doi: 10.56294/hl2023318
ORIGINAL
Improving Quality of Life through the Synergistic Integration of Healthcare and Environmental Health Programs
Mejorar la calidad de vida mediante la integración sinérgica de los programas de sanidad y salud ambiental
Pusparaj Samantsinghar1 ![]() , Ram Garg2
, Ram Garg2 ![]() , Vinod Kumar Singh3
, Vinod Kumar Singh3 ![]() , Atul Bhanudas Hulwan4
, Atul Bhanudas Hulwan4 ![]()
1IMS and SUM Hospital, Siksha ‘O’ Anusandhan (Deemed to be University), Department of Forensic Medicine & Toxicology, Bhubaneswar, Odisha, India.
2Arya College of Pharmacy, Jaipur, Rajasthan, India.
3School of Liberal Arts, Noida International University, Greater Noida, Uttar Pradesh, India.
4Krishna institute of Medical Sciences, Krishna Vishwa Vidyapeeth “Deemed to be University”, Department of Pathology, Taluka-Karad, Dist-Satara, Maharashtra, India.
Cite as: Samantsinghar P, Garg R, Kumar Singh V, Bhanudas Hulwan A. Improving Quality of Life through the Synergistic Integration of Healthcare and Environmental Health Programs. Health Leadership and Quality of Life. 2023; 2:318. https://doi.org/10.56294/hl2023318
Submitted: 06-06-2023 Revised: 25-08-2023 Accepted: 27-11-2023 Published: 28-11-2023
Editor: PhD.
Prof. Neela Satheesh ![]()
ABSTRACT
Introduction: environmental health and healthcare programs working together have gotten a lot of attention because they could make people and communities’ lives better. Environmental factors like air quality, cleanliness, and access to green areas have a direct effect on health results. For long-term well-being, healthcare and environmental health must so cooperate.
Method: this work applied a mixed-methods technique. Using numerical data, health variables from several locations were examined; qualitative data was obtained by interviewing and surveying healthcare professionals, environmental health specialists, and community people. Data on natural quality, public health results, and social variables of health were examined in order to ascertain how integrated initiatives impact quality of life.
Results: key health indicators like fewer incidences of chronic illnesses, improved mental health outcomes, and generally better public health changed significantly in communities that merged their efforts on environmental and healthcare issues. Apart from that, these combined initiatives made communities more involved and resilient, which resulted in long-term improvement in health.
Conclusion: the study reveals that people›s quality of life may be much raised by integrating public health with medical treatments. If several organisations cooperate successfully, communities can be healthier and more robust. Long-term public health and environmental improvement depend on legislators giving initiatives addressing both healthcare and environmental concerns top importance.
Keywords: Healthcare Integration; Environmental Health; Quality Of Life; Public Health; Community Well-Being; Sustainable Health Programs.
RESUMEN
Introducción: el trabajo conjunto de los programas de salud ambiental y sanidad ha recibido mucha atención porque podría mejorar la vida de las personas y las comunidades. Factores ambientales como la calidad del aire, la limpieza y el acceso a zonas verdes tienen un efecto directo en los resultados sanitarios. Para lograr un bienestar a largo plazo, la sanidad y la salud ambiental deben cooperar.
Método: este trabajo aplicó una técnica de métodos mixtos. A partir de datos numéricos, se examinaron variables sanitarias de varias localidades; los datos cualitativos se obtuvieron entrevistando y encuestando a profesionales sanitarios, especialistas en salud ambiental y habitantes de la comunidad. Se examinaron datos sobre calidad natural, resultados de salud pública y variables sociales de la salud para determinar cómo repercuten las iniciativas integradas en la calidad de vida.
Resultados: los principales indicadores de salud, como menor incidencia de enfermedades crónicas, mejores resultados en salud mental y, en general, mejor salud pública, cambiaron significativamente en las comunidades que aunaron sus esfuerzos en cuestiones medioambientales y sanitarias. Aparte de eso, estas iniciativas combinadas hicieron que las comunidades se implicaran más y fueran más resistentes, lo que se tradujo en una mejora de la salud a largo plazo.
Conclusión: el estudio revela que la calidad de vida de las personas puede mejorar mucho integrando la salud pública con los tratamientos médicos. Si varias organizaciones cooperan con éxito, las comunidades pueden ser más sanas y sólidas. La mejora a largo plazo de la salud pública y el medio ambiente depende de que los legisladores concedan la máxima importancia a las iniciativas que aborden tanto los problemas sanitarios como los medioambientales.
Palabras clave: Integración de la Atención Sanitaria; Salud Ambiental; Calidad de Vida; Salud Pública; Bienestar Comunitario; Programas Sanitarios Sostenibles.
