doi: 10.56294/hl2023294
ORIGINAL
A Comparative Analysis of Environmental Health Policies Across Varied Healthcare Systems
Análisis comparativo de las políticas de salud ambiental en distintos sistemas sanitarios
Abhijeet Nashte1 ![]() , Shankar Lal Soni2
, Shankar Lal Soni2 ![]() , Manashree Mane3
, Manashree Mane3 ![]() , Sudesh Sangwan4
, Sudesh Sangwan4 ![]() , Rajendra Prasad Satapathy5
, Rajendra Prasad Satapathy5 ![]()
1Krishna Institute of Medical Sciences, Krishna Vishwa Vidyapeeth “Deemed to be University”, Dept. of Medicine. Taluka-Karad, Dist-Satara, Maharashtra, India.
2Arya College of Pharmacy. Jaipur, Rajasthan, India.
3JAIN (Deemed-to-be University), Department of Forensic Science. Bangalore, Karnataka, India.
4School of Liberal Arts, Noida International University. Greater Noida, Uttar Pradesh, India.
5IMS and SUM Hospital, Siksha ‘O’ Anusandhan (Deemed to be University), Department of Cardiology. Bhubaneswar, Odisha, India.
Cite as: Nashte A, Soni SL, Mane M, Sangwan S, Prasad Satapathy R. A Comparative Analysis of Environmental Health Policies Across Varied Healthcare Systems. Health Leadership and Quality of Life. 2023; 2:294. https://doi.org/10.56294/hl2023294
Submitted: 13-05-2023 Revised: 28-07-2023 Accepted: 17-10-2023 Published: 18-10-2023
Editor:
PhD.
Prof. Neela Satheesh ![]()
ABSTRACT
Natural health is a recently developed discipline acknowledging the significant influence natural elements have on human well-being. Policies that consider how outside events influence people’s health must be consistent in order to reduce risks and enhance general well-off. This paper examines environmental health policy of many healthcare systems. It demonstrates the variations in policy frameworks, legal procedures, and public health protection capacity among them. From those with universal coverage to those with privatised systems, the research examines several nations with various healthcare systems. Its aim is to identify the most important legislative projects addressing environmental health issues including waste management, water quality, air pollution, and climate change adaptation. The paper examines how various nations handle environmental health concerns within their own healthcare systems. It achieves this by means of both qualitative and quantitative research approaches, including policy evaluation, statistics on health outcomes, and interaction with important legislators and health professionals. The research mainly examines the variations between the regulations in countries like the US depending on commercial health care models and those in Scandinavia with robust public health care systems. It looks at how these systems use environmental health studies to plan and make policies for healthcare and the problems they face when trying to balance health and environmental goals. At the end of the study, the best practices from the different healthcare systems are highlighted, problems with putting policies into action are pointed out, and suggestions for change are made. To get long-lasting health results, it is very important that environmental health strategies are well integrated into healthcare systems. The results show that working together across sectors, making policies stronger, and making people more aware are all important for improving the health of the environment and reducing its effects on people who are already weak. Also, encouraging international cooperation and learning from different healthcare systems can help shape future policies that aim to improve health around the world and protect the environment.
Keywords: Environmental Health; Healthcare Systems; Policy Analysis; Public Health; Sustainable Health.
RESUMEN
La salud natural es una disciplina de reciente desarrollo que reconoce la importante influencia de los elementos naturales en el bienestar humano. Las políticas que tienen en cuenta cómo influyen los acontecimientos externos en la salud de las personas deben ser coherentes para reducir los riesgos y mejorar el bienestar general. Este artículo examina la política de salud ambiental de muchos sistemas sanitarios. Demuestra las variaciones que existen entre ellos en cuanto a marcos políticos, procedimientos legales y capacidad de protección de la salud pública. Desde los que tienen cobertura universal hasta los que cuentan con sistemas privatizados, la investigación examina varias naciones con diversos sistemas sanitarios. Su objetivo es identificar los proyectos legislativos más importantes que abordan cuestiones de salud ambiental como la gestión de residuos, la calidad del agua, la contaminación atmosférica y la adaptación al cambio climático. El documento examina cómo gestionan las distintas naciones los problemas de salud ambiental dentro de sus propios sistemas sanitarios. Para ello utiliza métodos de investigación cualitativos y cuantitativos, como la evaluación de políticas, estadísticas sobre resultados sanitarios y la interacción con importantes legisladores y profesionales sanitarios. La investigación examina principalmente las variaciones entre las normativas de países como EE.UU., que dependen de modelos sanitarios comerciales, y las de Escandinavia, con sólidos sistemas sanitarios públicos. Analiza cómo utilizan estos sistemas los estudios de salud ambiental para planificar y elaborar políticas de asistencia sanitaria y los problemas a los que se enfrentan cuando intentan equilibrar los objetivos sanitarios y ambientales. Al final del estudio se destacan las mejores prácticas de los distintos sistemas sanitarios, se señalan los problemas que plantea la puesta en práctica de las políticas y se hacen sugerencias para el cambio. Para obtener resultados sanitarios duraderos, es muy importante que las estrategias de salud ambiental estén bien integradas en los sistemas sanitarios. Los resultados muestran que la colaboración entre sectores, el refuerzo de las políticas y la concienciación de la población son importantes para mejorar la salud del medio ambiente y reducir sus efectos en las personas ya de por sí débiles. Asimismo, fomentar la cooperación internacional y aprender de los distintos sistemas sanitarios puede ayudar a configurar futuras políticas encaminadas a mejorar la salud en todo el mundo y proteger el medio ambiente.
Palabras clave: Salud Ambiental; Sistemas Sanitarios; Análisis de Políticas; Salud Pública; Salud Sostenible.
INTRODUCTION
Environmental health is becoming more and more important to public health because the places where people live, work, and play have a direct effect on their health. More attention is being paid to incorporating environmental health concerns into public health policies now that it is known that environmental factors, such as garbage management, climate change, and the quality of the air and water, play a big role in the spread of disease. These natural problems, like pollution, climate change, and ecology damage, are getting worse, so it's clear that healthcare systems all over the world need to change and adapt to deal with them properly. Depending on the country's health care system, public health laws are very different. These differences are often caused by different cultural settings, healthcare methods, economic situations, and government systems. The way outdoor health risks are dealt with and the rules meant to lower them depend on the goals of the healthcare system, which could be public, private, or a mix of the two. Different healthcare systems may include plans for everyone to get medical care, like in many European countries, or systems that are paid for privately, like most of the time in the US. All healthcare systems have problems when they try to include environmental health issues in their policies, even though they provide and cover different types of care. This is especially true when it comes to big global problems like climate change, biodiversity loss, and new environmental hazards. The goal of environmental health policies is to stop health problems that are caused by the environment and to make living situations better in ways that are good for everyone. But these policies often only work if the healthcare system is strong and reaches a lot of people, if politicians are willing to enforce environmental laws, and if the environmental, public health, and healthcare sectors work together well.
Furthermore greatly influencing policy decisions and execution are the political and social context of a nation. Countries with well-funded public healthcare systems might be more suited to apply environmental health initiatives impacting the general population. Conversely, nations with privatised healthcare systems might find it more difficult to ensure that every one of their citizens has comparable access to environmental health advantages. This research aims to investigate how various healthcare systems arrange their environmental health policies and contrast their effectiveness in safeguarding public health from environmental risk factors. The research examines many nations' healthcare systems across diverse categories. It covers Nordic nations with universal health care, the US with private health insurance, Canada and the United Kingdom with a blend of their two forms of systems.(1) Examining policy initiatives, medical facilities, and health outcomes, this article provides insightful analysis of the advantages and drawbacks of many approaches for environmental health governance. Examining how environmental health studies may be used in the administration and planning of healthcare systems is crucial in the comparison. Many healthcare systems struggle to guarantee that public health objectives and environmental regulations complement one other. For instance, initiatives to enhance water quality or reduce the consequences of air pollution on public health usually call for a great degree of collaboration throughout many spheres, including between environmental authorities, urban planning, and healthcare systems.(2) Coordinating these sorts of activities may be challenging in areas where health services are outsourced or decentralised, which would result in variations in the state of public health. Among the most critical issues facing environmental health policy is climate change. As global temperatures increase and more catastrophic events strike, the healthcare system must adapt to handle fresh challenges. Rising temperatures, for instance, worsen air pollution, heat-induced ailments, and the spread of diseases carried by insects. Moreover, more and more people are migrating and being compelled to do so due to climate change, which strains infrastructure and healthcare systems especially.
