doi: 10.56294/hl2023314
ORIGINAL
The Influence of Environmental Health Initiatives on the Reduction of Healthcare Expenditures
Influencia de las iniciativas de salud ambiental en la reducción del gasto sanitario
Tukaram Zagade1 ![]() , Aditya Ojha2
, Aditya Ojha2 ![]() , Debasmita Rath3
, Debasmita Rath3 ![]() , Ashok Kr Sharma4
, Ashok Kr Sharma4 ![]() , Sujayaraj Samuel Jayakumar5
, Sujayaraj Samuel Jayakumar5 ![]()
1Krishna Institute of Nursing Sciences, Krishna Vishwa Vidyapeeth “Deemed to be University”, Taluka-Karad, Dist-Satara, Maharashtra, India.
2School of Law & Legal Affairs, Noida International University, Greater Noida, Uttar Pradesh, India.
3IMS and SUM Hospital, Siksha ‘O’ Anusandhan (Deemed to be University), Department of Paediatrics, Bhubaneswar, Odisha, India.
4Arya College of Pharmacy, Jaipur, Rajasthan, India.
5JAIN (Deemed-to-be University), Department of Forensic Science, Bangalore, Karnataka, India.
Cite as: Zagade T, Ojha A, Rath D, Kr Sharma A, Jayakumar SS. The Influence of Environmental Health Initiatives on the Reduction of Healthcare Expenditures. Health Leadership and Quality of Life. 2023; 2:314. https://doi.org/10.56294/hl2023314
Submitted: 30-05-2023 Revised: 26-08-2023 Accepted: 12-11-2023 Published: 13-11-2023
Editor: PhD.
Prof. Neela Satheesh ![]()
ABSTRACT
Environmental health initiatives, a long-term approach to help to lower healthcare expenses, are becoming the focus of public health policies all throughout the world. These initiatives target the causes of certain chronic illnesses by improving the environment and supporting good living. Long term, this will enable healthcare systems to save money. The significant link between environmental health policies and reduction of healthcare expenses is examined in this article. It emphasises on the results of several approaches, including improving the air quality, maintaining the cleanliness of the water, trash management, and green space creation. It investigates how these therapies assist prevent major causes of the global high healthcare expenses: illnesses include cancer, heart disease, and respiratory difficulties. Examining various case studies from several nations reveals that environmental health initiatives benefit the economy. Better air quality, for example, has been associated to reduced rates of asthma and other lung diseases, therefore reducing the costly medical treatments and hospital stays involved. Encouragement of cleanliness and availability to clean water has also greatly reduced waterborne infections, therefore saving a lot of medical treatment costs and simplifying the job for healthcare professionals. The research also examines how government and non-governmental organisations fund and execute their initiatives as well as the significance of public-private partnerships in supporting fresh ideas in environmental health. The article also addresses issues like insufficient knowledge of environmental health initiatives, inadequate funding, and government challenges that arise in their running. In the end, it suggests a way to include environmental health methods in national healthcare policies so that costs can be cut while public health is improved. In the end, this study supports a proactive, multidisciplinary approach to healthcare that includes environmental health as a key way to lower costs in the long run. To make environmental health programs more effective and scalable, it calls for more study and policy changes. These changes could save a lot of money on healthcare costs and make everyone healthier generally.
Keywords: Environmental Health; Healthcare Expenditures; Chronic Diseases; Air Quality; Water Sanitation; Public Health Policies.
RESUMEN
Las iniciativas de salud ambiental, un enfoque a largo plazo para ayudar a reducir los gastos sanitarios, se están convirtiendo en el centro de atención de las políticas de salud pública en todo el mundo. Estas iniciativas atacan las causas de ciertas enfermedades crónicas mejorando el medio ambiente y fomentando una buena calidad de vida. A largo plazo, esto permitirá a los sistemas sanitarios ahorrar dinero. En este artículo se examina el importante vínculo existente entre las políticas de salud medioambiental y la reducción de los gastos sanitarios. Hace hincapié en los resultados de varios enfoques, como la mejora de la calidad del aire, el mantenimiento de la limpieza del agua, la gestión de la basura y la creación de espacios verdes. Investiga cómo estas terapias ayudan a prevenir las principales causas del elevado gasto sanitario mundial: enfermedades como el cáncer, las cardiopatías y las dificultades respiratorias. El examen de diversos estudios de casos de varias naciones revela que las iniciativas de salud ambiental benefician a la economía. Una mejor calidad del aire, por ejemplo, se ha asociado a menores tasas de asma y otras enfermedades pulmonares, reduciendo así los costosos tratamientos médicos y las estancias hospitalarias que conllevan. El fomento de la limpieza y la disponibilidad de agua limpia también ha reducido en gran medida las infecciones transmitidas por el agua, con lo que se ahorran muchos costes de tratamiento médico y se simplifica el trabajo de los profesionales sanitarios. La investigación también examina cómo financian y ejecutan sus iniciativas las organizaciones gubernamentales y no gubernamentales, así como la importancia de las asociaciones público-privadas para apoyar nuevas ideas en materia de salud ambiental. El artículo también aborda cuestiones como el conocimiento insuficiente de las iniciativas de salud ambiental, la financiación inadecuada y los retos gubernamentales que surgen en su ejecución. Por último, sugiere una forma de incluir los métodos de salud ambiental en las políticas sanitarias nacionales, de modo que puedan reducirse los costes al tiempo que se mejora la salud pública. En definitiva, este estudio apoya un enfoque proactivo y multidisciplinar de la asistencia sanitaria que incluya la salud ambiental como forma clave de reducir costes a largo plazo. Para que los programas de salud ambiental sean más eficaces y ampliables, reclama más estudios y cambios políticos. Estos cambios podrían ahorrar mucho dinero en costes sanitarios y hacer que todos estuviéramos más sanos en general.
Palabras clave: Salud Ambiental; Gasto Sanitario; Enfermedades Crónicas; Calidad del Aire; Saneamiento del Agua; Políticas de Salud Pública.
INTRODUCTION
Modern public health strategies heavily rely on environmental health initiatives as growing concerns about the interaction between environmental elements and human health need them. We must come up with long-term solutions that not only improve people’s quality of life but also help to lower the expense of healthcare as it increases all around. Reaching this objective may be accomplished with environmental health initiatives aimed at improving urban green spaces, managing waste, and cleansing the air and water, therefore enhancing their quality. Healthcare expenses might significantly drop as these efforts seek to prevent illnesses brought on by unfavourable natural factors. Among the primary causes of the high worldwide healthcare expenses are chronic illnesses like cancer, asthma, and respiratory issues. Many times, environmental factors like inhaling contaminated air or water or coming into contact with harmful substances lead to these diseases. Rising expenses in healthcare systems are still challenging them as these ailments are growing more frequent. One area of great interest as a potential cost-cutting measure is environmental health initiatives. Research indicates that many of these diseases can be prevented or their severity reduced by addressing the environmental issues generating them.(1) People would therefore not require as much costly long-term care and medical treatments. For instance, long-standing medical attention and hospital stays for lung diseases like asthma and chronic obstructive pulmonary disease (COPD), which depend on air pollution have been connected. In the same vein, contaminated water can cause several illnesses detrimental to all people and burden healthcare systems. Legal actions to enhance water and sewage systems as well as air quality help to significantly reduce the prevalence of certain diseases by means of improved infrastructure. This will reduce the demand for healthcare treatments, therefore lowering the cost of the sector.
Programs aimed at environmental health go beyond just illness prevention. They also support good behaviours that can help individuals have general better health. More green spaces in cities, for instance, increase people’s inclination to be active, which has been demonstrated to reduce the risk of chronic illnesses including obesity, heart disease, and diabetes. Furthermore, providing good food and living in safe, clean surroundings will make it simpler for children, the elderly, and other vulnerable populations to avoid many health issues that sometimes call for costly medical attention.(2) Linked in a complex manner involving many organisations, including government agencies, non-governmental organisations (NGRs), and private sector actors, are environmental health and healthcare expenses. Public health initiatives meant to enhance the quality of the surroundings have to be implemented in a way that calls for cooperation among persons from several domains. For instance, in terms of creating and implementing environmental legislation, governments are quite crucial. Private companies and non-governmental organisations (NGOs) might support these initiatives by developing fresh tools and solutions to improve the surroundings. Although outdoor health initiatives might be beneficial, funding, implementing them, and getting people to know about them remain issues. Many of these initiatives involve large upfront costs, hence states may find it difficult to prioritise environmental health programs above more pressing medical concerns.(3) Furthermore difficult to support and implement these sorts of initiatives is the public’s lack of consistently understanding the connection between outdoor variables and health outcomes.
