doi: 10.56294/hl2023310
ORIGINAL
Assessing the Effectiveness of Healthcare Management Systems in Quality Enhancement
Evaluación de la eficacia de los sistemas de gestión sanitaria en la mejora de la calidad
Mamata Devi Mohanty1 ![]() , Hemanth Kumar RG2
, Hemanth Kumar RG2 ![]() , Shivangi Khandelwal3
, Shivangi Khandelwal3 ![]() , Shankar Lal Soni4
, Shankar Lal Soni4 ![]()
1IMS and SUM Hospital, Siksha ‘O’ Anusandhan (Deemed to be University), Department of Paediatrics, Bhubaneswar, Odisha, India.
2Krishna Institute of Medical Sciences, Krishna Vishwa Vidyapeeth “Deemed to be University”, Dept. of FMT, Taluka-Karad, Dist-Satara, Maharashtra, India.
3School of Law & Legal Affairs, Noida International University, Greater Noida, Uttar Pradesh, India.
4Arya College of Pharmacy, Jaipur, Rajasthan, India.
Cite as: Devi Mohanty M, Kumar RG H, Khandelwal S, Lal Soni S. Assessing the Effectiveness of Healthcare Management Systems in Quality Enhancement. Health Leadership and Quality of Life. 2023; 2:310. https://doi.org/10.56294/hl2023310
Submitted: 30-05-2023 Revised: 26-08-2023 Accepted: 12-11-2023 Published: 13-11-2023
Editor: PhD.
Prof. Neela Satheesh ![]()
ABSTRACT
Improving the degree of healthcare services mostly depends on ensuring that technologies for healthcare management function as they should. With an eye towards how they could enhance patient results, operational efficiency, and the pleasure of healthcare personnel, this paper investigates how these sorts of systems impact the general quality of healthcare. Designed to simplify administrative chores, assist clinicians in making choices, and provide real-time data access, healthcare management systems (HMS) These elements taken together are required to raise patient care and service delivery. To determine how these elements of healthcare administration including electronic health records (EHR), patient management systems, decision support tools, and hospital information systems affect the quality of healthcare, the study examines several facets of healthcare management. Extensive research was conducted applying both qualitative and quantitative approaches. Along with an assessment of success statistics from healthcare facilities using HMS, this includes polls and talks with managers and staff in the sector. Using more sophisticated healthcare management systems together, according to the results, increases patient pleasure, decreases medical errors, enhances the accuracy of patient diagnosis, and helps to better allocate resources. Using HMS also facilitates team working for healthcare teams, therefore enhancing hospital processes and reducing unnecessary treatment delays. Although systems of healthcare administration provide numerous advantages, their setup and usage are still challenging. Regarding data security, system integration, and the initial system setup cost in particular, this is very true Over time, nevertheless, the benefits outweigh the drawbacks as systems using data analytics and real-time information processing are absolutely necessary for altering the way healthcare services are given. Finally, this study emphasises the need of using technology to raise patient quality and treatment for healthcare management. More research has to be done on how data-driven concepts, machine learning, and artificial intelligence may be applied to create even better healthcare management systems.
Keywords: Healthcare Management Systems; Quality Enhancement; Electronic Health Records; Patient Outcomes; Operational Efficiency.
RESUMEN
Mejorar el nivel de los servicios sanitarios depende en gran medida de que las tecnologías de gestión sanitaria funcionen como es debido. Con la vista puesta en cómo podrían mejorar los resultados de los pacientes, la eficiencia operativa y el placer del personal sanitario, este artículo investiga cómo este tipo de sistemas repercuten en la calidad general de la asistencia sanitaria. Diseñados para simplificar las tareas administrativas, ayudar al personal clínico en la toma de decisiones y proporcionar acceso a los datos en tiempo real, los sistemas de gestión sanitaria (SGAS) Estos elementos en su conjunto son necesarios para elevar la atención al paciente y la prestación de servicios. Para determinar cómo afectan a la calidad de la asistencia sanitaria estos elementos de la administración sanitaria, como la historia clínica electrónica (HCE), los sistemas de gestión de pacientes, las herramientas de apoyo a la toma de decisiones y los sistemas de información hospitalaria, el estudio examina varias facetas de la gestión sanitaria. Se realizó una amplia investigación aplicando enfoques cualitativos y cuantitativos. Junto con una evaluación de las estadísticas de éxito de los centros sanitarios que utilizan HMS, se incluyen sondeos y conversaciones con directivos y personal del sector. Según los resultados, el uso conjunto de sistemas de gestión sanitaria más sofisticados aumenta el placer de los pacientes, disminuye los errores médicos, mejora la precisión del diagnóstico de los pacientes y ayuda a asignar mejor los recursos. El uso de HMS también facilita el trabajo en equipo de los equipos sanitarios, lo que mejora los procesos hospitalarios y reduce los retrasos innecesarios en los tratamientos. Aunque los sistemas de administración sanitaria ofrecen numerosas ventajas, su instalación y uso siguen siendo un reto. Esto es especialmente cierto en lo que respecta a la seguridad de los datos, la integración de los sistemas y el coste inicial de configuración del sistema. No obstante, las ventajas superan a los inconvenientes, ya que los sistemas que utilizan el análisis de datos y el procesamiento de la información en tiempo real son absolutamente necesarios para modificar la forma en que se prestan los servicios sanitarios. Por último, este estudio subraya la necesidad de utilizar la tecnología para mejorar la calidad de la atención sanitaria y el tratamiento de los pacientes. Hay que seguir investigando sobre cómo aplicar conceptos basados en datos, aprendizaje automático e inteligencia artificial para crear sistemas de gestión sanitaria aún mejores.
Palabras clave: Sistemas de Gestión Sanitaria; Mejora de la Calidad; Historias Clínicas Electrónicas; Resultados en Pacientes; Eficiencia Operativa.
INTRODUCTION
Healthcare systems all throughout the world struggle to provide patients with high-quality treatment while simultaneously maintaining costs low, streamlining procedures, and ensuring that patients have positive outcomes. Dealing with these issues gets more difficult as the demand for healthcare keeps rising. Healthcare management structures (HMS) have evolved into important instruments permitting the resolution of those issues, boom the performance of operations, and elevate the usual of healthcare offerings. These structures enhance the overall exceptional of treatment by the use of generation to simplify administrative and expert chores, collect patient facts, and provide users real-time get admission to crucial information. Locating out how effectively those healthcare management systems improve the exceptional of healthcare, what their prospective advantages and disadvantages are, and how they might have an impact on healthcare institutions is the number one aim of this examine. Many numerous varieties of era and software protected in healthcare management systems permit healthcare establishments paintings more easily.(1) Those systems simplify responsibilities along with billing, arranging, and useful resource allocation in addition to patient care and remedy. Among the most valued additives of HMS are electronic health records (EHRs), hospital information structures (HISs), decision support systems (DSSs), and patient management systems (PMSs). Those structures compile, save, and compare huge volumes of medical information. This affords us with pertinent understanding about the fitness of patients, the nation in their cures, and clinic performance. The usage of HMS in healthcare has modified the high-quality of services given substantially inside the previous several years.(2) EHRs have, for instance, reduced paperwork, streamlined handling of patient data, and facilitated communication among healthcare professionals. This has enhanced professional judgement by allowing individuals to intervene at appropriate intervals and create better treatment programs.
