doi: 10.56294/hl2023307
ORIGINAL
Innovations in Healthcare Education to Improve Quality of Life for Patients with Diabetes
Innovaciones en educación sanitaria para mejorar la calidad de vida de los pacientes con diabetes
Manashree Mane1 ![]() , Shailly Gupta2
, Shailly Gupta2 ![]() , Priya P. Roy3
, Priya P. Roy3 ![]() , Girish Kumar Pati4
, Girish Kumar Pati4 ![]() , Ajab Singh Choudhary5
, Ajab Singh Choudhary5 ![]()
1JAIN (Deemed-to-be University), Department of Forensic Science, Bangalore, Karnataka, India.
2Arya College of Pharmacy, Jaipur, Rajasthan, India.
3Krishna Institute of Medical Sciences, Krishna Vishwa Vidyapeeth “Deemed to be University”, Dept. of Anatomy, Taluka-Karad, Dist-Satara, Maharashtra, India.
4IMS and SUM Hospital, Siksha ‘O’ Anusandhan (Deemed to be University), Department of Gastroenterology, Bhubaneswar, Odisha, India.
5School of Allied Health Sciences, Noida International University, Greater Noida, Uttar Pradesh, India.
Cite as: Mane M, Gupta S, Roy PP, Kumar Pati G, Singh Choudhary A. Innovations in Healthcare Education to Improve Quality of Life for Patients with Diabetes. Health Leadership and Quality of Life. 2023; 2:307. https://doi.org/10.56294/hl2023307
Submitted: 29-05-2023 Revised: 25-08-2023 Accepted: 12-11-2023 Published: 13-11-2023
Editor: PhD.
Prof. Neela Satheesh ![]()
ABSTRACT
Introduction: healthcare education strategies meant to enhance patient outcomes and quality of life must be revaluated since diabetes is growing more frequent all across the globe. This project investigates innovative approaches of teaching healthcare that can provide persons with diabetes the tools, knowledge, and abilities required to properly manage their illness.
Method: we compiled a comprehensive meta-analysis and evaluation of research examining diabetes educational initiatives. Various approaches were examined to assess how well they performed: digital health technologies, online learning sites, direct patient-provider interaction, etc. We examined clinical findings, changes in lifestyle, and patient capacity for self-care by use of information from randomised controlled trials and group research.
Results: the study revealed that glycaemic control, medicine adherence, and general patient contentment were greatly improved by patient training initiatives employing digital technologies. Furthermore found to be more effective in inspiring individuals were tailored learning strategies considering cultural context and personal preferences. Programs teaching individuals how to manage their own life such as nutrition advice, exercise routines, and stress management—showered greater long-term outcomes.
Conclusion: fresh concepts in healthcare education especially those involving technology and tailored care have great potential to improve the quality of life of diabetics. People can take charge of their health with these tactics, which leads to better disease control and fewer problems. Continuing to put money into diabetes instruction is important for improving care and results for patients.
Keywords: Diabetes; Healthcare Education; Patient Empowerment; Digital Health; Self-Management; Personalized Care.
RESUMEN
Introducción: las estrategias de educación sanitaria destinadas a mejorar los resultados y la calidad de vida de los pacientes deben reevaluarse, ya que la diabetes es cada vez más frecuente en todo el mundo. Este proyecto investiga enfoques innovadores de enseñanza sanitaria que puedan proporcionar a las personas con diabetes las herramientas, los conocimientos y las habilidades necesarias para gestionar adecuadamente su enfermedad.
Método: Recopilamos un metaanálisis exhaustivo y una evaluación de las investigaciones que examinan las iniciativas educativas sobre la diabetes. Se examinaron diversos enfoques para evaluar su eficacia: tecnologías sanitarias digitales, sitios de aprendizaje en línea, interacción directa paciente-proveedor, etc. Se examinaron los resultados clínicos, los cambios en el estilo de vida y la capacidad de autocuidado del paciente mediante el uso de información procedente de ensayos controlados aleatorizados e investigaciones en grupo.
Resultados: el estudio reveló que el control glucémico, la adherencia a la medicación y la satisfacción general del paciente mejoraban considerablemente con las iniciativas de formación de pacientes que empleaban tecnologías digitales. Además, las estrategias de aprendizaje adaptadas al contexto cultural y las preferencias personales resultaron más eficaces para inspirar a los pacientes. Los programas que enseñan a las personas a gestionar su propia vida, como consejos sobre nutrición, rutinas de ejercicio y control del estrés, obtuvieron mejores resultados a largo plazo.
Conclusión: los nuevos conceptos en educación sanitaria, especialmente los relacionados con la tecnología y la atención personalizada, tienen un gran potencial para mejorar la calidad de vida de los diabéticos. Las personas pueden tomar las riendas de su salud con estas tácticas, lo que se traduce en un mejor control de la enfermedad y menos problemas. Seguir invirtiendo dinero en la instrucción diabética es importante para mejorar la atención y los resultados para los pacientes.
Palabras clave: Diabetes; Educación Sanitaria; Empoderamiento Del Paciente; Salud Digital; Autogestión; Atención Personalizada.
