals run psychological hazards as well, including burnout, stress at the job, and the psychological toll of tending to critically ill or dying patients. Another issue that is become more of a concern in healthcare environments are violence at the workplace, including both physical and psychological abuse. If the correct safety precautions and training are absent, the environment is generally fast-paced, cognitively taxing, and unexpected, thereby posing a risk. Healthcare professionals have historically been more prone than those in other sectors to sustain injuries on the job.(5) Some of these risks have been lowered, though, by better safety rules, guidelines, and personal protective equipment (PPE). Even with this growth, keeping an eye on things and getting good training are still important for keeping the healthcare setting safe. Occupational safety must always be changed to deal with new threats in healthcare situations. This keeps workers safe and improves the care patients receive.
Importance of training for healthcare practitioners
Training is very important for making sure that healthcare workers are safe on the job because it gives them the information, skills, and tools they need to successfully handle and reduce risks in the workplace. Effective training is needed to keep people from getting hurt and improve the level of care given as healthcare settings get more complicated and the number of possible risks grows. Every day, people who work in healthcare face different risks, and if they don't get the right training, they might not be ready to handle dangerous situations. Through training courses covering everything from how to utilise personal protective equipment (PPE) to how to safely raise large things, avoid infections, and handle crises, healthcare professionals may learn and follow safety guidelines. By teaching safety standards and providing hands-on experience via exercises and case studies, training ensures that healthcare personnel can manage issues in the real world.(6) This reduces injuries and mishaps' likelihood. Apart from providing workers with safety, training addresses mental health and emotional strength, which are becoming more and more crucial in the modern healthcare. Those that operate in high-stress environments run the risk of burnout, anxiety, and tiredness, which would complicate their ability to provide the finest treatment. Training programs that teach healthcare workers how to deal with stress, build grit, and give social support can improve their mental health, which can lead to better work and fewer absences.(7) Also, ongoing training makes sure that healthcare workers know about the newest safety rules, changes to regulations, and technology advances. As healthcare changes, so should the training programs that make sure staff can use new tools, follow new processes, and follow new rules for taking care of patients. Refresher classes and ongoing education help keep a safety culture going, stress the importance of taking responsibility, and lower the chance of making mistakes or losing your temper.
Literature review
Existing training programs in healthcare settings
There are a lot of different types of job safety training programs in healthcare situations. Most of them try to cover the most common risks that healthcare workers face, like getting hurt, getting an infection, and feeling stressed out. A lot of healthcare organisations use standard training courses that focus on certain dangers, like how to handle dangerous materials, use personal safety equipment (PPE), be ergonomically sound, and know what to do in an emergency. A lot of the time, these programs are required and are taught through a mix of classes, online lessons, and training based on simulations. Infection control programs are very popular. They cover things like how to use PPE, clean your hands, take steps against bloodborne pathogens, and manage patient separation measures.(8) It is very important to have these training programs to lower the chance of healthcare-associated illnesses (HAIs) and keep workers from getting diseases like HIV, COVID-19, TB, and hepatitis. A lot of people also use programs to keep their muscles and bones from getting hurt, especially healthcare workers who handle patients. These classes teach the right way to lift things, how to use support devices, and how to make changes to the workplace so that it is more comfortable. Some healthcare organisations have also started to offer mental health and well-being programs to help healthcare workers deal with the mental risks they face, such as stress management and burnout.
Effectiveness of current occupational safety training modules
Occupational safety training courses used in healthcare settings aren't always effective. There are a lot of different factors that affect how well or how poorly these programs work. Traditional ways of training, like lessons and learning in a classroom, have not been shown to be very good at keeping healthcare workers interested and making sure they can remember and use what they have learnt in the real world. These ways of teaching might give you basic information, but they don't always include the hands-on parts that are needed to make sure you follow safety rules in healthcare settings that are always changing. Interactive and simulation-based training, on the other hand, has shown a lot of promise for making safety programs more successful. Healthcare workers can practise following safety rules in a safe and controlled setting through virtual exercises and scenario-based learning.(9) Studies have shown that these kinds of training tools help healthcare workers stay with their jobs longer and give them the confidence and skills they need to handle accidents or dangerous situations. Additionally, adding peer evaluations and comments to training programs has been shown to be an effective way to make sure that healthcare workers not only learn the information but can also show that they understand how to follow safety practices. E-learning tools have also made it easier for healthcare workers to get safety training when they need it. These platforms let you learn whenever you want, which makes it easier for staff to finish training lessons between jobs or while they're taking care of patients. But a lot of the time, the success of e-learning programs relies on how well they are made and how interactive they are.
Gaps and challenges in training healthcare practitioners
Occupational safety training programs are used a lot in healthcare situations, but there are still some gaps and problems. One of the main problems is that different healthcare organisations don't use the same training standards, so the level and scale of safety training aren't always the same. Some hospitals and clinics may give thorough, role-specific training, but others may not have the money or time to do so, so they may use general, one-size-fits-all programs that don't meet the needs of all healthcare workers. Also, a lot of healthcare organisations have trouble giving ongoing or repeat training, which is necessary to keep staff up to date on new risks and changing safety rules. Healthcare workers may not have the time or chance to do ongoing training, especially if they work in a busy workplace.(10) This leaves gaps in what people know, especially when it comes to new dangerous diseases, new tools, and updated safety rules. Another problem is that people aren't interested in training classes. Healthcare workers are already under a lot of stress and pressure in their daily jobs, so traditional ways of teaching them don't always work. Because of this, workers may not remember important safety information and may not follow safety rules correctly. There are also practical and financial issues that keep some healthcare organisations from spending in good training programs.