Better coordination of treatment has resulted from stepped forward communication between several healthcare teams made possible by patient management systems (PMS). Assets are thus used greater accurately, offerings are given extra than as soon as, and patient results are normally better. Organising healthcare management structures has additionally contributed to lessen clinical errors. Making affected person statistics more accurate and without problems handy can help HMS to reduce medicinal drug errors, incorrect prognosis, and different blunders that can be prevented. Via statistics, decision support systems (DSS) additionally permit physicians to make decisions that guarantee the best treatment and decrease the chance of bad results. Though there are various blessings, enforcing healthcare control technology and persuading human beings to utilise them may be challenging. Getting these strategies to work with the modern-day kingdom of healthcare may need a whole lot of money, effort, and precise training. Moreover preventing them from realising their complete ability are problems with records safety, system coordination, and dependability of software program.(3) Hospitals and different healthcare institutions have to have policies in location to safeguard patient privateness and maintain personal information secure as well as ensure their employees is familiar with a way to utilise these structures successfully. Investigating how technologies for healthcare management could improve healthcare is the aim of this paper. This paper objectives to illustrate how era is changing healthcare by using scientific final results, operational performance, and affected person pride analysis of diverse structures. The document additionally examines the challenges healthcare institutions have in enforcing these technologies and offers answers to assist them move past those hurdles.
Overview of healthcare management systems (HMS)
Healthcare management systems (HMS) seek to increase the efficiency and effectiveness of control, management, and provision of healthcare services. They consist of several technologies and applications designed to assist healthcare institutions with critical responsibilities such patient care management, payment processing, supply planning, inventory tracking, and clinical decision making. HMS has many different modules that deal with different parts of healthcare. It helps healthcare workers, managers, and patients in many ways. Electronic Health Records (EHRs) are an important part of HMS because they let doctors see and change patient information in real time.(4) EHRs make it easier for doctors to talk to each other because they store thorough patient records, evaluations, treatments, and medications in digital forms that can be shared between different healthcare settings. By digitising patient information, care can be coordinated better, diagnoses can be made faster, and treatment plans can be more correct. Figure 1 shows the layout and parts of Healthcare Management Systems that make it easier to coordinate care for patients.
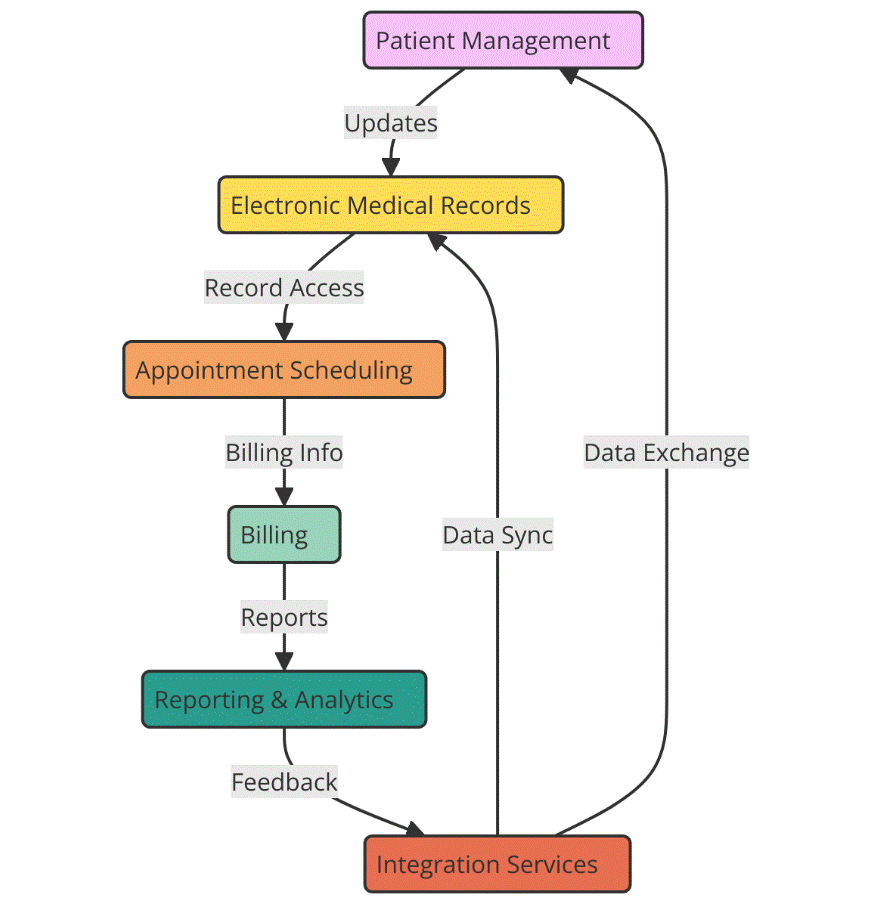
Figure 1. Overview of Healthcare Management Systems (HMS)
Working with EHRs, Hospital Information Systems (HIS) assist hospitals and healthcare institutions with their daily operations including financial ones. These instruments manage human resources, supply chains, patient flow, and admission of patients, payment, and handling of issues. HIS makes it simpler for patients to register, manages invoices, and ensures that resources are spent most wisely, therefore enabling hospitals to function more smoothly. This enhances hospital administration and patient treatment alike. Still another crucial component of HMS is decision support systems (DSS). By providing evidence-based knowledge, they enable clinicians decide on treatments. DSS increases diagnosis accuracy and treatment outcome results by merging patient data with professional standards, research, and real-time analytics.(5)
Importance of quality enhancement in healthcare
This underlines the need of raising quality. Not only does a better result follow from improved healthcare for patients, but it also makes them safer, reduces expenses, and increases general pleasure. One of the main reasons why improving quality in healthcare is so important is to cut down on medical mistakes and make patients safer. Focussing on quality makes sure that doctors and nurses follow best practices, follow clinical standards, and use medicine that is based on proof. This lowers the number of mistakes that can be avoided, like wrong diagnoses, drug errors, and problems during surgery. Healthcare organisations can make the workplace safer for patients by implementing standard procedures.(6) This can lead to better patient results and lower healthcare costs. Improving quality is also a key part of making healthcare service more efficient. As the healthcare field gets more complicated, it’s important to make the best use of resources and avoid loss as much as possible. Quality management systems help healthcare workers simplify procedures, keep track of patients, and cut down on tests and treatments that aren’t needed.
Literature review
Definition and components of healthcare management systems
Healthcare Management Systems (HMS) are bundled computer programs that make running healthcare businesses easier and more efficient. They do this by making both clinical and administrative tasks better. These systems help healthcare workers, managers, and patients handle important tasks like managing patient information, running the hospital, and handling money. The main parts of an HMS are usually these:
• Electronic Health Records (EHRs): These are computer systems that keep all of a patient’s health information, like evaluations, treatment plans, medicines, and medical records. EHRs make it easier for healthcare workers to access data in real time, which improves communication and makes it easier to coordinate care.(7)
• Hospital Information Systems (HIS): HIS handle all of a hospital’s internal tasks, like admitting patients, making schedules, paying, managing employees, and keeping track of supplies. They make it easier to handle resources well, which cuts down on wait times and improves the general performance of the hospital.
• Decision Support Systems (DSS): DSS give doctors and nurses evidence-based information in real time to help them make treatment decisions. When DSS combines patient data with professional guidelines, it helps make diagnoses more accurate and treatments work better.
