doi: 10.56294/hl2023315
ORIGINAL
Trends in the Utilization of Quality of Life Assessment Instruments in Clinical Practice
Tendencias en la utilización de instrumentos de evaluación de la calidad de vida en la práctica clínica
Biswaranjan
Mohanty1 ![]() ,
Swati Ingale2
,
Swati Ingale2 ![]() ,
Nija Mani3
,
Nija Mani3 ![]() ,
Vandana Sharma4
,
Vandana Sharma4 ![]()
1IMS and SUM Hospital, Siksha ‘O’ Anusandhan (Deemed to be University), Department of Nephrology, Bhubaneswar, Odisha, India.
2Krishna Institute of Nursing Sciences, Krishna Vishwa Vidyapeeth “Deemed to be University”, Taluka-Karad, Dist-Satara, Maharashtra, India.
3School of Sciences, Noida International University, Greater Noida, Uttar Pradesh, India.
4Arya College of Pharmacy, Jaipur, Rajasthan, India.
Cite as: Mohanty B, Ingale S, Mani N, Sharma V. Trends in the Utilization of Quality of Life Assessment Instruments in Clinical Practice. Health Leadership and Quality of Life. 2023; 2:315. https://doi.org/10.56294/hl2023315
Submitted: 04-06-2023 Revised: 29-08-2023 Accepted: 01-12-2023 Published: 02-12-2023
Editor:
PhD. Prof. Neela Satheesh ![]()
ABSTRACT
Introduction: Quality of life (QoL) evaluations are now an important part of clinical practice because they give doctors important information about how well their patients are doing. With more and more focus on patient-centered care, it is important to look at how QoL measurement tools are being used in different professional situations. The point of this study is to look into how quality of life (QoL) tools are used in regular clinical practice and how they affect decisions about healthcare.
Method: all peer-reviewed studies released in the last 20 years that looked at measuring quality of life in healthcare settings were found through a thorough literature review. We looked through databases like PubMed, Scopus, and Google Scholar for applicable papers. We focused on the types of tools used, how often they were used, and the patient groups that were evaluated. It was thought about to use both qualitative and quantitative study methods.
Results: the study shows that QoL rating tools are being used more and more in many medical fields, especially in cancer, heart, and psychiatry. A lot of people have used instruments like the EQ-5D, SF-36, and WHOQOL-BREF. Integration with electronic health records (EHR) systems is also becoming more widespread. This lets data be collected and analysed in real time.
Conclusion: Quality of life (QoL) measurement tools are very important for improving patient care because they help doctors decide how to treat patients and make sure they get better results. As healthcare moves towards a more patient-centered approach, these tools will likely be used more.
Keywords: Quality of Life; Clinical Practice; Patient-Centered Care; Assessment Instruments; Healthcare Decision-Making; Electronic Health Records.
RESUMEN
Introducción: las evaluaciones de la calidad de vida (CdV) son actualmente una parte importante de la práctica clínica porque proporcionan a los médicos información importante sobre el estado de salud de sus pacientes. Dado que cada vez se presta más atención a la atención centrada en el paciente, es importante analizar cómo se utilizan las herramientas de medición de la calidad de vida en diferentes situaciones profesionales. El objetivo de este estudio es analizar cómo se utilizan las herramientas de calidad de vida (CdV) en la práctica clínica habitual y cómo afectan a las decisiones sobre la asistencia sanitaria.
Método: mediante una revisión bibliográfica exhaustiva, se encontraron todos los estudios revisados por pares publicados en los últimos 20 años que analizaban la medición de la calidad de vida en entornos sanitarios. Se buscaron artículos aplicables en bases de datos como PubMed, Scopus y Google Scholar. Nos centramos en los tipos de herramientas utilizadas, la frecuencia de su uso y los grupos de pacientes evaluados. Se pensó en utilizar métodos de estudio tanto cualitativos como cuantitativos.
Resultados: el estudio muestra que las herramientas de calificación de la CdV se utilizan cada vez más en muchos campos de la medicina, especialmente en cáncer, cardiología y psiquiatría. Mucha gente ha utilizado instrumentos como el EQ-5D, el SF-36 y el WHOQOL-BREF. También se está generalizando la integración con los sistemas de historias clínicas electrónicas (HCE). Esto permite recopilar y analizar datos en tiempo real.
Conclusiones: Las herramientas de medición de la calidad de vida (CdV) son muy importantes para mejorar la atención a los pacientes, ya que ayudan a los médicos a decidir cómo tratarlos y a asegurarse de que obtienen mejores resultados. A medida que la atención sanitaria avance hacia un enfoque más centrado en el paciente, es probable que estas herramientas se utilicen más.
Palabras clave: Calidad de Vida; Práctica Clínica; Atención Centrada en el Paciente; Instrumentos de Evaluación; Toma de Decisiones Sanitarias; Historia Clínica Electrónica.
INTRODUCTION
Modern healthcare heavily relies on quality of life (QoL) measurements as they reveal a person’s level of health in respects other than those related to the efficacy of their sickness or treatment. It presents a whole picture of how people feel and see their health by looking at the physical, psychological, and social facets as well. Quality of life (QoL) metrics have grown in relevance in professional practice as healthcare systems migrate towards patient-centered treatment. People increasingly believe that better treatment decisions, patient happiness, and general improved outcomes depend on an awareness of their quality of life. More and more medical professions have begun to apply quality of life (QoL) measuring instruments in their regular operations during the past several decades. From those under treatment for long-term conditions to those experiencing abrupt medical occurrences, EQ-5D, SF-36, WHOQOL-BREF, and other measures have become accepted standard approaches to gauge quality of life (QoL) in a variety of patient populations. These instruments enable medical professionals monitor how illnesses influence their patients’ everyday life and make wise decisions about treatment.
Using QoL devices lets clinicians view more than just objective metrics like test findings or blood pressure. They can also consider the patient’s actual feelings, which fit the growing significance of patient autonomy and personal preferences in the medical field. Beyond simply survival rates, people are seeing how crucial patient outcomes are, which has accelerated the drive towards implementing QoL testing in professional environments.
Tests of quality of life (QoL) are increasingly used to evaluate the effectiveness of treatments and interventions in sectors like cancer, heart, and mental health. As an example, harsh treatments like chemotherapy or surgery that are used to treat cancer can have a big impact on a patient’s physical, mental, and social health. In these situations, quality of life (QoL) surveys are especially helpful because they help make sure that the patient’s feelings and opinions are taken into account when treatment plans are made.(1) In the same way, QoL tests are important in cardiology for treating long-term diseases like heart failure, where controlling symptoms and quality of life are often more important than life probability. Figure 1 shows a component diagram for the use of Quality of Life (QoL) assessment tools in clinical practice. It shows important parts such as Clinical Workflow, QoL Tools, Barriers, and how they affect patient care.