Concepts of Environmental Health
Definition and key components
Environmental health is the branch of public health that investigates how individuals interact with their surroundings and how such surroundings could influence individuals’ health and well-being. It entails determining the hazards to health resulting from physical, chemical, biological, and social elements in the environment and then acting to reduce those hazards. Environmental health seeks to ensure that the planet is safe and healthy, therefore benefiting everyone's health. Important aspects of environmental health include quality of the air and water, appropriate garbage management, food safety, noise control, and chemical safety. Air quality control is to prevent pollution of the air, therefore avoiding lung and heart diseases. Natural health depends much on water quality as it prevents the transmission of illnesses via this medium.(3) Maintaining the cleanliness of the environment and human health depends on the management of rubbish, which involves disposal of hazardous items and solid waste. Food safety rules are designed to reduce the possibility of acquiring illness by handling, storing, or contaminating food in dangerous manner. Noise management strategies seek to reduce noise pollution, which has been connected to heart disorders, stress, and hearing loss. Chemical safety is the regulation of harmful substances such as heavy metals and pesticides so as to minimise their effects on people. Together, these elements ensure that individuals live in environments fit for their social, psychological, and general health as well as their physical one. Environmental health practices seek to eliminate or minimise environmental hazards by means of policy implementation, control, education, and advocacy.(4) This helps to ensure that surroundings can endure, enhances quality of life, and prevents illness or injury among people.
Relationship between environment and public health
Public health and the surroundings are closely related as environmental circumstances greatly influence people's level of health. Environmental elements may directly influence people's and communities' social, psychological, and physical health as well as their beneficial or negative effects. The constructed, environmental, and social surroundings may greatly alter the many health hazards. Among the many instances include exposure to harmful chemicals, air and water pollution, and noise pollution. These exposures increase the likelihood of several health issues including lung ailments, heart disorders, malignancies, and mental health issues. For instance, among the primary environmental factors causing ailments like heart disease, COPD, and asthma is air pollution. Long-term health issues might result from the lungs swelling caused by pollutants like ground-level ozone and particulate matter (PM 2,5). Bad water quality, which is usually brought on by bacteria, chemicals, or heavy metals, may similarly lead to stomach illnesses, cholera, and other communicable diseases. Public health is much influenced by the built environment, which include transportation networks, municipal planning, and housing quality as well. Overcrowding, bad sanitation, and housing that isn't up to code can all help diseases spread and add to mental health problems.(5) Well-planned cities, on the other hand, with easy access to green spaces, clean air, and safe water systems, encourage healthy living and keep people from getting sick. The link between external factors and public health effects is shown in figure 1. Also, climate change has become a worldwide problem for the environment that has huge effects on people's health.
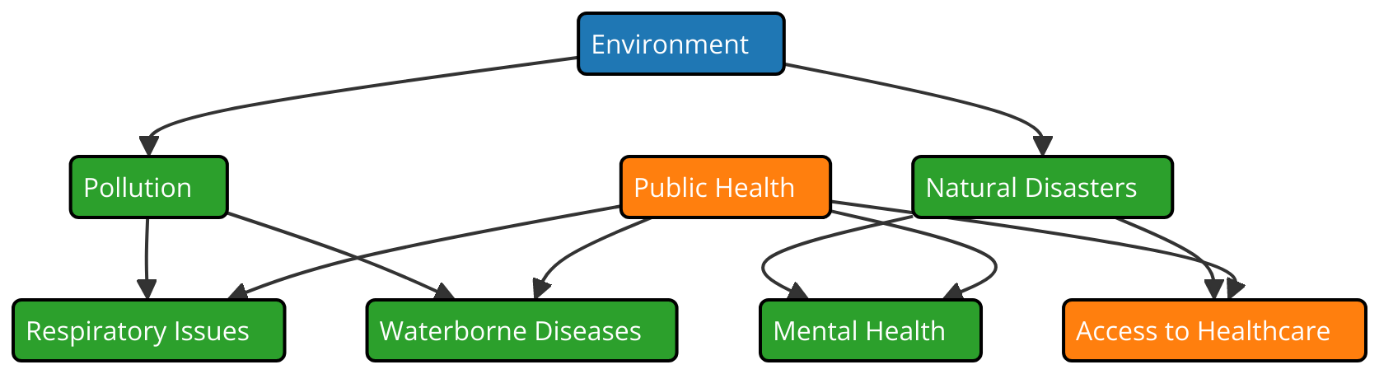
Figure 1. Illustrating the relationship between the environment and public health
As temperatures rise, extreme weather events happen more often, and disease patterns change, they all make health risks new and worse. Some groups are more likely to be hurt by environmental degradation than others. These groups include children, the elderly, and people who already have health problems.
Global environmental health challenges
The problems with global environmental health are getting harder to solve because of how natural, social, and economic issues affect each other. Climate change is one of the biggest problems because it is making health risks worse and making new ones. Rising temperatures, extreme weather events like storms, floods, and droughts, and changes in disease trends are all effects of climate change that have big effects on human health. For example, heatwaves make it more likely for people to get heat stress, heart disease, and become dehydrated. Water-borne diseases like cholera and dysentery can spread because of flooding. Changing temperature conditions make it easier for vector-borne diseases like malaria and dengue to spread to new areas. Air pollution is another big natural health problem.(6) Every year, it kills millions of people around the world. Global air pollution is tied to about 4,2 million early deaths every year, mostly from heart and lung illnesses, according to the World Health Organisation (WHO). Air quality is often not good in cities, where pollution from factories and cars is common. This makes health problems worse for people who are already at a disadvantage. Lack of clean water and water pollution are also big problems around the world, with millions of people not being able to get it. A lot of diseases that can be avoided, like cholera, dysentery, and typhoid fever, are spread by contaminated water sources. Environmental health ideas are summed up in table 1, which shows methods, rewards, obstacles, and effects.