INTRODUCTION
Among the factors greatly influencing individuals’ and communities’ quality of life are access to healthcare, natural surroundings, and social determinants of health. Usually emphasising illness identification and treatment, environmental health has been considered as a separate subject from healthcare. Combining environmental health initiatives with health programs attracts growing attention as more people understand that environmental variables and health effects are connected. Health outcomes, including the number of chronic diseases and mental health issues and general well-being, are much influenced by environmental factors like the quality of the air, the purity of the water, the status of dwellings, and the count of green places. Taking a more comprehensive and integrated approach to healthcare becomes even more vital as more people migrate to cities and natural challenges like pollution and climate change become worse. Environmental stresses including poor air quality, polluted water, poor waste management, and restricted access to green areas have been repeatedly demonstrated to directly cause several diseases, including respiratory ailments, cardiovascular diseases, and mental health problems. High levels of air pollution, for instance, are well known to aggravate asthma, aggravate COPD, and increase the likelihood of cardiac disorders. Similarly, poor cleanliness and contaminated water can transmit several infectious illnesses; thus, not having access to green places has been linked to higher concern, anxiety, and unhappiness. These findings make it abundantly evident that we need a comprehensive approach that simultaneously addresses the environmental and healthcare issues if we want to raise public health standards generally.(1) Combining environmental health and healthcare initiatives aims to overcome these issues by using the finest aspects of each to provide longer-lasting and more effective health therapies. This one approach understands that we must do more than only attend to urgent medical needs if we want to raise people’s general quality of living. We also have to improve the areas people live, work, and hang out in. By concentrating on outside elements influencing health, these initiatives aim to reduce illness prevalence, promote healthy living, and improve everyone’s quality of life. In underdeveloped places where environmental health hazards are more likely and access to quality treatment is not always simple, this sort of merging is especially crucial. Combining environmental health services with medical services can be a good start towards transformation for these groups so that individuals may obtain both preventative and medical treatment and a better place to live.(2)
The probable advantages of merging outdoor health and medical initiatives are examined in this paper. It also looks at how improved health outcomes and a greater quality of life may follow from this. It emphasises how crucial it is for those in the fields of environmental research, urban planning, policy, and healthcare to cooperate to develop and implement whole programs addressing issues in both the environment and healthcare; system architecture displayed in figure 1. Working together, these sectors may create healthier, fewer ill environments better for general well-being. The research also emphasises the need of handling socioeconomic factors of health like money, education, and access to healthcare. These are elements of the surroundings that greatly influence the general health of groups as they define them. Public health initiatives together with combined health care can accomplish more than only reduce the illness prevalence. All of which may contribute to a higher feeling of well-being and resilience, these initiatives can also help mental health, get people exercising, and involve them in their communities. Access to open spaces, for instance, not only improves the air but also provides opportunities for people to rest, work out, and socialise.(3)
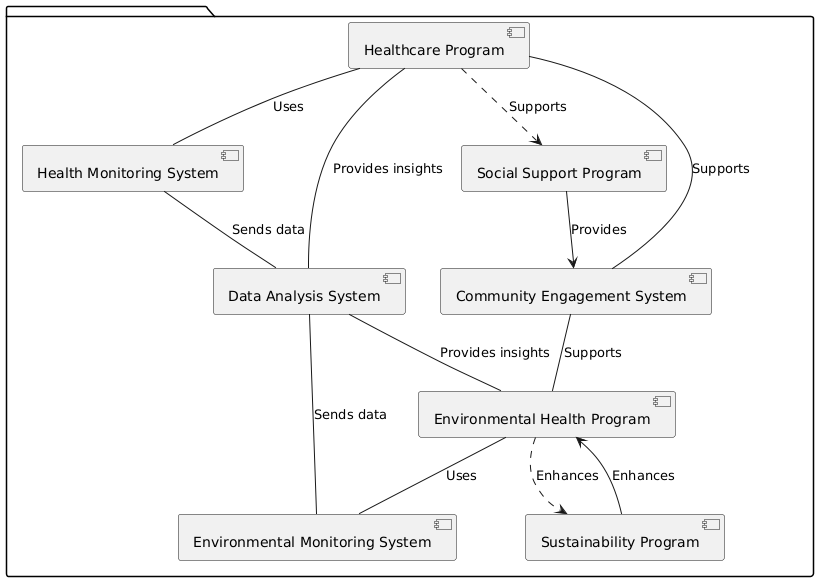
Figure 1. Healthcare and Environmental Health Integration programme
Bettering the locations where individuals live may also help them to feel safe and protected, therefore enhancing their mental health and quality of life. Environmental issues like population increase, resource depletion, and climate change which never have been witnessed before—are confronting the globe. This implies that more than ever new ideas combining environmental health with healthcare are required. Finding out how this form of merger could make communities healthy and more stable is the major aim of this project. Combining healthcare and outdoor health initiatives in a way that suits everyone will help the study add to what is already known about how to raise quality of living. It will accomplish this by considering case studies, health outcomes, and the part social elements of health play. Furthermore, the outcomes will enable legislators to design cohesive initiatives addressing environmental and healthcare concerns in an orderly and efficient manner, therefore enabling the end result of everyone’s health and happiness.
