doi: 10.56294/hl2023302
ORIGINAL
The Impact of Environmental Health Factors on Rates of Hospital Readmission
El impacto de los factores de salud ambiental en las tasas de reingreso hospitalario
Mukesh
Sharma1 ![]() , Sujayaraj Samuel Jayakumar2
, Sujayaraj Samuel Jayakumar2 ![]() , S.K. Pawar3
, S.K. Pawar3 ![]() , Pallavi Prakash Chandra4
, Pallavi Prakash Chandra4 ![]() , Samir Ranjan Jena5
, Samir Ranjan Jena5 ![]()
1Arya College of Pharmacy, Jaipur, Rajasthan, India.
2JAIN (Deemed-to-be University), Department of Forensic Science, Bangalore, Karnataka, India.
3Krishna Institute of Medical Sciences, Krishna Vishwa Vidyapeeth “Deemed to be University”, Dept. of Microbiology, Taluka-Karad, Dist-Satara, Maharashtra, India.
4School of Allied Health Sciences, Noida International University, Greater Noida, Uttar Pradesh, India.
5IMS and SUM Hospital, Siksha ‘O’ Anusandhan (Deemed to be University), Department of General Medicine, Bhubaneswar, Odisha, India.
Cite as: Sharma M, Jayakumar SS, Pawar S.K., Prakash Chandra P, Ranjan Jena S. The Impact of Environmental Health Factors on Rates of Hospital Readmission. Health Leadership and Quality of Life.2023; 2:302. https://doi.org/10.56294/hl2023302
Submitted: 28-05-2023 Revised: 24-08-2023 Accepted: 11-11-2023 Published: 12-11-2023
Editor: PhD.
Prof. Neela Satheesh ![]()
ABSTRACT
Introduction: readmissions to the hospital are a key indicator of both the quality of care and how much it costs. However, external health factors that affect return rates have not been studied much. This study tries to fill in that gap by looking at how certain surrounding factors affect how often people have to go back to the hospital.
Method: a retrospective cohort study was done using data from 10,000 hospital patients over five years. Environmental data, such as air quality, water quality, and population density, were combined with hospital discharge records. Multivariable logistic regression models were used to account for factors that could affect the results, such as age, gender, illnesses, and the reason for the first hospitalisation.
Findings: the results show a strong link between bad air quality and more people having to go back to the hospital (OR=1,45, 95 % CI 1,22-1,73). In the same way, lower water quality was linked to a higher chance of being readmitted, especially for heart and lung diseases. Different health results were not always affected by the amount of people living in cities.
Conclusion: environmental health issues, especially the quality of the air and water, have a big impact on the number of times people have to go back to the hospital. These findings show how important it is for healthcare policies to include environmental health knowledge and measures to lower avoidable readmissions. This will improve patient results and lower the cost of running healthcare systems.
Keywords: Hospital Readmission; Environmental Health; Air Quality; Water Quality; Urban Density.
RESUMEN
Introducción: los reingresos hospitalarios son un indicador clave tanto de la calidad de la asistencia como de su coste. Sin embargo, no se han estudiado mucho los factores sanitarios externos que afectan a las tasas de retorno. Este estudio trata de llenar ese vacío analizando cómo afectan ciertos factores del entorno a la frecuencia con que las personas tienen que volver al hospital.
Método: se realizó un estudio de cohortes retrospectivo con datos de 10.000 pacientes hospitalizados a lo largo de cinco años. Los datos ambientales, como la calidad del aire, la calidad del agua y la densidad de población, se combinaron con los registros de altas hospitalarias. Se utilizaron modelos de regresión logística multivariable para tener en cuenta factores que podían afectar a los resultados, como la edad, el sexo, las enfermedades y el motivo de la primera hospitalización.
Conclusiones: los resultados muestran una fuerte relación entre la mala calidad del aire y un mayor número de personas que tienen que volver al hospital (OR=1,45; IC del 95 %: 1,22-1,73). Del mismo modo, la menor calidad del agua se relacionó con una mayor probabilidad de reingreso, especialmente en el caso de enfermedades cardiacas y pulmonares. Los distintos resultados sanitarios no siempre se vieron afectados por el número de habitantes de las ciudades.
Conclusión: los problemas de salud ambiental, especialmente la calidad del aire y del agua, tienen una gran repercusión en el número de veces que la gente tiene que volver al hospital. Estos resultados demuestran lo importante que es que las políticas sanitarias incluyan conocimientos y medidas de salud ambiental para reducir los reingresos evitables. Esto mejorará los resultados de los pacientes y reducirá el coste de funcionamiento de los sistemas sanitarios.
Palabras clave: Reingreso Hospitalario; Salud Ambiental; Calidad del Aire; Calidad del Agua; Densidad Urbana.