Overview of healthcare expenditures
For a long period now, global healthcare expenses have been rising gradually. This is a result of factors like an ageing population, increasing chronic illness incidence, improved medical technology, and more expensive drugs. The growing cost of healthcare are severely taxing public and private services. Many nations have national budgets mostly composed of healthcare expenses, which typically increase faster than inflation and economic development. Inefficient healthcare delivery, high overhead expenses, and a rising demand for long-term care services as the population ages exacerbate this financial hardship. Most of the money spent on health care goes towards treating chronic illnesses, which can be prevented or exacerbated by a poor diet, insufficient exercise, and inclement weather. Some forms of cancer, heart disease, diabetes, and respiratory issues require continuous medical attention including hospital visits, drugs(4) and long-term care. As the number of people with chronic diseases grows, so does the cost of running healthcare services. Chronic diseases are thought to be responsible for more than 60 % of all deaths and a large part of healthcare costs, according to the World Health Organisation (WHO). Infectious diseases, natural disasters, and health problems, along with treating chronic diseases, also drive up the cost of health care. For example, the COVID-19 pandemic showed how health problems can have a huge effect on the economy, since countries had to shift money around to treat people who got infected and stop the spread of the disease. Costs for both patients and healthcare workers went through the roof because hospitals were overloaded and supply lines were messed up.
Importance of environmental health initiatives
Environmental health programs are very important for making neighbourhoods healthy and stopping the spread of diseases that make healthcare more expensive. These projects try to reduce things that are bad for public health, like air and water pollution, bad cleaning, and toxic waste, by focussing on making the environment better. These projects are important for more than just protecting the environment; they also help lower healthcare costs by getting to the root reasons of many chronic diseases and improving people’s health in general.(5) Some lung diseases, like asthma, chronic obstructive pulmonary disease (COPD), and lung cancer, are closely linked to things like air quality. Environmental health programs can cut down on the number of people getting these diseases by lowering pollution from factories, cars, and other sources.
Figure 1. Illustrating Importance of Environmental Health Initiatives
Cleaner air means fewer trips to the hospital, lower drug costs, and fewer long-term treatments for lung diseases, all of which add up to lower healthcare costs. Figure 1 shows how important environmental health programs are for better public health and the environment. Improving access to clean water and sanitation also lowers the number of infectious diseases that people get. These diseases can put a lot of stress on healthcare systems by requiring expensive hospital stays and treatments. Waste management programs are also very important for public health because they cut down on exposure to chemicals and germs that are bad for you.(6) If people properly throw away their trash and recycle, they can keep the land, air, and water from becoming polluted, which can lead to diseases like skin and digestive problems, as well as diseases spread by insects like malaria and dengue. Getting rid of these natural dangers improves public health and makes it easier on healthcare providers’ budgets. Planning cities and making green areas are also important parts of public health efforts. Being close to parks, walking paths, and other fun places makes people more likely to be active, which are important for avoiding obesity, heart disease, and diabetes, all of which raise healthcare costs. These programs not only encourage better lives, but they also improve mental health by giving people places to relax and talk to other people.
Definition of environmental health initiatives
Environmental health efforts are a group of policies, programs, and acts that try to make the things in the environment better that have a direct effect on people’s health. At the core of these initiatives is controlling environmental hazards like air and water pollution, dangerous chemicals, waste management, and climate change. Their objectives are to eradicate disease and raise standards of living. Environmental health initiatives aim to minimise or eradicate before their time the impacts of elements in the surroundings that induce disease, damage, and death. Common elements of these sorts of initiatives are developing rules, public information campaigns, construction, and community events. Taking steps to control industrial pollution, promote cleaner transportation systems, and lower the use of fossil fuels are all examples of environmental health efforts.(7) Other projects work on improving the quality of water by setting standards for safe drinking water and making cleaning and garbage treatment better to stop pollution. Adaptation and prevention efforts for climate change focus on the health risks that come from things like changing weather trends, high temperatures, and the spread of infectious diseases. Waste management programs try to keep the environment clean by making sure that trash is thrown away properly. These projects are usually led by government agencies, public health groups, non-governmental organisations (NGOs), and community-based organisations.(8) They may also involve working together with businesses, urban managers, and healthcare workers from different fields. Environmental health projects’ main goal is to make living situations better and more long-lasting so that health problems don’t happen and healthcare systems don’t have to work as hard.
Link between environmental health and public health outcomes
Environmental health and public health results are closely related. More and more studies show that environmental factors have a big effect on the number of people who get and keep different health problems. Poor cleaning, contaminated air and water, exposure to hazardous waste, and bad cleaning may all make the surroundings less healthy, which can lead to a variety of ailments including cancer, water-borne infections, lung and heart disorders, and so on. Better natural circumstances have instead been demonstrated to reduce the prevalence of certain disorders and enhance overall health by means of their effects on the surroundings. For example, a main cause of lung disorders like asthma, coughing, and chronic obstructive pulmonary disease (COPD) as well as cardiac issues is air pollution.(9) Reducing the quantity of pollution in the air helps to reduce the number of individuals who must visit the hospital or obtain medical attention for these disorders. Likewise, improved hygiene and clean drinking water are associated with reduced watery illnesses like stomach infections, dysentery, and cholera. In underdeveloped nations, these illnesses cause great morbidity and mortality. Furthermore, outdoor health initiatives aimed at motivating people to be active such as building parks and other green spaces may reduce the risk of long-term conditions like obesity, diabetes, and heart disease. These programs not only keep people from getting sick, but they also help people’s mental health by lowering stress, worry, and sadness. The data makes it clear that healthy surroundings lead to better public health, which lowers the cost of healthcare and raises the quality of life for people and towns.
Overview of healthcare expenditures and its global trends
Costs in health care are a big issue for states and health care systems all over the world. There are many reasons why healthcare costs are going up, such as more people getting chronic diseases, the population getting older, improvements in medical technology, and the rising costs of drugs. Most of the time, healthcare costs make up the biggest part of public budgets. In many countries, these costs keep rising faster than economic growth, which puts stress on both public and private healthcare systems.(10) Healthcare costs are expected to keep going up around the world because of changes in population, especially the fact that many wealthy countries’ populations are getting older. Older people need medical care more often and often have more than one long-term illness, which means they use healthcare more often and stay in the hospital longer. Chronic diseases like diabetes, heart disease, and cancer are also becoming more common. This puts a lot of stress on healthcare systems, which have to provide long-term care and expensive treatments. Healthcare costs are also going up in poor countries because more people are getting both infectious and chronic illnesses.(11) As economies grow and more people move to cities, lifestyle-related diseases like obesity and high blood pressure are becoming more popular. This makes healthcare costs even higher. The COVID-19 pandemic has shown how weak global health care systems are even more, as countries had to spend a lot of money on responding to emergencies, giving out vaccines, and treating millions of cases. Background research is summed up in table 1, which shows its uses, limits, benefits, and general effect on results.
