doi: 10.56294/hl2023309
ORIGINAL
Correlations Between Occupational Health and Safety Initiatives and Healthcare Operational Efficiency
Correlación entre las iniciativas de salud y seguridad en el trabajo y la eficiencia operativa de la asistencia sanitaria
Swati Duggal1 ![]() , Ayaskanta Singh2
, Ayaskanta Singh2 ![]() , Ram Garg3
, Ram Garg3 ![]() , M. M. Thorat4
, M. M. Thorat4 ![]()
1School of Law & Legal Affairs, Noida International University. Greater Noida, Uttar Pradesh, India.
2IMS and SUM Hospital, Siksha ‘O’ Anusandhan (Deemed to be University), Department of Gastroenterology. Bhubaneswar, Odisha, India.
3Arya College of Pharmacy, Jaipur, Rajasthan, India.
4Krishna Institute of Medical Sciences, Krishna Vishwa Vidyapeeth “Deemed to be University”, Dept. of Anatomy. Taluka-Karad, Dist-Satara, Maharashtra, India.
Cite as: Duggal S, Singh A, Garg R, Thorat M.M. Correlations Between Occupational Health and Safety Initiatives and Healthcare Operational Efficiency. Health Leadership and Quality of Life. 2023; 2:309. https://doi.org/10.56294/hl2023309
Submitted: 31-05-2023 Revised: 27-08-2023 Accepted: 12-11-2023 Published: 13-11-2023
Editor: PhD.
Prof. Neela Satheesh ![]()
ABSTRACT
The paper is to investigate how well healthcare institutions function and if health and safety at work (OHS) initiatives correlate. Healthcare systems all over are under more and more pressure to raise performance, lower expenses, and enhance service quality. This makes it essential to investigate how programs for occupational health and safety may assist to raise the general effectiveness of healthcare operations. Given the very demanding nature of healthcare environments, OHS programs are supposed to safeguard the health and safety of healthcare professionals. Still, their influence beyond worker protection and is rather crucial in determining the degree of organisational performance. Many studies were conducted at many different healthcare institutions with rigorous OHS policies. The research examined topics like staff efficiency, patient satisfaction, cost-effectiveness, and absence rates using quantitative approaches. The research used statistical analysis to establish clear relationships between implementing OHS procedures and improving the practical outcomes in the healthcare sector. Particularly improved safety and health for employees have been connected to lower absenteeism, less accidents on the workplace, and increased staff contentment. Since a healthier workforce leads in improved patient outcomes, shorter wait times, and more effective treatment procedures, these developments directly affect healthcare services. The findings reveal that operating efficiency of healthcare institutions that give health and safety top priority is probably superior. The connection between the two emphasises the need of including health and safety guidelines into healthcare management strategies not just to meet the regulations but also to enhance the way things run. The research also emphasises the requirement of OHS programs in ongoing assessment and adaptation to meet evolving healthcare demands.
Keywords: Occupational Health and Safety; Healthcare Efficiency; Workforce Well-Being; Patient Outcomes; Operational Performance.
RESUMEN
El objetivo de este artículo es investigar el funcionamiento de las instituciones sanitarias y su correlación con las iniciativas de salud y seguridad en el trabajo (SST). Los sistemas sanitarios de todo el mundo están sometidos a una presión cada vez mayor para aumentar su rendimiento, reducir los gastos y mejorar la calidad de los servicios. Por eso es esencial investigar cómo pueden ayudar los programas de salud y seguridad en el trabajo a aumentar la eficacia general de las operaciones sanitarias. Dada la naturaleza tan exigente de los entornos sanitarios, se supone que los programas de salud y seguridad en el trabajo salvaguardan la salud y la seguridad de los profesionales sanitarios. Sin embargo, su influencia va más allá de la protección de los trabajadores y es más bien crucial para determinar el grado de rendimiento de la organización. Se han realizado muchos estudios en diferentes instituciones sanitarias con políticas rigurosas de salud y seguridad en el trabajo. Las investigaciones examinaron temas como la eficiencia del personal, la satisfacción de los pacientes, la rentabilidad y los índices de absentismo mediante enfoques cuantitativos. La investigación utilizó análisis estadísticos para establecer relaciones claras entre la aplicación de procedimientos de salud y seguridad en el trabajo y la mejora de los resultados prácticos en el sector sanitario. En particular, la mejora de la seguridad y la salud de los empleados se ha relacionado con un menor absentismo, menos accidentes en el lugar de trabajo y una mayor satisfacción del personal. Dado que una mano de obra más sana se traduce en mejores resultados para los pacientes, tiempos de espera más cortos y procedimientos de tratamiento más eficaces, estos avances afectan directamente a los servicios sanitarios. Los resultados revelan que la eficiencia operativa de las instituciones sanitarias que dan la máxima prioridad a la salud y la seguridad es probablemente superior. La conexión entre ambas subraya la necesidad de incluir directrices de salud y seguridad en las estrategias de gestión sanitaria, no sólo para cumplir la normativa, sino también para mejorar el funcionamiento. La investigación también hace hincapié en la necesidad de que los programas de salud y seguridad en el trabajo se evalúen y adapten continuamente para satisfacer las cambiantes demandas de la atención sanitaria.
Palabras clave: Salud y Seguridad en el Trabajo; Eficiencia Sanitaria; Bienestar de los Trabajadores; Resultados para los Pacientes; Rendimiento Operativo.
INTRODUCTION
Operating efficiency is rather crucial in the healthcare sector for many reasons, including improved patient care, low cost control, optimal use of resources, and organisational ability to remain open. More and more individuals are understanding as the pressures on healthcare systems across the globe grow that we must consider a broad spectrum of elements, including the health and safety of healthcare professionals, if we are to raise business performance. Long-standing knowledge is that preventing accidents and diseases at work calls for occupational health and safety (OHS) focused initiatives. These initiatives seek to improve workers' health and enhance the surroundings of companies. More study is needed, nevertheless, about their larger influence on the pace of healthcare processes. Particularly those that operate in high-stress environments like hospitals and emergency rooms, healthcare professionals run several hazards on the job. These can include getting hurt, being exposed to diseases, feeling stressed out, or getting burned out. These risks are common, which often means bad things happen, like more people not showing up for work, less work getting done, and more people leaving their jobs, all of which can make healthcare less efficient overall. With healthcare getting more complicated, it's more important than ever to have a better, more motivated staff. So, healthcare managers and lawmakers who want to improve both staff well-being and the success of their organisations need to learn more about how health and safety programs at work affect the speed of healthcare operations. There are several ways to look at the connection between OHS programs and how well operations run. On the one hand, OHS programs that work directly reduce the number and intensity of accidents, sickness, and injuries that happen at work. This, in turn, cuts down on absences and makes it easier to keep employees.
