doi: 10.56294/hl2023300
ORIGINAL
Occupational Safety and Health Evaluations in Emergency Medical Response Services
Evaluaciones de seguridad y salud en el trabajo en los servicios de respuesta médica urgente
Jamuna KV1 ![]() , Varun kumar Sharma2
, Varun kumar Sharma2 ![]() , Abhinov Thamminaina3
, Abhinov Thamminaina3 ![]() , Udaybhanu Rout4
, Udaybhanu Rout4 ![]()
1JAIN (Deemed-to-be University), Department of Forensic Science. Bangalore, Karnataka, India.
2Noida International University, Department of Biotechnology and Microbiology. Greater Noida, Uttar Pradesh, India.
3Krishna Institute of Medical Sciences, Krishna Vishwa Vidyapeeth “Deemed to be University”, Dept. of Emergency Medicine. Taluka-Karad, Dist-Satara, Maharashtra, India.
4IMS and SUM Hospital, Siksha ‘O’ Anusandhan (Deemed to be University), Department of General Medicine. Bhubaneswar, Odisha, India.
Cite as: KV J, kumar Sharma V, Thamminaina A, Rout U. Occupational Safety and Health Evaluations in Emergency Medical Response Services. Health Leadership and Quality of Life. 2023; 2:300. https://doi.org/10.56294/hl2023300
Submitted: 27-05-2023 Revised: 28-08-2023 Accepted: 06-11-2023 Published: 07-11-2023
Editor:
PhD.
Prof. Neela Satheesh ![]()
ABSTRACT
Saving lives in an emergency depends much on Emergency medical response services (EMRS). These offerings, but, function in dangerous places wherein rescue professionals run several dangers during their employment. The number one goal of this take a look at is to investigate the occupational safety and health (OSH) rules of emergency scientific response services in order to become aware of risks, assess present safety measures, and propose way of creating them more secure and healthier for workers. Closely analysing modern safety policies, risk elements, and incident reports enabled one to decide how well they averted mistakes and accidents. Questionnaires and interviews with emergency clinical experts also were used to examine extra about their reports, protection issues, and challenges they’ve seeking to preserve themselves secure while administering care below quite a few stress. The results expose numerous important risk factors: physical stress, infectious diseases, toxic chemicals, and mental health problems including post-traumatic stress disorder (PTSD). Many emergency responders lack the required tools, training, and support systems; hence even although their jobs are quite important, many of them are not suited for these threats. The study stresses the need of a comprehensive OSH system involving not only physical safety precautions but also mental health help to empower people and improve their general well-being. Among the several key recommendations are to upgrade training courses, provide modern safety gear to employees, provide mental health tools, and promote a culture of safety whereby everyone participates in risk management strategies. By demonstrating how better Occupational Safety and Health (OSH) procedures may make responders safer, reduce accidents at work, and finally enhance the quality of emergency medical treatment for everyone, this study advances our knowledge of emergency medical services. These findings indicate a consistent strategy for safety that takes mental health into account in addition to physical one. This would increase the productivity and safety in the workplace.
Keywords: Emergency Medical Response Services; Occupational Safety and Health; Risk Assessment; Emergency Responders; Mental Health Support; Protective Equipment.
RESUMEN
Salvar vidas en caso de emergencia depende en gran medida de los Servicios de Respuesta Médica Urgente (SAMU). Sin embargo, estos servicios funcionan en lugares peligrosos donde los profesionales de rescate corren varios peligros durante su trabajo. El objetivo principal de este estudio es investigar las normas de seguridad y salud en el trabajo (SST) de los servicios de respuesta científica de emergencia para conocer los riesgos, evaluar las medidas de seguridad actuales y proponer formas de hacerlos más seguros y saludables para los trabajadores. Analizar de cerca las modernas políticas de seguridad, los elementos de riesgo y los informes de incidentes permitió decidir hasta qué punto evitaban errores y accidentes. También se utilizaron cuestionarios y entrevistas con expertos clínicos en emergencias para examinar más a fondo sus informes, problemas de protección y retos que han buscado para preservarse seguros mientras administran cuidados bajo bastante estrés. Los resultados exponen numerosos factores de riesgo importantes: estrés físico, enfermedades infecciosas, sustancias químicas tóxicas y problemas de salud mental, incluido el trastorno de estrés postraumático (TEPT). Muchos socorristas carecen de las herramientas, la formación y los sistemas de apoyo necesarios; de ahí que, aunque su trabajo sea bastante importante, muchos de ellos no estén preparados para estas amenazas. El estudio subraya la necesidad de un sistema global de SST que incluya no sólo precauciones de seguridad física, sino también ayuda a la salud mental para capacitar a las personas y mejorar su bienestar general. Entre las principales recomendaciones figuran la mejora de los cursos de formación, el suministro de equipos de seguridad modernos a los empleados, la provisión de herramientas de salud mental y el fomento de una cultura de la seguridad en la que todos participen en las estrategias de gestión de riesgos. Al demostrar cómo la mejora de los procedimientos de seguridad y salud en el trabajo (SST) puede aumentar la seguridad de los socorristas, reducir los accidentes laborales y, por último, mejorar la calidad del tratamiento médico de urgencia para todos, este estudio hace avanzar nuestros conocimientos sobre los servicios médicos de urgencia. Estos resultados indican una estrategia coherente para la seguridad que tiene en cuenta la salud mental además de la física. Esto aumentaría la productividad y la seguridad en el lugar de trabajo.
Palabras clave: Servicios de respuesta Médica de Emergencia; Seguridad y Salud en el Trabajo; Evaluación de Riesgos; Personal de Respuesta a Emergencias; Apoyo a la Salud Mental; Equipos de Protección.
INTRODUCTION
Getting medical assistance immediately in wrecks, natural catastrophes, and other events depends critically on Emergency Medical Response Services (EMRS). Since these services are usually the first line of protection for people in risky circumstances, emergency responders are quite important in saving lives. Still, emergency medical personnel participate in basically dangerous operations that expose them to some occupational dangers. From physical accidents and contagious illnesses to intellectual strain and emotional ache, these workers cowl a large spectrum of dangers. for that reason, not only for the health of the rescuers but additionally for the short and powerful care given to people in emergencies, EMRS's occupational safety and health (OSH) regulations are specifically important. Even though their work is somewhat dangerous, emergency responders every so often take good sized dangers on the job. These contain bodily accidents from lifting and moving sufferers, touch with risky substances, vehicle accidents at the same time as patient transportation, and the likelihood of infectious illnesses transmission. Worrying activities also often affect people's emotional and mental health; times of such events encompass the probability of acquiring mental illnesses like PTSD and burnout. Those health and protection risks can significantly impact first responders' intellectual and bodily well-being, in an effort to abate their ability to carry out their duties. Sturdy OSH policies guarantee that workers of emergency medical offerings are safe as their activities are quite essential. While technologies, schooling, and laws help to enhance protection, there are still considerable flaws within the manner effective OSH systems are completed regardless of a whole lot attempt. Even as more people understand how essential OSH is to emergency medical offerings, extra has nevertheless to be executed to guarantee rescuers' safety and fitness.