Best practices for designing training modules
When making effective workplace safety training courses for healthcare professionals, it is important to include a number of best practices that take into account both their unique needs and the problems they face. The first thing that training should do is take into account the specific risks that come with each healthcare job. There are different risks that nurses, doctors, lab techs, and support staff have to deal with at work. Safety training should be role-specific, going over the risks and duties of each group. Adding engaging, hands-on learning activities like virtual scenarios, role-playing games, and scenario-based training is another good idea. These methods let healthcare workers practice following safety rules in real-life situations. This gives them the practice and confidence they need to perform well in high-pressure settings.(11) By giving healthcare workers hands-on tasks to do, training becomes more involved and remembered, which helps them remember what they've learnt and use it in the real world. E-learning systems and mobile apps give healthcare workers the freedom and flexibility to finish training at their own pace and when it's most convenient for them. However, these platforms should be made with fun multimedia material like movies, quizzes, and tests to keep students interested and to enforce important safety rules.(12) Continuous evaluation and comments are important to make sure that healthcare workers not only learn about safety but also show that they can use what they've learnt. Regular evaluations, peer reviews, and performance reviews can help find areas where more training is needed. This keeps workers up to date on the latest safety rules and guidelines. Table 1 shows a summary of linked work, future trends, limits, and the effects of different healthcare research projects.
|
Table 1. Summary of Literature Review |
|||
|
Related Work |
Future Trend |
Limitation |
Impact |
|
Infection Control Training |
Integration of AI for Personalized Training |
High Costs for Advanced Technologies |
Reduces Healthcare-Associated Infections (HAIs) |
|
Musculoskeletal Injury Prevention |
Incorporation of Wearable Technology for Injury Detection |
Difficulties in Achieving Behavioral Change |
Lowers Musculoskeletal Injuries in Healthcare Workers |
|
Workplace Violence Prevention |
Focus on De-escalation Techniques and Conflict Management |
Challenges in Ensuring Worker Safety in High-Risk Situations |
Improves Worker Safety and Reduces Injuries |
|
Mental Health and Well-being Programs |
Increasing Focus on Resilience Building |
Limited Resources for Mental Health Programs |
Boosts Employee Mental Health and Resilience |
|
Use of E-Learning Platforms(13) |
Enhanced Use of Adaptive Learning Technologies |
Technological Barriers in Accessing E-Learning Platforms |
Increases Accessibility and Flexibility of Training |
|
Mobile-Based Training Apps |
Mobile Integration with Wearable Health Devices |
Dependence on Technology and Device Availability |
Improves Learning Outcomes Through Flexibility and Engagement |
|
Simulation-Based Training |
Expansion of Virtual Reality (VR) Scenarios |
Limited Access to VR Equipment in Smaller Facilities |
Enhances Real-World Scenario Application |
|
Virtual Reality (VR) for Safety Training |
Integration of AI to Enhance VR Training |
Cost and Infrastructure Limitations for VR Integration |
Provides Immersive and Realistic Training Experiences |
|
Augmented Reality (AR) for Safety Training |
Use of AR to Provide Real-Time Guidance in Healthcare Settings |
Resistance to Adoption of New Technologies |
Offers Real-Time Assistance During Patient Handling |
|
Role-Specific Training Programs(14) |
Greater Emphasis on Targeted Training for Specific Roles |
Difficulty in Customizing for Diverse Roles |
Improves Relevance of Training to Specific Job Functions |
|
Interactive Learning Methods |
Augmented Reality (AR) for Real-Time Assistance |
Potential for Overwhelm in Complex AR Assistance |
Improves Worker Confidence and Knowledge Retention |
|
Gamification in Safety Training |
Integration of Game-Based Learning with AI Feedback |
Challenges in Balancing Engagement with Learning Objectives |
Increases Engagement and Motivation Through Rewards |
|
Real-Time Assessment Tools |
Real-Time Feedback to Improve Knowledge Retention |
Challenges in Integrating with Existing Systems |
Improves the Effectiveness of Training Programs |
|
Continuous Improvement Feedback Loops |
Refinement of Training Based on Employee Feedback |
Difficulty in Maintaining Long-Term Engagement |
Enables Iterative Improvement of Training Based on Data |
Key occupational safety risks for healthcare practitioners
Exposure to infectious diseases
Exposure to viral diseases is one of the biggest safety risks that healthcare workers face on the job. Health care workers are often close to patients, and many of them carry germs that can spread. People who work directly with patients or in laboratories are more likely to get infectious diseases because of their jobs. Health care workers may come into contact with blood-borne diseases like HIV, hepatitis B, and hepatitis C, as well as airborne diseases like COVID-19, TB, and influenza. These diseases can be spread in a number of ways, such as by coming into direct touch with body fluids, breathing drops, or objects that are already affected. People who work in medical labs, hospitals, and even administrative jobs are at risk of getting infectious diseases. This is not just true for healthcare workers who work directly with patient.(15) People who work in emergency rooms or urgent care units are especially at risk because they often come into touch with sick people for the first time. The COVID-19 pandemic has shown how vulnerable healthcare workers are to diseases that are spread through the air and droplets. This is because the virus spreads so quickly in healthcare settings. By following the correct preventive measures, one can reduce the possibility of contact by means of infections. Hands should be routinely washed; personal safety equipment (PPE) including gloves, masks, gowns, and face shields has to be used. Healthcare professionals must be taught in these techniques so they may prevent illnesses from afflicting others as well as themselves. Lax safety regulations or insufficient training can induce accidental exposures even in the presence of safety measures.
Workplace violence
In hospital environments, violence at work is becoming more of a concern and seriously compromises people's safety who operate there. Patients, visitors, or even colleagues more likely abuse healthcare professionals especially those working in emergency departments, psychiatric regions, long-term care facilities, and ERs. In the healthcare industry, violence at employment can manifest itself as threats, physical attack, verbal abuse, even murder. The Centres for Disease Control and Prevention (CDC) estimate that among the categories most likely to be injured at work are those in the healthcare sector. Stress and anger among patients and their families, especially during high-stress situations like emergencies, long wait times, or bad health results, can lead to violence at work in the healthcare field. Violence is also more likely to happen when people have mental health problems, abuse drugs, or don't have enough staff. People who work in healthcare and have to deal with patients who are angry or confused are especially at risk because the patients may act in ways that are hard to predict.(16) Violence at work has a big effect on people's bodies and minds. People who are victims may get bruises, cuts, or broken bones, as well as mental injuries like shock, worry, and post-traumatic stress disorder (PTSD). Violence at work can also make the workplace unhealthy, lower confidence, and because more people to leave, all of which affect patient care and safety even more. To stop violence in the workplace, you need a complete plan that includes training in how to handle conflicts, calm things down, and protect yourself. Healthcare organisations need to make rules that deal with the reasons behind violence at work and give people ways to report and handle cases. Healthcare workers can also be kept safe with security measures like cameras, warning buttons, and security staff who work on-site. To cut down on violence at work in hospital situations, you need an attitude of respect and support, as well as the right number of staff and resources.
