doi: 10.56294/hl2023317
ORIGINAL
Healthcare Education as a Mechanism for Advancing Patient-Centric Care Frameworks
La educación sanitaria como mecanismo para impulsar marcos asistenciales centrados en el paciente
Wakeel Ahmed1
![]() ,
Shailly Gupta2
,
Shailly Gupta2 ![]() ,
Bhupal Pujari3
,
Bhupal Pujari3 ![]() ,
Rajashree Panigrahi4
,
Rajashree Panigrahi4 ![]()
1School of Liberal Arts, Noida International University, Greater Noida, Uttar Pradesh, India.
2Arya College of Pharmacy, Jaipur, Rajasthan, India.
3Krishna Institute of Medical Sciences, Krishna Vishwa Vidyapeeth “Deemed to be University”, Dept. of Medicine, Taluka-Karad, Dist-Satara, Maharashtra, India.
4IMS and SUM Hospital, Siksha ‘O’ Anusandhan (Deemed to be University), Department of Microbiology, Bhubaneswar, Odisha, India.
Cite as: Ahmed W, Gupta S, Pujari B, Panigrahi R. Healthcare Education as a Mechanism for Advancing Patient-Centric Care Frameworks. Health Leadership and Quality of Life. 2023; 2:317. https://doi.org/10.56294/hl2023317
Submitted: 05-06-2023 Revised: 21-08-2023 Accepted: 26-11-2023 Published: 27-11-2023
Editor:
PhD. Prof. Neela Satheesh ![]()
ABSTRACT
Healthcare education is very important for changing the way patients are cared for, especially when it comes to promoting patient-centered frameworks that put each person’s wants, desires, and values first. Changing our emphasis to patient-centered approaches is more crucial than ever as it grows more difficult for healthcare systems all over to manage big numbers of complex patients and enhance outcomes. Emphasising the need of healthcare professionals knowing what they are doing and for individuals to be active in their treatment, this article explores how healthcare education might assist bring about these significant improvements. Patient-centered care (PCC) is based on the principle that, with an eye towards cooperation among healthcare professionals, people should participate in choices regarding their own treatment. Education is mostly responsible for ensuring that patients and healthcare professionals with the knowledge, tools, and attitudes required for their dynamic cooperation. It enables physicians to better understand the cultural concerns, needs, and challenges that could compromise the treatment of a patient. It also enables patients to participate actively in their treatment regimens and make independent decisions. Furthermore, healthcare education promotes the development of interdisciplinary teams, therefore enabling individuals from several healthcare disciplines to collaborate and offer improved general treatment. By means of evidence-based practices, it also creates the conditions for continuous improvement, ensuring that patient care reflects the developments in medical knowledge and technology. Future healthcare professionals also acquire from their education empathy, cultural awareness, and effective communication skills that will enable them to handle the difficulties of patient-centered care. Ultimately, healthcare education not only improves the quality of the healthcare professionals but also makes patients happier, more inclined to follow their treatment programs, and generally healthier. This article argues for investing a lot of time in healthcare education to obtain patient-centered care models adopted by many people and thus increase the flexibility, openness, and fairness of the healthcare system.
Keywords: Patient-Centered Care; Healthcare Education; Patient Empowerment; Interdisciplinary Collaboration; Healthcare Systems Transformation.
RESUMEN
La educación sanitaria es muy importante para cambiar la forma de atender a los pacientes, especialmente cuando se trata de promover marcos centrados en el paciente que antepongan los deseos, anhelos y valores de cada persona. Cambiar nuestro énfasis hacia enfoques centrados en el paciente es más crucial que nunca, ya que cada vez es más difícil para los sistemas sanitarios de todo el mundo gestionar un gran número de pacientes complejos y mejorar los resultados. Este artículo, que hace hincapié en la necesidad de que los profesionales sanitarios sepan lo que hacen y de que las personas participen activamente en su tratamiento, explora cómo la educación sanitaria puede ayudar a conseguir estas mejoras significativas. La atención centrada en el paciente (ACP) se basa en el principio de que, con vistas a la cooperación entre los profesionales sanitarios, las personas deben participar en las decisiones relativas a su propio tratamiento. La educación es la principal responsable de garantizar que los pacientes y los profesionales sanitarios cuenten con los conocimientos, las herramientas y las actitudes necesarias para su cooperación dinámica. Permite a los médicos comprender mejor las preocupaciones, necesidades y retos culturales que podrían comprometer el tratamiento de un paciente. También permite a los pacientes participar activamente en sus regímenes de tratamiento y tomar decisiones independientes. Además, la educación sanitaria promueve el desarrollo de equipos interdisciplinares, lo que permite a personas de varias disciplinas sanitarias colaborar y ofrecer un mejor tratamiento general. Mediante prácticas basadas en la evidencia, también crea las condiciones para la mejora continua, garantizando que la atención al paciente refleje los avances del conocimiento médico y la tecnología. Los futuros profesionales sanitarios también adquieren con su educación empatía, conciencia cultural y habilidades de comunicación eficaces que les permitirán afrontar las dificultades de una atención centrada en el paciente. En última instancia, la educación sanitaria no sólo mejora la calidad de los profesionales sanitarios, sino que también hace que los pacientes estén más contentos, más dispuestos a seguir sus programas de tratamiento y, en general, más sanos. Este artículo aboga por invertir mucho tiempo en la educación sanitaria para conseguir modelos de atención centrada en el paciente adoptados por muchas personas y aumentar así la flexibilidad, apertura y equidad del sistema sanitario.
Palabras clave: Atención Centrada en el Paciente; Educación Sanitaria; Empoderamiento del Paciente; Colaboración Interdisciplinar; Transformación de los Sistemas Sanitarios.
INTRODUCTION
Patients’ requirements are evolving, medical technology is improving, and healthcare needs are growing more complex, which is causing major changes in the sector. One of the most obvious shifts of late is the shift towards patient-centered care (PCC). To offer more individualised and efficient healthcare, PCC is a method that emphasises the person’s interests, needs, and values. The foundation of this transformation is healthcare education, which also provides a great means of forward movement of patient-centered care models. Both consumers and healthcare professionals must be trained if we are to create a healthcare system where the patient takes front stage in decision-making and treatment delivery. The foundation of patient-centered care is the concept that treatment should be tailored to match the particular requirements of every patient rather than applied using a one-size-fits-all approach. This approach emphasises the need of treating patients as partners in their treatment and including them in decisions influencing their welfare and condition. Conversely, changing from conventional care models to patient-centered methods calls for a whole strategy.(1) A major component of bringing about this is healthcare education. Teaching fundamental skills is only one aspect of healthcare education; another is arming healthcare professionals with the values, tools, and attitudes they require to interact with patients and grasp all of their requirements. The effectiveness of patient-centered care depends much on the education of healthcare workers as it provides them the tools to interact with patients to make decisions with them, exhibit empathy, and express effectively.