INTRODUCTION
Diabetes is now one of the most common long-term illnesses in the world. The World Health Organisation says that about 422 million people have diabetes, and that number is projected to rise greatly over the next few decades. As the number of people with diabetes keeps going up, its effects on healthcare systems, individuals, and society as a whole have become very important. Diabetes is hard to control because you have to keep an eye on your blood sugar levels, take your medications as prescribed, and make changes to your lifestyle all the time. To improve patient results, healthcare educators need to teach patients effectively. In the past, healthcare methods have mostly focused on medical treatments. However, it is becoming more and clearer that educating patients is an important part of managing diabetes and making people’s lives better.(1) New ideas in healthcare education are vital for giving people with diabetes the tools they need to take charge of their condition. It has been shown that healthcare education programs that teach patients about their disease, how to take care of themselves, and how to live a healthy life have a big impact on how well patients follow their treatment plans, how few complications they have, and their overall quality of life. As technology improves, especially in the digital health field, new ways of teaching people about diabetes are being created and used. These give patients the tools they need to better control their condition and communicate with their healthcare workers more effectively. Mobile health apps, online learning platforms, and telemedicine have made it possible for personalised and engaging learning to happen.(2) These new tools get around the problems of location, time, and accessibility that have usually made it hard to teach people about diabetes. Along with new technologies, teaching methods that stress patient-centered care and self-management are becoming more popular. When making education programs, these methods recognise how important it is to take into account the cultural, social, and psychological backgrounds of patients. Adapting health education to each patient’s specific wants and needs has been shown to increase involvement, help people remember what they’ve learnt, and result in better healthcare outcomes. A key part of effective diabetes education is joint conversation between patients and providers, which build trust and helps patients make smart choices. Recent studies show how important it is to not only teach patients about the science side of diabetes, but also give them the tools they need to use what they’ve learnt in their daily lives. This will make living with a chronic disease easier on their minds and emotions.(3)
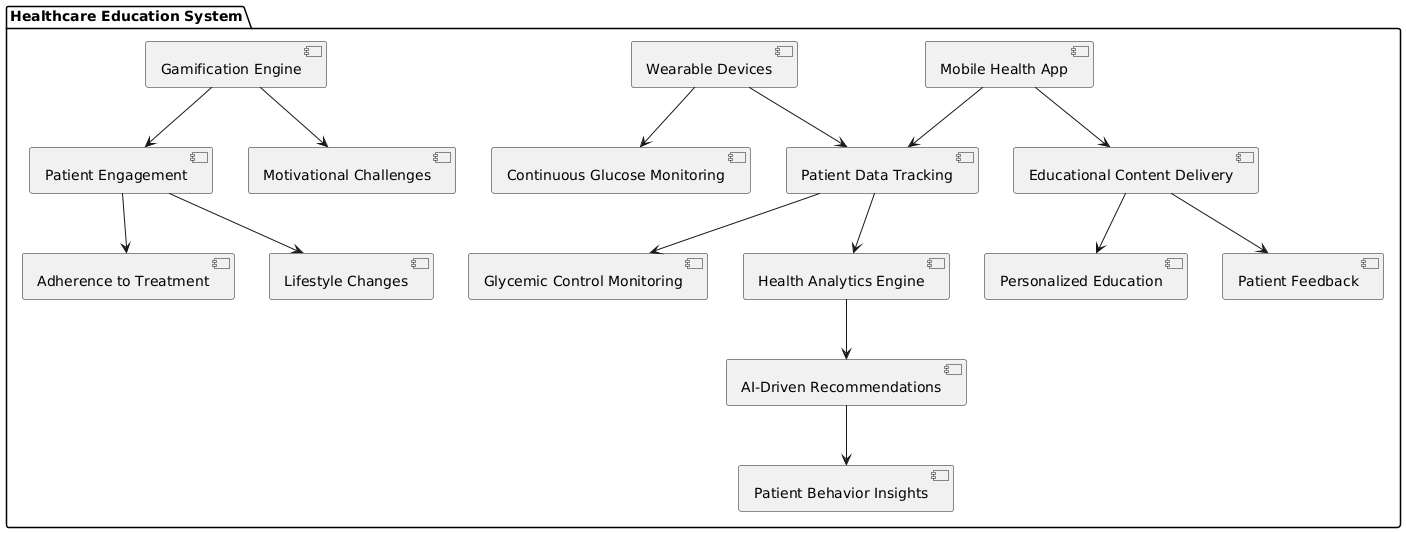
Figure 1. Overview of Healthcare education system architecture flowchart
Using technology in healthcare education has also led to the creation of real-time tracking systems that let people get feedback all the time and get personalised help. These methods help people keep track of their blood sugar levels, how often they exercise, what they eat, and when they take their medications. These kinds of tools help people make choices that have a direct effect on their health by giving them real-time information and tips, the system overview illustrate in figure 1. Social media and online groups have also made it easier for people to connect with others who have been through similar things. This has helped them get mental support, stay motivated, and learn from each other.(4) Even with all the progress, it’s still hard to make sure that everyone gets healthcare education, especially people who live in neglected or rural areas where technology and healthcare services are harder to get to. Also, because people respond differently to educational approaches, researchers and educators are always looking for the best ways to teach a wide range of patient groups. This essay’s goal is to look at these new developments in healthcare education and how they might help diabetes patients live better lives. It will do this by looking at both the technology and patient-centered methods that have come up in the last few years.