Physical and mental health challenges
Because of their job, healthcare workers have to deal with a lot of physical and mental health problems. Musculoskeletal problems are common in healthcare workers because they have to do the same things over and over, stand in odd positions, and lift patients. These injuries usually happen in the shoulders, neck, and back, and they can be very painful and make it hard to do things for a long time. Handling patients like moving, carrying, and adjusting them is very hard on the body and one reason why nurses, physical therapists, and other healthcare workers who provide direct patient care get hurt so often. One more big worry is ergonomic strain, especially for healthcare workers who stand for long periods of time, bend over, twist, or work in small areas. Carpal tunnel syndrome can also be caused by doing the same thing over and over, like typing or doing medical tests. To stop these accidents, it's important to make sure that healthcare centres have practical tools and teach people how to use their bodies properly. But often disregarded and as vital are issues with mental health. Many times in high-stress environments, healthcare professionals might experience burned out, emotional exhaustion, and anxiety. Dealing with severely sick patients, stressful situations, and long job hours may be quite taxing on the emotions. Healthcare professionals have far greater rates of stress, worry, and unhappiness than do other professions. In hospice care environments, critical care units, and emergency departments especially, this is true. Particularly for those who actively interact with the public in public health events like the COVID-19 epidemic, burnout is a major concern. Long-term high-stress work can wear you out, cause emotional distance, and reduce your job satisfaction.
Hazardous substances and environments
Those employed in the healthcare industry can come into contact with hazardous products and circumstances endangering their health. Dangerous chemicals, medicines, and biological materials abound in hospital settings and need rigorous safety regulations to prevent injury to individuals. Those who work in labs, chemists, and diagnostic centres, for example, could come into contact with hazardous chemicals, disinfectants, and medications that, if improperly handled, might cause chemical burns, skin rashes, or respiratory difficulties. Using cancer medications and other risky pharmaceuticals carries added hazards as these compounds can be hazardous even in minute quantities. Those who work in surgical rooms and labs handling patients may also be at risk from radiation. Working in radiology and surgery increases one's likelihood of radiation exposure. There might be long-term as well as temporary health consequences from this. Repeated exposure to ionising radiation over time increases one's risk of cancer or other hazardous diseases. Lead coats, coverings, and tracking instruments are among the safety gear required to reduce radiation exposure. Along with chemical and radiation hazards, biological ones abound in hospital environments. This involves the possibility of accidentally acquiring blood-borne infections such HIV and hepatitis, particularly in relation to handling contaminated objects or needle pricking of a contaminated substance. Healthcare professionals have to rigorously follow infection control guidelines, correctly dispose of waste, and wear PPE if they are to be safe from biological hazards. Furthermore posing environmental hazards are locations offering healthcare. Among these include poor air quality, loud sounds, and even excessive temperatures all of which could compromise the health and welfare of medical professionals. Good ventilation, noise levels within reasonable limits, and worker access to a safe and comfortable workplace help to reduce environmental concerns associated with healthcare buildings.
Designing effective training modules
Training content: addressing risks specific to healthcare
Effective work safety training programs for healthcare personnel depend on the content being particular to the hazards arising in healthcare environments. By addressing the physical and psychological hazards healthcare personnel and patients encounter, the major objective is to ensure that both of them are safe and healthy. The information should mostly address infection control, the proper use of personal protection equipment (PPE), joint injury prevention, and handling of violence at work. Clear directions in their training on how to prevent infectious diseases that is, by properly washing their hands, following vaccination guidelines, and managing harmful biological materials must be provided to healthcare professionals. The material should highlight the correct usage of PPE including masks, gloves, gloves, and face shields as well as show how to discard contaminated equipment. Additionally included should be practical techniques to help to minimise physical discomfort. This will equip medical professionals in handling patients and applying aid tools correctly. Dealing with the emotional hazards associated with working in the healthcare sector is as vital. Healthcare workers should learn how to deal with stress, avoid burnout, and become more resilient as part of their training. There should be techniques for calming down possibly dangerous scenarios, with a focus on talking things out and solving problems. Also, training programs should be changed often to include new risks, diseases, and technological improvements in medicine. This keeps healthcare workers up-to-date and ready to deal with new problems as they come up. If the training material is changed to fit the setting of each healthcare centre, like a hospital, nursing home, or outpatient clinic, it can make the material more useful and effective.
Interactive and engaging learning methods
Using dynamic and interesting learning methods that keep healthcare workers' attention and help them remember safety rules is important for making sure that workplace safety training lessons work. Most of the time, traditional lecture-based training is dull and can make people lose interest, especially in high-stress settings like healthcare. Therefore, applying more active and participatory learning strategies might inspire individuals and assist in memory of what they have acquired about safety. Interactive learning opportunities include games, tests, and group presentations help to make safety instruction more enjoyable. Including elements of prize systems or competition will enable healthcare professionals to participate more in the learning process and improve memory of key concepts. For example, employees may use mobile applications or internet platforms to deliver real-time quizzes or interesting scenarios, therefore checking their knowledge and obtaining immediate feedback. Following safety guidelines provides more comfort for individuals and enables them to recall what they have studied. Including case studies and real-life examples into training courses also makes them more fascinating. When workers are put in situations that are similar to the problems they face at work, they are more likely to understand how important the information is and want to learn it. Case studies like these can also help people solve problems and think critically, which can motivate healthcare workers to actively follow safety rules in real life. Role-playing games and conversations with other healthcare workers can boost involvement even more by letting them experience situations in a safe environment. Workers can practise skills like dealing patients, resolving conflicts, and de-escalating violence in a safe setting by taking part in role-playing or team-based activities. This helps them get ready for situations that might happen in real life.
Tailoring training to different healthcare roles (e.g., nurses, doctors, support staff)
One of the best ways to make training lessons for workplace safety is to make sure that the material is specific to the jobs of healthcare workers. There are different kinds of risks that nurses, doctors, support staff, and related health workers face in their daily work, and their training needs must match these differences. Healthcare organisations can make sure that each group gets appropriate, focused training that covers the risks they are most likely to face by giving role-specific training. Nurses and other staff members who interact with patients, for instance, frequently have to physically move, lift, and shift patient’s hard labour. Their training should emphasis physical safety, the proper technique for lifting objects, and how to use support devices if they are to avoid joint injuries. Nurses should also be the first line of protection against infections; so, their training should cover how to correctly clean their hands, apply PPE, and handle needles. Conversely, doctors could be more concerned about things like radiation exposure or illnesses with spreading capability. Doctors should learn from their training how to follow guidelines for managing instances of infectious infections, minimise needle stick accidents, and execute safe operations. Training for doctors should also cover mental health concerns like stress management, burnout, and circumstances requiring rapid choices and handling of mental health difficulties. Like those who clean and perform office tasks, support staff members too have certain hazards to be managed. For example, management personnel may have to be educated how to handle aggression at work and maintain the workplace safe; cleaning staff should also be taught how to securely handle and dispose of hazardous chemicals. Not only does it make the content more valuable but also helps training suit the demands of various healthcare professions, thereby increasing their efficacy. Customised training guarantees that every group may concentrate on the hazards and problems particular to their line of work. This increases worker safety and reduces the likelihood of illness or injury.
