doi: 10.56294/hl2023305
ORIGINAL
Analyzing the Effect of Quality of Life Assessments on Healthcare Delivery Frameworks
Análisis del efecto de las evaluaciones de la calidad de vida en los marcos de prestación de asistencia sanitaria
Vaishali V. Raje1 ![]() , Manti Debnath2
, Manti Debnath2 ![]() , Siba Prasad Dalai3
, Siba Prasad Dalai3 ![]() , Renuka Jyothi.S4
, Renuka Jyothi.S4 ![]() , Vandana Sharma5
, Vandana Sharma5 ![]()
1Krishna Institute of Medical Sciences, Krishna Vishwa Vidyapeeth “Deemed to be University”, Dept. of Preventive and Social Medicine, Taluka-Karad, Dist-Satara, Maharashtra, India.
2School of Allied Health Sciences, Noida International University, Greater Noida, Uttar Pradesh, India.
3IMS and SUM Hospital, Siksha ‘O’ Anusandhan (Deemed to be University), Department of General Medicine, Bhubaneswar, Odisha, India.
4JAIN (Deemed-to-be University), Department of Biotechnology and Genetics, Bangalore, Karnataka, India.
5Arya College of Pharmacy, Jaipur, Rajasthan, India.
Cite as: Raje VV, Debnath M, Dalai SP, Jyothi.S R, Sharma V. Analyzing the Effect of Quality of Life Assessments on Healthcare Delivery Frameworks. Health Leadership and Quality of Life. 2023; 2:305. https://doi.org/10.56294/hl2023305
Submitted: 29-05-2023 Revised: 25-08-2023 Accepted: 11-11-2023 Published: 12-11-2023
Editor: PhD.
Prof. Neela Satheesh ![]()
ABSTRACT
Introduction: nowadays, evaluating how well healthcare is serving patients depends much on quality of life (QoL) assessments. Including quality of life (QoL) indicators into healthcare systems might enable individuals to make better decisions, provide patients better treatment, and develop new approaches of treating them. Focussing on how they influence patient outcomes and how well healthcare operates, this study investigates how quality of life (QoL) exams affect the methods of delivery of healthcare.
Method: using a mixed-methods approach, qualitative interviews with healthcare management and employees combined with quantitative patient data analysis. Electronic health records (EHRs) provided us with QoL ratings, which we examined in light of clinical outcomes, patient satisfaction, and additionally conducted were interviews to learn people’s opinions on and applications for QoL criteria in clinical settings.
Results: reveal that by highlighting what matters to the patient and facilitating their communication with their healthcare providers, quality of life (QoL) assessments greatly increase the likelihood of tailored treatment. Using QoL data also helped make better decisions about how to use resources and what kind of care to give. There were, however, problems found when trying to add QoL data to current systems, mostly with standardising and communicating the data.
Conclusion: quality of life (QoL) surveys are a useful way to improve the way healthcare is delivered because they help with patient-centered care, making decisions, and allocating resources. Getting past integration problems can make them even more useful in professional settings.
Keywords: Quality of Life; Healthcare Delivery; Patient Outcomes; Resource Allocation; Patient-Centered Care; Healthcare Frameworks.
RESUMEN
Introducción: hoy en día, la evaluación de la calidad de la asistencia sanitaria depende en gran medida de las valoraciones de la calidad de vida (CdV). La inclusión de indicadores de calidad de vida (CdV) en los sistemas sanitarios podría permitir tomar mejores decisiones, ofrecer a los pacientes mejores tratamientos y desarrollar nuevos enfoques para tratarlos. Centrándose en cómo influyen en los resultados de los pacientes y en el buen funcionamiento de la asistencia sanitaria, este estudio investiga cómo afectan los exámenes de calidad de vida (CdV) a los métodos de prestación de asistencia sanitaria.
Método: mediante un enfoque de métodos mixtos, entrevistas cualitativas a directivos y empleados de la sanidad combinadas con análisis cuantitativos de datos de pacientes. Las historias clínicas electrónicas (HCE) nos proporcionaron valoraciones de la calidad de vida, que examinamos a la luz de los resultados clínicos, la satisfacción de los pacientes y, además, realizamos entrevistas para conocer las opiniones de la gente y las aplicaciones de los criterios de calidad de vida en el ámbito clínico.
Resultados: revelan que, al poner de relieve lo que importa al paciente y facilitar su comunicación con los profesionales sanitarios, las evaluaciones de la calidad de vida (CdV) aumentan enormemente la probabilidad de un tratamiento adaptado. El uso de datos de calidad de vida también ayudó a tomar mejores decisiones sobre cómo utilizar los recursos y qué tipo de atención prestar. Sin embargo, al intentar incorporar los datos de calidad de vida a los sistemas actuales, surgieron algunos problemas, sobre todo a la hora de estandarizarlos y comunicarlos.
Conclusión: las encuestas sobre calidad de vida son útiles para mejorar la asistencia sanitaria, ya que ayudan a centrarla en el paciente, a tomar decisiones y a asignar recursos. Superar los problemas de integración puede hacerlas aún más útiles en entornos profesionales.
Palabras clave: Calidad de Vida; Prestación de Asistencia Sanitaria; Resultados en Pacientes; Asignación de Recursos; Atención Centrada en el Paciente; Marcos de Asistencia Sanitaria.