Background work
Historical Context of Diabetes Education
Over the years, diabetes education has changed a lot to mirror changes in what doctors know, how they treat diabetes, and what people need. In the beginning, managing diabetes mostly meant making changes to the patient’s food and giving them insulin shots. Patient education wasn’t given much attention. As diabetes became more common in the middle of the 20th century, doctors realised how important it was to give people the tools they needed to take care of their disease. At first, education efforts focused on teaching patients about their illness and pushing them to take control of their diet, especially by counting carbs and eating smaller portions. Over time, as diabetes care got better with the help of blood glucose tracking and newer drug schedules, teaching programs grew to cover more aspects of self-management, such as taking medications as prescribed, working out, and dealing with stress. In the 1970s, the start of diabetes self-management education (DSME) programs was a big step towards formalising diabetes education. Patients were taught how to make choices about their care based on accurate information.(5) These days, the multidisciplinary approach to diabetes management heavily relies on diabetes education. It underlines the need of cooperating and putting the patient first as it is now a component of fundamental care procedures. This historical background prepared the ground for the novel approaches of diabetes education under investigation currently, particularly those involving technology and tailored care models.
Healthcare Education Models for Diabetes Management
Although there are several forms of healthcare education for controlling diabetes, their common objective is to equip individuals with the knowledge and tools required to properly manage their condition. Under conventional models, group education events take place in person and are typically run under the direction of endocrinologists, nurses, or chef’s health care experts. Usually including items like blood sugar monitoring, insulin management, dietary recommendations, and exercise guidance, these seminars also cover although these models have helped individuals behave in the near future, their accessibility and simplicity can restrict them.(6) Over the past several years, there has been a shift towards more transparent learning environments like online courses and mobile health applications allowing individuals access to resources whenever and wherever they so wish. These models may have interesting components such quizzes, videos, and monitoring tools to make patients more engaged. Using patient-centred models that fit each individual’s likes, cultural background, and degree of health knowledge is also become more and more common. This helps to modify instruction for every person. People with diabetes are more likely to be able to control their condition if they are taught in a way that is personalised and useful to them in their daily lives. Also, methods that involve healthcare workers, patients, and their families working together as a team are becoming more and more common. These models focus on giving the patient a strong network of support to help them stick to their treatment plan and have long-term success with controlling their diabetes.(7)
Technological Innovations in Healthcare Education for Chronic Disease Management
New technologies have changed the way healthcare is taught, especially when it comes to managing long-term diseases like diabetes. Digital health tools, like mobile apps, smart tech, and telemedicine platforms, have made it easier to teach people about diabetes and help them take better care of themselves. Mobile apps let patients keep track of their blood sugar levels, how well they’re taking their medications, how active they are, and what they eat. These apps give patients real-time feedback and personalised suggestions.(8) Most of the time, these apps work with other health systems, which lets doctors keep an eye on patients from afar and help them if they need to. Continuous glucose monitors (CGMs) that are worn on the pores and skin deliver patients actual-time information about their blood sugar ranges. This helps them make clever choices approximately their meals, exercising, and insulin use. That equipment work in real time, which has been proven to get patients extra worried and help them persist with their remedy plans. Telemedicine structures also allow patients and healthcare vendors have video meetings, which receives round local problems and gives people who cannot get to a medical doctor in person more options.(9) In conjunction with making diabetes training extra effortlessly to be had and less difficult, all of these technological tendencies permit individuals to recognize extra approximately their condition. Including artificial intelligence (AI) into those gadgets would possibly probably assist diabetic remedy to be even more tailor-made by means of presenting predictive insights and customized suggestions meant to increase results and reduce the hazard of complications.
Patient-Centered Approaches to Education
Patient-centered techniques to diabetes schooling emphasise the requirement of understanding and enjoyable the particular needs, desires, and scenario of every person. Patient-targeted schooling avoids a one-size-fits-all method. Instead, it emphasises making sure treatment plans complement the patient’s cultural history, way of life, and personal targets.(10) This approach considers the reality that patients are more likely to recall and grasp events related to their very own lifestyles. Coaching publications touchy to many cultures and thinking about troubles like language boundaries, nutritional styles, and social variables influencing fitness, as an instance, are more likely to have interaction a large spectrum of college students. Moreover, patient-centered practise centres the affected person in making selections about their treatment. By use of purpose-placing, motion planning, and development monitoring, this approach allows people to take obligation of their own fitness.(11) Moreover helping healthcare people set up believe with their patients and collaborate with them is by way of applying positive inquiry and shared decision-making methods. This approach enables patients to become active participants in their therapy instead of quiet users, therefore helping them to change their behaviour over time. The ultimate goal of patient-centered teaching is to enhance not only health results but also the general quality of life for people with diabetes.