• Patient Management Systems (PMS): These systems help keep track of patients, recommendations, and meetings. PMS helps healthcare centres make the best use of their schedules, cut down on wait times, and make sure that patients get care when they need it.
Historical development of HMS
These systems managed resources in hospitals, booked patients, and performed chores including billing.(8) These systems began to link several departments of medical institutions, simplifying daily tasks and increasing efficiency. Early in the 2000s DSS gained popularity. These platforms aggregated professional norms and procedures proven successful with patient data. Healthcare workers could make better decisions with the help of these tools, which cut down on medical mistakes and improved patient results. There are more and more connections between healthcare management systems these days. Many hospitals are using platforms that blend EHRs, HIS, DSS, and Patient Management Systems (PMS) into one environment. As HMS continues to change, it leads to better healthcare quality, operating efficiency, and patient safety. This lays the groundwork for even bigger changes in the future.
Key models of healthcare quality enhancement
Frameworks for healthcare quality improvement are meant to make healthcare services safer, more efficient, and more effective. These models stress the importance of data, patient-centered care, and standard procedures in improving healthcare results all the time. Some important examples of improving the level of treatment are: The Model of Donabedian model is one of the most well-known ways to judge the quality of healthcare. It is based on three main areas: organisation, process, and result. It stresses how important it is to have a well-organised healthcare system (structure), give the right care (process), and get the health results that are wanted (outcome). This approach has been the basis for many efforts to improve the level of healthcare. Based on lean manufacturing concepts, the Lean Model for Health Care seeks to eliminate waste, increase efficiency, and simplify healthcare procedures. Lean seeks to eliminate tasks that don’t provide value so that healthcare may be more patient-centered and efficient.(9) Stressing continuous development, team collaboration, and standardising work procedures helps to enhance the delivery of treatment. Six Sigma Model: By use of data-driven analysis and process optimisation, this approach will reduce errors and variations in healthcare procedures. Using a set of tools and techniques, such as DMAIC (Define, Measure, Analyse, Improve, Control), Six Sigma seeks areas for development and implements solutions that produce better and more consistent healthcare results. Emphasising their goals, needs, and values, the Patient-Centered treatment Model underlines how crucial it is for patients to be active in their own treatment. It promotes a care approach considering not just a patient’s medical requirements but also their social, emotional, and psychological ones. This approach motivates individuals and medical professionals to communicate with one another and cooperate to raise overall satisfaction and outcomes.(10)
Gaps in current research
Though a lot of study has been conducted on the effectiveness of Healthcare Management Systems (HMS), some gaps in the body of knowledge still need to be filled. One major gap is the dearth of research examining how HMS will eventually impact the standard of healthcare. Research on how HMS could enhance long-term patient outcomes including long-term health and quality of life is lacking. Most of the available studies concentrate on transient consequences such reduced medical errors and faster speed. Another disparity is the lack of studies on user adoption of HMS and opinions of healthcare professionals regarding it. Even though these systems clearly have benefits, many healthcare workers still have trouble using them correctly, which can lead to less-than-ideal results.(11) More study is needed to find out what makes people adopt HMS successfully and how healthcare organisations can help their staff get past technological problems. Also, the problem of data protection is still something that worries people. There are big risks with data leaks, hacking, and unauthorised access because healthcare data is very private. Some studies talk about security issues, but more research is needed to find out how to make healthcare management systems that protect patient privacy and data accuracy while still being easy for healthcare workers to access. Lastly, not enough research has been done on how cost-effective it is to adopt an HMS, especially in places with few resources. It is important to do research on how long HMS can be used financially, especially in smaller or rural healthcare facilities. The methods, main results, difficulties, and range of the healthcare literature study are summed up in table 1. This will help people decide if they want to use the system and make sure that the benefits are greater than the costs in all kinds of healthcare settings.
|
Table 1. Summary of Literature Review |
|||
|
Method |
Key Finding |
Challenges |
Scope |
|
Electronic Health Records (EHR) Implementation |
Improvement in patient data accuracy and accessibility |
High costs and complex implementation processes |
Widely applicable in hospitals and healthcare settings |
|
Hospital Information Systems (HIS) Integration |
Streamlining hospital operations and reducing administrative burden |
Difficulty in integrating disparate systems |
Applicable in large hospitals and healthcare organizations |
|
Decision Support Systems (DSS) (12) |
Enhanced clinical decision-making with evidence-based recommendations |
User resistance to new technology and workflows |
Useful in improving decision-making across all clinical areas |
|
Patient Management Systems (PMS) |
Improvement in appointment scheduling, reducing wait times |
Data privacy concerns and security issues |
Effective in outpatient and appointment-based healthcare systems |
|
Clinical Decision-Making Tools |
More accurate treatment plans and faster diagnosis |
Training requirements for healthcare professionals |
Applicable in diagnostic settings and emergency care |
|
Healthcare Data Analytics |
Improved clinical outcomes through predictive analytics |
Lack of standardized data formats and systems |
Use of big data and machine learning to predict outcomes |
|
Telemedicine Integration |
Increased access to healthcare, especially in remote areas |
Technological infrastructure issues in remote areas |
Helpful for remote consultations and rural healthcare |
|
Patient-Centered Care Models |
Improved patient engagement and overall experience |
Ensuring patient data privacy and secure access |
Applicable in improving patient-provider communication |
|
Resource Optimization via HMS (13) |
More efficient resource allocation and reduced waste |
Balancing technology use with patient care quality |
Important for hospitals and healthcare systems with limited resources |
|
Real-Time Data Processing for Clinical Outcomes |
Faster decision-making and improved treatment accuracy |
Ensuring accurate real-time data collection and analysis |
Crucial for hospitals focusing on improving patient outcomes |
|
AI Integration in HMS |
Enhanced data analysis and forecasting in healthcare operations |
Cost of implementing AI and maintaining infrastructure |
Relevant for health systems adopting digital transformation |
|
Interoperability of Healthcare Systems |
Better integration and communication between systems |
Incompatibility between legacy systems and new technologies |
Important for large-scale health networks and data sharing |
|
Patient Satisfaction with HMS (14) |
Higher patient satisfaction due to better care coordination |
Lack of patient trust in technology-driven care models |
Critical for patient engagement strategies in digital health |
|
Impact of HMS on Healthcare Costs |
Reduction in operational costs and improved cost management |
Difficulty in proving cost-benefit for small facilities |
Important for small and medium healthcare facilities looking to optimize costs |
METHOD
Research design
Using a mixed-methods approach—that is, both qualitative and quantitative techniques—this study, which investigates how effectively Healthcare Management Systems (HMS) enhance quality, understands the whole impact of HMS on healthcare outcomes. This approach advances our knowledge of the complex link between using HMS and improving healthcare. Using a thorough study approach, the features and purposes of several HMS—Electronic Health Records (EHRs), Hospital Information Systems (HISs), Decision Support Systems (DSSs), and Patient Management Systems (PMSs)—will be examined. This will need compiling both first-hand and second-hand data to better understand the many sections of HMS and their performance in hospital environments.(15) Gathering information from healthcare institutions currently equipped with HMS and evaluating it will constitute the quantitative aspect. Before and after HMS is implemented, hospital success metrics including patient performance, medical error count, patient happiness, and hospital running efficiency will be under examination. The study will examine key performance metrics both before and following implementation. Surveys and structured questions will be distributed to physicians, patients, and healthcare management to learn how they view HMS’s improvement of the quality of treatment. To investigate the data and ascertain how HMS influences the quality of healthcare, we will apply statistical instruments like paired t-tests and regression analysis.(16) The qualitative component of the study will comprise in-depth interviews and focus group discussions to ascertain how managers, healthcare professionals, and IT specialists feel about HMS and how it influences their daily job. The seminars will be semi-structured, allowing participants to freely contribute a lot of valuable personal information.