|
Table 1. Summary of Concepts of Environmental Health |
|||
|
Approach |
Benefits |
Challenges |
Impact |
|
Public Healthcare Systems (e.g., UK) |
Universal access to healthcare, comprehensive health protection |
High cost, budget allocation, potential delays |
Improved public health outcomes, reduced health inequities |
|
Private Healthcare Systems (e.g., USA) |
Faster service delivery, innovation, but unequal access |
Limited access for lower-income populations, policy inconsistency |
Widening health disparities, but advances in innovation and technology |
|
Mixed Healthcare Systems (e.g., Sweden)(7) |
Balanced system offering access and flexibility |
Balancing public and private sector interests, complex administration |
Well-rounded policies, balanced access, and sustainable development |
|
National Air Quality Regulations (USA) |
Improved air quality, reduced health issues from pollution |
Political resistance, economic interests |
Improved air quality, lower healthcare costs from respiratory issues |
|
Clean Water Regulations (UK) |
Safe drinking water, reduced waterborne diseases |
Funding constraints, enforcement challenges |
Reduced incidence of waterborne diseases, improved public health |
|
Climate Action Plans (Sweden) |
Reduced carbon footprint, improved public health resilience |
Global coordination, industry resistance |
Enhanced climate resilience, better healthcare infrastructure |
|
Environmental Health Education Programs |
Increased awareness and public engagement |
Lack of funding, inconsistent implementation |
Informed public, higher demand for environmentally-conscious policies |
|
Waste Management Policies (Denmark) |
Cleaner environments, reduced disease transmission |
Resource allocation, waste treatment infrastructure |
Better waste management, reduced environmental health risks |
|
Green Healthcare Initiatives (USA) |
Lower emissions, reduced healthcare costs from pollution-related diseases |
Initial high costs, resistance from industries |
Reduced pollution, long-term health benefits from cleaner air |
|
Eco-Friendly Urban Planning (UK)(8) |
Healthier urban environments, better mental health outcomes |
Urban sprawl, resistance from developers and local authorities |
Better quality of life, increased physical activity in urban spaces |
|
Sustainable Agriculture Practices (Denmark) |
Reduced pesticide use, healthier food production |
Short-term economic priorities, resistance from agricultural sectors |
Sustainable food systems, lower public health burden from pesticides |
|
Air Quality Monitoring Systems (India) |
Improved air quality, early detection of health risks |
Insufficient data, political barriers |
Early identification of health risks, better preparedness for health crises |
|
Public Health Campaigns (Global) |
Global collaboration, better disease prevention strategies |
Diverse regulations, varying public response across regions |
Global health improvements, reduced impact of pandemics and climate change |
Overview of Healthcare Systems
Classification of healthcare systems (public vs. private)
General speaking, there are two types of healthcare systems: public and private. How healthcare services are paid for, provided, and handled is what makes them different. In public health care schemes, the government is in charge of paying for and overseeing health care. The goal is to make sure that all people have access to healthcare, so these systems are usually paid for by taxes, fees, or other public sources of income. Standardised rules and policies can be put in place for public systems because they are usually run from one place. These rules and policies include environmental health policies that protect public health by controlling pollution, managing trash, and reducing the effects of climate change. The goal of public healthcare methods is to reduce health gaps by making sure that everyone, no matter their wealth or social class, has access to healthcare services.(9) Private healthcare systems, on the other hand, are built on the market, and private companies like insurance firms, healthcare providers, and drug companies play a big part in providing services. People or their companies usually pay for health care in these setups through private insurance or cash payments. Even though private systems may provide faster access to services and work better in some situations, they often lead to unequal access to care because people who can't afford treatments may be kept from getting them. If you live in a private system, environmental health policies are usually not as centralised because they rely more on people following the rules and market rewards rather than direct government action.(10)
Models of healthcare (e.g., universal healthcare, mixed systems)
There are several types of healthcare systems around the world. Each model is different in terms of who can get care, how it is paid for, and how much the government is involved. One very common approach is national healthcare, in which the government makes sure that all citizens can get medical care, even if they can't pay for it. This plan is usually paid for by taxes, and it focusses on fairness to try and even out health results between people from different social groups. In countries with universal health care systems, like the UK's National Health Service and Canada's, environmental health issues, like rules on water and air quality, are often taken into account when planning and providing healthcare. By covering everything, these systems can put the health of the whole community first and include steps to keep natural health risks to a minimum. There are parts of both public and private healthcare in mixed healthcare systems.(11) In mixed systems, like the ones in France and Germany, everyone can get basic healthcare services that are paid for by the government. However, people can also buy private insurance or go to private healthcare providers for extra services. This mixed method tries to find the best parts of both public and private systems so that everyone can get health care, but also lets healthcare providers be flexible and come up with new ideas.(11) Environmental health policies that cover everyone can be supported by mixed systems, but it can be hard to make sure that everyone has the same access to safety for their health, especially people with lower incomes who might not be able to pay for extra services or private insurance. There is also the single-payer system, which is used in places like Taiwan. In this plan, the government is the only provider, and it uses its resources to give all of its people health care. Because there is centralised control and the power to run large-scale environmental health programs, the single-payer system can better address environmental health issues. The hard part about these systems is keeping quality high and making sure that public health rules are followed the same way all over the country.
Influence of healthcare systems on environmental health policies
The way a healthcare system is set up and how it works have a big impact on how environmental health policies are made and used. Healthcare systems with more government input, like state healthcare systems, are more likely to make and follow strong environmental health rules. The reason for this is that these systems are centralised and can use standard methods to affect a large part of the people. Environmental health problems like air pollution, water poisoning, and trash management are often dealt with more proactively by governments in public healthcare systems. This is because it is part of their larger public health goals. Also, centralised methods make it easier to divide up funds for environmental health study, tracking, and policy enforcement. Environmental health risks are usually taken into account in national healthcare plans of countries with public healthcare.(12) This includes rules on energy use, greenhouse gas emissions, and adapting to climate change. Scandinavian countries, which have good public health care systems, have added environmental health to their health policies by controlling pollution and setting high standards for clean water and air. This has led to better public health. Environmental health programs can be used by many people because these policies are backed by a lot of money and help from the government. Private healthcare systems, on the other hand, don't always have the central organisation needed to make sure that environmental health rules are followed by everyone. Environmental rules can be made voluntarily or because of market pressures, but these systems usually give more weight to market-based methods than to broad public health actions.
Key Environmental Health Policies and Frameworks
National and international policy frameworks
National and foreign policy frameworks are very important for dealing with environmental health problems because they set rules, guides, and strategies for protecting the environment and people's health. At the national level, governments make and enforce rules that aim to lower the health risks that the climate poses to people. Most of the time, these rules are based on facts from science, economics, and society. They are usually organised by health, environmental, and government agencies. Legislation is often part of national systems to control dangerous garbage, handle air and water quality, lower exposure to poisonous chemicals, and stop the bad health effects of climate change.(13) The Clean Air Act in the US and the guidelines on water quality and garbage control in the EU are two important examples. International standards inspire people all over to cooperate in order to address environmental and health issues impacting many nations. Two of the most influential groups establishing world standards and supporting nations in developing policies safeguarding their natural health are the World Health Organisation (WHO) and the United Nations Environment Program (UNEP). International agreements as the Paris Agreement on Climate Change and the Minamata Convention on Mercury are aimed to reduce the health hazards resulting from the surroundings worldwide. These models inspire nations to cooperate, exchange data, develop one another's capabilities, and act together. For instance, the WHO's guidelines on air quality define worldwide standards to assist nations in lowering the detrimental consequences of air pollution, particularly in metropolitan areas.(14) Policies both national and international are continually evolving. To meet global standards, national governments often match their policies with international deals. But problems like different political goals, economic concerns, and levels of loyalty can make it harder to put these models into action. Even with these problems, national and foreign structures are still very important for making progress in environmental health.
Core principles of environmental health policies
Environmental health policies are based on a set of core values that are meant to protect public health, encourage resilience, and make things fair. Some of these concepts are taking precautions, fairness, longevity, and duty to future generations. The precautionary principle is a basic rule that says people should take precautions when there is a chance that something bad will happen to the public's health, even if there isn't enough scientific proof to prove it. In order to lower environmental risks before they have major health effects, it is necessary to act quickly. For instance, policies that try to lower greenhouse gas emissions and air pollution are usually based on the precautionary principle because it's hard to know what the long-term effects will be on health, but they could be very bad.(15) Another important idea in environmental health policy is equity, which means making sure that everyone, especially weaker groups, has the same chances to get environmental health benefits. This covers determining why certain individuals are more or less likely to be exposed to natural hazards include harmful living, poor air quality, and contaminated water. Environmental health policy should seek to reduce health inequalities by providing everyone, regardless of their socioeconomic level or location, the same degree of protection from environmental hazards. Environmental health is mostly dependent on sustainability, hence it emphasises the need of maintaining the environment healthy for next generations. This idea demands laws that strike a compromise between people's health requirements and the capacity of the surroundings to sustain life. It also encourages environmentally responsible behaviours include utilising green energy, constructing in a manner that fits the surroundings, and waste reduction. As part of being sustainable, hospital systems need to be changed so that they can handle problems like climate change.
Governance and policy implementation
For environmental health policies to have real-world effects, they need to be backed up by good government and policy implementation. Governance includes the systems, procedures, and organisations that make environmental health policies, carry them out, and keep an eye on them. For national government to work well, different areas like health, the environment, farming, and urban planning need to work together. Ministries of health and environmental protection, for example, are very important parts of the government because they make policy, set rules, and make sure people follow them. These organisations must cooperate to provide coherent and coordinated public health strategies. Implementing policies is often a difficult procedure including monitoring systems and methods for application of laws and regulations as well as putting them into programs that may be employed. Environmental health programs must be supported by robust laws, sufficient money, and qualified individuals to guarantee accurate execution if adoption is to be successful. Understanding how policies are functioning and making necessary adjustments depends on knowing the mechanisms for observing and assessing. For example, techniques that monitor air quality assist to track smog levels and guarantee adherence to policies. Working with other nations is another crucial component of governance and policy formation. Many environmental and health issues, like trash crossing boundaries and climate change, need on nations to cooperate in order to be solved. By providing professional assistance, data, and funding, international organisations like the WHO and UNEP enable nations to effectively implement their programs.