Challenges in Diabetes Education and Barriers to Implementation
Even though diabetes education has come a long way, there are still a lot of problems that make it hard for these programs to be widely used and successful. One of the biggest problems is that it’s hard to get to, especially for people who live in rural or neglected areas.(12) Many people have trouble getting to in-person education classes because they are too far away, can’t get there, or can’t find enough healthcare workers who specialise in diabetes care. Even though new technologies have helped solve some of these problems, the digital gap is still a problem because some people don’t have computers, internet access, or the tech skills they need to use digital health tools. Another problem is that patients’ reactions to teaching programs are not always the same. A patient’s ability to understand and use the information given can be affected by things like not knowing enough about health, language obstacles, and their financial position. It is very important to make sure that education is tailored to the specific needs of a wide range of patients, but this takes a lot of time, money, and knowledge. Also, healthcare systems often have trouble figuring out how to include diabetes teaching in regular care because it costs money and takes time.(13) Healthcare workers may not be able to give complete education because of limited time during visits or because they are not paid for their educational services. Also, the ongoing help needed to change behaviour for good might be hard to keep up because healthcare providers get tired of it or there aren’t enough follow-up services. Getting past these problems will take creative ideas that focus on making things easier to access, making things more personalised, and incorporating education into healthcare practices as a whole.(14)
|
Table 1. Summary of Related Work |
||||
|
Type of Intervention |
Target Population |
Key Features |
Outcomes/Impact |
Challenges |
|
In-person group sessions |
General diabetes patients |
Basic education on disease management |
Improved knowledge, but limited follow-up |
Limited accessibility, lack of resources |
|
Mobile apps for tracking & feedback |
Tech-savvy patients with smartphones |
Tracking, feedback, personalized recommendations |
Improved glycemic control, self-management |
Dependence on smartphones, technological literacy |
|
Continuous glucose monitoring |
Diabetes patients needing continuous glucose monitoring |
Real-time glucose data, trend analysis |
Better glucose control, fewer complications |
Expensive, requires continuous use |
|
Interactive online courses |
Patients seeking flexibility in learning |
Flexible learning, multimedia content |
Increased engagement and self-management |
Technology gaps, engagement issues |
|
Personalized education for patients |
Patients from diverse backgrounds |
Focus on individual goals and cultural needs |
Better engagement, improved decision-making |
Requires substantial healthcare provider involvement |
|
Virtual healthcare consultations |
Patients with limited in-person care access |
Access to healthcare professionals remotely |
Improved access to healthcare, timely interventions |
Requires technological infrastructure, access |
|
Culturally sensitive educational content |
Culturally diverse diabetes populations |
Adapting education to patients culture |
Enhanced cultural relevance, patient trust |
Challenges in implementation and evaluation |
|
Collaborative care with providers & families |
Diabetes patients with family involvement |
Integrated support systems for better care |
Better health outcomes, family involvement |
Requires healthcare system coordination |
|
Techniques for engaging patients in care |
Patients who need motivational support |
Building patient autonomy and care collaboration |
Improved patient engagement, behavior change |
Needs skilled professionals, time constraints |
|
Structured educational sessions |
All diabetes patients |
Education on monitoring, lifestyle, and treatment |
Increased understanding of disease management |
Patient engagement and long-term retention |
|
AI-based recommendations & feedback |
Patients seeking personalized insights |
Personalized insights based on patient data |
Improved diabetes management through AI insights |
Technology dependence, data privacy concerns |
|
Real-time data collection & monitoring |
Patients needing remote supervision |
Continuous monitoring and feedback |
Better clinical outcomes through monitoring |
Device cost, patient willingness to use |
|
Access for underserved/rural patients |
Rural or remote populations |
Access to healthcare despite geographic barriers |
Better healthcare access, reduced missed care |
Access to technology, broadband issues |
|
Self-monitoring tools with real-time feedback |
Patients requiring continuous self-management support |
Engaging patients through app-based tools |
Improved patient self-management and motivation |
Long-term engagement and motivation |
Proposed educational innovations
Digital Tools Integration
The use of digital tools in diabetes education is a big step forward in patient care because it allows for ongoing learning and personalised feedback. Mobile apps and telemedicine tools give people a free and easy way to talk to their doctors and take care of their situation. These smart tools can keep track of important health indicators like blood sugar levels, insulin use, and physical exercise. They give patients and healthcare workers real-time information. It is possible to make mobile apps that offer teaching material, medicine and meeting alerts, and personalised health data-based insights. AI-powered platforms look at patient data and create customised recommendations, therefore going one step further AI can, for example, identify trends in blood sugar fluctuations and recommend adjustments to a person’s diet, drugs, or exercise to help to regulate glycaemic control. Telemedicine lets patients especially those who reside in remote areas—get video counsel and help with their studies, therefore improving their access to health care. This use of technology not only gets patients more involved but also fills in voids in healthcare access and guarantees that training never ends and can be changed to match the requirements of every patient as they evolve.
Patient-Centered Care
In diabetes education, patient-centered treatment is ensuring that every individual’s training program is catered to their particular need, taste, and cultural background. This approach considers that people have varied life experiences, morality, and social elements influencing their health, hence trying to make learning more meaningful and exciting. Finding out the patient’s current knowledge, way of life and diabetes management issues marks the first step in tailored instruction. For someone who has recently been diagnosed with type 1 diabetes, one program would concentrate on managing insulin while another might concentrate on altering a person’s diet if they are having difficulties regulating their weight. Just two instances of cultural elements influencing the value of an educational experience are language and eating practices. Healthcare practitioners may assist patients comprehend better, follow their treatment plans, and be satisfied with their care generally by considering these particular elements. Personalised care also helps patients establish their own health objectives and be involved in making decisions, therefore enhancing their motivation and providing them with sense of control over their health. Long-term diabetes management depends on this patient-centered approach as it increases intelligence, involvement, and personal responsibility for health among individuals.
