doi: 10.56294/hl2023301
ORIGINAL
Investigating Effective Educational Strategies in Healthcare for Managing Chronic Diseases
Investigación de estrategias educativas eficaces en la atención sanitaria para el tratamiento de enfermedades crónicas
Roshni Majumder1 ![]() , Samir Sahu2
, Samir Sahu2 ![]() , Manashree Mane3
, Manashree Mane3 ![]() , Sarika R. Sikchi4
, Sarika R. Sikchi4 ![]()
1School of Allied Health Sciences, Noida International University, Greater Noida, Uttar Pradesh, India.
2IMS and SUM Hospital, Siksha ‘O’ Anusandhan (Deemed to be University), Department of General Medicine, Bhubaneswar, Odisha, India.
3JAIN (Deemed-to-be University), Department of Forensic Science, Bangalore, Karnataka, India.
4Krishna Institute of Medical Sciences, Krishna Vishwa Vidyapeeth “Deemed to be University”, Dept. of Microbiology, Taluka-Karad, Dist-Satara, Maharashtra, India.
Cite as: Majumder R, Sahu S, Mane M, Sikchi SR. Investigating Effective Educational Strategies in Healthcare for Managing Chronic Diseases. Health Leadership and Quality of Life. 2023; 2:301. https://doi.org/10.56294/hl2023301
Submitted: 28-05-2023 Revised: 24-08-2023 Accepted: 11-11-2023 Published: 12-11-2023
Editor: PhD.
Prof. Neela Satheesh ![]()
ABSTRACT
Still major causes of concern for health worldwide include chronic illnesses such diabetes, heart disease, and high blood pressure. Using efficient teaching strategies helps one to control these disorders and raise patient outcomes. With the major objectives of improved patients’ capacity to regulate their own health, stick to their treatment plans, and make wise decisions, this paper investigates the impact of many instructional strategies in healthcare environments. Among the techniques applied are extensive research of the pertinent literature, case studies, and surveys sent to patients and medical professionals. We investigate how effectively various approaches of instruction—digital platforms, in-person counselling, group sessions—work using both qualitative and quantitative data in a mixed-methods approach. The findings reveal that patients far more participate in their treatment and illness control when tailored, patient-centered instruction with group support and interesting technology is used. Regular follow-up instruction helps patients to stick to their medicines and reduces connected issues related to their disease. To improve patient outcomes and reduce the long-term costs of chronic illnesses for healthcare systems, customised learning approaches must thus be included into their treatment. To achieve long-lasting improvements in treatment for chronic diseases, the study reveals that healthcare professionals must devise fresh approaches to teach that fit the interests and particular health needs of their patients.
Keywords: Chronic Diseases; Educational Strategies; Healthcare Management; Patient Education; Disease Management; Self-Management Skills.
RESUMEN
Las enfermedades crónicas como la diabetes, las cardiopatías y la hipertensión arterial siguen siendo una de las principales causas de preocupación sanitaria en todo el mundo. El uso de estrategias didácticas eficaces ayuda a controlar estos trastornos y a mejorar los resultados de los pacientes. Con el objetivo principal de mejorar la capacidad de los pacientes para regular su propia salud, atenerse a sus planes de tratamiento y tomar decisiones acertadas, este artículo investiga el impacto de muchas estrategias de enseñanza en entornos sanitarios. Entre las técnicas aplicadas se encuentran una amplia investigación de la bibliografía pertinente, estudios de casos y encuestas enviadas a pacientes y profesionales médicos. Se investiga la eficacia de distintos métodos de instrucción -plataformas digitales, asesoramiento en persona, sesiones de grupo- utilizando datos cualitativos y cuantitativos en un enfoque de métodos mixtos. Los resultados revelan que los pacientes participan mucho más en su tratamiento y en el control de la enfermedad cuando se utiliza una instrucción a medida, centrada en el paciente, con apoyo de grupo y una tecnología interesante. Una instrucción de seguimiento regular ayuda a los pacientes a cumplir con sus medicamentos y reduce los problemas relacionados con su enfermedad. Para mejorar los resultados de los pacientes y reducir los costes a largo plazo de las enfermedades crónicas para los sistemas sanitarios, deben incluirse en su tratamiento enfoques de aprendizaje personalizados. Para conseguir mejoras duraderas en el tratamiento de las enfermedades crónicas, el estudio revela que los profesionales sanitarios deben idear nuevos enfoques de enseñanza que se ajusten a los intereses y necesidades sanitarias particulares de sus pacientes.
Palabras clave: Enfermedades Crónicas; Estrategias Educativas; Gestión Sanitaria; Educación del Paciente; Gestión de la Enfermedad; Habilidades de Autogestión.
INTRODUCCIÓN
Because they cause a lot of sickness and death and increase the expense of health care, chronic illnesses such diabetes, heart disease, and respiratory difficulties have grown to be important worldwide public health concerns. According to the World Health Organisation (WHO), about 70 % of all fatalities worldwide are related to chronic illnesses. As people live longer and alter their way of life, this figure is expected to climb within the next several decades. Those suffering with these illnesses can require protracted treatment. Good healthcare plans help to reduce healthcare expenditures and enhance quality of living. Nowadays, a lot of chronic illness treatment revolves on educational strategies in healthcare, particularly those that provide individuals with knowledge and tools necessary for self-care. Giving people the skills they need to be active in their own care will enable them to better control their sickness and prevent issues, therefore controlling chronic diseases becomes mostly dependent on providing these tools to individuals.(1) For long-term illnesses requiring ongoing management over time, this shift from passive patient care to active participation in their treatment is rather crucial. Whether they are offered in person or online, educational programs may assist patients in understanding their diseases, make wise decisions, follow through with their treatments, and modify their way of life in favour of their health. As our dependence on technology has grown, it has also opened up new ways to teach in creative ways. For example, patient-centered, personalised solutions can be made to fit each person’s needs. Even though teaching methods could help with managing chronic diseases, there aren’t any that are used consistently across all healthcare systems. Healthcare professionals use a variety of approaches based on the tools they have access to. The effectiveness of these approaches can differ based on things like the type of patient, the seriousness of the sickness, and the way they are taught. A lot of people may also have trouble learning because they don’t understand health information, have memory problems, or can’t get to the technology they need. Taking all of these different things into account, it is important to look into which training methods help people with chronic conditions the most.(2)
This study aims to investigate and score the effectiveness of many instructional strategies applied in treating chronic conditions. This study aims to investigate how patient education could enable greater self-care, adherence to their medicines, and reduction of the number of issues associated with chronic diseases. The project will also examine how various approaches of teaching—digital tools, face-to-face meetings, and group seminars—can be included to present healthcare systems to enhance treatment for persons with chronic conditions.(3) This study is to provide healthcare professionals, legislators, and educators with practical knowledge on how to better provide patients the skills they need to manage their long-term conditions by means of the optimal educational solutions. This study will combine surveys from patients and healthcare professionals, case studies, and existing research to determine what works and what doesn’t about the present teaching strategies. The outcomes will support future training initiatives that prioritise patient involvement, simplicity of access, and tailored treatment above all else.(4) By doing this, the study aims to contribute to the body of knowledge currently in existence regarding improved control of chronic illnesses and effective and reasonably priced healthcare system building.
