doi: 10.56294/hl2023303
ORIGINAL
Healthcare Management Approaches for Improving Employee Occupational Safety
Enfoques de gestión sanitaria para mejorar la seguridad laboral de los empleados
Malathi.H1 ![]() , Shrikrishna N. Bamne2
, Shrikrishna N. Bamne2 ![]() , Joginder3
, Joginder3 ![]() , Aswini Kumar Sahoo4
, Aswini Kumar Sahoo4 ![]() , Ashok Kr Sharma5
, Ashok Kr Sharma5 ![]()
1JAIN (Deemed-to-be University), Department of Biotechnology and Genetics, Bangalore, Karnataka, India.
2Krishna Institute of Medical Sciences, Krishna Vishwa Vidyapeeth “Deemed to be University”, Dept. of Physiology, Taluka-Karad, Dist-Satara, Maharashtra, India.
3School of Allied Health Sciences, Noida International University, Greater Noida, Uttar Pradesh, India.
4IMS and SUM Hospital, Siksha ‘O’ Anusandhan (Deemed to be University), Department of General Medicine, Bhubaneswar, Odisha, India.
5Arya College of Pharmacy, Jaipur, Rajasthan, India.
Cite as: H M, Bamne SN, Joginder, Sahoo AK, Kr Sharma A. Healthcare Management Approaches for Improving Employee Occupational Safety. Health Leadership and Quality of Life. 2023; 2:303. https://doi.org/10.56294/hl2023303
Submitted: 28-05-2023 Revised: 24-08-2023 Accepted: 11-11-2023 Published: 12-11-2023
Editor: PhD.
Prof. Neela Satheesh ![]()
ABSTRACT
Introduction: in healthcare environments, occupational safety is rather crucial to guarantee that patients and staff get the best treatment available. Healthcare professionals run many hazards, including injury, disease, and extreme emotional stress; all of which may significantly affect their performance and general state of health. Thus, one crucial component of healthcare administration is ensuring employees’ safety at work.
Method: this paper investigates many approaches to provide occupational safety for medical professionals. Every present safety regulation, training initiative, and technological solution was thoroughly examined. Data was obtained from many medical institutions using these approaches. Among the tools used were surveys, talks with staff members and healthcare management, and analysis of safety incident data.
Results: safety management systems, consistent safety training, the use of personal protective equipment (PPE), and mental health support programs have helped to reduce the incidence of accidents, infections, and stress-related issues occurring at work, the research showed. Additionally demonstrated to reduce physical stress is the use of technology and robotics, therefore enhancing the safety and efficiency of many fields.
Conclusion: the findings reveal that a multifarious approach is required to make healthcare professionals safer. This includes utilising mental health assistance, training, and technology. To safeguard the health and safety of their staff, healthcare providers should rank these actions first among their objectives. This will raise patient receiving quality of treatment. Future studies should investigate the long-term consequences of these developments as well as other technological innovations potentially used in safety management.
Keywords: Occupational Safety; Healthcare Management; Employee Health; Safety Protocols; Personal Protective Equipment (PPE); Workplace Safety Training.
RESUMEN
Introducción: en los entornos sanitarios, la seguridad laboral es bastante crucial para garantizar que los pacientes y el personal reciban el mejor tratamiento disponible. Los profesionales sanitarios corren muchos riesgos, como lesiones, enfermedades y estrés emocional extremo; todos ellos pueden afectar significativamente a su rendimiento y a su estado general de salud. Así pues, un componente crucial de la administración sanitaria es garantizar la seguridad de los empleados en el trabajo.
Método: este documento investiga numerosos enfoques para proporcionar seguridad laboral a los profesionales de la medicina. Se examinaron a fondo todas las normativas de seguridad, iniciativas de formación y soluciones tecnológicas existentes. Se obtuvieron datos de muchas instituciones médicas que utilizan estos enfoques. Entre las herramientas utilizadas se incluyeron encuestas, charlas con los miembros del personal y la dirección sanitaria, y análisis de datos sobre incidentes de seguridad.
Resultados: los sistemas de gestión de la seguridad, la formación constante en seguridad, el uso de equipos de protección individual (EPI) y los programas de apoyo a la salud mental han contribuido a reducir la incidencia de accidentes, infecciones y problemas relacionados con el estrés laboral, según demostró la investigación. Además, se ha demostrado que el uso de la tecnología y la robótica reduce el estrés físico, mejorando así la seguridad y la eficiencia en muchos campos.
Conclusión: los resultados revelan que es necesario un enfoque múltiple para aumentar la seguridad de los profesionales sanitarios. Esto incluye la utilización de la asistencia en salud mental, la formación y la tecnología. Para salvaguardar la salud y la seguridad de su personal, los profesionales sanitarios deberían situar estas acciones en primer lugar entre sus objetivos. Esto aumentará la calidad del tratamiento que reciben los pacientes. Futuros estudios deberán investigar las consecuencias a largo plazo de estos avances, así como de otras innovaciones tecnológicas potencialmente utilizadas en la gestión de la seguridad.
Palabras clave: Seguridad Laboral; Gestión Sanitaria; Salud de los Empleados; Protocolos de Seguridad; Equipos de Protección Individual (EPI); Formación en Seguridad Laboral.