Comparative Analysis of Environmental Health Policies
Healthcare System 1 (e.g., U.S. healthcare system)
Policy development and key initiatives
Emphasising personal freedom and private insurance, the U.S. healthcare system is essentially private and market-based. When it comes to monitoring and regulating healthcare policies—including those pertaining to environmental health—the federal government is quite crucial. Policies are often developed in the United States via a combination of court decisions, presidential guidelines, and legislature activity. Decisions are rendered at federal, state, and local levels of governance. Many significant environmental health initiatives are run by American government agencies such the Centres for Disease Control and Prevention (CDC) and the Environmental Protection Agency (EPA). For instance, the EPA is in responsibility of developing and maintaining guidelines for the environment aimed to reduce pollution and maintain human health. Two such legislative attempts are the Clean Air Act and the Clean Water Act. The Clean Water Act guarantees that water is safe and of excellent quality; the Clean Air Act establishes criteria for air quality to help to reduce pollution. The Safe Drinking Water Act guarantees that public water systems satisfy health criteria and prevent public exposure to harmful substances like toxins and other pollutants. Campaigns like the renewable New Deal have presented increasingly all-encompassing ideas in the last several years to reduce carbon emissions, substitute renewable energy sources, and promote environmental resilience in order to raise public health. There were also indirectly addressing environmental health aspects of the Affordable Care Act (ACA). These components enhanced healthcare coverage and improved access to preventative treatment, therefore helping underprivileged people cope with the consequences of environmental hazards. Political reasons and commercial interests frequently impact environmental health policies developed in the United States. Different administrations embrace control to varied degrees. Environmental and public health organisations should advocate for legislative improvements; nonetheless, environmental health is still a sensitive topic in relation to commercial pressure and economic objectives.
Focus on environmental health issues
The U.S. healthcare system is becoming more aware of how important it is to deal with environmental health problems, but it is still hard to make these issues a part of healthcare policy. In the United States, regulations, public health campaigns, and scientific research aiming at reducing exposure to harmful environmental factors like climate change, air pollution, and hazardous substances handle environmental health issues. Public health policies of the United States heavily rely on air quality. Affecting your lungs and heart, ground-level ozone and particle matter (PM 2,5) are two forms of air pollution that are very detrimental for your health. The EPA establishes national standards for air quality under the Clean Air Act, which regulates pollutants from power plants, businesses, and vehicles as well as from factories. However, implementation and compliance have been called under scrutiny several times, particularly in light of many government administrations' presence in power. This has led to arguments about how well air quality rules work. Focussing on water quality is another important thing to do. The Clean Water State Revolving Fund Program and the Safe Drinking Water Act are supposed to keep trash from companies, chemicals, and lead out of reach from water supplies. Flint, Michigan's water crisis demonstrated the value of clean water and the fragility of underprivileged communities against environmental health hazards. Public health rules in the United States are beginning to give climate change more of its due. Extreme weather and increasing temperatures directly affect public health; they increase the likelihood of individuals being sick from the heat, from being bitten by a mosquito, from breathing in polluted air. Starting many initiatives to detect and respond to the health impacts of climate change, including heat waves and higher incidences of illnesses carried by insects, including Lyme disease and West Nile virus, the U.S. Centres for Disease Control and Prevention (CDC).
Healthcare System 2 (e.g., UK healthcare system)
Policy development and key initiatives
Mostly funded by the government, the National Health Service (NHS) runs the healthcare system for the United Kingdom provides all individuals with a complete spectrum of health services. The UK has a centralised policy-making process, and the government greatly influences healthcare policies including those pertaining to environmental health even those pertaining to policy-making. Policies are created via laws, professional organisations, and public forums with an eye towards public health and justice. Often leading significant environmental health initiatives in the UK are the Department of Health and Social Care (DHSC) and environmental bodies such as the Environment Agency (EA) and Public Health England (PHE). These organisations cooperate to create and abide by guidelines that maintain the health of individuals against natural hazards. Among the most important schemes is the Clean Growth Strategy. Its aim is to reduce greenhouse gas emissions while nevertheless promoting economic development. The strategy calls for families and businesses to consume less energy, reduce carbon emissions from transportation, and go to greener energy sources. This approach aims to improve the quality of the air, therefore benefiting everyone's health, in addition to trying to halt climate change. Released in 2019, the NHS Long Term Plan likewise considers environmental health. It seeks, for instance, to reduce the carbon footprint of the NHS and make treatment more ecologically benign. By 2020 the NHS pledges to be carbon-neutral. This reveals a great will to handle the consequences of healthcare on the surroundings. Furthermore greatly improving air quality has been done by the UK government. Two instances of policies that have contributed to improve city air are the Clean Air Zone initiative and the Air Quality Standards Regulations. Furthermore underlined by regulations such as the Environment Bill is the need of long-term environmental policies in all spheres, including the medical one.
Focus on environmental health issues
The UK's healthcare system gives environmental health issues including those brought on by air pollution, water quality, and climate change much thought. With an eye towards both preventative and response strategies, environmental health is becoming more significant in healthcare policy and shows up in many different spheres. Among the main natural health concerns facing the UK is air pollution. It is believed that 40 000 individuals die too soon annually from this reason. The UK government has developed many laws meant to reduce detrimental pollution in order to address this issue. These include stricter corporate and automotive pollution rules. The Air Quality Standards Regulations restrict pollutants including particulate matter (PM 2,5) and nitrogen dioxide (NO2). The government has also established Clean Air Zones to help large cities' air quality be improved. Public health initiatives help people to become more aware of the negative consequences of poor air quality. Children and the elderly, who are more prone to have lung diseases, particularly this is true. Water quality is still another crucial issue. The Water Supply (Water Quality) Regulations provide guidelines for UK water safety. These guidelines ensure that drinking water does not include lead, pathogens, or compounds harmful for humans. Working with water businesses, the government maintains rigorous standards for water safety and seeks to avoid illnesses carried by water. This is done so as to safeguard public health. People believe increasingly that climate change poses a major public health issue. The UK government's attempt at handling this issue is the Climate Change Act 2008. With an eye towards adjusting to the health hazards climate change brings heat waves, floods, and the spread of diseases the UK needs to decrease its greenhouse gas emissions by 80 % by 2050. Reports on the health hazards of climate change have been issued by Public Health England (PHE).
Healthcare System 3 (e.g., Scandinavian countries)
Policy development and key initiatives
Like Sweden, Norway, Denmark, and Finland, Scandinavian nations have well-developed government-paid for healthcare systems. Emphasising equality, sustainability, and public health, these systems ensure that everyone can afford healthcare. In many nations, this kind of policymaking involves many diverse parties collaborating—public, healthcare professionals, environmental organisations, government agencies, etc. The major responsibility of the government is to ensure that social and environmental policies are tightly related to health policy. Among the most significant policy frameworks in Scandinavian nations is the Nordic Health Programme. It guides clinicians and planners on taking the environment and health into consideration when they develop and administer healthcare. These nations also were among the first to use sustainable healthcare practices. For instance, Sweden's National Environmental Health Action Plan focuses on integrating environmental issues into public health strategies. Figure 2 shows how healthcare policies and programs have changed over time in Scandinavian countries. It stresses the need for effective pollution control and long-term urban growth.
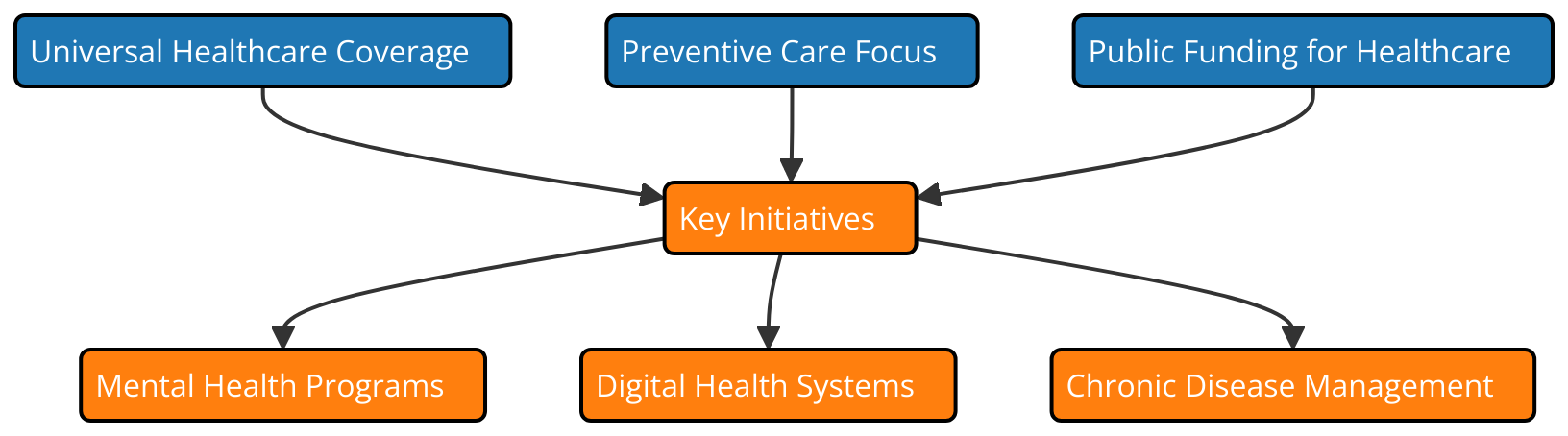
Figure 2. Healthcare system policy development and key initiatives in Scandinavian countries
Scandinavian countries have been at the front of the pack when it comes to supporting green technologies and cutting carbon pollution when it comes to energy and climate policy. By 2045, for instance, Sweden's Climate Act seeks to eliminate all greenhouse gas emissions. People's health will be much changed by this. Denmark's Green Growth Strategy promotes reduced pollution in the environment and ecologically friendly agricultural techniques, therefore preserving the surroundings and improving human health.