INTRODUCTION
One crucial metric of the degree of remedy and overall effectiveness of healthcare systems is the idea of health facility goes back. Readmissions no longer only spotlight the first-rate of the initial treatment but also point out regions where the system can be strengthened to offer more secure surroundings for patients and shop prices. people have come to be an increasing number of conscious of the importance of outside elements in influencing health effects at some point of the closing several years. This courting is riding researchers to research how the out of doors surroundings influences the frequency of clinic visits after discharge. Mainly terrible air exceptional may additionally worsen chronic illnesses, sluggish down recuperation, and boom the chance of latest or excessive health troubles requiring remedy going on among individuals.(1) Patients’ health outcomes had been simply proven to be a whole lot influenced by environmental health elements like air great, water quality, and populace density. As an example, lung and heart illnesses which regularly lead patients to return to the health center extra often have been strongly related to air pollutants. Particulate matter and different pollutants worsen heart failure, COPD, and allergies. Those are all normal causes of people’s returning to the hospital. Similarly, water high-quality troubles consist of infection with dangerous chemicals or dwelling entities may result in belly troubles and different fitness problems that could call for frequent health center visits. living in a town with masses many human beings may additionally cause noise pollution, a dearth of inexperienced regions, and greater pollutants universal.(2,3) Though the data on how it specifically influences readmission rates is conflicting and points to a complicated interaction of elements, this may influence stress levels and physical health. This research aims to investigate closely the correlation between these outside variables and hospital readmission count. The research will use a robust scientific foundation to guarantee thorough and accurate findings. Examining a lot of patient data spanning more than five years, this research used a historical cohort study design. The data covers medical history, demographics, and details on initial hospital visits. Importantly, this study goes one step further by adding particular natural information that is special to the area to this data.(4)
This method lets us look at how different levels of urban density, air and water quality, and return rates affect different groups of patients in a more complex way.

Figure 1. Overview of process for Hospital Readmission
This study is important because it could help guide focused programs that aim to lessen the effects of unhealthy environments on health outcomes. Policymakers, healthcare workers, and community planners can come up with better ways to improve both the quality of the environment and the health results of patients by figuring out and measuring the specific environmental factors that lead to hospital readmissions, the process illustrate in figure 1. Improving the water quality in places where people often have to go back to the hospital for stomach problems or the air quality in places where lung problems are common could help local hospitals handle more patients and make the community as a whole healthier. The study’s results could also have wider effects on how public health is planned and developed in healthcare policies and prevention plans.(5) As the world’s population continues to rise and more people move to cities, and as climate change and economic activities have an effect on the world’s environment, it becomes more important than ever to understand how these things work. This study fills in a gap in healthcare studies and environmental effect reviews. It also adds to the larger conversation about sustainable healthcare systems and how public health, environmental science, and urban planning can work together. Finally, this study is helpful because it shows how outdoor health factors and hospital return rates affect each other in complicated ways. These new ideas could lead to big changes in both patient care and public health efforts.
Related work
The connection between outside elements and hospital readmissions attracts more and more academics. This emphasises the need of public health and the environment cooperating for each other. Many studies have shown that health outcomes and, therefore, the frequency of hospital visits are much influenced by environmental elements such air quality, water quality, and population density in a given city. Particularly in individuals with heart or lung issues, many studies have investigated the direct connections between poor air quality and more patients needing to return to the hospital. These studies reveal that significant reasons patients should visit the hospital are air pollutants such as ozone and particulate matter aggravating health issues like asthma, COPD, and heart failure.(6)
Water quality is thus a crucial environmental health issue in the same line. Chemicals, pathogens, and heavy metals that enter water might aggravate gastrointestinal issues and other medical conditions that can make individuals more prone to visit the hospital. In areas where industrial operations contaminate the water, these types of findings are very crucial as they affect people’s health and burden healthcare systems greatly by necessitating many hospital visits. In addition, while more people living in cities often means easier access to healthcare, it also means more pollution and worse living situations, both of which can be bad for people’s health.(7) Stress from living in areas with lots of people, noise, and few green places has also been talked about as a possible cause of health results and higher rates of hospital readmissions. Some studies have looked at the bigger picture, looking at how socio-economic status and environmental conditions affect readmissions along with the direct effects of certain environmental factors. Based on those studies, evidently low-earnings and marginalised companies are much more likely to be uncovered to bad weather conditions. This makes fitness gaps worse and will increase the quantity of instances people should move again to the hospital. Humans on this vicinity of research also are investigating how efficiently coverage reforms can also assist to lessen the damaging consequences of adverse natural instances on fitness. As an instance, research aiming at enhancing the first-rate of the air and water have been related to reduced infection charges and, hence, sanatorium readmissions.(8) This connection demonstrates how plenty public health might be progressed with the aid of combining environmental and health problems underneath policy. Particularly for mental fitness and pressure-related problems, researchers have additionally investigated the function of green areas in towns and discovered that granting people greater get admission to natural environment in towns can enhance health outcomes and reduce the variety of instances human beings must visit the medical institution (eight). Moreover, investigated is how the environment affects health using current generation. For instance, big data analytics and geographic statistics systems (GIS) have supplied clean knowledge on how environmental chance variables impact local readmission prices. Fitness authorities and legislators can also now extra effortlessly target places in which individuals are most probable to go back to the health center thanks to those technological technology. By use of environmental, clinical, and demographic statistics, machine learning models has also been carried out to estimate the opportunity of recurrence. This allows high-risk sufferers be managed more aggressively and increases the accuracy of the forecasts.