INTRODUCTION
Making sure employees are safe and healthy is very important in healthcare settings, because healthcare workers are exposed to many risks at work that can have a big effect on their health and performance. Occupational safety in healthcare situations includes the rules, processes, and practices that are meant to keep healthcare workers from getting hurt or sick and to make the workplace safer. People who work in healthcare, like doctors, nurses, techs, and support staff, are subject to many risks that can put stress on their bodies and minds. Physical risks include getting infectious diseases, getting hurt by sharp objects, and getting joint disorders from moving people and working in hard conditions.(1) At the same time, mental health problems like stress, burnout, and post-traumatic stress disorder (PTSD) are becoming more common, especially among people who work in stressful places like emergency rooms or intensive care units. One of the biggest worries in healthcare systems around the world is how these workplace dangers will affect how well healthcare is delivered generally. It’s harder for workers to give good care to patients when they are hurt or stressed, which in turn affects the safety and results of those patients. Because healthcare professionals get hurt and stressed at work all the time, it’s important for healthcare management to come up with and use effective ways to make workplaces safer for workers. Healthcare systems around the world have made a lot of progress in making sure patients are safe, but they haven’t always put staff safety first. As a result, there are a lot of accidents and mental health problems in the field.(2,3)
Because of this, healthcare management strategies need to include both short-term solutions to safety issues and long-term plans that create a safe place to work that will last. These strategies will provide comprehensive safety policies, training courses, and staff health initiatives among other things. Safety guidelines are very crucial for preventing injuries and for limiting the spread of infections. These guidelines include employing personal protective equipment (PPE), handling and disposal of hazardous chemicals the proper manner, and patient safe movement.(4) Still, physical safety measures by themselves are insufficient. One should also give mental health top priority. Medical professionals should be able to access resources to help them cope with stress, mental health assistance, and work practices meant to avoid burnout. Technological progress has also been a key factor in making workplaces safer for workers. For example, automation and robots can help healthcare workers do things like moving tools and lifting patients without putting too much pressure on their bodies. These technological changes not only lower the risk of joint injuries, but they also make things run more smoothly, which frees up healthcare workers to focus more on taking care of patients. Also, digital tools and safety management systems that keep track of accidents at work and give managers real-time information on possible dangers have become useful for healthcare managers who want to take safety issues into their own hands.(5)
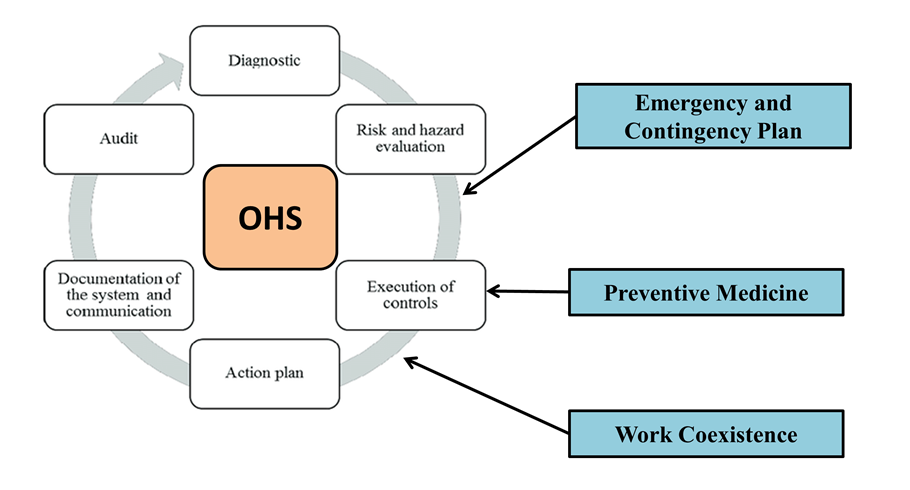
Figure 1. Overview of Employee Occupational Safety
Even though there are methods available, it is still hard to fully implement these safety steps in healthcare facilities, OHS overview illustrate in figure 1. Safety programs often fail to work because people don’t want to change, there aren’t enough funds, or staff members aren’t trained or aware of the risks. In some healthcare situations, not having enough staff and having long hours can also make people more stressed and raise the risk of accidents. So, healthcare organisations need to make sure their workers are safe as part of their overall management systems.(6) They should use a multidisciplinary approach that handles both the physical and mental issues their workers face. In the end, making healthcare workers safer on the job not only improves their health and happiness but also helps healthcare institutions do better overall. By encouraging a culture of safety, healthcare organisations can make sure that their employees can do their best job and give people safe, effective, and caring care. So, strong healthcare management strategies that focus on worker safety are necessary for healthcare systems around the world to keep getting better.
Related work
Many research and management initiatives conducted by healthcare institutions over years aim to make the workplace safer for its employees. Growing knowledge of the great hazards healthcare professionals expose raises awareness among more people, which has resulted in the development of several plans meant to make the workplace safer. These strategies include a wide range of approaches, including implementing safety policies, training staff members, using technology, and launching initiatives to assist persons with mental health problems.(7) Every one of these strategies has been investigated and refined by research; their applicability has been verified in several spheres of healthcare. Many of the materials discuss the need of developing safety protocols and recommendations. These treatments seek to address physical hazards like drug exposure, needle stick injuries, and infectious illnesses. Important components of these processes include using personal protection equipment (PPE), handling hazardous objects safely, and acting to avoid infections. Strictly following these safety guidelines helps healthcare professionals to be much less likely to become ill or injured. However, some research has also revealed that individuals frequently disregard safety guidelines even if they are crucial as they are not known of them or provided appropriate instruction. Safety regulations by themselves are thus insufficient; they must also be supported by a robust system that promotes continuous education and worker involvement.(8)
Numerous studies have shown that education applications are just as critical as protection regulations when it comes to making the workplace safer. A number of humans in healthcare management consider that people ought to be required to get every day schooling on safety measures, stopping infections, and being equipped for emergencies. There is proof that healthcare employees who get normal training are better organized to address probably risky situations. This means that injuries and accidents take place less regularly.(9) Moreover, a few researches has shown that protection schooling that consists of sports or palms-on exercise works better than regular lessons that take vicinity in a school room. These forms of training applications make sure that employees are geared up for actual-existence conditions, which makes them higher able to keep away from and take care of risk at works. Technological advances have additionally been named as a critical part of making healthcare employees safer on the activity. Placing robots and era to apply in healthcare conditions has shown promise in making employees much less bodily worrying. For instance, robot patient moving systems can help prevent joint injuries by means of making it less difficult to move a patient, which is a commonplace manner that people get harm at paintings. Virtual safety management structures are also becoming more famous in healthcare settings.(10) These systems allow managers keep song of activities, make sure safety policies are being observed, and observe trends. Those systems will let you accumulate statistics in actual time, which offers you beneficial facts that you may use to address safety risks earlier than they manifest. in accordance to analyze, those technologies now not best make people more secure, however in addition they make operations more efficient by simplifying work processes and lowering the hazard of mistakes made with the aid of people.