Furthermore, ensuring that clinicians remain current on new technologies, evidence-based approaches that can significantly enhance patient care even more, and innovative procedures depends mostly on healthcare education. Moving patient-centered treatment ahead depends much on patient education as well. Providing individuals with the knowledge required to grasp their symptoms, treatment options, and the probable outcomes of various treatments helps them to participate in the decision-making about their own health. Apart from making patients happier, this sense of autonomy helps them follow their treatment recommendations, therefore improving their long-term health outcomes. Patients can make better decisions about their care when they know more about the healthcare system, the tools that are available, and how to find their way around it. This builds a stronger relationship between the patient and the healthcare worker. Also, healthcare education encourages cooperation between different fields, which is an important part of patient-centered care.(2) A lot of the time, different healthcare experts work together to give the best care to a patient. Each brings their own unique skills to the treatment plan. To make sure that care is organised, quick, and patient-centered, it is important to teach students how to work together and communicate with people from different fields. Interdisciplinary training helps healthcare workers understand each other’s jobs better, share their ideas, and help provide better care for patients as a whole.
Definition of Patient-Centric Care
When someone is getting medical care, patient-centered care (PCC) puts the patient’s needs, wants, and beliefs first throughout the whole process. Traditional care models tend to focus on the illness or condition itself. Patient-centered care, on the other hand, sees the patient as a whole, taking into account not only their physical health but also their mental, psychological, and social well-being. Patients make choices about their own care, which is at the heart of PCC. This makes patients partners in the healing process. This method takes into account that each patient has specific needs and that their personal beliefs, culture, and life situations affect the healthcare decisions they make. Under a patient-centered care paradigm, doctors aim to perceive things from the patient’s point of view, have meaningful conversations with them about their care decisions, and assist them in making decisions grounded on factual information.(3) Making sure that treatment approaches not only benefit the patient but also match their values and tastes is another aim. This approach emphasises sensitivity, respect, and open communication between patients and healthcare professionals, therefore fostering trust and facilitating cooperation among all the staff. Often indicators of patient-centered care are improved patient contentment, improved compliance to treatment programs, and better health outcomes. PCC is also about ensuring that patients receive the correct services at the correct moment for their needs and about simplifying the access to care. It forces healthcare organisations to provide coordinated care combining several forms of treatment, including preventive, therapeutic, and hospice services, so better addressing the evolving demands of consumer.(4)
Importance of Healthcare Education in Patient-Centric Care
Education in healthcare is very important for promoting patient-centered care (PCC) because it gives healthcare workers the information, skills, and attitudes they need to connect with patients in a useful and caring way. Healthcare workers need to learn about the values of teamwork, communication, and shared decision-making in order to successfully use a patient-centered method. Figure 1 shows how important healthcare education is for providing care that is focused on the patient and making results better for patients.
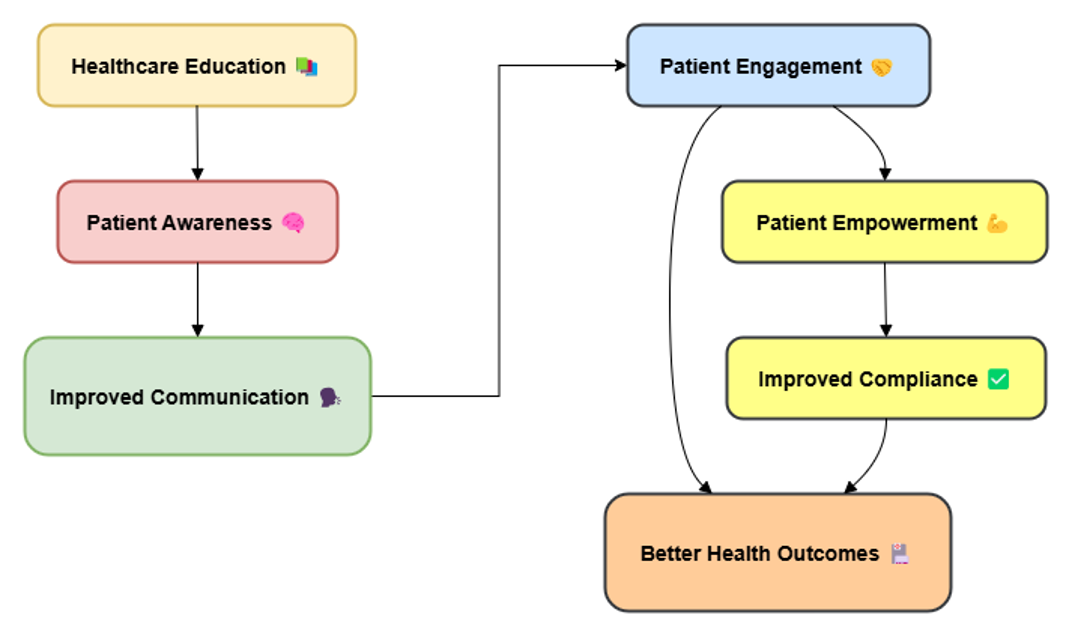
Figure 1. Importance of Healthcare Education in Patient-Centric Care
These values are built on PCC. Without the right education and training, healthcare workers might not fully grasp how important it is to include patients in choices about their care, which can make patient-centered projects less effective. Teaching healthcare experts the way to admire and hold close numerous cultures is a crucial component in their education in trendy. by using training professionals about the various reports, ideals, and requirements in their patients, training in healthcare guarantees that they are able to deliver remedy touchy to and respectful of cultural versions.(5) In the multinational healthcare environments of today, in which knowledge of the many needs and goals of individuals from many civilisations may also result in stepped forward treatment and effects, this is mainly vital. Coaching healthcare workers effective communication is likewise rather important for his or her schooling. Clean, compassionate conversation via medical doctors to their patients enables them to broaden nearer bonds and feel secure sufficient to percentage their wants and issues. Moreover imparting individuals with the tools they want to take part actively in their very own treatment is healthcare schooling. Teaching patients provides them with the information required to make wise decisions for their health. This advances patient freedom and involvement in the course of treatment. Patient education goes beyond only informing patients about medical conditions or treatments. Along with teaching kids their rights, how to use the healthcare system, and how to make decisions along with their personal beliefs and objectives.(6) This knowledge makes the relationship between the patient and therapist stronger. It also leads to better health results by making patients happier, more likely to follow their treatment plans, and healthier overall.
Evolution of Patient-Centric Care Models
Patient-centered care models have been slowly coming into being over time, with changes in both medical practice and social values playing a role. In the past, healthcare models relied on the provider’s knowledge, with doctors making most choices based on clinical standards and their own professional judgement. In these setups, people mostly just took care of themselves and didn’t have much say in what happened. Some people are saying that this method isn’t meeting all of patients’ needs because it doesn’t take their tastes, beliefs, or mental health into account. In the early 1900s, there was a slow change in how healthcare workers thought about involving patients. The idea of “patient autonomy,” which says that patients should be able to make their own health choices based on good information, started to catch on.(7) More individuals realising how crucial it is for patients and healthcare professionals to be able to communicate with one another and because patient rights were gaining more attention helped to drive this trend in part. The patient-centered care (PCC) concept evolved over time into a more all-encompable approach to operation. It underlines the significance of customising treatment to fit every patient’s particular requirement as well as patient liberty. The physical, psychological, social, and psychological aspects of treatment are merged in this approach. This helps to create a more compassionate and cooperative link between doctors and patients. The patient-centered approach has evolved into the standard for high-quality treatment in present medicine. It promotes shared decision-making whereby the patient and the practitioner participate in the treatment process and discuss the patient’s choices and ideas.(8) This change is especially supported by the adoption of digital health technologies, which enable improved interaction between patients and clinicians and more tailored treatment. As the need for more individualised treatment rises, patient-centered approaches are being applied in healthcare systems all around to try to enhance both the quality of treatment and patient pleasure.