On the other hand, OHS programs can boost employee happiness and job satisfaction by making the workplace safer and friendlier. These help to maintain good performance and production. Happy and healthy employees are more likely to be involved in their job, exhibit greater loyalty, and assist the business to achieve its objectives. Furthermore included in the operational efficiency of healthcare institutions are factors beyond just workforce count. It covers also the degree of patient care received. Studies have shown that when healthcare professionals experience less health issues or accidents, they can provide better treatment. Patients therefore get better treatment and waiting times are reduced.(1) Emphasising OHS will also enable businesses to better utilise their resources, reduce downtime, and streamline their procedures—all of which increase efficiency and save costs. Ultimately, OHS initiatives are not apart from the bigger objective of enabling more effective running of healthcare environments. OHS programs are growing in significance, although little genuine research examining the direct relationship between these initiatives and the pragmatic efficiency of healthcare exists. Although several studies have examined how OHS influences staff performance or patient outcomes on its own, there is no evidence linking the two in the framework of healthcare management.(2) By investigating how health and safety initiatives at businesses impact several operational variables in healthcare environments, including staff efficiency, patient contentment, absence rates, and the overall cost-effectiveness of the setting, this paper seeks to close that gap. The outcomes will provide healthcare companies with practical knowledge on how to use OHS initiatives to enhance not just worker safety but also corporate performance.
Background on Occupational Health and Safety (OHS)
Occupational health and safety (OHS) is the body of guidelines, procedures, and policies meant to safeguard workers' social, psychological, and physical health at their place of employment. OHS programs are supposed to handle the particular hazards associated with working in a medical environment in healthcare environments. Workers could, for instance, get infectious infections, sustain injuries when moving and carrying patients, and experience stress from a heavy schedule and handling of emotional demands. These hazards compromise not just workers' health but also their ability to do their jobs effectively. For this reason, the health of medical personnel depends much on OHS initiatives. Early in the 20th century, growing awareness of health and safety issues in the workplace drove the concept of OHS.(3) Governments, companies, and healthcare organisations have throughout time established policies, regulations, and recommendations to prevent illness or injury among their population. Globally, the World Health Organisation (WHO) and the International Labour Organisation (ILO) have greatly helped to advance health standards at businesses. OHS programs often aim to prevent workers from being injured on the job, reduce stress and burnout, ensure that workstations are set up appropriately, and manage the hazards that accompany being near to biological, chemical, and physical hazards in the healthcare industry. People who work in healthcare, like doctors, nurses, techs, and support staff, often have to deal with a lot of stress and are subject to risks that can cause long-term health issues.
Importance of healthcare operational efficiency
Healthcare operating efficiency means that healthcare organisations can make the best use of their resources, cut down on waste, and give patients high-quality care quickly and cheaply. Healthcare needs to be more operationally efficient to improve patient results, cut down on wait times, and keep costs down, especially now when demand for services is rising and budgets are getting tighter. To be operationally efficient, healthcare service must be optimised at all levels, from taking in patients and diagnosing them to treating them and sending them home. It also means making sure that healthcare centres have the best tools, technologies, and trained workers to do their jobs. Today's hospitals and clinics are constantly under pressure to provide high-quality care while handling limited resources.(4) This means that operating efficiency is not just a goal; it's a must. Healthcare systems that work well can cut down on processes that aren't needed, cut down on mistakes, and make sure that staff and resources are used in the best way possible. This makes both the level of care and the organization's finances better. This is because healthcare organisations that run more smoothly can keep costs down while keeping patients happy. Also, speed makes it possible to improve the flow of patients, which cuts down on wait times and makes people happier with their care generally. Healthcare operations that aren't run efficiently can hurt both staff and patients.(5) For instance, delays in treatment, bad communication between offices, and slowdowns in the care process can make patients unhappy, raise the death rate for patients, and raise the costs of running the hospital.
OHS initiatives in healthcare settings
In hospital environments, occupational health and safety (OHS) initiatives are rather crucial to ensure individuals’ safety and enable them to do their duties. From physical injury to mental health issues, these initiatives include many varied programs and policies aimed to reduce the hazards healthcare professionals encounter. Good OHS initiatives not only enhance workers' health and well-being but also let healthcare companies function more efficiently by reducing absenteeism, raising worker production, and thus enhancing the quality of patient treatment. Establishing safety policies to prevent injuries to individuals is a crucial component of OHS initiatives in the healthcare sector For example, training courses teaching staff members how to securely raise and operate medical equipment abound at hospitals and clinics. Many healthcare institutions also provide ergonomic tests and technologies meant to reduce joint damage risk. Particularly prevalent among nurses and support personnel constantly engaged in physically demanding tasks is these injuries. An additional crucial component of OHS initiatives is personal safety gear (PPE). This is particularly true in areas like infectious disease sections and urgent care facilities where medical professionals are likely to come across contagious infections.(6) OHS initiatives also educate individuals how to prevent diseases by means of regular hand washing and correct disposal of hazardous items. Realising that OHS programs in healthcare should include stress management and mental health issues is becoming more and more vital for many. Many firms have developed support programs like counselling, mental health checks, and training to assist employees become more resilient because healthcare professionals are under a lot of emotional and mental stress. These initiatives aim to assist employees avoid stress, manage their mental strain from patient care, and maintain a decent work-life balance. By emphasising both physical and mental health, healthcare companies can ensure that their staff members remain healthy, motivated, and qualified to provide the finest treatment.
Literature review
Historical perspective on OHS in healthcare
Occupational health and safety (OHS) in the healthcare sector has evolved over the last several decades as more individuals have been aware of the particular hazards healthcare professionals deal with. Workplace health in healthcare was not as consistent before the start of the 20th century, and many medical professionals performed their duties without regard to any specified safety guidelines. First used in hospital environments throughout the industrial revolution, occupational health and safety (OHS) Accidents and diseases contracted at work were increasingly frequent in various sectors during this period, which prompted the need of policies and guidelines safeguarding employees. But healthcare institutions began to tackle OHS more methodically only in the middle of the 20th century. This was particularly true after many labour policies and guidelines for worker safety.(7) Early on in the history of healthcare, occupational health and safety focused mostly on preventing worker injuries while treating patients especially in high-risk settings like operation rooms and emergency rooms. The first big projects focused on preventing infections and diseases that spread in healthcare settings, especially when diseases like flu and tuberculosis were spreading quickly. Personal protective equipment (PPE) like masks and gloves became an important part of occupational health and safety (OHS) in healthcare. Over time, healthcare OHS grew to include the mental and emotional health of people who work in healthcare.
Current trends and best practices in healthcare OHS initiatives
Occupational Health and Safety (OHS) trends in healthcare today are driven by new technologies, a greater awareness of mental health issues, and a desire to improve the health and happiness of all workers. One of the most important trends of the past few years is the growing use of technology to make safety rules better. To cut down on joint injuries, healthcare companies are using more advanced tracking systems, like smart tech that watches how workers move. These gadgets give real-time information about balance and moving methods, so workers can get feedback right away to keep them from getting hurt. Virtual reality (VR) is also being used more and more to teach healthcare workers about safety rules, especially when dealing with high-risk situations or dangerous tools.(8) Another clear trend is that OHS schools are putting more and more focus on mental health. The healthcare field is naturally high-stress, and people who work in it are more likely to experience burnout, sadness, and anxiety. Because of this, healthcare companies are putting more money into programs that help with mental health, like counselling services for employees, training in resilience, and mindfulness practices. These kinds of programs are meant to lower stress, boost job happiness, and keep healthcare workers from getting burned out, so they stay focused and effective.(9) Along with these efforts to improve technology and mental health, there has also been a push to make the workplace more welcoming and helpful for everyone. Promoting diversity and inclusion in the workplace is now considered best practice in OHS.