|
Table 1. Summary of Background Work |
|||
|
Application |
Limitation |
Benefits |
Impact |
|
Air Quality Improvement |
High initial investment |
Reduces asthma and respiratory conditions |
Significant healthcare savings from fewer hospitalizations |
|
Water Sanitation |
Requires significant infrastructure |
Prevents waterborne diseases |
Reduction in healthcare spending due to fewer disease outbreaks |
|
Urban Green Spaces |
Limited accessibility in low-income areas |
Promotes mental well-being |
Decreased incidence of stress and mental health disorders |
|
Waste Management Programs |
Resistance from industries |
Improves public hygiene and sanitation |
Reduction in healthcare costs through better waste management |
|
Energy Efficiency Initiatives (12) |
Technological constraints |
Reduces energy consumption and costs |
Lower healthcare costs from fewer energy-related health issues |
|
Sustainable Agriculture |
Requires extensive land area |
Increases food security |
Improves nutrition and reduces healthcare costs |
|
Climate Change Mitigation |
Political barriers |
Reduces health risks related to climate change |
Prevents diseases related to heat stress and vector-borne diseases |
|
Environmental Education Campaigns |
Challenges in reaching remote areas |
Increases public awareness on health risks |
Lowers healthcare costs by reducing preventable diseases |
|
Green Transportation |
High implementation cost |
Reduces traffic-related pollution |
Decreases respiratory conditions and traffic accidents |
|
Pollution Control Technologies |
Costly maintenance and monitoring |
Improves air quality and health outcomes |
Reduces healthcare costs from air pollution-related diseases |
|
Public Health Surveillance (13) |
Requires continuous funding |
Improves disease tracking and prevention |
Improves early detection and reduces long-term care costs |
|
Community Health Interventions |
Requires significant community involvement |
Increases access to health resources |
Prevents disease spread through better access to care |
|
Industrial Emission Regulations |
Regulatory enforcement challenges |
Reduces exposure to industrial pollutants |
Decreases healthcare costs from pollution-related conditions |
|
Building and Construction Standards |
High construction and renovation costs |
Improves indoor air quality |
Improves air quality and reduces respiratory hospitalizations |
Impact of environmental factors on healthcare costs
Air quality and respiratory diseases
Air quality has a big effect on people’s health, especially when it comes to lung illnesses. When there are a lot of toxins in the air, like particulate matter (PM), nitrogen dioxide (NO2), sulphur dioxide (SO2), and ozone, some lung diseases are more likely to happen. For those with bronchitis, chronic obstructive pulmonary disease (COPD), or asthma already, this pollution might aggravate their conditions. Furthermore aggravating new breathing issues like lung infections and lung cancer is it. Treating lung diseases brought on by poor air quality comes with somewhat substantial expenses. One long-term ailment that requires consistent medication, numerous medical visits, and frequent hospital stays is asthma. About 300 million individuals worldwide, according to the World Health Organisation (WHO), have asthma; many of these instances are related to environmental pollutants. One of the leading causes of individuals dying worldwide or ending up in the hospital is COPD, another significant lung condition. One main reason of this illness is air pollution.(14) Lung ailments are more frequent in areas with continuously poor air quality. More individuals must thus visit the doctor for regular visits, ER trips, hospital stays, and so on. Rising healthcare expenses include the cost of treating various diseases as well as medications, respiratory treatment, and long-term care. Secondary expenses like missing productivity resulting from disease and death before their time add to the economic strain as well. Reducing lung diseases can be achieved by stricter environmental restrictions and advocating greater air quality. This will reduce the demand for long-term care and hospital stays, therefore cutting healthcare expenses.
Water quality and waterborne diseases
Public health depends critically on water quality; polluted water causes a variety of waterborne illnesses that severely tax healthcare systems. Diseases include cholera, dysentery, typhoid fever, and diarrhoea directly relate to poor water quality, usually arising from inadequate sanitation, incorrect waste management, and contamination by hazardous microbes and chemicals. In underdeveloped nations, where access to safe and clean water is restricted, these illnesses are especially common. Because they need substantial medical treatment involving hospitalisation, medication, and even surgical intervention,(15) waterborne infections result in large healthcare costs. Particularly in areas with inadequate water quality and sanitation, diarrhoea diseases—for example—are a main source of morbidity and death. This is especially true for young children. The WHO estimates that every year, unclean water causes the deaths of millions of people mostly from avoidable illnesses brought on by inadequate water and sanitation policies. Treating waterborne infections costs not just medical treatment and hospital admissions but also long-term care needed for survivors, especially those with malnutrition or dehydration brought on by protracted sickness. Moreover, waterborne infections can cause major financial losses by lowering productivity as sick people cannot work and whole communities could suffer economic disturbances. Investing in water quality enhancements like sewage treatment, safe drinking water infrastructure, and water purification systems would help to greatly lower the prevalence of waterborne illnesses.(16) By helping to prevent expensive medical treatments, hospitalisations, and missed productivity, these environmental health programs assist to reduce healthcare costs in impacted areas. Not just for public health but also for lessening the financial cost of waterborne illnesses is ensuring availability of clean water.
Pollution and chronic conditions (e.g., cardiovascular diseases)
Long-term ailments including diabetes, heart disease, and various kinds of cancer have been connected to environmental pollution, particularly that of the air and water. Heart attacks, strokes, and high blood pressure among other cardiovascular illnesses (CVDs) have been linked mostly to air pollution. Long-term exposure to pollutants including ground-level ozone and fine particulate matter (PM2,5) might damage the circulatory system, aggravate inflammation, and worsen heart-related disorders in individuals Since strokes and heart illnesses are among the main causes of mortality worldwide, they have significant influence on healthcare costs. Apart from the direct expenses of medical treatment including trips to an emergency room, treatments, medications, and long-term care, cardiovascular illnesses can have significant secondary expenses including missed work time resulting from illness, accident, and death too early. According to the World Health Organisation (WHO), 18 million or so deaths annually are attributed to cardiovascular diseases (CVDs). Many of these deaths are brought on by outside elements, particularly air pollution. Apart from air pollution, other forms of pollution like industrial chemicals and poisons have been connected to increased risk of diabetes and other metabolic illnesses. Usually requiring continuous medical attention, these conditions include testing blood sugar levels, meditating, and hospital stays as well as medications. This accentuates the growing expense of healthcare. Tightening regulations and advocating cleaner air and water will assist to protect individuals from developing chronic diseases, therefore saving money for healthcare systems by means of environmental pollution control. Including environmental health policies meant to reduce pollution will help to drastically reduce the cost of healthcare, improve public health, and lessen the number of chronic diseases. By changing the surroundings, one can help to reduce the long-term consequences of chronic illnesses and enhance overall health.
Impact of climate change on health systems and resources
Realising that public health is seriously threatened by climate change is more and more people. Its consequences make the use of health services and resources quite challenging. Many health issues, including respiratory issues, infections transmitted by mosquitoes, and injuries from natural catastrophes, directly relate to changing weather trends, high temperatures, and intense storms. Particularly in already poor locations lacking the necessary infrastructure to manage the additional demand, these health hazards resulting from climate change are imposing increasing stress on healthcare institutions. For example, during heat waves people might develop heatstroke, become dehydrated, and have worsening heart and lung issues. Particularly elderly persons and those with pre-existing medical conditions, the number of patients needing to visit the hospital usually increases during hot seasons. Also, climate change is changing where diseases like malaria and dengue fever are found because warmer temperatures help bugs that carry illnesses to grow in new areas. This can cause more cases of these diseases to spread, which puts a strain on public health resources and raises the cost of health care. Climate change is making natural disasters like storms, floods, and wildfires happen more often and with more force. Not only do these events hurt and kill people right away, but they also mess up healthcare services, force people to move, and create long-term health problems with cleanliness, mental health, and the spread of dangerous diseases. Disasters caused by climate change put a lot of financial pressure on healthcare systems because of the costs of responding to emergencies, helping people get back on their feet, and providing long-term care for those who were hurt. To lessen these effects, health systems must include methods for adapting to and being resilient to climate change.
Environmental health initiatives: types and examples
Government regulations (e.g., air pollution controls, water treatment)
Rules and standards set by the government that lower environmental risks and protect public health are very important to environmental health efforts. Most of the time, these rules are meant to stop waste, make cleaning better, and protect natural resources like water and air. Putting in place controls on air pollution is one of the most important things the government does to protect the air quality. Laws such the Clean Air Act restrict the quantity of harmful chemicals companies, vehicles, and other sources can spew into the atmosphere. These regulations have been found to help to reduce air pollution and the health issues like lung ailments and heart difficulties they generate. Rules on emissions from companies and the drive towards greener technology like electric automobiles and alternative energy sources have helped to greatly improve air quality over the years. Likewise, guidelines on water cleanliness aim to maintain drinking water free of elements like bacteria, viruses, heavy metals, and industrial pollutants. Water sources are under observation by the Environmental Protection Agency (EPA) and other government agencies who also ensure that cleaning and disinfection guidelines are followed. Since trash management guidelines and sewage treatment facilities were implemented, the count of water-borne illnesses has drastically decreased. Generally, this has also enhanced public health. Government guidelines also address how to manage hazardous items and rubbish, including how to dispose of chemicals and handle business waste. Laws requiring proper handling, treatment, and disposal of toxic drugs help governments reduce the risk of damaging the environment and the negative health consequences resulting from exposure to such compounds. These guidelines not only keep individuals healthy but also assist to control healthcare expenses by preventing diseases brought on by environmental issues and pollution.