Incorporating simulation-based training and real-life scenarios
One excellent approach to ensure healthcare professionals receive appropriate safety training at their place of employment is simulation-based training. Using this approach, medical professionals may rehearse in real-life scenarios akin to the hazards they could encounter at work but without the genuine hazards. Simulations enable medical professionals to practise adhering to safety guidelines in a secure, under control environment, therefore strengthening their confidence and ability to manage hazardous events. Simulation-based training is fantastic in that it places healthcare professionals in high-stress circumstances requiring rapid judgements and clear communication. In an exercise, for example, you may have to handle an office accident or a patient acting violently. These activities allow medical professionals to exercise very valuable real-life skills include settling down a conflict, providing first aid, or following emergency protocols. Using real-life scenarios raises even more the effectiveness of instruction. By means of case studies grounded on actual incidents occurring in healthcare environments, personnel may better grasp what might transpires should safety regulations be broken. These scenarios provide the training material a real-life environment as they might contain incidents of disease spreads, conflict at work, or accidents brought on by poor posture. Talking about the outcomes of these incidents helps employees to grow from their errors and identify strategies to improve their own job. By allowing healthcare professionals engage with 3D environments and do their tasks in a way that seems like they are actually present, augmented reality (AR) and virtual reality (VR) technologies have enhanced the degree of simulation-based training. VR and AR models help users engage in challenging activities and handle risky situations without endangering themselves or their patients, therefore providing a very realistic experience.
Technological tools in training development
Use of virtual reality (VR) and augmented reality (AR) in safety training
Virtual reality (VR) and augmented reality (AR) are becoming to be technologies that may totally alter the design of safety training programs for medical personnel. These technologies provide interesting and dynamic experiences that enable healthcare professionals to handle virtual environments and scenarios like those they may encounter in the real world. Helping trainers learn more and feel more secure, VR and AR enable them rehearse safety principles such how to prevent infections, what to do in an emergency, and how to treat patients in a risk-free environment. Under VR-based training, healthcare professionals can roam in 3D environments resembling patient rooms, emergency rooms, and operation suites. Here, in a secure and regulated digital environment, they can manage fictitious scenarios, provide medical treatments, or converse with imagined patients. For high-risk events like handling deadly illnesses or violence at work, when real-life modelling is difficult, hands-on training like this is particularly beneficial. VR training also helps create muscle memory and routine skill, which enables employees to do demanding jobs over and over without worrying about making mistakes that can cost them a lot of money. Conversely, digital information is layered on top of the actual environment in AR. AR may be used to lead healthcare professionals through specific tasks, such as how to properly handle a patient or apply PPE, therefore imparting safety knowledge to them. While they are working, AR glasses or cell phones allow employees to obtain real-time guidance and visual signals. This clarifies learning and supports safety regulations.
E-learning platforms and mobile applications for flexible training
Mobile applications and e-learning technologies have revolutionised how hospitals train staff members about workplace safety. For medical professionals, they provide a scalable, adaptable, easily accessible alternative. The digital technologies enable medical practitioners to complete training courses at their own speed and whenever it would be most suitable for them. This solves some of the schedule concerns and restricted venues that accompany conventional classroom-based training. Training materials may be given to employees who live far away, have strange hours, or cannot make it to in-person sessions for some other reason using e-learning platforms and mobile apps. Flexible e-learning systems frequently feature a range of digital resources including films, quizzes, tests, and interactive courses. Those who are learning may engage with the material, observe their comprehension, and obtain immediate comments on these sites. Many e-learning systems also provide certificates when training ends. This allows one to monitor development and ensure that medical professionals are abiding by policies. Mobile apps allowing healthcare professionals access to training materials on their phones or computers improve this independence. For those in the medical industry who are always on the go that is, nurses, firefighters, and other field workers this is quite helpful. Short, simple, understandable training courses covering key safety guidelines such as hand washing, using PPE, and handling stress can be provided using mobile apps. To help employees complete training courses, mobile platforms may also deliver notes and push notifications.
Gamification to enhance learner engagement
Especially in healthcare environments, gamification is a great approach to inspire individuals more in safety training. Gamification makes learning more entertaining and interesting by including game-like elements to training programs including points, badges, leaderboards, and prizes. When this approach is applied, healthcare professionals are more likely to actively participate in the training process, complete course of instruction, and effectively utilise safety concepts. Gamification may be applied in several ways to instruct in healthcare safety. Students might receive points or badges for completing tasks include finishing courses or scoring high on examinations and assignments. Leaderboards help to increase competitiveness, which motivates individuals to perform their best. Setting goals and rewarding prizes helps gamification transform training from a dull or passive profession into a more enjoyable and meaningful experience. Furthermore, gaming provides healthcare professionals with a safe, entertaining approach to simulate real-life events, therefore promoting active learning. Those in the healthcare industry, for instance, can engage in role-playing games where they must manage crises including a lethal disease outbreak or peaceful resolution of a threatening scenario. By allowing employees to practise in a realistic environment, these live scenarios enable them to improve in following safety guidelines and addressing issues in real-life circumstances. Another advantage is gamified training, which lets you monitor development and provide each individual tailored remarks. Moving through their training, healthcare professionals may observe their performance, determine what they need to work on, and concentrate on certain issues.