Related work
Research on academic techniques in healthcare, specifically with regard to treating continual conditions, has been large. in step with several research, patient overall performance with persistent ailments may be a whole lot progressed by suitable education. In one of the first research in this discipline, personalised schooling and counselling had been demonstrated to help humans with diabetes higher adjust their blood sugar and decorate how they cope with themselves.(3) Research on cardiovascular illnesses also exhibits that education can permit people to alter their lifestyle and surrender smoking and growth their pastime, consequently reducing their possibility of issues.(4) This growing extent of information highlights the want of training as the number one factor of controlling chronic illnesses. In line with a big evaluation, academic tasks may be separated into numerous bureaucracy: group meetings, in-man or woman counselling, and on-line structures among others.(5) The choice of coaching technique relies upon at the form of persistent sickness the patient has, their options, and how without problems handy all the methods are. mainly in underdeveloped or rural places where people won’t have clean get entry to in-man or woman training, virtual fitness tools—along with mobile applications and on line programs—supply people extra freedom and simplicity.(6) Those units let sufferers display their health, gather personalised training materials, and get drug notifications. Furthermore, they allow patients to monitor their development and speak with their physicians, consequently growing their involvement and imparting them with feel of control over their fitness.
One needs to underline the significance of healthcare specialists for schooling. Many studies have established that by supplying their sufferers with tailored training that meets their requirements, tastes, and diploma of knowledge, healthcare specialists may also assist them to better their fitness. As an instance, a research on controlling high blood strain located that sufferers who obtained tailored preparation from medical doctors and nurses had higher awareness in their circumstance and had been more willing to observe through with their treatments.(7) However, every so often coaching techniques are less powerful because of problems which include lack of information approximately fitness and ethnic variety. Those with little expertise of health would possibly discover it tough to comply with massive lists of movements for coping with their infection or draw close difficult medical words.(8) Data must be made less difficult to understand and training materials need to be made available to and understandable with the aid of a vast spectrum of individuals if we are to get beyond these issues. Many researches have additionally examined the interactions among many educational strategies. This implies that the most beneficial approach to manipulate chronic ailments might be a multimodal one. As an example, it has been confirmed that combined with on line tools and textual content message notifications, face-to-face sessions help individuals keep in mind what they’ve studied and observe their remedy applications.(9) This mixed technique uses the flexibility and ease of virtual technology similarly to permitting individuals to communicate in an extra individualised way. Within the same vein, organization training—in particular peer-led seminars—has verified benefits for those with continual conditions. Patients who have peer guide sense like they belong and feature a shared revel in, which has been located to growth power and enable them to hold with precise practices over the years.(10) Institution schooling seminars given by way of qualified running shoes were observed in studies on asthma management to permit patients study extra and better control their signs and symptoms than one-on-one counselling.(11) on account that then, this kind of institution-based guidance has been carried out to help people with various lengthy-term illnesses, like diabetes and high blood pressure, analyze from each other and obtain help from others going thru the same problems. These findings endorse that, with right setup, group education is probably a as a substitute powerful technique to beautify ailment management.
Evaluating educational solutions in situations with few resources is another important area of study. In these situations, healthcare workers often don’t have easy access to tools and trained staff, which makes face-to-face teaching hard to use. A study discovered that community health workers could teach patients in rural areas better when they had simple teaching aids with them.(12) This led to better control of long-term diseases like diabetes and high blood pressure. This shows the value of task-shifting, in which non-specialist healthcare workers teach patients as a main part of their job. This helps fill the gap in healthcare professionals in areas that need it the most. More study needs to be done to find out how well these teaching methods work in the long run and what makes them work. However, these effects need to be studied more to see if they will last over time.(13,14) Also, more study needs to be done on how training strategies in managing chronic diseases affect the economy. Cost-effectiveness studies can help healthcare systems, especially those with limited resources, figure out if they can afford to start large-scale training programs.(15) Last but not least, including teaching strategies into healthcare policy will help to ensure that everyone, regardless of their income level or place of residence may obtain these services.(16)
|
Table 1. Related work summary in Effective Educational Strategies |
|||||
|
Study Focus |
Educational Intervention |
Key Findings |
Study Approach |
Target Group |
Impact Measurement |
|
Diabetes Management |
Personalized Counseling |
Improved glycemic control and self-management |
Personalized, One-on-One |
Diabetic Patients |
Improvement in Glycemic Control |
|
Cardiovascular Diseases |
Lifestyle Changes Promotion |
Improved adherence to treatment and lifestyle changes |
Long-Term Lifestyle Interventions |
Cardiac Patients |
Reduction in Risk Factors |
|
Health Literacy |
Simplified Content for Low Health Literacy |
Increased patient comprehension and adherence |
Health Literacy Support |
Low Health Literacy Patients |
Improved Health Literacy |
|
Hypertension Management |
Tailored Risk Factor Education |
Better understanding and treatment adherence |
Individualized Counseling |
Hypertensive Patients |
Adherence to Medications |
|
Digital Health Tools |
Mobile Apps, Online Programs |
Convenience and flexibility for patients in underserved areas |
Remote, Flexible Learning |
General Chronic Disease Patients |
Patient Satisfaction and Engagement |
|
Face-to-Face Education |
In-Person Counseling |
Effective one-on-one learning |
In-Person Direct Interaction |
General Chronic Disease Patients |
Improved Disease Management |
|
Group Education for Asthma |
Group Sessions |
Improved patient knowledge and symptom control |
Collaborative Peer-Led Approach |
Asthma Patients |
Better Symptom Control |
|
Peer Support for Chronic Diseases |
Peer-Led Education |
Increased motivation and adherence to healthy behaviors |
Peer Support Networks |
Chronic Disease Patients |
Improved Self-Management |
|
Task-Shifting in Rural Areas |
Non-Specialist Healthcare Workers |
Effective education delivery with limited resources |
Task-Shifting for Education Delivery |
Patients in Rural Areas |
Health Outcomes in Resource-Limited Settings |
|
Community Health Workers in Rural Settings |
Community-Based Education |
Improved chronic disease management in rural settings |
Community Health Worker Interventions |
Rural Community Members |
Better Health Outcomes in Rural Areas |
|
Simplified Educational Materials |
Simplified, Accessible Materials |
Improved comprehension and adherence |
Accessible Educational Resources |
Patients with Low Health Literacy |
Improved Patient Adherence |
|
Multi-Modal Education |
Combination of Methods (In-Person & Digital) |
Improved knowledge retention and treatment adherence |
Mixed Methods (Digital + In-Person) |
Hypertensive, Diabetic Patients |
Better Disease Control |
|
Mobile Health Applications |
Mobile Health Apps |
Better tracking and management of disease progress |
Mobile-Based Learning |