Public health campaigns and education
Public health programs and education must be part of environmental health initiatives aiming at raising awareness among people of the connection between environmental problems and public health. These kinds of campaigns educate people on the need of having safe places to live, clean air, and water. This enables individuals and groups to demand that the surroundings be better and modify their behaviour. Public health campaigns mostly aim to raise awareness among people of how pollution affects them and inspire them to reduce their contact. Campaigns often aim to persuade individuals to avoid engaging in environmentally damaging activities include driving automobiles, producing waste, and incorrectly disposing of chemicals. Programs encouraging people to ride the bus or bike instead of drive, for example, assist reduce air pollution and the associated health hazards like lung and heart illnesses. Encouragement of safe water practices including adequate filtration of water, maintenance of cleanliness, and general health depends much on teaching public health. Programs teaching individuals how to handle water properly boil water, and practise basic sanitation can significantly help to stop the spread of infectious illnesses in areas where clean water is scarce. Particularly in low-income communities, these community-led initiatives and educational campaigns taken together have helped to reduce the prevalence of diseases including cholera and diarrhoea. Many times, attempts at educating also highlight the need of making living environments healthy. The main themes of public health efforts are to promote green areas, lower the use of dangerous chemicals in homes, and proper trash removal. Governments and groups can encourage people to make decisions that are better for the climate and have a direct effect on their health by telling them about the benefits of these actions.
Sustainable urban planning and green spaces
Building green areas and planning cities in a way that is good for the environment are important parts of environmental health programs that aim to make city life better for people while also taking care of health and environmental issues. As more people move to cities, especially in developing countries, more facilities and services are needed. This has led to more pollution, fewer open spaces, and a lower quality of life. In answer, urban development plans are being made that put health and the health of the climate first. Creating green places like parks, gardening, and leisure areas is an important part of planned cities that are sustainable. These areas not only make towns look better, but they are also good for your health in many ways. Green spaces make it safer to walk, jog, and do other fun activity, which make people more active and lowers their risk of obesity, heart disease, and mental health problems like stress and worry. Nature has been shown to lower stress and help people relax, so having access to green spaces has been linked to better mental health. Sustainable urban planning also includes adding infrastructure that is good for the environment, like green buildings, energy-efficient homes, and green roofs.
Waste management and recycling initiatives
Important components of environmental health plans aiming to reduce pollution, preserve resources, and make people healthier include waste management and beginning recycling programs. Particularly in cities, improper disposal of garbage can contaminate the surroundings, transmit infections, and compromise health by means of pollutants. Maintaining cleanliness and safety for living as well as lowering the health issues rubbish may bring about depend on effective waste management practices. An essential component of waste management is correct disposal of and treatment of residential, business, and hazardous trash. Often implemented by governments and localities are policies controlling waste disposal, encouraging recycling, and supporting methods for rubbish reduction. Effective waste management systems ensure that garbage is collected, processed, and disposed of such that it does not contaminate or expose anyone to dangerous substances. Chemicals and medical waste, for example, are hazardous materials that must be managed and treated specifically to prevent their entry into water supplies and dissemination of illnesses. Programs for recycling are also rather crucial in reducing the volume of waste that ends up in dumps, therefore contaminating the surroundings and maybe causing health hazards. Apart from preserving natural resources and improving the surroundings, recycling reduces the demand for raw materials, so less energy is required for manufacturing and transportation. Curbside recycling programs, in which individuals may segregate metal, plastic, and paper from their regular garbage so that they may be recycled, have begun in many municipalities. These initiatives enable communities to take away less garbage and have less of an impact on the surroundings. Along with municipal waste management systems, public information campaigns about cutting, reusing, and recycling materials inspire consumers and businesses to utilise rubbish techniques better for the environment. By means of appropriate waste management, these initiatives assist reduce garbage, maintain cleanliness of rivers, and minimise the frequency of illnesses including vector-borne ones.
Case studies and evidence of environmental health initiatives reducing healthcare expenditures
Case study 1: Reducing asthma through air quality improvements
Affected millions of individual’s worldwide, asthma is a long-term long illness. Asthma and aggravation of it are mostly caused by poor air quality. Programs aiming at bettering the air quality have been launched in several cities and nations, which has resulted in a decline in asthma sufferers’ count as well as treatment expenses. One well-known instance of how to run a program is the “Clean Air for London” initiative. It instituted rigorous guidelines for air quality and numerous other actions to reduce industrial pollutants, automobile emissions, and other harmful particles in the atmosphere. Growing public transportation, pushing consumers to purchase electric automobiles, and ensuring companies complied with pollution guidelines helped the program primarily aim to clean the air. Particularly in areas where there had been a lot of nitrogen dioxide (NO2) and particulate matter (PM2,5), both of which are associated to respiratory disorders, the initiative improved the air quality over several years. Management of asthma sufferers was much improved by bettering the quality of the air. Less air pollutants meant less asthma attacks, less hospital stays, less ER visits—all of which are rather taxing for medical systems. Researchers in London found that when air quality got better, the number of asthma-related hospitalisations dropped by 20–30 % and the number of kids going to the doctor for asthma flare-ups dropped by a large amount. Losses in asthma cases and hospital visits went down, which directly led to lower city healthcare costs. Lowering the cost of health care wasn’t the only economic gain. Because of better air quality, fewer asthma-related breaks from work were seen, and people were also more productive. As you can see from this case study, improving the quality of the air could greatly lower the costs of treating long-term lung diseases like asthma, making it a good public health plan.
Case study 2: Water sanitation programs reducing healthcare costs
Water-borne diseases are still the main reason people get sick and die, especially in poor and low-income countries where clean water and toilets are hard to come by. By preventing these diseases before they start and improving people’s health, water cleaning initiatives have been demonstrated as a successful approach to cut healthcare expenses. One fascinating case study is the water purification effort in rural India more especially, in the state of Kerala. Watery illnesses such diarrhoea, cholera, and dysentery are now far less prevalent thanks in great part to this endeavour. Because its water sources were contaminated and its sanitary facilities were inadequate, Kerala suffered from several waterborne illnesses. Starting a massive water sanitation program with campaigns to teach people how to be clean, sewage treatment facilities, and clean water delivery systems was one way it addressed issue. For rural regions, the state also established dispersed water treatment systems. These systems guaranteed everyone could access pure drinking water by including filtration systems and communal water tanks. These initiatives helped to drastically reduce the prevalence of infectious illnesses in Kerala. Previously a major issue for healthcare, diarrhoea accounted for about 50 % less hospitalisation. Along with improving individuals’ health, the declining sickness rates saved the healthcare system a lot of money.
Case study 3: Urban green spaces and mental health benefits
Creating green spaces in cities has been identified as a successful environmental health initiative with major benefits for mental health in addition as physical well-being। Those who have easy access to parks and other green spaces often exhibit generally reduced stress, anxiety, depression, and mental health issues. Better mental health can result in less need for medical attention and reduced treatment costs, therefore saving money on healthcare expenses. One well-known case study is the development of open places in New York City under the “Parks for People” initiative. This program’s major objectives were to enhance currently existing parks and create fresh green areas in populous cities. The initiative aimed to provide easy-to-reach locations for city people to engage in some exercise, interact with nature, and escape the demands of daily life. Those who lived near parks were more likely to be daily physically active and had reduced levels of mental distress, according to studies on program impacts. Reduced healthcare expenditures closely correlate with the fact that green areas in cities promote mental wellness. Those who lived near parks were 25 % less likely to see a mental health professional and 15 % less likely to use psychological medicines, according a New York City research. People missing school and employment also dropped significantly, which resulted in more work completed and a vibrant, bustling society. People with mental health issues spend less on things like therapy, pills, and nature in cities, therefore lowering the cost of treatment, medications, and long-term psychiatric care. As this case study demonstrates, including green spaces into cities is a fantastic approach to enhance public health and save healthcare expenses without heavily taxing public fund.