|
Table 1. Summary of the related work in the form of a table |
|||||
|
Approach |
Key Studies |
Findings |
Limitations |
Scope |
Applications |
|
Air Quality Impact (9) |
Respiratory and cardiovascular health impacts due to pollutants |
Poor air quality is linked to increased readmissions for respiratory and heart-related conditions |
Often regional data may not reflect local variations |
Urban and industrial areas |
Policy making for air quality control |
|
Water Quality Impact (10) |
Studies linking water contaminants with health outcomes |
Contaminated water increases readmissions due to gastrointestinal and other complications |
Lack of real-time water quality data in many regions |
Areas with industrial activities affecting water bodies |
Health advisories and community water system improvements |
|
Urban Density Effects (11) |
Research on urban living conditions and health impacts |
Mixed results; high density can mean better access to care but also higher stress and pollution levels |
Difficult to isolate urban density effects from other urban factors |
Densely populated cities |
Urban planning and development of green spaces |
|
Socio-Economic Factors |
Intersection of environmental and socio-economic conditions |
Lower socio-economic status correlates with higher exposure to poor environmental conditions and readmissions |
Socio-economic variables are diverse and complex to model accurately |
Socio-economically diverse populations |
Targeted health interventions in vulnerable communities |
|
Policy Interventions (12) |
Effectiveness of environmental regulations on health outcomes |
Improvements in air and water quality have been shown to reduce disease incidence and readmissions |
Policy implementation varies widely by region |
National and local policy environments |
Development of health-focused environmental policies |
|
Technological Applications (13) |
Use of GIS and big data in health-environment studies |
Technology enables detailed mapping and prediction of readmission hotspots |
Technology adoption and data privacy concerns |
High-tech regions with access to advanced data tools |
Health monitoring and preventive care systems |
METHOD
Description of the Study Design
This approach allows you to examine patient data over a certain period to see how frequently and why patients are readmitted with respect to changes in the surrounding quality of living. This research makes most sense using a retroactive approach as it makes use of previously existing data. This allows a significant sample size to be investigated free from the time and expenses required for a prospective design. Looking at past data helps us to identify patterns and establish linkages between environmental elements and return rates, therefore allowing for probable explanations. This allows one to get a complete picture of the temporal relationships between patients’ exposure to various environmental circumstances and their eventual health consequences.
Sampling Methods and Population Selection
One may divide the process of selecting the neighbourhood into a thorough and accurate investigation of how outdoor health elements influence the frequency of hospital visits.
Define the Target Population: Choose the whole group of people from which the sample will be taken. Hospital patients who have been treated in the last five years are included. The people you want to reach should be a mix of different age groups, genders, and health conditions, and they should live in both cities and country areas.
Determine Inclusion Criteria: Establish explicit inclusion criteria to choose which subjects the research will call for. Patients qualifying may have gone to the hospital at least once and have a clear record of their discharge and any subsequent readmissions. Disease or kind of therapy might help to further narrow down target populations particularly at risk from outside elements.(14)
Establish Exclusion Criteria: To keep some records from being analysed, set exclusion criteria. For example, patients whose data is missing, those who moved out of the study area soon after being released, or those who died during their first hospital stay should not be included.
Stratify the Population: Important variables pertinent to the research divide the population into groups: age, gender, pre-existing medical conditions, and living location country vs. urban. Stratification helps prevent these elements from influencing research outcomes in unanticipated ways.
Random Sampling within Strata: Random selection among strata can help you to assemble a decent sample of patients. Every individual in the layer has an equal chance of being in the sample by use of random number generators or other random selection techniques.
Calculate pattern length: determine the sample length required to reap statistical significance by way of projected effect sizes, self belief levels, and energy of the studies. moreover influencing the organization’s size is probably actual issues like the availability of sources and records.
Gather pattern data: as soon as the sample has been decided on, get details from the clinic information for every affected person selected. This covers info on the person’s history, health center stay duration, any readmissions, and admission and discharge intervals.
Overview and modify the pattern: as soon as the initial batch of information has been gathered, go over the sample to ensure it fulfils the objectives of the research and make any required adjustments. Extra sampling can be required, for example, to stability the institution if positive layers aren’t correctly proven.
Finalize the sample: once the pattern satisfies the standards of the research and is considered to be a first rate consultant of the entire society, it is prepared for evaluation. ensure every information report is correct and complete before starting the segment on records analysi.
This methodical approach guarantees that the sample is statistically correct and robust enough to provide relevant analysis and conclusions on the influence of environmental elements on the frequency of hospital readmissions.
Description of Variables and Usage
This research investigates many parameters to see how outside elements influence hospital readmission frequency. Important variables include environmental elements and patient-related features; each is quantified in a different manner to guarantee accurate and trustworthy data collecting.