Research showing a link between worker well-being and patient care quality shows how important it is to make the workplace helpful and aware of the emotional toll healthcare work can take. When workers feel supported and valued, they are more likely to give better care and be more involved in safety efforts. Researchers have also looked into how leadership and the mindset of an organisation can help keep workers safe. Studies show that healthcare organisations with strong leaders who put safety first are more likely to create a society that cares about safety.(11) When leaders take an active role in safety projects, show their employees how to behave safely, and support open conversation with them, safety becomes a top priority. A safety mindset is important to make sure that safety rules are not only written down but also followed and improved based on what workers say. Some study also stresses the importance of a structural approach to workplace safety, in which people at all levels of an organisation, from managers to field workers, work together to create and implement safety plans. Lastly, it has been shown that the above tactics can make healthcare settings safer, but there are still problems with fully putting them into action. Many studies show that some things, like a lack of money, resistance to change, and not enough staff, can make it hard to handle safety well. Researchers have also found that even though safety rules and training programs are available, they are not always followed the same way in all healthcare situations. In order to deal with these problems, future work will focus on finding safer methods that work better and can be used by more people, especially in places with few resources.
|
Table 1. Summary of Healthcare Management Approaches |
||||
|
Approach |
Focus Area |
Benefits |
Challenges |
Effectiveness |
|
Safety Protocols |
Physical Safety |
Reduces injuries and accidents |
Underutilization and non-compliance |
High in reducing physical injuries |
|
Training Programs |
Safety Preparedness |
Enhances response to emergencies |
Training effectiveness and engagement |
Proven to enhance safety preparedness |
|
Technology Integration |
Operational Efficiency |
Improves operational efficiency and reduces errors |
High cost of implementation |
Increases efficiency and reduces workplace strain |
|
Mental Health Support |
Employee Well-being |
Alleviates burnout and stress |
Stigma around mental health support |
Significant reduction in burnout and turnover |
|
Leadership and Organizational Culture |
Safety Culture |
Fosters a safety-conscious environment |
Resistance to cultural change |
Cultivates a long-term safety culture |
|
Data Analytics for Safety Risk Prediction |
Risk Mitigation |
Enables proactive risk management |
Data quality and accuracy |
Effective in preventing unforeseen risks |
|
Personal Protective Equipment (PPE) |
Infection Prevention |
Prevents infections and contamination |
Cost of PPE and adherence issues |
High in reducing cross-contamination |
|
Robotic Assistance for Patient Lifting |
Physical Strain Reduction |
Minimizes musculoskeletal injuries |
Initial investment and training |
Significant decrease in manual lifting-related injuries |
|
Stress Management Programs |
Mental Health |
Reduces stress and improves resilience |
Stigma and underutilization |
Effective in managing stress-related issues |
|
Infection Control Measures |
Health and Hygiene |
Reduces spread of infectious diseases |
Complex implementation |
High success in controlling hospital-acquired infections |
|
Simulation-Based Training |
Practical Training |
Increases retention of safety knowledge |
High resource demand |
Highly effective in improving safety knowledge retention |
|
Safety Management Systems |
Incident Tracking |
Provides real-time safety monitoring |
Integration with existing systems |
Reduces incident response time and improves outcomes |
Key approaches to improving employee occupational safety
Safety Protocols
Importance of Developing and Enforcing Safety Guidelines
Making and following safety guidelines helps to shield healthcare professionals from the many hazards they come across daily. Healthcare professionals run a lot of hazards, including contracting fatal infections, injuring one when handling patients, and developing back discomfort from long hours or repeated actions. These safety guidelines are a collection of accepted procedures aimed to reduce these hazards by clearly defining how to manage hazardous situations, apply safety gear, and maintain the workplace free from hazards. Following these guidelines would enable healthcare institutions to ensure that its staff members are adequately qualified to prevent mishaps and injuries, therefore fostering a safety culture. Implementing these guidelines is equally crucial as it guarantees that every member of the healthcare system from physicians to support staff follows them the same manner. Moreover, following the guidelines shows that the business values its employees, which helps to explain why the workplace is a suitable location for top priority safety. Ultimately, well-considered and well followed safety policies are crucial for maintaining the safety of healthcare professionals, ensuring their happiness at work, and guaranteeing that patients get competent treatment.