Role of Education in Healthcare Systems
Making healthcare systems run better and ensuring that healthcare professionals with the knowledge, tools, and attitudes required to provide quality of treatment depend mostly on education. Education in the context of healthcare refers to imparting knowledge to professionals at all levels from medical students to seasoned physicians. It also involves teaching patients so they could equip themselves to actively participate in their own healthcare. Healthcare education focusses on teaching students both the clinical skills they need to work with patients and the social skills they need to get along with others. Professional training programs and medical schools stress not only technical skills but also conversation, understanding, and cultural awareness.(9) By teaching healthcare workers about these topics, they can build strong, trusted connections with patients, which is an important part of patient-centered care. Professional growth also makes sure that healthcare professionals stay up to date on new medical advances, evidence-based methods, and new tools, which lets them provide the best care possible. For the patient, learning is just as important. People can make choices that are in line with their values when they are better informed about their health problems, treatment options, and the healthcare system. Educating patients makes their whole healthcare experience better by getting them more involved, happier, and more likely to stick to their treatment plans. It is especially important when dealing with chronic diseases, where making smart decisions and taking care of oneself are important parts of good care.
Previous Studies on Healthcare Education and Patient Care
Previous research on healthcare education and how it affects patient care has shown how important it is for both professionals and patients to learn more about how to get better healthcare. Research has shown over and over that healthcare professionals who are well-trained are more likely to use patient-centered practices, which improves patient happiness and health results. A big part of many studies is looking at how healthcare education can help make care more equal.(10) Researchers have found that healthcare professionals who are trained in cultural competence and patient-centered communication are better able to treat patients from a range of backgrounds in a way that supports their differences. This makes healthcare fairer for everyone. These studies show that doctors who are taught to understand and meet the unique cultural, social, and psychological needs of their patients have a lot happier patients. On the patient side, studies have shown that education is key to better health knowledge, treatment retention, and results. Patients can take an active part in their care when they are informed about their illnesses and the treatment choices that are open to them. For example, research on managing chronic diseases has shown that people who are well-informed are more likely to follow their treatment plans and make healthy living choices. This leads to better disease control and quality of life. The literature review is summed up in table 1, which shows linked work, important results, obstacles, and the study’s focus.
|
Table 1. Summary of Literature Review |
|||
|
Aspect |
Key Findings |
Challenges |
Scope |
|
Impact of Healthcare Education on Provider-Patient Communication |
Improved communication leads to better patient outcomes. |
Institutional resistance to new educational models. |
Healthcare communication improvement and training. |
|
Role of Patient Education in Chronic Disease Management |
Patient education enhances self-management and treatment adherence. |
Limited resources and access to technology in underserved areas. |
Chronic disease management and long-term care planning. |
|
AI in Healthcare Provider Education (11) |
AI improves personalization and accessibility in education. |
AI implementation requires data security and integration challenges. |
Widespread adoption of AI in healthcare education. |
|
Patient-Centered Care and Patient Satisfaction |
PCC increases patient satisfaction and trust in providers. |
Cultural differences can hinder the implementation of PCC. |
Enhancing healthcare delivery through patient-centered approaches. |
|
Technology-Enhanced Education for Healthcare Providers |
Tech-based education increases provider engagement and skill retention. |
Limited internet access in rural areas for digital learning. |
Leveraging technology for continuous professional development. |
|
Role of Digital Health Tools in Patient Education |
Digital health tools offer continuous education for patients. |
Patients may not engage with digital health tools regularly. |
Expanding access to patient education through mobile health platforms. |
|
Culturally Competent Education in Healthcare |
Culturally competent education improves patient trust and care. |
Lack of culturally competent educational materials. |
Improving patient trust and care outcomes in multicultural settings. |
|
Healthcare Education and Health Literacy |
Improved health literacy leads to better care decision-making. |
Low health literacy among diverse populations. |
Promoting health literacy as a cornerstone of effective care. |
|
Simulation-Based Education for Healthcare Providers |
Simulation improves practical skills and decision-making abilities. |
High cost and time commitment for simulation-based learning. |
Enhancing clinical decision-making through simulation. |
|
Telemedicine and Education in Rural Healthcare |
Telemedicine helps overcome geographic barriers to education. |
Rural healthcare providers lack access to telemedicine infrastructure. |
Improving healthcare access in remote and underserved areas. |
|
Collaborative Education Models for Healthcare Teams |
Collaboration improves team communication and patient outcomes. |
Collaboration barriers due to organizational silos. |
Building cohesive healthcare teams for better patient outcomes. |
|
Patient Education and Medication Adherence (12) |
Patient education directly improves medication adherence. |
Patient reluctance to change medication adherence habits. |
Improving treatment adherence and patient compliance with education. |
|
Use of Virtual Reality in Healthcare Training |
Virtual reality enhances clinical skills and patient interaction. |
High cost and accessibility issues with VR education tools. |
Innovating clinical training and patient interaction through VR. |
|
Global Health Education and Equity |
Education can reduce health disparities globally. |
Global inequities in healthcare education access. |
Expanding global healthcare education access to reduce disparities. |
Healthcare education models
Traditional Healthcare Education
Medical education has been based on traditional healthcare education for a long time, with a main focus on teaching scientific information and practice skills. Structured classroom-based teaching is usually part of this model, along with hands-on training in hospital settings. Basic ideas and methods are taught to students in medical schools, nursing programs, and related health classes through talks, texts, and hands-on examples. Clinical rotations and jobs give students real-world experience where they can use what they’ve learnt while being supervised by workers with more experience. In standard healthcare education, the teacher guides the students through the process and puts a lot of stress on memorising medical facts, diagnosis methods, and treatment plans. This method has worked well for helping healthcare workers build a strong body of information and expert skills. However, it doesn’t always put enough focus on developing human skills like conversation, empathy, and cultural competence, which are very important for patient-centered care. Traditional schooling has given doctors a good background in medicine, but it is becoming clearer that it is not enough to prepare them for the complicated nature of current patient care.(13) Focussing on technical skills and professional information can leave gaps in areas such as communicating with patients, making decisions together, and working together as a team with people from different fields. Also, the strict structure of standard healthcare education can make it take a while to react to changes in care methods, medical research, and technology. Because of this, many schools have started using new methods to better meet the changing needs of healthcare systems.
Modern Approaches in Healthcare Education
Modern approaches of instruction show the continuous shift towards more flexible and patient-centered care paradigms. These approaches adopt a more whole, comprehensive view of patient care than only stressing fundamental skills and medical knowledge. Important components of contemporary healthcare education are critical thinking, problem-solving, and “soft skills” like discussion, understanding, and cultural competency. Patient-centered treatment demands these abilities. Current healthcare education emphasises the need of learning from several spheres together. Trained together in this approach, students from several healthcare fields including nursing, medicine, pharmacy, and social work are encouraged to collaborate cooperatively as a team. This education combining several disciplines helps to remove obstacles in the healthcare system, therefore promoting a more homogeneous approach of patient treatment. Learning how to coexist peacefully with people from all backgrounds helps students enhance collaboration and the general degree of patient care. Modern healthcare education also stresses evidence-based practice and constant acquiring new skills a lot. The world of healthcare is changing quickly these days.(14) Medical information and tools are also changing quickly. Healthcare workers need to keep up with the newest studies and innovations. Continuous professional development is a part of modern educational methods that encourages healthcare professionals to keep learning throughout their jobs. Modern healthcare education also puts more stress on the social drivers of health.(15) This is because it is understood that patient care includes more than just professional exchanges and includes things like education, income, and access to resources. This all-around method makes sure that healthcare workers can better understand the bigger picture of a patient’s health and provide care that is truly patient-centered.