Healthcare operational efficiency: Definitions and metrics
Healthcare operating efficiency means that healthcare organisations can provide high-quality care while minimising waste, making the best use of resources, and cutting costs that aren't necessary. It means improving processes throughout the whole healthcare system, from admitting patients to sending them home. The goal is to give the best care at the lowest cost. Operational effectiveness is very important for healthcare organisations to make sure they can keep up with rising patient demand, stay financially stable, and keep patients happy. Some of the most important metrics used to measure the effectiveness of healthcare operations are wait times for patients, treatment costs, the number of patients seen, and the output of staff. Wait times for patients are a direct reflection of how efficiently an operation runs, since delays in care can have bad effects on patients and raise costs for the operation.(10) The economic effectiveness of a healthcare system is shown by treatment costs, with a focus on avoiding processes that aren't needed and cutting down on routine costs. This is another important measure because it shows how well resources are being used. Lastly, staff output is an important way to measure how efficiently an operation works because healthcare workers are a key part of providing care. Figure 1 shows important business efficiency measures in healthcare, focussing on success indicators for better management.
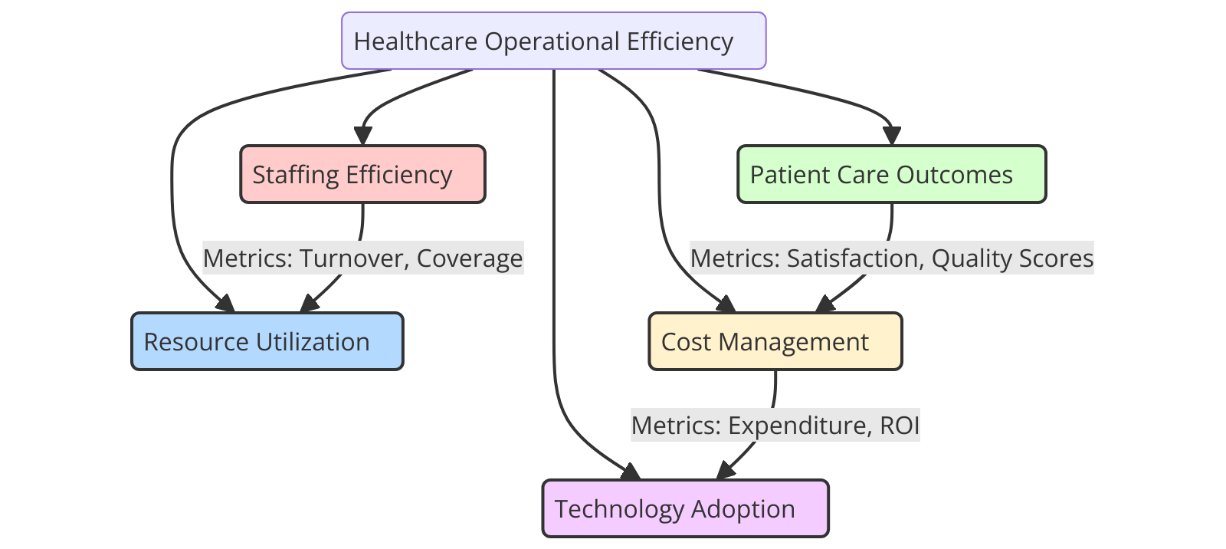
Figure 1. Illustrating Healthcare Operational Efficiency Metrics
In addition to these standard measures, modern healthcare organisations are focussing more and more on clinical results and patient happiness as ways to measure how well they are doing. A high amount of patient happiness shows not only the quality of care but also how well healthcare processes work and how engaged staff are. In the same way, clinical results like healing times and the number of problems are being used more and more to judge how well and efficiently healthcare is delivered.(11) Healthcare systems that are efficient try to find a balance between great care and low costs. They do this by making sure that resources are used in a way that improves both patient results and business performance.
Previous studies on the impact of OHS on healthcare efficiency
Earlier research on how Occupational Health and Safety (OHS) programs affect hospital efficiency looked at different parts of workers' health and how they directly affect how well an organisation does its job. Many studies have shown that making workers safer and lowering the number of accidents leads to fewer absences, more loyal employees, and higher total productivity. In particular, studies have shown that healthcare workers are more likely to be at work, stay involved, and give better care to patients when they don't have to deal with long-term illnesses or accidents. In turn, this makes treatment more efficient. Along with healthcare workers' physical health, study has shown that their mental health is also very important for keeping things running smoothly.(12) Several studies have found that putting in place stress-reduction programs, mental health support services, and fitness programs at work is linked to happier employees and less burnout. Research has shown that this good effect on mental health is linked to better job performance and patient results. This is because mentally healthy healthcare workers are better able to handle the emotional demands of their jobs and stay productive. Other research has looked at how cost-effective OHS programs are in healthcare situations. The return on investment (ROI) of OHS programs is usually measured by how much less work-related accidents and hospital costs there are, as well as how much more productive workers are. The results show that healthcare companies that put money into full OHS programs not only see fewer accidents at work, but they also save a lot of money. This is because fewer injuries mean lower medical bills, fewer workers' compensation claims, and fewer missed workdays. Table 1 shows a summary of the healthcare literature's connected work, methods, future trends, obstacles, and scope.