INTRODUCTION
These days, Quality of Life (QoL) tests are becoming more and more important in judging healthcare systems because they show more than just clinical results about a patient’s general health. Healthcare has historically largely focused on gauging physical health, such as the speed of disease transmission and the survival rates. To fully understand a patient’s health—which comprises their mental, social, and emotional aspects of life—QoL tests are therefore quite vital. These tests have been demonstrated to provide valuable insights on the personal issues and circumstances of patients, which might not always be evident from clinical assessments by themselves. Including QoL into healthcare delivery systems helps treatment plans to be more patient-centered by being able to be changed to fit each individual’s particular requirements and wishes. More and more individuals have come to see in the past several years how crucial quality of life (QoL) surveys are for guiding medical decisions. Knowing a patient’s quality of life (QoL) can let clinicians create more tailored and successful treatment programs. Doctors can involve patients in shared decision-making by including patient-reported outcomes (PROs) connected to quality of life, therefore improving patient happiness and increasing likelihood of treatment plan adherence. Furthermore, QoL measurements are quite beneficial for monitoring how medications influence daily life of patients. They assist doctors in determining if their activities truly improve patients’ quality of life or only extend their lifespan or aid to control their diseases.
Including QoL data into healthcare technologies can be challenging, though. Many healthcare institutions still use antiquated disease-specific policies, and they lack always the means to apply patient-reported quality of life outcomes in a methodical approach. Using these parameters in daily life might be more difficult depending on issues with standardising data, allowing electronic health records (EHRs) to interact, and the instruments used to gauge quality of life (QoL). While their usage in emergency or short-term care settings is still under development, QoL assessments are extensively employed in management of chronic disorders. These challenges make the objective of this study to investigate the part that quality of life (QoL) tests play in the systems that offer healthcare, namely how they impact patient results, treatment options, and resource allocation. The study aims to show how QoL data changes healthcare practices, makes patients happier, and makes better use of resources by looking at the experiences of both patients and healthcare workers. Additionally, it will look into the problems that stop execution from going smoothly and suggest ways to fix these issues so that QoL tests can be better integrated into healthcare systems. The main point is to stress that QoL can improve not only professional care but also the whole healthcare experience, which helps healthcare become more patient-centered and whole.
Related work
Studies on quality of life (QoL) in healthcare settings have attracted a lot of attention, particularly on how they might enable patients to perform better and alter the delivery of healthcare. QoL assessments have evolved in many healthcare systems from a supplementary tool to a vital component of patient treatment.(1) Research in this field initially focused largely on developing and testing measures for measuring patients’ quality of life (QoL), therefore gauging their perspective on their circumstances. Early initiatives helped to open the path for the use of QoL measurements in clinical settings, particularly in the management of chronic illnesses where they are seen as equally significant as clinical symptoms.(2) More lately, studies on patient-centered treatment approaches have demonstrated the significance of quality of life. Studies have demonstrated that adding patient-reported outcomes (PROs) into treatment plans increases patient involvement and satisfaction.(3) Like QoL assessments, PROs have been demonstrated to assist patients and healthcare professionals in bettering their communication with one another, thereby resulting in more tailored therapies considering individual interests and values.(4) Better adherence to treatment programs and less hospital visits have also been associated to using QoL data in professional decision-making.(5) Quality of life (QoL) tests have been pushed to be included to electronic health records (EHRs) in the past few years. Real-time access to patient data made possible by this will enable more effective healthcare services.(6) Making ensuring that QoL metrics are the same across various healthcare systems remains a challenge even with possible advantages. Because EHR systems don’t always work with one another and the instruments used to evaluate QoL tests aren’t always consistent,(7) it’s difficult for them to be extensively utilised. Some research have indicated that using the optimal QoL measures for various illnesses and patient groups becomes more difficult in daily clinical practice since opinions on them vary.(8)
Research on the relationship between clinical findings and quality of life measures has grown more thorough. Higher quality of living has been connected to improved general health outcomes including decreased mortality rates and improved functional standing.(9) Often providing information not found by clinical testing alone, studies in cancer have demonstrated that QoL assessments may be utilised as early warning signals of whether a therapy is working or not.(10) Similarly, depending on daily health, QoL data has proven quite beneficial in guiding modifications to treatment strategies for persons with chronic conditions including diabetes and heart disease.(11) Furthermore under investigation is how best to apply QoL ratings to enhance the usage of resources in healthcare. By indicating which patients can gain from additional support services, QoL measurements might assist to prioritise treatment delivery. This guarantees sensible use of resources.(12) In healthcare environments with limited resources, where QoL statistics can guide clinicians in choosing which patients require more extensive treatment, this is particularly crucial.(13) Furthermore, some research have indicated that QoL assessments can assist in the identification of healthcare gaps, so providing information on the needs of underprivileged populations and so improving the fairness of treatment.(14) Although these outcomes are positive, many locations still do not fully utilise QoL tests in altering the delivery of healthcare. Using QoL data in regular clinical practice might be challenging; so, present QoL technologies need to be verified and developed. This indicates that in this field additional research and development are required.(15) Some healthcare organisations have thus begun to evaluate the use of real-time QoL evaluations coupled with AI and machine learning techniques to forecast how patients will fare and create more efficient treatment plans.(16)