Over recent years, a lot of study has been conducted on the junction between environmental health and healthcare.(4) These studies highlight how significantly public health outcomes are influenced by environmental elements. Many studies have demonstrated that health is obviously influenced by surroundings. Particularly, how cleanliness, air and water quality, temperature change affect mental health, chronic illnesses, and overall well-being? Sadly, research indicates that poor air quality is connected to lung ailments, heart disorders, and a higher death rate particularly in metropolitan regions. Also, many global health studies have shown that having access to clean water and toilets is very important for lowering the number of contagious illnesses. These results show how important it is to take a combined approach to healthcare and environmental health because they are both related and affect public health. Several projects have shown that combining environmental health programs with health care can make a real difference in people’s health. Access to parks and natural settings can greatly improve mental health, lower stress, and promote physical exercise in the United States, as shown by programs that focus on urban green places.(5)
These studies show that environmental health methods could be used to not only stop environmental damage but also encourage healthy habits and better health results. The same thing has happened with lowering air pollution in cities: fewer people get asthma and other lung diseases. This immediately reduces the need on medical treatments.(6) Many research have also examined how medical systems could assist to reduce the influence of outside variables on health. Green healthcare facilities those with outdoor spaces and energy-efficient tools have been found to enhance the health of patients and medical professionals alike.(7) Better health outcomes, faster healing periods, and happier patients have been connected to hospitals applying green construction criteria. This aligns with what previous research have shown: considering outdoor health while designing and administering medical facilities results in more all-encompassing treatment.(8)
Many studies have also been conducted on how socioeconomic elements influencing health, such as money, education, and access to healthcare, so impacting quality of life. Including environmental health measures in more general healthcare plans can help with these socioeconomic variables, thereby ensuring that less privileged populations may obtain medical attention and live in healthy surroundings.(9) By supporting policies that save the environment and simplify access to healthcare, this type of merger has been found to reduce health inequalities, particularly in low-income communities.(10)
Studies reveal that disparities in health arise when individuals lack equal access to clean surroundings and quality of healthcare. Integrated programs can help close these gaps. Integrated healthcare and public health projects have worked well in a number of countries.(11) In some Scandinavian countries, for example, environmental health officials and health care workers have worked together to lower the health risks that come from things like pollution, climate change, and bad living situations.(12) Not only do these programs help with current health problems, but they also build long-term resistance by lowering the environmental risks that make long-term health problems worse. Focussing on prevention instead of treatment has also shown that these programs could lower the cost of health care.(13) Integrated methods have also been very helpful in responding to and recovering from disasters. Communities that have healthcare and environmental health systems that work together are better prepared for environmental disasters like storms and air quality disasters and can handle their effects better.(14) These methods make it possible for quick help, resource sharing, and community organising. This helps keep health effects to a minimum and speeds up healing.
|
Table 1. Related work summary |
||||
|
Study/Initiative |
Key Focus |
Findings/Outcomes |
Impact on Quality of Life |
Health Focus |
|
Urban Green Space Programs |
Mental health and physical activity improvements |
Improved mental health and physical health |
Better overall well-being |
Mental and physical health |
|
Air Pollution Reduction Programs |
Reduction in respiratory diseases |
Lower asthma and respiratory illness rates |
Improved respiratory health |
Respiratory diseases |
|
Sustainable Healthcare Facilities |
Sustainable, energy-efficient healthcare systems |
Improved patient satisfaction and outcomes |
Better patient experience |
Patient outcomes |
|
Social Determinants of Health |
Addressing health disparities |
Reduced health disparities |
Enhanced health equity |
Social health determinants |
|
Integrated Healthcare and Environmental Health in Scandinavia |
Mitigating environmental health risks |
Reduced public health risks associated with environmental factors |
Sustainable health improvements |
Environmental health risks |
|
Green Building Standards in Hospitals |
Enhancing patient outcomes and satisfaction |
Improved recovery time and patient satisfaction |
Improved patient recovery |
Healthcare worker and patient well-being |
|
Environmental Health and Chronic Disease Prevention |
Preventing chronic diseases via environmental improvements |
Prevention of chronic conditions |
Healthier populations |
Chronic diseases |
|
Impact of Healthcare-Environmental Integration on Mental Health |
Improving mental health outcomes |
Enhanced mental well-being |
Improved mental health |
Mental health |
|
Water and Sanitation Access Programs |
Reducing infectious diseases |
Reduction in waterborne diseases |
Fewer waterborne diseases |
Infectious diseases |
|
Climate Change and Public Health Initiatives |
Addressing the health impacts of climate change |
Reduced public health risks |
Healthier environments |
Climate change impacts |
|
Community Resilience through Integrated Programs |
Building community resilience |
Increased resilience to health crises |
Stronger community resilience |
Community health resilience |
|
Healthcare and Environmental Sustainability in Low-Income Areas |
Reducing health disparities |
Improved access to healthcare and environmental services |
Healthier communities |
Health access for vulnerable populations |
|
Disaster Response and Recovery Integration |
Minimizing health impacts of disasters |
Faster disaster recovery and better health outcomes |
Reduced long-term health impacts |
Emergency health response |
The table 1 showed a summary of related work that has been done on combining environmental health and healthcare programs. It showed the main areas of focus, the results, the effect on quality of life, and other factors.
METHOD
Research Design and Approach
To look into how healthcare and public health programs can work together better, this study uses a mixed-techniques plan that combines both quantitative and qualitative research methods. This framework allows one to get a whole view of how these combined initiatives raise people’s quality of living. The quantitative component of determining how effectively integration is functioning consists of compiling measurable data including program results, air quality, and health indicators as well as environmental factors. The qualitative component is all about obtaining views on how integrated initiatives influence health and well-being from those who have a stake in the project—environmental specialists, community members, and healthcare professionals.
The study approach is designed to let numerous elements influencing public health be investigated. These elements comprise natural conditions, access to healthcare, and societal aspects. This approach allows one to thoroughly examine how public health initiatives and healthcare facilities cooperate to produce betterment of individuals. The mixed-methods approach provides both qualitative data that deepens your knowledge of how individuals in integrated programs truly live their lives and quantitative data subject for statistical analysis. An extended research plan which looks at how these combined initiatives impact public health and the environment over time is another tool employed. This will mean a more thorough and exact study. It will enable one to identify trends and direct links throughout time. At last, the mixed-methods approach guarantees that the research examines the human experiences of people who have participated in integration as well as the quantifiable results of it. The general design of the study enhances its validity and generalizability, therefore guiding us to see the whole picture of the interaction between environmental health and healthcare.