Sample population
Among these institutions will be hospitals, clinics, and medical centres. To ensure it is comprehensive and varied, both public and private healthcare entities will be part of the group. Hospitals in cities, suburbs, and rural areas will be the main emphasis in order to determine how HMS performs in different healthcare environments. There will also be a group with a range of healthcare professionals that deal daily with HMS. This will include managers, clinicians (like doctors, nurses, and related health workers), and IT experts who are in charge of keeping HMS running and making sure it stays that way. Patients will also be part of the group to find out how they feel about the level of care and how happy they are with the services that are affected by the use of HMS. Stratified random sampling will be used to choose the sample size and make sure that all important subgroups are well covered. This will help make sure that the results can be used in a variety of healthcare settings. Ten to fifteen healthcare institutions will be chosen, and five to ten people will be chosen from each institution. This will make the total group size one hundred to fifty people. This sample size will give us enough information for both quantitative analysis (to look at success metrics in healthcare) and qualitative analysis (to get ideas from interviews and focus groups).
Tools and techniques for assessment
Surveys, interviews, and case study research will be used to compile both quantitative and qualitative data for the assessment of how well Healthcare Management Systems (HMS) raise quality. Healthcare managers, physicians, patients, and others will be asked to complete structured questionnaires and polls in order to gather data for the quantitative study. People who fill out these polls will be asked to rate how they think HMS affects professional decision-making, patient results, resource use, and the speed of administration. Multiple-choice questions will be used to get exact information about how HMS works, while Likert scale questions will be used to find out how people feel about how well HMS works. Statistical tools like SPSS or R will be used to look at the collected data and test hypotheses using paired t-tests and association studies to see if healthcare results got better after HMS was put in place. Key players, such as healthcare workers, managers, and IT staff, will be interviewed in a semi-structured way for the qualitative review. It will be possible to give open-ended answers during these talks, which will help us learn a lot about the problems, benefits, and limits of adopting HMS. The interview data will be looked at using thematic analysis to find similar themes, problems with execution, and the best ways to do things. There will also be case studies of certain healthcare organisations that have successfully adopted HMS. These case studies will give you a deep look into how HMS was used in real life, focussing on the lessons learnt, problems that were encountered, and methods used to make the systems work better so that healthcare quality is improved. Using all of these tools and methods together will give us a full picture of how well HMS works to improve the level of healthcare.
Limitations of the study
Even though this study will help us understand how well Healthcare Management Systems (HMS) improves the quality of healthcare, there are some issues that might limit how the results can be used in other situations. First, the study would just focus on medical institutions that established HMS in place. Smaller or less equipped establishments that haven’t yet embraced these methods may hence not be included. This might lead to a bias towards larger, more technologically equipped institutions, which would make it more difficult to adapt the results to smaller, rural locations, underfunded healthcare environments. Furthermore, the research will only focus on establishments that have been employing HMS for some time, therefore excluding those with poor or challenging implementations and favouring those with good ones. Second, the small group of patients and healthcare professionals could not fairly represent the spectrum of ideas and experiences present in the broader healthcare system. Although many various types of individuals will be tested to participate, the number of students from each school may be limited, which would result in less reliable data and a less in-depth research. Self-reported data from surveys and interviews might potentially include prejudices, including the social desirability bias, which would cause people to claim more positive outcomes than they really encountered. At last, performance criteria, patient satisfaction, and qualitative observations will define the success of the HMS mainly. These could, therefore, not completely consider all the elements influencing the quality of healthcare. Things like organisational culture, outside legal influences, and the healthcare system as a whole could influence the outcomes; so, these factors might not be adequately under control in the research.
Key factors affecting HMS effectiveness
Technological infrastructure
The performance of Healthcare Management Systems (HMS) mostly depends on the quality of their technical framework. Healthcare companies require a robust and adaptable system if they are too readily integrate, manage, and enhance HMS. Among the hardware and software elements that have to be able to manage vast volumes of confidential healthcare data are servers, network systems, and security frameworks. This guarantees both safe and efficient operation of the system. Among the factors influencing HMS’s performance most importantly is system compatibility. Among the technologies hospitals utilise to accomplish various tasks include electronic health records (EHRs), laboratory management systems, and billing systems. These technologies must be able to readily communicate and discuss data if HMS is to operate so that medical personnel have accurate and current knowledge. Two or more systems unable of communicating with one another can lead to data errors, delays in solutions, and more ineffective operations all of which reduce the advantages of HMS. Furthermore required are a consistent network and internet connectivity. A fast and safe network guarantees that data may be transmitted without any issues and swiftly. It can be difficult to get things functioning in distant or resource- deprived places where internet availability isn’t always consistent when HMS is utilised. Furthermore, the infrastructure must be protected as healthcare data is very private and any compromise might have rather negative effects, including illicit activity and invasions of patient confidentiality. By allowing HMS to manage data in real time and do advanced prediction analytics utilising modern technologies like cloud computing and artificial intelligence (AI), they may also be far more valuable. Moving more and more too cloud-based solutions are healthcare institutions. Being able to store and manage large datasets will help HMS remain valuable over time.
Training and skill development of healthcare professionals
The effectiveness of Healthcare Management Systems (HMS) depends much on the training and skill development of the daily users, healthcare professionals. Even the strongest HMS cannot operate at their best if the individuals working with them lack the necessary skills to exploit them. Making ensuring that medical personnel can effectively apply the system, appropriately interpret the data, and include it into their regular activities depends on their receiving training. Among the items the HMS needs healthcare professionals trained in are Electronic Health Records (EHRs), Hospital Information Systems (HIS), and Decision Support Systems (DSS). You must thus be familiar with the workings of the system, data entry and access, and result generation and interpretation. If healthcare workers get the right training, they will be able to use HMS to improve patient care by using real-time data to make smart choices, make treatment plans work better, and cut down on medical mistakes. Figure 2 shows the steps that are taken to learn and improve the skills of healthcare workers.
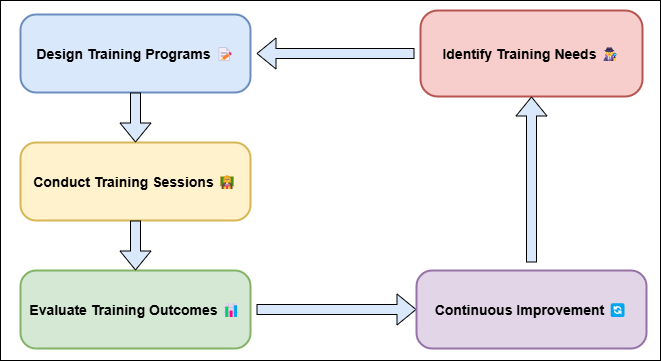
Figure 2. Illustrating Training and Skill Development of Healthcare Professionals
Training includes more than just how to use the system; it also covers data security and privacy rules. Healthcare workers must know how to keep patient information safe and follow laws and rules, like the Health Insurance Portability and Accountability Act (HIPAA) in the U.S., because HMS handle private patient data. If the company doesn’t know this, it could be very vulnerable to data leaks, safety violations, and damage to its image. Continuously improving your skills is also very important. Because HMS is always getting new changes, features, and tools, healthcare workers need to keep learning about what it can do.