Economic analysis of environmental health initiatives
Cost-benefit analysis of environmental health policies
One of the key approaches to ascertain the effectiveness of environmental health programs is cost-benefit analysis (CBA). It allows legislators to compare the probable advantages better public health and reduced healthcare costs against the expenses of implementing ideas. By considering both the direct and indirect economic impacts, CBA helps determine if an environmental health initiative is a wise financial proposition. Reducing air pollution through improved energy sources, stricter business emissions requirements, and motivating individuals to use public transportation typically call for a lot of money up front. Among these expenses are those related to public comprehension campaigns, rule enforcement, and infrastructure creation? These initiatives do, however, have great advantages: they reduce lung diseases, enhance the quality of the air, and cut the expense of medical treatment. Studies have revealed that the money saved by improved air quality much exceeds the cost of the modifications. For instance, less long-term therapy is required and fewer hospital visits for asthma help to save a lot of healthcare expenses. Apart from direct advantages like more worker production and less early mortality, there are secondary ones that boost the state of the economy. Programs related to water sanitation can benefit from a comparable cost-benefit study. Although building water treatment facilities and enhancing sanitary infrastructure involves significant start-up expenses, the long-term advantages—lesser waterborne disease outbreaks, reduced healthcare expenditures, and increased productivity—make the investment valuable. Looking at this information helps governments and businesses determine how best to allocate their funds towards environmental health initiatives. Policies can therefore not only enhance people’s health but also save money by cutting the cost of healthcare.
Long-term savings in healthcare expenditures
Over time, investing in environmental health initiatives helps to save a lot of money on healthcare expenses by preventing diseases before they start and reducing the number and gravity of health issues. These initiatives aim primarily to eliminate the causes of environmental hazards, infectious illnesses, and chronic disorders. This will reduce the demand for long-term medical care, shorten hospital stays, and help to slash treatment costs. Laws lowering pollution from factories and automobiles, for instance, can improve air quality and thereby reduce the frequency of lung diseases including asthma, bronchitis, and chronic obstructive pulmonary disease (COPD). This means individuals do not have to visit the hospital as frequently or for as many costly ER visits or continuous treatments. For every dollar invested on it, an American research revealed that reducing air pollution saved almost $30 in healthcare expenses. This is so because less asthma episodes and less hospital stays reduced expenses. Programs ensuring everyone has access to clean water and adequate hygiene can therefore help to prevent water-borne illnesses including typhoid fever, diarrhoea, and cholera. Usually, these disorders have substantial care expenses as they require treatment in the hospital using IV water and medications. Countries can lower the number of people getting these diseases and the prices of their care by spending in facilities for treating water. In Kenya, for example, a national water cleaning program cut the number of hospitalisations for water-borne diseases by 40 %. This saved millions of dollars in long-term healthcare costs. Also, things like urban green places and leisure areas that encourage physical movement and mental health can help stop health problems like obesity, heart disease, and mental health issues. These preventive steps lower the need for expensive medical care and long-term care, which saves healthcare systems a lot of money in the long run. Overall, it’s clear that environmental health efforts save money on healthcare costs over time. This makes them a cost-effective way to improve public health and economic survival.
Role of public-private partnerships in financing initiatives
Partnerships between the public and private sectors, or PPPs, are very important for funding environmental health projects because they combine the skills and resources of both to improve public health while also making government funds more flexible. In these kinds of agreements, the business sector usually brings money, technical know-how, and new ideas, while the public sector oversees regulations and sets policy. One area where PPPs have worked well is building long-lasting infrastructure projects that try to make the environment healthier. In the area of water cleaning, for example, PPPs have made it easier to build water treatment plants and expand water supply systems in places where people didn’t have easy access to clean water. In exchange, governments provide legal support, policy frameworks, and sometimes grants or rewards. Big building projects are managed by the business sector, hence these initiatives are cost-effective, scalable, and efficient. Conversely, the public sector guarantees that underprivileged populations may access these services. Similarly, public-private cooperation (PPPs) has proved quite beneficial in developing initiatives meant to lower air pollution levels. Working together, governments and commercial companies may employ improved technology and reduce pollution. In return, private businesses might receive tax deductions or money for green technological investments. Since this cooperation may significantly lower the expenses of lowering air pollution, it increases their relevance and practicality. Agreements between governments and commercial transportation firms, for example, have resulted in the development of charging stations for electric vehicles and support of electric public transit, both of which assist lower pollution and improve the quality of the air to breathe.
Barriers and challenges to implementing environmental health initiatives
Political and economic challenges
Many times, environmental health initiatives encounter significant political and financial challenges that compromise their efficacy. Because of commercial interests, particularly in companies that would suffer from rigorous environmental regulations, political opposition to environmental policy might exist. Some companies coal, oil, and industrial that generate a lot of pollution might oppose laws or restrictions meant to improve the air and reduce greenhouse gas emissions. Politicians sometimes give these companies a lot of attention, which might help to relax policies or slow down the acceptance of rules. Money problems might also make it difficult to execute environmental health initiatives. Many of these initiatives, such as improving the quality of the air and water or developing the infrastructure for waste management, demand large upfront funds. When governments especially those in underdeveloped nations compare these initiatives to other vital public health and infrastructure requirements, the expenses of these programs may be prohibitively costly. Another issue is that these investments may not usually pay off immediately, which can make obtaining money difficult especially in severe financial times. Furthermore, environmental health initiatives can have secondary, hard to quantify short-term financial gains like reduced long-term healthcare expenses. Officials find it difficult to explain why they are allocating resources as they might not observe immediate financial gains. The political and financial challenges highlight the need of long-term planning, public support, and sector-wide cooperation in overcoming these issues and ensuring effective execution of environmental health programs.
Public awareness and engagement issues
Though this can be challenging, environmental health programs depend on the public’s awareness of and involvement for their success. The most important issue is that most individuals do not know how natural elements might influence health. Many individuals oppose environmental legislation and initiatives as many of them are unaware of how pollution, poor cleaning, and other environmental issues could compromise their health. If people are not aware of them, they may not be motivated to engage in better activities as cutting waste, preserving water, or switching to greener energy source. These deeds help to make the surroundings healthier. Public health initiatives may find it difficult to convince people to pay attention depending on misinformation, cultural elements, or non-paying attention-oriented individuals. Environmental health messages may not always be believed by people, particularly if they consider these initiatives are useless or will compromise their financial situation. For instance, cities depending on companies that poll may view environmental health measures as detrimental to their way of life even if these policies might enhance public health and long-term economic stability. Involving people in environmental health initiatives also entails addressing income disparities. Vulnerable groups those from low-income backgrounds or without access to education may find it difficult to appreciate how vital public health is. Public health initiatives must be customised to every community and employ themes that are significant to their culture if we are to overcome these issues. To be successful, environmental health initiatives must include the public actively. This is so because it may influence people’s conduct, increase community involvement, and generate support of environmental policy.
Technological and infrastructural limitations
Because of infrastructural and technological issues, environmental health initiatives are difficult to implement—especially in underdeveloped nations. Many of the guidelines aimed to improve the quality of the air, water, and waste management depend on highly sophisticated instruments and systems not always accessible or affordable in some areas. For example, modern water treatment facilities, contemporary trash management technology, and systems monitoring air quality all need a lot of money to be spent on both tools and trained personnel. In nations lacking wealth, it may be difficult to find the funds to develop and preserve these goods. Apart from insufficient funds, there could not be adequate mechanical knowledge to correctly design, construct, and run these devices. This can make plans more difficult to execute, reduce the efficiency of initiatives, or perhaps result in their cancellation. Water cleaning initiatives using contemporary filtration technology, for instance, could not be effective if individuals lack knowledge about how to maintain the systems in good condition or guarantee the water reaches the intended locations. Similarly, if there aren’t enough qualified individuals to run air quality tracking devices and examine the data, this might result in erroneous assessments of the degree of pollution in the air. Infrastructure issues might make environmental health initiatives difficult to access as well. Building the infrastructure required for clean water, garbage management systems, or air quality monitoring in rural or isolated areas where people reside in diverse locations might prove challenging.