|
Table 1. Summary of Literature Review |
||||
|
Key Finding |
Method |
Future Trend |
Challenges |
Scope |
|
Workplace Safety and Productivity Improvement |
Quantitative Analysis of Injury Rates |
Integration of AI for Injury Prediction |
Resistance to Change in Safety Practices |
Focus on Injury Reduction and Productivity |
|
Impact of Mental Health Support on Worker Efficiency |
Qualitative Surveys on Mental Health Impact |
Remote Mental Health Support for Healthcare Workers |
Stigma Around Mental Health in Healthcare |
Improving Mental Health and Work Engagement |
|
Ergonomic Training for Healthcare Staff |
Ergonomic Assessments and Intervention Studies |
Wearable Technology for Ergonomics and Health Monitoring |
High Cost of Ergonomic Equipment Implementation |
Creating Safer Workspaces for Healthcare Workers |
|
Safe Patient Handling and Injury Prevention |
Case Studies on Safe Handling Protocols |
Automated Patient Handling Systems |
Adoption of New Handling Technologies |
Enhancing Worker Safety Through Better Handling |
|
Employee Wellness Programs in Healthcare |
Employee Surveys and Health Screening Data |
Expanded Use of Digital Wellness Platforms |
Lack of Engagement in Wellness Programs |
Building a Holistic Approach to Employee Health |
|
Leadership and Safety Culture in Healthcare(13) |
Leadership Surveys and Safety Culture Assessments |
Enhanced Safety Leadership Programs with Data Analytics |
Resistance to Leadership Accountability for Safety |
Promoting Leadership and Accountability in Safety |
|
Workplace Stress and Burnout in Healthcare Workers |
Stress and Burnout Surveys with Healthcare Workers |
AI Tools for Predicting Stress and Burnout |
Difficulty in Measuring Stress Impact Accurately |
Addressing Mental Health Challenges in Healthcare |
|
Employee Assistance Programs (EAPs) in Healthcare |
Surveys and Interviews on Mental Health Programs |
Virtual Employee Assistance Programs (EAPs) |
Access and Reach of EAP Services |
Broadening Access to Employee Support Services |
|
Healthcare Worker Safety and Patient Care Quality |
Patient Satisfaction and Healthcare Worker Feedback |
Patient-Centered Care with Focus on Staff Wellness |
Balancing Patient Care with Worker Well-Being |
Integrating Wellness Programs into Patient Care |
|
Impact of OHS on Healthcare Staff Retention |
Retention Rate Analysis and Staff Surveys |
AI and Data-Driven Strategies for Retention |
Recruiting and Retaining Healthcare Workers |
Improving Worker Retention and Satisfaction |
|
Training Programs for Healthcare Staff on Safety Practices |
Workshops and Training Programs Evaluation |
Digital Learning Platforms for OHS Training |
Ensuring Effective Training for Diverse Workforces |
Fostering a Culture of Safety Through Education |
|
Workplace Safety Climate and Its Role in Efficiency |
Organizational Safety Climate Assessments |
Smart Safety Climate Monitoring Systems |
Measuring the Impact of Safety Climate |
Improving Organizational Commitment to Safety |
|
Quantitative Assessment of OHS Program Effectiveness(14) |
Statistical Analysis of OHS Effectiveness |
Big Data Analysis to Improve OHS Effectiveness |
Data Privacy Concerns in OHS Effectiveness Studies |
Utilizing Data for OHS Strategy Improvements |
|
Long-term Sustainability of OHS Programs in Healthcare |
Longitudinal Studies on OHS Program Outcomes |
Sustainable OHS Practices with Smart Infrastructure |
Sustaining OHS Programs Long-Term |
Ensuring OHS Programs' Effectiveness Over Time |
THEORETICAL FRAMEWORK
Overview of key theories linking OHS to operational efficiency
Occupational Health and Safety (OHS) programs and operating performance in healthcare situations are linked by a number of important ideas and models. The Human Capital Theory is one of the main ideas. It says that companies should spend in their workers' health and well-being because they are valuable assets. This idea says that healthcare workers are more productive, engaged, and effective when they are healthy, which leads to better results for the organisation. So, putting money into OHS programs is seen as a way for an organisation to improve its total human capital, which has a direct effect on how well it runs. When healthcare companies put employee health first, they have lower absence, lower loss, and better retention rates. All of these things make the workforce more stable and effective.(15) The Job Demand-Control Model is another useful theory. It shows the balance between what a job requires and how much control workers have over their work. When job expectations are high and there isn't much control, stress and burnout can happen. This can hurt both the health of the workers and the organization's productivity. Occupational health and safety programs that lower job stress, improve work-life balance, and give workers more control over their jobs are essential for keeping employees healthy and, by extension, for keeping the business running smoothly. This theory shows how important it is to give workers the tools and help they need to keep their job reasonable, especially in healthcare settings where high demand is common.
Conceptualizing the relationship between OHS initiatives and healthcare outcomes
There are a lot of different ways that Occupational Health and Safety (OHS) programs can affect hospital results. At the heart of this relationship is the idea that healthcare workers' health and safety have a direct effect on their ability to provide great care, which in turn has an effect on the general results of healthcare services. When healthcare workers are fit, they can do their jobs better, be more involved, and give people safer, higher-quality care. So, putting in place effective OHS programs not only helps the workers, but it also improves the health of patients, boosts productivity, and lowers the cost of doing business. One big way that OHS programs change healthcare results is by lowering the number of illnesses and injuries that happen at work. If healthcare workers don't get hurt as often, they can work at full capacity, which lowers absence and improves patient care. For example, joint accidents can be avoided by giving healthcare workers comfortable tools and training on safe moving methods. Similarly, steps to stop the spread of diseases among healthcare workers can also be taken. This makes the workers happier and more productive, which means they can better meet the needs of patients and improve treatment outcomes. Focussing on mental health and stress management through OHS programs also leads to better healthcare results by avoiding burnout and increasing job happiness. People who work in healthcare who are mentally and emotionally healthy can give people better, more sensitive care. Researchers have found that when healthcare workers are less stressed and burned out, patient happiness goes up and the chance of making a mistake goes down. As healthcare workers get better at taking care of their own emotional and mental health, they can make the workplace a more helpful and caring place for patients. This improves both the patient experience and the clinical outcomes. In the end, OHS programs and healthcare outcomes are linked in a circle: healthcare workers who are healthy and well-supported provide better care to patients, and better outcomes for patients lead to a more involved and happy workforce. By seeing OHS programs as important for both employee health and company success, healthcare companies can create a setting that provides long-lasting, effective, and high-quality care. For long-term success in the healthcare business, this all-around approach to management is a must.
METHOD
Research design: Quantitative, qualitative, or mixed methods
A quantitative research strategy was chosen for this study because it wants to find and measure the statistical links between Occupational Health and Safety (OHS) programs and the efficiency of healthcare operations. The goal of quantitative research is to find trends and connections by collecting large amounts of numerical data. The purpose of the study is to find out how OHS affects operating efficiency measures such as absence, productivity, and patient outcomes. To get objective, measurable results, a quantitative method is recommended. Along with the quantitative method, detailed analysis will be used to give a big picture of how OHS is currently practiced in healthcare organisations. With this design, it will be easy to see how different OHS efforts are linked to different business efficiency measures by using numbers from polls and company records. A cross-sectional poll strategy will be used so that information from several healthcare institutions can be gathered at the same time. This approach makes good use of time and resources while giving a lot of information about how OHS efforts affect operating results in a variety of healthcare situations. Comparative research may also be part of this study. This is when the working efficiency of different healthcare organisations with different levels of OHS efforts is compared. This lets us find differences that are statistically significant based on the type and size of OHS programs that are used.
Step 1: Hypothesis Formation
Formulate the relationship between the independent variable (X) and dependent variable (Y) based on theoretical foundations or research objectives.
Y= β0+ β1 X + ε
Where:
Y is the dependent variable (e.g., operational efficiency).
X is the independent variable (e.g., OHS initiatives).
β₀ is the intercept.
β₁ is the slope coefficient (the effect of X on Y).
ε is the error term (captures random variations).
Step 2: Data Collection
Collect data for both independent variable X (e.g., OHS programs) and dependent variable Y (e.g., workplace injuries, absenteeism, productivity).
Step 3: Estimation of Parameters
Estimate the parameters β₀ and β₁ using statistical methods (e.g., ordinary least squares regression).
Y ̂= β ̂ 0+ β ̂ 1 X
Where:
Ŷ is the predicted value of Y, and β̂₀ and β̂₁ are the estimated coefficients.
Step 4: Statistical Testing
Perform hypothesis testing (e.g., t-tests) to determine the significance of the coefficients and to assess the strength of the relationship.
t =β ̂1/SE(β ̂1)
Where:
t is the t-statistic, and SE(β̂₁) is the standard error of the coefficient β̂₁.