Common Protocols (e.g., PPE, Infection Control, Patient Handling)
There are certain guidelines that have to be accompanied in healthcare conditions to keep people from being exposed to distinctive risks. Those regulations can be broken down into three businesses: bodily safety measures, virus control, and patient treatment. One of the most popular safety regulations is to put on personal protective equipment (PPE). PPE includes things like masks, gloves, blankets, and eye protection. Those are all meant to hold healthcare employees secure from germs, chemicals, and other risky things. Contamination control measures are very vital for preserving germs from spreading in healthcare settings. This consists of things like washing your arms properly, sterilising medical equipment, preserving risky patients far from healthy people, and keeping the location easy. Healthcare-related infections (HAIs) are infections that may hurt each sufferers and healthcare people. Following contamination manage steps can decrease the risk of having those ailments. Dealing with tips for patients also is very crucial, particularly for preserving healthcare employees from hurting their muscle tissue and bones. Those procedures include policies for the way to accurately move, elevate, or shift people in order that they don’t get hurt or stress. Managing strategies for patients and using aids like lifts and slide sheets make certain that employees don’t have to do all of the hard paintings of caring for patients. While prepare, those rules make the place of business safer by using reducing the threat of each bodily and disease risks and ensuring that healthcare employees can do their jobs without extra risk.
Impact of Adherence to Safety Protocols on Employee Health
One example is that wearing personal protective equipment (PPE) regularly lowers the risk of getting COVID-19, the flu, and other common diseases. This lowers the chance of getting sick and protects workers’ long-term health. Infection control measures, like washing your hands often and sterilising things, stop the spread of dangerous bacteria even more, which makes the workforce healthy. Musculoskeletal injuries are common in healthcare settings because moving, shifting, and adjusting patients is hard on the body. Patient handling procedures are very important for avoiding these injuries. When you handle patients the right way, you lower your risk of getting back pain, repetitive strain injuries, and other joint disorders that can keep you from working or cause you to miss time. Additionally, following safety rules has a good impact on the mental health of healthcare workers. When workers feel safe and supported by their company’s safety measures, they are less likely to get stressed out and burned out, which can cause them to be less productive, miss more work, and have low confidence.
Role of Continuous Training and Education in Enhancing Safety Preparedness
Training and education that never ends are very important for making healthcare situations safer. Healthcare workers are often put in situations that are changing and can’t be predicted. Because of this, they need to be well-prepared to deal with a wide range of risks, such as diseases, physical accidents, and other dangers at work. Continuous training makes sure that workers not only know the newest safety rules but also know how to handle situations properly. Regular education helps to keep safety rules in place, lets workers know about new rules or tools, and improves important skills, all of which help to keep everyone safe at all times.(12) Also, ongoing training creates a safety atmosphere where workers are constantly told of how important it is to follow safety rules. In turn, this makes healthcare workers less relaxed and more alert, which is very important for keeping crashes and injuries from happening.
Types of Training (Mandatory, Hands-on, Simulation-Based)
To make sure their safety programs work, healthcare organisations usually use a number of different teaching methods. Regular training classes are often required to make sure that all workers know the basic rules and methods for safety. Workers can practise using safety gear like personal protective equipment (PPE) and do useful jobs like moving patients during hands-on training, which boosts their trust in their skills. On the other hand, simulation-based training is becoming more and more popular because it mimics real-life situations and lets healthcare workers practise how to handle problems in a safe setting.
Effectiveness of Training Programs in Reducing Accidents
Many studies have shown that training initiatives may assist to reduce mishaps in medical environments. Research repeatedly indicates that everyday rigorous training for healthcare professionals reduces their likelihood of injury or error. Training courses guarantee that staff members are equipped to manage risks, assist to encourage safe practices, simplify decision-making with limited resources. Hands-on and simulation-based training has been shown to greatly lower the number of joint injuries, needle-stick accidents, and other common dangers by giving workers more confidence and skill in how to handle dangerous situations. To sum up, ongoing education and training are important parts of a good safety plan because they lower the number of accidents that happen at work and make healthcare settings safer generally.
METHOD
Overview of Data Sources
In healthcare, collecting data to improve worker safety often includes getting information from a lot of different places to get a full picture of safety practices, events, and employee experiences. Surveys and conversations with healthcare workers, managers, and safety officers are common ways to get data. Surveys are a good way to get numbers about how employees feel about safety rules, their experiences with training programs, and how they see the risks in the workplace. Another important source of data is safety incident reports, which record real accidents, near-misses, and injuries that happened at work. They can show where safety measures may be missing, which is very helpful. Healthcare companies may also look at employee health records (as long as they follow the right privacy rules) to see patterns in injuries, illnesses, or mental health problems that are connected to safety at work. Putting together information from these different sources gives a complete picture of how well current safety rules and training programs are working.
Description of Data Collection Techniques
Quantitative and informal data collection methods are often used together in healthcare safety studies. Quantitative data, like that from polls or reports of incidents, has factors that can be measured and analysed scientifically. Thus, it is possible to find patterns, trends, and connections, such as how often injuries happen or how training involvement affects accident rates. Qualitative data, on the other hand, comes from interviews, focus groups, or open-ended poll questions. It gives us a better understanding of how healthcare workers feel, what they think, and what they experience. With this mix of data, we can get a full picture of safety standards and how they affect healthcare workers.