Digital and Remote Learning Platforms
The rise of online and digital learning tools has changed the way healthcare is taught, giving students and workers new ways to learn and improve their skills. These systems make learning flexible and easy to access by using online tools, virtual models, and live material. Digital learning is especially helpful in healthcare education because it can meet the needs of students, workers, and patients, giving them access to educational material at any time and in any place, even if they are far away. One great thing about internet healthcare education is that you can learn at your own pace. Students can use educational tools, films, and exercises to learn at their own pace, going over ideas again if they need to or moving on faster to areas where they already know a lot. For medical professionals juggling their nursing responsibilities with ongoing education, this is quite beneficial. Another aspect of remote learning technologies that has grown to be crucial for contemporary healthcare education is training through simulations. Virtual patient scenarios, for instance, help students train in a controlled, safe environment making professional judgements, diagnosis of issues, and treatment planning. From basic check-ups to complex medical issues, these models can act out a great range of events. This makes pupils more ready for life and confident. Furthermore facilitating global collaboration among healthcare professionals and students is digital tools. People from many healthcare systems and places may more easily exchange their expertise and experiences via online classes, discussion forums, and seminars. Particularly in healthcare environments and cultures that differ from one another, this global perspective is quite beneficial in helping one to see patient care in its whole. For continuous education and professional development as well, platforms for digital and online learning have grown to be quite vital.
Challenges in implementing healthcare education
Institutional Barriers
Imposing efficient healthcare education on occasion effects in most important structural problems that would preclude the provision of, patient-targeted remedy. Among these issues are insufficient cash, terrible centers, and healthcare institutions unwilling of alternate. Many scientific institutions have rules and tactics firmly anchored in conventional strategies of remedy. Enforcing new coaching strategies that centre on patient freedom and involvement will become hard as end result. The primary structural impediment is the insufficient financing for healthcare training. Many healthcare structures have confined budget, for this reason they cannot have enough money to perform packages to train patients, offer academic substances, or train their employees. Healthcare vendors might also as a result lack the time or price range to organise patient-targeted training tasks or to keep their personal getting to know. Moreover, many times they have got too many each day responsibilities, which leaves little time to educate patients or set up connections with them that would empower them. Any other troubles are institutions that resist change. Healthcare institutions won’t include new teaching techniques if they consider the brand new processes are too tough to comprehend or in the event that they doubt their applicability or if they wish to alter established approaches. In regions where sufferers have no longer had a whole lot impact in selections and treatment has been administered in a regimented way for a long term, this resistance can be in particular powerful. Leaders devoted to constructing a lifestyle of learning and patient-targeted care as well as laws supporting healthcare experts and patients to maintain their schooling and education will assist us to conquer bureaucratic resistance.
Technological Limitations
Among the main issues arising when healthcare education is implemented are access, usability, and the capacity to effectively mix new technology into healthcare systems. While digital platforms and online technologies might totally alter the way healthcare is taught, not all healthcare systems are equipped to apply them efficiently. If individuals cannot access decent digital infrastructure, particularly in areas with little resources, digital healthcare education may not be extensively used. People’s access to technology varies greatly depending on where they live—in cities or in rural areas. Many remote or impoverished healthcare facilities as well as patients lack the necessary devices to employ online learning tools or consistent internet connectivity. This digital divide aggravates health inequalities as individuals in these areas would not have as many opportunities to participate in training courses that could enable them learn more about their health and enhance their outcomes. Furthermore, healthcare professionals in these regions might not have access to the newest digital tools for continuous education, which would make it more difficult for them to follow developments in medicine. Furthermore difficult to apply technology in healthcare education is insufficient technical expertise and training. Healthcare workers may find it difficult to become acquainted to new digital technologies if they are not well qualified on their use. This can lead to ineffective use of technology and neglect of the full advantages it can provide. Moreover, developing excellent digital learning resources grounded on research requires a lot of time, knowledge, and resources all of which might not be accessible in every healthcare environment.
Socioeconomic and Cultural Barriers
Adopting healthcare education is challenging because of socioeconomic and cultural barriers. These obstacles influence the patients who can gain from the education as well as the medical professionals who impart knowledge. Different healthcare education resulting from these issues makes it more difficult for some populations to get patient-centered treatment and properly take care of their health. Among the main social issues are not being able to attend classes. Lower-income patients may find it difficult to obtain healthcare education either they cannot pay it, cannot get there, or cannot quickly access online resources. Figure 2 highlights how cultural and economic situation create obstacles, so influencing patient care and healthcare access.
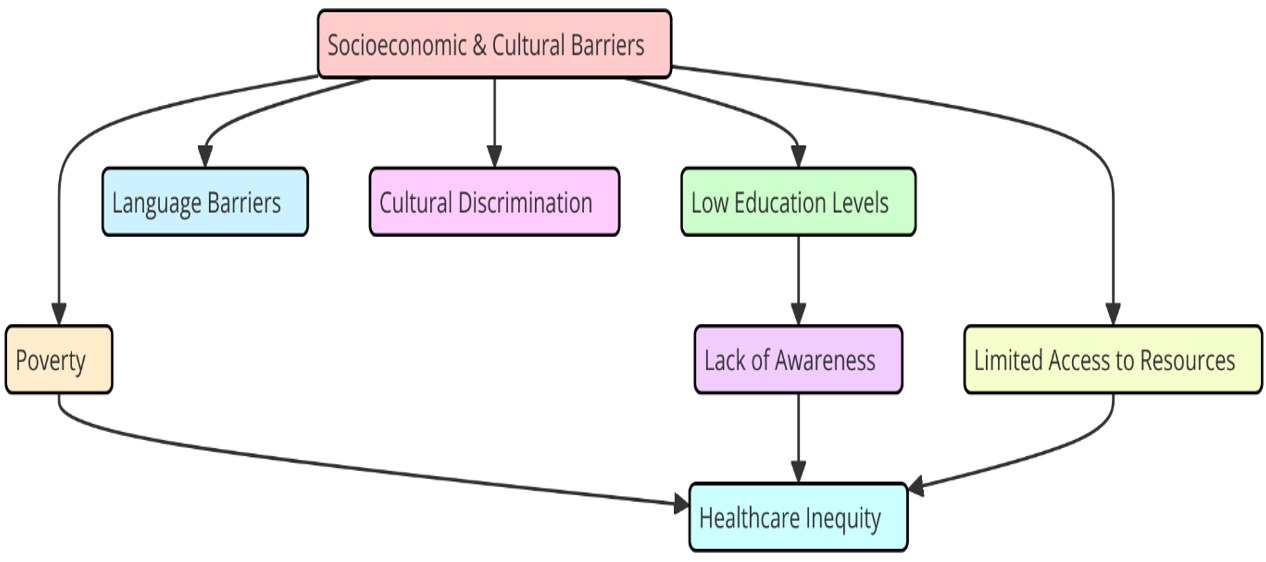
Figure 2. Illustrating Socioeconomic and Cultural Barriers
People who are impoverished, for example, may find it difficult to afford laptops, tablets, or internet connection all of which are typical needs for participating in online training courses. These obstacles prevent access to vital health information, therefore sustaining health inequities and producing negative outcomes in terms of health. People from lower socioeconomic levels might possibly not know much about health, which makes it more difficult for them to comprehend and apply knowledge about healthcare. Patients who find medical directives, prescription regimens, or treatment choices confusing may find it more difficult to adequately manage their diseases. Under these circumstances, healthcare education has to be simple to grasp, accessible, and sensitive to many cultures so that it stays with the people it is meant for.