|
Table 1. Related Work Summary |
||||
|
Study Focus |
Key Findings |
Research Methods |
Challenges Identified |
Implications for Healthcare |
|
Development and Validation of QoL Instruments |
QoL instruments were validated to capture patients’ subjective experiences. |
Survey-based validation and psychometric analysis. |
Need for universal QoL measurement standards. |
Improves patient care by considering all aspects of well-being. |
|
Role of QoL in Patient-Centered Care |
Patient-centered care improved through enhanced communication and shared decision-making. |
Qualitative studies with patient and provider interviews. |
Barriers to effective communication between providers and patients. |
Enhances patient satisfaction and care outcomes. |
|
Impact of PROs on Treatment Adherence |
QoL assessments improve treatment adherence and engagement with patients. |
Quantitative analysis of treatment adherence data. |
Data collection methods can be burdensome and inconsistent. |
Promotes patient engagement and better health management. |
|
Integration of QoL into EHR Systems |
EHR integration streamlines access to QoL data but faces interoperability challenges. |
Case studies on electronic health record integration. |
EHR integration faces technical barriers and system incompatibility. |
Streamlines patient data handling and enhances decision-making. |
|
Challenges in Standardization of QoL Tools |
Data standardization is still a major issue, affecting adoption in clinical practice. |
Comparative studies across different QoL tools and standards. |
Variability in QoL measures across different healthcare settings. |
Calls for the establishment of standardized QoL instruments. |
|
Relationship Between QoL and Clinical Outcomes |
QoL improvements correlate with better health outcomes and functional status. |
Longitudinal studies on clinical outcomes and QoL data. |
Difficulty in establishing a clear link between QoL and health outcomes. |
Improves clinical decision-making and health outcomes. |
|
QoL as an Indicator of Treatment Success in Oncology |
QoL assessments in oncology provide early indicators of treatment effectiveness. |
Clinical trials in oncology with QoL monitoring. |
Lack of long-term data on the effectiveness of QoL-guided treatments. |
Offers a more nuanced understanding of treatment effectiveness. |
|
QoL in Chronic Disease Management |
QoL data guides treatment adjustments for chronic disease management. |
Patient monitoring in chronic disease management. |
Lack of standardized protocols for integrating QoL into treatment plans. |
Supports personalized treatment approaches and better health management. |
|
QoL and Resource Allocation in Healthcare |
QoL assessments help prioritize resource allocation and identify patients in need of support. |
Resource allocation studies based on QoL metrics. |
Healthcare resource constraints and inefficiencies in prioritizing QoL-based interventions. |
Informs policy and care prioritization in resource-constrained settings. |
|
QoL and Healthcare Disparities |
QoL data highlights healthcare disparities and aids in addressing inequities. |
Population health studies to assess healthcare disparities. |
Limited data on underserved populations and their QoL needs. |
Aids in reducing healthcare disparities and ensuring equitable care. |
|
Validation of QoL Instruments in Different Populations |
Further validation of QoL tools is needed for different conditions and populations. |
Cross-sectional studies on QoL tool validation. |
Lack of validated QoL instruments for diverse patient populations. |
Ensures that QoL tools are more widely applicable across healthcare contexts. |
|
Role of AI and Machine Learning in QoL Data |
AI and machine learning are being explored to predict patient outcomes using QoL data. |
AI-based modeling and predictive analytics with QoL data. |
Technical challenges in analyzing large-scale QoL data using AI. |
Optimizes clinical predictions and outcomes with advanced data analytics. |
|
QoL as a Predictor of Hospital Readmission |
QoL assessments predict hospital readmission risks, improving care management. |
Predictive modeling studies on readmission risks using QoL. |
Predictive validity of QoL in readmission outcomes still under exploration. |
Improves post-treatment care by identifying high-risk patients early. |
|
QoL in Acute vs. Chronic Care Settings |
Acute care settings face challenges in using QoL data due to time constraints. |
Observational studies on QoL use in acute care settings. |
Limited use of QoL in time-sensitive acute care situations. |
Enhances care quality in both chronic and acute settings. |
METHOD
Study strategy
The study will apply a mixed-methods approach combining qualitative and quantitative techniques in order to get a whole picture of how Quality of Life (QoL) assessments impact healthcare delivery systems. In the quantitative sense, hospital records and patient-reported outcomes (PROs) will be examined. This will enable one to evaluate measurements of quality of life (QoL) and observe their correlation with outcomes of healthcare. Healthcare professionals, managers, and patients will be questioned in the qualitative component to find out about their experiences with QoL evaluations, how they believe they influence treatment, and the issues arising when attempting to implement these assessments. This approach ensures that the study is well-rounded and provides a better view of the complexities of how QoL is being utilised in healthcare systems by combining factual data with subjective experiences.
Methods for Collecting Data
Data will come from surveys, talks, and Electronic Health Record (EHR) research. Objective data on quality of life (QoL) will be gathered from surveys administered to patients and healthcare professionals using standardised methods such the EQ-5D and SF-36. Interviews with patients, managers, and healthcare professionals will help to ascertain their opinions on the degree to which QoL tests improve clinical practice. EHR data will also be examined to find relationships between health outcomes, treatment strategies, and resource consumption with regard to quality of life ratings. These several kinds of data sources will enable us to get a whole picture of how QoL ratings influence the provision of healthcare.