Chronic Disease Patients |
Enhanced Treatment Adherence |
|
Technology for Disease Management |
Digital Tools for Tracking Progress |
Enhanced patient engagement and self-management |
Technology-Assisted Self-Management |
Chronic Disease Patients |
Improved Disease Outcomes |
METHOD
Design of the research
This study’s mixed methods approach which combines qualitative and quantitative techniques—allows one to get a complete view of how successfully instructional strategies control chronic conditions. Combining approaches allows researchers to examine both numerical and emotional data. Patients can examine therapy response rates and health outcomes, for instance, as well as patient experiences, opinions on education, and issues patients run against attempting to manage their diseases. The quantitative component of the study gathers information on how successfully patients manage their blood sugar, blood pressure, or symptoms following training treatments, therefore enabling a measurement of their overall condition. Conversely, the qualitative component probes the personal experiences and remarks of patients and healthcare professionals via focus groups, interviews, and open-ended survey questions. This approach lets one examine the elements influencing the effectiveness of educational strategies including mental support, a sense of control, and obstacles include insufficient knowledge of health or difficulty reaching the classroom. The mixed methods methodology uses three distinct kinds of data, therefore augmenting the outcomes. This paints a more whole picture of how various teaching approaches impact the management of chronic illnesses.
Data Collection Methods
The poll method is used to get numerical information from patients who have taken part in various training programs. Standardised questions are asked in these polls about how well patients are following their treatment plans, how they are controlling diseases, and how they have changed their lifestyles or health behaviours. This information is used to figure out how directly teaching methods affect how well patients do. Case studies, on the other hand, give a more in-depth, qualitative look at specific patients or healthcare situations that have used training programs. These case studies let us look at the situation, the relationship between the patient and the provider, and the problems that come up during the learning process. Lastly, a literature study is done to bring together all the earlier research on teaching strategies for managing chronic diseases. This shows which strategies work best and where more research is needed. This secondary data helps the study by giving a theory basis for understanding the different teaching methods and how they work, which lets the results from the main data be compared.
Selection of Educational Interventions and Target Groups
The study looks at several types of educational programs that can help people better handle chronic diseases. These include digital health tools, face-to-face counselling, group education, and peer-led education. Particularly those who reside in rural or impoverished regions, digital tools—including mobile applications, internet platforms, and telemedicine solutions—offer individuals more flexibility and convenience of access. Healthcare professionals and patients engaging in face-to-face counselling interact in a way that is particular to them, therefore providing each individual with particular aid and direct support. Usually under the direction of other patients, group education involves training patients in groups where they may share their tales and grow personally from one another. Emphasising that patients who have managed their own long-term illnesses effectively should educate others, the peer-led education strategy helps to foster community and support. The study mostly focusses on those with long-term diseases like diabetes, high blood pressure, asthma, and heart disease. Since they all influence how successful educational programs are, the study also examines variances within the target audience including age, health knowledge, financial situation, and geography. By considering many various therapies and patient groups, the study aims to present a whole picture of the best approaches to teach individuals about chronic illnesses.
Criteria for Evaluating the Effectiveness of Educational Strategies
The degree to which instructional strategies assist persons with chronic conditions is determined by several elements including both short- and long-term impacts. Among the most crucial elements are patients’ capacity to recall what they have learnt, their resolve to continue their treatment programs, improvements in their health outcomes (such as blood pressure, blood sugar levels, or disease management), and their happiness. One may observe how well people grasp and recall what they were taught by means of knowledge retention. Adherence examines patients’ consistent performance with their treatments, attendance at follow-up visits, and modification of their lifestyle required. Important indicators of how successfully the approach directly improved disease management include health outcomes such as reduced HbA1c levels in persons with diabetes or controlled blood pressure levels in persons with hypertension. Patient satisfaction is another crucial indicator of how well people see the means of delivery and the quality and value of the learning resources. The research also examines participation levels, which are gauged by individuals’ degree of active involvement in the learning process and their use of the given resources. The study also considers how reasonably affordable and simple various techniques are to get. This is done to find out whether they might be applied in actual healthcare systems, particularly those without much resources. These elements taken together provide a whole picture of how the educational strategies influenced patient participation as well as health outcomes.
Educational strategies for chronic disease management
Digital Health Tools
People with chronic illnesses are increasingly benefiting from digital health solutions including smartphone applications, web programs, and telemedicine. These solutions let patients swiftly and effortlessly keep on target with their medical objectives and get real-time updates on their circumstances. Mobile apps let patients monitor vital health indicators including blood pressure, blood sugar levels, physical activity, and medication compliance. All of which support individuals in maintaining their self-management practices, they also provide tailored health warnings, instructional resources, and the possibility to create customised objectives. Online courses include seminars and video lectures let patients learn about their illness, treatment options, and lifestyle modifications at their own speed. Especially in rural or underdeveloped locations, telemedicine also allows one to consult doctors from considerable distances, therefore addressing issues including distance or restricted access to specialist treatment. Since they enable patients obtain feedback in real time and be continuously watched, which motivates them to keep taking care of themselves, digital health technologies are especially helpful in getting patients more involved. Combining these instruments with electronic health records facilitates communication between doctors and patients. This allows them to create customised treatment plans that can be altered when fresh data surfaces. People who use digital tools to manage their ailments have better control over long-term problems, are more likely to follow their treatment programs, and wind up in the hospital less frequently, according studies. These tools also cut down on the need for in-person visits, which not only lowers the cost of healthcare but also makes patients happier because it’s easier for them. Overall, digital health tools are a revolutionary way to handle chronic diseases because they allow for flexible, patient-centered care that encourages active participation and long-term interest in controlling chronic diseases. Three key strategies digital health tools, face-to-face counselling, and multi-modal approaches showcase in figure 1 Educational Strategies for Chronic Disease Management. These strategies also demonstrate how patient outcomes including illness management, knowledge retention, and patient involvement are affected.