Furthermore greatly influencing the effectiveness of healthcare education are cultural-based obstacles. Patients from many backgrounds could see health, sickness, and treatment differently. These variations in culture can influence people’s interpretation and use of medical information. Certain ethnic groups could have traditional beliefs that contradict what doctors advice is best for them or they might be less likely to trust Western treatment. Healthcare providers should be culturally sensitive and consider these variations when they educate so that the material respects the opinions and practices of the patients.
Patient-centric care frameworks
Definition and Core Principles of Patient-Centric Care
PCC, often known as patient-centered care, is a method of delivering treatment in which the individual patient’s needs, preferences, and beliefs firstly. This paradigm seeks to shift the conventional top-down approach to healthcare—in which doctors are considered as the only ones who can make decisions—to one in which people and healthcare professionals collaborate more. PCC emphasises that patients should participate in all aspect of their healthcare so that their opinions may be heard in all treatment plans and choices. Main concepts of patient-centered care are respect for the patient’s decisions, mental support, family and friend engagement, clear communication, and coordination of treatment. PCC heavily relies on shared decision-making. This helps results and reduces dispersed care. Furthermore well-known in patient-centered care is the need of providing knowledge to individuals in a method they can grasp and quickly access. This ensures that individuals participate in their own treatment and may make decisions grounded on correct knowledge. PCC’s primary objective is to improve health outcomes by creating adaptive healthcare settings fit for every patient’s requirements and preferences.
Integrating Education with Patient-Centric Models
Including education into patient-centered care strategies is absolutely crucial so that patients possess the knowledge, tools, and confidence required to make decisions regarding their health. Patient-centered care emphasises education as it enables patients to participate in their own treatment, therefore enhancing their health outcomes, engagement, and dedication. Doctors in a patient-centered care system have to teach patients about their illnesses, treatment choices, and possible outcomes in addition to treating their physical components. Through this education, patients may learn about their illness, the advantages and drawbacks of various therapies, and the best strategies for managing their health. When patients receive easily comprehensible information, they are more suited to make decisions in keeping with their beliefs and interests. Including education into patient care also helps healthcare professionals and patients trust each other and communicate better. The therapeutic connection improves when clinicians show their patients that they are ready to cooperate by spending time teaching them and consulting with them regarding their treatment plans. This link is rather crucial for patient-centered care to be successful as shared decision-making is fundamental in the healing process. Patients should also be taught how to take care of themselves should they have chronic conditions requiring continuous attention. By educating patients how to monitor and manage their condition, providers allow them to keep in better control of their health and reduce their risk of complications. This knowledge is very important because it gives people the power to make changes to their lifestyles, take their medications as prescribed, and spot early signs of possible health problems.
Benefits of Combining Education with Care Models
Putting together healthcare education and patient-centered care methods has many benefits, such as making patients happier, improving their health, lowering costs, and making care delivery more efficient. Adding education to care models improves both the level of care and the patient’s experience with the healthcare system as a whole. One of the main perks is that patients are more involved. When patients learn about their symptoms, treatment options, and the probable hazards and advantages of various techniques, they participate actively in their own care. This advice not only guides individuals towards better judgements but also increases their inclination to follow their treatment regimens. Studies have indicated that those who understand their treatment plan and can explain why they are following it are more likely to make the necessary changes to their life. This can therefore help to reduce the need for travels back to the hospital or emergency treatment and enhance health outcomes. Teaching with patient-centered treatment helps patients and healthcare professionals communicate more easily as well. When patients are informed, they are more likely to feel secure reporting problems, posing questions, and offering comments on their treatment. Working jointly guarantees that treatment strategies are grounded in the beliefs and wants of the patient. This helps the patient to be happier and fosters confidence in the medical system. Reducing health inequalities also depends on teaching individuals and putting their needs first in treatment. By providing the knowledge and resources people need to make wise decisions about their health, healthcare institutions can empower persons from all walks of life. This is true independent of their income level or resources availability. Those who are better knowledgeable about preventative care are more inclined to use it, therefore enhancing their long-term health and reducing the healthcare costs.
Strategic implementation of education in patient-centric frameworks
Educational Strategies for Healthcare Providers
Good training programs are therefore crucial so that healthcare professionals may deliver patient-centered care and make decisions alongside their patients. These techniques are aimed to enhance social and professional abilities, therefore promoting a whole-person approach to patient care that considers every individual’s social, psychological, and physical requirements. One of the most crucial approaches to raise the quality of education is applying instruction from many domains concurrently. Working with experts from several disciplines—including nursing, medicine, social work, and mental health—helps healthcare personnel learn more about how to treat patients. This approach guarantees that every aspect of a patient’s treatment is considered and managed properly, therefore supporting unity and collaboration. Teaching healthcare professionals how to interact effectively and grasp several cultures is also quite important. Key component of patient-centered care is trust, so providing healthcare providers with the tools they need to interact with patients in a fair, caring, and clear manner improves the relationships and helps develop trust. One of another crucial teaching strategies should be given to providers evidence-based approaches. Ensuring that medical personnel are aware of the most recent studies and best practices will enable them to provide scientifically sound and patient-oriented treatment. People should thus be reminded of the need of making decisions jointly, allow patients make their own decisions, and consider each person’s beliefs and likes while designing their treatment. People should also learn more about patient-centered approaches. Simulation-based learning is another excellent approach to educate medical practitioners. Safe means for professionals to rehearse making healthcare decisions and communicating with patients are virtual models, role-playing, and case studies. These activities enable doctors to become more adept in applying their knowledge in practical settings, therefore preparing them for interactions with challenging patients.
Patient Education Techniques and Best Practices
Giving patients the ability to participate in their own treatment depends on techniques for teaching them, which also affect their level of enjoyment and outcome of better health. Effective patient education mostly depends on providing individuals with clear, easily available, and practical knowledge that guides their wise decisions about their health. Many strategies and best practices may be applied to let individuals completely grasp their diseases, their course of treatment, and what they can do to get better. One useful tip is to employ basic vocabulary. Since many individuals find medical jargon difficult to grasp and frightening, physicians and nurses should especially make great care to adopt straightforward, uncomplicated language when discussing diseases and treatment courses.