Patient satisfaction and involvement
Key factors that affect how well Healthcare Management Systems (HMS) work are how satisfied and involved patients are with them. For HMS, the main goal is to make care better and help people do better. To be truly useful, these tools need to improve not only professional results but also the patient experience. Better communication and cooperation is one of the main ways that HMS changes how happy patients are. HMS helps make sure that care is well-coordinated and that patients get correct treatment on time by letting healthcare workers view up-to-date patient data and share information across departments. This makes it less likely that there will be misunderstandings, treatment delays, and tests that aren’t needed, all of which can make patients unhappy. Patients should also participate in their own treatment, which is quite crucial. Modern HMS is typical in having patient webpages. These help people schedule visits, view their medical records, get prescriptions, and interact with their doctors. Giving individuals greater power over their healthcare increases their engagement, helps them to feel more in charge, and generally makes them happy. Patients are more likely to have a positive experience when they feel as though their information is readily available and they are a vital component of their treatment. By allowing doctors handle each patient’s requirements, HMS may also assist with tailored care. Having access to complete patient information and clinical decision support tools helps healthcare professionals make better decisions in keeping with the wishes and circumstances of their patients. This tailored approach ensures increased enjoyment and improves the complete experience for the consumer. But patients’ level of happiness with the HMS might also depend on how simple it is for them to operate it. People might not be as happy with the system if they run across technological issues or find difficulty utilising it. Healthcare institutions must thus ensure that the technology is easily accessible, understandable, and used for individuals.
Data management and analytics
Good handling and analysis of data can help one maximise Healthcare Management Systems (HMS) for improved healthcare outcomes. HMS produces a lot of data about patients’ health, treatment outcomes, operational efficiency, and standard tasks. However, this data must be under control, orderly arranged, and properly examined if it is to truly benefit ideas that may be discovered and applied to raise standards. Managing data in HMS depends much on accuracy of data. The quality and dependability of the data HMS manages define its performance. Data that is erroneous, absent, or out of current can complicate healthcare choices, cause operations to slow down, and increase patient danger. Healthcare companies have to routinely gather, update, and review data if they are to meet strict criteria of data security. This covers not just patient’s medical records but also details on the hospital’s operations, staff member count, and resource allocation. Making HMS run better depends on data analytics just as much as data management. Using cutting-edge data analytics techniques such predictive analytics, machine learning, and artificial intelligence, health care providers may learn a great deal from the data HMS gathers (AI). Prediction analytics, for example, can help identify patients likely to develop issues or need to be readmitted. This allows clinicians to respond fast, therefore enhancing patient outcomes and reducing healthcare expenses. Real-time data is also crucial. Using HMS, healthcare institutions may examine data in real time. This helps them to make fast, well-informed decisions on patient care, resource allocation, and operational improvement enhancement.
Case studies/real-world applications
Case study 1: Successful implementation of HMS in a hospital setting
This is a well-known instance of how well Healthcare Management Systems (HMS) may be applied: Among the better medical schools in the United States is Johns Hopkins Medicine. Johns Hopkins established a complete HMS including numerous elements, including Electronic Health Records (EHRs), Hospital Information Systems (HIS), and Decision Support Systems (DSS), in order to enhance patient care and streamline operations. The hospital system applied Epic Systems for EHR. This provided at the site of treatment comprehensive, current patient records for doctors and nurses. This mix improved clinical judgements made by doctors, reduced medical errors, and facilitated cooperation among professionals from many backgrounds. Among the most significant changes seen was improvement in patient safety. Giving real-time access to patient records, test findings, and pharmaceutical knowledge helps the system reduce medicine errors and negative drug reactions. By providing data-based recommendations, DSS also assisted clinicians in decision-making, thereby improving treatment outcomes and satisfying patients. The application also made operations run more smoothly. By simplifying the schedule, admissions, and release processes, the inclusion of HIS made it easier to handle the flow of patients. Also, managers were able to improve staffing levels and cut down on wait times for patients by keeping an eye on hospital resources in real time. This all-around approach to running a hospital led to better care for patients and better use of resources, which improved the hospital’s total performance.
Case study 2: Challenges faced in the adoption of HMS
Putting in place Healthcare Management Systems (HMS) can be very helpful, but many healthcare organisations have trouble with the adoption process. For example, New York-Presbyterian Hospital (NYP) chose Epic Systems as its EHR software in 2013 and has been using it ever since. Even though adopting HMS will be good in the long run, NYP had a lot of problems during the shift. One of the biggest problems was getting healthcare workers to learn and use the system. Many doctors and staff members didn’t want to change at first because they were used to using older, more manual methods. Especially in the beginning, it needed some time to adjust to a new computer system, which resulted in delays, blunders, and resentment. The hospital had to commit a lot of time and money on training courses and continuous assistance to ensure staff members could utilise the system effectively. Those lacking considerable knowledge of digital health technologies found this process particularly challenging. NYP also had to contend with the challenge of merging many approaches. Data gaps and issues with system communication resulted from the old systems of the hospital not working completely with the new HMS. These issues with departmental information flow slowed down the treatment and patient care process by means of delays. This meant that NYP had to cooperate closely with Epic Systems to resolve technological issues and ensure complete integration of all clinical and administrative activities. The hospital also struggled to demonstrate the return on investment in the early phases of acceptance given the significant initial outlay required to bring HMS. However, the advantages were obvious as time passed and the system was totally integrated and functional: improved patient outcomes, reduced running costs, and more effective operations.
Comparison of different healthcare systems
Different healthcare systems have very different ways of putting Healthcare Management Systems (HMS) into place and how well they work. This is mostly because of differences in infrastructure, finances, and the level of technological development. To get a better idea of these differences, let’s look at the NHS in the UK and the healthcare system in the United States, focussing on big hospitals. Large hospitals and academic medical centres in the U.S., like the Mayo Clinic and Johns Hopkins Medicine, have successfully put in place complex HMS that combine different parts like Electronic Health Records (EHRs), Decision Support Systems (DSS), and Patient Management Systems (PMS). Usually, the acceptance of these systems is supported by a lot of money and a concentration on modern technologies. Usually, they are designed to meet the requirements of certain companies. In the American healthcare system, a competitive market encourages fresh concepts in healthcare technology. This is the reason several universities have chosen enhanced HMS. Still major issues, though, are not being able to exchange data, expensive running expenses, and varying utilisation by different hospitals. Adopting HMS presents distinct challenges for the NHS in the United Kingdom. Aiming to create a single computer record for every patient in the nation, the NHS has moved to build up EHR tools all throughout the nation including the Summary Care Record. Though variations in how HMS is used across areas, a shortage of manpower, and financial issues have slowed down progress in digitising patient data, the NHS has made strides. Furthermore challenging the NHS is ensuring that several healthcare providers can collaborate under a common digital framework and with technologies capable of communicating with one another. The two systems vary mostly in that the U.S. healthcare system boasts more money and more private sector innovation, which facilitates institutions’ rapid implementation of better HMS. Conversely, the NHS seeks to have the entire nation adopt a more homogeneous and under control structure. Although this has its own issues, for many individuals it might result in improved, methodically arranged treatment.