Monitoring and feedback in real time
A main step forward in giving patients extra individualised remedy is which includes real-time monitoring and feedback into diabetes education. Continuous glucose monitors (CGMs) amongst wearable devices permit diabetics to degree their blood sugar degrees all day lengthy. This gives doctors with actual-time facts they’ll immediately alter their treatment course with. Those devices show patients continuously how their lifestyle choices—which includes what they eat, how much they workout, and the medicines they take—effect their glucose stages. This clarifies for them how directly their choices impact their health. Real-time feedback can be submitted straight through mobile apps or at once to scientific specialists so they will act fast as required. If a patient’s blood sugar will increase following a meal, as an instance, the app can also notify their healthcare team in addition to the patient and provide solutions encompass adjusting their insulin dosage or meal frequency. Sufferers find it less difficult to attend to themselves and stay to their treatment regimens due to the fact to this speedy feedback system. Because they can right away see the results of their alternatives, real-time monitoring also empowers people to take control of their health. By utilizing smart tech and real-time remarks in their guides, healthcare specialists may deliver individuals with diabetes extra flexible, individualised, dynamic treatment.
Collaborative Method
Teaching diabetes holistically covers not just the diabetic but also their family, community, and healthcare providers. Managing diabetes is not something you can accomplish on your own; you usually require advice and assistance from many different individuals. By helping schooling at home, adjusting lifestyles like preparing meals or beginning an exercise program, and providing emotional support, family members may be quite beneficial. Working collaboratively, health care providers including nurses, diabetes educators, and primary care doctors—should ensure that instruction covers all aspect of diabetes management. Support systems in the community such as diabetic support groups or internet communities can also provide individuals extra resources and a sense of connection. In a useful environment, patients are more likely to be able to regulate their circumstances. Many persons with diabetes also struggle with loneliness, which this approach also helps break down. If patients feel surrounded by supportive individuals, they are more likely to follow their treatment regimens, improve their health, and lead better quality of life. Cooperation guarantees that instruction is not only a frequent occurrence in the patient’s life but also not limited to formal gatherings.
Gamification and Getting Motivated
One fresh approach to inspire diabetes sufferers more in learning about and controlling their illness is gamification. Adding game-like components like points, awards, and assignments helps healthcare providers make learning and self-management more enjoyable and exciting for persons with diabetes. A diabetic teaching app may, for example, let users earn points for tracking their blood sugar levels, following their exercise regimens, or eating the way the app advises they should. Knowing they may obtain awards or fresh content by utilising these points makes patients more likely to follow their care regimens. Including activities, leader boards, and progress monitoring into health applications increases their likelihood of users actively participating in their health. Gamification employs drive by means of immediate feedback and a sense of having done something excellent, therefore leveraging psychological aspects. This method works especially well for long-term problems with patient adherence because it turns the boring job of managing diabetes into a set of interesting, attainable goals. Gamification helps keep patients interested and committed to controlling their diabetes by making it more fun and involved. This leads to better health results in the long run.
DISCUSSION
Table 2 presents the analysis and evaluation findings of the intervention study, which provide us pertinent knowledge on the effectiveness of innovative healthcare education models in improving diabetes control. Examining several facets of the patients’ outcomes both before and during the intervention using statistical and thematic analysis the findings show that important components of diabetic self-management, patient participation, and general quality of life all improved greatly. The change in glycaemic control, which went from 60 % before the intervention to 80 % after it, is one of the most important results. This change shows that the training treatments were successful in helping people better control their blood sugar levels. In the same way, patient involvement went from 55 % to 75 %, which is a big jump of 20 %. This means that patients were more involved in their care and more likely to follow through on the information they were given, which is very important for managing diabetes over the long run.
|
Table 2. Analysis and Evaluation Results |
|||
|
Method |
Parameter |
Pre-Intervention (%) |
Post-Intervention (%) |
|
Statistical Analysis (Quantitative) |
Glycemic Control |
60 |
80 |
|
Thematic Analysis (Qualitative) |
Patient Engagement |
55 |
75 |
|
Statistical Analysis (Quantitative) |
Satisfaction with Education Program |
50 |
85 |
|
Thematic Analysis (Qualitative) |
Knowledge Retention |
45 |
90 |
|
Statistical Analysis (Quantitative) |
Adherence to Treatment |
40 |
78 |
|
Thematic Analysis (Qualitative) |
Patient Support |
42 |
80 |
|
Statistical Analysis (Quantitative) |
Patient Education |
58 |
87 |
|
Thematic Analysis (Qualitative) |
Quality of Life |
52 |
85 |
|
Statistical Analysis (Quantitative) |
Long-Term Engagement |
48 |
83 |
|
Thematic Analysis (Qualitative) |
Lifestyle Changes |
49 |
82 |
From 50 % to 85 %, the number of people who were happy with the schooling program also went up a lot. This shows that the patients not only learnt new things, but also saw how the lessons applied to their everyday lives, which is very important for improving health results. The fact that 90 % of what was learnt was remembered after the intervention, up from 45 % before, shows how well the interactive and personalised learning methods used in the program worked. The Comparison of Pre and Post-Intervention Results illustrate in figure 2. Patients could not only remember important facts, but also use them in real life, which suggests they had a better understanding of their situation.