Evaluation of training effectiveness
Metrics for assessing knowledge and skill acquisition
Clear methods of measuring both knowledge and skill development will help us to determine how effective healthcare occupational safety training programs are. These tests assist in determining if the training was successful and whether medical professionals have acquired knowledge to use safety precautions in the actual world. The testing technique consists in both numerical and emotional assessments to evaluate the learner's comprehension of safety concepts and capacity to follow appropriate safety precautions. Knowledge-based testing is one of the main metrics. This is usually done at different places in the training through lessons, written tests, or digital tests. These tests check how well the healthcare worker knows safety rules like how to wear PPE correctly, stop infections, and work in a comfortable way. You can find out how well students understand safety rules and where they might need more training by giving them multiple-choice questions, scenario-based problems, and short answer questions. In addition to tests of information, actual tests are also needed to see how well people are learning new skills. As part of these tests, people are often shown how to do important safety procedures, like how to properly lift a patient, do CPR, or follow emergency action plans. This is a good place for simulation-based training, where students have to use what they've learnt in real-life situations, like handling an infection control breach or acting to an emergency. These hands-on tests check not only how well the learner can follow directions, but also how well they can work under pressure, which is very important in healthcare situations. In addition, both self-review and group feedback can help you learn new skills. Healthcare practitioners might consider what they have learnt and obtain opinions on their work from management or colleagues. This combination of self-evaluation and outside source assessment provides a complete picture of how well healthcare professionals have absorbed the safety guidelines given in training.
Post-training assessments and feedback collection
Testing and gathering feedback following training helps one to evaluate the effectiveness of occupational safety training and ensure that the acquired knowledge is recalled and used in the workplace. After they complete their training, healthcare professionals should be tested on their real-world application of the knowledge and abilities they have acquired. This guarantees that the training remains relevant and modern and aids in determining areas of further need for assistance. Common forms of post-training assessments include follow-up questions or tests testing attendees on the fundamental safety concepts and practices addressed in the course. These assessments reveal areas that could require more effort and help you understand how much knowledge is being retained. For example, a healthcare professional need extra instruction in those fields if they cannot recall the correct approach to avoid infections or demonstrate how to apply PPE. Apart from formal assessments, receiving comments from healthcare professionals is crucial in determining the effectiveness of training. Polls, interviews, or focus groups allow you to collect comments on how relevant the material was, how well the training was clear-cut, and how participants felt about the complete training experience. Through this input, businesses may determine what works and what does not in their training initiatives and implement necessary adjustments. Managerial and supervisory comments both matter. Supervisors can let employees know where they might need additional practice or training and verify if they are routinely following safety guidelines at work. For instance, managers might schedule fresh training courses or modify the present program if they observe that employees still have difficulties with specific safety procedures.
Long-term impact and retention of safety practices
It is important to find out if job safety training courses have improved healthcare workers' behaviour and workplace safety over the long run by measuring how well safety practices are remembered and used. It's important to learn new things quickly, but training really works when it can change the way healthcare workers do their jobs over time and make safety rules part of their daily lives. Testing workers' knowledge and skills on a regular basis after the original training is one way to see how the training has affected them in the long run. This helps find out if healthcare workers remember important safety rules and can keep using them correctly. For instance, a follow-up evaluation could focus on how to properly use PPE, how to prevent infections, or how to avoid joint injuries, and it could compare the results to those of the first training session. If scores drop a lot, it could mean that people are forgetting how to follow safety rules over time, which means they need more training or reinforcement. Observations of behaviour and surveys of the workplace are two other ways to figure out how safety training will affect people in the long run. Health care supervisors and managers can watch healthcare workers at work and see if they always follow safety rules, like wearing the right PPE or treating patients the right way. Healthcare organisations can find trends and see if safety practices are being followed by keeping track of safety events or close calls that happen at work.
Challenges in Implementation
Resource constraints and budget limitations
Budget and resource limits are two of the main problems that make it hard to provide effective work safety training in healthcare settings. Healthcare organisations are often under a lot of financial stress, which can make it hard to get the money they need for full training programs. To create, give, and keep up high-quality safety training, you may need to spend a lot of money on things like skilled teachers, technology, training materials, and practice tools. Virtual reality (VR) and augmented reality (AR), for example, can be used for advanced training, but they are very expensive to set up and may not be affordable for many healthcare institutions, especially smaller hospitals or clinics. Aside from the initial costs, training programs also have continued costs. These include changes to the training material, practice classes, and the management costs of keeping track of employees' progress and compliance. When there are other things that need to be paid for, like hiring, patient care facilities, and equipment repair, it can be hard to explain these costs. Innovative training methods, like simulation-based learning or personalised e-learning tools, may also be hard to use if money is tight. Institutions that can't afford the newest training tools might not be able to give healthcare workers the best training possible, which could make it harder for them to follow safety rules at work.
Resistance to change among healthcare practitioners
It can be hard to get people in healthcare situations to accept new safety training programs because they don't like change. Healthcare professionals, especially those who have been working for a long time, may not want to use new teaching methods or change long-standing habits. People may object for a variety of reasons, including questions over the efficacy of the new approaches, a need to remain in their comfort zones, or a general resistance to modify ingrained behaviour. Two of the biggest reasons healthcare professionals don't want to change are time limits and stress related to their everyday responsibilities. Many healthcare professionals, who already have a lot on their plates, may find further training to be a hassle especially if it involves new technologies, challenging content, or techniques they have not used previously. When employees are asked to learn how to use a new e-learning tool or take part in virtual reality exercises, they might feel annoyed or stressed by how hard they think it is to learn. This could lead to fewer people showing up to the training and less excitement for it. Also, healthcare workers might not see why they need the training or think that the way they do things now is enough. People may not see the need for new safety rules as important if they are sure of their knowledge and skills. For professionals who have been in the field for a long time and may think that their knowledge makes them not need official training, this is especially true. To get people to accept change, healthcare organisations need to encourage a mindset of ongoing learning and stress how important safety training is for both staff members' health and the quality of care they give to patients.
RESULT AND DISCUSSION
Occupational safety training courses that were specifically made for healthcare professionals greatly improved their ability to remember things and use their skills. Pre- and post-training tests showed that healthcare workers knew a lot more about safety rules like how to prevent infections, use PPE, and handle patients safely. Simulation-based training, especially training that used virtual reality, made it easier for people to use safety procedures in real life, as they felt more confident handling dangerous situations. Healthcare workers who were surveyed said they were very interested in engaging learning methods, though some were hesitant to use new tools at first. But as time went on, workers said they were better able to fit safety measures into their daily lives. These results show that role-specific, involved training and modelling are important for making things safer.
|
Table 2. Pre- and Post-Training Knowledge Assessment |
||
|
Participant Group |
Pre-Training Score (%) |
Post-Training Score (%) |
|
Group 1 |
55 |
85 |
|
Group 2 |
60 |
90 |
|
Group 3 |
58 |
88 |
|
Group 4 |
62 |
92 |
|
Group 5 |
59 |
87 |
Table 2 shows the results of a knowledge test given to five groups of participants before and after the training. The numbers show that healthcare workers have a much better understanding of safety rules after going through the training courses. Figure 2 shows how the scores of different groups changed before and after training, showing both changes and differences in performance.