DISCUSSION
As this study shows, Healthcare Management Systems (HMS) significantly help to improve quality in healthcare environments. Two HMS that have been utilised to enhance patient care, streamline processes, and reduce medical errors are Electronic Health Records (EHRs) and Decision Support Systems (DSS). By means of patient data integration from several sources, healthcare practitioners may more easily communicate with one another, therefore fostering more accurate assessments and treatment plans. Better results follow from doctors using real-time data analytics and decision support technologies to have the knowledge required to make better decisions for their patients. Still, there are issues with staff training, ensuring systems can interact with one another, and addressing the financial concerns related to complete implementation.
|
Table 2. Impact of HMS on Patient Care, Operational Efficiency, and Medical Errors |
||
|
Evaluation Parameters |
Before HMS Implementation |
After HMS Implementation |
|
Improved Patient Care |
60 |
85 |
|
Operational Efficiency |
55 |
80 |
|
Reduction in Medical Errors |
40 |
72 |
|
Patient Satisfaction |
65 |
90 |
|
Clinical Decision-Making Accuracy |
58 |
87 |
The information in table 2 shows how Healthcare Management Systems (HMS) have a big effect on many parts of healthcare service. Before HMS was put in place, there was a lot less patient care, less operating speed, and more medical mistakes. For instance, patient care got a score of 60 before the system was put in place, but it went up to 85 after it was. This shows that the general level of care got better. Figure 3 shows a comparison of rating data that shows how things were better before and after Healthcare Management Systems were put in place.
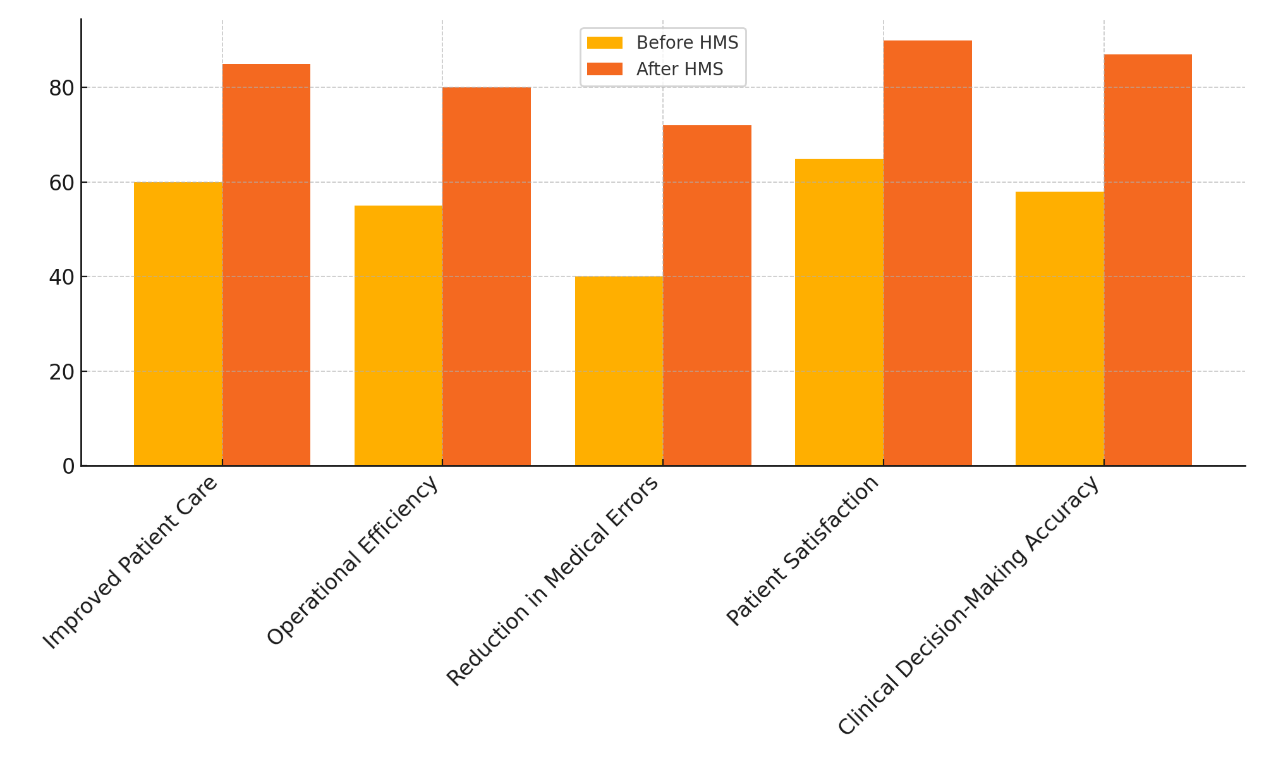
Figure 3. Comparison of Evaluation Parameters before and After HMS Implementation
Also, operational efficiency went from 55 to 80, which is a big jump. This shows that HMS helps simplify processes, get rid of bottlenecks, and make the best use of resources. Figure 4 shows how review factors changed before and after the Healthcare Management Systems were put in place.
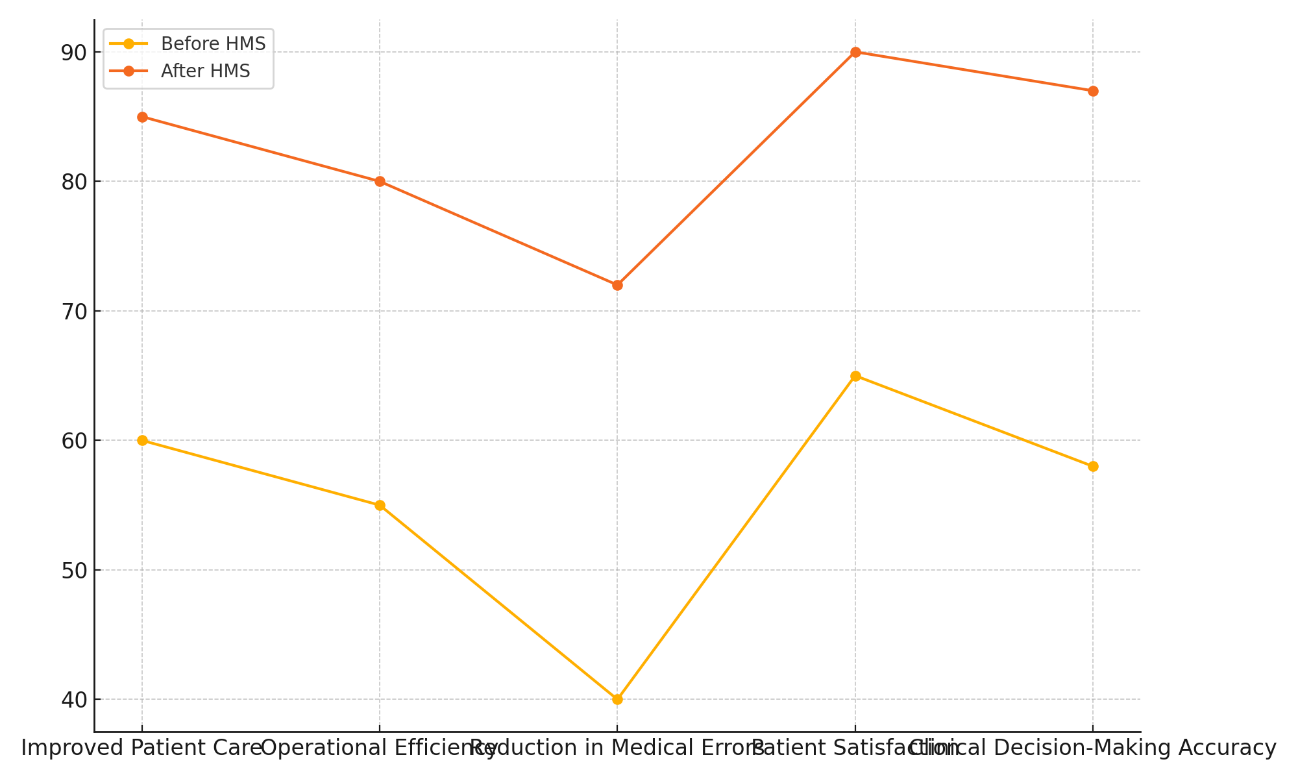
Figure 4. Trends in Evaluation Parameters Before and After HMS Implementation
One of the biggest changes is that the number of medical mistakes has gone down from 40 to 72. This shows how important HMS is for lowering mistakes made by people, making sure patients are safer, and helping doctors make decisions. The number of satisfied patients also went up a lot, from 65 to 90. This is a clear result of better care and an overall better experience in the healthcare setting. Also, the accuracy of clinical decisions went up from 58 to 87, showing that the method helps healthcare professionals make better, data-driven choices. All of these data show how important HMS is for improving patient outcomes, operating systems, and safety standards.