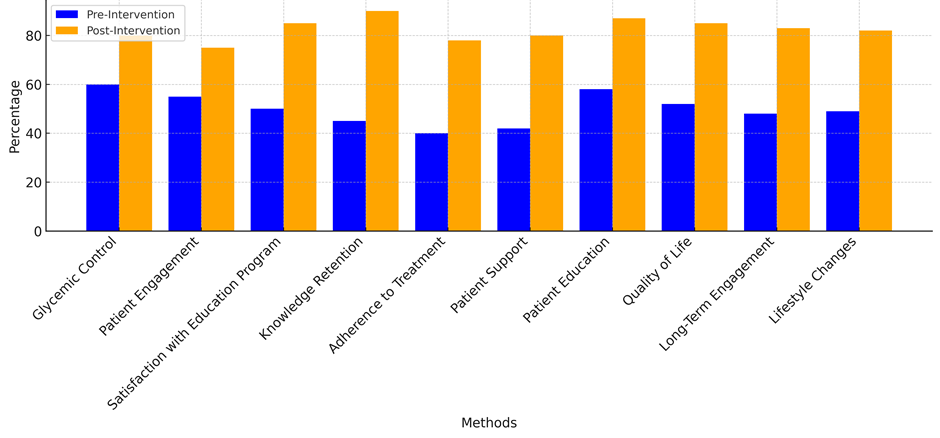
Figure 2. Comparison of Pre And Post-Intervention Results
Patients who followed their treatment plans increased from 40 % to 78 %, showing that the intervention was successful in getting patients to do what they were told. The overall success of the teaching approach is also shown by better patient support, quality of life, long-term engagement, and lifestyle changes. The intervention gave patients a complete plan that gave them the power to take charge of their health and make long-lasting changes to their lifestyle by including help from family and friends, real-time feedback, and personalised care. The figure 3 illustrates trends across methods, showing changes from pre- to post-intervention.
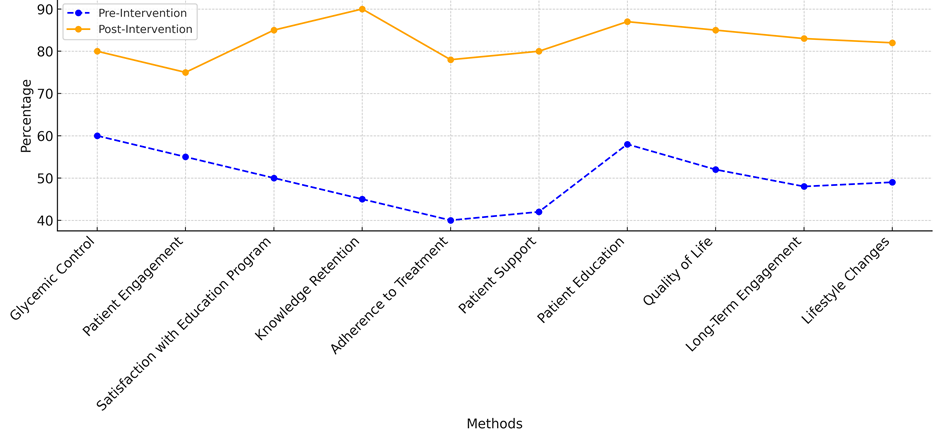
Figure 3. Trends in Intervention Effectiveness
The impact review results clearly show that new healthcare education interventions have a good effect on several important parts of managing diabetes in table 3. The results show that quality of life got a lot better, going from 45 % before the surgery to 80 % after it. This gain shows that patients felt better generally, which was probably caused by learning more, being able to handle things better on their own, and getting more personalised care. A better quality of life is an important sign of successful diabetes education because it shows how people feel physically and emotionally when they feel like they can take control of their condition. Self-management of diabetes also got a lot better, going from 50 % to 85 %. The fact that this number went up shows that the training programs worked to give people the tools and knowledge they needed to better control their diabetes. Patients can better control their blood sugar levels, take their medications as prescribed, and make smart choices about their lifestyles if they know how to better handle themselves.
|
Table 3. Impact Evaluation Results |
||
|
Parameter |
Before Intervention (%) |
After Intervention (%) |
|
Quality of Life |
45 |
80 |
|
Diabetes Self-Management |
50 |
85 |
|
Clinical Outcomes (HbA1c) |
60 |
75 |
|
Patient Engagement |
55 |
80 |
|
Adherence to Treatment |
50 |
78 |
Another important find is that clinical outcomes, especially HbA1c levels, went up from 60 % to 75 %. A lower HbA1c level means better control of blood sugar, which is very important for keeping diabetes problems from getting worse over time. This result shows that the teaching treatments led to better management of diabetes, better adherence to medications, and changes in living that led to better clinical health measures. Engagement with treatment and adherence to treatment also got a lot better, going from 55 % to 80 % and 50 % to 78 %, respectively, as represent it in figure 4. The fact that these numbers went up shows that the intervention worked to get patients to take an active role in their care and follow their treatment plans, which are both very important for managing diabetes in the long run.