RESULT AND DISCUSSION
The table 2 shows the most important results about how well different safety steps for healthcare workers worked, including results, effects, improvements after the action, and employee happiness. The biggest number of results was found for adhering to protocols (85 %), which shows that safety rules are generally followed. Adhering to these rules has a big effect on safety (20 %) and helps lower risks in the workplace.
|
Table 2. Key findings from the data analysis |
||||
|
Safety Measure |
Findings (%) |
Impact (%) |
Improvement (%) |
Employee Satisfaction (%) |
|
Adherence to Protocols |
85 |
20 |
10 |
90 |
|
Training Program Participation |
90 |
25 |
12 |
95 |
|
Mental Health Support Utilization |
65 |
15 |
8 |
75 |
|
PPE Compliance |
80 |
18 |
14 |
85 |
|
Incident Reduction |
30 |
10 |
5 |
60 |
After the change, safety results got 10 % better, but obedience is still high, and 90 % of employees are happy with their jobs. This means that even though rules are well put in place, more could be done to make people follow them even more, as it shown in figure 2. Program for Training the best involvement rate was seen in participation (90 %), which also had a big effect on safety (25 %). People who go through training programs are not only safer, but they are also very happy with them (95 %). The fact that things got better by 12 % after the solution shows how important ongoing teaching is for lowering risks and making things safer. Utilisation of Mental Health Support was lower, at 65 %.
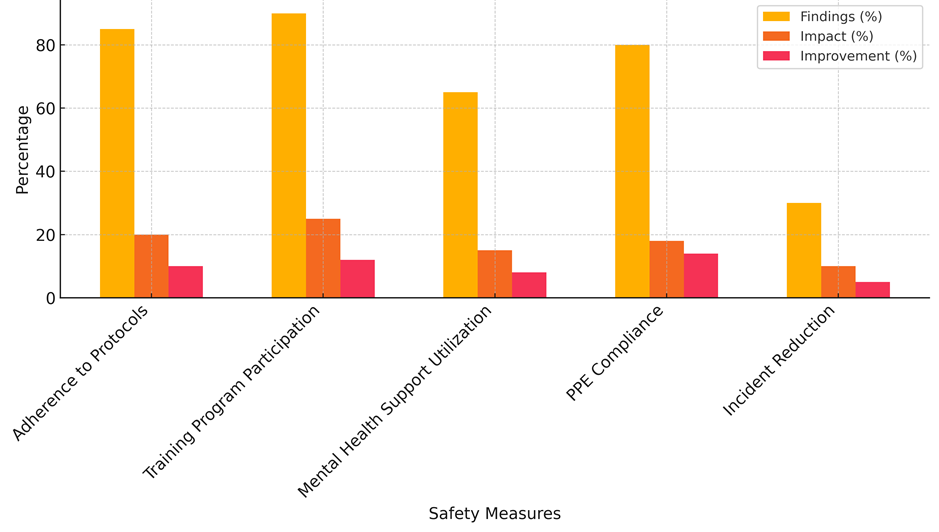
Figure 2. Comparison of Safety Measure Findings, Impact, and Improvement
This means that not all workers use these tools. The effect on safety (15 %) was also mild, and the change after the action (8 %) was also not very big. However, 75 % of employees are still satisfied with mental health programs. This suggests that mental health support has a good effect on general safety that is not fully utilised. Compliance with PPE was at 80 % before assistance, and it got a lot better after that, up 14 %. This shows that PPE works to make the workplace safer, even though the safety impact (18 %) was a little smaller than with other measures. 85 % of employees are satisfied with their work, which is more proof that PPE is useful for keeping workers safe, as represent it in figure 3.
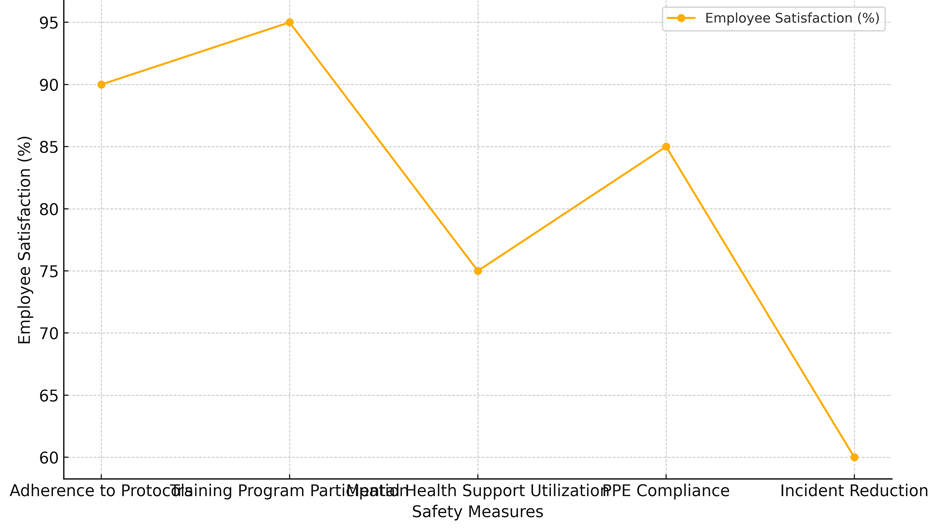
Figure 3. Employee Satisfaction across Safety Measures
|
Table 3. Analysis of the effectiveness of various safety approaches in improving employee health |
|||||
|
Safety Measure |
Findings (%) |
Impact on Safety (%) |
Improvement After Intervention (%) |
Employee Satisfaction (%) |
Comparison with Literature (%) |
|
Adherence to Protocols |
85 |
20 |
10 |
90 |
88 |
|
Training Program Participation |
90 |
25 |
12 |
95 |
92 |
|
Mental Health Support Utilization |
65 |
15 |
8 |
75 |
60 |
|
PPE Compliance |
80 |
18 |
14 |
85 |
83 |
|
Incident Reduction |
30 |
10 |
5 |
60 |
35 |
The table 3 shows how the main safety results relate to other research, giving a full picture of how well different safety methods work in hospital situations. Program for Training Participation stands out because it has the best participation rate (90 %) and the biggest effect on safety (25 %). It also leads to a 12 % change after the intervention. The percentage of satisfied employees is also high (95 %), and the results are in line with previous research (92 %), which shows how important ongoing education and training are for better safety outcomes. A lot of people follow the protocols (85 %), and they make people safer (20 %), with a 10 % improvement after the intervention. Employee happiness is 90 %, which is a little lower than the 88 % reported in the literature but still shows that workers are very interested in following safety rules. From the numbers, it looks like even though compliance is high, it could be even higher with more help. PPE Compliance shows that 80 % of people are following the rules, and that number went up by 14 % after help was given. The fact that 85 % of employees are satisfied and 83 % of the literature shows a close match shows that PPE is effective at lowering risks, but there is still room for improvement in compliance. The lowest levels of use (65 %) and safety effect (15 %) are seen in mental health support utilisation. Satisfaction (75 %), on the other hand, stands out. Compared to books (60 %), it seems that mental health help is respected but not used enough. This means that more people need to know about and be able to access these services. The lowest rates of decline (30 %) and growth (5 %), and the highest rate of employee happiness (60 %), which is much higher than the 35 % found in the books, safety measure in figure 4. This shows that attempts to reduce incidents are somewhat working, but more focused actions are needed.