Focus on environmental health issues
In Scandinavian nations, where individuals are very conscious of the links between the environment and their health, environmental health plays a major role in healthcare policy. These nations are acting to address environmental health issues by means of large-scale strategies including activities against climate change, pollution control, and enhancement of public health. In many Scandinavian cities, a major environmental and health issue is air pollution. This is particularly true in metropolitan areas where vehicle-related pollution presents challenges. Sweden has implemented many initiatives to improve the air quality, including urging consumers to purchase electric vehicles, charging those to drive in large cities, and factory emission control. Norway has set policies to lower transport pollution by pushing people to adopt electric vehicles in order to become a zero-emissions society by 2025. Reducing lung and heart problems connected to air pollution is the aim here. One other crucial consideration should be the water's quality. High requirements for clean drinking water are well-known among Scandinavian nations. To avoid illnesses transmitted by water, Finland's Water Safety Policy emphasises the importance of maintaining and enhancing the quality of both surface and subteractive water. The government regularly monitors water quality and strictly enforces policies to guarantee that everyone has clean drinking water. People in Scandinavia are becoming more concerned about how environmental change will compromise their health. Rising temperatures and altering weather patterns lead to health issues including heat waves, storms, and the spread of infectious illnesses. To shield vulnerable populations from these hazards, Sweden and Finland have developed strategies to respond to climate change. For instance, Sweden's Climate Adaptation Strategy calls for actions to guard against heat-related illnesses and improve healthcare systems so they may manage health emergencies brought on by climate change. The strategy also addresses how to handle anxiety and other mental health consequences of climate change.
Challenges in Policy Implementation
Economic barriers and funding issues
Implementing public health initiatives comes with a major challenge as insufficient funds are available. Environmental health policies may call for large expenditures in areas like infrastructure, technology, research, and methods of ensuring its execution. Changing to better energy sources, cleaning the air and water, or creating long-term waste management strategies all cost a lot of money. Finding the funds to handle environmental health issues in locations where budgets are limited or the economy is faltering may be challenging. This is particularly true in cases of other pressing needs like bettering access to healthcare, education, or economic development that call for immediate attention. Lack of finances in state healthcare systems may lead rules to not be followed exactly. Since long-term environmental health initiatives are considered as less vital right now than short-term healthcare services, governments may not fund them as much. Investing in pollution management or clean energy, for instance, calls for long-term planning and upfront expenses, but the health advantages such as fewer lung and heart diseases may not be immediately clear-cut. Politicians often refuse to do this as they can be more concerned with immediate gains than with long-term outcomes of health. Similar economic issues might surface in private healthcare systems, particularly with regard to implementing sustainable practices that preserve the surroundings. For example, generally requiring a large upfront expenditure, changing to greener technology or lessening the environmental impact of healthcare facilities calls for In areas where healthcare is primarily private, these expenses might be passed on to patients or healthcare providers, therefore affecting the size and efficiency of these initiatives. In terms of global endeavours to address environmental health issues, variations in wealth between rich and underdeveloped nations might hinder efforts. Low-income nations can lack the means to provide the necessary infrastructure or implement robust environmental policies. Helping underdeveloped nations with their environmental health initiatives and overcoming these challenges requires worldwide collaboration and financing sources such as international health funds or climate change expenditure.
Political influence and public resistance
Effective implementation of environmental health interventions is difficult in view of political pressure and public resistance. Political objectives may interfere with environmental health regulations, therefore hindering development in many areas. Some companies such as those in the mining, fossil fuels, or industrial sectors have financial stake in undertaking activities detrimental to the surroundings. This may affect politics and lead to delays in policies, gaps or even the elimination of present laws. These companies might attempt to convince legislators to reduce environmental safeguards or postpone enforcing stricter regulations, therefore prioritising revenue and economic development over public health. Environmental health issues may become highly politicised in highly divided political environments, which complicates policy decisions. Climate change is one of the most significant natural health issues; nonetheless, it has long been the topic of debate as various political parties or interest groups support different views. This separation may lead to deadlock, therefore preventing the passage of crucial legislation meant to reduce environmental health hazards. Policies may lose their potency even after they are adopted if they are not regularly enforced or if changing administrations periodically reverse them. One further issue is popular opposition. Sometimes people battle against laws they believe will restrict their freedom or negatively affect their money. Companies, labour organisations, and communities fearing job loss or higher living expenses, for example, might object to legislation taxing carbon or restricting industrial emissions. Certain groups or individuals may also minimise the health hazards associated with environmental issues such as air pollution or chemical exposure, therefore reducing the likelihood of support for environmental health regulations. We must educate people, speak openly, and create laws that the pubic finds reasonable if we are to overcome this resistance.
Lack of public awareness and education
A lot of people might not fully understand how natural factors affect health, which could mean that the public doesn't back laws that are needed. For instance, people might not know the long-term effects on their health of breathing in dirty air, drinking water that isn't clean, or being around dangerous chemicals. People might not see how important it is for policymakers to take action to lower these risks if they don't fully understand how external factors affect their health. A lot of the time, efforts or training programs that raise knowledge of environmental health problems are not properly funded or pushed. If people aren't taught about the health risks of the environment, they might not ask their governments for stricter rules, and lawmakers might not put environmental health issues at the top of their lists of priorities. It can be hard to make people more aware of environmental health problems in places like rural areas or poor countries where they aren't as obvious. In addition, public health instruction isn't always a part of neighbourhood or school activities. If kids don't learn about the value of environmental health from a young age, they might not be able to make smart choices when they vote on laws or start doing things that are better for the environment. Governments and support groups need to put money into educating the public by making materials and campaigns that are easy for everyone to understand that show how damage to the environment can lead to health problems. To raise knowledge, specific steps need to be taken to involve communities, make environmental health risks information easy to find, and boost trust in scientific study. It's also important for public health efforts to make the benefits of environmental health policies clear. For example, they should stress how avoiding health problems improves people's quality of life and saves money in the long run.
Conflicting policy priorities
Environmental health projects are often hard to carry out because governmental goals aren't always in line with each other. It can be hard for governments to decide what is most important for natural health when different areas have competing needs, like national security, economic growth, and healthcare. Many times, lawmakers are torn between the need to protect public health and the need to help the economy grow, create jobs, and advance industries. For instance, rules that limit pollution from factories or power plants might be seen as too much for industries that help the economy grow. This could lead to opposition from business groups or local governments that depend on these industries. The fight between economic growth and natural health is even stronger in new countries. Many countries that don't have a lot of money put short-term economic growth, like industrialisation or expanding infrastructure, ahead of long-term environmental protection. As people try to make more money, they might not care about how pollution, bad waste management, or cutting down trees affect the health of the environment. Even though these countries usually know they need environmental health policies, they might find it hard to put them in place because they also need to focus on things like economic growth, reducing poverty, and building up their infrastructure. There are also times when different countries have different policy objectives. For instance, natural health rules, industry growth goals, and foreign trade deals may not always agree with each other. Some countries may put trade liberalisation and economic success ahead of strict health and environmental standards because they are afraid that strict rules will make it harder to trade or invest. This makes things difficult in global environmental health government, where combining public health with economic growth often needs a lot of complicated talks and deals.