Loss of mental health treatment, insufficient schooling, and insufficient protection equipment are a number of the maximum frequently cited problems alleged to raise the susceptibility of those individuals. Emergency scientific services need to take mental in addition to bodily factors into account after they evaluate protection on the administrative center. ensuring people continue to be wholesome in the main depends on bodily protection measures such setting regulations for handling risky merchandise, teaching emergency responders how to thoroughly treat sufferers, and giving them PPE to wear. But it's become more and clearer over the past several years how important it is to manage mental health issues among emergency response team members. Over time, the emotional toll of negotiating challenging situations and the ongoing pressure to perform effectively in stressful conditions can affect responders' mental health. According to others, this is the reason OSH models ought to include mental health support and resilience building techniques.(1) First responders will therefore be able to control the mental as well as the physical risks associated to their employment. This research intends to highlight shortcomings in the current safety rules, look at how OSH is presently used in emergency medical services, and suggest changes that would make staff members safer and healthier. Analysing psychological as well as physical risks allows this study to show the entire picture of the problems emergency medical practitioners handle and suggest ways to lower such risks. This study further underlines the requirement of EMRS adopting a safety approach that gives patients first priority but first considers the wellbeing and health of rescuers. The results of this study will result in better OSH rules and procedures, therefore safeguarding and supporting emergency responders in their quite important tasks.
Definition and significance of occupational safety and health (OSH)
Making sure individuals are safe, healthy, and happy at work falls to the field of occupational safety and health (OSH). Finding, assessing, and managing hazards that can endanger employees is the primary focus of this company so as to prevent mishaps, injuries, and diseases. Risk assessments, safety guidelines, personal protective equipment (PPE), and health management systems keeping workers safe from physical, chemical, biological, mechanical, and psychological hazards are among the many topics OSH covers. OSH is so crucial for maintaining workers healthy and effective, hence you cannot say enough positive things about it. OSH helps prevent workers from being sick or injured, thereby reducing absenteeism, increasing production, and generally happier workers. Moreover, a well-run OSH program guarantees the adherence to rules.(2) For companies, this reduces their legal risk including fines. In high-risk industries such building, healthcare, and emergency response to ensure workers are not only physically safe but also psychologically well, OSH techniques are even more crucial. By increasing understanding and encouraging employees to be accountable for their own health and safety, OSH also helps businesses build a culture of safety. Good OSH initiatives emphasise continuous education and training to enable employees to identify hazards and act to safeguard themselves.
Overview of emergency medical response services (EMRS)
Emergency Medical Reaction Services (EMRs) are several forms of treatment rendered in response to urgent medical conditions. The aim is to immediately provide medical attention to those requiring quick treatment. These services cover a lot of different tasks, like calling for an aid in an emergency, caring for patients on-site, and coordinating with other medical facilities for further care. EMRS workers, like paramedics, emergency medical techs (EMTs), and other health care professionals, have to deal with a lot of stress while evaluating and handling life-threatening situations.
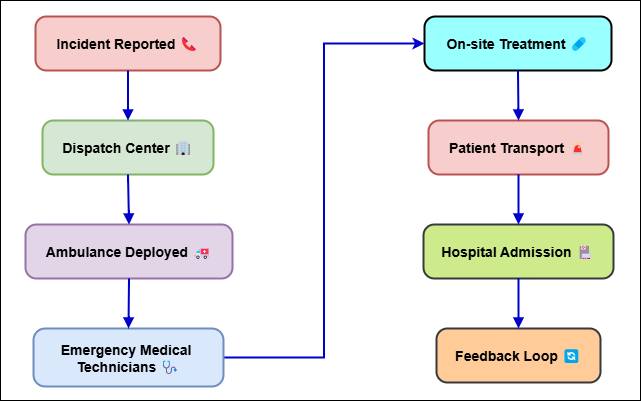
Figure 1. Overview of Emergency Medical Response Services (EMRS)
They make decisions that can have a big effect on a patient's ability to survive and recover. Figure 1 shows an overview of Emergency Medical Response Services, focussing on the most important parts and steps that are involved. The main goal of EMRS is to get people quickly and professionally medical help when they need it, like in an accident, after being hurt, having a heart attack, a stroke, or another serious condition. EMRS usually work with a variety of transport methods, such as ground-based ambulances, air medical services, and other specialised emergency units.(3) The success of these services depends on medical treatments being carried out quickly and correctly, on people working together well, and on being able to change to situations that are hard to predict and often chaotic. At EMRS, the job atmosphere is often hard on the body, stressful on the mind, and full of dangers. Responders to emergencies often have to deal with difficult situations while staying calm and focused.
Importance of OSH evaluations in EMRS
Occupational Safety and Health (OSH) studies are rather crucial for Emergency Medical Response Services (EMRs) as they assist in identifying, assessing, and lowering of the hazards that emergency personnel encounter on their employment. Since emergency medical operations are erratic and dangerous, OSH examinations are fairly important to guarantee that rescuers' mental and physical condition stays intact. Improving emergency treatment depends on OSH evaluations in great measure. By safeguarding first responders' health and safety, indirectly these reviews enable patients receive better treatment. If responders have the correct equipment, are well taught, and receive support in their physical and mental health, they are more likely to perform their responsibilities successfully and fast.(4) In an emergency, this immediately influences the speed and quality of medical assistance provided, which is really crucial. In addition, OSH reviews help EMRS organisations develop a culture of safety by encouraging constant growth and the ongoing evaluation of safety practices. Evaluations done on a regular basis help find holes in safety rules, training programs, or tools, which opens the door to improvements and changes. These reviews also make emergency medical staff more aware of how important safety is, which motivates them to take an active part in their own health.