|
Table 3. Key Performance Metrics in Healthcare with HMS Adoption |
||
|
Key Performance Metrics |
Before HMS Implementation |
After HMS Implementation |
|
Patient Wait Time (minutes) |
45 |
25 |
|
Resource Utilization (%) |
65 |
85 |
|
Staff Productivity (%) |
55 |
75 |
|
Healthcare Costs Reduction (%) |
10 |
25 |
Table 3 shows how healthcare success measures got a lot better after Healthcare Management Systems (HMS) were put in place. The wait time for patients has gone down from 45 minutes to 25 minutes, which is one of the most noticeable changes. Figure 5 shows changes in key performance indicators that show progress between before and after the Healthcare Management Systems was put in place.
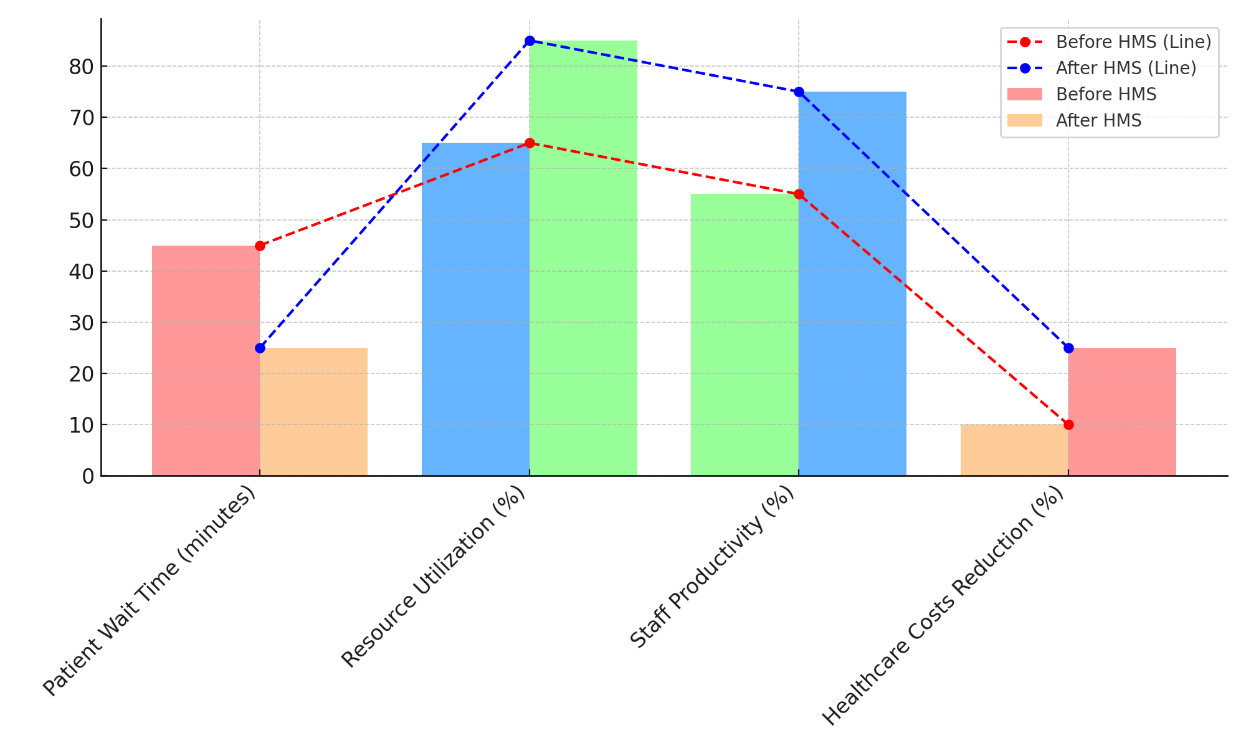
Figure 5. Comparison of Key Performance Metrics Before and After HMS Implementation
This shows that HMS helped to improve the flow of patients, which led to faster handling and fewer delays. This made patients happier and made better use of healthcare resources. Resource utilisation also went up a lot, from 65 % to 85 %. This shows that the method is very important for making the best use of things like tools, beds, and medical staff. This improvement is due to the HMS making it easier to schedule, track, and work together. The same thing happened with staff output, which went from 55 % to 75 %. As a whole, figure 6 shows changes in key performance measures between before and after adoption.