Effectiveness of Environmental Health Policies
Health outcomes related to environmental health policies
Environmental health strategies can be judged by how well they affect public health in both direct and indirect ways. Health can get a lot better when policies are put in place to lower environmental risks like climate change, pollution of the air and water, and exposure to dangerous chemicals. For instance, rules that make factories and transportation systems put out less pollution can lower the number of people who get lung diseases like asthma, bronchitis, and chronic obstructive pulmonary disease (COPD), which are highly connected to bad air quality. In places where air pollution has gone down a lot, like parts of Europe and the U.S., lung illnesses have gone down and life expectancy has gone up overall. Also, measures that improve water quality and cleanliness can lower the number of diseases that are spread by water, like cholera, diarrhoea, and typhoid fever. GI diseases can be greatly reduced by properly handling trash and controlling chemical contaminants in water. This is especially true in low-income countries where getting clean water is still hard. Climate policies that deal with heatwaves, flooding, and diseases spread by insects can also stop heat-related illnesses, heart diseases, and the spread of diseases like dengue and malaria. For example, places like New York and Paris that have heat action plans have seen fewer deaths from heatstroke and fewer people being admitted to the hospital during times of high heat. Policies that support green areas and environmentally friendly city planning can enhance mental health by creating places where people can be active and socialise, thereby lowering the number of mental health problems connected to living in cities and stress.
Case studies and real-world examples
Case studies from different countries can teach us a lot about how well environmental health policies work to solve public health problems. While the Clean Air Act in the US is one of the most well-known examples, air pollution levels have dropped dramatically since it was signed into law in 1970. Many people say that the act stopped hundreds of thousands of early deaths and millions of cases of lung illnesses. For instance, studies by the EPA revealed that the Clean Air Act annually saves around 230,000 lives and improves air quality. It has also spared many from needing to visit a hospital. By use of Clean Air Zones in cities like London, the UK has been able to reduce air pollution and enhance public health. Clear decrease in asthma-related hospital visits results from these zones reducing harmful pollution from vehicles and trucks. In order to further pollution management, the UK additionally established the Air Quality Guidelines Regulations This has helped to match the air's quality with EU recommendations. The success of these programs indicates that guidelines aimed to enhance the surroundings might have positive impact on health. An additional significant case study is Sweden's Climate Act. It has enabled the nation to make significant progress towards environmental protection and reduction of carbon footprint. The pledge of the Swedish government to accomplish net-zero pollution by 2045 has hastened the evolution of sustainable city design, renewable energy, and green transportation. Lower rates of pulmonary and cardiovascular diseases demonstrate how directly these policies have reduced pollution and improved public health. Not so in India, where affairs are more challenging. The nation boasts some of the worst air quality worldwide; hence even if certain things have improved, air pollution remains a major threat for public health. Programs like the National Clean Air Program, however, aim to improve monitoring systems, ensure emissions satisfy criteria, and promote the use of greener energy sources, thereby cleansing the air in 102 regions.
Analysis of successes and failures in policy implementation
Depending on several elements, including political will, economic resources, public support, and the capacity to ensure regulations are followed, environmental health programs may either succeed or fail. When all of these elements come together, environmental health policy may have major positive impact on public health. In the United States, for instance, many see the Clean Air Act as a triumph. In significant regions, it has reduced air pollution by more than 70 % which has actual health consequences including a decline in lung and heart ailments. The legislation was effective as it established a comprehensive controlling system, robust enforcement policies, and a long-term objective to improve the air quality. Similarly, via cleaner air, reduced number of pollution-related ailments, and more stable environment, Sweden's Climate Act and Denmark's initiatives to minimise carbon emissions have enhanced public health. A strong government resolve, general understanding, and a desire to spend in green technologies all back up these policies. But some policies have had trouble being put into place and working as planned. Even though India started the National Clean Air Program, air pollution levels in its biggest towns are still very bad, killing thousands of people every year. This failure is because regulation is weak, tracking isn't good enough, and polluting businesses have a lot of economic and political power. Also, environmental rules haven't always been put ahead of economic growth, which has caused problems between progress and the health of the environment.
RESULTS AND DISCUSSION
This comparison of environmental health policies in different healthcare systems shows big differences in how policies are made and how they are put into place. Environmental health issues are usually better taken care of in countries with public healthcare systems, like Scandinavia and the UK. This is because these countries have centralised government, funds, and effective laws. For instance, the Clean Air Zones in the UK and the Climate Act in Sweden have made the air quality and general health better in a measured way. But in places like the U.S. where public services have been privatised, environmental health laws are often weaker because of political opposition and pressure from businesses. Even though there are problems, programs like the U.S. Clean Air Act and India's National Clean Air Programme show that big steps can be taken with strong rules and public education.
|
Table 2. Environmental Health Policy Effectiveness Evaluation |
||||
|
Country |
Policy Enforcement (%) |
Public Health Improvement (%) |
Economic Investment (USD billion) |
Environmental Health Risk Reduction (%) |
|
USA |
72 |
66 |
2,5 |
10 |
|
UK |
80 |
90 |
4 |
15 |
|
Sweden |
94 |
89 |
5,5 |
20 |
|
India |
64 |
56 |
1 |
5 |
The table 2 shows how well environmental health policies in four countries—the USA, the UK, Sweden, and India—are doing in four main areas: enforcing policies, improving public health, attracting investments, and lowering environmental health risks. The USA does not do very well at enforcing policies (72 % of the time) or improving public health (66 % of the time). This suggests that there are policies, but they are not always followed or have a big effect. The $2,5 billion economic investment is less than what other countries have done, which shows that there isn't enough money for environmental health programs. Figure 3 shows how much money different countries spend on health care.
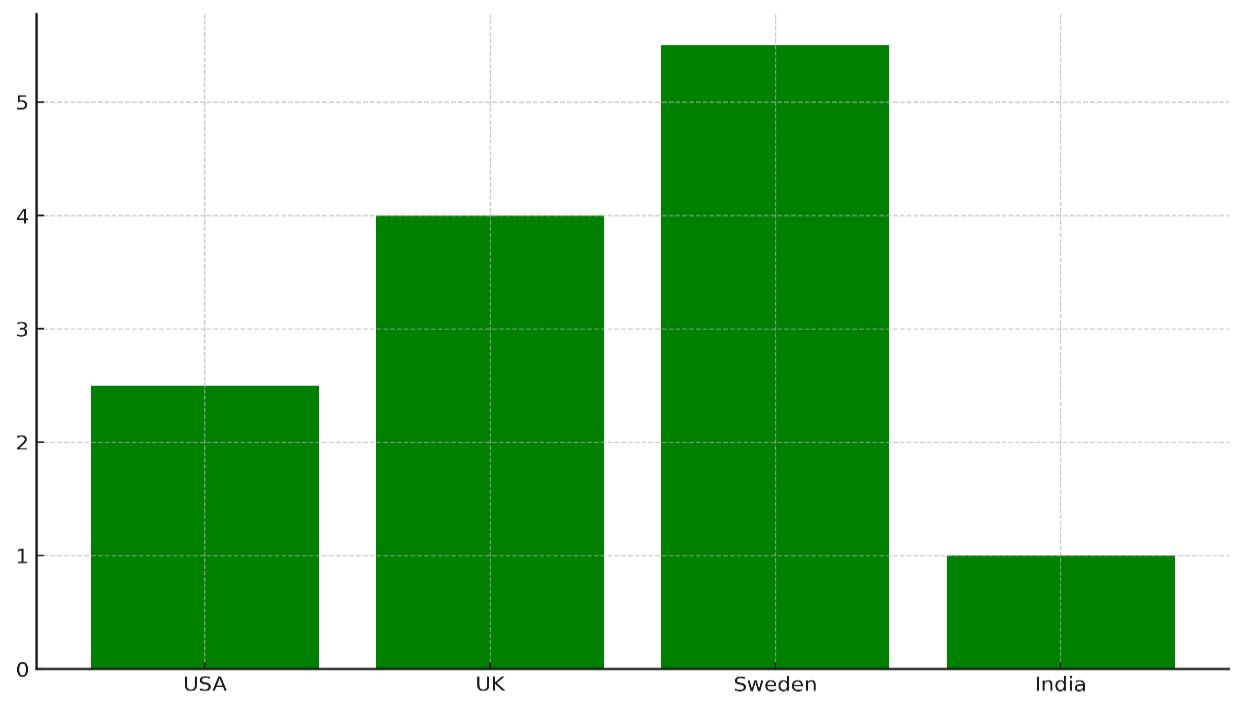
Figure 3. Economic Investment by Country
The environmental health risk has gone down by 10 %, which means that these measures have made a small positive impact on public health. The UK has a better level of policy compliance (80 %) and a major change in public health (90 %), which shows that the government is more committed to putting in place effective environmental health measures. Figure 4 shows how policy execution and gains in public health have changed over time.