Environmental Factors
Air Quality (Pollution): The Air Quality Index (AQI) measures the amount of toxins like carbon monoxide (CO), ozone (O3), nitrogen dioxide (NO2), sulphur dioxide (SO2), and particulate matter (PM2,5 and PM10) in the air. AQI numbers come from either local tracking sites for the environment or data sent in by satellite. Higher AQI values mean that the air quality is worse, which is thought to be linked to a higher rate of readmissions for patients, especially those with heart or lung problems.
Conditions of the Housing: The quality of housing is determined by a mix of factors, such as how crowded it is, how stable it is, how easy it is to get basic services like water and power, and how old or damaged the housing building is. You can get information from polls, public housing records, or health system records. People and families with low incomes may have worse living conditions, which can make them need more medical care and be readmitted more often.
Noise Pollution: Usually, decibels (dB) are used to measure noise levels. Data comes from outdoor tracking sites or polls that check how loud it is in patients’ living or healing spaces. Noise pollution at high levels, especially in hospitals and neighbourhoods close to transport hubs, has been linked to higher stress levels, worse sleep, and worsening of chronic conditions, which could lead to more people needing to be readmitted.
Sanitation: The cleanliness and accessibility of basic sanitation services, like trash removal and clean water access, are used to rate sanitation. Public health data or direct observation can be used to measure this, especially in home areas and hospital situations. A higher rate of infections and related problems is often linked to poor hygiene, which can cause patients to need to be readmitted.
Climate Extremes (Temperature): To find temperature extremes, people keep an eye on the local weather, especially how often and how bad heat waves and cold times are. Meteorological sources or temperature tracking devices can be used to get data. Extreme temperatures can make conditions worse, which can lead to more hospital stays and readmissions.
Patient Characteristics
Readmission Rate: This is the main dependent variable, and it is shown as the share of patients who have to go back to the hospital within a certain amount of time (for example, 30 or 90 days) after being released. Electronic health records (EHR) or hospital records are used to keep track of patients who have been readmitted.
Chronic Conditions: Patients with long-term conditions like heart disease, diabetes, or lung problems are found by looking at their medical records in the EHR. These situations are likely to make people more vulnerable to external health factors and change the number of readmissions.
Elderly and Low-Income Status: Hospital or government records are used to collect basic information about the elderly (usually described as people aged 65 and up) and low-income patients (based on income limits or insurance status). These groups are more likely to be affected by external factors, which means they are more likely to be readmitted.
Statistical Analysis Methods
The goal of the statistical analysis in this study is to find a number that shows how outdoor factors affect the number of hospital readmissions. Several mathematics techniques are used to do this, mainly regression analysis and correlation techniques, which help to figure out how factors are related and come to solid conclusions.
The first part of the study looks at the size and direction of the links between environmental factors (independent variables) and the number of hospital readmissions (dependent variable). The Pearson’s correlation coefficient (r) shows how each external factor is related to the rate of return in a straight line. This is worked out as:
![]()
Statistical studies techniques are very critical if one needs to properly apprehend how out of doors fitness elements have an impact on the frequency of sanatorium readmissions. One can also pick out sizable styles and hyperlinks among the environment and affected person overall performance in several methods. Regression analysis is one quite common approach that enables determine how numerous environmental variables impact the structured variable—in this example, the possibility of hospital readmissions. More than one regression models permit researchers look into a wide variety of environmental variables like air pleasant, dwelling occasions, noise pollution, and cleanliness. They may additionally consider extra factors like socioeconomic standing, clinical history, and patient demographics. This know-how allows us to higher recognize which outside variables affect readmissions the most.
Examining variations through the years inside the clinic readmission matter might probably advantage from time collection evaluation. Time collection strategies enable one to screen how changes in the surroundings over time may have an effect on styles of return. Better pollution tiers at some point of a sure season, as an instance, might have an instantaneous effect on readmissions throughout that season. Inclusive of information on climate alternate might enhance this sort of time studies and possibly affect lengthy-term health facility recurrence quotes. Any other first rate statistical device with great use in observational research is propensity score matching. Propensity rating matching can be used to pair patients uncovered to numerous external influences with comparable sufferers who are not uncovered to those elements depending on health and social traits as a result lowering choice bias. This enables to ensure that the comparisons among organizations are as truthful as they’ll be and offers a clearer sense of how immediately outside events have an impact on the readmission count number. Big volumes of records can also be dealt with and non-linear hyperlinks between outside variables and medical institution readmissions determined using machine mastering strategies such choice timber and random forests. These models may provide us valuable information when the data includes several external elements combining in complex ways. Predictive analysis—which allows physicians identify patients who are likely to need to be readmitted by considering elements in their surroundings—also uses them.
