doi: 10.56294/hl2023320
ORIGINAL
The Impact of Effective Healthcare Management in Mitigating Medical Errors
El impacto de una gestión sanitaria eficaz en la mitigación de los errores médicos
N.J. Patil1 ![]() , Puneet Yadav2
, Puneet Yadav2 ![]() , Mukesh Sharma3
, Mukesh Sharma3 ![]() , Malathi H4
, Malathi H4 ![]() , Jaya Bhanu Kanwar5
, Jaya Bhanu Kanwar5 ![]()
1Krishna institute of Medical Sciences, Krishna Vishwa Vidyapeeth “Deemed to be University”, Department of Pathology, Taluka-Karad, Dist-Satara, Maharashtra, India.
2School of Liberal Arts, Noida International University, Greater Noida, Uttar Pradesh, India.
3Arya College of Pharmacy, Jaipur, Rajasthan, India.
4JAIN (Deemed-to-be University), Department of Biotechnology and Genetics, Bangalore, Karnataka, India.
5IMS and SUM Hospital, Siksha ‘O’ Anusandhan (Deemed to be University), Department of Endocrinology, Bhubaneswar, Odisha, India.
Cite as: Patil N J, Yadav P, Sharma M, H M, Bhanu Kanwar J. The Impact of Effective Healthcare Management in Mitigating Medical Errors. The Impact of Effective Healthcare Management in Mitigating Medical Errors. Health Leadership and Quality of Life. 2023; 2:320. https://doi.org/10.56294/hl2023320
Submitted: 07-06-2023 Revised: 28-08-2023 Accepted: 27-11-2023 Published: 28-11-2023
Editor: PhD.
Prof. Neela Satheesh ![]()
ABSTRACT
Good healthcare administration helps to prevent medical mistakes, keeps patients safe, and raises the general quality of healthcare provided. Because they affect patients’ outcomes, result in longer hospital stays, and increase healthcare expenses, medical errors are a major global issue. Strong management practices help healthcare institutions to reduce these errors, increase the accuracy of evaluations, enhance treatment plans, and foster a safe atmosphere. Investigating the relationship between better healthcare administration and less medical errors is the aim of this paper. Discussed are important subjects such leadership, communication, training, using technology in healthcare administration that could directly affect reducing mistake rates. Good leadership creates a secure atmosphere where medical experts feel comfortable to report mistakes without thinking about repercussions. This allows one to resolve problems and preserve ongoing environmental progress. Accurate delivery of important patient information to another healthcare provider relies on good communication. This lowers the chance of misunderstanding and false diagnosis. Advanced technologies including electronic health records (EHR), decision support systems (DSS), and artificial intelligence (AI) can help people make better decisions, lower the number of mistakes people make, and provide doctors real-time support in addition to ongoing education and training courses for healthcare personnel. Moreover encouraging openness and guaranteeing better treatment is a patient-centered approach in which individuals participate in choices about their treatment. This article emphasises the need of treating healthcare in such a manner that all of its components cooperate to improve patient care and reduce the error rates. For these reasons, daily application of effective healthcare management strategies is crucial to improve the healthcare system and ensure patient receive quality treatment.
Keywords: Healthcare Management; Medical Errors; Patient Safety; Leadership; Communication.
RESUMEN
Una buena administración sanitaria ayuda a prevenir errores médicos, mantiene a salvo a los pacientes y mejora la calidad general de la asistencia sanitaria prestada. Los errores médicos son un grave problema mundial, ya que afectan a la evolución de los pacientes, prolongan la estancia hospitalaria y aumentan los gastos sanitarios. Unas buenas prácticas de gestión ayudan a las instituciones sanitarias a reducir estos errores, aumentar la precisión de las evaluaciones, mejorar los planes de tratamiento y fomentar un ambiente seguro. El objetivo de este artículo es investigar la relación entre una mejor administración sanitaria y menos errores médicos. Se tratan temas importantes como el liderazgo, la comunicación, la formación y el uso de la tecnología en la administración sanitaria, que podrían influir directamente en la reducción de las tasas de error. Un buen liderazgo crea una atmósfera de seguridad en la que los expertos médicos se sienten cómodos para informar de los errores sin pensar en las repercusiones. Esto permite resolver los problemas y preservar el progreso continuo del entorno. La transmisión precisa de información importante sobre el paciente a otro profesional sanitario depende de una buena comunicación. Así se reducen las posibilidades de malentendidos y falsos diagnósticos. Las tecnologías avanzadas, como las historias clínicas electrónicas (HCE), los sistemas de apoyo a la toma de decisiones (SAD) y la inteligencia artificial (IA), pueden ayudar a las personas a tomar mejores decisiones, reducir el número de errores que cometen y ofrecer a los médicos apoyo en tiempo real, además de cursos de educación y formación continua para el personal sanitario. Además, fomentar la apertura y garantizar un mejor tratamiento es un enfoque centrado en el paciente en el que las personas participan en las decisiones sobre su tratamiento. Este artículo subraya la necesidad de tratar la asistencia sanitaria de forma que todos sus componentes cooperen para mejorar la atención al paciente y reducir los índices de error. Por estas razones, la aplicación diaria de estrategias eficaces de gestión sanitaria es crucial para mejorar el sistema sanitario y garantizar que el paciente reciba un tratamiento de calidad.
Palabras clave: Gestión Sanitaria; Errores Médicos; Seguridad del Paciente; Liderazgo; Comunicación.
INTRODUCTION
An integral aspect of society, the healthcare sector keeps and enhances people’s health and well-being. Medical blunders are still a frequent and significant issue in healthcare environments even if treatment strategies and equipment have advanced greatly. For patients, these errors can have negative outcomes; longer hospital stays, more expensive healthcare, and sometimes death. This emphasises the need of acting fast to resolve this issue. Good healthcare management is ever increasingly crucial as healthcare systems evolve in reducing medical errors and ensuring patient safety. Healthcare management is essentially planning, coordinating, and supervising of healthcare services. Making the best use of resources, enhancing patient care, and ensuring that medical professionals have the tools and support required to deliver safe and efficient treatment are the objectives here. Many locations where healthcare is given have direct correlation with fewer errors by means of well-defined management strategies. Among the elements of healthcare administration are staff training, patient participation, leadership, communication, and application of modern technologies. These all contribute to reduce error risk. Among the biggest causes of errors in the medical industry is inadequate communication among healthcare professionals. Bad communication is a significant source of errors in professional employment, particularly during hand-off or change in care. Incorrect assessments, treatment delays, and incorrect kind of behaviour might result from improper sharing of vital patient information. This makes good management of healthcare mostly dependent on effective communication. Making ensuring healthcare professionals can communicate properly and fast can help to significantly prevent mistakes.