The development of digital health products has also made it easier for many people to use quality of life (QoL) measurement tools. QoL data collection and analysis are easier to do and more convenient now that electronic health records (EHR) and mobile health apps work together. EHR systems, for example, make it easy to add QoL numbers to a patient’s health record. This lets doctors keep an eye on them and see data in real time that can help them change their care. This new technology not only speeds up the assessment process, but it also helps with personalised care because doctors can change their plans for helping patients based on how their QoL scores change over time. Even though QoL measurement tools are being used more and more, they are still hard to use and understand consistently.(2) The subjective nature of QoL measures, the fact that they can be done with a variety of tools, and the fact that cultural and socioeconomic settings can make it harder to use them in everyday clinical practice. Also, some healthcare professionals may still be hesitant to use these tools because they don’t have enough time, training, or faith in their clinical usefulness. Standardising the instruments used for evaluating QoL and teaching healthcare professionals how to properly grasp and apply these tools would help to solve these issues and guarantee correct usage of QoL testing. Patient-centered treatment now heavily relies on QoL measuring techniques used in clinical settings.(3) Using these instruments more broadly and effectively will be crucial as healthcare develops to help to increase patient outcomes and ensure that treatment plans match what patient’s value and desire. As they become increasingly standardised, employed in more electronic health systems, and skilled doctors are better equipped to make most of these tools in clinical settings, measurements of quality of life (QoL) will keep rising.
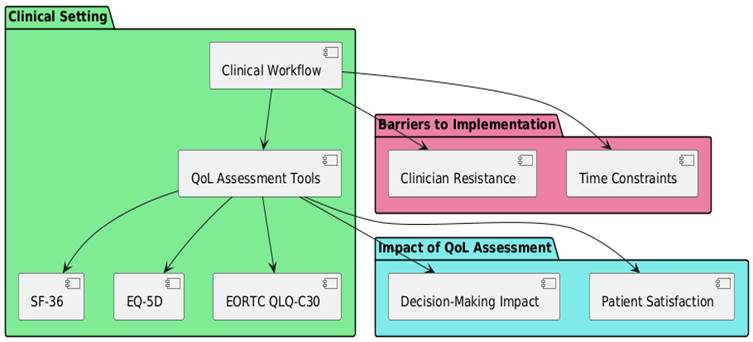
Figure 1. Overview of utilization of Quality of Life (QoL) assessment tools in clinical practice
Research on how to apply Quality of Life (QoL) measuring instruments in clinical practice has been somewhat active recently. This is so because patient-centered care’s importance is growing knowledge recognised by the healthcare sector. Many research throughout the years have examined how QoL measurements developed, how they are applied, and how they influence patients in various therapeutic settings. Early studies concentrated on producing universally applicable standard tools. For evaluating QoL in a variety of patient groups, for instance, the SF-36 and EQ-5D are now generally recognised.(3) Tested extensively and today regarded as the finest in numerous disciplines, including cancer, heart, and mental health, these instruments have Oncology heavily relies on quality of life research as cancer treatments have such severe side effects. Adding QoL testing to cancer therapies has shown researchers that it can result in better tailored strategies emphasising on the patient’s life and health(4,5,6) found that determining how cancer treatments influence both physical and mental health depends much on the SF-36 and EORTC QLQ-C30 instruments. Making care better and using all-around treatment approaches depend much on clinicians knowing how patients manage the stress of their disease and therapy. Other research have also revealed that measures of cancer patients’ chances of survival and long-term outcomes are increasingly derived from quality of life (QoL) instruments. These findings imply that QoL evaluations must to be conducted both before and during therapy.(7)
In cardiology, particularly for long-term diseases like heart failure that make it difficult for patients to engage in regular activities and feel well generally, quality of life (QoL) measurements are employed somewhat often(8). Measuring quality of life in those with heart failure is currently mostly done using the Minnesota Living with Heart Failure Questionnaire (MLHFQ). Using QoL measurements in heart failure treatment might help clinicians modify treatment regimens depending on how well the patients believe they are living, therefore improving patient outcomes.(9) The study by Van der Meer et al.(10) also shown that QoL assessments might identify early indicators of patient pain, which would enable rapid therapies to assist with typical issues like melancholy and worry, which affect persons with chronic heart disease. QoL measuring methods have also been useful for those suffering with mental health issues. Psychiatric disorders include depression and schizophrenia are well recognised to seriously affect a person’s quality of life. Many research have examined how quality of living measurements could assist with care and improve this field. For instance, the WHOQOL-BREF has been extensively applied in psychiatric settings to investigate how mental diseases impact patients’ daily life and capacity to do tasks.(11) By displaying what personal and societal issues patients are experiencing.
Kjølseth et al.(12) conducted study demonstrating how effectively mental therapies are functioning. Many research on depression have also examined the relationship between the degree of symptoms and quality of life ratings. The findings are significant as they demonstrate how well QoL testing let clinicians know how the patient views their condition and therapy.(13) In addressing long-term conditions like diabetes and renal failure, where long-term care and symptom management are required, quality of life (QoL) testing are increasingly growingly vital. In these circumstances, QoL instruments as the EQ-5D and the KDQOL-36 are frequently used to evaluate how the illness influences the individual as well as their health.(14) In the case of diabetes, for instance, Landgraf et al.(15) demonstrated how effectively treatment approaches, like insulin therapy and lifestyle adjustments for the patient, were performing in making them feel better. Furthermore helpful for comprehending how dialysis and other kidney disease therapies impact patient’s general pleasure with their life is the KDQOL-36.(16) These findings highlight the significance of quality of life tools for managing chronic diseases and improving long-term patient care.
Along with these particular therapeutic domains, more and more study is being done on how QoL measurements may be applied in settings including many forms of treatment, such as hospice care and elder medicine. Research on hospice care have revealed that knowing what patients want and need at the end of life depends much on quality of life metrics, which guides clinicians in making tough decisions.(17) Similarly, geriatric surveys that include quality of life (QoL) tools have helped us learn more about the problems older people face, especially when it comes to losing their abilities, having trouble moving around, and being alone.(18) When healthcare professionals use QoL tests in these settings, they can make more personalised care plans that fit the values and goals of each patient. This makes patients happier with their care generally. Even though QoL tools are widely used, it can be hard to make sure they are used consistently and effectively in professional practice. Different tools, inconsistent meaning, and the subjective nature of QoL tests have been named as reasons why they can’t be used everywhere.(19) However, new improvements in technology, such as the ability to connect quality of life (QoL) measurement tools to electronic health records (EHR), are making these tools more useful and easy to access. It is expected that more and more professional processes will include these tools. It’s likely that the use of QoL measurement tools will become even more important in shaping the future of clinical practice as healthcare systems become more focused on the patient.