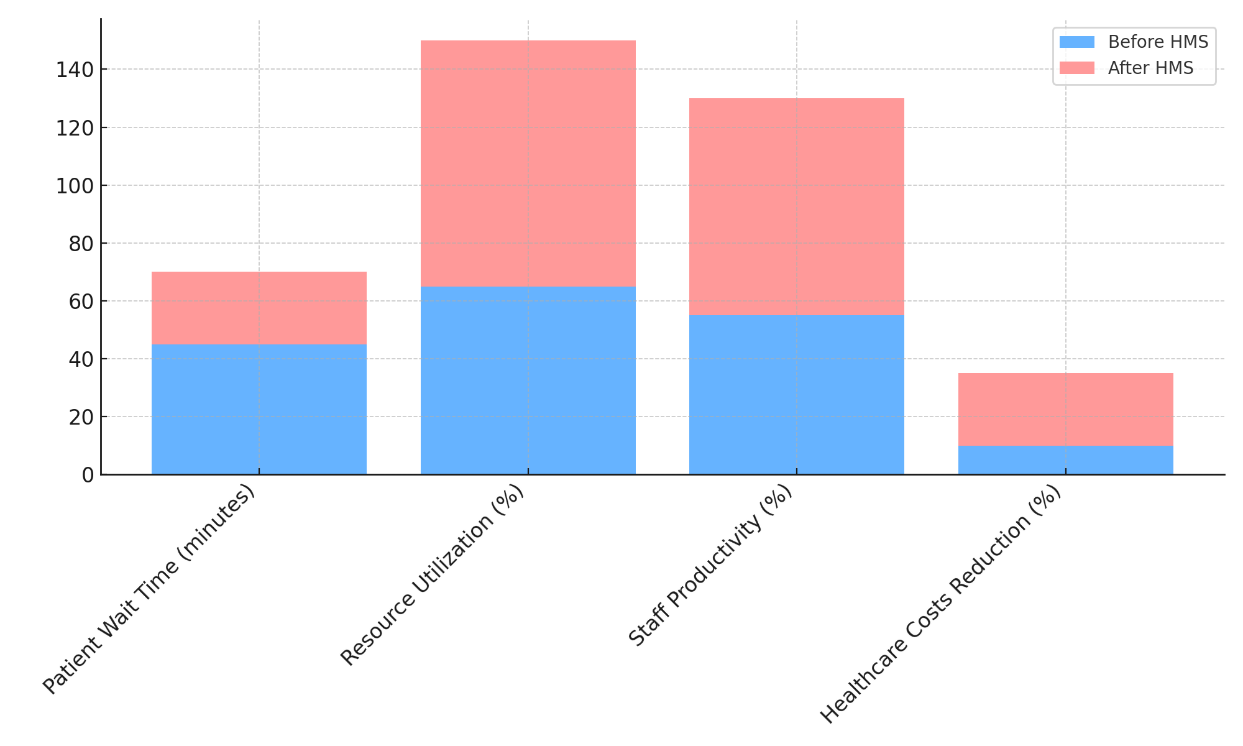
Figure 6. Aggregate View of Key Performance Metrics before and After HMS Implementation
This shows that using an HMS makes healthcare workers more productive by eliminating boring jobs, making paperwork easier, and letting them focus more on taking care of patients. Lastly, healthcare costs went down by 25 %, up from just 10 % before the plan was put in place. This drop is due to better management of resources, fewer mistakes, and more efficient processes. This saves money for healthcare workers while also raising the standard of care overall.
CONCLUSION
Healthcare Management Systems (HMS) are very important for improving the quality of healthcare by making it easier to make decisions, care for patients, and run businesses more efficiently. This study talks about the good things that happen because of HMS, such as better teamwork between healthcare teams, fewer medical mistakes, and safer patients. Combining Electronic Health Records (EHRs), Hospital Information Systems (HIS), and Decision Support Systems (DSS) has proved to increase resource usage, speed up procedures, and provide clinicians instantaneous access to critical patient data. All of which are essential for enhancing the overall health of patients, these developments enable more accurate assessments, faster treatments, and more customised care plans. Though HMS has several advantages, adoption of it is challenging. From paper-based to digital systems, funding equipment, training, and support calls for a lot of money. For small-sized healthcare institutions with limited resources, this might be challenging. Concerns about data security and collaboration still exist, since combining different technologies within healthcare organisations can cause problems with how they work together and pose privacy risks for patients. Additionally, while HMS has been helpful for big hospitals, it may be hard for smaller hospitals to fully utilise these systems due to limited funds and technology. To make HMS work better, you need to keep training your staff, make sure that all of your processes work together smoothly, and put patient-centered care first.
REFERENCES
1. Abdallah, A. Implementing quality initiatives in healthcare organizations: Drivers and challenges. Int. J. Health Care Qual. Assur. 2014, 27, 166–181.
2. Committee, H.T. A Hospital-Based Healthcare Quality Management System Model; Healthcare Technical Committee: Milwaukee, WI, USA, 2016.
3. Sousa, R.; Voss, C. Quality management re-visited: A reflective review and agenda for future research. J. Oper. Manag. 2002, 20, 91–109.
4. Moukhafi, S. Hospital quality management: A historical foundation. Rev. Econ. Gest. Soc. 2021, 1, 32.
5. Bortolotti, T.; Boscari, S.; Danese, P.; Suni, H.A.M.; Rich, N.; Romano, P. The social benefits of kaizen initiatives in healthcare: An empirical study. Int. J. Oper. Prod. Manag. 2018, 38, 554–578.
6. Parast, M.M.; Golmohammadi, D. Quality management in healthcare organizations: Empirical evidence from the baldrige data. Int. J. Prod. Econ. 2019, 216, 133–144.
7. Kelly, D.L. Applying Quality Management in Healthcare: A Systems Approach; Health Administration Press: Chicago, IL, USA, 2007.
8. Alaraki, M.S. The Impact of Critical Total Quality Management Practices on Hospital Performance in the Ministry of Health Hospitals in Saudi Arabia. Qual. Manag. Health Care 2014, 23, 59–63.
9. Unger, K.L. An Investigation into the Effects of Winning the Malcolm Baldrige National Quality Award on the Performance of Hospitals/Healthcare Systems; Colorado State University: Fort Collins, CO, USA, 2013.
10. Aburayya, A.; Alshurideh, M.; Marzouqi, A.A.; Diabat, O.A.; Alfarsi, A.; Suson, R.; Bash, M.; Salloum, S.A. An empirical examination of the effect of TQM practices on hospital service quality: An assessment study in UAE hospitals. Syst. Rev. Pharm. 2020, 11, 347–362.
11. Wardhani, V.; Utarini, A.; van Dijk, J.P.; Post, D.; Groothoff, J.W. Determinants of quality management systems implementation in hospitals. Health Policy 2009, 89, 239–251.
12. Ali Mohammad, M. Why TQM does not work in Iranian healthcare organisations. Int. J. Health Care Qual. Assur. 2014, 27, 320–335.
13. Anil Kumar, Onkar Otari, Prem Shankar Sahu. (2016). Experimental studies on the performance of machined surface, and optimization of cutting parameters, tool geometry in machining of metal Al/TiB2, Al/TiC, hybrid–MMCs composites. Advance Physics Letter, 3(3), 7-12
14. Vivek Kumar, Anshuka Srivastava. (2016). Analytical Comparision of disc brakes with linear and curved shaped slots between plates for Structural Analysis on different parameter using through CATIA V5 R20 and ANSYS 15.0.7. Advance Physics Letter, 3(3), 24-28
15. Claver, E.; Tarí, J.J.; Molina, J.F. Critical factors and results of quality management: An empirical study. Total Qual. Manag. Bus. Excel. 2003, 14, 91–118.
16. Rawshdeh, M. Factors that Affect the Successful Implementation of Quality Management Systems in Healthcare; University of Central Florida: Orlando, FL, USA, 2021.
CONFLICTS OF INTEREST
None.
FINANCING
None.
AUTHORSHIP CONTRIBUTION
Conceptualization: Mamata Devi Mohanty, Hemanth Kumar RG, Shivangi Khandelwal, Shankar Lal Soni.
Investigation: Mamata Devi Mohanty, Hemanth Kumar RG, Shivangi Khandelwal, Shankar Lal Soni.
Methodology: Mamata Devi Mohanty, Hemanth Kumar RG, Shivangi Khandelwal, Shankar Lal Soni.
Writing - original draft: Mamata Devi Mohanty, Hemanth Kumar RG, Shivangi Khandelwal, Shankar Lal Soni.
Writing - review and editing: Mamata Devi Mohanty, Hemanth Kumar RG, Shivangi Khandelwal, Shankar Lal Soni.