Collaboration Between Educators, Healthcare Providers, and Patients
Patient-centered care programs cannot be successful without cooperation among educators, medical professionals, and patients. Working together, these organisations can ensure that individuals have the skills they need to be active participants in their own healthcare, therefore ensuring their education, involvement, and development. Working together helps reduce the gap between what physicians know and what patients need, therefore producing more individualised and successful treatment. Working together involves not only healthcare professionals but also teachers in the process of patient education. Teaching individuals about their issues, treatment options, and self-care practices depends much on educators—just as in medical education and health coaching. Working with healthcare experts allows teachers to ensure that the knowledge individuals acquire is accurate, practical, and particular to their requirements. Following the information that patients provide, healthcare professionals may then ensure that it is constantly shared and understood during therapy. Participating in their own education helps patients take more ownership for their health. Priority one in cooperative education should be shared decision-making whereby patients actively participate in discussions concerning their diagnosis, treatment options, and care plans. This guarantees that decisions on treatment align with the objectives, values, and interests of the patient. Involvement in the learning process helps patients to take good care of their health and follow treatment regimens. Doctors, patients, trainers, and other professionals should also be constantly able to provide and receive remarks along with working together. When healthcare professionals and educators promote honest communication, patients may ask questions, voice concerns, and offer comments on their educational requirements. This enables their shift in behaviour. This evolving method ensures that instruction remains relevant and current for patients all during their treatment.
Future directions
Policy and Institutional Recommendations
Several policy and administrative suggestions should be thought about in order to make the best use of healthcare education within patient-centered care systems. These suggestions are meant to get rid of current problems, improve the way healthcare education is given, and encourage the use of patient-centered methods at all levels of care. One very important suggestion is to make rules that make it a priority for healthcare workers to learn about patient-centered care concepts. Medical, nursing, and related health schools should teach students how to communicate, understand other cultures, and make decisions together. This approach guarantees that medical professionals engage with patients in a way that respects, values, and satisfies their needs. To inspire practitioners to never stop learning, healthcare institutions should also provide continuous training in patient education, communication, and collaborative care models. Policies supporting the application of these training approaches would help to produce a healthcare workforce fit for the demands of modern, patient-centered care. Ensuring appropriate funds and instruments for patient education initiatives is another crucial policy recommendation. Digital tools, instructional materials, and technology that simplify patient instruction in a manner that is both high-quality and easily accessible should be investments made by healthcare organisations in these areas. This implies ensuring that tools fit persons with various degrees of literacy, languages, and cultural backgrounds and are available in a spectrum of formats, including written, oral, and visual resources. Healthcare systems should also pay for the creation and upkeep of telehealth platforms, which can help patient education programs reach and help more people, especially in rural or underdeveloped areas.
Potential for Global Health Systems
Putting healthcare education into patient-centered care models has a lot of potential to make global health systems better, especially as systems around the world try to provide more efficient, fair, and personalised care. The focus on patient-centered care is growing, and digital tools, AI, and mobile health technologies are improving quickly. This offers an opportunity to transform healthcare education worldwide, therefore improving health results, happier patients, and better use of healthcare resources. Particularly in LMICs (low- and middle-income countries), patient-centered education is one wonderful thing as it may help equal out health variations. Educated patients are more likely to engage in behaviours that benefit their health, like following their prescriptions, attending visits, and visiting a doctor as advised when they should. Healthcare systems may reduce the number of diseases that can be prevented, improve the general health of the society, and finally save money on healthcare expenses by teaching individuals how to take care of their own health. Including global health education into medical systems may also let individuals from many nations exchange best practices, research, and fresh ideas? Teaching patients and healthcare professionals globally together will improve the quality of treatment and help to unite the worldwide health system.