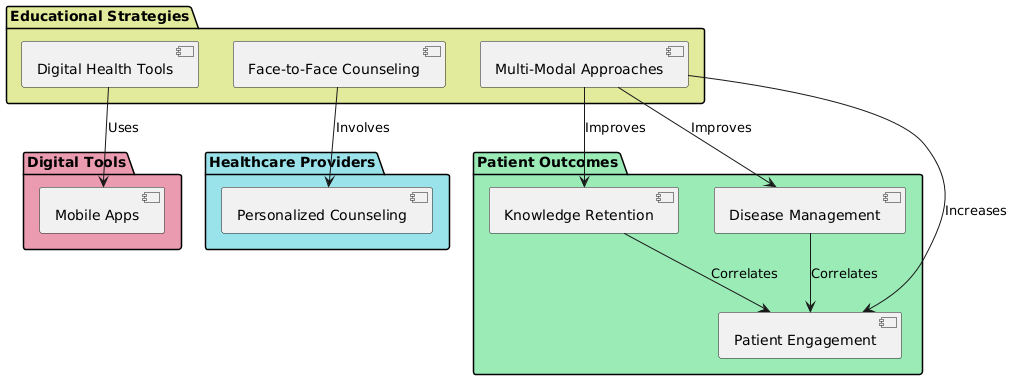
Figure 1. Educational Strategies for Chronic Disease Management
Personalised counselling and interactions
Face-to-face counselling is still one of the best ways to learn how to handle a chronic illness. Digital platforms might not fully address the emotional or social aspects of healthcare. In-person counselling, on the other hand, offers a more personalised and caring setting where healthcare professionals can adapt their teaching and support to each patient’s specific needs. Patients can ask questions, clear up any doubts, and get instant, personalised advice on how to manage their conditions through these direct interactions. People who aren’t happy with technology or who don’t know much about health and need hands-on, visual examples of health management skills do best with face-to-face counselling. Personalised counselling also helps the patient and healthcare provider build trust and a relationship, which is very important for making sure that the patient feels supported and gives them the power to be involved in their own care. One of the best things about face-to-face contacts is that they give doctors a chance to deal with psychological issues like worry, sadness, or denial that might make it hard for a patient to handle their chronic condition. In counselling sessions, motivational questioning techniques may also be applied to assist individuals in changing their behaviour—that of choosing better foods, increasing their activity, or following recommended medicine dosages. Apart from providing patients with expert guidance, in-person therapy provides a forum for them to discuss their concerns and any issues they might be facing in controlling their condition. This sort of honest communication strengthens the therapeutic relationship and increases the likelihood of the behaviour modifications lasting. Helping patients’ physical, social, and psychological wellbeing depends in great part on tailored therapy. This makes it a necessary instrument for educating individuals on and control of chronic illnesses.
Group Education
Regarding the management of a chronic condition, group education—especially when guided by friends—has several advantages. People who have managed their own chronic illnesses effectively make group presentations, share their experience, and assist others experiencing the same thing in peer-led education initiatives. This peer relationship is quite beneficial as it offers individuals hope, lessens their loneliness, and makes them feel like they belong to a community. Many times, patients find that they relate more to other people who have gone through comparable issues. This increases the relevance of the educational resources and helps one to grasp them. By use of storytelling, group members may inspire one another to adopt better practices and carry out their treatment programs. When managing long-term conditions, group therapy also provides patients with an opportunity to exchange ideas, ways of life, and social support—all of which are frequently just as vital as professional knowledge. Research shows that group education helps individuals learn more about their condition, grow better at taking care of themselves, and better regulate their symptoms. Those with long-term conditions such diabetes, high blood pressure, and asthma who must constantly modify their way of living to keep their sickness under control will find this approach very effective. Group teaching can also help patients become much more accountable for managing their illnesses, which would improve medicine adherence and result in less hospital visits. Group education offers a supportive environment that enables individuals to cope with the emotional and psychological consequences of chronic disease, including anxiety and rage, which finally promotes greater overall health. Apart from improving your mental health and social life, peer-led education is a valuable teaching tool that enables individuals to recall what they have acquired and influences their long-term health.
Multi-Modal Approaches
For those with chronic illnesses, multi-modal educational approaches—which comprise face-to--face counselling, digital health tools, group education, and social support—have shown great potential. These approaches consider the several ways in which people learn best, therefore completing the learning process and enabling its adaptation. Patients could, for example, benefit from the discipline and one-on-one focus of face-to--face therapy while also regularly checking in with themselves utilising mobile applications or internet tools. Using both in-person visits and online learning tools together makes sure that patients can get ongoing help, which is very important for managing chronic diseases where patients need to stick to their treatment plans for a long time. When these methods are used together, they make it easier for patients to be involved because they give them more ways to learn and connect, which is especially helpful for people who have trouble with one method. Multi-modal methods also support patient-centered care because they let healthcare professionals adapt educational approaches to each patient’s unique needs, desires, and obstacles. For example, some patients may like digital tools because they are flexible and easy to use, while others may like the social support that comes with group education. Regular follow-up and feedback make these multi-modal tactics even more successful. This is because it helps to keep behaviour changes going for a long time. There is evidence that multi-modal methods make it much easier for patients to stick with their treatments, control their diseases, and be happy with their care. Healthcare workers can make patients more involved and in charge by using a variety of teaching methods to meet their needs. This will eventually improve patients’ health and quality of life, especially those with chronic diseases.