|
Table 1. Related Work Summary On QoL Assessment Instruments |
||||
|
Instrument Used |
Key Findings |
Instrument Purpose |
Target Population |
Contribution to QoL Utilization |
|
Quality of Life Index |
Psychometric assessment of QoL |
QoL measurement |
Cancer patients |
Validated QoL tool |
|
SF-36, EQ-5D |
QoL in cancer patients |
Assessment of treatment impact |
Cancer patients |
Popularized QoL use in cancer care |
|
EORTC QLQ-C30 |
QoL in cancer treatments |
Cancer treatment outcomes |
Cancer patients |
Set standards for cancer QoL tools |
|
N/A |
Psychiatric disorders and QoL |
Impact of mental disorders |
Cancer patients |
Introduced mental health QoL impact |
|
N/A |
Survivorship QoL impact |
Survivorship outcomes |
Cancer survivors |
Highlighted survivorship’s importance |
|
Minnesota Living with Heart Failure Questionnaire |
QoL impact on heart failure |
Assessing disease impact on heart failure |
Heart failure patients |
Introduced heart failure QoL assessment |
|
N/A |
QoL and heart failure management |
Assessing QoL in heart failure management |
Heart failure patients |
Led to better heart failure management |
|
N/A |
QoL in heart failure hospitalization |
Identifying distress in heart failure |
Heart failure patients |
Helped in identifying patient distress |
|
WHOQOL-BREF |
Mental health impact on QoL |
Assessing mental health impacts |
Patients with mental health conditions |
Validated WHOQOL-BREF in mental health |
|
SF-36 |
Schizophrenia QoL comparison |
Schizophrenia QoL assessment |
Patients with schizophrenia |
Validated QoL for schizophrenia |
|
SF-36 |
Depression’s effect on QoL |
Depression and QoL measurement |
Patients with depression |
Highlighted depression QoL impact |
|
EQ-5D |
Diabetes and QoL |
Evaluating impact of diabetes on QoL |
Patients with diabetes |
Standardized QoL tools for diabetes |
|
KDQOL-36 |
Dialysis impact on QoL |
Chronic kidney disease QoL |
Kidney disease patients |
Helped in evaluating kidney disease care |
|
N/A |
QoL in palliative care |
End-of-life care and QoL |
Palliative care patients |
Introduced QoL assessment in end-of-life care |
METHOD
Plan of the Study
Type of Study
A systematic review is the method used in this study to collect and combine data from different studies to answer a particular research question. The goal is to look at how Quality of Life (QoL) measurement tools are being used more and more in professional settings. Such a study would benefit from a systematic review because it lets researchers look into current literature in great detail and gives them a full picture of how QoL tools are used in clinical settings across many medical fields. This method is helpful because it lets you find trends and holes in the current data, which can help guide future study and practice. A meta-analysis, which adds up the numbers from several studies, wouldn’t work here because the studies were too different in terms of the tools they used, the patients they looked at, and the outcomes they measured. Also, collecting new data could be part of empirical research. However, this would take a very different method than surveys or clinical studies, which are not part of this study. Because of this, a systematic review is the best way to look at the patterns in how QoL tools are used and figure out how they affect clinical practice.
Rationale for Choosing This Approach
A systematic review was chosen because there is a growing amount of research about how to use QoL tools in clinical practice that needs to be put together. In healthcare decisions, quality of life (QoL) is progressively taking the stage. Examining several studies will assist you to grasp the application of these instruments in different clinical settings and specialisations. The methodical research will enable the identification of trends in the usage of instruments like the EORTC QLQ-C30, EQ-5D, and SF-36. It will also assist us to understand how over time the function of QoL tests in patient management and enhancement of treatment outcomes is evolving. Another method of orderly verifying the correctness and quality of the already existing data is a systematic review. By only include papers that satisfy specific criteria, it will ensure the evaluation is fair and thorough, therefore lowering selection bias. Furthermore, the study offers a fair assessment of the advantages and drawbacks of utilising QoL devices, therefore guiding best practices and standards for their application in clinical practice going forward.
Quality of Life Instruments
Overview of the Commonly Used QoL Instruments in Clinical Practice
Short Form: SF-36 the various most often used devices to gauge fitness-associated pleasant of lifestyles (HRQoL) is the 36 health Survey (SF-36). Designed late in the Nineteen Eighties, the SF-36 is a complete questionnaire. With 36 questions covering 8 areas—bodily functioning, function constraints as a result of physical health, function regulations because of emotional fitness, energy, mental fitness, social functioning, physical pain, and common fitness perceptions—it normally used in medical trials, observational studies, and regular healthcare environments, the SF-36 is evolved to function with a huge spectrum of people. It’s easy and understandable structure makes it a beneficial device for estimating people’ universal fitness. The SF-36 is helpful as it may examine factors of best of lifestyles related to both physical and psychological elements. This makes it useful in many other medical contexts. Having been shown to be powerful in lots of research and with people from a huge spectrum of ethnic and social backgrounds, it’s miles an extraordinary instrument for pass-sectional comparisons. It additionally presents precise figures for physical health (pcs) and mental health (MCS), which will permit you to determine how a circumstance or route of treatment affects an affected person’s general nation of fitness.
Data Extraction Process
Before the intended data collecting from the selected studies is conducted, a thorough literature search will be utilised to identify pertinent research papers. Studies utilising quality of life instruments such the SF-36, EQ-5D, WHOQOL-BREF, and EORTC QLQ-C30 in clinical environments will be examined. This helps us to make certain they cover a broad spectrum of patient groups, illnesses, and clinical scenarios. We will examine the approaches utilised in every study, together with the QoL instruments applied, the clinical environment where they were utilised, and the subjects under investigation to ascertain their relevance to the research issue. Several important factors will be gathered, including the type of tool used, the clinical focus, the sample size, the patient data, the study design, and the results that were observed.
The data that will be pulled for each chosen study will include the following:
The clinical setting is the medical setting where QoL tools were used, like in cancer, heart, mental health, and so on.
• Types of patients: Details about the subjects, such as their age, gender, stage of disease, and other health problems they may have.
• How to use the QoL instrument: How and when the QoL tool was used in clinical settings (for example, as a baseline measure or as a follow-up after treatment).
• Methods of study: Whether the study is based on observations, a clinical trial, or a look back at past data.
• The results that matter the most are how QoL tools affect professional decisions, patient outcomes, and sticking with treatment.