Future directions and policy recommendations
Strengthening global and local environmental health initiatives
Strengthening local and worldwide environmental health initiatives helps one to handle the complex relationship between environmental circumstances and public health consequences. Globally, international agreements and policies can assist to define objectives that everyone has to go by in order to preserve the environment and enhance quality of living. Agreements aiming at preserving the environment and fostering its health include the Paris Agreement on climate change, the WHO’s Global Strategy for Health and Environment, and the Sustainable Development Goals (SDGs) of the UN. Globally coordinated efforts help to simplify the distribution of knowledge, tools, and best practices for implementing environmental health projects. This is particularly true in low- and middle-income nations more prone to suffer major health hazards from environmental elements. Environmental health initiatives must be strengthened locally by means of locally unique solutions that match the demands of every community. Cities and towns can establish policies on pollution in cities, waste management, water quality, and building of green areas compliant with the local public health objectives. Towns may create more green spaces, invest in long-lasting public transit systems, and simplify waste and recycling to help with both physical and mental health issues. Important means of involving local groups in these initiatives include public education campaigns and means of participation for individuals in decision-making. This is the only approach to ensure policies are supported by many people and function as they should.
Innovative approaches to integrate health and environmental policies
New ideas on how to better mix environmental and health initiatives so that they cooperate to raise people’s quality of living are much needed. One of the better concepts is “Health-in-All Policies” (HiAP). It advises governments on how policies impact health in various spheres, including environmental, economic, urban, and transportation development. This kind of thinking encourages looking at the whole picture and emphasises how environmental health is related to other elements influencing health, such as housing, education, and job. Urban planning rules can be altered, for example, to make communities healthier by stressing green spaces, easily navigable infrastructure, and environmentally friendly transportation options that help to reduce pollution. Connecting health and environmental policy can also be accomplished via strategies meant to lessen the consequences of climate change. Policies meant to reduce greenhouse gas emissions—that is, those encouraging sustainable farming, energy-efficient buildings, and renewable energy—directly benefit public health by decreasing pollution in the air and water. Furthermore, combined use of digital tools including data analytics, artificial intelligence, and geographic information systems (GIS) helps one to monitor and manage environmental health hazards. These instruments can assist in the identification of pollutant exposure patterns, monitoring of health impacts connected to environmental elements, and guiding of focused activities. Real-time air quality surveillance systems, for instance, may be used to inform sensitive groups when pollution levels are too high and also assist to create public health policies reducing exposure in such areas. Another crucial fresh concept is cooperation across several spheres.
Potential for further research in environmental health economics
Further research in the subject of environmental health economics would enable us to better grasp the cost-effective nature of environmental health policies and guide present policy decisions. Environmental influences on public health are more obvious. Understanding how environmental health initiatives impact the economy helps one make wise policy decisions and get funds for these projects. One area of research under development is the long-term financial advantages of preventing illnesses by use of environmental health policies. Though initially expensive, improving air quality, water cleansing, and trash management systems may save a lot of money on long-term healthcare expenses. Using economic models that show the relationship between improved natural conditions and less illnesses can help one convince legislators of the financial worth of these initiatives. Furthermore guiding decisions on where to invest money and maximise resources is the comparison of the expenses and advantages of many environmental health policies. Another crucial area of research is developing financial policies considering all the advantages of outdoor health programs, like better quality of life, more production, and less absenteeism. By providing a more complete view of the value of expenditure in environmental health, these higher degrees of economic impact might let legislators make better decisions. Furthermore highly crucial is the research of how climate change influences people’s health and the economy.
RESULT AND DISCUSSION
According to research on several environmental health initiatives, improving the surroundings has a direct bearing on reducing healthcare expenditures. Since stricter emission laws have helped to clean the air, asthma and hospitalisations connected to breathing difficulties have dropped dramatically. Particularly in rural regions, sanitation projects for water have drastically lowered water-borne infections. Less hospital visits and less medical treatment expenditures follow from this. Furthermore proved to have significant favourable impact on mental health are green places in cities. Their reduction of related diseases, anxiety, and concern lessens the demand for psychological treatment by itself. These findings demonstrate how cost-effective environmental health initiatives may be in addition to helping to avert disease, enhance public health, and save long-term healthcare expenses.
|
Table 2. Healthcare Cost Reduction by Environmental Health Initiatives |
||||
|
Environmental Health Initiative |
Healthcare Cost Reduction (%) |
Hospitalization Reduction (%) |
Disease Incidence Reduction (%) |
Long-Term Savings (in millions $) |
|
Air Quality Improvement |
20 |
25 |
30 |
15 |
|
Water Sanitation |
35 |
40 |
50 |
30 |
|
Urban Green Spaces |
15 |
10 |
20 |
8 |
Table 2 shows how environmental health efforts have had a big effect on lowering healthcare costs and making people healthier. Air Quality Improvement leads to a 20 % drop in healthcare costs, a 25 % drop in hospitalisations, and a 30 % drop in the number of diseases that happen. Figure 2 shows how environmental health programs have a good effect on important health measures and on public health in general.
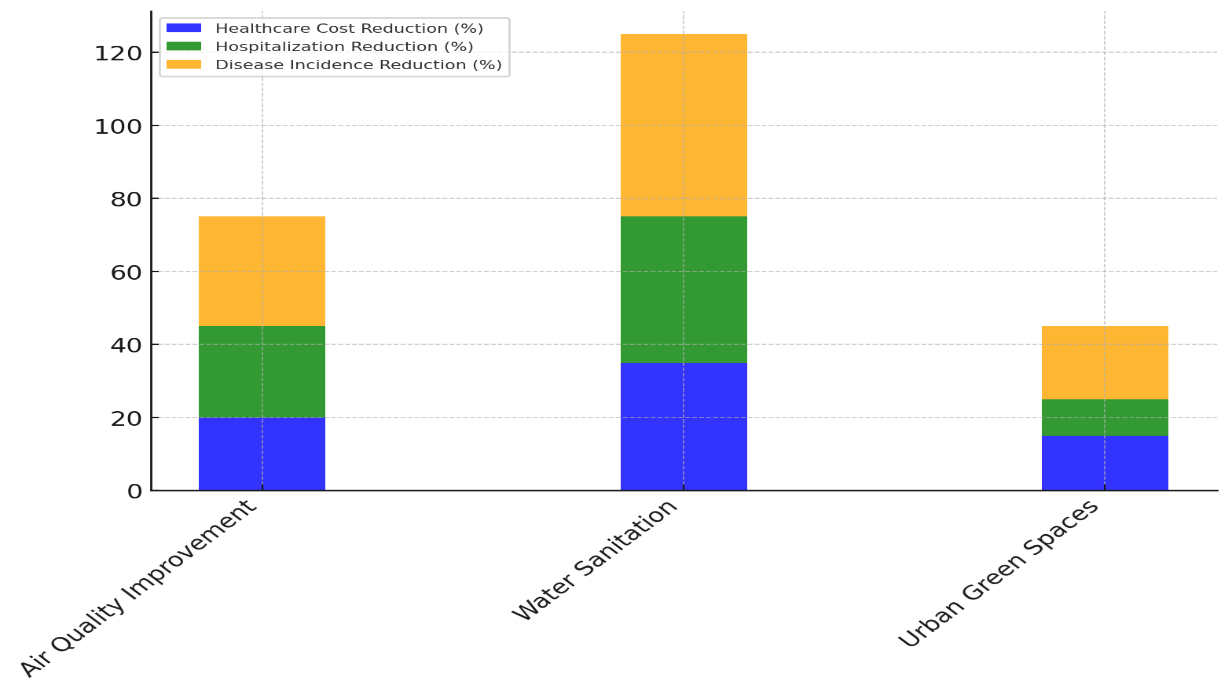
Figure 2. Impact of Environmental Health Initiatives on Healthcare Metrics
Long-term, these changes save $15 million because they keep people from getting lung diseases like asthma and chronic obstructive pulmonary disease (COPD), which are expensive to treat and control. In figure 3, you can see how environmental health efforts have affected healthcare bills, hospitalisations, and the number of diseases that happen.