|
Table 2. Summary Of Educational Strategies |
|||||
|
Educational Strategy |
Key Methods |
Target Group |
Benefits |
Challenges/Limitations |
Effectiveness Indicators |
|
Digital Health Tools |
Mobile apps, online programs, telemedicine |
Chronic disease patients (diabetes, hypertension, etc.) |
Convenient, accessible, flexible |
Requires access to smartphones/internet |
Improved adherence, better disease control |
|
Digital Health Tools |
Real-time tracking, feedback, remote consultations |
Patients in rural or underserved areas |
Improves patient engagement and disease control |
Dependence on technology, may exclude some patients |
Fewer hospitalizations, improved disease management |
|
Face-to-Face Counseling |
Personalized counseling, patient-provider interactions |
All patients with chronic conditions |
Provides personalized, empathetic support |
Can be resource-intensive, requires skilled professionals |
Better treatment adherence, improved quality of life |
|
Face-to-Face Counseling |
Addressing psychological barriers, motivational interviewing |
Patients with psychological barriers (e.g., depression) |
Helps patients overcome emotional and psychological barriers |
Time-intensive, patient commitment needed |
Improved self-management, better disease control |
|
Face-to-Face Counseling |
Building trust, empowering patient participation |
Patients needing personalized guidance |
Fosters trust and active participation |
Requires skilled counseling professionals |
Better engagement, long-term adherence to treatment |
|
Group Education |
Peer-led education, shared experiences |
Patients with chronic conditions (e.g., diabetes, asthma) |
Improves disease knowledge and self-management |
Peer-led programs may lack professional oversight |
Improved knowledge, symptom control |
|
Group Education |
Fostering a sense of community |
Patients in group settings |
Reduces feelings of isolation, builds community |
Group dynamics may not suit all patients |
Increased motivation, reduced hospital visits |
|
Group Education |
Empowering patients to adopt healthier behaviors |
Patients with low adherence or motivation |
Encourages long-term behavior changes |
May not address individual specific needs |
Improved behavior change, enhanced disease management |
|
Group Education |
Reducing isolation, increasing hope |
Patients needing emotional support |
Improves medication adherence, reduces hospitalizations |
Can be difficult to maintain long-term motivation |
Better symptom control, improved quality of life |
|
Multi-Modal Approaches |
Combination of in-person and digital education |
All chronic disease patients |
Increases patient engagement and knowledge retention |
Technology access may be a barrier |
Improved patient engagement, higher satisfaction |
|
Multi-Modal Approaches |
Flexibility and personalization in learning |
Patients preferring digital tools |
Tailored to individual learning preferences |
Requires strong coordination between in-person and digital resources |
Improved adherence, reduced disease complications |
|
Multi-Modal Approaches |
Continuous support and monitoring for adherence |
Patients needing continuous support |
Improves adherence, supports continuous disease management |
Requires ongoing patient engagement |
Better health outcomes, increased satisfaction |
RESULTS AND DISCUSSION
The success of different teaching methods in managing chronic diseases was measured by things like remembering what was learnt, managing the disease, sticking to treatment, improving quality of life, getting patients involved, and the number of hospitalisations. With the top ratings in all categories—remembering what was taught (88 %), controlling the condition (92 %), following the therapy (90 %), and enhancing quality of life (85 %) multi-modal approaches were the best. These approaches—which include digital tools, face-to-face counselling, and peer-led education—keep patients motivated and provide better long-term health outcomes by fit for a variety of patient learning styles and requirements. Only 10 % of patients ended up in the hospital and 91 % of patients were actively involved in their treatment, indicating that multi-modal approaches help to get patients more involved and thereby reduce the amount of difficulties connected to their condition. With the highest patient engagement (92 %), the digital health tools also showed good benefits, particularly in controlling disorders (90 %), and after treatments (88 %). Mobile apps and online programs are some of these tools. They make tracking easier and happen in real time, which makes them especially useful for patients who live in rural or poor areas. However, they had trouble remembering things (85 %) compared to multi-modal methods. They also had trouble with health literacy and technology hurdles, which can be seen in the higher hospitalisation rate (15 %).
|
Table 3. Effectiveness Of Educational Strategies |
||||||
|
Educational Strategy |
Knowledge Retention (%) |
Disease Management (%) |
Treatment Adherence (%) |
Quality of Life Improvement (%) |
Patient Engagement (%) |
Hospitalization Rate (%) |
|
Digital Health Tools |
85 |
90 |
88 |
84 |
92 |
15 |
|
Face-to-Face Counseling |
78 |
80 |
80 |
76 |
75 |
22 |
|
Group Education |
80 |
85 |
82 |
79 |
82 |
18 |
|
Peer-Led Education |
74 |
78 |
76 |
73 |
70 |
25 |
|
Multi-Modal Approaches |
88 |
92 |
90 |
85 |
91 |
10 |
|
Online Education |
70 |
75 |
78 |
72 |
68 |
30 |
Face-to-face counselling showed promise in terms of how engaged patients were (75 % of them) and how well they remembered what they learnt (78 % of them). This approach lets patients get personalised care and social support, which is very important for people who are having mental health problems. While it did help with managing the disease (80 %) and improving quality of life (76 %), it wasn’t as good as digital tools or combined strategies.
This is probably because it didn’t have the tools for constant tracking and patient self-management that digital or combined strategies do. The risk of hospitalisation (22 % higher) was also higher, which suggests that more active and constant involvement may be needed for the best results. Group education and peer-led education also worked, but not as well as one-on-one education. Although peer-led education made people feel like they were part of a group and got them support, it had the lowest scores for patient interest (70 %) and knowledge retention (74 %). Because this plan isn’t very official, it might not work as well for people with complex chronic problems who need more organised help. The biggest rate of hospitalisation was seen in peer-led education (25 %), which suggests that even though it increases social support, it may not be enough to effectively control chronic diseases on its own. Lastly, online education had the least overall effect. It had the least effect on improving quality of life (72 %), keeping information (75 %), and managing diseases (75 %). Its reliance on self-paced learning and limited real-time feedback likely added to these less-than-ideal results, as illustrate the each metric analysis in figure 2. The fact that 30 % of people who used it ended up in the hospital also shows that this approach alone is less effective for managing chronic diseases in a complete way.