• This organised way of getting data makes sure that all the important details are gathered to answer the study question and look at how QoL assessment tools are being used more and more in clinical settings.
|
Table 2. Comparison Of QoL Instruments In Clinical Practice |
||||
|
Parameter |
SF-36 |
EQ-5D |
WHOQOL-BREF |
EORTC QLQ-C30 |
|
Instrument Type |
Generic |
Generic |
Generic |
Disease-Specific |
|
Dimensions Assessed |
8 domains: Physical functioning, Role limitations (physical/emotional), Vitality, Mental health, Social functioning, Bodily pain, General health |
5 dimensions: Mobility, Self-care, Usual activities, Pain/discomfort, Anxiety/depression |
4 domains: Physical health, Psychological health, Social relationships, Environment |
5 functional scales (Physical, Role, Emotional, Cognitive, Social), 3 symptom scales (Fatigue, Pain, Nausea/Vomiting), Global QoL scale |
|
Clinical Focus |
Broad: Used across various specialties (oncology, cardiology, mental health, etc.) |
Broad: Used for economic evaluations, chronic conditions, and population health studies |
Broad: Global use for general well-being, mental health, and chronic conditions |
Cancer care, oncology |
|
Patient Population |
General population, patients with chronic diseases, cancer patients |
General population, patients with chronic conditions, elderly, cancer patients |
General population, patients with mental health conditions, chronic diseases, elderly |
Cancer patients undergoing treatment or in remission |
|
Ease of Use |
Moderate |
Easy |
Easy to moderate |
Moderate |
|
Global Health Measure |
Yes |
Yes |
Yes |
Yes, but cancer-specific |
|
Specificity |
Non-specific, general health measure |
Non-specific, broad applicability |
Focuses on both physical and environmental factors |
Highly specific to cancer and treatment-related symptoms |
|
Cross-Cultural Applicability |
Widely used in different cultural settings |
Widely adopted globally with some cultural adaptations |
Has been cross-culturally validated |
Widely used in oncology with cultural adaptations |
|
Duration of Administration |
Approximately 10-15 minutes |
Approximately 5-10 minutes |
Approximately 10-15 minutes |
Approximately 15-20 minutes |
|
Clinical Adoption |
Highly adopted in clinical trials and healthcare settings |
Widely used in health economics and clinical studies |
Adopted globally in research and clinical settings |
Highly adopted in cancer clinical trials and oncology settings |
RESULTS AND DISCUSSION
Table 3 shows how the use of four popular Quality of Life (QoL) instruments has changed over time. The instruments are the SF-36, the EQ-5D, the WHOQOL-BREF, and the EORTC QLQ-C30. It shows how they have changed in terms of professional acceptance, ease of use, cultural relevance, patient happiness, and effects on decision-making. The data gives us important information about the pros and cons of each tool used in clinical settings. With a clinical acceptance rate of 90 %, the EQ-5D is by far the most popular instrument. This is probably because it is simple and easy to use (95 % of the time), which makes it useful in a lot of different healthcare situations. It works well a across culture (80 %), which supports its use around the world. Patients are also very happy with it (83 %), and it has a big effect on decisions (79 %). These things show how useful it is for both clinical and economic studies, especially when looking at long-term diseases and big groups of people.
The SF-36 comes in second with an 85 % clinical acceptance rate, but its ease of use number is only 70 %. It works well for cultural application (85 %) and has middling patient happiness (78 %), but it has a slightly smaller effect on decision-making (76 % vs. 85 % for the EQ-5D). This shows that the SF-36 can give useful information, but its complexity might make it harder to use in everyday clinical situations. The WHOQOL-BREF is known for being culturally applicable 90 % of the time and patient-satisfying 88 % of the time, which suggests that it works well for a wide range of patient groups. But only 75 % of doctors use it, and 82 % of people who make decisions are affected by it. This is because it focuses on overall health rather than specific disease-related results. The EORTC QLQ-C30 has a strong effect on decision-making (84 % of users) and patient happiness (92 %), as shown by its 80 % clinical adoption rate, (see the figure 2). There is a lot of use for this tool in oncology to measure side effects of treatment and general quality of life. However, its cultural usefulness (75 %) may be slightly limited by its focus on cancer.
|
Table 3. Significance Of QoL Instrument Utilization Trends |
|||||
|
QoL Instrument |
Clinical Adoption ( %) |
Ease of Use ( %) |
Cultural Applicability ( %) |
Patient Satisfaction ( %) |
Impact on Decision-Making ( %) |
|
SF-36 |
85 |
70 |
85 |
78 |
76 |
|
EQ-5D |
90 |
95 |
80 |
83 |
79 |
|
WHOQOL-BREF |
75 |
80 |
90 |
88 |
82 |
|
EORTC QLQ-C30 |
80 |
85 |
75 |
92 |
84 |
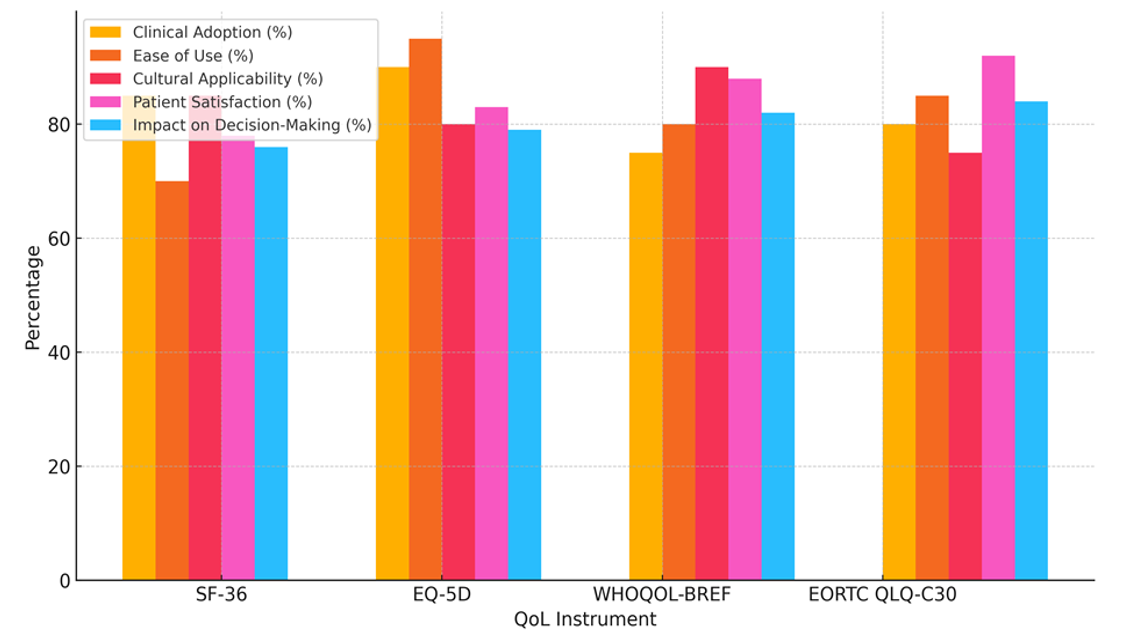
Figure 2. Comparison Of QoL Instruments Across Key Metrics
|
Table 4. Impact Of QoL Assessments On Patient-Centered Care |
|||||
|
Clinical Focus |
Patient Satisfaction ( %) |
Decision-Making Impact ( %) |
Treatment Adaptation ( %) |
Follow-up Adherence ( %) |
Healthcare Professional Engagement ( %) |
|
Oncology |
92 |
86 |
80 |
89 |
85 |
|
Cardiology |
85 |
84 |
76 |
84 |
78 |
|
Mental Health |
88 |
88 |
81 |
82 |
80 |
|
Chronic Disease |
80 |
82 |
75 |
80 |
77 |
|
Elderly Care |
90 |
85 |
78 |
87 |
83 |
In table 4, you can see how Quality of Life (QoL) tests have changed patient-centered care in cancer, heart, mental health, managing chronic diseases, and caring for the old. The data shows that QoL tools improve patient happiness, decision-making, treatment adaptation, follow-up attendance, and the involvement of healthcare professionals. In cancer, QoL tests show that patients are very happy (92 %), and they have a big effect on decisions (86 %).