Designed to increase consistency and reduce the possibility of mistakes resulting from misinterpretation, structured communication methods such as the SBAR (Situation-Background-Assessment-Recommendation) approach have Good leadership is also rather crucial in helping to prevent medical errors. Good leaders in their workplaces establish a secure atmosphere whereby staff members feel free to disclose errors without concern of consequences. Leaders that give patient safety top importance and prioritise learning from errors help to foster a responsible culture and ongoing development. Enough said about how crucial it is for hospital executives to establish policies, staff training, and ensure adherence to safety guidelines. Concerned about patient safety leaders may influence the behaviour of medical professionals and ensure that routinely used strategies for error prevention are followed throughout the whole company. Moreover, good management of healthcare depends much on education and training. Healthcare professionals should be aware of the most recent medical discoveries, fresh approaches of patient treatment, and modern technology.(1) Through continuous training courses, clinicians may learn about new safety standards, recognise prospective hazards, and use best practices that help to lower errors. When persons lack appropriate training, mistakes might occur particularly in relation to utilising new instruments or performing complex medical treatments. Furthermore proved to assist significantly reduce errors in various major spheres is the application of technology in healthcare administration. Giving clinician’s real-time access to patient data, assisting them in making choices, and alerting them about probable errors has altered the healthcare industry via Electronic Health Records (EHRs), Decision Support Systems (DSS), and Artificial Intelligence (AI.(2) Electronic health records (EHRs) for instance instantly display drug combinations, allergies, and incorrect dosages, therefore helping to reduce medication errors.
Definition of healthcare management
Healthcare management is the supervision and coordination of healthcare operations and services aimed at ensuring that patient treatment is prompt, efficient, and of highest quality. This implies monitoring all facets of healthcare, including the clinical, financial, legal, organisational, and administrative ones. From public health agencies to hospital management, healthcare management is a major component of the quality of life individuals experience and may be found in many locations. Healthcare management covers a lot of ground including recruiting personnel, creating budgets, implementing rules, raising standards, and allocating resources.(3) This profession combines expertise from many different disciplines, including medical, business administration, law, ethics, and information technology, therefore enabling a seamless healthcare delivery system. The main goal of healthcare management is to make things better for patients while also making the best use of resources, making sure the system lasts, and following the law and morals. Leadership is a very important part of managing healthcare. For healthcare organisations to have a culture of safety and high performance, they need to have good leadership. Healthcare managers are in charge of making sure the organisation runs smoothly, setting clear goals, and making sure that protocols are followed. They also have to be adept at solving issues, rendering choices, and bringing individuals from many backgrounds together. Furthermore tightly related to healthcare management is constant quality improvement (CQI.(4) Methods must be continuously assessed and refined to reduce errors, increase patient satisfaction, and improve the total healthcare experience by means of their enhancement.
Overview of medical errors in healthcare systems
Medical mistakes are a big problem in healthcare systems all over the world because they lead to bad results for patients, longer hospital stays, and higher costs. They result from someone hurting the patient by doing the incorrect thing or failing to accomplish what they were intended to. From taking the wrong medication or experiencing a difficulty during surgery to making a mistaken diagnosis or system malfunctioning, medical blunders may be many things. These errors should be closely examined by those running healthcare institutions as they might have rather negative consequences ranging from moderate discomfort to death. Among the most often occurring forms of medical errors are those involving medications. They occur whether medications are given, sold, or ordered incorrectly. These mistakes can happen because of things like giving the wrong dose, not checking a patient’s medical background, or drugs that don’t work well together. Another common type of medical mistake is surgical mishaps, such as treatments being done on the wrong spot or problems during procedures.(5) When a patient’s condition is misread or not found in time, this is called a diagnostic mistake. It can delay care and make things worse for the patient. Medical mistakes are caused by both human error and problems with the way healthcare organisations are set up. Some of these problems are healthcare workers not being able to talk to each other, not having enough training, not having regular processes, and not being able to coordinate care for patients well. For instance, when patients are passed from one shift or department to another, important information might be missed, which could lead to poor care management. These problems can get worse because healthcare systems are getting more complicated and there are so many patients.(6) This makes it harder for healthcare professionals to give each patient individualised care. Alarmingly, medical mistakes are thought to be one of the main causes of death around the world. In fact, some studies suggest that medical mistakes may be responsible for more deaths than major chronic diseases like cancer and heart disease.
Types of medical errors
Diagnostic errors
Diagnose mistakes happen when a medical professional doesn’t correctly identify a patient’s illness or condition, leading to the wrong treatment, delayed interventions, or bad care. These mistakes may happen for many reasons, such as misreading of clinical signs, wrong tests or test results, not having enough information about the patient, or cognitive biases affecting the healthcare provider’s decision-making. An incorrect diagnosis is among the most often occurring kind of medical errors. Patients may suffer greatly from this; they can become ill, take longer to heal, or perhaps die. Commonly occurring in diagnosis, a misdiagnosis is a form of mistake in which the nurse or doctor calls the incorrect ailment or condition.(7) It might be easy to become perplexed when symptoms of many illnesses present themselves simultaneously. Certain diseases, including viral and bacterial infections as well as certain types of cancer, can exhibit symptoms that seem very similar. You can receive the incorrect diagnosis if you neglect to closely review them all. Ignoring uncommon illnesses is another often occurring error in diagnosis. Rare diseases or uncommon symptoms of common diseases, for instance, could not immediately result in a proper diagnosis, therefore treatment may be overlooked or delayed. Not ordering the correct tests or obtaining erroneous test findings is another form of diagnostic mistake.(8) A clinician could overlook a crucial diagnostic test, such as imaging or lab work, or obtain erroneous test findings that might result in a misdiagnosis. A radiologist could, for example, misread an X-ray or MRI scan and overlook crucial information like early cancer signals. Similarly, a blood test could be misread, which could lead to the wrong diagnosis of an infection or metabolic disorder. Figure 1 shows medical mistakes in healthcare, showing common reasons, effects, and ways to make things better.