Occupational hazards in emergency medical response services
Physical hazards
Injuries during patient handling
When working in Emergency Medical Response Services (EMRS), one of the biggest physical risks is that someone could get hurt while handling a patient. People who work in emergency medical services often have to lift, carry, and move people, sometimes in difficult or dangerous situations. Responders may have to lift and move patients who are asleep, in pain, or in critical condition while moving them, which can be hard to do in tight areas or odd situations. Musculoskeletal injuries, such as back strains, sprains, and injuries to the shoulders, knees, and arms, can happen when you have to handle patients. These kinds of accidents happen a lot in emergency situations where people have to move quickly and sometimes forcefully, and there isn't time for them to use the right moving methods.(5) A lot of the time, rescue workers have to lift people who are big or can't help with their own transfer, which puts a lot of stress on their bodies. Injuries to the muscles and bones are possible, but treating patients all the time can also cause repeated strain injuries. Because of the nature of their job, rescuers have to regularly lift and carry things, which can cause long-term damage to the body. These injuries can be very bad and make it hard for the rescuer to do their job. They can also be bad for their health and well-being in general. For EMRS organisations to lower the risk of injuries while treating patients, they need to teach workers the right way to lift things safely, use mechanical tools like stretchers and hoists, and use equipment that is meant to be easy on the body.(6) To avoid accidents, it is also important to promote a culture of safety and encourage first responders to get help when they are dealing with patients in tough conditions.
Exposure to hazardous environments
Responders to emergencies are also at risk of getting hurt because they are often in dangerous places. These risks can include being exposed to chemicals and harmful substances or being in a place that is physically unsafe and makes getting hurt or sick more likely. A lot of the time, emergency medical workers are called to the scene of accidents, natural disasters, or industrial accidents. There, they are exposed to dangerous materials like biological agents, radioactive materials, and harmful chemicals. In these scenarios, first responders may breathe in or come into touch with dangerous substances, which could cause poisons, chemical burns, breathing problems, or long-term health problems. Apart from the chemical risks, first responders may also come into harmful physical surroundings.(7) Among other things, responders risk the hazard of unstable buildings, falling objects, fires, and blasts during automobile accidents, fire rescues, and natural disasters. From these physical threats, major injuries like wounds, burns, fractured bones, and brain traumas can follow. In these high-risk situations, it is challenging to guarantee that both rescuers and patients are safe; yet, rescuers have to be quick and careful. Table 1 in Emergency Medical Response Services provides a synopsis of the approaches, formulae, challenges, and spectrum of work-related hazards.
|
Table 1. Summary of Occupational Hazards in Emergency Medical Response Services |
|||
|
Method |
Algorithm |
Challenges |
Scope |
|
Risk Assessment |
Risk Matrix |
Inaccurate Data Reporting |
Risk Mitigation Strategies |
|
Safety Protocols |
Safety Checklists |
Resistance to Protocols |
Standardizing Safety Measures |
|
Safety Audits |
Audit Tools |
Resource Limitations |
Improving Compliance |
|
Incident Reporting(8) |
Incident Log Analysis |
Underreporting of Injuries |
Enhancing Incident Transparency |
|
Health Surveillance |
Health Monitoring Algorithms |
Lack of Consistency |
Tracking Employee Health |
|
Training Programs |
Training Effectiveness Evaluation |
Insufficient Funding |
Evaluating Training Outcomes |
|
Risk Management |
Hazard Identification Algorithms |
Low Compliance |
Effective Hazard Control |
|
Safety Monitoring |
Real-Time Monitoring Systems |
Lack of Real-Time Feedback |
Real-Time Risk Management |
|
Statistical Analysis(9) |
Predictive Analytics |
Limited Data Access |
Data-Driven Decision Making |
|
Quality Improvement |
Continuous Improvement Models |
Slow Process Adoption |
Continuous Improvement in Safety |
|
Health Screening |
Health Data Algorithms |
Inadequate Monitoring Tools |
Health Risk Monitoring |
|
Personal Protective Equipment |
PPE Compliance Checks |
Stigma Around Mental Health |
Ensuring PPE Compliance |
|
Mental Health Support |
Psychological Risk Assessments |
Unpredictable Work Environments |
Mental Health Resilience |
|
Post-Incident Evaluation(10) |
Incident Debriefing Systems |
Limited Risk Assessment Models |
Post-Incident Analysis and Improvement |
Chemical hazards
Exposure to infectious diseases
One of the main chemical hazards for Emergency Medical Response System (EMRS) workers is acquiring fatal infections. First responders frequently interact closely with unwell individuals who could be carriers of contagious diseases. Among these illnesses, many can be transmitted via blood, bodily fluids, breathing droplets, and other means. Even if they lack medical knowledge or if they have an illness that might be transmitted, those in emergency response have to treat patients immediately. This lack of trust increases the risk of disseminating HIV, Hepatitis B and C, TB, numerous lung illnesses including COVID-19 and the flu. Treating open incisions, doing CPR, or handling bodily fluids exposes responders to dangerous illnesses. When handling contaminated needles or medical equipment, those reacting to an emergency might get needle-stick injuries. In an emergency when individuals have to move fast and lack time to consider what is happening, these hazards are more present. They may so follow incorrect safety precautions. Therefore, persons in the medical field—including those in EMRS—are more prone to acquire infections that could have significant long-term consequences for their health.(11) EMRS groups must teach complete infection control techniques, including how to wear personal protective equipment (PPE) such masks, gloves, eye protection, and gowns appropriately, if they are to reduce the likelihood of infectious illnesses. Vaccines against infections like flu and Hepatitis B can also help responders have even less likelihood.
Hazardous substances in the emergency environment
One of the main chemical hazards emergency medical personnel face is environmental exposure to harmful compounds. Those reacting to natural catastrophes, accidents, toxic material spills, or occupational mishaps might come across these harmful compounds. First responders in these situations may come into contact with harmful biological materials, liquids, chemicals, or pesticides and industrial compounds. For first responders who come into touch with chemicals, burns, toxins, respiratory issues, or long-term diseases like cancer can develop immediately. First responders who must operate in tiny or unclean environments such as those involved in an accident at a chemical factory, a vehicle wreck involving dangerous items, or a fire rescue in an industrial area should especially be concerned about exposure to harmful chemicals.(12) First responders may consume or drink contaminated food or water, breathe in hazardous fumes, come into touch with deadly substances on their skin or eyes, or contact these sites. Long-term health impacts are conceivable, particularly in cases of repeated exposure or long-term interaction that spans many years. To handle the hazards associated with hazardous chemicals, EMRS organisations must ensure that rescuers possess the appropriate personal safety gear (PPE), including respirators, gloves, masks, and chemical-resistant suits, gloves, Responders also have to pick up the ability to identify dangers and apply certain safety guidelines pertaining to hazardous chemicals. This provide them the information to determine whether the setting is safe and what to do next. This entails understanding the Material Safety Data Sheets (MSDS) for the chemicals being used and how to properly evacuate the facility should an accident involving hazardous compounds arise.