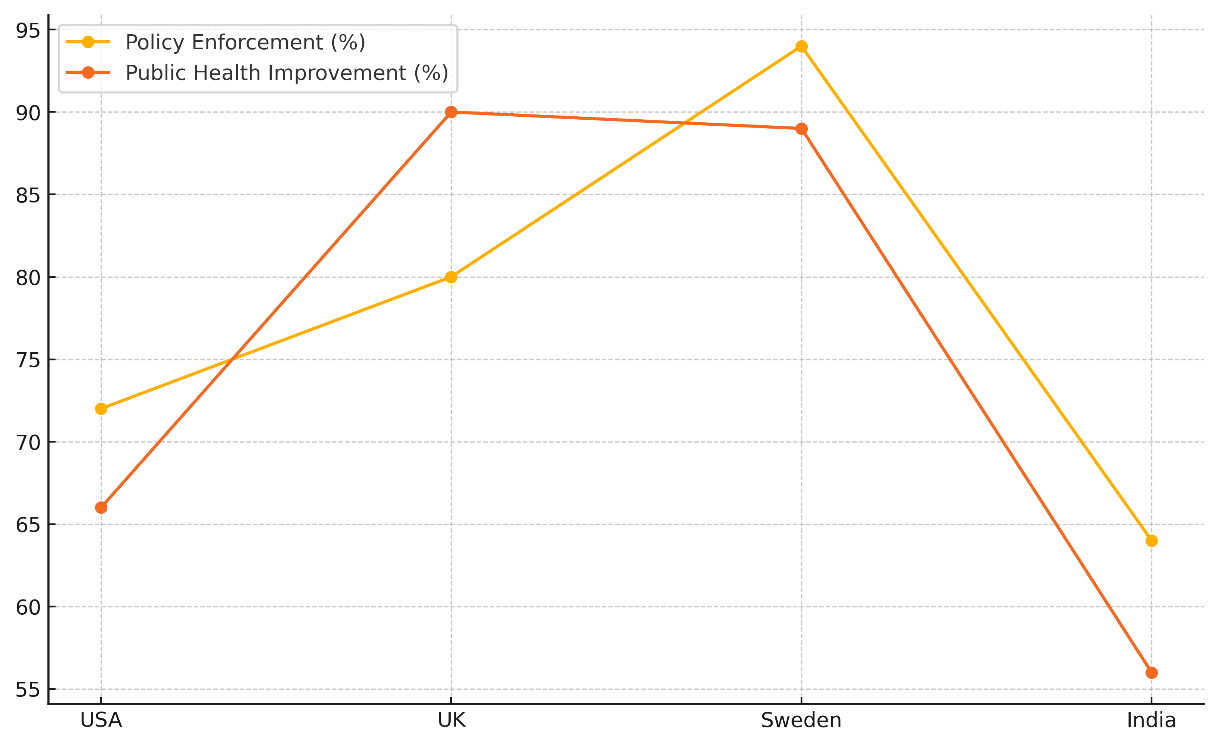
Figure 4. Policy Enforcement and Public Health Improvement Trends
An economic investment of $4 billion will fund broad environmental projects that will lower health risks in the environment by 15 %. Sweden has the best policy implementation (94 %), and its public health has improved the most (89 %). This shows that its policies are well-integrated and are being followed. With Sweden's $5,5 billion funding, big efforts are supported, and natural health risks are cut by 20 %.
|
Table 3. Additional Evaluation Parameters |
||||
|
Country |
Air Quality Improvement (%) |
Reduction in Respiratory Diseases (%) |
Public Support for Policies (%) |
Climate Adaptation Policies (%) |
|
USA |
15 |
10 |
66 |
72 |
|
UK |
20 |
15 |
80 |
92 |
|
Sweden |
25 |
18 |
90 |
87 |
|
India |
10 |
7 |
53 |
60 |
Figure 3 shows more ways to judge environmental health policies. It focusses on how to improve air quality, lower the number of lung diseases, get people to support policies, and look at climate resilience policies in the US, UK, Sweden, and India. The United States has made some progress, with the air quality getting better by 15 % and the number of lung diseases going down by 10 %. Figure 5 shows how the air quality has gotten better over time in different countries.
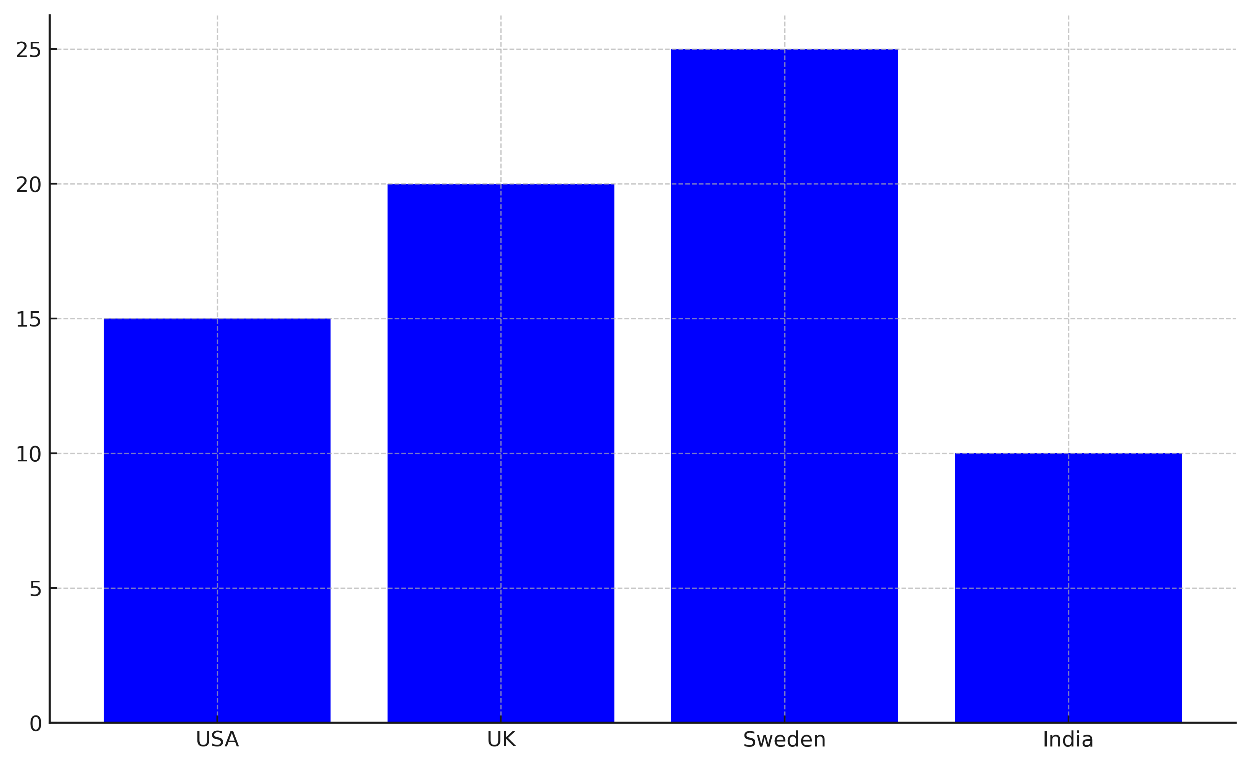
Figure 5. Air Quality Improvement by Country
But only 66 % of people support environmental health policies. This means that even though the policies work somewhat, they don't have much support from the public. At 72 %, climate resilience strategies are pretty strong, which means that steps are being taken to deal with health risks linked to climate change. With a 20 % improvement in air quality and a 15 % drop in lung diseases, the UK has done a great job. At 80 %, public support is higher, showing that most people agree with environmental measures. The UK also has great strategies for adapting to climate change (92 %), which shows that they are taking a complete approach to reducing the health effects of climate change. Sweden does better than the others because the air quality has improved by 25 % and the number of lung diseases has dropped by 18 %. Support from the public is high (90 %), and plans for adapting to climate change are strong (87 %). Figure 6 shows how policies have affected public health in different countries over time.