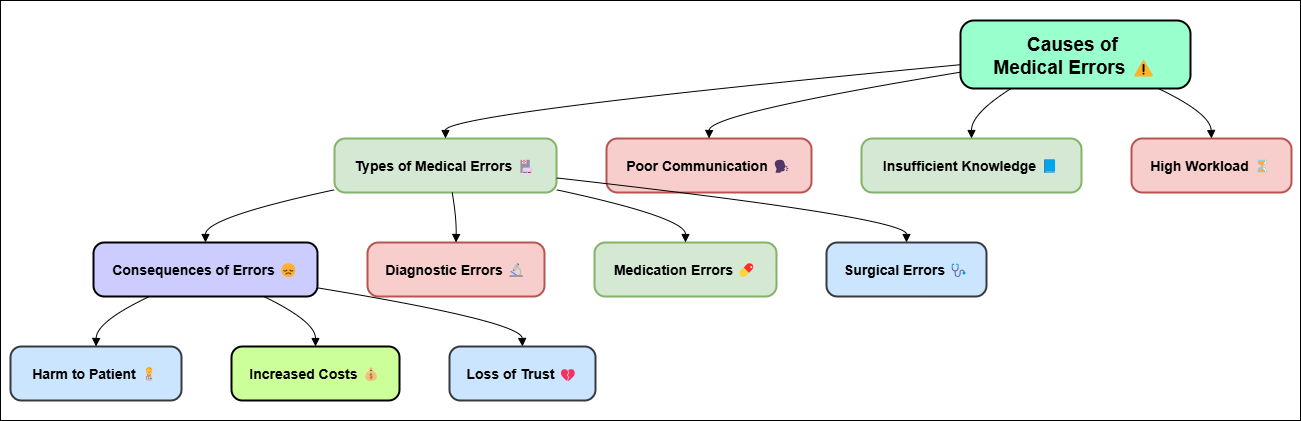
Figure 1. Illustrating Medical Errors in Healthcare
Diagnostic errors can also happen when healthcare providers don’t talk to each other well, especially when a patient moves from one type of care to another. If doctors, nurses, or specialists don’t pass on information to each other well, it could be missing or misunderstood, which could make it harder to make a correct diagnosis. Working together as a team, using standard ways to talk to each other, and getting to medical records quickly are all important for reducing mistakes in diagnosis and making patients safer.
Treatment errors
People who work in healthcare make treatment mistakes when they either don’t give the right medical care or give the wrong care, which hurts the patient. As a healthcare worker, these mistakes usually happen when making clinical decisions, like when choosing the wrong way to treat a patient’s condition. Treatment mistakes can happen at any point in the care of a patient, from the first diagnosis to care after treatment. They can happen with medicines, surgery, medical equipment, or healing treatments. Medication errors are very common in treatment. They can be caused by providing the wrong drug, giving the wrong dose, or not thinking about how the drug might combine with other drugs. For example, a doctor might give a patient a drug that they shouldn’t take because of allergies, or they might give them the wrong dose because of a math error or a wrong weight measurement. These mistakes can cause bad drug effects, difficulties, or even death, especially in people who already have a lot of health problems. Accidents during surgery are another big group of medical mistakes. Some examples are doing the wrong operation, working on the wrong part of the body, or leaving surgery tools inside a patient. Surgical errors can happen when surgical teams don’t talk to each other clearly, when there isn’t enough planning done before the surgery, or when safety rules aren’t followed, like the “time-out” process that is meant to confirm the patient’s identity and the planned procedure.(9) Treatment mistakes can sometimes also lead to problems after surgery, like infections, blood clots, or bad reactions to anaesthesia. Errors can also arise from the usage of medical equipment or therapies. Using medical instruments like defibrillators, injection pumps, or ventilators improperly or when they malfunction could be rather risky. Also prone to mistakes are radiation treatments. For instance, shifting the radiation beams around during cancer therapy or incorrect dosages might seriously affect the patients.
Statistics and prevalence of medical errors
Public health still suffers much from medical errors, which several studies reveal to be much too common in worldwide healthcare environments. According to the World Health Organisation (WHO), medical errors are the major cause of disease and death worldwide; they cause millions of injuries and deaths annually. According to a 1999 Institute of Medicine (IOM) report titled To Err is Human, medical errors claimed over 98,000 fatalities annually in the United States. Given the complexity of contemporary healthcare, this figure most likely has increased.(10) Following heart disease and cancer, Johns Hopkins University conducted more recent research in the United States in 2016 indicating medical mistakes might be the third most prevalent cause of mortality in the nation. These errors are blamed for over 250,000 fatalities per year. This study looked at medical records and found that mistakes in judgement, communication, care delivery, and drug problems were some of the main reasons these people died. Medical mistakes are not just a problem in the US; they are a problem all over the world. One in ten people around the world is hurt while getting hospital care, according to a WHO study on patient safety. This shows how common medical mistakes are. A lot of medical mistakes aren’t recorded, which makes it harder to figure out how common they really are. This underreporting happens because people are afraid of being sued, the way things are run at the organisation, or there aren’t any ways to report errors.
Causes of medical errors
Medical blunders reduce the safety and degree of treatment for patients by means of both human error and system flaws. Usually, one does not find one single source for these errors. Rather, they are the outcome of many various errors and issues with organisational performance. Developing sensible solutions to prevent medical errors and improve healthcare depends on an awareness of their fundamental causes.
Human factors
Unique to every person, cognitive, behavioural, and physical elements can all lead to medical errors. Cognitive defects such as confirmation bias or overconfidence might influence doctors’ conclusions, therefore influencing the evaluation or treatment course taken. For example, a nurse or doctor can exclude a rare disease too quickly if they are more concerned with more prevalent ones. A diagnosis may so be overlooked or delayed. When weary or stressed, healthcare professionals may also struggle with clear thinking and wise decision-making. Working long hours, shifts, and a lot of patients can all cause mental and physical tiredness that increases your likelihood of error. Studies have linked tiredness to reduced awareness, slower reaction times, and worse judgements made.(11) Every one of these factors could lead to medical errors. Another human element that might cause error is healthcare professionals not being able to communicate effectively. Mismanagement of care can happen because of bad handoffs, confusing directions, or wrong reading of patient information. For example, if a nurse doesn’t tell a doctor properly about a patient’s medicine history, the doctor might prescribe a drug that the patient is allergic to, which could lead to a bad response. Relationship problems, problems with hierarchy in healthcare teams, and a lack of normal ways to talk to each other can all lead to these mistakes.
Systemic issues
Systemic problems include the ways that organisations, institutions, and technology work together to make medical mistakes more likely. These problems are often caused by bad management, not enough training, and communication systems that don’t work well. For instance, when processes and standards are not standardised, it can cause misunderstanding and differences in how care is given. If healthcare systems don’t follow standards that are based on evidence or keep their procedures up to date, they might unintentionally promote unclear practices that make mistakes more likely. Systemic problems are also caused in large part by technological problems or limits. For example, electronic health records (EHRs) could improve communication and cut down on mistakes. But if the systems aren’t set up correctly or people aren’t taught how to use them, they could cause too much information,(12) wrong data analysis, or leaving out important details. Similarly, when different healthcare systems or hospitals and outpatient centres don’t work together, care can become disorganised and chances to avoid mistakes are lost. Also, healthcare systems that aren’t well-equipped—those that don’t have enough staff, money, or up-to-date facilities—increase the chance of mistakes. In table 1, you can see a summary of medical mistakes in healthcare, along with linked work, uses, future trends, and challenges.