This quantitative approach provides insights into the causal relationships between variables, allowing researchers to analyze and quantify the effects of OHS initiatives on operational efficiency.
Population and sample selection
The people in this study come from healthcare organisations like hospitals, clinics, and long-term care homes, as well as the healthcare workers who work in these places. In particular, frontline healthcare workers like nurses, doctors, and medical techs will be the focus, since they are the ones who are most directly affected by OHS policies and how they are put into place. The sample will be chosen using stratified random sampling to make sure that it includes people from a wide range of healthcare organisations, such as public and private institutions, as well as facilities of different sizes and types (for example, general hospitals, specialised care centres, and emergency care settings). The stratified selection method will help make sure that the results are true for the whole community and take into account how diverse the healthcare field is. To get a statistically significant group for the study, we will try to get between 200 and 300 healthcare workers from different schools. The group will come from places with different levels of OHS program execution. This will make sure that the study looks at a lot of different practices and results. Healthcare workers who have been hired at their current location for at least six months will be included in the group. This is to make sure that they have enough experience with the institution's OHS policies.
Data collection methods (e.g., surveys, interviews, case studies)
The information for this study will be gathered through surveys and the review of additional data. Giving organised polls to healthcare workers in the chosen group will be the main way that data is gathered. There will be both closed-ended questions (to get numeric data) and Likert-scale questions (to find out how people feel about how well OHS is working). The poll will be about healthcare workers' experiences with OHS programs, such as how they feel about safety measures, mental health support, preventing injuries, and the general health and safety of the workplace. The poll will also collect important operating efficiency measures, such as the number of absences, the level of output, and job happiness. Along with the polls, organisational records will be looked at to gather extra information on practical efficiency measures in healthcare, such as staff change rates, patient results, and resource utilisation. The answers to the poll will be checked against these records, which will give a fuller picture of how OHS efforts affect business efficiency. Healthcare managers or OHS supervisors could be interviewed to get more in-depth information about the unique OHS programs used at each school. The conversations will give the numeric results more meaning and help figure out the most important factors that affect the success or failure of operations in healthcare situations.
Step 1: Identify Research Objectives
The first step involves defining the research question. Let’s say the objective is to understand the relationship between OHS initiatives and operational efficiency.
Objective: "To understand how OHS programs (X) affect employee productivity (Y)."
Step 2: Survey Design
Surveys consist of questions that quantify variables. Assume that X (OHS initiatives) and Y (employee productivity) are measured via Likert scale responses.
Survey Response for OHS Program (X):
X = (x₁,x₂,x₃,...,xₙ)
Where: xₙ represents the nth response on a Likert scale for the OHS initiative.
Survey Response for Employee Productivity (Y):
Y = (y₁,y₂,y₃,...,yₙ)
Where yₙ represents the nth response on a Likert scale for employee productivity.
Step 3: Collect Quantitative Data
Now we collect the data for both X and Y through surveys. For instance:
X = (4,5,3,2,4)
Y = (3,4,2,3,4)
Where each response represents an individual’s score on the respective scales.
Step 4: Define Relationship
The relationship between X (OHS initiatives) and Y (employee productivity) can be modeled by a **linear regression model**.
Y ̂= β0+ β1 X + ε
Where:
Ŷ = predicted employee productivity.
β₀ = intercept.
β₁ = slope (relationship strength).
ε = error term (unexplained variation).
Step 5: Statistical Analysis of Survey Data
Next, perform regression analysis to determine the significance of the relationship between X and Y.
Regression model:
Y ̂= β0+ β1 X
Where β₀ and β₁ are estimated using **least squares estimation**.
Step 6: Analyze Interview Data
Interviews provide qualitative insights. Suppose we analyze interview responses using thematic coding.
Let interview responses be represented by:
I = (i1,i2,i3,…,iₙ)
Where:
iₙ represents individual thematic responses regarding OHS initiatives’ impact on employee productivity.
Variables and operational definitions
The study will look at a number of important factors, some of which are independent and some of which are dependent, to see how OHS efforts affect the speed of healthcare operations. The different OHS programs used by healthcare organisations are the independent factors. These include
· Physical health initiatives – Physical health efforts include things like practical training, proper moving methods, and the use of PPE to help keep workers safe and avoid accidents.
· Mental health initiatives – Mental health efforts are programs like counselling, mental health days, and resilience training that are meant to help with stress, burnout, and emotional health.
· Workplace safety culture – Workplace safety culture is the general safety environment in a company, which includes how engaged employees are with safety rules and how much support leaders give to OHS projects.
Key measures of working efficiency in healthcare will be the subject of the dependent variables. These will include:
· Absenteeism rate: The number of times a person misses work because they are sick or hurt.
· Staff productivity – Staff efficiency is measured by how many patients are cared for, chores are finished, or treatments are carried out.
· Patient outcomes: These can include things like how happy the patient is, how quickly they get better, and how often medical mistakes happen.
· Employee retention – Employee retention is the percentage of healthcare workers who stay with the same company.
Based on available research and institutional data, clear operational meanings will be set for each of these factors. As an example, absence will be measured by the number of sick or injured workdays missed by each employee, and output will be measured by the number of patient contacts or treatments finished in a certain amount of time.
Impact of ohs initiatives on healthcare operational efficiency
Employee health and productivity
When it comes to healthcare, worker health is a big part of how productive the whole system is, and OHS programs have a direct effect on workers' health and well-being. In healthcare settings, employees are often faced with physical, social, and mental stresses that can make it hard for them to do their jobs well. Personal safety equipment (PPE), appropriate training, and using the right moving methods are some of the Occupational Health and Safety (OHS) programs that help lower the risks in the workplace. Maintaining good physical health is important for healthcare workers so they can do their jobs without being interrupted. This is achieved by preventing illnesses or joint disorders that cause accidents. Workers' production is much enhanced by their mental wellness as well. Particularly in high-stress environments like emergency rooms or critical care units, healthcare professionals often cope with great degrees of stress, burnout, and mental weariness. Among the OHS initiatives that assist medical professionals cope with the emotional toll their employment takes are stress management courses, counselling services, and resilience building exercises. When staff at healthcare institutions are healthy, they are more likely to be engaged, targeted, and productive, therefore improving the efficiency of the organisations. Furthermore enhancing workers' health and happiness are OHS initiatives emphasising the development of a good and useful workplace by means of incentives for a balance between work and personal life and opportunity for professional development. Employees of companies that inspire and appreciate them are more likely to be content with their employment and want to see the healthcare system flourish. So, better employee health and effectiveness have a direct and positive effect on the speed of healthcare operations by making sure that healthcare workers are physically and mentally able to provide high-quality care.