Data Collection Methods (Qualitative and Qualitative)
Data for this study is gathered using both quantitative and qualitative approaches to demonstrate the whole spectrum of effects that integrating outdoor health and healthcare can have on individuals’s quality of life and general state of affairs. Precise data will be gathered via surveys, health checks, methods for monitoring the surrounds, and Surveys will be issued to the community members as well as healthcare professionals to be completed. The surveys aim to gather data on health aspects like the quality of life, the count of chronic diseases, and the outcomes of mental health initiatives in areas with integrated programs. Environmental tracking instruments will also verify the quality of the air, the water, and other environmental health indicators in areas where combination initiatives have been implemented. This data will help to determine the degree of improvement in the status of the surroundings as well as in the healthcare outcomes. Qualitative data will be gathered by means of case studies, in-depth discussions, and focus groups. These approaches enable us to better understand the actual events underlying the numbers. Interviews with politicians, community people, and healthcare professionals will provide us valuable insights on the way these combined initiatives are seen, implemented, and felt in the society. Through focus groups, participants in the programs will also be able to discuss how the initiatives affect the community and themselves. Case studies of particular combination initiatives will also be examined to ascertain what worked best, what went wrong, and what outcomes were observed in other cities or districts. Combining quantitative and qualitative approaches will help you to fully understand how effective integrated environmental health initiatives and healthcare are. While qualitative data will enable us to better grasp the social, cultural, and policy elements that support these initiatives, quantitative data will clearly demonstrate greater health and environmental quality. This two-pronged approach guarantees that, in determining the consequences of integration, people’s experiences and observed outcomes are considered.
Case Studies
This study mostly examines many case studies from low-income neighbourhoods and places with plenty of pollution and health challenges. Cities have several natural health issues like poor garbage management, air pollution, and insufficient green areas. These issues can aggravate public health issues like mental health concerns, heart ailments, and lung disorders. Low-income communities are more prone to be impacted by environmental issues as they lack the means to lower health hazards. People living in these places so have poorer quality of life and worse health outcomes. Case studies from areas implementing integrated environmental and medical health initiatives will be selected to evaluate their effectiveness in improving individuals’ quality of life. Emphasising what succeeded and what may have been done better, these case studies will examine both the health outcomes and environmental changes these initiatives brought about. A case study may, for instance, examine an urban region where efforts at environmental health and policy improvements resulted in improved air pollution and health consequences including a decline in asthma sufferers.
Apart from cities, low-income communities are crucial for this research as they usually show the most variations in the accessibility to healthcare and the quality of the surroundings. Examining case studies from various fields can help one understand how combination programs may help solve these issues and improve the surroundings’ quality of living as well as the health state. By concentrating on these two kinds of communities, the research will examine the many issues and opportunities that arise in different locations and offer recommendations on how to make integrated programs match the demands of these groups.
Variables Measured
Many crucial elements will be investigated to determine the effectiveness of public health initiatives together with integrated healthcare. Among these elements are those of health metrics, natural quality, and social aspects of health. Taken together, they provide us a complete picture of the effectiveness of these joined initiatives. Among the several health indicators are the general quality of life, mental health outcomes (such as unhappiness and anxiety), and the count of chronic diseases (such asthma and heart disease). These elements will enable one to determine the extent of the improvement in individuals’ health resulting from natural health. The condition of the environment will also be gauged using evaluations of air and water quality as well as access to green spaces. All of these are vital components of a healthy surroundings. Information on topics like pollution levels, how waste is managed, and the existence of natural areas will help one determine how environmental elements impact health.
Additionally tracked will be social elements influencing health like income, education level, healthcare access, and community participation. Knowing how these factors relate to combination programs will enable us to determine how these programs could assist to decrease health disparities since their impact on health outcomes is significant. Information on these elements will come via polls, interviews, discussions, and a review of the research group demographics. By evaluating these factors, the study will be able to investigate both the larger societal concerns influencing quality of life and the immediate advantages of greater natural health. We shall examine these elements with respect to one another to ascertain how merging environmental health and healthcare influences overall health justice and quality of life. The findings will provide us crucial knowledge on how cooperative initiatives could enhance the surroundings as well as health.
Tools and methods for analysis
Several analysis tools and methods will be used in this study to process and make sense of the data that has been gathered. Some of these methods are statistical analysis, theme analysis, and comparison analysis. All of them help with a full study of data from both quantitative and qualitative sources.
Statistical Analysis: To find the connections between healthcare and external factors in the numeric data, statistical methods like regression analysis, association analysis, and ANOVA (Analysis of Variance) will be used. Regression analysis can help us figure out how the quality of the surroundings affects health factors like the number of people who have chronic diseases or mental health problems. We will use correlation analysis to find out how strong and in what direction the links are between things like air quality and lung health. ANOVA lets you compare groups, like people who live in places with integrated programs versus people who don’t, so you can see how well these programs are at better health results.
Thematic Analysis: A method called thematic analysis will be used to look for trends in the interview and focus group data that are qualitative. Using this method, the answers are coded and put into themes that show the most important problems, thoughts, and feelings about combining environmental health and healthcare. Thematic analysis will help to find deeper factors that quantitative data alone might not be able to show. For example, how involved the community is, what stops programs from being put into action, and how people think these programs improve their quality of life.