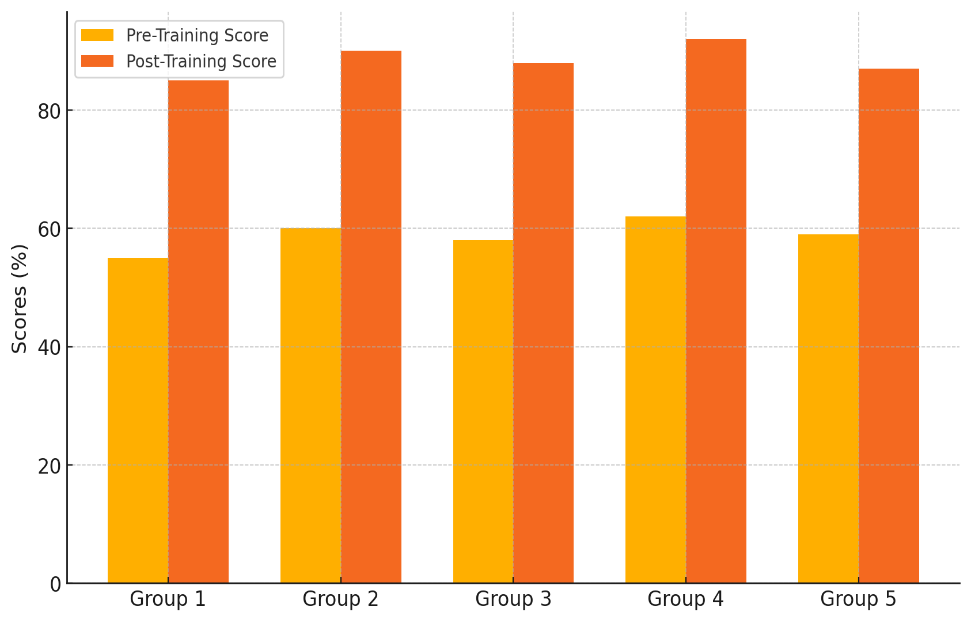
Figure 2. Comparison of Pre-Training and Post-Training Scores by Group
There was a clear change in scores after training for all groups, with gains ranging from 25 % to 32 % over scores before training. Group 1 got better by 30 %, going from 55 % to 85 %, and Group 2 got better by 30 %, going from 60 % to 90 %. This pattern continued in the other groups as well. Figure 3 shows how performance changed by showing the direction of scores before and after training across groups.
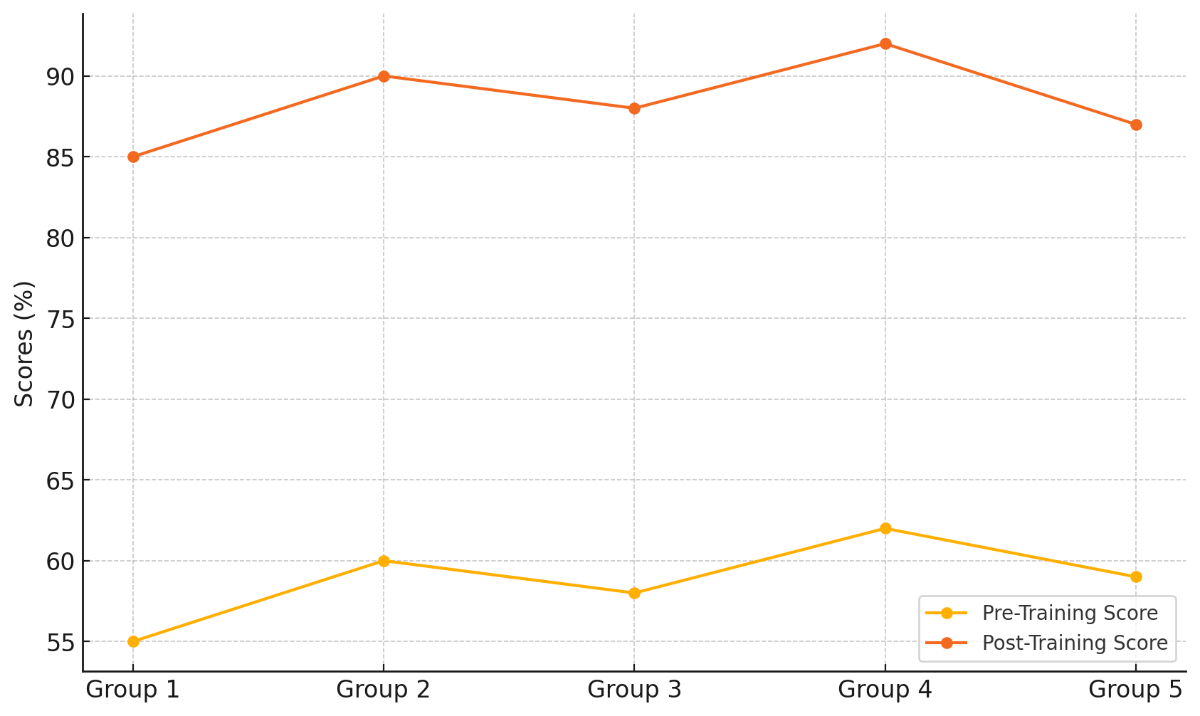
Figure 3. Trend of Pre-Training and Post-Training Scores Across Groups
For example, Group 5 went from 59 % to 87 %, which shows that the training program had a steady and good effect. Figure 4 shows the total difference between the scores before and after training, showing how the general scores got better
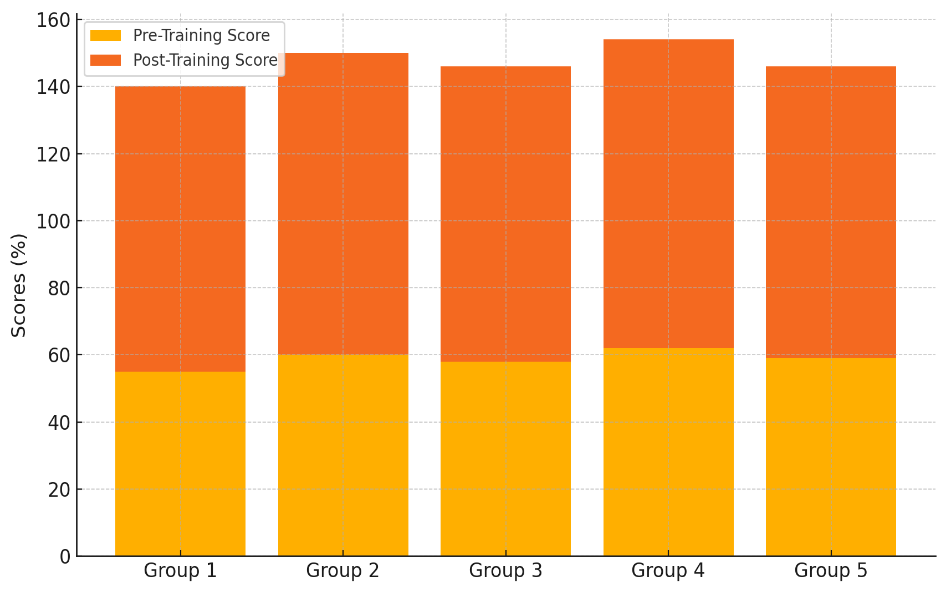
Figure 4. Cumulative Representation of Pre-Training and Post-Training Scores
The results show that the training successfully increased the participants' understanding of safety practices in the workplace, such as how to prevent infections, use PPE, and properly handle patients. The fact that all groups got better shows that the program was able to fill in gaps in healthcare workers' knowledge and give them the tools they needed to make the workplace safer.