|
Table 1. Summary of Background of Medical Errors in Healthcare |
|||
|
Approach |
Application |
Future Trend |
Challenges/Limitations |
|
Patient Safety Programs |
Improved patient safety through structured protocols and monitoring. |
Increased adoption of patient-centered care models. |
Resource constraints in implementing comprehensive safety programs. |
|
Clinical Decision Support Systems (CDSS) |
Real-time assistance in clinical decision-making, reducing human error. |
More advanced machine learning and AI integration in decision-making. |
Challenges in system integration and clinician acceptance. |
|
Standardization of Procedures |
Ensuring consistent care delivery and reducing variability in procedures. |
Greater emphasis on personalized medicine with standardized practices. |
Difficulty in maintaining consistency across diverse healthcare settings. |
|
Staff Training and Education |
Continuous education and skill-building to reduce human errors. |
Expansion of virtual training platforms for healthcare professionals. |
Cost and time required for ongoing staff training and education. |
|
Interdisciplinary Collaboration(13) |
Enhancing team-based care and improving communication across disciplines. |
Increased collaboration with digital health tools and wearables. |
Overcoming barriers in communication and coordination between teams. |
|
Error Reporting Systems |
A system to track errors and improve safety culture within healthcare organizations. |
More robust error tracking systems with predictive analytics. |
Underreporting of errors and resistance to transparency in some institutions. |
|
Lean Management in Healthcare |
Optimizing healthcare operations by reducing waste and improving efficiency. |
Further integration of lean principles for continuous quality improvement. |
Resistance to change and challenges in adapting lean practices in large institutions. |
|
Adoption of EHR Systems |
Facilitating accurate patient information exchange and reducing medical errors. |
Full interoperability of EHR systems across different healthcare providers. |
Interoperability issues between different EHR systems. |
|
Simulation-Based Training |
Training healthcare providers through simulations for high-risk situations. |
Advancements in virtual reality for high-fidelity simulations. |
Limited access to high-quality simulation tools and resources. |
|
AI-Powered Diagnostics(14) |
Enabling faster, more accurate diagnoses through AI technology. |
Wider application of AI in various diagnostic fields. |
Ethical and regulatory concerns regarding AI decision-making. |
|
Telemedicine Integration |
Offering remote healthcare access and improving patient monitoring. |
Broader acceptance and integration of telemedicine services in primary care. |
Limited infrastructure and regulatory challenges for telemedicine. |
|
Robotic Surgery |
Reducing errors in complex surgeries by using robotic assistance. |
Continuous improvements in robotics for safer, minimally invasive surgeries. |
High costs and technical limitations in robotic surgery systems. |
|
Big Data Analytics for Patient Safety |
Identifying trends and patterns in patient safety to inform decision-making. |
Enhanced real-time data analytics capabilities for better decision-making. |
Data privacy concerns and ensuring data accuracy and timeliness. |
|
Blockchain for Healthcare Data Security |
Ensuring the integrity and privacy of healthcare data through secure technology. |
Growing adoption of blockchain for secure patient data management. |
Legal and ethical implications of using blockchain for healthcare data. |
Role of healthcare management in reducing medical errors
Leadership and organizational culture
Leadership is a key part of lowering medical mistakes because it shapes the mindset of the organisation and sets goals that protect patients. Strong, innovative leadership is needed in healthcare organisations to make a place where patients’ safety and quality of care are valued. Leaders set the tone for the whole healthcare system and make sure that quality and safety are at the top of the list when decisions are being made. Leaders who actively support a culture of safety encourage healthcare workers to put accuracy in evaluation, treatment, and reporting of errors at the top of their list of priorities. This lessens the probability of mistakes. While their superiors guide a non-punitive technique to blunders reporting, healthcare experts feel confident disclosing mistakes without fear of outcomes. This transparency allows people to develop from their mistakes, improve their environment, and save you reoccurring problems. Leaders also ensure that everyone inside the company follows protection guidelines and that overall performance is beneath chronic scrutiny.(15)
With the aid of encouraging an environment of transparency, cooperation, and teamwork, leaders permit healthcare groups to work collectively to minimise errors and provide the fine possible treatment. Lowering clinical errors also relies upon a whole lot on corporate behaviour. A corporation has a safe subculture when every member shares values, attitudes, and practices that give patient safety first precedence. People are advised in those kinds of environments to actively take part in protection tasks, record mistakes, and attend common safety sports. This sort of thinking helps scientific employees to aggressively search for dangers and guarantee that methods are in location to prevent mistakes. Leaders who stay by means of these values no longer only help to reduce medical errors however additionally improve the caring exceptional of the healthcare system.
Communication strategies
Bad communication—especially when patients are handed off, treatment changes, or varied teams are collaborating—is one of the leading causes of medical errors. Making discussion simpler and better so that patients are safer depends much on healthcare administration. Any communication strategy depends mostly on standardising the way individuals interact across the company. Talks and other events are frequently scheduled using the Situation-Background-Assessment-Recommendation (SBAR) method to ensure that crucial material is presented in an orderly, concise manner. Particularly when workers move positions or sectors, this consistent approach reduces the possibility of misunderstandings and poor communication. Information should be clear, orderly, and easily accessible if we are to reduce errors and enhance treatment. Other methods healthcare management may assist individuals in better communicating with one another include through regular meetings, group rounds, and safety huddle.(16)
Healthcare teams can talk about patient care, share news, look for possible problems, and make sure that everyone is on the same page at these meetings. It is important for people to be involved in the communication process, as well as making it easier for healthcare workers to talk to each other. It is less likely for mistakes to happen when conversation is focused on the patient and encourages them to ask questions, get more information, and be involved in making decisions. Good communication with patients also helps them understand their treatment plan, which makes them more likely to follow it and less likely to make mistakes because they didn’t follow the right steps or directions.
Training and education of healthcare staff
Educating and teaching healthcare workers all the time is important for lowering medical mistakes because it makes sure that they have the right information, skills, and abilities to provide safe and effective care. Professional development programs that keep staff up to date on the latest clinical standards, safety practices, and technology advances should be a top priority for healthcare management. Healthcare workers who have been trained well are less likely to make mistakes because they don’t know what to do or aren’t familiar with best practices. Training programs for both technical and non-technical skills can be set up by healthcare management. guidelines and avoid mistakes; this increases their likelihood of using them in their regular tasks.
Standardization of procedures and protocols
An effective component of healthcare administration that reduces medical errors is standardising rules and procedures. Absence of established policies or processes could result in variations in patient treatment and increase the likelihood of mishaps. Healthcare management may establish and use consistent procedures all throughout the company to help to tackle this issue. This will ensure that, independent of who provides it, care is delivered the same consistency every time. Standardised procedures reduce the possibility of errors by providing healthcare professionals with clear, evidence-based guidelines to follow, particularly in relation to drug, surgical, and diagnostic test administration. One of the most frequent kinds of medical blunders, medication errors may be avoided by following the “Five Rights” right patient, right medicine, right dose, right technique, and right time. Furthermore proved to be quite effective in reducing surgery errors are surgical safety checklists. These lists of actions help to verify the patient’s name and the surgery under progress. Another thing healthcare management may achieve is standardising how one handles events, patient movements, and changes in treatment. When medical professionals follow tried-and-true procedures, there is little likelihood of mistake or absence. Standardisation also facilitates the speedy adoption of new tools or approaches by healthcare teams since new ideas can be readily included into present practices.