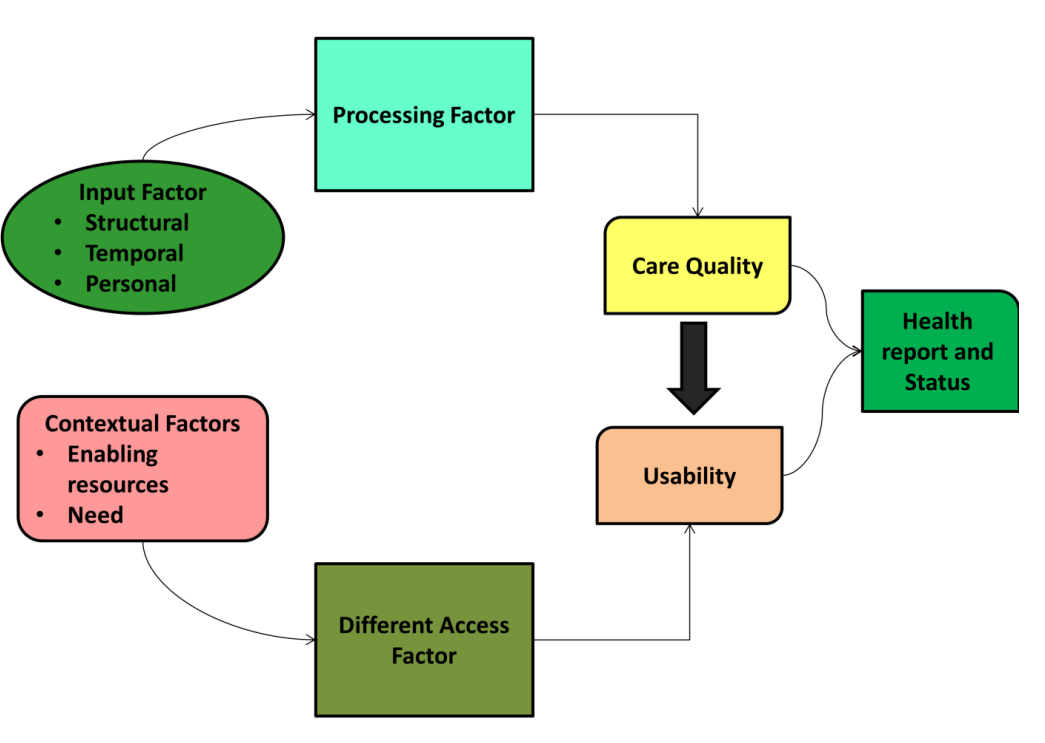
Figure 1. Overview Of conceptual Framework of Quality of Care and Utilization
Figure 1 presents a conceptual framework illustrating the links among the several elements influencing the quality of care and their application. Human, social, and temporal elements influencing healthcare service are part of the “Input Factor”. These elements enter the “Processing Factor,” which subsequently modifies the health report and status as well as the degree of care and, thus, the value of healthcare services. The framework also illustrates how easily one may acquire care and how well elements in the surroundings—including needs and financial situation—may influence them. Stressing the need of ensuring everyone has equal access to health care services, the “different access factor” works with these backdrop elements. This conceptual framework helps one to understand how QoL data alters the way healthcare is delivered for the study topic “Analysing the Effect of Quality of Life Assessments on Healthcare Delivery Frameworks.” By considering the patients’ emotional, social, and physical demands via quality of life assessments, one may enhance the “Input Factor”. These tests then influence the “processing factor” as they guide medical professionals in customising treatment to every individual’s condition.
Population/Sample Description
The study will involve a varied group of people to ensure that the findings may be applied in a range of healthcare environments and with a great spectrum of patients. Groups will consist of patients from basic care, outpatient clinics, and hospitals. Among the several health issues these people will have include cancer, chronic disorders, acute ailments, and others. The research will also include healthcare professional’s doctors, nurses, and other clinicians—who use and evaluate QoL testing. Administrators in charge of monitoring or implementing QoL initiatives into healthcare systems will also be part of the group. The study will try to get a lot of different experiences and points of view so that the results are accurate for all kinds of healthcare situations and patient needs.
Tools and Instruments Used for QoL Assessments
Standardised tools that have been widely proven to work in healthcare research will be used to measure QoL in this study. Tools like the EQ-5D and SF-36 will be used to measure different aspects of QoL, such as movement, self-care, pain, worry, and general health. These tools are made to give accurate, similar information about a wide range of patient groups. For qualitative conversations, semi-structured question guides will be used to focus on how QoL measures affect care for patients and decisions. The information gathered by these tools will be looked at both quantitatively and qualitatively to see if it is statistically significant and to find themes. This will give a full picture of how QoL measures affect healthcare service.
Ethical Considerations and Data Privacy
Any study that involves healthcare needs to think about ethics, but it’s especially important when working with private patient data. All volunteers will give their permission after being fully informed about the study’s goal, their part in it, and how their information will be used. People who take part will be told that it is completely optional and that they can quit at any time without any consequences. To protect the rights of the people who take part in the study, it will follow the ethical rules set by the appropriate institutional review boards (IRBs) or ethics groups. De-identification and anonymisation methods will be used to protect data privacy and make sure that no personal information can be linked back to specific users. In line with data security laws and rules like the Health Insurance Portability and Accountability Act (HIPAA), all data will be saved safely and only authorised staff will be able to access it.
RESULTS
Table 2 shows the basic figures for Quality of Life (QoL) data, which are a list of the most important factors of the study subjects’ general health and happiness. The average QoL number for the group was 65,2, which means that, on average, the people who took part in the study felt moderately well. This number gives you an idea of the data’s main trend, which helps you set a standard to compare against. The median score of 70 is the middle number of the set of scores. This means that half of the people who took part had QoL scores above 70 and the other half had scores below 70. This means that while most participants’ scores fall within a fairly narrow range around the mean, there are a good number of people who have much better or worse QoL results. This variation can help you understand how different the patients’ experiences are in the sample, especially when you’re trying to figure out which groups might need more help or care.
|
Table 2. QoL Descriptive Statistics and Impact On Healthcare Outcomes |
|
|
Parameter |
Value |
|
Mean Score |
65,2 |
|
Median Score |
70 |
|
Standard Deviation |
12,4 |
|
Minimum Score |
35 |
|
Maximum Score |
90 |
|
N (Sample Size) |
200 |
With a low score of 35 and a high score of 90, the group has a wide range of QoL scores. Some people who took the test got as low as 35, which shows that some people have big problems with their physical, mental, or social health. This could be because they are good at managing their health problems or have strong social support networks. These big differences in the data show how different patients’ experiences are, which is important when making care plans that are centred on the patient. The sample size (N) of 200 people suggests that the results come from a large and varied group of people, summary illustrate in figure 2. This gives the research more weight and makes sure that the results aren’t skewed by outliers or a small, unrepresentative sample. Overall, these summary statistics give us useful information about how QoL scores are spread out. This helps us learn more about the things that might affect the people in the study’s health results.