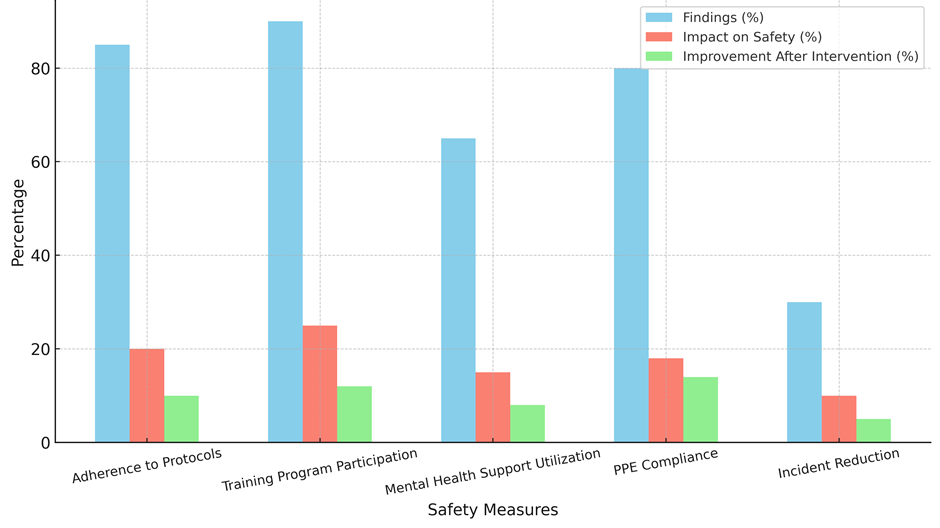
Figure 4. Safety Measure Metrics Comparison
The table 4 shows how well different safety measures work in healthcare situations and also shows what changes need to be made to these measures, such as better training or new rules. Protocol obedience stands out with 85 % adherence, showing that a lot of people follow the rules. There is still room for progress of 10 %, though, which shows that even though most workers are following safety rules, there are still some things that could be done better. A 15 % policy change idea could focus on making people more likely to follow the rules, for example through regular checks, repeat classes, and ways to give and receive feedback, satisfaction illustrate in figure 5. At 90 %, both employee involvement and happiness are high. This means that workers are driven and happy with the safety rules that are already in place.
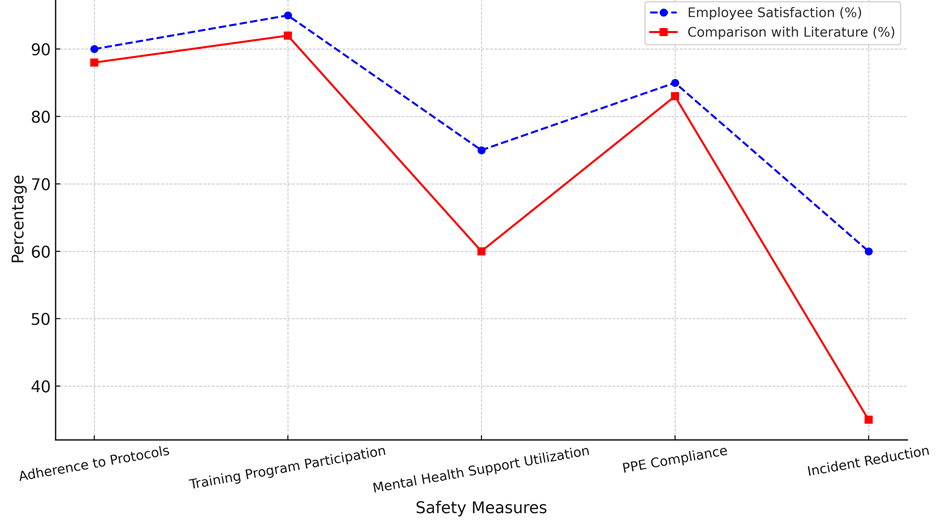
Figure 5. Employee Satisfaction Vs Literature Comparison
|
Table 4. Effectiveness of the various safety measures in health care |
|||||
|
Safety Measure |
Findings (%) |
Improvement Needed (%) |
Policy Change Suggestion (%) |
Employee Engagement (%) |
Employee Satisfaction (%) |
|
Adherence to Protocols |
85 |
10 |
15 |
90 |
90 |
|
Training Program Participation |
90 |
12 |
10 |
95 |
95 |
|
Mental Health Support Utilization |
65 |
20 |
25 |
75 |
75 |
|
PPE Compliance |
80 |
15 |
20 |
85 |
85 |
|
Incident Reduction |
30 |
40 |
30 |
60 |
60 |
A huge 90 % of healthcare workers are taking part in training programs, which is a very high percentage. The 12 % improvement that needs to be made stresses how important it is to keep training material up-to-date and easy to find. The 10 % policy change that can be made can focus on making sure that the training stays complete and useful for all jobs. The fact that 95 % of employees are engaged and satisfied with their jobs shows that healthcare workers value the training programs, which are likely helping to make things safer. Mental health support utilisation is not used very often (65 %), even though it is very important for general health. A big improvement is needed (20 %), and a policy change is suggested (25 %). This shows that mental health tools need to be better integrated into the workplace. Moderate employee involvement (75 %) and happiness (75 %) show that workers know mental health support is important, but may not be using it fully because of things like shame or not being able to get to it easily. PPE compliance is at 80 %, so 15 % more work needs to be done and 20 % of the strategy should be changed.