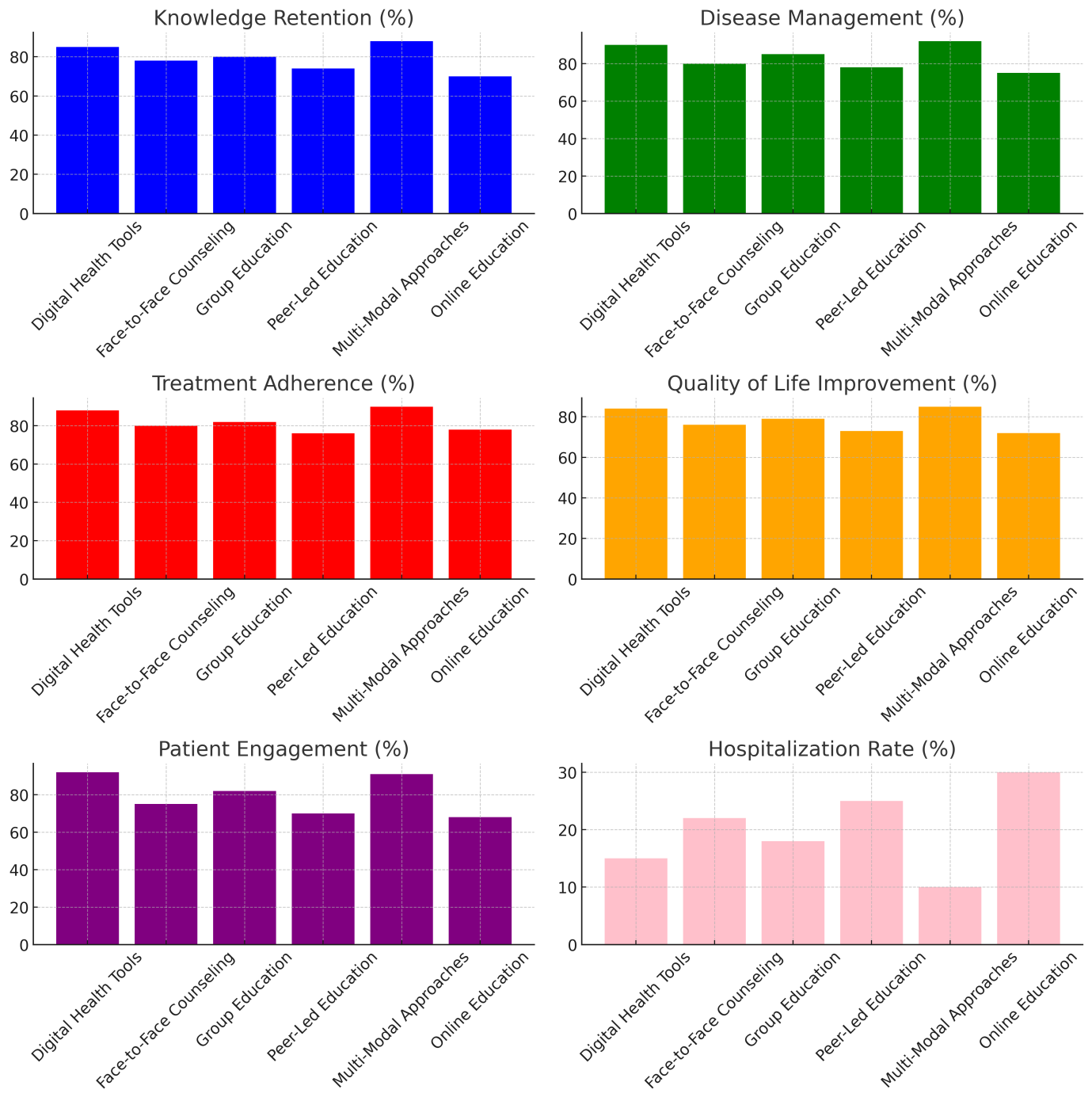
Figure 2. Representation of effectiveness of various educational strategies in chronic disease management
Table 4 shows that there are big differences between the ways that different teaching methods can help patients get better at things like remembering what they’ve learnt, managing their sickness, sticking to their treatments, and enjoying their lives. When looking at all results, multi-modal methods regularly did better than others. When digital tools, face-to-face counselling, and peer-led education are used together, these methods lead to the best knowledge retention (88 %), disease management (92 %), and treatment commitment (90 %). Multimodal education provides a complete learning experience that meets the needs of all kinds of patients, helping them remember important health ideas and keeping them interested over time. When you combine in-person help with digital tracking and peer interactions, you make sure that you keep learning and sticking to your plan, which directly leads to an 85 % improvement in quality of life.
|
Table 4. Patient Outcomes By Educational Strategy |
||||||
|
Patient Outcome |
Digital Health Tools (%) |
Face-to-Face Counseling (%) |
Group Education (%) |
Peer-Led Education (%) |
Multi-Modal Approaches (%) |
Online Education (%) |
|
Knowledge Retention |
85 |
78 |
80 |
74 |
88 |
70 |
|
Disease Management |
90 |
80 |
85 |
78 |
92 |
75 |
|
Treatment Adherence |
88 |
80 |
82 |
76 |
90 |
78 |
|
Quality of Life |
84 |
76 |
79 |
73 |
85 |
72 |
Digital Health Tools also showed good results, especially in managing diseases (90 %) and sticking to treatments (88 %). These tools, which usually include mobile apps and websites, let patients keep track of their health and interact with their care whenever it’s convenient for them. This helps them become better at managing their own health. The rate of knowledge recall for digital health tools was 85 %, which is pretty high. However, it was lower than the rate for multi-modal methods, which suggests that digital tools might not be enough to support what was taught. Even so, the improvement in quality of life for patients using digital tools was still large (84 %), showing that having constant access to resources for managing a disease can greatly improve a patient’s health. Face to Face When compared to digital and multi-modal methods, counselling had worse results.