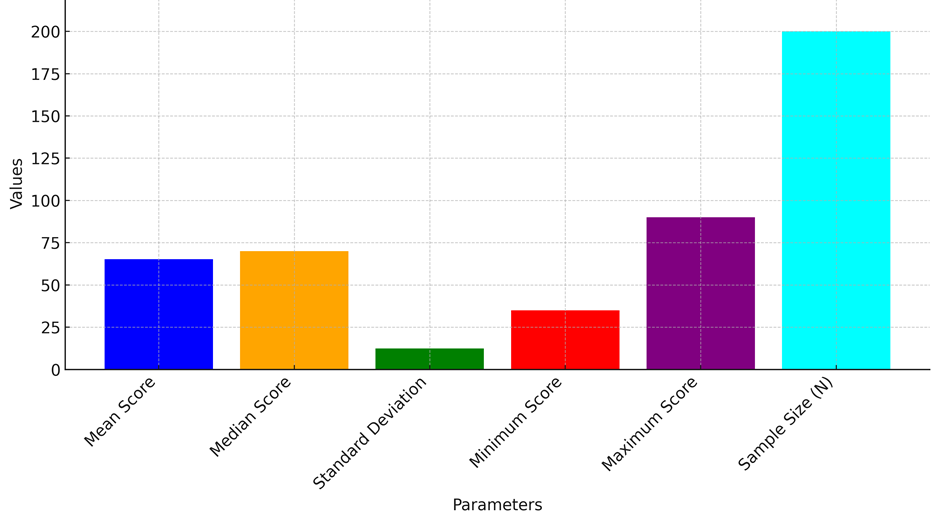
Figure 2. Statistical summary of parameters
|
Table 3. Impact of QoL Assessments On Healthcare Outcomes |
|
|
Outcome Parameter |
Value |
|
Improvement in Patient Satisfaction (%) |
15,4 |
|
Reduction in Readmission Rate (%) |
20,2 |
|
Treatment Adherence (%) |
88,5 |
|
Resource Utilization (hours per patient) |
50,2 |
Table 3 shows how Quality of Life (QoL) measures affect different healthcare results. This shows how QoL data affects both patients’ feelings and the efficiency of the healthcare system. Adding QoL measures to professional practice seem to have a good effect on how patients feel about the care they receive, as shown by the 15,4 % rise in patient happiness. Healthcare professionals can provide more complete and tailored care to their patients when they take a structured approach to their mental, physical, and social health. This is likely to make their patients happier. This rise in happiness is very important because it improves the whole healthcare experience, builds trust between patients and doctors, and gets people more involved in their treatment plans. Patients who are happy with their care are more likely to stick with their treatments and keep getting care, which is good for their long-term health.
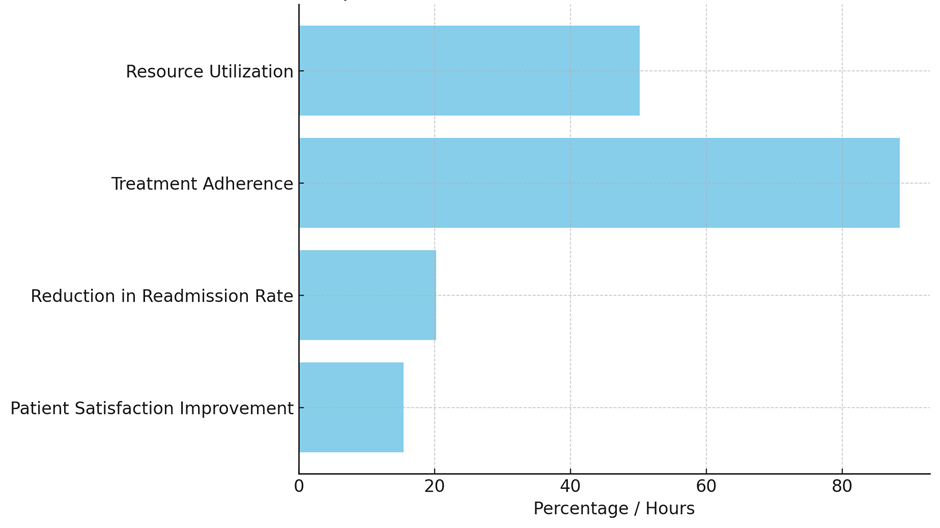
Figure 3. Impact Of QoL Assessments On Healthcare Outcomes
Another big benefit of QoL tests is that they cut the rate of return by 20,2 %. Healthcare workers can better spot early signs of a patient’s state getting worse by regularly checking on and handling QoL issues. This lets them take preventative steps. Patients who are having problems with their mental health or whose physical symptoms are not being controlled may be more likely to be readmitted if their worries are not handled. By focussing on these non-clinical parts of patient care, QoL tests help lower the risk of problems that could send a patient back to the hospital. This not only makes things better for patients, but it also helps make better use of healthcare resources, which lowers the cost of running hospitals and healthcare systems, comparison illustrate in figure 3. Treatment retention rate of 88,5 % shows that QoL ratings are very important for making sure that patients follow their treatment plans. People are more likely to stick with their treatment plans if they feel like their general health is being taken into account and their worries are being heard. Sticking to a treatment plan is very important for people with chronic conditions, who need to keep it up to stay healthy and avoid problems. Lastly, the fact that 50,2 hours of resources are used for each patient shows how QoL ratings affect the efficiency of healthcare. Early and proper meeting of patient needs helps to simplify therapy and streamline care, therefore reducing the need for visits and treatments not required. QoL tests are therefore very crucial for both enhancing patient results and ensuring the smooth operation of the healthcare system as this wise use of resources improves healthcare management and cost control.