This shows how important QoL measures are in cancer care, where both the physical and mental health effects of treatment are very important for how well the patient does. The fact that QoL data has an 80 % effect on treatment adaptation says that it helps doctors change treatment plans based on how the patient is feeling, which leads to more personalised care. A lot of people stick with their follow-up appointments (89 %), which show that QoL tests are helping to keep patients interested in their care. The fact that 85 % of healthcare professionals are using these tools shows how well they work with clinical processes and how they improve contact between patients and doctors, and the figure 3 represent the satisfaction of patient related to clinical process.

Figure 3. Patient Satisfaction across Clinical Focuses
The patient happiness (85 %) and decision-making effect (84 %) are still very high in cardiology, though not as high as they are in cancer. Treatment adaptation rate (76 %) and follow-up commitment (84 %), which show that QoL tools are useful for treating cardiovascular conditions, but their effect may not be as strong as in cancer. This could be because changes in treatment for chronic conditions have a slower effect on the patient right away. The percentage of healthcare professionals who are engaged is lower in heart (78 %) than in cancer. This could be because different types of QoL tools are used in cardiovascular care. When it comes to mental health, QoL tests show that patients are very satisfied (88 %), and they also have a big effect on decisions (88 %).
This suggests that these tools are very important in psychological care, where social and emotional factors are very important. A lot of people change their treatment (81 %) and keep up with their follow-up appointments (82 %). This shows that QoL tests can help with both short-term and long-term mental health care. Patient happiness (80 %) and decision-making effect (82 %) are still high in chronic disease care, but not as high as they are in the other areas. Treatment adaptation (75 %) and follow-up commitment (80 %) show that QoL surveys have a middling effect. This means that these tools are helpful, but it may be hard to use them consistently to manage chronic diseases. QoL tests are very useful for caring for the old because they lead to high patient happiness (90 %), decision-making effect (85 %), strong follow-up commitment (87 %), and healthcare worker engagement (83 %). These results show that QoL tests are very helpful for caring for the old because they help meet the complicated, varied needs of this age group, the figure 4 illustrate the comparison of assessment impact.
Problems and things that make it hard for Quality of Life (QoL) rating tools to be widely used in clinical practice are shown in Table 5. The data points out five main issues that make it hard for people to accept and use QoL tools effectively: a lack of time, pushback from clinicians, limited resources, problems with integrating data, and problems with training. Time limits (70 %) are the biggest reason why people don’t use QoL tools more. A lot of doctors have busy schedules that make it hard for them to give and understand QoL tests during regular appointments. This is especially important in places where time is limited, like emergency rooms or offices with a lot of patients. There are time limits in every part of healthcare, but the stress of putting urgent clinical issues ahead of full exams makes it harder to include QoL measures.
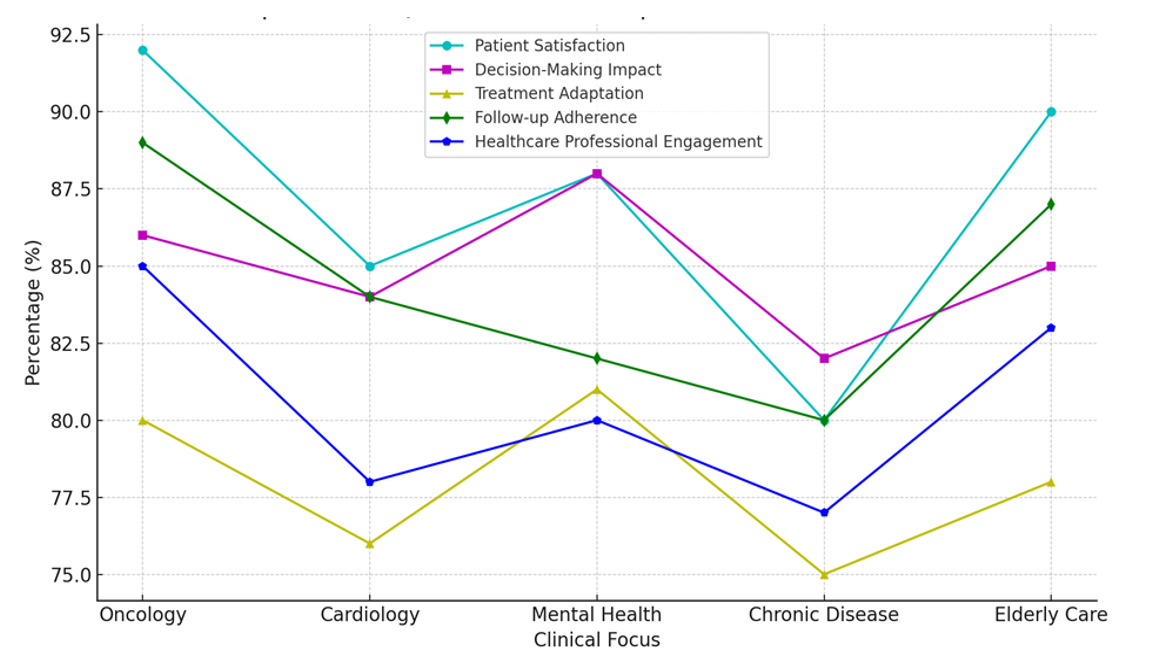
Figure 4. Comparison of QoL Assessment Impact across Clinical Focuses
|
Table 5. Challenges and Analysis with Widespread Use of QoL Tools |
|||||
|
Barrier |
Time Constraints ( %) |
Clinician Resistance ( %) |
Lack of Training ( %) |
Resource Limitations ( %) |
Data Integration Issues ( %) |
|
Time Constraints |
70 |
25 |
35 |
40 |
25 |
|
Clinician Resistance |
30 |
60 |
40 |
50 |
20 |
|
Lack of Training |
25 |
30 |
60 |
20 |
30 |
|
Resource Limitations |
20 |
10 |
50 |
60 |
35 |
|
Data Integration Issues |
40 |
15 |
30 |
45 |
30 |
Another big problem is that 60 % of clinicians don’t want to change. Many doctors might be hesitant to use QoL tests because they don’t know how to use them, aren’t sure how useful they are in the clinical setting, or are worried about the extra work that will come with them. This pushback is especially clear in fields like heart and some areas of chronic disease care that haven’t generally focused on what patients say about their results. It might be easier to get people to use quality of life (QoL) tools if you stress how they can improve medical care and help people make decisions together. Sixty percent of healthcare workers say they don’t have the right training to use and understand quality of life (QoL) tools. This is a big problem. If doctors get the right training, they will be able to correctly evaluate and react to the information these tools give them, which is very important for their successful integration into clinical practice, analysis illustrate in figure 5. If people aren’t trained enough, QoL tests might not be used to their full potential, which could lead to poor patient care. 60 % of the time, not having enough resources is also a big issue, especially in places with few resources or healthcare systems that don’t have the right facilities to support the broad use of QoL tools. This includes both the money to buy and set up the tools and the people who will be needed to monitor and analyse the results.