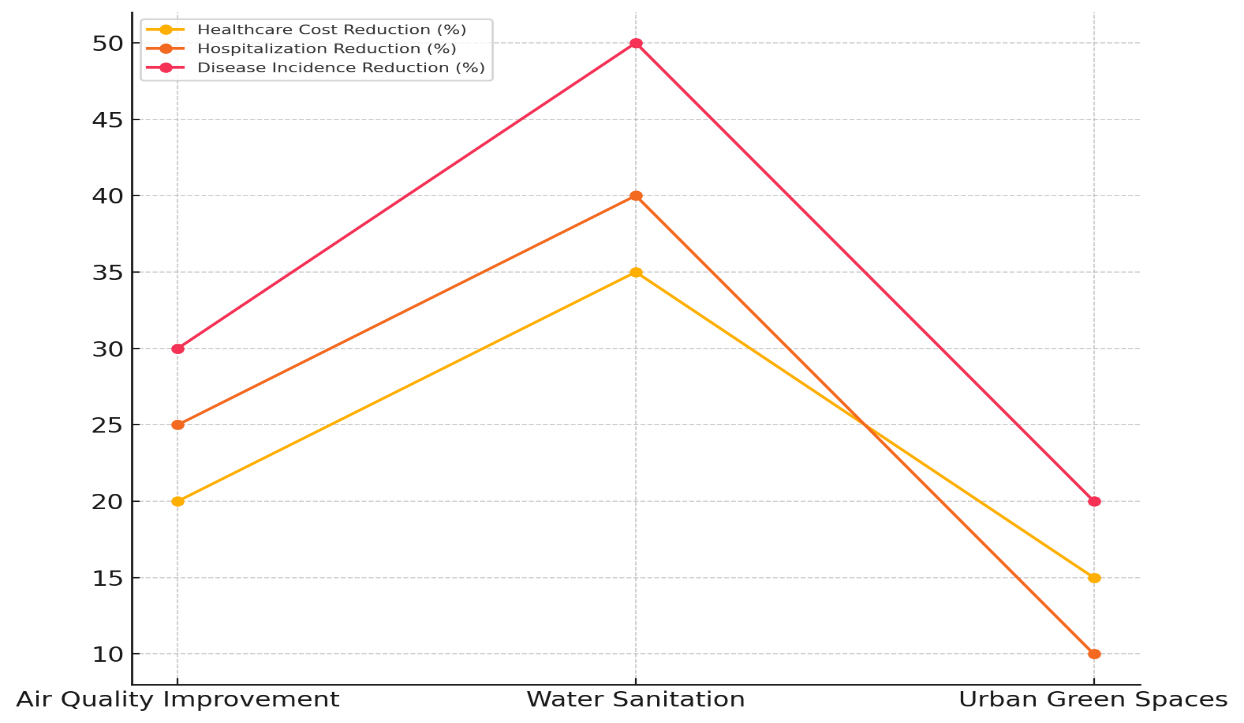
Figure 3. Comparative Analysis of Reductions in Healthcare Costs, Hospitalizations, and Disease Incidence
With a 35 % drop in healthcare costs, a 40 % drop in hospitalisations, and a 50 % drop in disease frequency, water sanitation has the most significant effect. These data show how important clean water is for avoiding infectious diseases like cholera and dysentery, which account for a lot of medical costs, especially in poor areas. Savings of $30 million over the long term show that investment in water infrastructure is good for the economy. Figure 4 shows how the different projects add up to save money on healthcare over the long run.
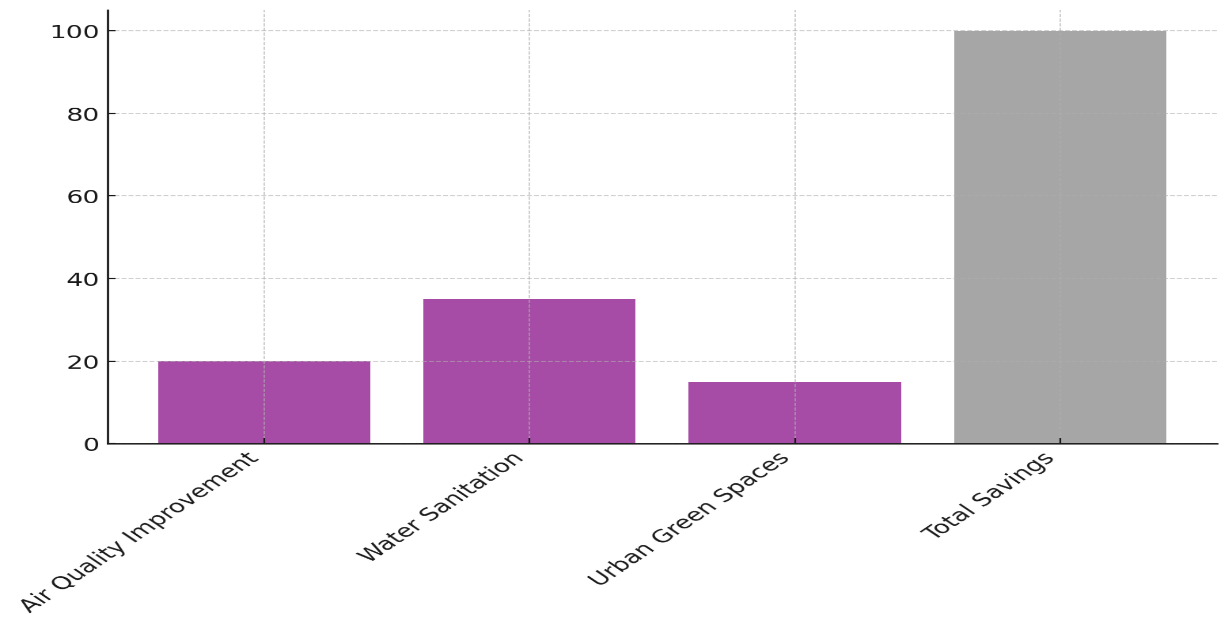
Figure 4. Cumulative Contributions of Initiatives to Total Long-Term Savings
Urban green spaces lower healthcare costs by 15 %, lower the number of hospitalisations by 10 %, and lower the number of diseases that happen by 20 %.
|
Table 3. Impact of Air Quality on Healthcare Expenditures |
||||
|
Region/City |
Air Quality Index (Before) AQI |
Air Quality Index (After) AQI |
Asthma Hospitalizations Reduction (%) |
Healthcare Cost Reduction ($ Million) |
|
City A |
150 |
80 |
25 |
12 |
|
City B |
180 |
90 |
30 |
22 |
|
City C |
140 |
70 |
20 |
10 |
Table 3 shows how much better air quality has affected the cost of health care in different places or regions. The Air Quality Index (AQI) dropped from 150 to 80 in City A.

Figure 5. Comparison of Air Quality Index (Before and After) Across Cities
In figure 5, you can see the difference between the Air Quality Index before and after towns started environmental health programs. This led to a 25 % drop in asthma-related hospitalisations and a $12 million drop in healthcare costs. This increase shows that lowering air pollution directly improves public health by lowering the need for expensive medical treatments for asthma attacks and other breathing problems. Figure 6 shows how better air quality affects the number of people with asthma and how much it costs to treat them.