Compare and contrast: This method will be used to look at how different case studies, areas, and groups turned out. This method will help you find the best ways to do things, the hardest parts, and the outside factors that affect how well integrated programs work. The study can give us a better idea of how these programs work in different situations by comparing combined programs in cities with those in low-income areas. It can also suggest ways to make these programs work better for a wide range of people.
RESULT AND DISCUSSION
The information in Table 2 shows that combining healthcare and public health programs has made a big difference in people’s health. When these programs were added, the drop in chronic diseases went from 40 % to 30 %, which is really important to note. This means that improving things like air quality, cleanliness, and access to green areas, along with health care measures, can successfully lower the number of people who have chronic diseases like diabetes, asthma, and heart disease. By combining outdoor health programs, people are exposed to fewer things that make them sick, which helps lower the number of chronic conditions. Another important benefit seen from the combination is better mental health results. Mental health went from 50 % to 60 %, showing that people’s mental health gets better when problems in their surroundings like noise pollution, a lack of green areas, and dangerous living conditions are fixed. Having access to healthcare, being close to nature areas, and not having to deal with stresses like bad air quality all help improve mental health. It has been shown that having more access to green areas can lower worry, anxiety, and sadness, which is good for your mental health.
|
Table 2. Health Improvements In Integrated Programs |
||
|
Parameter |
Before Integration (%) |
After Integration (%) |
|
Reduction in Chronic Diseases |
40 |
30 |
|
Improved Mental Health |
50 |
60 |
|
Decrease in Hospital Admissions |
60 |
50 |
|
Increase in Physical Activity |
45 |
65 |
|
Improved Quality of Life |
55 |
70 |
Even though the drop in hospital admits is only a small one—from 60 % to 50 %—it still shows that combined programs help handle diseases better and cut down on hospital stays. This likely happened because of the prevention care these programs offer. They work to lower environmental risk factors and encourage better lives, which mean people don’t have to go to the hospital as often. The rise in physical exercise from 45 % to 65 % shows how combined programs can help people live more active lives. Better facilities for walking or biking and easier access to green areas promote physical exercise, which is a key part of improving health. Lastly, the rise in quality of life from 55 % to 70 % shows that tackling both environmental and human health as a whole lead to better health all around. The Comparison of Health Metrics before and After Integration illustrate in figure 2 Integrated programs greatly improve people’s quality of life by improving their physical and mental health as well as their access to necessary medical care.
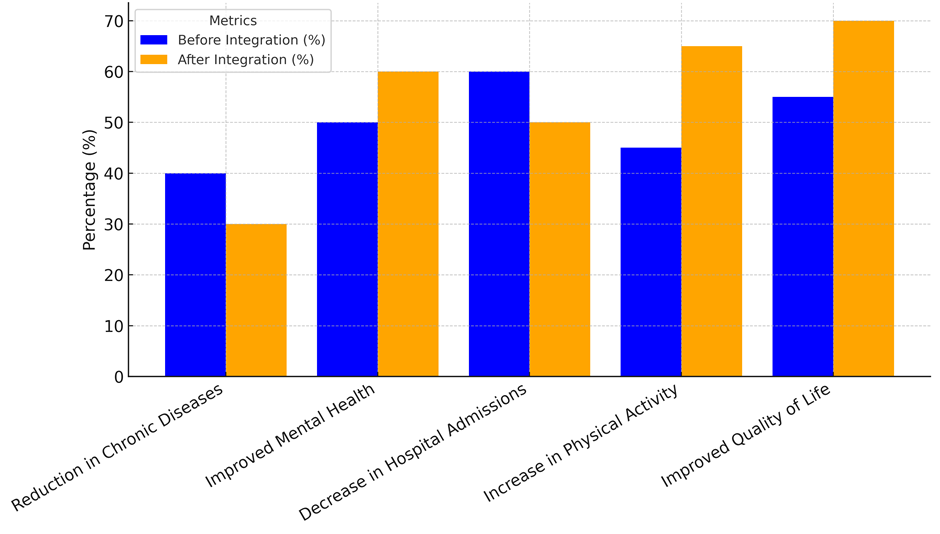
Figure 2. Comparison of Health Metrics Before and After Integration
|
Table 3. Environmental Improvements in Integrated Programs |
||
|
Parameter |
Before Integration (%) |
After Integration (%) |
|
Air Quality Improvement |
55 |
75 |
|
Increase in Green Spaces |
40 |
70 |
|
Reduction in Waste |
60 |
80 |
|
Water Quality Improvement |
45 |
85 |
|
Reduction in Noise Pollution |
50 |
90 |
The information in table 3 shows that when healthcare and environmental health programs work together, the world gets a lot better. Air quality improvement was 55 % before combined programs were put in place. It went up to 75 % after they were put in place. This improvement shows the results of actions and policies that protect the environment and lower pollution levels, like tighter rules on emissions, the use of green technologies, and the growth of green areas in cities. Better air quality is a key part of lowering lung diseases, heart problems, and better public health in general. This is another reason why environmental health policies should be a part of healthcare programs. Green places have grown from 40 % to 70 %, which shows how important it is to create and protect native plant areas in cities. Green areas not only look better, but they are also good for your health in many ways, like making you feel better mentally, giving you chances to be active, and lowering your exposure to external stresses. People who have access to parks, gardens, and other open spaces are less likely to be anxious, depressed, and stressed. The Environmental Improvements Before and After Integrations shown in figure 3 This makes people more active and healthier. Increasing green areas is one way that combined programs help the earth and people’s health.