Lastly, problems with integrating data (45 %) make it hard for QoL tools to be used easily in clinical practice. Putting quality of life (QoL) data into electronic health records (EHR) systems can be hard, and the fact that different healthcare platforms don’t all use the same standards can make it harder to keep track of and compare patient data over time. For keeping an eye on patient results and making professional choices, it’s important to integrate data correctly.
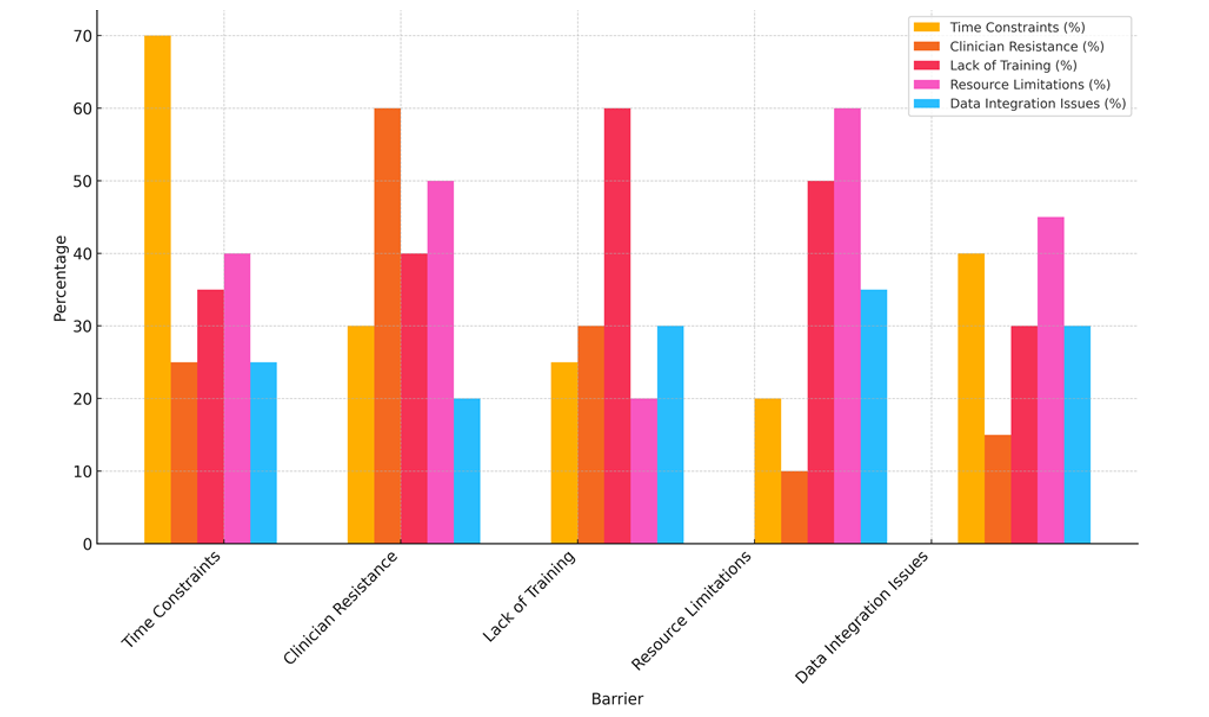
Figure 5. Analysis of Barriers across Metrics
|
Table 6. Variability Across Clinical Settings |
|||||
|
Clinical Setting |
Instrument Utilization ( %) |
Patient Population Coverage ( %) |
Implementation Barriers ( %) |
Clinical Decision-Making Impact ( %) |
Follow-up Monitoring ( %) |
|
Oncology |
85 |
95 |
40 |
82 |
77 |
|
Cardiology |
75 |
80 |
55 |
79 |
72 |
|
Mental Health |
80 |
85 |
45 |
86 |
78 |
|
Palliative Care |
90 |
88 |
60 |
84 |
81 |
|
Primary Care |
70 |
90 |
30 |
78 |
74 |
From cancer to heart to mental health to hospice care to general care, a variety of clinical settings find application for quality of life (QoL) measuring instruments. Table 6 compiles a synopsis of these variations. It looks at many crucial elements, including how the instruments are utilised, how many patients they cover, what challenges there are to adoption, how they influence professional decision-making, and how they are tracked after the fact. This shows how QoL tools are used differently in different specialities. In oncology, a lot of QoL instruments are used (85 %), which shows how important it is to look at the physical and mental effects of cancer treatments. With a 95 % patient coverage rate, oncology is one of the most common clinical areas that uses QoL tools. These tools help doctors figure out how cancer and its medicines affect patients’ lives in every way.
However, the application hurdles (40 % of the total) show that there are still problems putting these tools to use in everyday clinical practice. For example, clinicians may not want to use them or may not have enough time. In spite of this, the effect on professional decision-making is strong (82 %), showing that QoL ratings are useful for changing care and making things better for patients. Follow-up tracking is also important (77 %), making sure that people continue to get help after treatment, though it’s not as important as it is in hospice care. 75 % of people in cardiology don’t use QoL tools as much as people in cancer do. This is because cardiovascular diseases are more complicated and last longer. Coverage of the patient group is average (80 %), and the effect on professional decision-making is still big (79 %), but not as strong as in cancer. Obstacles to implementation in cardiology (55 %) include problems with physician acceptance and how useful people think QoL tests are for people with long-term diseases. Following up with patients is also not done as often (72 %), which might be because cardiology focuses on medical treatments and managing sudden events, impact analysis illustrate in figure 6.