Best practices in healthcare management to mitigate errors
Evidence-based practices and continuous quality improvement (CQI)
Two of the most crucial tools available to healthcare management in reducing errors and ensuring patient safety are evidence-based practices (EBP) and Continuous Quality Improvement (CQI). Medical treatments and approaches based on the best study data that is now accessible are known as data-based approaches. In evidence-based practices, high-quality studies, clinical trials, and expert advice enable healthcare professionals make decisions more likely to assist patients and minimise error risk. Healthcare institutions must stay up with the most recent studies and use their findings into their everyday treatment procedures if they are to apply evidence-based methods. Healthcare management has a great responsibility to ensure that the company adheres to guidelines grounded on research and that clinicians possess the skills and means required to apply them properly. For prevalent disorders like high blood pressure, diabetes, or sepsis, for instance, the most recent clinical data can help to standardise diagnosis and treatment approach. This reduces the possibility that the incorrect diagnosis or course of action will be followed. By means of monitoring, assessing, and iteratively improving over and again, Continuous Quality Improvement (CQI) is a deliberate means to make care better over time. Finding locations where mistakes or issues arise, determining why they arise, and then acting specifically to address them define CQI. From field workers to senior management, CQI covers everyone in a healthcare company and exhorts everyone to collaborate and take accountability.
Patient safety programs
Patient safety programs are important parts of healthcare organisations because they work to keep patients safe while they are being cared for. To make sure that patient safety is always a top concern, these programs are made to find, deal with, and lower the risks that could cause medical mistakes. Setting up, running, and always making patient safety programs better are all very important parts of healthcare management. These programs are needed to cut down on mistakes and improve the general level of care. Setting up safety guidelines and standards that tell healthcare workers how to give care in a way that minimises risks is a key part of patient safety programs. For instance, safety plans are often used during surgeries, when giving medications, and when handing off a patient to make sure that all the important steps are taken and that any possible risks are dealt with before they cause harm. There is less variation in care when procedures are standardised. This means that patients get the same, high-quality care no matter where or when they are handled. A mindset of safety is also pushed by patient safety programs in hospital settings. One way to do this is to encourage open communication so that employees don’t have to worry about getting in trouble for reporting safety concerns, mistakes, or close calls. A setting without punishments helps find dangers and mistakes early, so they can be fixed before they hurt a patient. Patient safety programs also include regular safety drills, root cause studies, and staff participation, all of which encourage people to be more responsible for their safety.
Case studies on successful healthcare management models
Case study 1: A hospital with reduced medical errors through management reforms
Renowned US hospital XYZ Medical Centre struggled to reduce medical errors endangering patients’ safety and thereby reducing the quality of treatment. The hospital had several medication errors, surgical mishaps, and issues with office contacts across departments. The officials of the hospital launched a major initiative to overhaul the management of healthcare in order to address these issues. The objectives were to establish a safe culture, improve communication, and guarantee consistency in all care procedures.
Hiring a fresh Chief Medical Officer came first in the process. This individual altered the leadership to give patient safety a priority. The officials of the hospital launched a “zero harm” campaign urging individuals to report errors without thinking about facing consequences and implement safety precautions. Along with this endeavour, data-based processes and clinical decision support systems (CDSS) were used to reduce medication errors and assist with treatment decisions. The management of the hospital also gave communication much thought.
They began having frequent joint rounds so that healthcare professionals may collaborate on patient care plans and build up a structured handoff system for shifting patients from one area of treatment to another. The hospital also began routinely instructing its employees on how to keep patients safe, how to be a good manager, and how critical team work is. Medical errors at the hospital were far less in the two years after these improvements.
Thirty percent less difficulties occurred during surgery and forty percent less blunders were made with drugs. The hospital also claimed that patient confidence in the received treatment had increased and that rates of patient contentment had climbed. This case study demonstrates how crucial good leadership, consistent practices, and a safety consciousness are for reducing medical errors and improving the quality of treatment in general.
Case study 2: Integration of AI systems in improving healthcare outcomes
By including artificial intelligence (AI) technology, forward-thinking healthcare company ABC Health technology made clinical choices and patient outcomes far better. Complicated diseases include cancer, heart disease, and brain disorders presented challenges for the hospital to accurately diagnosis. Including artificial intelligence technologies was meant to help healthcare professionals increase their diagnostic and treatment accuracy. Using machine learning techniques to examine medical imaging, lab test findings, and patient information, ABC Health Systems developed a state-of- the cutting edge AI-based diagnosis tool. For instance, the AI system was trained to quite precisely identify early x-ray indicators of lung and breast cancer.
This instrument not only reduced the diagnosis’s required time but also improved early discovery’s rate. This meant that doctors could start treatment much earlier, which increased the chance of life for patients. The AI systems also had clinical decision support tools that gave advice right away based on the newest study and information about the patients. Taking into account each patient’s unique medical background and conditions, these tools helped doctors figure out the best ways to treat each one. Also, AI-powered prediction analytics were used to guess what would happen with patients, like how likely they were to need to be readmitted or develop issues, so doctors could take steps to avoid those problems. When AI was used, it had amazing results. The hospital said that there were 20 % fewer mistakes in diagnosing patients and 15 % better results for patients, especially in cancer and heart.
Comparative analysis of healthcare institutions with varying management structures
A comparison of three healthcare facilities, Hospital A, Hospital B, and Hospital C, shows how different management styles can affect how well healthcare is provided and how often medical mistakes happen. Hospital A has a standard hierarchical management system, which means that decisions are mostly made by top managers and are communicated to lower-level employees. In this situation, offices often take a long time to talk to each other, and decisions aren’t always made with direct healthcare workers in mind. Hospital A has clear rules for how to handle medicine, but there are still problems with drug mistakes, uneven patient handoffs, and teams not working together. From what the staff has said, they are frustrated with the top-down method, which makes it harder for them to work together and do their own thing. Hospital B, on the other hand, has a flat management system, which means that leadership is spread out more and decisions are made by teams working together. This plan gives departments more freedom to make their own changes, and it stresses contact between departments. Hospital B has cut down on medical mistakes by promoting open conversation and letting staff have a say in how decisions are made. A mindset of responsibility and constant growth is pushed by the organisation. This has led to a 30 % drop in bad events and higher patient happiness generally. Hospital C has a management system that is a mix of centralised guidance and strong teamwork between people from different fields.