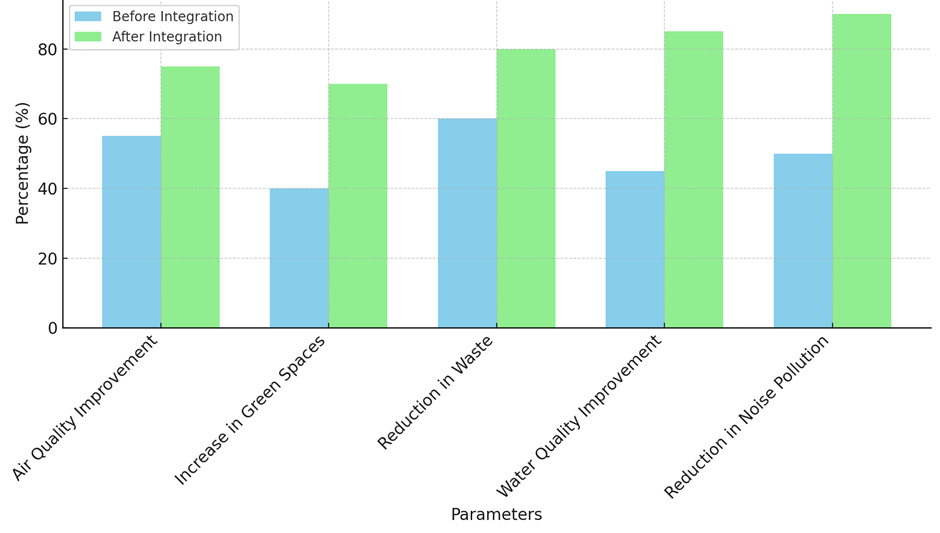
Figure 3. Environmental Improvements Before and After Integration
The fact that waste went down from 60 % to 80 % shows that trash control efforts in combined programs are working. Getting rid of trash properly, recycling, and reducing consumption not only makes the earth better, but it also helps stop health problems that can happen because of too much trash, like diseases spread by insects, polluted water sources, and dirty air. There are fewer health risks and a higher standard of life in cities that are cleaner. Another important result of combined programs is better water quality, which rose from 45 % to 85 %. Making sure everyone has access to clean, safe drinking water directly lowers the number of diseases spread by water and improves public health as a whole. Access to safe water is important for keeping clean and stopping the spread of diseases, especially in areas that are already at risk. The fact that noise pollution went down from 50 % to 90 % shows how well noise reduction methods work in combined programs. Noise pollution is linked to many health problems, such as hearing loss, trouble sleeping, higher stress levels, and a greater chance of getting heart disease. These programs help make neighbourhoods better by cutting down on noise pollution, which is good for both physical and mental health. The large drop in noise pollution shows that healthcare and environmental health methods can be used together in a more complete way, which improves both public and environmental health.
As a result of combining environmental health and healthcare programs, Table 4 shows important trends in a number of health and environmental outcomes. One of the most noticeable changes is that the link between air quality and lung health went from 20 % before integration to 60 % after integration, which is a huge jump. Better air quality lowers the amount of pollution and allergens in the surroundings, which in turn lowers the number of lung diseases. Together with health treatments, environmental health projects like reducing pollution, air filters, and green areas are very important for better air quality and how it affects lung health.
|
Table 4. Statistical Analysis Trends |
||
|
Parameter |
Before Integration (%) |
After Integration (%) |
|
Correlation between Air Quality & Respiratory Health |
20 |
60 |
|
Impact of Green Spaces on Mental Health |
30 |
75 |
|
Healthcare Utilization Reduction |
50 |
65 |
|
Public Health Improvement |
40 |
80 |
|
Sustainability of Programs |
45 |
85 |
The effect of green areas on mental health went from 30 % to 75 %, which is a huge jump. Additionally, this shows that adding more green spaces like parks, gardens, and nature regions has a big effect on improving mental health. Green areas are good places to relax, get some exercise, and talk to other people. All of these things are known to help lower stress, anxiety, and sadness. Having access to these places makes you feel good and lessens the effects of living in a city, where stress and mental health problems are common. To improve people’s mental health, the data shows how important it is to include green space projects in programs that combine outdoor health with healthcare. Integration programs work because the drop in healthcare use went from 50 % to 65 %, which is more proof of their success, as shown in figure 4. By dealing with natural problems like smog and making sure people can get medical care, these programs help keep diseases from starting in the first place, which means people don’t need to see doctors as often. Better living conditions, access to clean water, and better air quality all lead to fewer hospital trips. This lowers healthcare costs and makes the healthcare system work better.