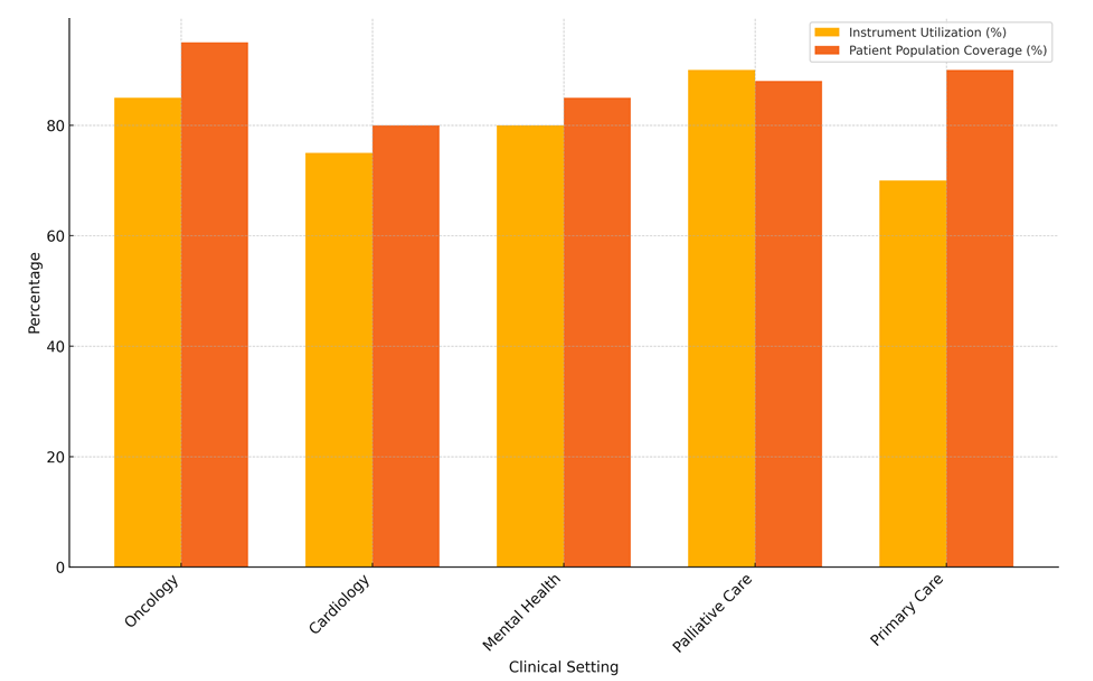
Figure 6. Instrument Utilization and Patient Population Coverage by Clinical Setting
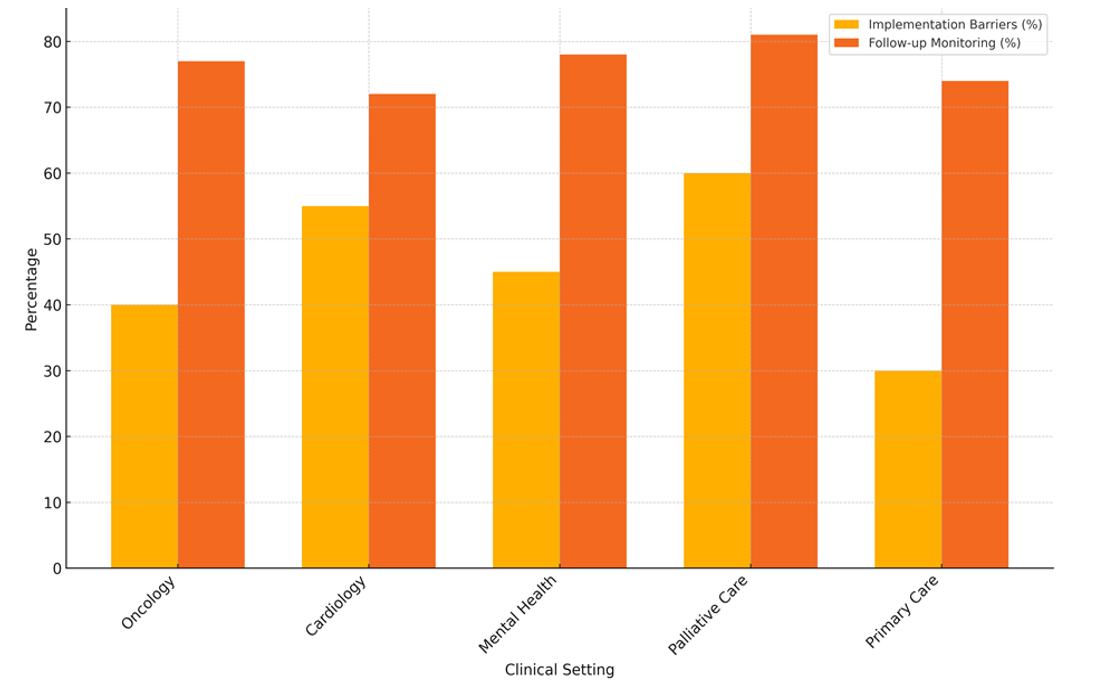
Figure 7. Implementation Barriers and Follow-up Monitoring by Clinical Setting
In mental health, QoL tools are used moderately (80 %) and are well covered by patients (85 %). This shows that QoL surveys are especially helpful for treating psychiatric conditions, where mental, emotional, and social factors play a big role. The effect on making decisions (86 % of the time) is very high, which shows how useful QoL tools are for helping to plan mental health care. Follow-up tracking (78 %) is also emphasised, since managing mental health for a long time often needs regular evaluations.
The most QoL tools are used in palliative care (90 %), which shows how important these tests are for end-of-life care, where knowing the patient’s quality of life is key to giving them considerate care. Strong patient group coverage (88 %) and follow-up tracking (81 %) show how important it is to provide ongoing care. However, application hurdles (60 % of settings) are the largest. This is probably because it’s hard to combine these tools with a very individualised care approach, as shown in figure 7.
Lastly, only 70 % of QoL tools are used in primary care, which may be because primary care focuses more on general health and preventing illness than on managing chronic conditions or specific conditions in detail. Even though the study included 90 % of patients, it had a relatively small effect on clinical decision-making (78 %), and follow-up monitoring (74 %). This suggests that while QoL assessments are helpful, they are not as central to decision-making in this setting as they are in more specialised areas like oncology or palliative care.
CONCLUSION
This study showed how Quality of Life (QoL) rating tools are becoming more important and common in clinical practice across many medical fields. The main results show that tools like the SF-36, EQ-5D, WHOQOL-BREF, and EORTC QLQ-C30 are becoming more and more popular in many clinical settings, including cancer, heart, mental health, and managing chronic diseases. These tools work well at measuring many parts of a patient’s health, like their physical, mental, and social well-being. This gives a more complete picture of how well the patient did. Patient-centered care has been much enhanced by quality of life (QoL) surveys, which also help doctors design more tailored treatment plans, make patients happier, and influence their decisions. They empower medical personnel to modify therapies depending on the feelings of every patient, therefore enhancing the general quality of therapy. The study found that even though QoL tools have benefits, they are not widely used because of things like lack of time, pushback from clinicians, and inadequate training. These problems make it clear that QoL tests need to be more fully integrated into clinical processes and that these problems need to be fixed so that they work as well as possible. There will be more changes in the role of QoL surveys in the future, especially as digital health improves and is linked to electronic health data. QoL tools could improve patient results, make healthcare more efficient, and promote a more patient-centered approach to care if they can get past their current limits and be used in more healthcare situations. In the end, QoL tests are very helpful in connecting clinical results with patient experiences. This makes them an essential part of modern healthcare.