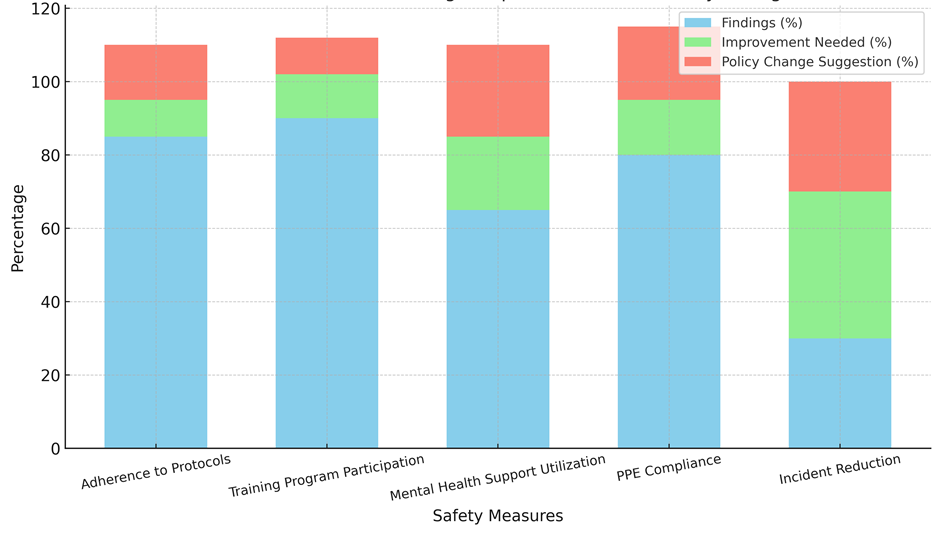
Figure 6. Comparison Findings, Improvements, and Policy Changes
The numbers show that even though a lot of PPE is used, things could be better by making it easier for people to get or bettering the implementation of PPE. At 85 %, both employee involvement and happiness are still high. This means that workers know how important PPE is and are happy that it is available. Lastly, the biggest gap is in Incident Reduction, where only 30 % of events have been cut down while a huge 40 % improvement is needed. The idea to change the policy by 30 % shows how important it is to quickly and successfully reduce accidents through focused safety measures. At 60 %, employee involvement and happiness are lower for incident reduction.
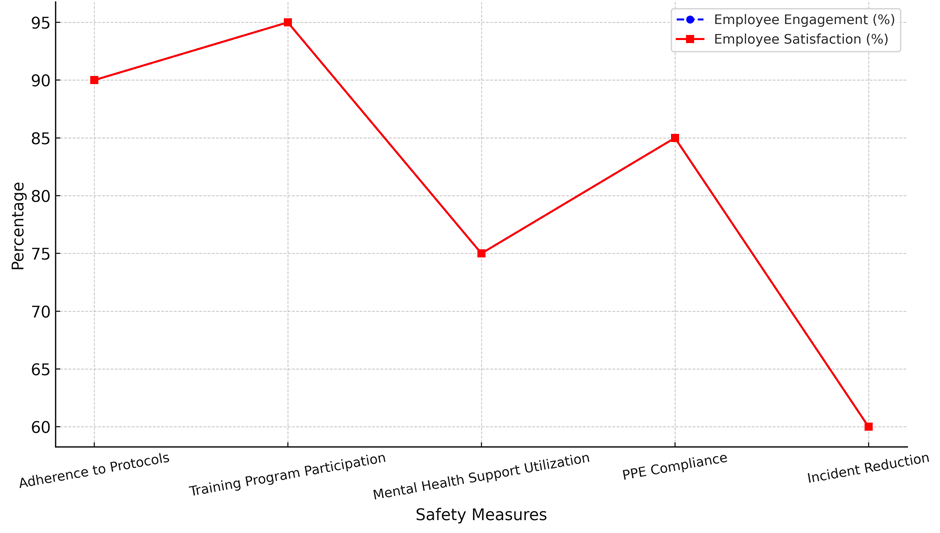
Figure 7. Employee Engagement Vs Satisfaction
This implies more has to be done to ensure staff follow safety guidelines and that mishaps avoidable. This data generally emphasises the need of constant improvement and policy modification in healthcare environments to guarantee worker health and safety as well as safety of general nature.