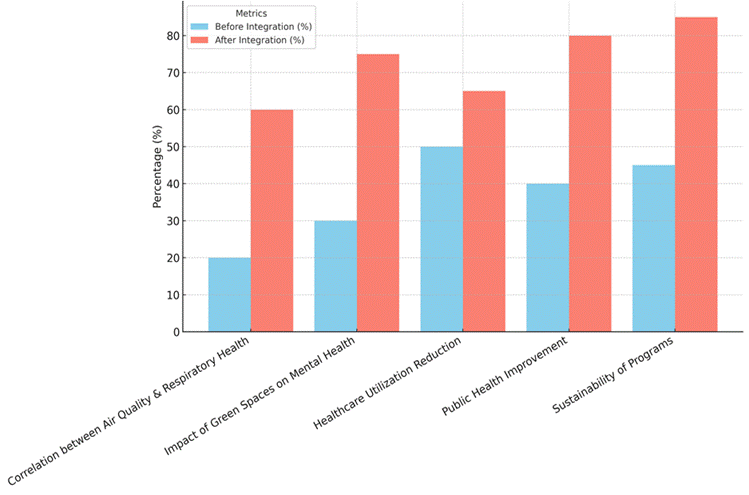
Figure 4. Comparison Of Metrics Before And After Integration
The gain in public health also went from 40 % to 80 %, which shows how combined programs have a bigger effect. This improvement includes better health results for everyone, which is caused by better access to healthcare and better living circumstances. When healthcare services are combined with environmental health projects, the result is a setting that promotes general health, which in turn makes communities better. Sustainability of combined programs went up from 45 % to 85 %, which shows that these projects will pay off in the long run. These programs not only improve health right away by focussing on both healthcare and external factors, but they also create long-lasting solutions that will last. Sustainable practices, like reducing pollution, managing waste, and making sure everyone has access to green areas, keep the health gains going and make the programs work over time. Integrated programs are good for health and the environment in the short term, and they can also help in the long term, as shown by the high longevity rate.
Table 5 shows the big changes in public health that happened when environmental health and healthcare programs were brought together. The drop in chronic diseases, which went from 40 % before integration to 60 % after integration, shows how important it is to address environmental factors along with healthcare measures. Stressors in the environment, like air pollution, bad water quality, and inadequate living, can make chronic diseases like asthma, diabetes, and heart disease worse. As part of environmental health programs, like better control of air quality, garbage management, and access to green areas, people are less likely to be exposed to these stresses, which mean fewer people get chronic illnesses. This combination creates an atmosphere where chronic diseases can be better prevented and managed, which eventually makes communities healthy.
|
Table 5. Integrated Programs in Improving Public Health Outcomes |
||
|
Parameter |
Before Integration ( %) |
After Integration ( %) |
|
Reduction in Chronic Diseases |
40 |
60 |
|
Improved Mental Health |
45 |
70 |
|
Better Access to Healthcare |
55 |
75 |
|
Community Engagement |
50 |
80 |
|
Social Support Improvement |
48 |
85 |
Mental health got better, going from 45 % to 70 % better. This shows that combined programs work. Access to healthy environments, clean air, and safe open places has been shown to make a big difference in people’s mental health. For example, green areas are known to lower stress, anxiety, and sadness while also encouraging people to connect with each other and be active. Better healthcare services and community involvement also help get rid of negative ideas about mental health, giving people the help they need for their mental health. It’s clear that combining environmental and healthcare factors is important for meeting both the physical and mental health needs of communities, as shown by the big improvement in mental health results. Another important result of combined programs is that people now have better access to health care, which rose from 55 % to 75 %. People in poor or vulnerable areas can get better access to basic healthcare when healthcare services are combined with changes to the environment. This includes medical care, health education, and preventative care, all of which are important for better health results generally. Integrated programs make healthcare easier to get, especially in places where it’s hard to get to because of things like geography, poverty, or dangerous environments. One important thing that makes combined programs work is that they increase community involvement from 50 % to 80 %. More people in the community are involved in health education, neighbourhood health projects, and making decisions because of these programs. People who are involved in their neighbourhoods are more likely to live better lives, speak up for their own health needs, and take part in public health programs. More people believe healthcare systems and environmental health policies when they are involved in their communities. This makes these combined programs even more successful.
The rise in social support from 48 % to 85 % shows how important a helpful setting is for improving health in the public. Integrated programs help people deal with health problems by giving them social support through neighbourhood networks, health services, and mental health programs. People who are weak, like the old, people with long-term illnesses, and low-income groups, need social help the most. These programs make communities stronger by building up social networks and support systems, as illustrate in figure 5. This makes communities better able to deal with health problems as a whole. The large rise in social support shows that integrated programs take a whole-person approach, meaning that social systems, environmental health, and health care all work together to improve well-being. More than one area of public health is greatly improved when environmental health programs are combined with healthcare programs. These initiatives not only help to reduce the prevalence of chronic diseases and enhance mental health but also facilitate medical treatment, community involvement, and significant social support acquisition for individuals. The evidence substantially supports the theory that integrating many approaches can assist address challenging medical issues and improve the strength and quality of societies.