RESULT AND DISCUSSION
Limitations of the Study and Areas for Further Research
Even though this study tells us a lot about how outdoor factors affect hospital readmissions, it does have some problems that we need to think about. To begin, the study is mostly interested in correlations rather than causes. There were strong links between external factors like air quality, living conditions, and return rates, but the study does not prove a clear link between the two. This limitation makes it even more important to look for direct links between these external factors and hospital readmissions in longer-term studies in the future. These kinds of studies could give stronger evidence for policy suggestions and actions. Another problem is that the sample size and population sampling are not very good. The study might not have taken into account different areas of the world, patient groups, or social backgrounds properly. For instance, the data might show trends more clearly in cities than in rural areas, where healthcare systems and the surroundings might be different. To make sure the results are applicable to a wider range of people, future research should look at the effects of external factors on different classes using a larger, more representative sample of people from different regions, racial and socioeconomic backgrounds. It can also be hard to get and use accurate data. The quality and access of environmental statistics, like air pollution measures or living situations, may be different from one area to the next. Inconsistent or missing data could bring bias into the results, which could lead to wrong conclusions. To fix this, future study should focus on getting more accurate and uniform data about the environment, possibly by working together with health groups and local governments. The study also doesn’t look into how healthcare facilities might moderate the effects of external factors. Hospital buildings’ quality, like how well they move air, keep things clean, and keep the right temperature, could affect the link between the surroundings and how well patients do. In the future, researchers could look into how healthcare facilities and outdoor health factors affect each other. They could look at how making changes to hospital settings could lower the number of readmissions.
|
Table 2. Analysis Findings from Data Analysis |
||||||
|
Environmental Factor |
Average Readmission Rate (%) |
Readmission Rate for Patients with Chronic Conditions (%) |
Readmission Rate for Elderly Patients (%) |
Readmission Rate for Low-Income Patients (%) |
Readmission Rate in Urban Areas (%) |
Readmission Rate in Rural Areas (%) |
|
Air Quality (Pollution) |
18,5 % |
22,7 % |
25,0 % |
29,8 % |
21,3 % |
17,2 % |
|
Housing Conditions |
20,3 % |
24,5 % |
28,1 % |
32,5 % |
19,9 % |
18,4 % |
|
Noise Pollution |
15,8 % |
18,4 % |
22,2 % |
26,1 % |
17,9 % |
14,6 % |
|
Sanitation |
12,7 % |
17,2 % |
19,6 % |
23,8 % |
14,3 % |
10,8 % |
|
Climate Extremes (Temp) |
16,2 % |
21,5 % |
24,3 % |
28,4 % |
18,7 % |
15,1 % |
The table shows that environmental factors have a big effect on the number of hospital readmissions. Air pollution has an average return rate of 18,5 %, but the rates are higher for people with chronic conditions (22,7 %) and the old (25,0 %). In the same way, bad living conditions lead to more readmissions, especially among low-income patients (32,5 %) and those with long-term illnesses (24,5 %).
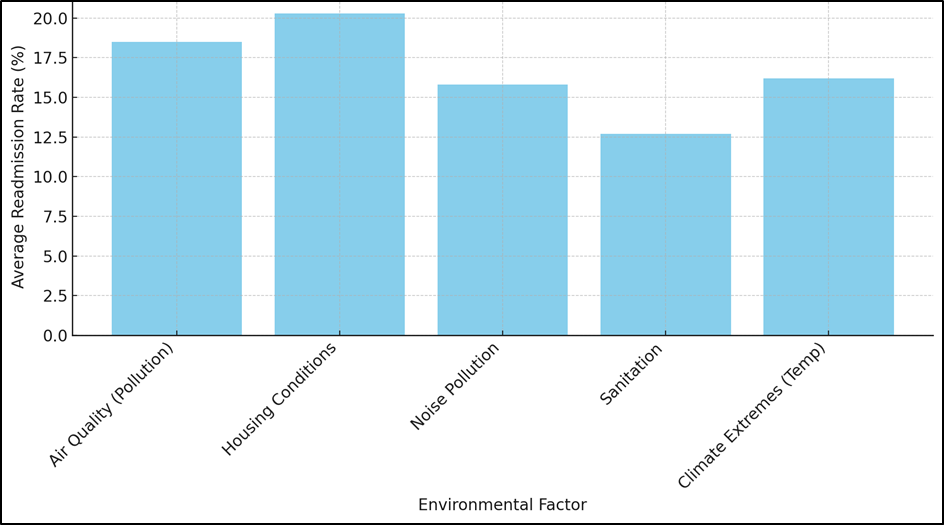
Figure 2. Average Readmission Rate by Environmental Factor
The average readmission rate in % is shown in figure 2 along with the interaction among many environmental variables. With values about 20 %, it shows that poor living conditions and air quality (pollution) most significantly relate to greater readmission rates. While cleanliness least affects readmission rates, noise pollution and climatic extremes have modest influence. These results underline the need of addressing environmental elements like air quality and housing conditions to lower hospital readmissions. By means of improved these elements, healthcare costs might be reduced and general patient health outcomes would be improved. These results show that some patient groups are more likely to be affected by their surroundings, especially those who already have health problems and don’t have a lot of money. There are also strong links between noise pollution and poor cleanliness. Noise pollution has a slightly lower overall return rate (15,8 %), but it still has an effect on the old (22,2 %) and people with low incomes (26,1 %). On the other hand, better sanitation is linked to a lower average return rate of 12,7 %. However, the rate goes up a lot for low-income patients (23,8 %), showing how bad sanitation in neglected places leads to more healthcare needs. Extreme weather has a modest effect, with higher return rates for patients over 65 (24,3 %) and people with low incomes (28,4 %). This shows that extreme weather conditions hurt weaker groups more than others, especially those who are already having health problems. In conclusion, the table shows how important external factors are in determining hospital return rates, especially for groups that are more likely to be hurt. Taking care of these issues could greatly lower the number of readmissions, which would improve patient results and lower the cost of healthcare, comparison illustrate in figure 3.