RESULT AND DISCUSSION
Putting healthcare education into models for patient-centered care has shown a lot of promise for making things better for patients. Healthcare professionals who are educated can communicate better, understand different cultures better, and include patients in decision-making processes. Similarly, educating patients gives them more power, makes them more likely to stick to their treatment plans, and makes it easier for them to take care of their own chronic illnesses. The spread of healthcare education has grown thanks to AI-powered tools and digital platforms that make learning more available and personalised. Patient-centered education is still not fully used, though, because of problems like limited technology, governmental pushback, and financial hurdles. To get the most out of healthcare education and how it affects patient care, it is important to deal with these problems by strategically investing in resources, training, and technology.
The Healthcare Provider Performance Evaluation, which can be seen in Table 2, shows that after education, healthcare providers did much better in a number of areas. Communication Skills got better, going from a score of 3,5 to 4,5, which is a big change. In Figure 3, measurement factors were compared before and after schooling. This shows that patient care results got better.
This shows that healthcare education is very important for making it easier for providers to talk to patients in a clear way. Better communication builds trust and strong ties between patients and providers, both of which are necessary for patient-centered care. Cultural Competence went from a 3 to a 4,4, which is another important area that got better. This shows that healthcare education makes it a lot easier for workers to understand and accept people from different cultures. This means that patients from different cultures get better, more personalised care. Understanding cultural differences better makes patients happier and lowers the chance of mistakes. Shared Decision-Making went up from 3,2 to 4,3, which suggests that doctors who get more training are better able to include patients in choices about their care. Trends in rating factors are shown in Figure 4, which shows that things got better before and after schooling was put in place.
|
Table 2. Healthcare Provider Performance Evaluation |
||
|
Evaluation Parameters |
Before Education |
After Education |
|
Communication Skills |
3,5 |
4,5 |
|
Cultural Competence |
3 |
4,4 |
|
Shared Decision-Making |
3,2 |
4,3 |
|
Patient Engagement |
3,4 |
4,6 |
|
Clinical Knowledge |
3,7 |
4,8 |
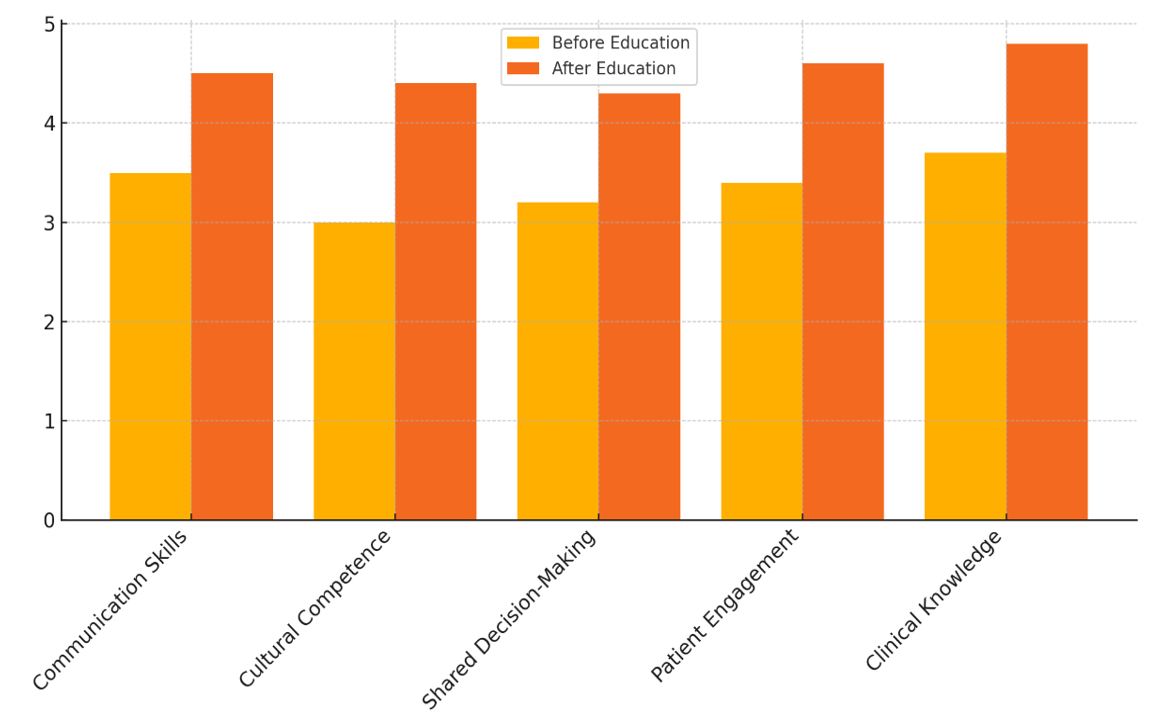
Figure 3. Comparison of Evaluation Parameters Before and After Education
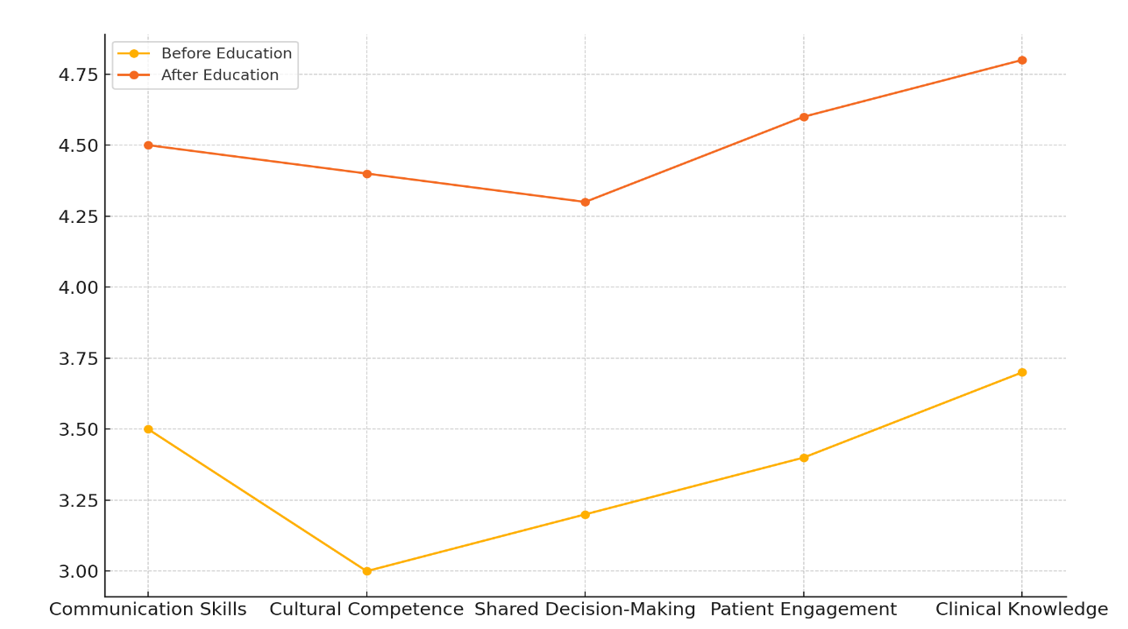
Figure 4. Trends in Evaluation Parameters Before and After Education
This teamwork not only makes patients happier, but it also helps them stick to their treatment plans and improves their general health.
|
Table 3. Patient Outcomes Evaluation |
||
|
Evaluation Parameters |
Before Education ( %) |
After Education ( %) |
|
Medication Adherence |
60 |
85 |
|
Self-Management Skills |
55 |
80 |
|
Patient Satisfaction |
70 |
90 |
|
Health Literacy |
65 |
88 |
|
Treatment Adherence |
75 |
95 |
The Patient results Evaluation, which can be seen in Table 3, shows that schooling has a good effect on patient results. Figure 5 shows how the different factors added up to make the overall change in patient results.
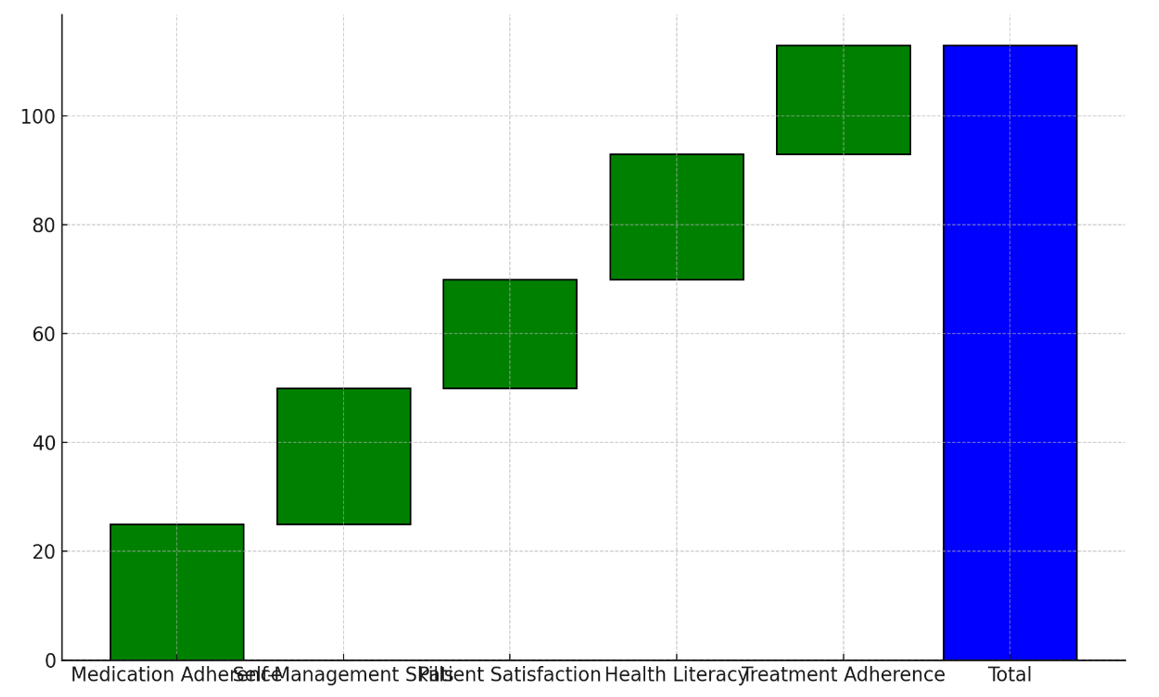
Figure 5. Cumulative Contribution to Total Improvement in Patient Outcomes
The number of people who took their medications as recommended went from 60 % to 85 %, showing that patients are more likely to follow their treatment plans when they are told about their conditions and how important it is to do so. This change is very important for keeping chronic conditions under control and avoiding problems. Figure 6 shows the differences in patient measures between before and after the teaching program. It shows that results got a lot better.
Self-Management Skills went up from 55 % to 80 %, which shows that schooling gives people the power to take charge of their own health. Patients who are educated can better keep an eye on their symptoms, make changes to their lifestyle, and understand how their daily habits affect their situation, all of which can lead to better health results. Patients are more likely to have good experiences with their healthcare workers when they are taught about their health. This is shown by the fact that customer satisfaction went from 70 % to 90 %. Patients who know more about the process are also more likely to feel accepted and valued when decisions are being made. Health Literacy went up from 65 % to 88 %, which shows that healthcare education helps people understand medical information better, which lets them make better decisions about their care.