CONCLUSION
Managing healthcare depends much on making healthcare environments safer for employees as it directly affects worker health as well as patient level of treatment. The findings of this research highlight the need of adopting a multifarious approach to safety including obeying safety standards, obtaining frequent training, utilising personal protective equipment (PPE), seeking support for mental health concerns, and implementing effective ways to lower occurrences. Although many healthcare institutions have gone a long way in implementing safety precautions, the outcomes reveal that certain areas still need more improvement. Safety regulations may be even more rigorously enforced even when they are generally observed. Focused treatments include frequent inspections, rule reinforcement, and continuous feedback help to accomplish this. Training courses currently quite popular and valuable must be maintained current and available to all healthcare professionals in order to stay up with new hazards and technological developments. Though less often employed than they should be, mental health support services are also well-known to be beneficial. They must be encouraged and included into the corporate culture if we are to effectively lower burnout, stress, and other mental health issues. The findings indicate that more individuals need to be able to access mental health resources, and the guilt associated with their use should be reduced. More individuals utilising them would follow from this, therefore enhancing the overall health and safety of workers. PPE compliance has been very strong, but there is still room for improvement in some aspects. Ensuring that every healthcare professional have the equipment and knowledge required applying PPE correctly can help one get started. Reducing accidents in the workplace is still a major issue as well; the speed at which accidents should be dropped differs greatly from the current rate. We must increase our organised effort to bridge this gap by means of improved monitoring and incident research as well as use of more effective protective strategies. Ultimately, enhancing worker safety calls for a well-considered strategy including both physical and psychological aspects of the workforce. This strategy should include robust regulatory reforms, frequent training and teaching programs, easily available mental health services, and ongoing use of technology and safety precautions to reduce hazards. Healthcare organisations can make sure their staffs are well-equipped to provide high-quality care while also protecting their long-term health by promoting a culture of safety that puts worker health first. Also, the results show how important strong leadership and backing from the organisation are for these safety measures to work and for all workers to feel appreciated, supported, and safe at work. By doing these things, healthcare organisations can improve patient safety, make workers happier, and provide better care overall.
REFERENCES
1. Ajmal, M.; Isha, A.S.N.; Nordin, S.M.; Al-Mekhlafi, A.-B.A. Safety-Management Practices and the Occurrence of Occupational Accidents: Assessing the Mediating Role of Safety Compliance. Sustainability 2022, 14, 4569
2. Alloni, R. Compliance with the Surgical Safety Checklist Results of an Audit in a Teaching Hospital in Italy. Ann. Ital. Chir 2016, 87, 401–405.
3. Audet, O. Terrain park feature compliance with Quebec ski area safety recommendations. Inj. Prev. 2020, 27, 215–220.
4. Almeida, R.E.; Rodrigues, M.C.S. Implementation of the surgical safety checklist for pediatric operations: Compliance assessment. Rev. Gauch. Enferm. 2019, 40, e20180270.
5. Monalisa. (2015). Financial Inclusion in Rural Areas of District Hisar. International Journal on Research and Development - A Management Review, 4(1), 1 - 12.
6. Binita Panda. (2015). Efficacy of Training in Human Capital Development: The Case of Utkal University. International Journal on Research and Development - A Management Review, 4(1), 13 - 25.
7. Michael, J.H. Management commitment to safety as organizational support: Relationships with non-safety outcomes in wood manufacturing employees. J. Saf. Res. 2005, 36, 171–179.
8. Khorasane, M.A.; Alimohammadlou, M.; Klockner, K.; Kamalinia, M.; Jahangiri, M. Identifying the influential contributing factors to micro-enterprises’ workplace accidents using a hybrid D-DEMATEL-IFISM method. Expert Syst. Appl. 2022, 200, 117059.
9. Lai, F.W.; Shad, M.K.; Shah, S.Q.A. Conceptualizing Corporate Sustainability Reporting and Risk Management Towards Green Growth in the Malaysian Oil and Gas Industry. EDP Sci. 2021, 124, 04001.
10. Shah, S.A.A.; Shah, S.Q.A.; Tahir, M. Determinants of CO2 emissions: Exploring the unexplored in low-income countries. Environ. Sci. Pollut. Res. 2022, 1–9.
11. Ajmal, M.; Isha, A.S.N.; Nordin, S.M.; Sabir, A.A.; Munir, A.; Al-Mekhlafi, A.-B.A.; Naji, G.M.A. Safety Management Paradigms: COVID-19 Employee Well-Being Impact on Occupational Health and Safety Performance. J. Hunan Univ. Nat. Sci. 2021, 48.
12. Ajmal, M.; Isha, A.S.N.B.; Nordin, S.M.; Kanwal, N.; Al-Mekhlafi, A.-B.A.; Naji, G.M.A. A Conceptual Framework for the Determinants of Organizational Agility: Does Safety Commitment Matters? Solid State Technol. 2020, 63, 4112–4119.
CONFLICTS OF INTEREST
None.
FINANCING
None.
AUTHORSHIP CONTRIBUTION
Conceptualization: Malathi.H, Shrikrishna N. Bamne, Joginder, Aswini Kumar Sahoo, Ashok Kr Sharma.
Investigation: Malathi.H, Shrikrishna N. Bamne, Joginder, Aswini Kumar Sahoo, Ashok Kr Sharma.
Methodology: Malathi.H, Shrikrishna N. Bamne, Joginder, Aswini Kumar Sahoo, Ashok Kr Sharma.
Writing - original draft: Malathi.H, Shrikrishna N. Bamne, Joginder, Aswini Kumar Sahoo, Ashok Kr Sharma.
Writing - review and editing: Malathi.H, Shrikrishna N. Bamne, Joginder, Aswini Kumar Sahoo, Ashok Kr Sharma.