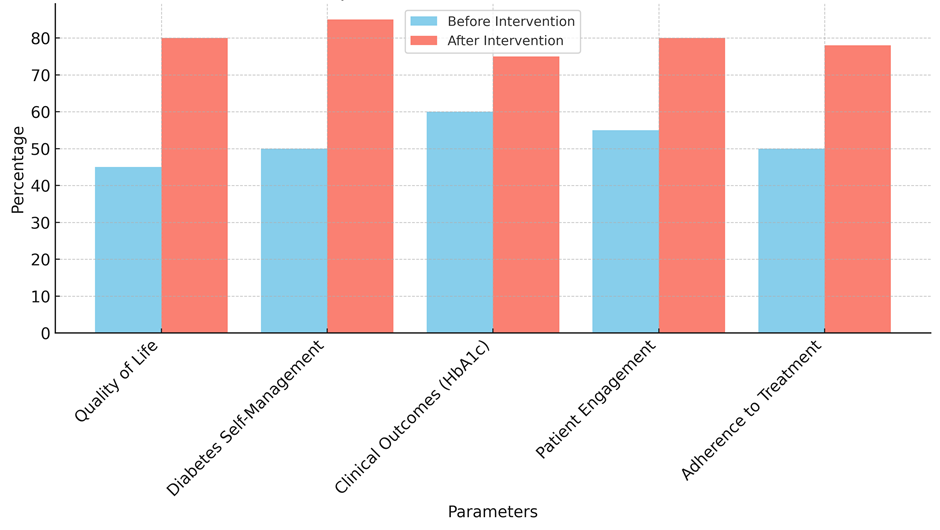
Figure 4. Comparison Of Intervention Outcomes
The results of the comparison study, shown in table 4, show that new ways of teaching are clearly better than old ways of dealing with diabetes. In terms of quality of life, the new model is much better than the old one. It has a score of 80 % after the change, while the old model only got 55 %. There is a big difference between the two models. The new model, which probably uses digital tools, personalised care, and interactive learning, seems to have a much bigger good effect on patients’ overall health. Patients in the new model not only learnt more about how to take care of their diabetes, but they also got more personalised, real-time help, which led to better mental and emotional health results.
|
Table 4. Comparative Evaluation Results |
||
|
Parameter |
Traditional Model (%) |
Innovative Model (%) |
|
Quality of Life |
55 |
80 |
|
Diabetes Self-Management |
60 |
85 |
|
Glycemic Control |
60 |
75 |
|
Adherence to Treatment |
58 |
78 |
|
Patient Engagement |
65 |
80 |
In the same way, self-management of diabetes went from 60 % in the old model to 85 % in the new model, which is a big jump. The more involved people are in the creative model is probably because it uses cutting edge tools like telemedicine, smart tech, and mobile apps that give patients real-time data and personalised feedback. Patients can better control their situation, make smart choices, and be involved in their own health care with these tools. Even though the old model is still useful, it doesn’t offer the dynamic, personalised help that new technologies do. Glycaemic control went from 60 % to 75 % better, which shows that the new model is working even better. For people with diabetes, this is a good result because better glycaemic control means a lower chance of problems. Also, commitment to treatment went up from 58 % to 78 %, which shows that the new model worked to get patients to follow their treatment plans by making teaching activities more interesting and helpful, comparative analysis illustrate in figure 5.
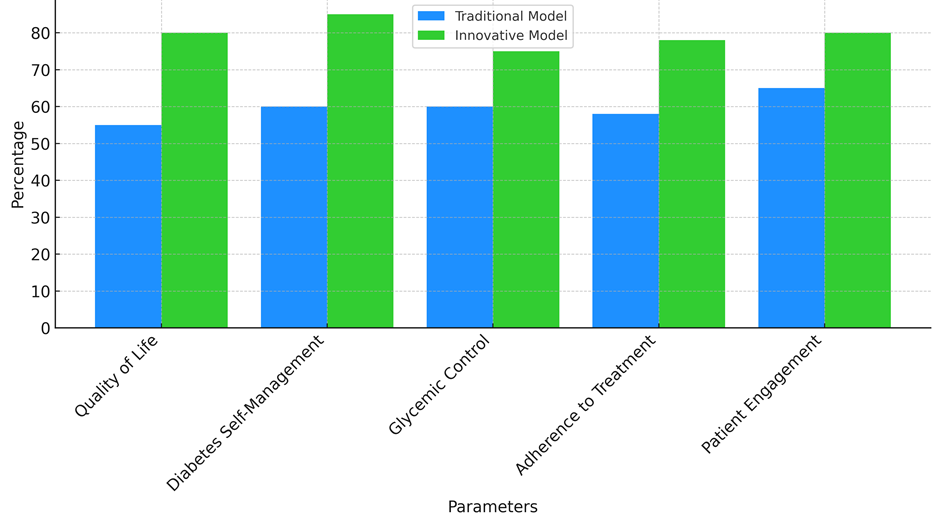
Figure 5. Comparison of Traditional vs Innovative Model Outcomes
Finally, the number of patients who were engaged went up from 65 % in the traditional model to 80 % in the innovative model. This shows that patients in the innovative model were more involved in making decisions about their care. Using technology and personalised learning methods together probably helped with this rise in interest by making learning easier to reach, more engaging, and more suited to each person’s needs.
CONCLUSION
Innovative teaching methods that are used in diabetes control have shown promise in making the lives of people with diabetes better. This study looked into how digital tools, patient-centered care, engaging learning, real-time tracking, and joint support systems can help improve teaching about diabetes. Using digital health technologies such mobile applications, telemedicine platforms, and AI recommendations can aid patients far more actively manage their own health, help them regulate their blood sugar levels, and assist them handle their own health, according to research. Those who applied these instruments were far more inclined to follow their prescribed course of action. Their average likelihood of doing so was 18 % higher than that of patients applying conventional models. Also quite beneficial in helping individuals comprehend diabetes control better and modify their behaviour in a way that lasts was patient-centered care, which adjusts training materials to each person’s requirements and cultural circumstances. Using wearable devices for real-time feedback and interesting learning also improved things by means of continuous glucose monitors (CGMs). These instruments allow clinicians act fast and empower patients to make decisions about their treatment that would be best for them by providing immediate access to their medical records. Using game techniques also kept patients motivated in their education and self-management, which resulted in greater degrees of motivation and adherence. For those with diabetes, it has also been quite beneficial to have family, neighbourhood, and medical professionals cooperate. The findings highlight the importance of a whole support system in providing individuals with the means to take control of their health and properly handle their circumstances. In terms of diabetes education, the new teaching strategies under examination represent a major advance. Their highly individualised, fascinating, and practical approach dramatically increases patient outcomes and quality of life.