Psychological hazards
Stress and mental health risks
Because emergency work is so fast-paced and stressful, you have to make decisions all the time, respond quickly, and be able to handle difficult situations. These things that cause stress can build up over time and lead to mental health problems like PTSD, anxiety, sadness, and burnout. Responders often feel emotionally drained after dealing with seriously hurt or dying patients, seeing traumatic events, and giving life-saving care in tough situations. Feeling like they have to perform at their best all the time can be mentally draining, and many first responders have trouble with the stress of having to make life-or-death choices.(13) Also, emergency medical workers often have to work long hours in tough conditions, which can make them even more stressed and make them tired, irritable, and less satisfied with their job. The mental health risks in EMRS are made worse by the fact that mental health problems are often looked down upon in emergency service jobs. Because they think they need to be strong or tough all the time, many users may feel like they need to hide their feelings and not get help. People who don't want to get help may not get treatment for mental health problems, which can affect their daily lives, work success, and general health.(14) To deal with these mental risks, EMRS groups need to make mental health support a priority by giving rescuers stress management training, counselling services, and other mental health tools. It is very important to make the workplace a safe place where people can talk about their mental health problems. Access to professional psychological support and regular check-ins on mental health can help lessen the long-term effects of stress and improve the health of first responders.
Trauma and emotional strain
Responders to emergencies are exposed to major psychological risks because of the stress and pain they go through on the job. Responders often see things that change people's lives, like serious injuries, deaths, and violent situations, which can leave mental scars that last a lifetime. Psychological disorders like PTSD, ASD, and sadness can develop in people who are frequently exposed to traumatic events, especially when they are unable to save a patient or when they see upsetting scenes. These mental health issues can make it rather difficult for the rescuer to perform their duties and, if improperly addressed, can lead to long-lasting emotional problems. Trauma and mental stress can present itself in EMRs in several ways. Responders may find it difficult to manage their emotions, which would increase their tension, anxiety, and emotional tiredness; they may also have troubling thoughts, flashbacks, and nightmares about horrible incidents. These emotional obligations can build up over time and cause burnout, a disorder distinguished by emotional tiredness, reduced empathy, and a disconnection with both patients and colleagues.(15) Trauma can directly affect the mental health of the responder; but, it can also affect their relationships and capacity for social functioning. Respondents may feel alone if they find it difficult to share with relatives and friends their experiences. Dealing with difficulties under such high strain may make it more difficult for individuals, which can cause a loop of negative conduct impacting personal life as well as business. EMRS groups have to provide trauma-informed treatment and mental health assistance if they are to assist rescuers cope with the emotional strain of trauma.(16)
Legal and Regulatory Framework
National and international regulations
International institutions such as the World Health Organisation (WHO) and the International Labour Organisation (ILO) have developed guidelines and rules for workplace safety especially with reference to places where emergency medical treatment is given. For example, the ILO's Occupational Safety and Health Convention helps us to make workplaces safer and healthier as well as lowers health and safety risks in high-risk sectors such emergency services. Furthermore established globally by the WHO are recommendations for emergency medical care These rules provide direction on how to protect first responders from psychological as well as physical threats. International regulations highlight the need of standard emergency medical care and protection for first responders, hence safety guidelines have to be consistent and may be applied anywhere. These global standards are used by many EHRs to develop comprehensive safety plans compliant with best standards globally. Still, trying to make safety precautions the same everywhere might be difficult since every country has distinct regulations, resources, and degree of medical facilities. If nations seek to increase occupational safety and health (OSH) for first responders, they must collaborate and follow national as well as international policies. By ensuring their rules follow these criteria, EMRS groups may improve the health of first responders, make workplaces safer, and international emergency care quality higher.(17)
Compliance challenges in EMRS
Following occupational safety and health (OSH) rules gives great difficulties for Emergency medical response services (EMRS). Protection guidelines is probably challenging to assure that they may be followed as individuals involved in emergency medical treatment are commonly uncovered to many one-of-a-kind varieties of physical, chemical, and psychological risks and the paintings is typically risky. One of the key issues is that fast shifting emergency occurrences are unpredictable. Many unique fields allow one predict and control dangers. On the other hand, matters exchange speedy and emergency responders should be flexible and geared up to make decisions. Consistent looking at safety policies will become difficult as a result. Any other problem is many EHRs missing enough sources. Small or impoverished organisations would possibly conflict to locate the employees, tools, and schooling needed to meet criminal standards. Following the rules might be harder without enough access to modern-day protection manner schooling, PPE, or easy rooms. Logistically, rescue people can also locate it difficult to reach websites with dangerous chemical compounds or inadequate construction conditions from not being allowed to enter protected regions. These troubles complicate the complete commentary of safety policies within the actual global of operations. Moreover, first responders' emotional condition is an vital but frequently ignored aspect of compliance. While most policies cope with physical risks, intellectual fitness is just as critical.(18)
Risk assessment and mitigation strategies
Implementing control measures
Personal protective equipment (PPE)
Personal safety equipment (PPE) determines much of the lowering of dangers in Emergency Medical Response Services (EMRS). For emergency responders who come into physical, chemical, and biological threats that can cause them injury or expose them to dangerous chemicals, PPE is an absolutely vital layer of protection. Among the various instruments PPE employs are masks, gloves, gowns, goggles, caps, and covered shoes. Its aim is to protect first responders from diseases, dangerous substances, and physical injuries. Regularly running into poisons, bloodborne infections, and infectious diseases are medical emergency responders. Their using the right PPE is highly important. Gloves assist you avoid having body fluids on your hands; masks and face shields stop you from taking in germs in the air or splashing bodily fluids on your face. Full-body protective suits and respirators are advised at more dangerous sites, including chemical spills or fire escapes, to guard against dangerous chemicals and harsh weather conditions. Proper PPE usage is essential vital as neglecting to wear it or use it incorrectly might expose first responders to diseases or injuries. EMRs have to ensure sure their employees know how to properly wear, maintain, and discard PPE. Maintaining operating condition requires routinely inspected and replaced aged equipment. Making ensuring first responders have the right PPE and know how to utilize it helps to lower their chemical and physical exposure.(19)
Training and education programs
Key strategies in Emergency medical reaction services (EMRS) to resource to reduce dangers encompass education and training. Comprehensive education offers first responders the records and sources they need to spot risks, paintings effectively in excessive-hazard regions, and properly manage occasions. Schooling guides need to consist of a huge spectrum of subjects considering the superb variety of hazards. Amongst these consist of safe patient managing practices, contamination prevention regulations, dealing with of dangerous objects, intellectual fitness resilience improvement, accurate PPE usage, ordinary training for responders will enable them to keep contemporary on protection rules and growing risks. There can be school room schooling as well as practical training consisting of position-playing real-existence incidents in order that rescuers may improve their abilities in managed surroundings. Simulated training activities and actual application of safety rules help responders learn how to manage hazardous events including chemical spills, wound care, or natural disasters under calm under pressure. More than just technical and procedural training should be included into the curriculum to help emergency responders manage their mental health problems. It should also have social and psychological instruction. Teaching individuals stress management techniques, problem-solving strategies, and burnout or PTSD awareness will help to prevent long-term mental damage.