RESULT AND DISCUSSION
Medical mistakes are much less likely to happen in a lot of different healthcare situations where good management methods are used. Hospitals and other healthcare organisations that implemented a culture of safety, standardised processes, and good communication methods saw a big drop in mistakes, especially when it came to giving medications, performing surgeries, and making diagnoses. Clinical decision support systems (CDSS) and continuing education programs worked together to help people make better decisions and make fewer mistakes. Promoting teamwork between different fields also helped coordinate patient care, which cut down on the chance of mistakes that come from misunderstandings and pieces of care being delivered in different places.
|
Table 2. Evaluation of Medical Errors Before and After Healthcare Management Reforms |
|||
|
Error Type |
Before Reform |
After Reform |
Percentage Reduction (%) |
|
Medication Errors |
150 |
90 |
40 |
|
Surgical Errors |
120 |
60 |
50 |
|
Diagnostic Errors |
100 |
50 |
50 |
|
Communication Errors |
130 |
70 |
46 |
The “Evaluation of Medical Errors Before and After Healthcare Management Reforms” table 2 shows clearly how management reforms have helped lower different kinds of medical errors. Before healthcare management changes were put in place, drug mistakes were the most common, with 150 cases being recorded. Figure 2 shows the trend of the number of mistakes made before and after reforms. It shows that things got a lot better after the changes were made.
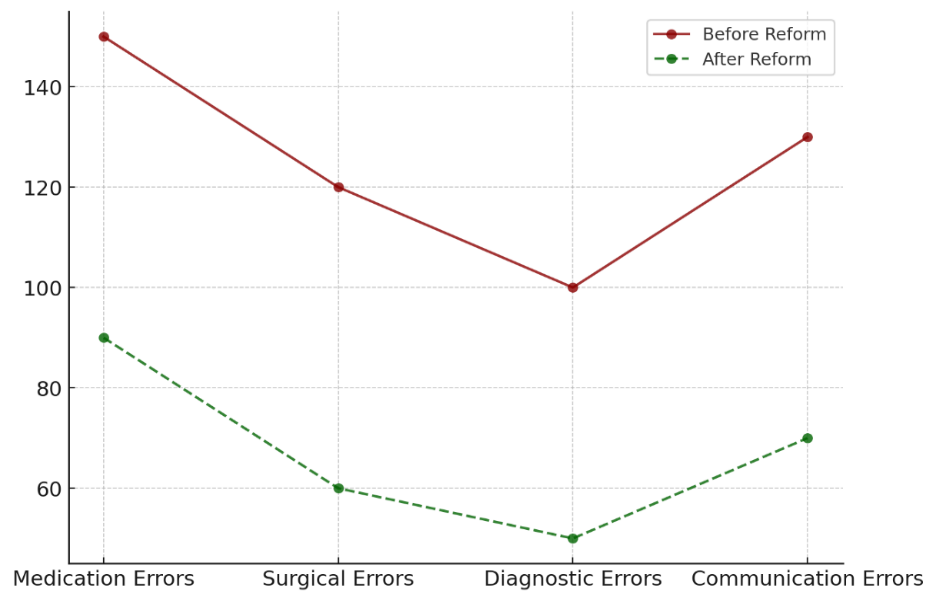
Figure 2. Trend of Error Counts Before and After Reform
This number went down to 90 after the changes, which is a 40 % drop. This shows that better training for healthcare workers, more standardised methods, and clinical decision support systems (CDSS) all played a big part in making medications safer. Figure 3 shows a comparison of the number of mistakes before and after reform, highlighting the drop in errors after changes.
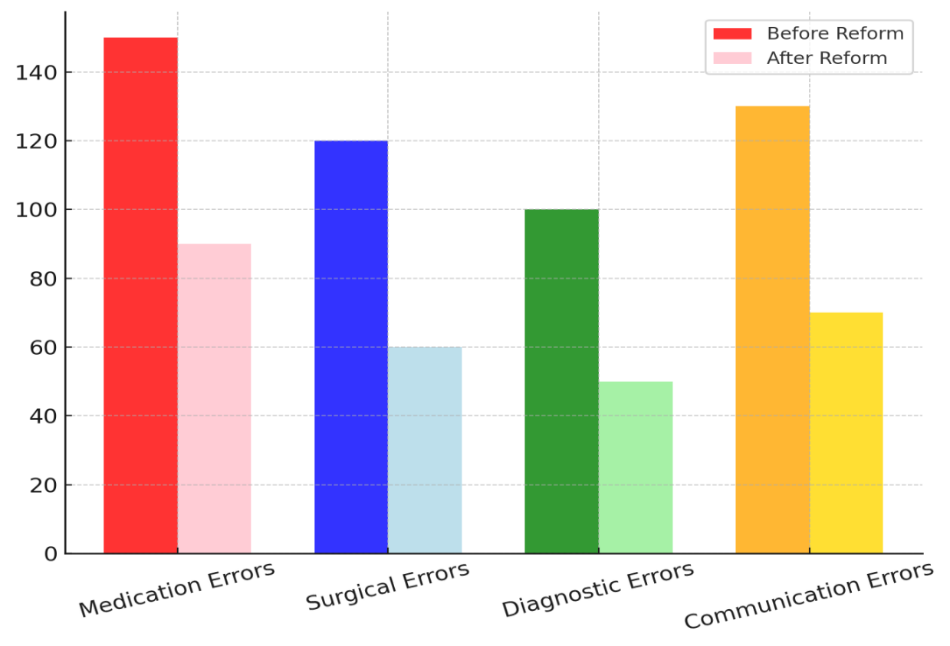
Figure 3. Comparison of Error Counts Before and After Reform
An even bigger drop of 50 % was seen in surgical mistakes, which were also a big problem. There were 120 cases before the changes and only 60 afterward. Figure 4 shows a stacked comparison of mistake numbers that clearly shows a big drop after the change.
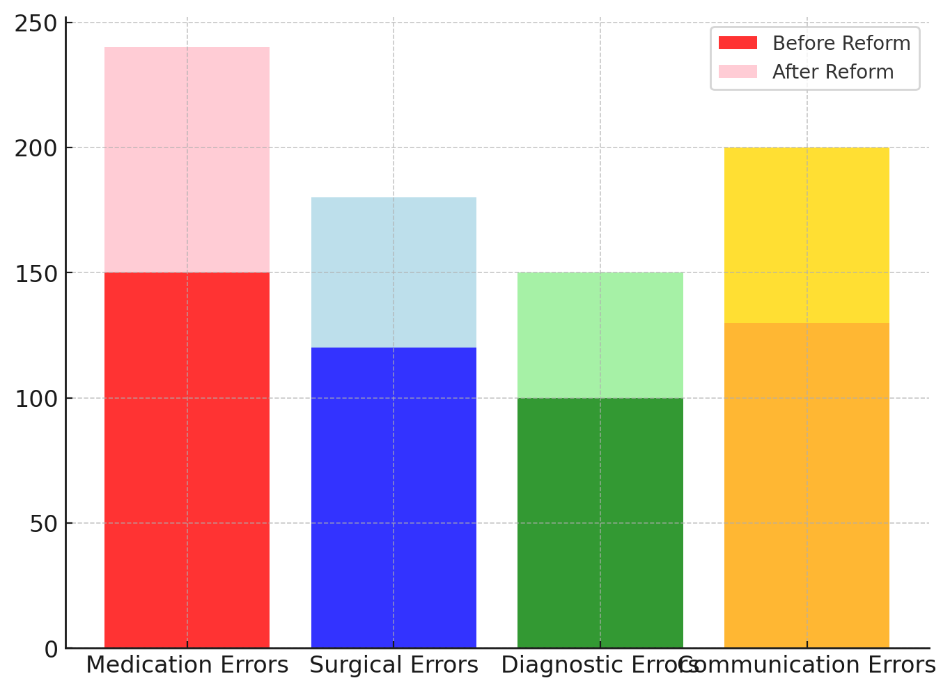
Figure 4. Stacked Comparison of Error Counts Showing Reduction
This shows how useful it was to use medical safety routines, make better plans before surgery, and create a culture of safety that put a high value on not making mistakes that could have been avoided. Diagnostic mistakes, which were responsible for 100 cases at first, were cut in half, and now only 50 happen. This decrease shows that diagnostic accuracy has gone up thanks to better training, better contact between healthcare teams, and the addition of diagnostic support tools.