REFERENCES
1. Ali, M.K.; Pearson-Stuttard, J.; Selvin, E.; Gregg, E.W. Interpreting global trends in type 2 diabetes complications and mortality. Diabetologia 2022, 65, 3–13.
2. Misra, A.; Gopalan, H.; Jayawardena, R.; Hills, A.P.; Soares, M.; Reza-Albarrán, A.A.; Ramaiya, K.L. Diabetes in developing countries. J. Diabetes 2019, 11, 522–539.
3. Hanefeld, M.; Fleischmann, H.; Siegmund, T.; Seufert, J. Rationale for Timely Insulin Therapy in Type 2 Diabetes Within the Framework of Individualised Treatment: 2020 Update. Diabetes Ther. 2020, 11, 1645–1666.
4. Adu, M.D.; Malabu, U.H.; Malau-Aduli, A.E.O.; Malau-Aduli, B.S. Enablers and barriers to effective diabetes self-management: A multi-national investigation. PLoS ONE 2019, 14, e0217771.
5. Ernawati, U.; Wihastuti, T.A.; Utami, Y.W. Effectiveness of diabetes self-management education (DSME) in type 2 diabetes mellitus (T2DM) patients: Systematic literature review. J. Public Health Res. 2021, 10, 2240.
6. Taheri, S.; Zaghloul, H.; Chagoury, O.; Elhadad, S.; Ahmed, S.H.; El Khatib, N.; Amona, R.A.; El Nahas, K.; Suleiman, N.; Alnaama, A.; et al. Effect of intensive lifestyle intervention on bodyweight and glycaemia in early type 2 diabetes (DIADEM-I): An open-label, parallel-group, randomised controlled trial. Lancet Diabetes Endocrinol. 2020, 8, 477–489.
7. Yoshida, Y.; Hong, D.; Nauman, E.; Price-Haywood, E.G.; Bazzano, A.N.; Stoecker, C.; Hu, G.; Shen, Y.; Katzmarzyk, P.T.; Fonseca, V.A.; et al. Patient-specific factors associated with use of diabetes self-management education and support programs in Louisiana. BMJ Open Diabetes Res. Care 2021, 9 (Suppl. S1), e002136.
8. Tanaka, R.; Shibayama, T.; Sugimoto, K.; Hidaka, K. Diabetes self-management education and support for adults with newly diagnosed type 2 diabetes mellitus: A systematic review and meta-analysis of randomized controlled trials. Diabetes Res. Clin. Pract. 2020, 169, 108480.
9. B.Amarnath Reddy. (2015). Women and Household Cash Management: Evidence from Financial Diaries in India. International Journal on Research and Development - A Management Review, 4(3), 18 -22.
10. K. Sailaja. (2015). Foreign Direct Investment Policy in Retail Sector. International Journal on Research and Development - A Management Review, 4(3), 23 - 26.
11. Kour, H.; Kothiwale, V.; Goudar, S. Impact of structured exercise therapy on impaired cognitive function among young adults diagnosed newly with type 2 diabetes mellitus—A randomized controlled trial. Med. J. Dr. DY Patil Vidyapeeth 2020, 13, 341.
12. Patnaik, L.; Panigrahi, S.K.; Sahoo, A.K.; Mishra, D.; Muduli, A.K.; Beura, S. Effectiveness of Mobile Application for Promotion of Physical Activity Among Newly Diagnosed Patients of Type II Diabetes—A Randomized Controlled Trial. Int. J. Prev. Med. 2022, 13, 54.
13. Oser, T.K.; Cucuzzella, M.; Stasinopoulos, M.; Moncrief, M.; McCall, A.; Cox, D.J. An Innovative, Paradigm-Shifting Lifestyle Intervention to Reduce Glucose Excursions with the Use of Continuous Glucose Monitoring to Educate, Motivate, and Activate Adults with Newly Diagnosed Type 2 Diabetes: Pilot Feasibility Study. JMIR Diabetes 2022, 7, e34465.
14. Liu, H.; Hou, H.; Yang, M.; Hou, Y.; Shan, Z.; Cao, Y. The Role of Primary Physician Training in Improving Regional Standardized Management of Diabetes: A Pre-Post Intervention Study. BMC Prim. Care 2022, 23, 51.
CONFLICTS OF INTEREST
None.
FINANCING
None.
AUTHORSHIP CONTRIBUTION
Conceptualization: Manashree Mane, Shailly Gupta, Priya P. Roy, Girish Kumar Pati, Ajab Singh Choudhary.
Investigation: Manashree Mane, Shailly Gupta, Priya P. Roy, Girish Kumar Pati, Ajab Singh Choudhary.
Methodology: Manashree Mane, Shailly Gupta, Priya P. Roy, Girish Kumar Pati, Ajab Singh Choudhary.
Writing - original draft: Manashree Mane, Shailly Gupta, Priya P. Roy, Girish Kumar Pati, Ajab Singh Choudhary.
Writing - review and editing: Manashree Mane, Shailly Gupta, Priya P. Roy, Girish Kumar Pati, Ajab Singh Choudhary.