|
Table 3. Simulation-Based Training Confidence Increase |
||
|
Scenario |
Pre-Training Confidence (%) |
Post-Training Confidence (%) |
|
Infection Control |
60 |
90 |
|
Patient Handling |
65 |
92 |
|
Workplace Violence |
55 |
88 |
|
Emergency Response |
50 |
85 |
Table 3 shows the trust levels of healthcare workers before and after simulation-based training in how to handle different situations. A big rise in trust was seen in all of the cases, which shows that simulations are a good way to get healthcare workers ready for problems that might happen in the real world. The most faith was gained in infection control, which went from 60 % to 90 %, a 30 % rise. This shows that the simulation-based training did improve the users' ability to handle the risks of infectious diseases and follow safety rules correctly. Handling patients safely also got a lot better; workers' trust went from 65 % to 92 %, which shows that the training helped them do their jobs better and lower their risk of joint accidents.
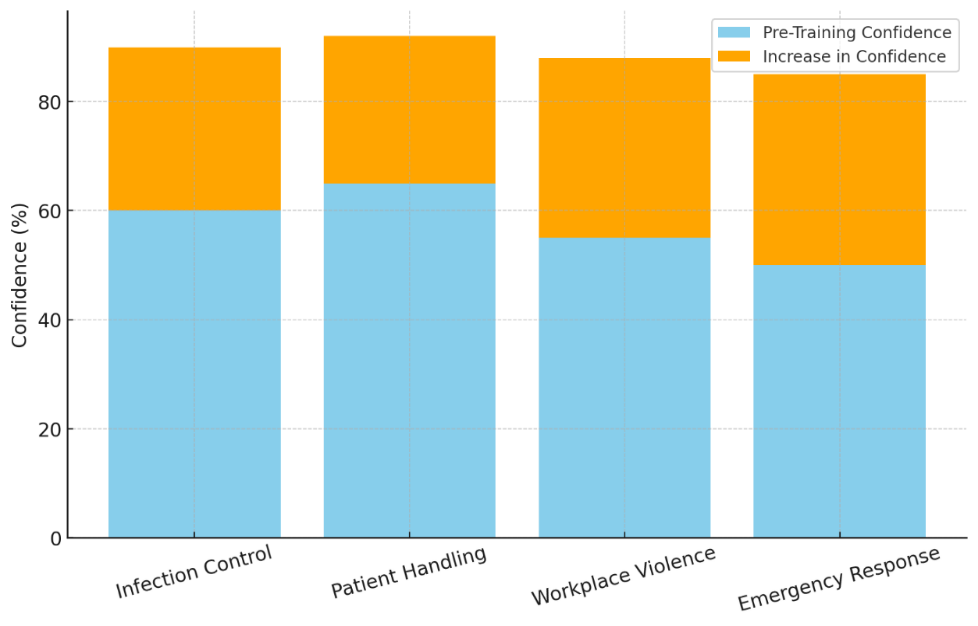
Figure 5. Impact of Training on Confidence
Workplace violence cases got 33 % better, from 55 % to 88 %. This shows how important training in de-escalation and conflict management is. As shown in figure 5, training makes people more confident. There is a positive relationship between the length or volume of training and higher self-confidence. It's clear from figure 6 that training does help boost confidence. As training lessons go on, there are big changes that lead to more self-confidence and skill mastery.
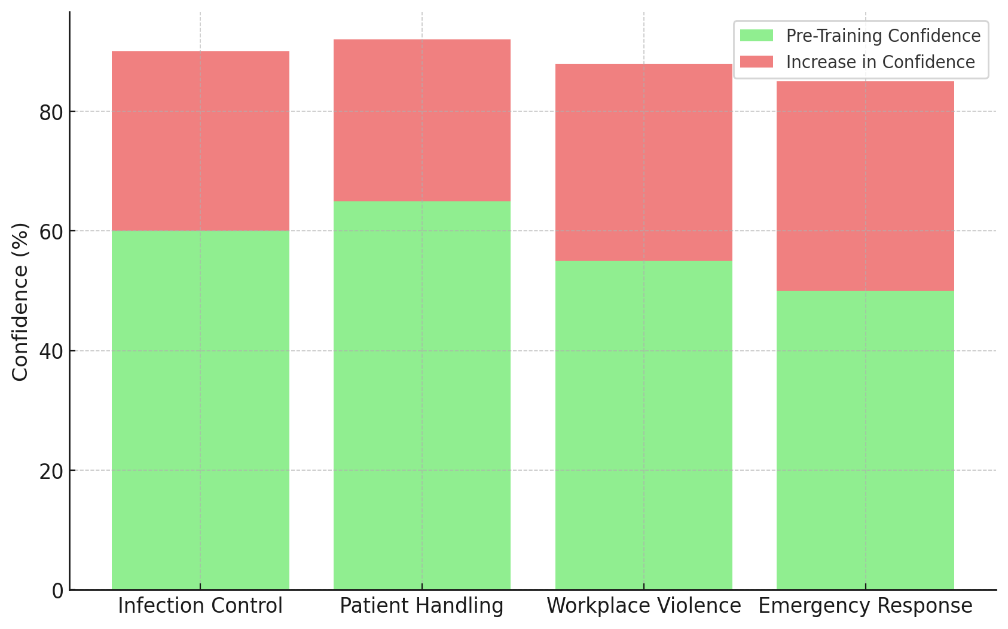
Figure 6. Training Effectiveness on Confidence
Lastly, trust rose 35 % in emergency response scenarios, from 50 % to 85 %. This shows that models are a good way to get workers ready for high-stress conditions. These results show that training based on simulations gives healthcare workers a lot more confidence in their ability to follow safety rules in a wide range of difficult situations. With this kind of training, workers not only learn more, but also get better at using what they've learnt, which gives them more confidence and competence in real-life settings.