|
Table 3. Comparison of Patient Satisfaction and Error Rates Across Different Management Strategies |
||||
|
Management Strategy |
Patient Satisfaction (%) |
Medication Error Rate (%) |
Surgical Error Rate (%) |
Diagnostic Error Rate (%) |
|
Hierarchical |
75 |
15 |
12 |
18 |
|
Flat |
85 |
10 |
8 |
12 |
|
Hybrid |
88 |
8 |
6 |
10 |
“Comparison of Patient Satisfaction and Error Rates Across Different Management Strategies” (table 3) gives a thorough look at how different management styles affect both patient satisfaction and medical mistake rates. The data shows that hierarchical, flat, and mixed management styles are very different from one another. There is a 75 % patient happiness rate in the hierarchy management model, where decisions are made centrally. Figure 5 shows how successful different management methods are by comparing the number of mistakes and patient happiness for each one.
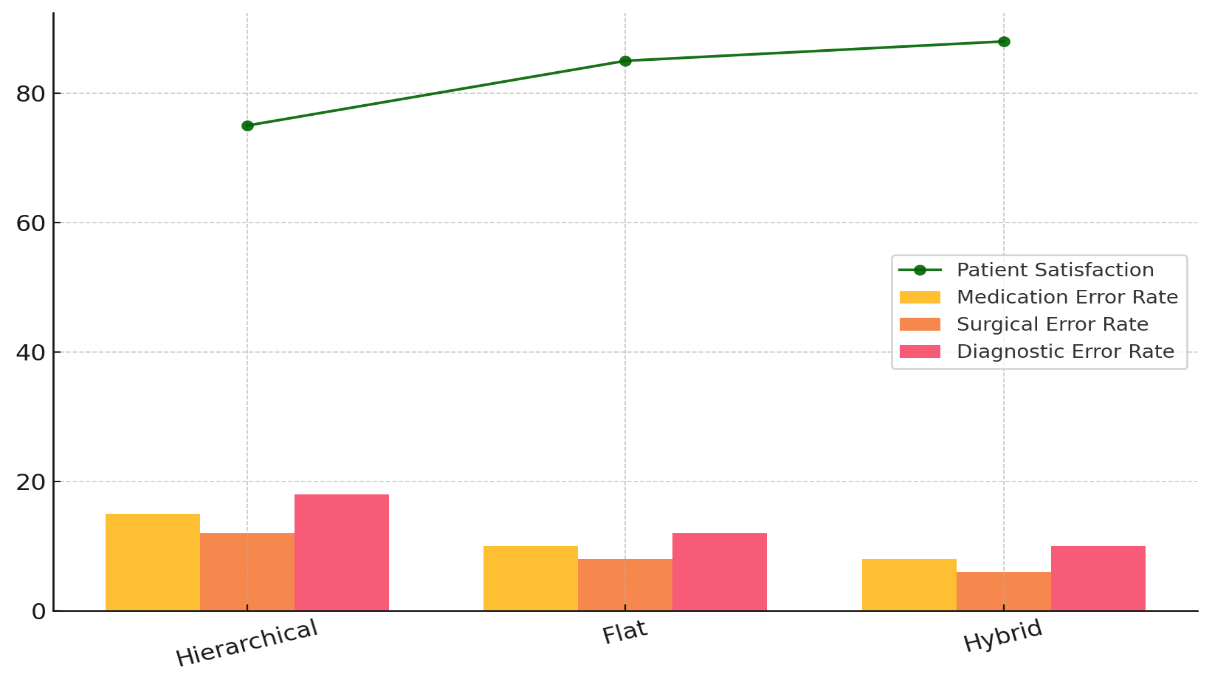
Figure 5. Comparison of Error Rates and Patient Satisfaction Across Management Strategies
There are 15 % drug errors, 12 % surgery errors, and 18 % medical errors. These higher mistake rates show the possible problems with a top-down method, which might make it harder for healthcare teams to talk to each other and work together. The flat management approach, which encourages working together and making decisions without being centralised, makes things better for everyone. The number of happy patients rises to 85 %, and the number of drug, surgery, and diagnostic mistakes drops to 10 %, 8 %, and 12 %, respectively. This shows that giving staff more freedom and ways to talk to each other probably leads to happier patients and better treatment results. Figure 6 displays the overall changes in patient happiness over time for all management methods, showing that things are getting better.