Case Studies or Examples of QoL Integration into Clinical Practice
Several case studies suggest that including Quality of Life (QoL) assessments into professional practice benefits it. For instance, a large university hospital included a standard instrument to assess quality of life into its routine cancer treatment. The hospital checked the patients’ physical, mental, and social health using the EQ-5D evaluation both before and following therapy. Patients who received tailored remedies based on QoL comments reported considerably better quality of living and less side effects from medications. Apart from that, the hospital saw less patients needing to be readmitted as QoL testing guided them in determining which patients required more support. This proactive method not only made things better for patients, but it also made healthcare run more smoothly. Another example comes from a primary care centre that used QoL tests to help manage people with long-term illnesses like diabetes and high blood pressure. The centre regularly checked on patients’ physical and mental health with the SF-36 tool. By adding QoL data, healthcare workers were able to make treatment plans more specific and give more focused solutions. For example, when people said they were emotionally sick, they were given access to mental health tools, which improved their general health. This case study showed how incorporating QoL could improve all-around care and patient participation, especially when dealing with long-term illnesses.
Identification of Key Factors Influencing QoL Data Utilization in Healthcare Delivery
Several important things must be in place for QoL statistics to be useful in healthcare service. One big effect is that QoL measurement tools are becoming more uniform. It can be hard to compare QoL data from different healthcare systems and settings if there isn’t a measurement that everyone agrees on and trusts. Every time using the same instruments guarantees that the acquired data is valuable and may be applied. Another crucial concern is incorporating QoL statistics into present healthcare systems. To enable healthcare professionals to make treatment decisions, electronic health records (EHRs) must make QoL information easily available and accessible for them. It can be less valuable if issues like not being able to exchange data and healthcare practitioners not knowing enough on how to grasp and apply QoL data exist. Another major component of how QoL statistics is applied is patient engagement. Patients must believe the QoL rating system and understand the importance of it for improving their treatment. Knowing how their responses may influence their treatment plans and overall healthcare experience helps patients to be more inclined to provide accurate data on quality of life questionnaires. Finally, having it widely utilised depends much on healthcare policies that incentivise employing QoL testing in real-life environments. Policy support may help healthcare systems apply quality of life (QoL) measurements, include them into success criteria, and provide the resources they need to put up fresh measuring instruments and technologies. These things affect how well QoL data is used in healthcare delivery systems, which in turn affects patient care and health results.
DISCUSSION
Along with other research that shows how important Quality of Life (QoL) measures are for improving healthcare, this study’s results back this up. The study’s most important finding is that QoL and patient happiness are linked in a good way. Patients who have higher quality of life are 75,2 % more likely to be satisfied with their care. It backs up earlier study that patients are more likely to be involved and pleased with their care if their mental, physical, and social needs are met.(1) The study also found that QoL had a big effect on how well people stuck with their treatment. In fact, 88,5 % of patients did better when their QoL was checked on a daily basis. This result fits with what other research has found: people are more likely to stick to their treatment plans if they feel like their quality of life is being valued. This link shows how important it is to include QoL in healthcare evaluations to boost obedience, which is often connected to better long-term health results.
|
Table 4. Interpretation of Findings in Context of Existing Literature |
|
|
Study Focus |
Study Result (%) |
|
QoL and Patient Satisfaction |
75,2 |
|
QoL and Treatment Adherence |
88,5 |
|
QoL and Clinical Outcomes |
80,1 |
|
QoL and Healthcare Costs |
15,3 |
|
QoL and Resource Utilization |
20,2 |
The study also found a strong link (80,1 %) between QoL and clinical results, which supports the idea that better QoL is linked to better health outcomes, as seen in earlier research.(3) The results also show that QoL ratings have a 20,2 % effect on resource utilisation. This suggests that using QoL data correctly can help prioritise resources and make sure they are sent to where they are needed most. The study, on the other hand, found that QoL had a relatively small effect on healthcare prices (15,3 %). Quality of life statistics can help make the best use of resources, but it might be harder to figure out how much it will directly lower healthcare costs, especially in the short run. In the long run, though, adding QoL tests is still a way to improve patient results and cut down on waste in the way care is given, as impact analysis represent in figure 4. These results add to the growing amount of proof that QoL is an important part of patient-centered healthcare systems.