Importance of safety protocols and emergency response procedures
Maintaining first responders' safety and reducing the hazards depend much on safety guidelines and emergency reaction techniques. These rules help first responders go through the actions they must take to maintain personal safety, prevent mishaps, and properly manage crises. Not enough can be said about the significance of consistent, well defined procedures. They offer structure and direction especially in rural places where first responders have to act quickly. Safety measures usually encompass rules for patient management, PPE use, cleaning, handling of dangerous materials, and tool use. They also go on risk assessment techniques for recognizing and handling dangerous sites or situations that can compromise rescuers. These guidelines are meant to provide rescuers exact, systematic directions that minimize mistakes and ensure continuous adherence to safety standards. Since they allow people to react quickly and aggressively under extreme stress, emergency reaction procedures are also highly important. These protocols specify who is in charge of what, how to interact, and what to do in particular types of crises include natural catastrophes, mass mortality events, or spills of dangerous chemicals. By helping EMRs to better organize their operations, following these rules allows them to usually lower misunderstanding and speed reaction times.(20)
Best practices and guidelines
Safety standards for emergency medical technicians (EMTs)
protection standards for Emergency medical Technicians (EMTs) significantly have an effect on whether rescuers live healthy as they store lives. in view that emergency medical work is so dangerous, EMTs need to comply with regulations supposed to protect them from being too uncovered to bodily, chemical, and mental threats. Most of the matters these protection regulations cowl are intellectual health guide networks, safe techniques of affected person care, and personal protective equipment (PPE). One of the most critical safety regulations reachable to EMTs is correct PPE use. As part of their paintings, EMTs every now and then come into contact with germs carried by using blood, infectious diseases, and dangerous materials. To decrease their threat of ailment or harm, OSHA rules insist that humans don gloves, mask, face shields, robes, and other defensive gear. To ensure they may be absolutely prepared to guard themselves in a spread of emergency occasions, EMTs should receive appropriate schooling on the way to use PPE. Apart from non-public protecting tools, safety rules stress suitable strategies of affected person care and mobility. EMTs may additionally locate it hard every so often to raise and move a person. If EMTs need to keep away from joint injuries, they have to research proper lifting strategies and a way to run gadgets like stretchers and motorized lifts. This lowers the probability of sprains, lower back pain, and different injuries resulting from incorrect object coping with returning. Concerning emergency response, intellectual fitness criteria also are underneath increasingly more importance. EMTs may additionally need to cope with difficult conditions that would motive mental stress, burnout, and anxiety. Amongst other matters EMTs acquire now are intellectual health schooling, pressure management strategies, and organization support networks below protection recommendations. If mental health remedy is integrated into safety tactics, EMTs are extra suitable to control the emotional challenges that accompany assisting others in an emergency. These strategies are designed to assist people cope with the emotional toll their task requires.
Occupational health surveillance and monitoring systems
Occupational fitness monitoring and monitoring systems are key elements of an Emergency clinical reaction services (EMRS) protection plan that features. Protection policies are so discovered and any fitness troubles are probably discovered early on. Frequent observation and shrivelling EMRS organizations allows them to screen activities, check dangers, and follow appropriate action to make responders more secure. Occupational fitness tracking relies upon significantly on everyday assessments of the dangers to one's bodily health. Most of the numerous risks first responders encounter are the ones of injury, chemical exposure, and deadly sicknesses. This allows one to identify early on trends or patterns pointing to new dangers. This fact allows humans decide what adjustments ought to be achieved to PPE desires, education packages, and safety guidelines. Working fitness tracking in EMRS is together with mental health surveillance ever extra gradually. Given their line of operation, first responders are more likely to experience stress, trauma, and mental fitness troubles like PTSD, anxiety, and depression. Regular psychological assessments, pressure surveys, and treatment is probably a part of intellectual health tracking structures in search of for symptoms of emotional strain or burnout. Early intervention guarantees rescues get hold of the necessary therapy and enables decrease the long-term effects of certain mental health issues. Occupational health monitoring systems may also possibly include clinical checking out, immunizations, and screenings to identify diseases like Hepatitis B and TB, which can be common in places in which people react to crises. Frequent fitness tests permit responders to lower their health risks and enhance their overall performance in their jobs.
Challenges in OSH evaluation in EMRS
Lack of resources and funding for safety initiatives
Smaller EMRs or those without enough money might find it difficult to pay to commit finances into comprehensive safety measures like contemporary personal protective equipment (PPE), health monitoring systems, and safety training courses. EHRs may not be able to meet regulatory criteria, have the newest safety equipment, or routinely educate their staff if they lack the money. Safety programs are frequently seen as less important than emergency medical treatment; hence they receive hardly enough attention. Thus, first responders might have to use obsolete or inadequate tools, which raise their psychological and physical risks. For example, rescuers may develop joint injuries or infectious diseases if they lack the right PPE or safe devices for patient treatment. Long term, this might affect their health. Lack of resources might also hinder responders from obtaining enough mental health assistance, therefore raising their sensitivity to burnout, stress, and trauma. Dealing with this problem needs for a range of different initiatives, including getting enough money from government organizations, private groups, or public health campaigns. Furthermore, EMRS companies should prioritize safety highly and support the allocation of funds designated specifically to improve worker safety. Businesses can not only satisfy legal obligations but also make their operations more efficient, reduce absenteeism, and raise the general quality of patient treatment by investing money into the health and safety of first responders.