REFERENCES
1. Verster JC, Sandalova E, Garssen J, Bruce G. The use of single-item ratings versus traditional multiple-item questionnaires to assess mood and health. Eur J Investig Health Psychol Educ. 2021;11:183-98.
2. Van Oostrom EC, Mulder KEW, Verheul MCE, Hendriksen PA, Thijssen S, Kraneveld AD, et al. A healthier diet is associated with greater immune fitness. PharmaNutrition. 2022;21:100306.
3. Topp CW, Østergaard SD, Søndergaard S, Bech P. The WHO-5 Well-Being Index: A systematic review of the literature. Psychother Psychosom. 2015;84:167-76.
4. Terwee CB, Mokkink LB, Knol DL, Ostelo RWJG, Bouter LM, de Vet HCW. Rating the methodological quality in systematic reviews of studies on measurement properties: A scoring system for the COSMIN checklist. Qual Life Res. 2021;21:651-7.
5. Kiani P, Merlo A, Saeed HM, Benson S, Bruce G, Hoorn R, et al. Immune fitness, and the psychosocial and health consequences of the COVID-19 pandemic lockdown in The Netherlands: Methodology and design of the CLOFIT study. Eur J Investig Health Psychol Educ. 2021;11:199-218.
6. Rautenberg T, Hodgkinson B, Zerwes U, Downes M. Meta-analysis of health state utility values measured by EuroQol 5-Domains (EQ5D) questionnaire in Chinese women with breast cancer. BMC Cancer. 2022;22:52.
7. Holst M, Ryttergaard L, Frandsen LS, Vinter-Jensen L, Rasmussen HH. Quality of life in HPN patients measured by EQ5D-3L including VAS. J Clin Nutr Metab. 2018;2:1-5.
8. Herdman M, Gudex C, Lloyd A, Janssen MF, Kind P, Parkin D, et al. Development and preliminary testing of the new five-level version of EQ-5D (EQ-5D-5L). Qual Life Res. 2011;20:1727-36.
9. Feng YS, Kohlmann T, Janssen MF, Buchholz I. Psychometric properties of the EQ-5D-5L: A systematic review of the literature. Qual Life Res. 2021;30:647-73.
10. Scalone L, Ciampichini R, Fagiuoli S, Gardini I, Fusco F, Gaeta L, et al. Comparing the performance of the standard EQ-5D 3L with the new version EQ-5D 5L in patients with chronic hepatic diseases. Qual Life Res. 2013;22:1707-16.
11. Krajewski PK, Marrón SE, Gomez-Barrera M, Tomas-Aragones L, Gilaberte-Calzada Y, Szepietowski JC. The use of HSQoL-24 in an assessment of quality-of-life impairment among hidradenitis suppurativa patients: First look at real-life data. J Clin Med. 2021;10:5446.
12. Del Duca E, Morelli P, Bennardo L, Di Raimondo C, Nisticò SP. Cytokine pathways and investigational target therapies in hidradenitis suppurativa. Int J Mol Sci. 2020;21:8436.
13. Krajewski P, Matusiak Ł, von Stebut E, Schultheis M, Kirschner U, Nikolakis G, et al. Quality-of-life impairment among patients with hidradenitis suppurativa: A cross-sectional study of 1795 patients. Life. 2021;11:34.
14. Chernyshov P, Finlay A, Tomas-Aragones L, Poot F, Sampogna F, Marron S, et al. Quality of life in hidradenitis suppurativa: An update. Int J Environ Res Public Health. 2021;18:6131.
15. Marron S, Gomez-Barrera M, Aragones L, Goni-Navarro A, Vilarrasa E, Diaz-Diaz R, et al. Quality of life in hidradenitis suppurativa: Validation of the HSQoL. Acta Derm Venereol. 2021;101:adv00529.
16. Dhruw B, Sahu LK. Improve transient and dynamic stability by using DC supply in HVAC line and analysis its fault operation and their recovery method. Adv Phys Lett. 2017;4(1):14-9.
17. Dhruw B, Sahu LK. Improve transient and dynamic stability by using DC supply in HVAC line and analysis its fault operation and their recovery method. Adv Phys Lett. 2017;4(1):14-9.
18. Kirby J, Thorlacius L, Villumsen B, Ingram J, Garg A, Christensen K, et al. The Hidradenitis Suppurativa Quality of Life (HiSQOL) score: Development and validation of a measure for clinical trials. Br J Dermatol. 2019;183:340-8.
19. Greffin K, Muehlan H, van den Berg N, Hoffmann W, Ritter O, Oeff M, et al. Setting-sensitive conceptualization and assessment of quality of life in telemedical care—Study protocol of the Tele-QoL Project. Int J Environ Res Public Health. 2021;18:10454.
FINANCING
The authors did not receive financing for the development of this research.
CONFLICT OF INTEREST
The authors declare that there is no conflict of interest.
AUTHORSHIP CONTRIBUTION
Conceptualization: Biswaranjan Mohanty, Swati Ingale, Nija Mani, Vandana Sharma.
Formal analysis: Lulup Biswaranjan Mohanty, Swati Ingale, Nija Mani, Vandana Sharma. Kumar Sahoo, Fazil Hasan, RenukaJyothi S.
Research: Biswaranjan Mohanty, Swati Ingale, Nija Mani, Vandana Sharma.
Methodology: Biswaranjan Mohanty, Swati Ingale, Nija Mani, Vandana Sharma.
Project management: Biswaranjan Mohanty, Swati Ingale, Nija Mani, Vandana Sharma.
Resources: Biswaranjan Mohanty, Swati Ingale, Nija Mani, Vandana Sharma.
Software: Biswaranjan Mohanty, Swati Ingale, Nija Mani, Vandana Sharma.
Supervision: Biswaranjan Mohanty, Swati Ingale, Nija Mani, Vandana Sharma.
Validation: Biswaranjan Mohanty, Swati Ingale, Nija Mani, Vandana Sharma.
Display: Biswaranjan Mohanty, Swati Ingale, Nija Mani, Vandana Sharma.
Writing - original draft: Biswaranjan Mohanty, Swati Ingale, Nija Mani, Vandana Sharma.
Writing - proofreading and editing: Biswaranjan Mohanty, Swati Ingale, Nija Mani, Vandana Sharma.