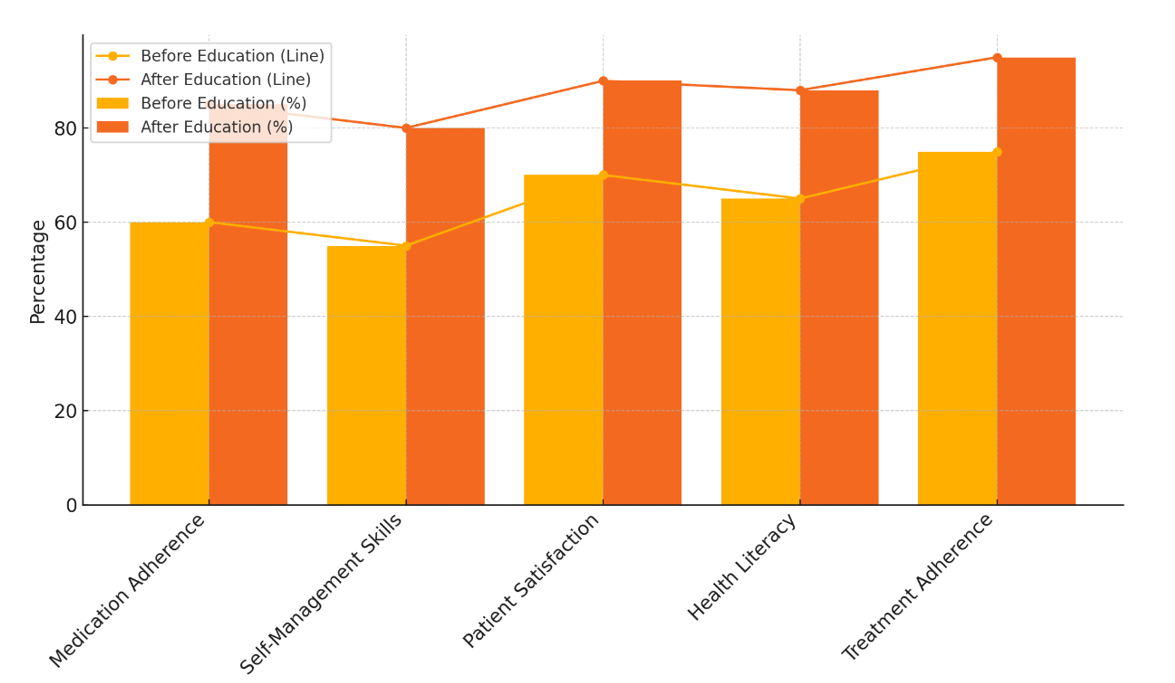
Figure 6. Comparison of Patient Metrics before and After Education Program
CONCLUSION
Patient-centered care frameworks put the wants, desires, and beliefs of each patient first, and healthcare education is a key part of promoting these frameworks. Education improves the quality and timeliness of healthcare service by giving healthcare professionals the skills and information they need to speak clearly, provide care that is sensitive to different cultures, and include patients in decision-making. Also, educating patients gives them the power to be involved in their own health, which makes them more likely to follow their treatment plans and encourages them to take preventative care actions Using AI and digital platforms in healthcare education opens up exciting new ways to customize and expand learning materials, which will make healthcare knowledge easier for a wider range of patients, including those who live in rural or underserved areas. But healthcare education can only reach its full potential if structural problems like limited resources, resistance to change, and technology limits are fixed. Healthcare systems need to put money into infrastructure, training, and working together across disciplines to make sure that both patients and healthcare workers get the information they need for good, patient-centered care. Also, encouraging people from all over the world to work together and share their best ideas can help solve problems like health gaps, making education more fair and better health results around the world. Healthcare systems can improve care management, patient happiness, and long-term health results by educating both doctors and patients more about healthcare. This can also lower costs and encourage more environmentally friendly healthcare practices. To sum up, healthcare education is an important part of patient-centered care, and it needs to be a part of healthcare systems if we want to improve patient results and make healthcare more flexible and patient-focused.
REFERENCES
1. Mosadeghrad AM. Factors influencing healthcare service quality. Int J Health Policy Manag. 2014;3:77.
2. Pheng LS, Rui Z. Facilities management and Singapore’s healthcare system. In: Service quality for facilities management in hospitals. Singapore: Springer; 2016. p. 9–23.
3. Saedi S, Kundakcioglu OE, Henry AC. Mitigating the impact of drug shortages for a healthcare facility: An inventory management approach. Eur J Oper Res. 2016;251:107–23.
4. Maestre JM, Fernández MI, Jurado I. An application of economic model predictive control to inventory management in hospitals. Control Eng Pract. 2018;71:120–8.
5. Paul T. Investment experience & state of mind – A case study of mutual fund investors. Int J Res Dev Manag Rev. 2015;4(4):56–60.
6. Padhi B, Panda AK. A study on employee engagement models for sustainability of organization. Int J Res Dev Manag Rev. 2015;4(4):79–85.
7. Lavy S, Shohet IM. A strategic integrated healthcare facility management model. Int J Strateg Prop Manag. 2007;11:125–42.
8. Wang Y, Kung L, Byrd TA. Big data analytics: Understanding its capabilities and potential benefits for healthcare organizations. Technol Forecast Soc Change. 2018;126:3–13.
9. Wang Z, Bulbul T, Lucas J. A case study of BIM-based model adaptation for healthcare facility management—Information needs analysis. In: Computing in civil engineering. Reston, VA, USA: American Society of Civil Engineers; 2015. p. 395–402.
10. Yousefli Z, Nasiri F, Moselhi O. Maintenance workflow management in hospitals: An automated multi-agent facility management system. J Build Eng. 2020;32:101431.
11. Allen EP, Muhwezi WW, Henriksson DK, Mbonye AK. Health facility management and access: A qualitative analysis of challenges to seeking healthcare for children under five in Uganda. Health Policy Plan. 2017;32:934–42.
12. Normalization C. EN 15221-1: European standard in facility management–Part 1: Terms and definitions. Brussels, Belgium: CEN; 2006.
13. Chen IJ, Paulraj A. Towards a theory of supply chain management: The constructs and measurements. J Oper Manag. 2004;22:119–50.
14. Kannan VR, Tan KC. Just in time, total quality management, and supply chain management: Understanding their linkages and impact on business performance. Omega. 2005;33:153–62.
15. Meijboom B, Schmidt-Bakx S, Westert G. Supply chain management practices for improving patient-oriented care. Supply Chain Manag. 2011;16:166–75.
FINANCING
The authors did not receive financing for the development of this research.
CONFLICT OF INTEREST
The authors declare that there is no conflict of interest.
AUTHORSHIP CONTRIBUTION
Conceptualization: Wakeel Ahmed, Shailly Gupta, Bhupal Pujari, Rajashree Panigrahi.
Research: Wakeel Ahmed, Shailly Gupta, Bhupal Pujari, Rajashree Panigrahi.
Writing - original draft: Wakeel Ahmed, Shailly Gupta, Bhupal Pujari, Rajashree Panigrahi.
Writing - proofreading and editing: Wakeel Ahmed, Shailly Gupta, Bhupal Pujari, Rajashree Panigrahi.