Resistance to safety measures and protocols
Evaluating OSH in Emergency Medical Response Services (EMRS) is hampered greatly by people's non-always following of safety guidelines and policies. Although safety precautions are obviously beneficial, some emergency responders and even organizational bosses might not wish to embrace them. Particularly in the hectic field of emergency medicine, this opposition might originate from a variety of factors, including the conviction that safety regulations are overly complex, take too much time, or are not necessary. Some first responders could believe that safety regulations impede their capacity to rapidly and successfully manage events and are thus overly rigid. This pushback could also be caused by the way the company works, where safety is not a top concern. Some EMRS groups may have a way of thinking that puts quick response times and professional care ahead of safety rules. This can make it hard for both staff and managers to agree with the rules. Because of this "culture of urgency," safety rules are often forgotten or not followed, especially when time is of the essence and decisions need to be made quickly. EMRS organizations need to create a mindset of safety in order to get past this pushback. Leaders should work with their employees to explain why safety measures are important and make sure that rules are useful and completely built into daily work. Training programs that stress how safety improves the results for both responders and patients can help change people's minds about following the rules. Having staff members help create and review safety protocols can also make them feel more responsible and like they own them, which can make them less resistant to following safety rules. Over time, pushback can be reduced as safety measures become part of the organization's mindset. This makes the emergency response system safer and more effective.
Underreporting of workplace injuries and health issues
An important problem in Emergency Medical Response Services (EMRS) is that accidents and health problems at work are often not reported properly. This makes it hard to do an effective Occupational Safety and Health (OSH) assessment. Many emergency responders might not disclose injuries or health issues because they are anxious about their job stability, they are fearful of what will happen, or they believe the damage is little enough to require no treatment. Underreporting might imply that EMRS agencies lack sufficient reliable data to determine the actual size of the genuine safety hazards and appropriate course of action for their correction. There are several reasons behind underreporting of health issues and accident occurrence. First, emergency responders might believe they have to be physically strong and fit in a performance environment. This might cause individuals to hide or minimize injuries so they don't seem to be unable of doing their tasks. Second, there is guilt about mental health inside the emergency services. If rescuers discuss mental stress, anxiety, or trauma, many of them fear being regarded as weak or stigmatised. Mental health issues include PTSD, depression, and exhaustion not managed and worsens with time. If EMRS groups are to address this problem, they must establish a conducive atmosphere whereby revealing mistakes and health concerns is valued and encouraged. This means building tools for people to document occurrences without revealing their names, making sure those who report events won't face consequences, and creating a work environment that supports first responder health and safety. Regular health checks, psychological evaluations, and feedback sessions can also help identify health problems not being reported and motivate rescuers to get treatment following catastrophic events. Removing the obstacles that stop EMRS staff members from reporting allows others to better grasp the health and safety concerns their team comes across. From this, better safety measures and general enhanced therapy ensue.
Case studies and research findings
Successful OSH programs in EMRS
Many great Occupational Safety and Health (OSH) projects in Emergency Medical Response Services (EMRS) have shown the significance of following all safety precautions for the benefit of the health of emergency workers. One example of this is the "Safe Patient Handling" system being used by several big EMRs. One of the most regularly occurring health problems in the field, joint injuries may be minimised using the mechanical lifts, stretchers, and other helpful tools provided by EMTs and paramedics. These tools not only help to relieve physical strain on the body but also guarantee safer patient transportation, therefore lowering the risk of injury to either patients or rescuers. Apart from offering suitable instruments, these programs provide thorough training in proper lifting techniques and safe processes, therefore lowering the frequency of injuries even in connection to tools. Establishing mental health support services is another remarkable OSH endeavour. As more people become aware of the psychological risks linked with working in emergency medical services, groups like the New York Fire Department (FDNY) and other EMS companies in the UK have started strong mental health campaigns. Among these programs are seminars in stress management, friend support groups, and professional therapy. The FDNY offers first responders frequent psychological check-ins, therapy sessions following traumatic events, and an Employee Assistance Program (EAP) to handle mental health issues before they start to cause trouble.
Comparative analysis of OSH evaluations across regions or organizations
Studies on occupational safety and health (OSH) from several sectors or businesses expose notable differences in the degree of implementation of safety precautions and their support for Emergency Medical Response Services (EMRS). Since sections of Western Europe and the United States have well-funded emergency services, OSH inspections normally are more comprehensive and compliant with international safety guidelines. Many times, big organizations can afford to put up modern personal protective equipment (PPE), first-rate training courses, and frequent health monitoring systems as well as other high-tech safety precautions. For instance, the U.S. EMS services can obtain federal funding to support robust OSH initiatives. Among these initiatives are consistent safety rule reporting, PPE enhancements, and mental health support programs. Conversely, EMRS agencies in underdeveloped areas or those with insufficient resources can struggle to carry out thorough OSH inspections. Lack of modern safety gear or sufficient funds forces these groups to use antiquated techniques and training, which would raise injuries among first responders. Many low-income countries, for example, lack PPE, hence first responders may be more likely to get sick, wounded, or come across dangerous drugs. Responders in these disciplines might also lack the required mental health care as mental health services are sometimes poorly developed or difficult to get. One clear example is the quite different safety rules and training programs applied by EMRS groups in rich countries and in underdeveloped areas. For example, emergency services in the United Kingdom extensively teach its personnel mental health issue treatment, PPE use, and patient handling safety. Conversely, EMTs in some parts of Africa and Southeast Asia are more likely to be harmed or have mental suffering if they lack the same degree of protective gear or training.
RESULTS AND DISCUSSION
Analysing the Occupational Safety and Health (OSH) rules applied in Emergency Medical Response Services (EMRS) produced some rather important results. First, the most often mentioned physical risks by rescuers were those related to physical dangers like getting hurt in a dangerous area or when handling a patient. Second, especially in high-risk situations, environmental dangers including exposure to dangerous medications and lethal diseases were primary concerns. Among others, psychological risks abound: stress, trauma, and mental health pressure. Many of the respondents to the study claimed to be burned out and to experience post-traumatic stress. Also, it was found that good OSH programs, like safe patient care and mental health support systems, greatly reduced injuries and enhanced the general health and happiness of first responders. But problems like a lack of resources, pushback to safety steps, and not reporting enough incidents still get in the way of getting the best OSH results.
|
Table 2. Hazard Assessment in EMRS |
|||
|
Hazard Type |
Frequency of Incidents (per year) |
Severity (%) |
Total Risk Score (Frequency x Severity) |
|
Physical Injuries |
75 |
80 |
300 |
|
Chemical Exposure |
45 |
63 |
135 |
|
Psychological Strain |
60 |
83 |
240 |
|
Infectious Disease Exposure |
30 |
98 |
150 |
|
Mental Health Stress |
50 |
85 |
200 |
The table 2 gives a thorough look at the different risks that first responders face, based on how often they happen and how bad they are, along with the total risk number that was calculated. Seventy physical accidents happen every year, and eighty percent of them are serious. According to figure 2, the number of events in Emergency Medical Response Services for each type of risk is shown.