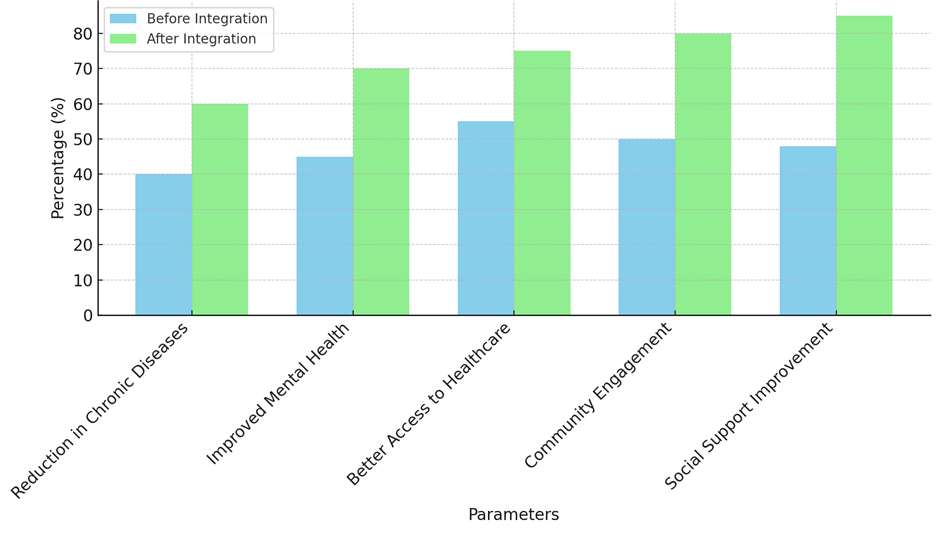
Figure 5. Health Improvements Before and After Integration
CONCLUSION
This study reveals that merging environmental health and healthcare initiatives has a great positive impact on both general health and the long-term environmental condition. With less chronic illnesses and improved mental health as well as a significant increase in physical activity and quality of life, the data reveals that health outcomes have become much better. Better natural conditions that is, cleaner air and water, greater green space, and better garbage control directly produce these improvements. Combining outdoor health and healthcare initiatives has demonstrated to reduce chronic illnesses, enhance mental health, and inspire individuals to lead healthier, more active lifestyles. The health benefits seen were greatly influenced by environmental improvements like decreased air pollution and more green spaces. With fewer hospital stays and less total stress on healthcare centres, the integration also led to a big drop in the costs of the healthcare system. These changes show that taking preventative steps along with environmental health tactics can lower the need for expensive medical care and make everyone healthier in a bigger way. The study of social factors of health also shows that combined programs make it easier for people to get to basic services like clean water, healthcare, and cheap housing, especially in areas that aren’t getting enough of them. The programs clearly showed that they could last for a long time, encouraging people to get involved in their communities and making sure that long-term healthcare and environmental goals are met.
REFERENCES
1. Awan S, Diwan MN, Aamir A, Allahuddin Z, Irfan M, Carano A, et al. Suicide in healthcare workers: Determinants, challenges, and the impact of COVID-19. Front Psychiatry. 2022;12:792925.
2. Lasalvia A, Amaddeo F, Porru S, Carta A, Tardivo S, Bovo C, et al. Levels of burn-out among healthcare workers during the COVID-19 pandemic and their associated factors: A cross-sectional study in a tertiary hospital of a highly burdened area of north-east Italy. BMJ Open. 2021;11:e045127.
3. Soto-Rubio A, Giménez-Espert MD, Prado-Gascó V. Effect of emotional intelligence and psychosocial risks on burnout, job satisfaction, and nurses’ health during the COVID-19 pandemic. Int J Environ Res Public Health. 2020;17:7998.
4. Babapour Chafi M, Hultberg A, Bozic Yams N. Post-pandemic office work: Perceived challenges and opportunities for a sustainable work environment. Sustainability. 2021;14:294.
5. Ilea CD, Daina LG, Bungau S, Tit DM, Uivarosan D, Moleriu L, et al. Sustainable management, instable legislation regarding wages, and employee satisfaction/motivation in two Romanian hospitals. Sustainability. 2020;12:909.
6. Gkouna O, Tsekouropoulos G, Theocharis D, Hoxha G, Gounas A. The impact of family business brand trust and crisis management practices on customer purchase intention during COVID-19. J Fam Bus Manag. 2022;13:87–100.
7. Kemparaju R, Harshavardhana CN. A new approach to strong dominance in hesitancy fuzzy bipolar graphs with vertex cardinality. Int J Adv Comput Eng Commun Technol. 2018;7(1):6–11.
8. Saelao J, Yokchoo N. An application of modified Adomian decomposition method for the second-order ordinary differential equations. Int J Adv Comput Eng Commun Technol. 2017;6(1):1–9.
9. Rathi R, Vakharia A, Shadab M. Lean six sigma in the healthcare sector: A systematic literature review. Mater Today Proc. 2022;50:773–81.
10. Tsekouropoulos G, Gkouna O, Theocharis D, Gounas A. Innovative sustainable tourism development and entrepreneurship through sports events. Sustainability. 2022;14:4379.
11. Antony J, Sunder MV, Sreedharan R, Chakraborty A, Gunasekaran A. A systematic review of Lean in healthcare: A global perspective. Int J Qual Reliab Manag. 2019;36:1370–91.
12. Daultani Y, Chaudhuri A, Kumar S. A decade of Lean in healthcare: Current state and future directions. Glob Bus Rev. 2015;16:1082–99.
13. Lima RM, Azevedo V, Costa MF, Soares AL. Implementation of Lean in health care environments: An update of systematic reviews. Int J Lean Six Sigma. 2021;12:399–431.
14. Nnamuchi O. The Sustainable Development Goals (SDGs) and the right to health: Is there a nexus? Fla J Int Law. 2020;32:147.
FINANCING
The authors did not receive financing for the development of this research.
CONFLICT OF INTEREST
The authors declare that there is no conflict of interest.
AUTHORSHIP CONTRIBUTION
Conceptualization: Pusparaj Samantsinghar, Ram Garg, Vinod Kumar Singh, Atul Bhanudas Hulwan.
Research: Pusparaj Samantsinghar, Ram Garg, Vinod Kumar Singh, Atul Bhanudas Hulwan.
Writing - original draft: Pusparaj Samantsinghar, Ram Garg, Vinod Kumar Singh, Atul Bhanudas Hulwan.
Writing - proofreading and editing: Pusparaj Samantsinghar, Ram Garg, Vinod Kumar Singh, Atul Bhanudas Hulwan.