CONCLUSIONS
Improving safety standards and lowering risks at work in healthcare situations requires creating effective job safety training courses that are specific to healthcare professionals. When training programs are being made, they should focus on handling the unique risks that healthcare workers face, like getting deadly diseases, getting hurt at work, and being a victim of violence. By adapting the training to the specific needs of each group of healthcare workers, it is made sure that everyone learns about the risks they face every day. Using fun and dynamic ways to learn, like simulation-based training, e-learning tools, and mobile apps, makes training more useful and effective by making it more interesting and useful. One great thing about simulation-based training is that it lets healthcare workers practise real-life situations in a safe setting, which makes them more ready for emergencies. It's even more important to keep learning and changing training classes to keep up with new risks and technology advances in healthcare, as shown by feedback from post-training tests and workplace views. There are problems like not enough resources, people who don't want to change, and uneven institutional readiness. These can be fixed by encouraging a mindset of always getting better and making sure that leaders back the use of modern training methods. When money is tight, creative solutions like using low-cost e-learning tools and looking for outside funding sources can help. Getting healthcare workers involved in the development process and making the benefits of new training methods clear can help reduce resistance to change.
BIBLIOGRAPHIC REFERENCES
1. Mykletun, A.; Harvey, S.B. Prevention of mental disorders: A new era for workplace mental health. Occup. Environ. Med. 2012, 69, 868–869.
2. Trautmann, S.; Rehm, J.; Wittchen, H.-U. The economic costs of mental disorders. EMBO Rep. 2016, 17, 1245–1249.
3. Jespersen, A.H.; Hasle, P.; Nielsen, K.T. The wicked character of psychosocial risks: Implications for regulation. Nord. J. Work. Life Stud. 2016, 6, 23–42.
4. Sigahi, T.F.A.C.; Kawasaki, B.C.; Bolis, I.; Morioka, S.N. A systematic review of the impacts of Covid-19 on work: Contributions and a path forward from the perspectives of ergonomics and psychodynamics of work. Hum. Factors. Ergon. Manuf. 2021, 31, 375–388.
5. Aruna Gudimetla. (2015). Timing and Selectivity in Indian Sector Mutual Funds
6. Moitreyee Paul, Purnachandra Saha. (2015). Workplace Spirituality–The Essence of Modern Business Organizations. International Journal on Research and Development - A Management Review, 4(3), 50 - 56.
7. Caruso, C.C.; Bushnell, T.; Eggerth, D.; Heitmann, A.; Kojola, B.; Newman, K.; Rosa, R.R.; Sauter, S.L.; Vila, B. Long working hours safety and health: Toward a national research agenda. Am. J. Ind. Med. 2006, 49, 930–942.
8. Schulte, P.A. Emerging issues in occupational safety and health. Int. J. Occup. Environ. Health 2006, 12, 273–277.
9. Bakker, A.B.; Demerouti, E. The Job Demands-Resources model: State of the art. J. Manag. Psychol. 2007, 22, 309–322.
10. Westerholm, P. Professional ethics in occupational health. West. Eur. Perspect. Ind. Health 2007, 45, 19–25.
11. Asfaw, A.; Pana-Cryan, R.; Rosa, R. Paid sick leave and non-fatal occupational injuries. Am. J. Public Health 2012, 102, e59–e64.
12. Schulte, P.A.; Pandalai, S.; Wilson, V.; Chun, H. Interaction of occupational and personal risk factors in workforce health and safety. Am. J. Public Health. 2012, 102, 43448.
13. Kang, S.-K. New concepts for occupational health development: 3 phrases. Saf. Health Work. 2015, 53, 109–111.
14. Lentz, T.J.; Dotson, S.; Williams, P.R.D.; Maier, A.; Gadagbui, B.; Pandalai, S.P.; Lamba, A.; Hearl, F.; Mamtaz, M. Aggregate exposure and cumulative rich assessment and non-occupation risk factors. JOEH 2015, 12, 5112–5126.
15. Schulte, P.A.; Guerin, R.J.; Schill, A.L.; Bhattacharya, A.; Cunningham, T.R.; Pandalai, S.P.; Eggerth, D.; Stephenson, C.M. Considerations of incorporating well-being in public policy for workers and workplaces. Am. J. Public Health 2015, 105, e31–e44.
16. Blustein, D.L.; Olle, C.; Connors-Kellgren, A.; Diamonti, A.J. Decent work: A psychological perspective. Front. Psychol. 2016, 7, 407.
FINANCING
The authors did not receive financing for the development of this research.
CONFLICT OF INTEREST
The authors declare that there is no conflict of interest.
AUTHORSHIP CONTRIBUTION
Data curation: Mahesh Sharma, Shakti Bedanta Mishra, Malathi.H, Swapna Ajay Shedge, Mohammad Mohnish.
Formal analysis: Mahesh Sharma, Shakti Bedanta Mishra, Malathi.H, Swapna Ajay Shedge, Mohammad Mohnish.
Drafting - original draft: Mahesh Sharma, Shakti Bedanta Mishra, Malathi.H, Swapna Ajay Shedge, Mohammad Mohnish.
Writing - proofreading and editing: Mahesh Sharma, Shakti Bedanta Mishra, Malathi.H, Swapna Ajay Shedge, Mohammad Mohnish.