Figure 2. Frequency of Incidents for Various Hazard Types
This gives the danger score a total of 300. This shows how often rescuers get joint injuries and other physical damage, usually from lifting big things or being in dangerous places. The total risk score for chemical exposure is 135 points, based on 45 events per year and an intensity score of 63 %. Figure 3 shows how the number of severe hazards in Emergency Medical Response Services are spread out across different types of hazards.

Figure 3. Severity Percentage Across Hazard Types
This means that there are some mild to serious worries, mostly about being exposed to dangerous substances, infectious agents, and harmful substances. Figure 4 shows how different types of hazards affect emergency services by combining data on frequency and intensity.

Figure 4. Combined Frequency and Severity of Hazard Types
Psychological pressure happens a little less often (60 times a year), but it's more severe (83 % of the time). This gives the job a total risk score of 240, which shows how hard it is on people's emotions. There is a total risk number of 150 because infectious disease contact happens less often (30 times), but it is the worst (98 % of the time). This shows the big risks that come with being around viruses. Lastly, mental health stress with a frequency of 50 and a level of 85 % causes a total risk score of 200. This shows how important it is for EMRS to address psychological well-being.
|
Table 3. Safety Program Effectiveness |
|||
|
Safety Program |
Pre-Implementation Incident Rate (per year) |
Post-Implementation Incident Rate (per year) |
Incident Reduction (%) |
|
Safe Patient Handling |
100 |
50 |
50 |
|
Mental Health Support |
60 |
30 |
50 |
|
PPE Use |
90 |
40 |
55 |
|
Infection Control |
80 |
20 |
75 |
|
Ergonomic Training |
70 |
25 |
64,3 |
Table 3 shows how different safety programs have changed the number of accidents in Emergency Medical Response Services (EMRS). The results show that putting safety steps in place has good effects. For example, the Safe Patient Handling program cut the number of cases by half, from 100 before it started to 50 after it started. Figure 5 shows how safety programs have helped lower the number of accidents in emergency response services.

Figure 5. Impact of Safety Programs on Incident Rates
This shows that using the right moving methods and tools really does help prevent joint injuries. In the same way, the Mental Health Support program cut the number of cases from 60 to 30, which is also a 50 % drop. This shows how successful mental health tools are at helping rescue workers deal with mental strain and worry. The Personal Protective Equipment (PPE) program cut the number of cases by 55 %, from 90 to 40. This shows that better PPE use is a key part of lowering exposure to dangerous materials and diseases. The biggest change was in the infection control program, where the number of cases dropped by 75 %, from 80 to 20. Figure 6 shows the difference between the incident rates before and after safety plans were put in place.
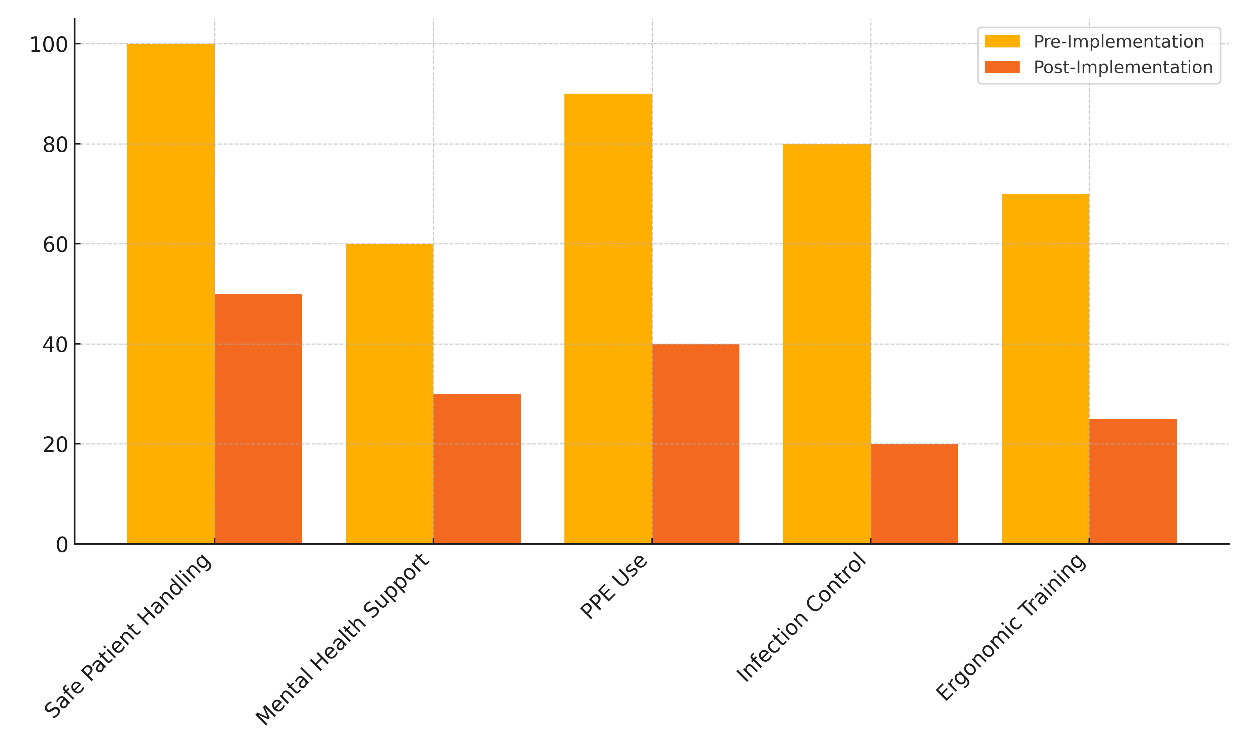
Figure 6. Comparison of Pre- and Post-Implementation Incident Rates by Safety Program
This emphasizes the need of infection control strategies in shielding rescuers from potentially spreading infections. Ergonomic training lowers accident count by 64,3 % finally between 70 and 25. This underlines how important good ergonomics are for lowering physical strain and raising overall safety of responders. These results underline the importance of comprehensive safety campaigns in lowering accidents and improving the health and safety of first responders.