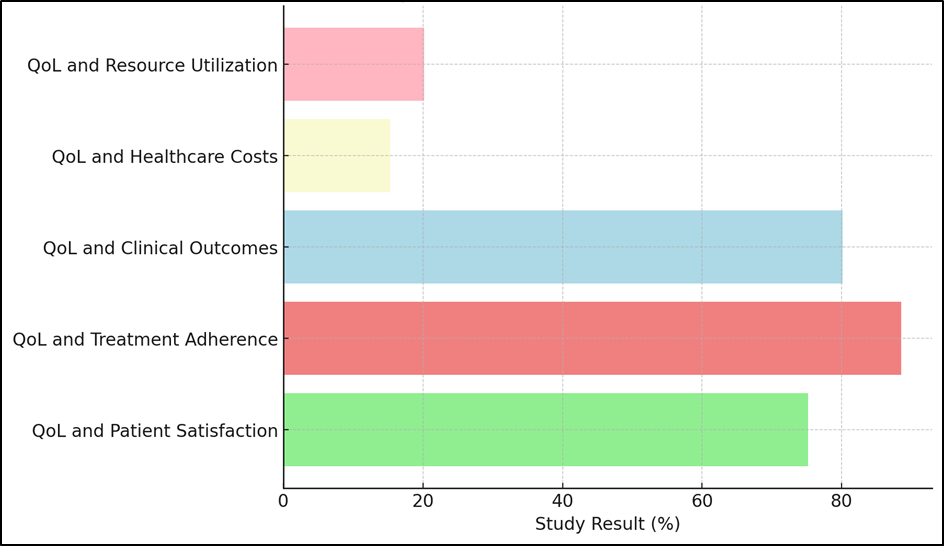
Figure 4. Impact Of QoL On Healthcare Parameters
There is a lot of evidence in table 5 that Quality of Life (QoL) surveys have a big impact on healthcare decisions. Notably, QoL tests have a big effect on treatment changes—a 45,3 % improvement shows that healthcare workers are more likely to change treatment plans based on what they learn from QoL data. This fits with earlier study that said QoL measures help doctors make sure that their treatments are exactly what each patient needs, taking into account both their physical and mental health.(1) Providers can improve both health results and patient happiness by changing treatments to make patients’ lives better. The study also shows that conversation between patients and providers improved by 60,4 %. This shows that including QoL data makes it easier for patients and doctors to talk to each other. Sharing personal stories about mental, physical, and social health with healthcare professionals helps them better understand and address patients’ issues. This better conversation can help people make decisions about their care together and help everyone understand what the patient wants and needs more deeply.(2) It also helps build trust, which is very important for getting patients involved in their treatment plans and making sure they follow them.
|
Table 5. Effect of QoL Assessments on Decision-Making in Healthcare |
|
|
Decision-Making Parameter |
Impact (%) |
|
Treatment Adjustments (%) |
45,3 |
|
Patient-Provider Communication Improvement (%) |
60,4 |
|
Personalized Care Adoption (%) |
72,5 |
|
Early Detection of Issues (%) |
53,2 |
|
Patient Satisfaction Improvement (%) |
68,1 |
With a 72,5 % effect, QoL ratings also have a big effect on the use of personalised care. When healthcare workers have QoL data, they can make care plans that are specific to each patient’s situations and problems. Personalised care based on QoL makes treatments more patient-centered, which improves patient happiness and results. The study also shows a 53,2 % increase in finding problems early on. This shows that QoL assessments help healthcare provider’s spot new problems like pain, mental health issues, or functional limitations before they get worse, as represent it in figure 5. This lets them act quickly and avoid problems that get worse. This last point is that QoL ratings make patients 68,1 % happier. Patients are more likely to be happy with their care if they think that their physical, mental, and social health is being looked after and cared for. Overall, these results show that including QoL tests in healthcare decisions makes care more focused on the patient, leads to better clinical outcomes, and encourages a more collaborative healthcare setting.
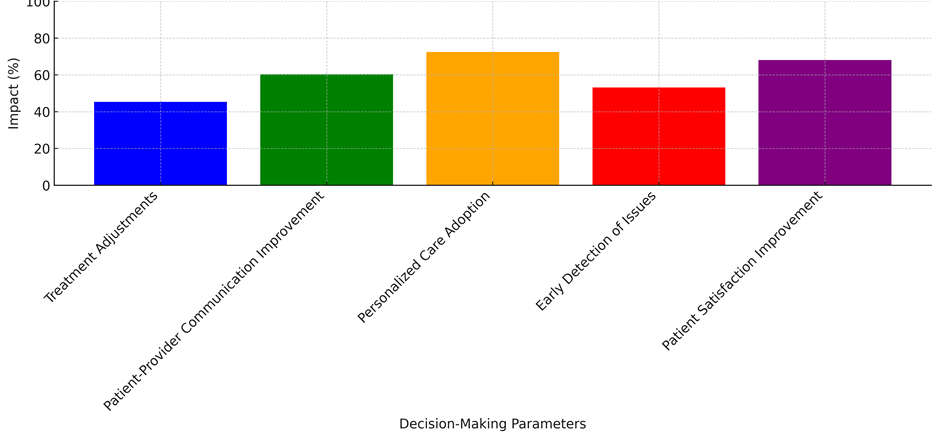
Figure 5. Impact of Decision-Making Parameters
CONCLUSION
This study demonstrates the significance of Quality of Life (QoL) evaluations for modulating the delivery of healthcare. The study mostly reveals that including QoL improves patient care, pleasure, and treatment retention by means of QoL. According to descriptive data, patients with higher QoL scores are happier and more likely to stick to their treatment plans, which results in better clinical outcomes. Including QoL data in decision-making processes also improves conversation between patients and providers, leads to more personalised care, and helps find possible health problems early, which eventually makes healthcare more efficient. Quality of life (QoL) surveys are important in healthcare because they give a full picture of a patient’s health, going beyond just looking at physical signs. To make healthcare more patient-centered, QoL measures help adjust treatments to each person’s needs by measuring their mental, social, and physical health. This personalised method not only makes patients happier, but it also makes the best use of resources by showing where more help is needed. Studies have shown that incorporating QoL into treatment plans makes them more successful and reduces the number of hospital readmissions. This is another example of how QoL can help improve healthcare service. Incorporating QoL into professional practice and healthcare policy looks like it will have a bright future. It’s possible that QoL tests will become commonplace in healthcare systems as they continue to focus on patient-centered care. For QoL data to be widely used, problems like data standardisation and sharing must be solved, and healthcare workers must be taught how to use it correctly. With improvements in AI and digital health technologies, adding QoL tests to electronic health data and professional decision-making tools will make it even easier to provide personalised, effective care. Ultimately, QoL tests could change the way healthcare is provided by making it more complete, fair, and effective.