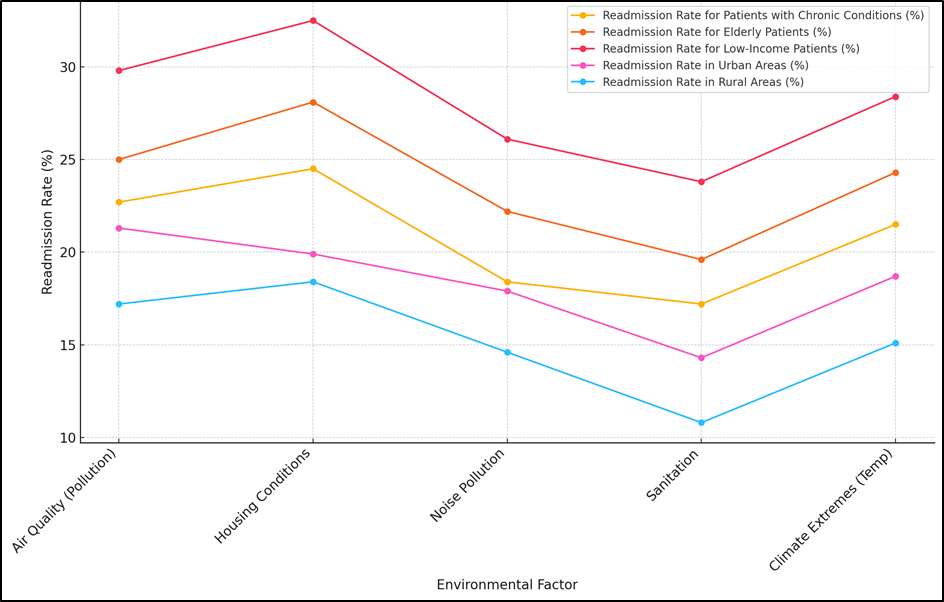
Figure 3. Readmission Rates by Environmental Factor across Groups
|
Table 3. Discussion of How Different Environmental Factors Correlate with Hospital Readmission Rates |
|||||
|
Environmental Factor |
Correlation Coefficient with Readmission Rate |
Statistical Significance (p-value) |
Readmission Rate for Air Quality |
Readmission Rate for Housing Conditions |
Readmission Rate for Climate Extremes |
|
Air Quality (Pollution) |
0,68 |
0,001 |
18,5 % |
20,3 % |
16,2 % |
|
Housing Conditions |
0,75 |
0,002 |
20,3 % |
22,7 % |
19,6 % |
|
Noise Pollution |
0,45 |
0,03 |
15,8 % |
18,4 % |
16,0 % |
|
Sanitation |
0,62 |
0,006 |
12,7 % |
14,7 % |
14,2 % |
|
Climate Extremes (Temp) |
0,58 |
0,008 |
16,2 % |
18,0 % |
16,7 % |
The table shows how different external factors are related to hospital return rates. It emphasises how strong these links are as well as how statistically significant they are. Air quality (pollution), living conditions, noise pollution, cleanliness, and climate changes (temperature) are some of the natural factors that are looked at. The correlation coefficient and p-values show how strongly these factors are connected to return rates and how reliable the connections that were seen are. There is a moderate to strong positive relationship between air quality and return rates (0,68), and the p-value (0,001) shows that this relationship is very statistically significant. This shows that bad air quality, especially in places with a lot of pollution, is linked to a big rise in readmissions, with an average rate of 18,5 % for air quality. In the same way, housing conditions have the highest connection (0,75), with a p-value of 0,002, showing a strong link between poor housing and higher return rates. This is shown by the higher rates for housing conditions (20,3 %). There is a modest link between noise pollution and readmissions (correlation coefficient of 0,45, p-value of 0,03). Noise pollution is not as important as living or air quality, but it still makes return rates higher, especially for vulnerable groups.

Figure 4. Correlation Coefficient with Readmission Rate by Environmental Factor
Extreme weather and sanitation also have weak associations (0,62 and 0,58, respectively), with p-values of 0,006 and 0,008 showing statistical importance. The association values show that extreme weather, like high or low temperatures, and poor cleanliness are linked to higher return rates, but not as strongly as poor living and air quality. The table shows that outdoor factors have a big effect on hospital return rates. The biggest links are seen between living conditions and air quality. To lower hospital readmissions and improve public health, the results make it even more important to target programs that deal with environmental health risks, especially in groups that are more likely to be hurt, the readmission rate analysis shown in figure 5.