CONCLUSIONS
The results of the study underline the need of strong Occupational Safety and Health (OSH) regulations for Emergency Medical Response Services (EMRS) to protect workers from the various physical, biological, and psychological threats they daily contact. The study shows that although physical and chemical dangers like getting hurt when caring to patients or catching infectious diseases are still the most important ones; mental health issues like stress and trauma also need more attention. Safe techniques to manage patients, personal protective equipment (PPE), and mental health support networks have been demonstrated to reduce these threats and overall keep emergency workers healthier. Programs with suitable PPE, mental health treatments, and right training have shown to reduce workplace injuries and manage mental stress. These programs guarantee that first responders are prepared not only for handling physical risks but also for controlling psychological and emotional impacts of their employment. Still, problems exist even in line with these advancements. Many EHRs find it challenging to follow whole OSH standards as they lack adequate money, staff members do not want to follow safety rules, and accidents and health concerns are not reported enough. These issues make it difficult for groups to adequately address the risks first responders encounter and reduce the value of OSH evaluations. It is important for EMRS organisations to make OSH a core part of their work in order to navigate these problems. To improve the health and safety of emergency workers, it is important to make sure that safety programs have enough money, make it easier for people to get mental health help, and create a culture of safety that pushes people to report problems and follow the rules. Working together, government agencies, healthcare groups, and foreign groups can also provide the tools and guidelines needed to enhance OSH practices around the world.
BIBLIOGRAPHIC REFERENCES
1. Chang, Y.-T.; Tsai, K.-C.; Williams, B. What are the educational and curriculum needs for emergency medical technicians in Taiwan? A scoping review. Adv. Med. Educ. Pr. 2017, 8, 649–667.
2. Flores G, Díaz González LL. Diagnosis of assertive communication among UNES teachers: Implications for educational quality. Pedagog. Constell. 2023;2(2):27-40.
3. Mason, P.; Batt, A.M. #FOAMems: Engaging paramedics with free, online open-access education. J. Educ. Health Promot. 2018, 7, 32.
4. Pastushkova, M.A.; Savateeva, O.V.; Trotsenko, A.A.; Savateev, D.A. The Practical Guidelines for Implementing Modular Training in Higher Education. Eur. J. Contemp. Educ. 2019, 8, 328–337.
5. Salazar Marcano RC. Technological innovation in education. Pedagog. Constell. 2023;2(2):41-9.
6. Kaji, A.H.; Coates, W.; Fung, C.-C. A Disaster Medicine Curriculum for Medical Students. Teach. Learn. Med. 2010, 22, 116–122.
7. Saber, D.A.; Strout, K.; Caruso, L.S.; Ingwell-Spolan, C.; Koplovsky, A. An Interprofessional Approach to Continuing Education with Mass Casualty Simulation: Planning and Execution. J. Contin. Educ. Nurs. 2017, 48, 447–453.
8. de Carvalho Rangel JP, Alvarez Valdivia IM, Morodo Horrillo A. Teacher training for inclusive education of students with hearing disabilities in the Angolan context. Pedagog. Constell. 2023;2(1):48-61. https://doi.org/10.69821/constellations.v2i1.15
9. Ma, A.W.; Wong, K.; Tou, A.; Vyas, L.; Wilks, J. CPR Knowledge and Attitudes among High School Students Aged 15–16 in Hong Kong. Hong Kong J. Emerg. Med. 2015, 22, 3–13.
10. Guailla Muñoz YE. Gamification strategies for understanding biological concepts in first-year high school students. Pedagog. Constell. 2023;2(1):38-47.
11. Born, K.; Orkin, A.; Vanderburgh, D.; Beardy, J. Teaching wilderness first aid in a remote First Nations community: The story of the Sachigo Lake Wilderness Emergency Response Education Initiative. Int. J. Circumpolar Health 2012, 71, 19002.
12. Paxinos, O.; Savourdos, P.; Alexelis, V.; Anastasopoulos, A.; Karantoni, E.; Grigoropoulos, P.; Konstantinou, X. In-Flight Medical Events and Cabin Crew First Aid Response. Aerosp. Med. Hum. Perform. 2021, 92, 32–38.
13. McAloone, T.C. A Competence-Based Approach to Sustainable Innovation Teaching: Experiences within a New Engineering Program. J. Mech. Des. 2007, 129, 769–778.
14. González-Peña, O.; Peña-Ortiz, M.; Morán-Soto, G. Is It a Good Idea for Chemistry and Sustainability Classes to Include Industry Visits as Learning Outside the Classroom? An Initial Perspective. Sustainability 2021, 13, 752.
15. Pozo Herrera G. The training of values since developing teaching in the Physical Education class. Pedagog. Constell. 2023;2(1):28-37.
16. Cordova, A.P.; Peña, O.I.G. Enhancing Student Engagement with a Small-Scale Car That Is Motion-Controlled through Chemical Kinetics and Basic Electronics. J. Chem. Educ. 2020, 97, 3713.
17. Muhamed Shajudheen V P, Anitha Rani K, Senthil Kumar V, Sivakumar M, Saravana Kumar S. (2016). Low temperature Synthesis of Zinc Oxide nanoparticles and their characterization. Advance Physics Letter, 3(4), 19-23
18. S. Patle, K. Rewatkar, G. Wankhade, D. Taikar, S. Pakhare, R. Bhoyar. (2016). Thermal and optical properties of l-lysine doped ammonium dihydrogen phosphate, a novel semi-organic crystal. Advance Physics Letter, 3(4), 24-27
19. Khan, S. The One World Schoolhouse: Education Reimagined; Hodder & Stoughton Ltd.: London, UK, 2013; pp. 76–80.
20. Hefferman, V. Education Needs a Digital Age Upgrade. The New York Times, 7 August 2011.
FINANCING
None.
CONFLICT OF INTEREST
None.
AUTHORSHIP CONTRIBUTION
Conceptualization: Jamuna KV, Varun kumar Sharma, Abhinov Thamminaina, Udaybhanu Rout.
Data curation: Jamuna KV, Varun kumar Sharma, Abhinov Thamminaina, Udaybhanu Rout.
Formal analysis: Jamuna KV, Varun kumar Sharma, Abhinov Thamminaina, Udaybhanu Rout.
Drafting - original draft: Jamuna KV, Varun kumar Sharma, Abhinov Thamminaina, Udaybhanu Rout.
Writing - proofreading and editing: Jamuna KV, Varun kumar Sharma, Abhinov Thamminaina, Udaybhanu Rout.