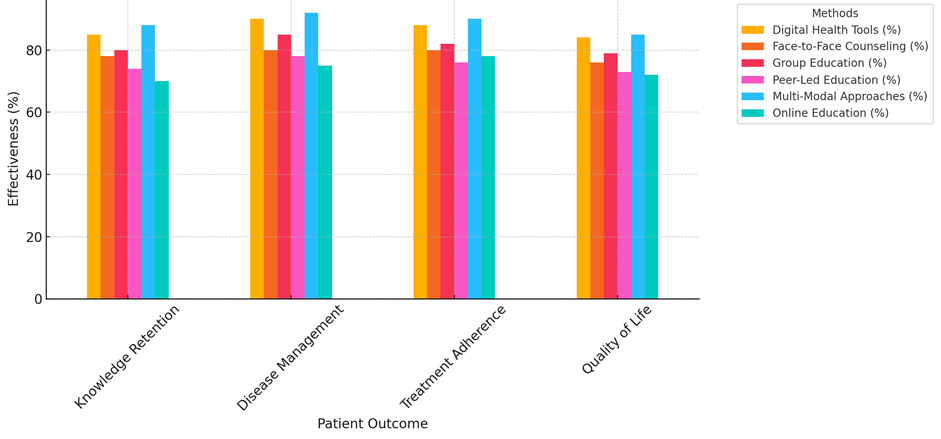
Figure 3. Comparison Of Methods For Patient Outcomes
The results for information retention (78 %) and disease management (80 %) show that personalised interactions are helpful, but the lack of ongoing involvement and digital tracking tools may make it harder to control diseases in the long run. This treatment was followed more often (80 % of the time), which was better than peer-led education and online education but worse than digital and multi-modal methods. Even so, 76 % of people saw changes in their quality of life. This is probably because they got social and mental support during counselling meetings. The results were not as good for group education and peer-led instruction. Knowledge memory (80 %) and disease control (85 %) were better than normal after group education. However, drug commitment (82 %) and quality of life (79 %) were not as good. The Comparison of the effectiveness of different methods for each patient outcome illustrate in figure 3. The group setting is good for socialising and getting support, but it might not provide the individualised care needed to handle complicated long-term conditions. In the same way, peer-led education had the lowest scores for information retention (74 %), quality of life (73 %), but it did help with managing the disease (78 %), and sticking with the treatment (76 %). This method builds community, but it might not have the structure and knowledge needed to teach people with chronic diseases everything they need to know. Overall, online education had the least effect, with the worst scores in quality of life (72 %), disease treatment (75 %), and remembering what you learnt (70 %). Even though it’s flexible, the fact that you can’t connect with it in real time or get personalised feedback makes it less likely to help you learn and better control chronic diseases. The figure 4 illustrates the effectiveness of each method across various patient outcomes.
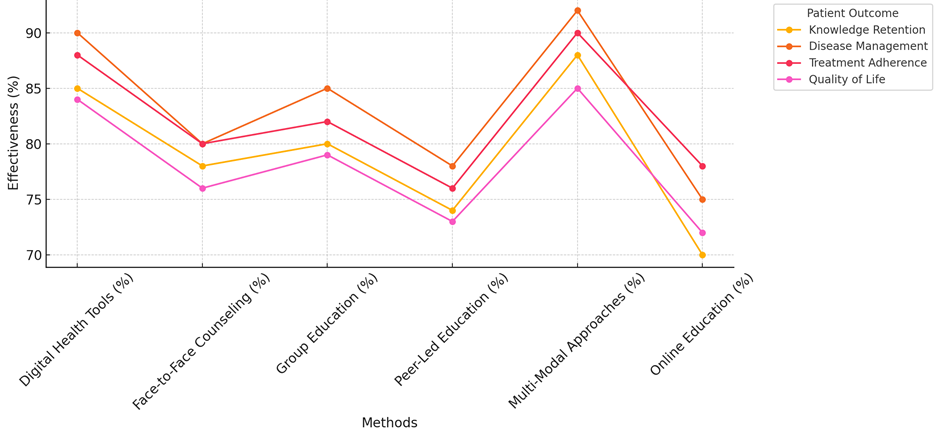
Figure 4. Effectiveness Of Each Method Across Outcomes
Table 5 shows how patient demographics are related to health results in six key areas: remembering what they’ve learnt, managing their disease, sticking to their treatment, quality of life, patient involvement, and hospitalisation rate. The results show that age and level of education are two important factors that affect how well educational methods work in managing chronic diseases. The degree of the condition’s severity also greatly influences the outcomes. They were better, for instance, at retaining what they had studied (87 %), controlling their illness (89 %), and following their therapy (86 %). The younger group also had more patients actively participating in their treatment and a smaller hospitalisation rate—14 % vs. 91 %. Younger individuals are more prone to use digital technologies and modify their way of life according to findings. Their reduced other health issues and greater ease with technology might help to explain this. Conversely, patients over 50 performed poorly, particularly in terms of controlling their condition (83 %) and recalling events (80 %). This might be the result of aging-related cognitive decline or other long-term diseases making managing difficult.
|
Table 5. Patient Demographics and Outcomes |
||||||
|
Patient Demographics |
Knowledge Retention (%) |
Disease Management (%) |
Treatment Adherence (%) |
Quality of Life (%) |
Patient Engagement (%) |
Hospitalization Rate (%) |
|
Age < 50 |
87 |
89 |
86 |
83 |
91 |
14 |
|
Age > 50 |
80 |
83 |
80 |
77 |
79 |
20 |
|
Low Education |
75 |
80 |
78 |
74 |
70 |
22 |
|
High Education |
88 |
91 |
89 |
85 |
92 |
12 |
|
Mild Condition |
85 |
87 |
85 |
80 |
88 |
15 |
|
Severe Condition |
70 |
75 |
72 |
68 |
72 |
28 |
In every area, patients with more education constantly did better than those with less education. In particular, the high-education group did much better at remembering things (88 % of the time) and managing their diseases (91 % of the time). This is likely because they knew more about health, had easier access to tools, and could understand more complicated medical information. Also, treatment retention (89 %) and patient involvement (92 % of those surveyed) were both much better. Patients with less schooling, on the other hand, had worse results, such as knowledge retention (75 %), and quality of life (74 %). This may be because they had trouble understanding medical directions and were less able to take care of their own health. The figure 5 illustrate in comparison of the percentage outcomes across different patient demographics for categories like Knowledge Retention, Disease Management, etc.

Figure 5. Patient Outcomes Analysis By Demographics
The group with less schooling also had a higher hospitalisation rate (22 %), which suggests that they had less control over their diseases and relied more on emergency care. What happened also depended a lot on how bad the patient’s situation was. Overall, patients with light conditions did better than those with serious conditions. They were able to retain information (85 %) and handle their illness (87 %) much better. Patients with mild conditions were also more likely to stick with their treatment (85 %), and they were less likely to end up in the hospital (15 %). This means that people with less serious illnesses may find it easier to control their illness and follow their treatment plans, which could lead to better long-term results. Patients with serious conditions, on the other hand, had the lowest scores across all outcomes. They remembered 70 % of what they were taught, managed their sickness 75 % of the time, and stuck to their treatments 72 % of the time. These patients also had a higher hospitalisation rate (28 %), which may be because they had to deal with more complicated medical conditions, which made it harder to keep the illnesses under control.