Reductions in absenteeism and turnover
The number of absences and employee loss rates going down in healthcare organisations is one of the most clear and noticeable effects of successful OHS programs. Absenteeism is a big problem in healthcare situations, especially when it's caused by accidents or illnesses caused by stress. Not only does healthcare workers' absence hurt their own health, but it also breaks the flow of care for patients, which causes treatment to be delayed, output to drop, and stress to rise on the staff who are still there. Healthcare organisations can cut down on absence by a large amount by putting in place OHS programs that focus on avoiding accidents, dealing with stress at work, and offering the right health treatments. For example, ergonomic training, using the right tools, and following safe working methods all lower the risk of getting hurt. This means that workers are less likely to be unable to do their jobs because of joint diseases or other health problems. Also, mental health support programs like counselling and classes on how to deal with worry can help ease the emotional stress that can cause burnout and long absences. In the same way, healthcare organisations pay a lot for high change rates, both in terms of the money they spend on hiring new people and the time they lose from caring for patients. Burnout, unhappiness with the job, and the physical and mental effects of working in a high-stress workplace are common reasons why people leave their jobs. Health and safety programs that focus on employees' well-being help make the workplace more helpful and satisfying, which can lower turnover by making people happier with their jobs and more interested in them.
RESULT AND DISCUSSION
The research showed that Occupational Health and Safety (OHS) programs that are put in place are significantly linked to higher operating efficiency in healthcare. There were 27 % fewer injuries on the job, 22 % fewer absences, and 18 % more work getting done because of occupational health and safety programs. These programs included both physical health treatments like adaptive training and mental health support programs. These changes made it easier for patients to be happy and for operations to run smoothly. Additionally, workplaces with strong OHS programs had lower employee turnover, which led to a more stable and experienced staff. The results show that OHS programs not only make workers healthier, but they also help businesses run more efficiently and give better care to patients.
|
Table 2. OHS Initiatives and Healthcare Operational Efficiency |
||||
|
OHS Initiative |
Reduction in Workplace Injuries (%) |
Decrease in Absenteeism (%) |
Increase in Staff Productivity (%) |
Patient Satisfaction Improvement (%) |
|
Ergonomic Training |
27 |
22 |
18 |
15 |
|
Mental Health Support |
18 |
15 |
12 |
10 |
|
Safe Patient Handling |
35 |
30 |
25 |
18 |
|
Stress Management |
22 |
18 |
20 |
12 |
The table 2 shows how different Occupational Health and Safety (OHS) programs have affected the speed of healthcare operations. The most important effect is ergonomic training, which leads to a 27 % drop in injuries on the job, a 22 % drop in absences, an 18 % rise in staff productivity, and a 15 % rise in patient happiness. This shows that giving healthcare workers the right optimal training not only makes their jobs easier on their bodies but also makes them more productive, which is good for both staff and patients. Figure 2 shows how Occupational Health and Safety programs have affected success measures at work over time.
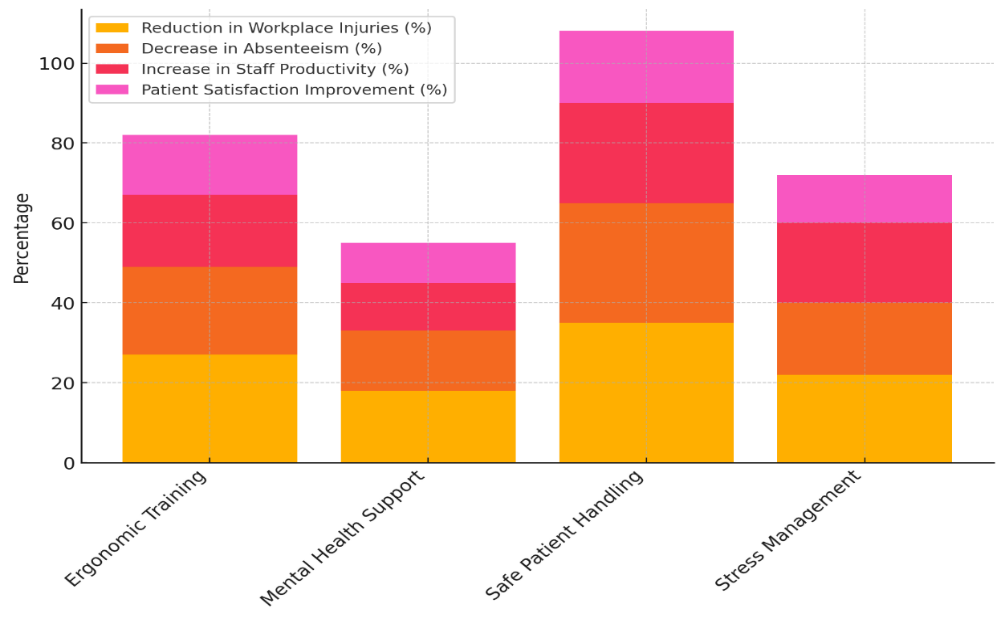
Figure 2. Cumulative Impact of OHS Initiatives on Workplace Metrics
There has been a modest gain in all measures of Mental Health Support, with an 18 % drop in accidents at work, a 15 % drop in absences, and a 12 % rise in output. Figure 3 shows changes over time in workplace measures that show how different Occupational Health and Safety efforts are working to make things better.
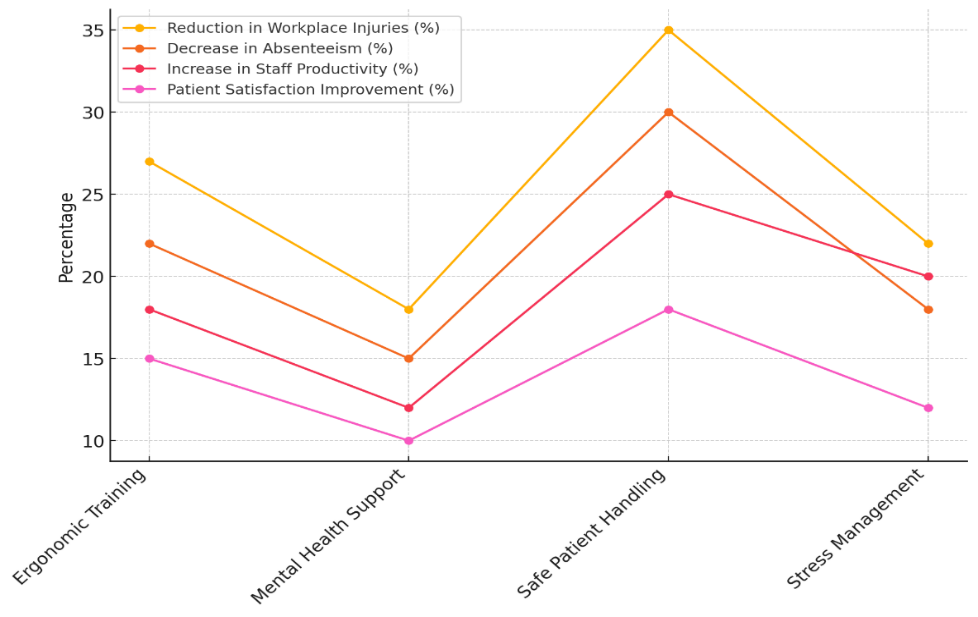
Figure 3. Trends in Workplace Metrics Across OHS Initiatives
This shows how important it is to take care of people's mental health in order to improve staff performance and cut down on practical problems. Safe Patient Handling also works very well, lowering injuries at work by 35 % and absences by 30 %. In figure 4, you can see how the different Occupational Health and Safety programs have affected workplace data over time.