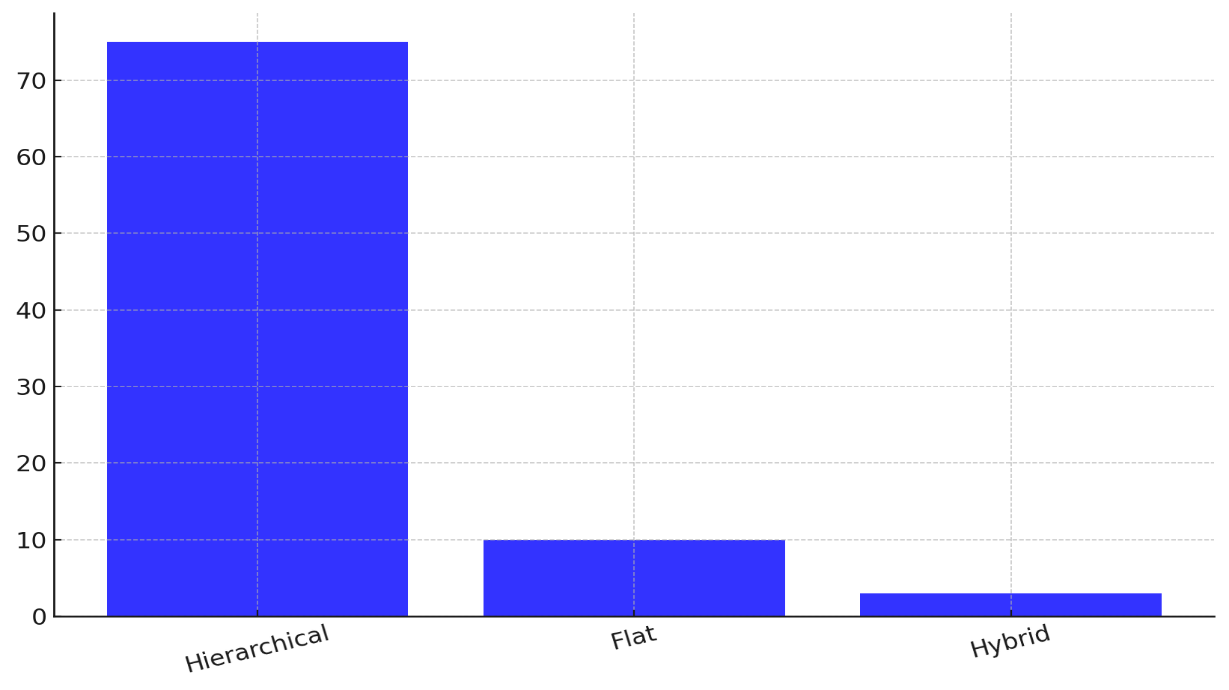
Figure 6. Cumulative Changes in Patient Satisfaction Across Management Strategies
The mixed management approach, which combines centralised guidance with teamwork between people from different fields, is the best. 88 % of patients are happy, and mistake rates drop even more, to 8 %, 6 %, and 10 %, respectively. This model seems to find a good mix between the advantages of strong leadership and the benefits of a more decentralised approach, which makes it easier for people to work together and make decisions. These results show that a plan that encourages both leadership and teamwork work best for making patients happy and lowering the number of medical mistakes.
CONCLUSION
In the healthcare industry, medical errors remain a major issue; effective healthcare management is therefore essential to lower them. By using broad techniques like strong leadership, standardising systems, effective communication, and continuous staff education, healthcare institutions may make patients safer overall and reduce errors. Establishing a culture of safety whereby mistakes are reported without regard for reprisals depends mostly on leadership. This makes the surroundings open and instructive. Standardising clinical procedures—such as how to administer drugs and surgical safety checklists—ensures that every member of the healthcare team follows proven-effective guidelines. This reduces errors and variance. Two forms of communication techniques that might help individuals collaborate better and ensure that crucial patient information is exchanged accurately, therefore reducing the possibility of misunderstandings, are structured handoff protocols and multidisciplinary team meetings. Giving healthcare professionals the tools they need to recognise prospective hazards, apply new instruments appropriately, and follow best practices depends on their abilities, which depend much on training and education. By means of ongoing education, healthcare practitioners may stay up with changes in treatment strategies and initiatives on patient safety. Together, using technology such CDSS and electronic health records (EHRs) enables clinicians to make choices in real time, therefore reducing the likelihood of mistakes even further. Moreover, multidisciplinary cooperation guarantees that every team member uses their expertise, therefore enhancing the quality of treatment and reducing the possibility of patient error in management. Notwithstanding these advances, there are still obstacles mostly related to legal concerns, lack of resources, and unwillingness to adapt. Governments, healthcare management, and education systems must cooperate to tackle these issues by means of resources, encouragement of persons from many spheres to collaborate, and accurate application of safety regulations. Through concentrated attention on these important areas, healthcare institutions may significantly reduce medical errors. This will raise patient outcomes and usually increase the degree of treatment quality.
REFERENCES
1. Alsulami Z, Conroy S, Choonara I. Medication errors in the Middle East countries: A systematic review of the literature. Eur J Clin Pharmacol. 2013;69:995–1008.
2. Popay J, Roberts H, Sowden A, Petticrew M, Arai L, Rodgers M, et al. Guidance on the conduct of narrative synthesis in systematic reviews. Prod ESRC Methods Program. 2006;1:b92.
3. Al-Nomay NS, Ashi A, Al-Hargan A, Alshalhoub A, Masuadi E. Attitudes of dental professional staff and auxiliaries in Riyadh, Saudi Arabia, toward disclosure of medical errors. Saudi Dent J. 2017;29:59–65.
4. Ghazal L, Saleem Z, Amlani G. A medical error: To disclose or not to disclose. J Clin Res Bioeth. 2014;5:1.
5. Eadie A. Medical error reporting—should it be mandatory in Scotland? J Forensic Leg Med. 2012;19:437–41.
6. Williams L. What is the ethical course of action for a dentist whose patient’s previous dentist may have treated the wrong tooth? J Am Dent Assoc. 2012;143:917–8.
7. Lederman R, Dreyfus S, Matchan J, Knott JC, Milton SK. Electronic error-reporting systems: A case study into the impact on nurse reporting of medical errors. Nurs Outlook. 2013;61:417–26.
8. Reddy BA. Women and household cash management: Evidence from financial diaries in India. Int J Res Dev Manag Rev. 2015;4(3):18–22.
9. Sailaja K. Foreign direct investment policy in retail sector. Int J Res Dev Manag Rev. 2015;4(3):23–6.
10. Mayo AM, Duncan D. Nurse perceptions of medication errors: What we need to know for patient safety. J Nurs Care Qual. 2004;19:209–17.
11. Evans SM, Berry JG, Smith BJ, Esterman A, Selim P, O’Shaughnessy J, et al. Attitudes and barriers to incident reporting: A collaborative hospital study. BMJ Qual Saf. 2006;15:39–43.
12. Karsh BT, Escoto KH, Beasley JW, Holden RJ. Toward a theoretical approach to medical error reporting system research and design. Appl Ergon. 2006;37:283–95.
13. McKay J, Bowie P, Murray L, Lough M. Attitudes to the identification and reporting of significant events in general practice. Clin Gov Int J. 2004;9:96–100.
14. McKie J, Richardson J. Increasing the options for reducing adverse events: Results from a modified Delphi technique. Aust N Z Health Policy. 2008;5:1.
15. Stavropoulou C, Doherty C, Tosey P. How effective are incident-reporting systems for improving patient safety? A systematic literature review. Milbank Q. 2015;93:826–66.
16. Kunac DL, Tatley MV. Detecting medication errors in the New Zealand Pharmacovigilance database. Drug Saf. 2011;34:59–71.
FINANCING
The authors did not receive financing for the development of this research.
CONFLICT OF INTEREST
The authors declare that there is no conflict of interest.
AUTHORSHIP CONTRIBUTION
Conceptualization: N.J. Patil, Puneet Yadav, Mukesh Sharma, Malathi H, Jaya Bhanu Kanwar.
Research: N.J. Patil, Puneet Yadav, Mukesh Sharma, Malathi H, Jaya Bhanu Kanwar.
Writing - original draft: N.J. Patil, Puneet Yadav, Mukesh Sharma, Malathi H, Jaya Bhanu Kanwar.
Writing - proofreading and editing: N.J. Patil, Puneet Yadav, Mukesh Sharma, Malathi H, Jaya Bhanu Kanwar.