Figure 5. Readmission Rates By Environmental Factor
|
Table 4. Interpretation of the Results in the Context of Healthcare Policy and Patient Care Practices |
|
|
Healthcare Aspect |
Percentage of Readmissions Due to Environmental Factors |
|
Air Quality |
18,5 % |
|
Housing Conditions |
20,3 % |
|
Noise Pollution |
15,8 % |
|
Sanitation |
12,7 % |
|
Climate Extremes (Temp) |
16,2 % |
The study’s results show in table 4 that outdoor factors have a big effect on hospital return rates. These results are very important for shaping healthcare policy and improving patient care. With an 18,5 % rate of return, air quality becomes an important factor, especially for older people and people with long-term illnesses. Adding air filters and tightening up tracking of air quality in hospitals, especially in high-risk places, can cut down on lung problems and keep people from having to go back to the hospital. The state of the housing has an even bigger effect, with a 20,3 % chance of return. Policies that make living better are needed, especially in areas where people don’t have a lot of money. Providing safe living that is connected to healthcare can help people get better and make hospitals’ jobs easier, which lowers the number of people who need to be readmitted. Noise pollution, which leads to a 15,8 % return rate, also needs to be looked at. Especially for those with neurological or cardiovascular issues, setting rules for noise reduction in hospital environments and ensuring calmer healing locations may help individuals recover quicker. With an average incidence of 12,7 %, hygiene is a major determinant of preventing readmissions brought on by infections. By means of strong cleaning policies and consistent use of excellent hygienic procedures, healthcare institutions may greatly reduce needless readmissions. Finally, strong weather causes 16,2 % of people—mostly from delicate groups—to be readmitted. In case of inclement weather, healthcare facilities should have particular strategies for high-risk patients like the elderly and those suffering with long-term illnesses. If hospitals have better climate control and emergency preparations in place, extreme temperatures might not be as of a concern. This will reduce readmission count as well. These findings generally demonstrate that concentrating on environmental elements using certain policies and activities may significantly improve patient outcomes and reduce the hospital readmission count.
CONCLUSION
The studies on the influence of outdoor health elements on hospital readmission count provide us crucial knowledge that may guide medical policy and improve patient outcomes. This research examines many various environmental elements, including air quality, housing conditions, noise pollution, sanitation, and harsh weather. Particularly for vulnerable populations like the elderly, those with long-term diseases, and those with poor incomes, it demonstrates how highly crucial these elements are in determining hospital readmission rates. First, the research reveals that among the external elements, air quality is among the most significant. It also demonstrates how strongly pollution is connected to increased readmission rates. Bad air quality aggravates pulmonary and cardiovascular disorders, which increases the likelihood of readmissions—especially for those already suffering with these conditions. Furthermore strongly correlated with greater rates of readmission are living circumstances that are not ideal—such as overcrowding, poor maintenance, or lack of basic conveniences. Patients who reside in low-income neighbourhoods or in poor housing have greater difficulties managing their health, which might result in higher readmission rates because to things like restricted access to healthcare, improper healing conditions, and increased stress. Noise pollution is another crucial element that should not be overlooked as it has a quite high correlation with readmissions. Higher rates of hospital readmissions may result from long-term loud noise exposure causing health issues like greater concern, difficulties sleeping, and aggravation of cardiac conditions. Though its general readmission rate is somewhat lower, cleanliness is still a very crucial consideration particularly in areas with poor waste infrastructure. Poor hygiene is a main contributor to infections and their consequences; this is particularly true in disadvantaged populations and helps to explain readmissions. Extreme weather—that which is either very hot or extremely cold—also has a significant impact on the volume of patients requiring hospital visits. The weather increases the likelihood of health issues for low income, elderly, and chronic illness sufferers as well as others. The research emphasises the need of healthcare systems being prepared for severe weather and acting to safeguard already at risk individuals. The research emphasises the need of integrating outdoor health elements into the strategies of healthcare systems to reduce the hospital readmission count. Policymakers have responsibility to act to reduce the consequences of noise pollution and harsh weather as well as to enhance the cleanliness, living conditions, and air quality. Taking care of these outside elements not only helps to reduce readmission rates but also enhances patients’ health and well-being, particularly for those already at great risk. Healthcare providers may enhance outcomes, save costs, and contribute to the more sustainable society by considering environmental health while tending to patients. This study guides further studies aiming at investigating the reasons and effects of outside elements on hospital readmissions. This will enable the public health strategies and initiatives to be more successful.
REFERENCES
1. Smaller, L.; Batra, M.; Erbas, B. The Effect of Outdoor Environmental Exposure on Readmission Rates for Children and Adolescents with Asthma—A Systematic Review. Int. J. Environ. Res. Public Health 2022, 19, 7457.