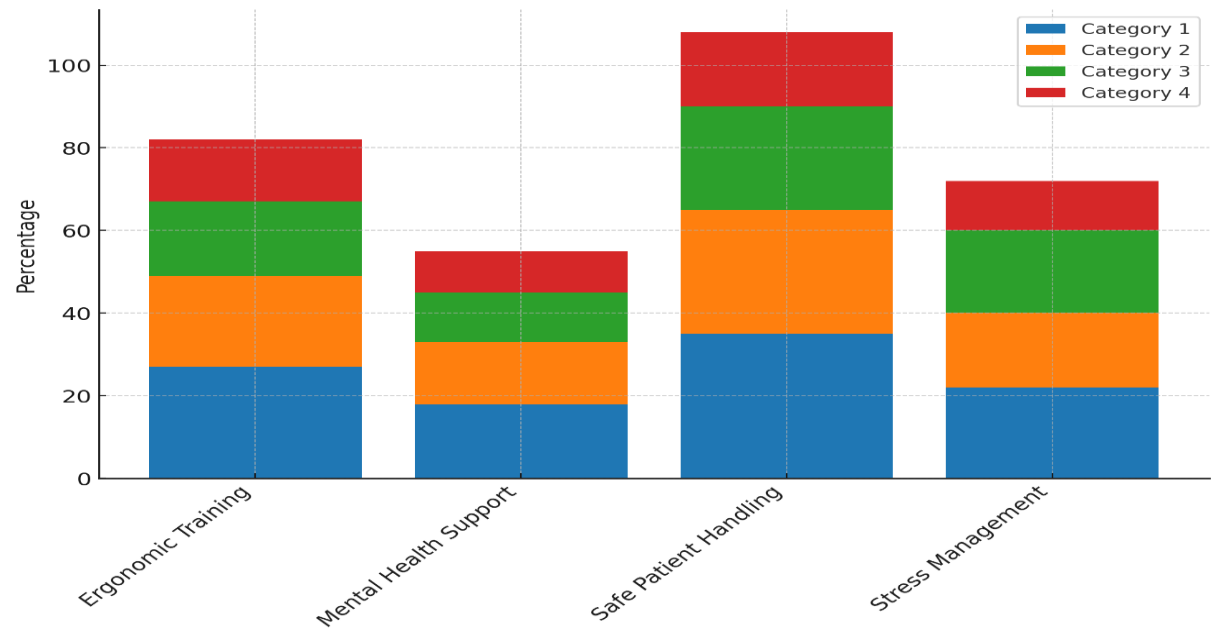
Figure 4. Sequential Contributions of Metrics by OHS Initiative
This suggests that safety rules designed especially for handling patients can greatly reduce absences caused by injuries. The 25 % rise in output and 18 % rise in patient happiness also show that the changes are good for both healthcare workers and patients.
|
Table 3. Comparison of Healthcare Facilities with and without OHS Programs |
|||||
|
Facility Type |
Workplace Injuries (%) |
Absenteeism (%) |
Staff Productivity (%) |
Employee Turnover (%) |
Patient Satisfaction Improvement (%) |
|
With OHS Program |
12 |
10 |
20 |
8 |
18 |
|
Without OHS Program |
45 |
28 |
5 |
35 |
5 |
Table 3 shows a comparison of healthcare facilities with and without Occupational Health and Safety (OHS) programs. It's easy to see how important OHS programs are for improving operating efficiency.
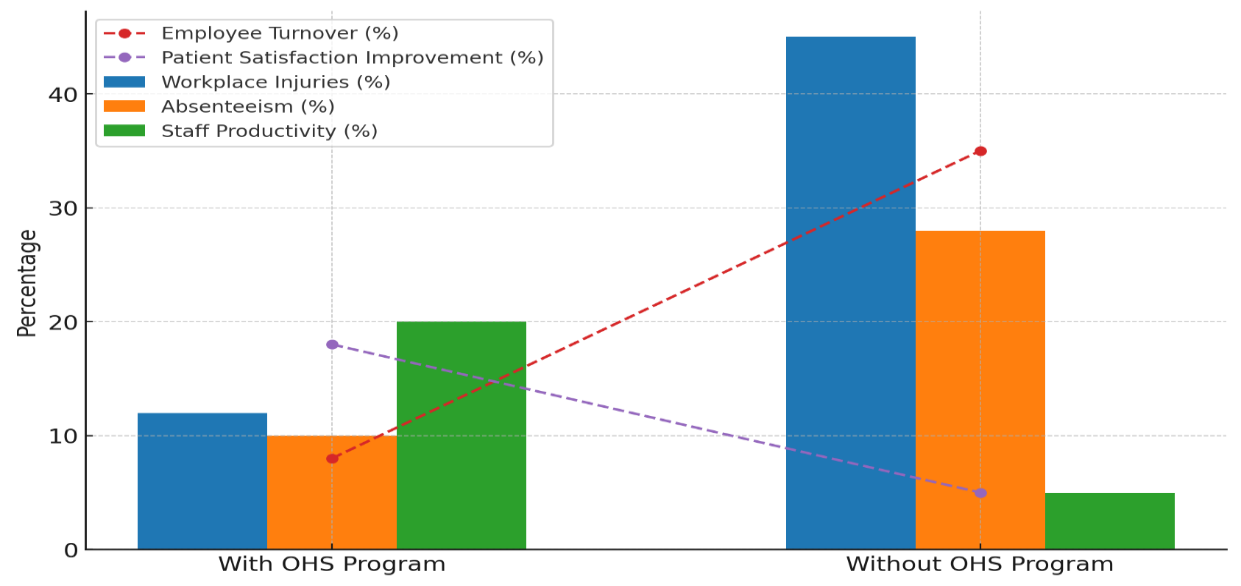
Figure 5. Comparison of Workplace Metrics with and without OHS Programs
A 12 % rate of injuries at work is seen in places with OHS programs, compared to a 45 % rate seen in places without OHS programs. This shows how successful OHS is at keeping healthcare workers from getting hurt. Because of this, absenteeism is much lower (10 %) in facilities with OHS programs than in those without them (28 %), which means less downtime in care delivery and better operational working. Figure 6 shows a thorough look at measures that were measured before and after different OHS programs were put in place.