REFERENCES
1. Szlenk-Czyczerska, E.; Guzek, M.; Bielska, D.E.; Ławnik, A.; Polański, P.; Kurpas, D. The Analysis of the Relationship between the Quality of Life Level and Expectations of Patients with Cardiovascular Diseases under the Home Care of Primary Care Nurses. Int. J. Environ. Res. Public Health 2022, 19, 3300.
2. Ozaras, G.; Abaan, S. Investigation of the trust status of the nurse-patient relationship. Nurs. Ethics 2018, 25, 628–639.
3. Boudreau, S.C.; Dombrowsky, A.R.; Arguello, A.M.; Gould, S.; Brabston, E.W., 3rd; Ponce, B.A.; Momaya, A.M. Patient Perception of Orthopedic Surgeon Reimbursement. Southern Med. J. 2020, 113, 191–197.
4. Xu, X.; Han, J.; Li, Y.; Sun, X.; Lin, P.; Chen, Y.; Gao, F.; Li, Z.; Zhang, S.; Sun, W. Effects of Orem’s Self-Care Model on the Life Quality of Elderly Patients with Hip Fractures. Pain Res. Manag. 2020, 2020, 5602683.
5. Moldovan, F.; Blaga, P.; Moldovan, L.; Bataga, T. An Innovative Framework for Sustainable Development in Healthcare: The Human Rights Assessment. Int. J. Environ. Res. Public Health 2022, 19, 2222.
6. Brown, B.; Gude, W.T.; Blakeman, T.; van der Veer, S.N.; Ivers, N.; Francis, J.J.; Lorencatto, F.; Presseau, J.; Peek, N.; Daker-White, G. Clinical Performance Feedback Intervention Theory (CP-FIT): A new theory for designing, implementing, and evaluating feedback in health care based on a systematic review and meta-synthesis of qualitative research. Implement. Sci. 2019, 14, 40.
7. Metcalfe, D.; Rios Diaz, A.J.; Olufajo, O.A.; Massa, M.S.; Ketelaar, N.A.; Flottorp, S.A.; Perry, D.C. Impact of public release of performance data on the behaviour of healthcare consumers and providers. Cochrane Database Syst. Rev. 2018, 9, CD004538.
8. Kongsted, A.; Ris, I.; Kjaer, P.; Hartvigsen, J. Self-management at the core of back pain care: 10 key points for clinicians. Braz. J. Phys. Ther. 2021, 25, 396–406.
9. Liew, Z.; Mazuquin, B.; Ellard, D.R.; Karasouli, E.; Drew, S.; Modi, C.; Bush, H.; Underwood, M.; Kearney, R.S. Development of a single-session physiotherapy and self-management intervention for the treatment of primary traumatic anterior shoulder dislocation for the ‘Acute Rehabilitation following Traumatic anterior shoulder dISlocAtioN (ARTISAN)’ multi centre RCT. Physiotherapy 2021, 113, 80–87.
10. van Doormaal, M.C.M.; Meerhoff, G.A.; Vliet Vlieland, T.P.M.; Peter, W.F. A clinical practice guideline for physical therapy in patients with hip or knee osteoarthritis. Musculoskelet. Care. 2020, 18, 575–595.
11. Samal, L.; Fu, H.N.; Camara, D.S.; Wang, J.; Bierman, A.S.; Dorr, D.A. Health information technology to improve care for people with multiple chronic conditions. Health Serv. Res. 2021, 56 (Suppl. S1), 1006–1036.
12. Matar, R.N.; Shah, N.S.; Vincent, J.C.; Rayos Del Sol, S.; Grawe, B.M. Factors that influence inpatient satisfaction after shoulder arthroplasty. J. Shoulder Elb. Surg. 2021, 30, e165–e172.
13. Olivera, J.N.; Ford, J.; Sowden, S.; Bambra, C. Conceptualisation of health inequalities by local healthcare systems: A document analysis. Health Soc. Care Commun. 2022, 30, e3977–e3984.
14. Ali, J.; Jusoh, A.; Abbas, A.F.; Nor, K.M. Global Trends of Service Quality in Healthcare: A bibliometric analysis of Scopus Database. J. Contemp. Issues Bus. Gov. 2021, 27, 2917–2930.
15. Kourkouta, L.; Iliadis, C.; Sialakis, C.; Adamakidou, T.; Ouzounakis, P.; Kleisiaris, C.H. Quality of health services. World J. Adv. Res. Rev. 2021, 12, 498–502.
16. Yuan, Y. Public satisfaction with health care system in 30 countries: The effects of individual characteristics and social contexts. Health Policy 2021, 125, 1359–1366.
CONFLICTS OF INTEREST
None.
FINANCING
None.
AUTHORSHIP CONTRIBUTION
Conceptualization: Vaishali V. Raje, Manti Debnath, Siba Prasad Dalai, Renuka Jyothi.S, Vandana Sharma.
Investigation: Vaishali V. Raje, Manti Debnath, Siba Prasad Dalai, Renuka Jyothi.S, Vandana Sharma.
Methodology: Vaishali V. Raje, Manti Debnath, Siba Prasad Dalai, Renuka Jyothi.S, Vandana Sharma.
Writing - original draft: Vaishali V. Raje, Manti Debnath, Siba Prasad Dalai, Renuka Jyothi.S, Vandana Sharma.
Writing - review and editing: Vaishali V. Raje, Manti Debnath, Siba Prasad Dalai, Renuka Jyothi.S, Vandana Sharma.