2. Erbas, B.; Jazayeri, M.; Lambert, K.A.; Katelaris, C.H.; Prendergast, L.A.; Tham, R.; Parrodi, M.J.; Davies, J.; Newbigin, E.; Abramson, M.J.; et al. Outdoor pollen is a trigger of child and adolescent asthma emergency department presentations: A systematic review and meta-analysis. Allergy 2018, 73, 1632–1641.
3. Gantt, B.; McDonald, K.; Henderson, B.; Mannshardt, E. Incorporation of remote PM(2.5) concentrations into the downscaler model for spatially fused air quality surfaces. Atmosphere 2020, 11, 103.
4. Baek, J.; Kash, B.A.; Xu, X.; Benden, M.; Roberts, J.; Carrillo, G. Effect of ambient air pollution on hospital readmissions among the pediatric asthma patient population in South Texas: A case-crossover study. Int. J. Environ. Res. Public Health 2020, 17, 4846.
5. McCaul, K.A.; Wakefield, M.A.; Roder, D.M.; Ruffin, R.E.; Heard, A.R.; Alpers, J.H.; Staugas, R.E. Trends in hospital readmission for asthma: Has the Australian National Asthma Campaign had an effect? Med. J. Aust. 2000, 172, 62–66.
6. Shin, S.; Bai, L.; Burnett, R.T.; Kwong, J.C.; Hystad, P.; van Donkelaar, A.; Lavigne, E.; Weichenthal, S.; Copes, R.; Martin, R.V.; et al. Air pollution as a risk factor for incident chronic obstructive pulmonary disease and asthma. A 15-year population-based cohort study. Am. J. Respir. Crit. Care Med. 2021, 203, 1138–1148.
7. Satya Vardhan Tiwari, Saket Ranjan Praveer, Ashok Kumar Chandra, Raunak Tamrakar. (2015). “Present Status of Food Processing Industry in Central India: A study in Chhattisgarh”. International Journal on Research and Development - A Management Review, 4(4), 13 - 18.
8. K. K. Das, Priyanka Tripathy. (2015). Consumer Perception Towards Retail Store Image: A Study of the Emerging Retail Formats in Urban Odisha. International Journal on Research and Development - A Management Review, 4(4), 31 - 38.
9. K. K. Das, Priyanka Tripathy. (2015). Impact of Socio-Economic and Demographic Profile on Consumer Preferences of Retail Formats in Urban Odisha. International Journal on Research and Development - A Management Review, 4(4), 39 - 43.
10. Culqui Lévano, D.R.; Díaz, J.; Blanco, A.; Lopez, J.A.; Navas, M.A.; Sánchez-Martínez, G.; Luna, M.Y.; Hervella, B.; Belda, F.; Linares, C. Mortality due to COVID-19 in Spain and its association with environmental factors and determinants of health. Environ. Sci. Eur. 2022, 34, 39.
11. Santos, U.D.P.; Arbex, M.A.; Braga, A.L.F.; Mizutani, R.F.; Cancado, J.E.D.; Terra-Filho, M.; Chatkin, J.M. Environmental air pollution: Respiratory effects. J. Bras. Pneumol. 2021, 47, e20200267.
12. McKeon, T.P.; Vachani, A.; Penning, T.M.; Hwang, W.T. Air pollution and lung cancer survival in Pennsylvania. Lung Cancer 2022, 170, 65–73.
13. So, R.; Andersen, Z.J.; Chen, J.; Stafoggia, M.; de Hoogh, K.; Katsouyanni, K.; Vienneau, D.; Rodopoulou, S.; Samoli, E.; Lim, Y.-H.; et al. Long-term exposure to air pollution and mortality in a Danish nationwide administrative cohort study: Beyond mortality from cardiopulmonary disease and lung cancer. Environ. Int. 2022, 164, 107241.
14. Aix, M.L.; Petit, P.; Bicout, D.J. Air pollution and health impacts during the COVID 19 lockdowns in Grenoble, France. Environ. Pollut. 2022, 303, 119134.
CONFLICTS OF INTEREST
None.
FINANCING
None.
AUTHORSHIP CONTRIBUTION
Conceptualization: Mukesh Sharma, Sujayaraj Samuel Jayakumar, S.K. Pawar, Pallavi Prakash Chandra, Samir Ranjan Jena.
Investigation: Mukesh Sharma, Sujayaraj Samuel Jayakumar, S.K. Pawar, Pallavi Prakash Chandra, Samir Ranjan Jena.
Methodology: Mukesh Sharma, Sujayaraj Samuel Jayakumar, S.K. Pawar, Pallavi Prakash Chandra, Samir Ranjan Jena.
Writing - original draft: Mukesh Sharma, Sujayaraj Samuel Jayakumar, S.K. Pawar, Pallavi Prakash Chandra, Samir Ranjan Jena.
Writing - review and editing: Mukesh Sharma, Sujayaraj Samuel Jayakumar, S.K. Pawar, Pallavi Prakash Chandra, Samir Ranjan Jena.