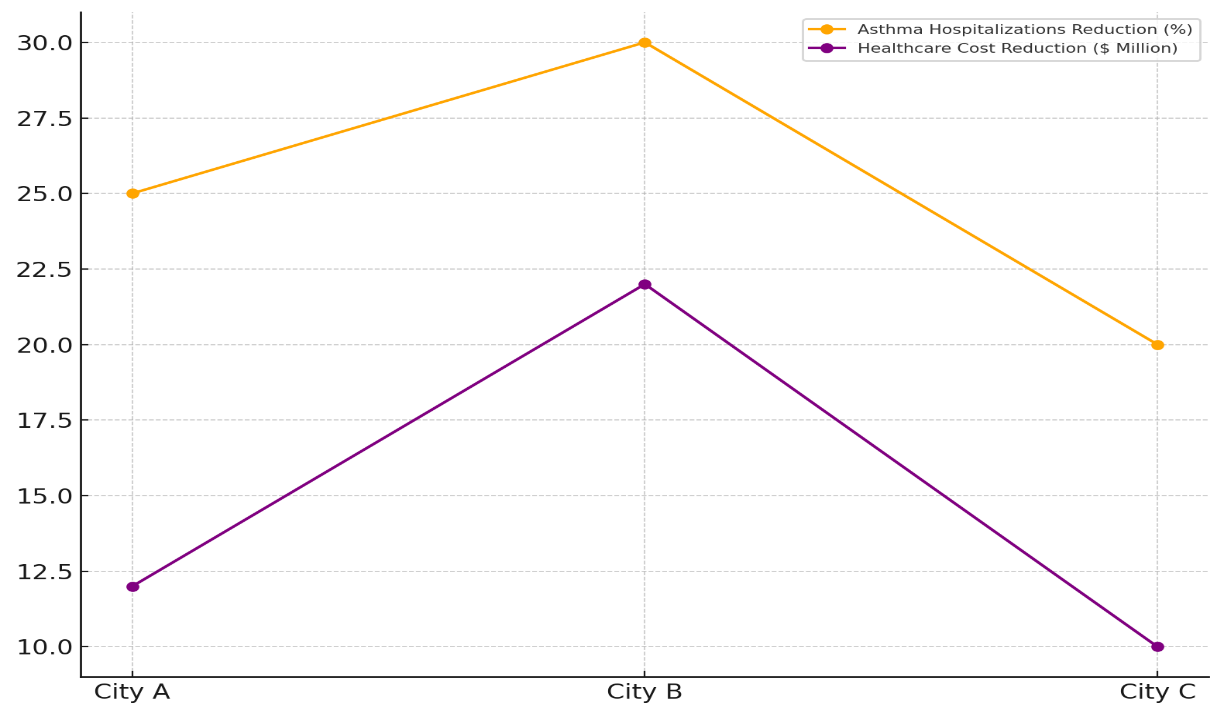
Figure 6. Impact of Air Quality Improvement on Asthma and Healthcare Costs
The AQI dropped from 180 to 90 in City B, which was the best affected. This cut the number of hospitalisations for asthma by 30 % and saved $22 million on healthcare costs. The big gains in air quality probably helped lower the number of asthma attacks and other lung illnesses, which saved a lot of money on hospital and emergency room bills. As the AQI went from 140 to 70 in City C, 20 % fewer people with asthma were hospitalised, which saved $10 million on healthcare costs. The data show that cleaner air does have clear cash benefits, even though the change wasn’t as big as in other places.
CONCLUSION
By getting to the root reasons of many chronic diseases and environmental health risks, environmental health projects are a long-term way to lower healthcare costs. Improving the quality of the air and water, as well as creating open areas in cities, has shown that these projects have a lot of potential to lower healthcare costs in the short and long run. Case studies show that efforts to control air pollution have successfully lowered the number of lung illnesses, which has led to fewer hospital stays and lower treatment costs. In the same way, attempts to clean up water have greatly decreased the number of water-borne diseases, which has saved a lot of money on medical bills. Green areas in cities have not only improved physical health by getting people to move around more, but they have also helped mental health by reducing the number of people who end up in psychiatric hospitals and making people happier and healthier overall. By spending in environmental health, these projects have shown that it not only improves people’s quality of life but also makes healthcare systems more financially stable. But putting these plans into action is hard because of things like government opposition, limited funds, and a lack of general knowledge. For these problems to be solved, states, the business sector, and local groups need to work together, and more money needs to be put into study and public schools. As part of complete healthcare reform plans, policymakers need to put environmental health projects at the top of their lists. This is because fixing the environment is a cost-effective way to improve public health and lower long-term healthcare costs.
REFERENCES
1. Alimi, O.Y.; Ajide, K.B.; Isola, W.A. Environmental quality and health expenditure in ECOWAS. Environ. Dev. Sustain. 2019, 22, 5105–5127
2. Anwar, M.A.; Madni, G.R.; Yasin, I. Environmental quality, forestation, and health expenditure: A cross-country evidence. Environ. Dev. Sustain. 2021, 23, 16454–16480.
3. Narayan, P.K.; Narayan, S. Does environmental quality influence health expenditures? Empirical evidence from a panel of selected OECD countries. Ecol. Econ. 2008, 65, 367–374.
4. Shen, J.-S.; Wang, Q.; Shen, H.-P. Does Industrial Air Pollution Increase Health Care Expenditure? Evidence from China. Front. Public Health 2021, 9, 632.
5. Yahaya, A.; Nor, N.M.; Habibullah, M.S.; Ghani, J.A.; Noor, Z.M. How relevant is environmental quality to per capita health expenditures? Empirical evidence from panel of developing countries. SpringerPlus 2016, 5, 925.
6. Zaman, S.B.; Hossain, N.; Mehta, V.; Sharmin, S.; Mahmood, S.A.I. An association of total health expenditure with GDP and life expectancy. J. Med. Res. Innov. 2017, 1, AU7–AU12.
7. Akca, N.; Sönmez, S.; Yilmaz, A. Determinants of health expenditure in OECD countries: A decision tree model. Pak. J. Med Sci. 2017, 33, 1490–1494.
8. Nghiem, S.H.; Connelly, L.B. Convergence and determinants of health expenditures in OECD countries. Health. Econ. Rev. 2017, 7, 29.
9. Tong, M.X.; Wondmagegn, B.Y.; Williams, S.; Hansen, A.; Dear, K.; Pisaniello, D.; Xiang, J.; Xiao, J.; Jian, L.; Scalley, B.; et al. Hospital healthcare costs attributable to heat and future estimations in the context of climate change in Perth, Western Australia. Adv. Clim. Chang. Res. 2021, 12, 638–648.
10. Wondmagegn, B.Y.; Xiang, J.; Williams, S.; Pisaniello, D.; Bi, P. What do we know about the healthcare costs of extreme heat exposure? A comprehensive literature review. Sci. Total Environ. 2019, 657, 608–618.
11. Churchill, S.A.; Inekwe, J.; Ivanovski, K.; Smyth, R. The Environmental Kuznets Curve in the OECD: 1870–2014. Energy Econ. 2018, 75, 389–399.
12. Destek, M.A.; Sarkodie, S.A. Investigation of environmental Kuznets curve for ecological footprint: The role of energy and financial development. Sci. Total Environ. 2018, 650, 2483–2489.
13. Kim, Y.; Manley, J.; Radoias, V. Medium-and long-term consequences of pollution on labor supply: Evidence from Indonesia. IZA J. Labor Econ. 2017, 6, 1–15.
14. Jitendra Ahirwar, Vinod Kumar Singh, Ratnesh Tiwari . (2016). Textile Antenna for Bluetooth Devices Applications. Advance Physics Letter, 3(3), 13-16
15. Muktikanta Panigrahi, Benorita Prusty, Munesh Chandra Adhikary. (2016). Investigation of electrochemical ccitance of core-shell structured poly (m-Aminophenol) (PmAP)/MoO3 composite. Advance Physics Letter, 3(3), 17-23
16. Bakhsh, K.; Latif, A.; Ali, R.; Yasin, M.A. Relationship between adaptation to climate change and provincial government expenditure in Pakistan. Environ. Sci. Pollut. Res. 2020, 28, 8384–8391.
CONFLICTS OF INTEREST
None.
FINANCING
None.
AUTHORSHIP CONTRIBUTION
Conceptualization: Tukaram Zagade, Aditya Ojha, Debasmita Rath, Ashok Kr Sharma, Sujayaraj Samuel Jayakumar.
Investigation: Tukaram Zagade, Aditya Ojha, Debasmita Rath, Ashok Kr Sharma, Sujayaraj Samuel Jayakumar.
Methodology: Tukaram Zagade, Aditya Ojha, Debasmita Rath, Ashok Kr Sharma, Sujayaraj Samuel Jayakumar.
Writing - original draft: Tukaram Zagade, Aditya Ojha, Debasmita Rath, Ashok Kr Sharma, Sujayaraj Samuel Jayakumar.
Writing - review and editing: Tukaram Zagade, Aditya Ojha, Debasmita Rath, Ashok Kr Sharma, Sujayaraj Samuel Jayakumar.