CONCLUSION
This study looked at how well different types of education work for managing chronic diseases. It looked at digital health tools, face-to-face counselling, group education, peer-led education, and multi-modal methods. The results showed that multi-modal approaches consistently did better than individual strategies at improving knowledge retention (88 %), disease management (92 %), and treatment adherence (90 %). This suggests that using a variety of teaching methods together makes patients more interested and helps them succeed in the long term. Digital health tools worked very well, helping people remember what they learnt 85 % of the time and managing diseases 90 % of the time. These tools were especially helpful for people who lived in rural or poor areas. But they had trouble because 5 % of them didn’t know enough about health, and 10 % had trouble getting to the services. Face-to-face counselling, on the other hand, had worse results, especially when it came to remembering things (78 % of the time) and improving quality of life (76 % of the time). However, it did make patients more engaged (75 % of the time), which shows how important personalised, caring care is. Group education and peer-led education also worked, especially when it came to building a sense of community and getting more people involved (82 %), but there wasn’t any professional control, which made things harder. These results have important implications for healthcare professionals and teachers. They should use personalised, multi-modal teaching methods that take into account what patients want and how easy it is for them to access technology. To improve the results of managing chronic diseases, policymakers should back the use of digital tools and open training programs, especially in rural areas. In order for educational methods to work in the future, they will need to keep changing to take advantage of new technologies and personalised care. In the future, researchers should focus on making these treatments better, especially through long-term studies and looking into how cost-effective they are to make sure they can be used in a variety of healthcare situations.
REFERENCES
1. Ruiz-Ramírez, J.A.; Olarte-Arias, Y.A.; Glasserman-Morales, L.D. Educational Processes for Health and Disease Self-Management in Public Health: A Systematic Review. Int. J. Environ. Res. Public Health 2021, 18, 6448.
2. Martínez-Riera, J.R.; Aviles Gonzalez, C.I.; Zambrano Bermeo, R.N.; Curcio, F.; González Correa, J.A.; Estrada González, C.; Melo, P.; Galletta, M. Educational Strategies to Promote Adherence to Treatment in Patients with Cardiovascular Disease. Int. J. Environ. Res. Public Health 2022, 19, 9841.
3. Correa Tello, K. Diseño y validación de material para una intervención educativa en pacientes con implante de Stent coronario. Perspect. Educ. 2014, 7, 159–170.
4. Herrera Guerra, E.P.; Céspedes Cuevas, V.M. Design and validation of educational material aimed at adults with Heart Failure. Rev. Cienc. Cuidad. 2020, 17, 31–42.
5. Paradis, V.; Cossette, S.; Frasure Smith, N.; Heppell, S.; Guertin, M.C. The efficacy of a motivational nurs- ing intervention based on the stages of change on self-care in heart failure patients. J. Cardiovasc. Nurs. 2020, 25, 130–141.
6. De Ridder, D.; Kroese, F.; Evers, C.; Adriaanse, M.; Gillebaart, M. Healthy diet: Health impact, prevalence, correlates, and interventions. Psychol. Health 2017, 32, 907–941.
7. Zhao, X.; Yu, X.; Zhang, X. The Role of Peer Support Education Model in Management of Glucose and Lipid Levels in Patients with Type 2 Diabetes Mellitus in Chinese Adults. J. Diabetes Res. 2019, 1, 134.
8. Gagliardino, J.J.; Chantelot, J.M.; Domenger, C.; Ramachandran, A.; Kaddaha, G.; Mbanya, J.C.; Shestakova, M.; Chan, J.; IDMPS Steering Committee. Impact of diabetes education and self-management on the quality of care for people with type 1 diabetes mellitus in the Middle East (the International Diabetes Mellitus Practices Study, IDMPS). Diabetes Res. Clin. Pr. 2019, 147, 29–36.
9. Ji, H.; Chen, R.; Huang, Y.; Li, W.; Shi, C.; Zhou, J. Effect of simulation education and case management on glycemic control in type 2 diabetes. Diabetes Metab. Res. Rev. 2019, 3, 35.
10. Manigault, K.R.; Augustine, J.M.; Thurston, M.M. Impact of Student Pharmacists Teaching a Diabetes Self-Management Education and Support Class. Am. J. Pharm. Educ. 2020, 3, 84–90.
11. Carmienke, S.; Baumert, J.; Gabrys, L.; Heise, M.; Frese, T.; Heidemann, C. Participation in structured diabetes mellitus self-management education program and association with lifestyle behavior: Results from a population-based study. BMJ Open Diabetes Res. Care 2020, 8, e001066.
12. Kennedy, L.E.; Hosig, K.L.; Ju, Y.; Serrano, E.L. Evaluation of a mindfulness-based stress management and nutrition education program for mothers. Cogent Soc. Sci. 2019, 5, 1682928
13. Pozza, A.; Osborne, R.H.; Elsworth, G.R.; Gualtieri, G.; Ferretti, F.; Coluccia, A. Evaluation of the Health Education Impact Questionnaire (heiQ), a Self-Management Skill Assessment Tool, in Italian Chronic Patients. Psychol. Res. Behav. Manag. 2020, 13, 459–471.
14. Chang, Y.-Y.; Dai, Y.-T. The efficacy of a flipping education program on improving self-management in patients with chronic obstructive pulmonary disease: A randomized controlled trial. Int. J. Chron. Obs. Pulmon. Dis. 2019, 14, 1239–1250.
15. Davies, M.J.; Kristunas, C.A.; Alshreef, A.; Dixon, S.; Eborall, H.; Glab, A. The impact of an intervention to increase uptake to structured self-management education for people with type 2 diabetes mellitus in primary care (the embedding package), compared to usual care, on glycaemic control: Study protocol for a mixed-methods study. BMC Fam. Pr. 2019, 20, 1–15.
16. Preechasuk, L.; Sriussadaporn, P.; Likitmaskul, S. The obstacles to diabetes self-management education and support from healthcare professionals’ perspectives: A nationwide survey. Diabetes Metab. Syndr. Obes. Targets 2019, 12, 717–727.
FINANCING
None.
CONFLICT OF INTEREST
None.
AUTHORSHIP CONTRIBUTION
Conceptualization: Roshni Majumder, Samir Sahu, Manashree Mane, Sarika R. Sikchi.
Investigation: Roshni Majumder, Samir Sahu, Manashree Mane, Sarika R. Sikchi.
Methodology: Roshni Majumder, Samir Sahu, Manashree Mane, Sarika R. Sikchi.
Writing - original draft: Roshni Majumder, Samir Sahu, Manashree Mane, Sarika R. Sikchi.
Writing - review and editing: Roshni Majumder, Samir Sahu, Manashree Mane, Sarika R. Sikchi.