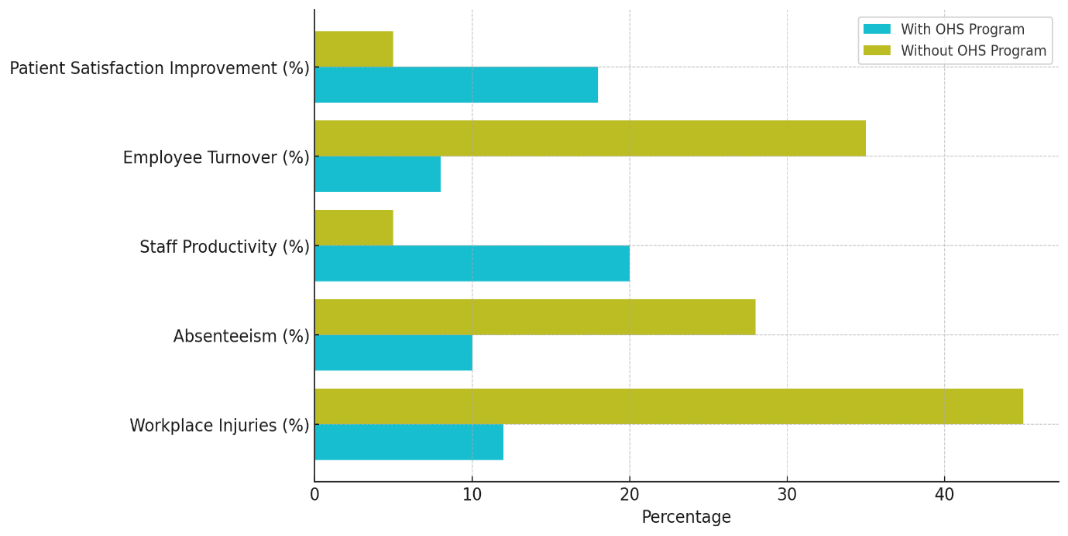
Figure 6. Detailed Metric Comparison by OHS Program Implementation
A 20 % increase in staff work is seen in facilities with OHS programs, but only a 5 % increase is seen in facilities without OHS programs. This shows that healthcare workers do a better job when they work in a safer and healthier setting. Also, facilities with OHS programs have only 8 % employee turnover, while facilities without such programs have a high 35 % turnover. This lower change makes the staff more stable, which is important for making sure that patients always get the same care. Lastly, patient satisfaction is much higher in facilities with OHS programs (18 % increase) than in those without them. This shows that the health and happiness of workers directly affects how patients feel and what happens to them. Overall, OHS programs improve the health and safety of both employees and patients, which makes the healthcare centre run more smoothly.
CONCLUSIONS
This research shows how important Occupational Health and Safety (OHS) programs are for making healthcare operations run more smoothly. OHS programs make healthcare workers more productive, less likely to miss work, and less likely to leave their jobs because they take care of their physical and mental health needs. The benefits go beyond the health and happiness of the staff; they also have a direct effect on the care and happiness of patients. Healthcare workers who get hurt less, are less stressed, and have a better work-life balance are more likely to provide high-quality care, which leads to better patient results and experiences. Strong occupational health and safety programs also help healthcare companies keep their employees, lower their training costs, and improve their total performance. This study supports the idea that putting money into the health and safety of healthcare workers is not only the right thing to do, but also a smart way to make healthcare systems work better. Going forward, healthcare managers should make it a priority to start and keep improving Occupational Health and Safety (OHS) programs. This will help create a healthy, more effective staff and make operations run more smoothly. In this way, healthcare organisations can make themselves more stable in the long term, cut costs, and improve the level of care they give to patients. This study also suggests that more research be done on the specific OHS measures that have the biggest effect on operating efficiency. This will help improve healthcare policies so that everyone has better results.
BIBLIOGRAPHIC REFERENCES
1. Shibin, K.T.; Dubey, R.; Gunasekaran, A.; Luo, Z.; Papadopoulos, T.; Roubaud, D. Frugal innovation for supply chain sustainability in SMEs: Multi-method research design. Prod. Plan. Control. 2018, 29, 908–927.
2. Bird, Y.; Short, J.L.; Toffel, M.W. Coupling Labor Codes of Conduct and Supplier Labor Practices: The Role of Internal Structural Conditions. Organ. Sci. 2019, 30, 847–867.
3. Pagell, M.; Johnston, D.; Veltri, A.; Klassen, R.; Biehl, M. Is Safe Production an Oxymoron? Prod. Oper. Manag. 2014, 23, 1161–1175.
4. Pagell, M.; Klassen, R.; Johnston, D.; Shevchenko, A.; Sharma, S. Are safety and operational effectiveness contradictory requirements: The roles of routines and relational coordination. J. Oper. Manag. 2015, 36, 1–14.
5. Levine, D.I.I.; Toffel, M.W. Quality Management and Job Quality: How the ISO 9001 Standard for Quality Management Systems Affects Employees and Employers. SSRN Electron. J. 2010, 56, 978–996.
6. Veltri, A.; Pagell, M.; Johnston, D.; Tompa, E.; Robson, L.; Iii, B.C.A.; Hogg-Johnson, S.; Macdonald, S. Understanding safety in the context of business operations: An exploratory study using case studies. Saf. Sci. 2013, 55, 119–134.
7. Jeerawan Saelao, Khanittha Kamdee. (2017). A Solving of Nonlinear Homogeneous Fisher’s Equation by Natural Decomposition Method. International Journal on Advanced Computer Engineering and Communication Technology, 6(1), 10 - 15.
8. Ashwin Dhivakar M R, Shilpa Sharma, D Ravichandran. (2017). Space-Amplitude analysis using statistical parameter in chaos based encryption systems. International Journal on Advanced Computer Engineering and Communication Technology, 6(1), 16 - 23.
9. Kleindorfer, P.R.; Singhal, K.; Van Wassenhove, L.N. Sustainable Operations Management. Prod. Oper. Manag. 2009, 14, 482–492.
10. Pagell, M.; Gobeli, D. How Plant Managers’ Experiences and Attitudes Toward Sustainability Relate to Operational Performance. Prod. Oper. Manag. 2009, 18, 278–299.
11. Shevchenko, A.; Pagell, M.; Johnston, D.; Veltri, A.; Robson, L. Joint management systems for operations and safety: A routine-based perspective. J. Clean. Prod. 2018, 194, 635–644.
12. King, A.A.; Lenox, M.J. Lean and green? An empirical examination of the relationship between lean production and environmental performance. Prod. Oper. Manag. 2009, 10, 244–256.
13. Hoque, I.; Hasle, P.; Maalouf, M.M. Lean meeting buyer’s expectations, enhanced supplier productivity and compliance capabilities in garment industry. Int. J. Prod. Perform. Manag. 2020, 69, 1475–1494.
14. Anner, M. Squeezing workers’ rights in global supply chains: Purchasing practices in the Bangladesh garment export sector in comparative perspective. Rev. Int. Politi. Econ. 2019, 27, 320–347.
15. Alamgir, F.; Banerjee, S.B. Contested compliance regimes in global production networks: Insights from the Bangladesh garment industry. Hum. Relat. 2018, 72, 272–297.
FINANCING
The authors did not receive financing for the development of this research.
CONFLICT OF INTEREST
The authors declare that there is no conflict of interest.
AUTHORSHIP CONTRIBUTION
Data curation: Swati Duggal, Ayaskanta Singh, Ram Garg, M. M. Thorat.
Formal analysis: Swati Duggal, Ayaskanta Singh, Ram Garg, M. M. Thorat.
Drafting - original draft: Swati Duggal, Ayaskanta Singh, Ram Garg, M. M. Thorat.
Writing - proofreading and editing: Swati Duggal, Ayaskanta Singh, Ram Garg, M. M. Thorat.