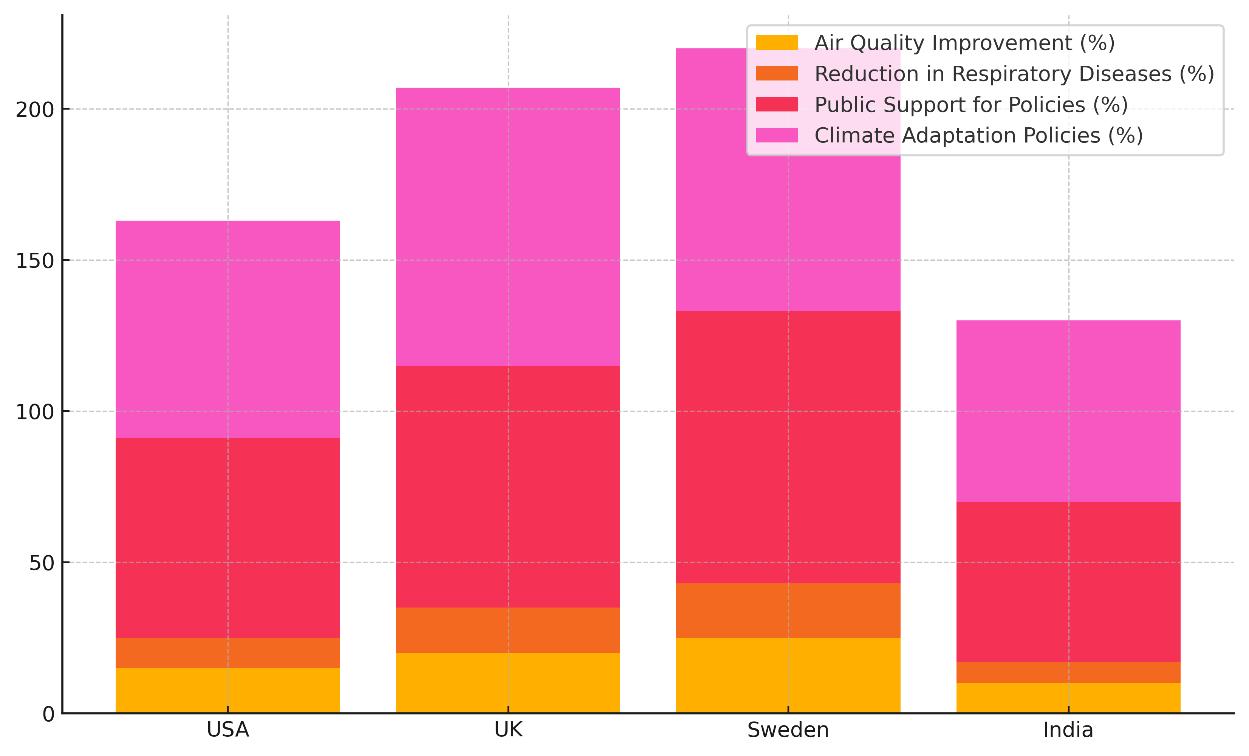
Figure 6. Cumulative Policy Impacts by Country
This shows that Sweden is a leader in incorporating environmental health into public policy. India has the worst scores in every category. They have a lot of problems, like poorer air quality (10 %), fewer lung diseases (7 %), and not much public support (53 %). These problems are made worse by problems with resources and putting them into action.
CONCLUSIONS
Policies about environmental health are very important for keeping people healthy and encouraging sustainability. This study shows how healthcare systems whether they are public, private, or a mix of the two affect how well these strategies work. Environmental health has been handled more comprehensively and orderly in public healthcare systems in the UK and Scandinavians. This is primarily due to government intervention that has included environmental concerns into medical procedures. These systems better enforce laws, promote preventive actions, and ensure that everyone has equitable access to environmental health advantages. They also concentrate on long-term health outcomes. Conversely, privatised systems such as the United States struggle to implement sensible environmental health measures because to split governance, polarised politics, and resistance from strong industries. Laws like the Clean Air Act have helped to improve air quality; yet, greater progress is difficult to achieve as the private sector has great influence and national policy is not uniform. This research emphasises among other things how crucial political will, financial resources, and public involvement are for implementing programs that have results. Even in rich nations with first-rate healthcare systems, the political and financial might of companies harming the environment might impede advancement. Also, public opposition and ignorance are still big problems that make it hard for policies to work. To get past these problems, we need to work together internationally and share the best ways to do things. Countries that want to improve public health can learn a lot from global structures like the Paris Agreement and the World Health Organization's recommendations. Countries can make better and longer-lasting environmental health policies by putting the health effects of environmental problems at the top of their lists, boosting teamwork across sectors, and making sure everyone has equal access to healthcare and environmental laws.
BIBLIOGRAPHIC REFERENCES
1. Küster, A.; Adler, N. Pharmaceuticals in the environment: Scientific evidence of risks and its regulation. Philos. Trans. R. Soc. B 2014, 369, 20130587.
2. Swan, G.; Naidoo, V.; Cuthbert, R.; Green, R.E.; Pain, D.J.; Swarup, D.; Prakash, V.; Taggart, M.; Bekker, L.; Das, D.; et al. Removing the Threat of Diclofenac to Critically Endangered Asian Vultures. PLoS Biol. 2006, 4, e66.
3. Nash, J.P.; Kime, D.E.; Van Der Ven, L.T.M.; Wester, P.W.; Brion, F.; Maack, G.; Stahlschmidt-Allner, P.; Tyler, C.R. Long-term exposure to environmental concentrations of the pharmaceutical ethynylestradiol causes reproductive failure in fish. Environ. Health Perspect. 2004, 112, 1725–1733.
4. Ebert, I.; Bachmann, J.; Kühnen, U.; Küster, A.; Kussatz, C.; Maletzki, D.; Schlüter, C. Toxicity of the Fluoroquinolone Antibiotics Enrofloxacin and Ciprofloxacin to Photoautotrophic Aquatic Organisms. Environ. Toxicol. Chem. 2011, 30, 2786–2792.
5. Brausch, J.M.; Connors, K.A.; Brooks, B.W.; Rand, G.M. Human pharmaceuticals in the aquatic environment: A review of recent toxicological studies and considerations for toxicity testing. Rev. Environ. Contam. Toxicol. 2012, 218, 1–99.
6. Richmond, E.K.; Rosi, E.J.; Reisinger, A.J.; Hanrahan, B.R.; Thompson, R.M.; Grace, M.R. Influences of the antidepressant fluoxetine on stream ecosystem function and aquatic insect emergence at environmentally realistic concentrations. J. Freshw. Ecol. 2019, 34, 513–531.
7. Richmond, E.K.; Rosi, E.J.; Walters, D.M.; Fick, J.; Hamilton, S.K.; Brodin, T.; Sundelin, A.; Grace, M.R. A diverse suite of pharmaceuticals contaminates stream and riparian food webs. Nat. Commun. 2018, 9, 1–9.
8. Bexfield, L.M.; Toccalino, P.L.; Belitz, K.; Foreman, W.T.; Furlong, E.T. Hormones and pharmaceuticals in groundwater used as a source of drinking water across the United States. Environ. Sci. Technol. 2019, 53, 2950–2960.
9. C. R. Das. (2015). Social Forestry in Odisha: An Extraordinary International Aided Initiative Towards Revival and Restoration of Forests.. International Journal on Research and Development - A Management Review, 4(2), 28 - 49.
10. P. Raja Babu. (2015). Global Financial Inclusion: Challenges and Opportunities. International Journal on Research and Development - A Management Review, 4(2), 50 - 52.
11. Njoku, A.; Joseph, M.; Felix, R. Changing the Narrative: Structural Barriers and Racial and Ethnic Inequities in COVID-19 Vaccination. Int. J. Environ. Res. Public Health 2021, 18, 9904.
12. Kenny, C.; Priyadarshini, A. Review of current healthcare waste management methods and their effect on global health. Healthcare 2021, 9, 284.
13. Shannon, A.L.; Woolridge, A. Medical waste. Waste 2011, 329–339.
14. Goodman, D.; Arisco, N.; Jaacks, L.M. Synthetic Chemical Trade as a Potential Driver of Global Health Disparities and Data Gaps on Synthetic Chemicals in Vulnerable Populations. Curr. Environ. Health Rep. 2020, 7, 1–12.
15. Schwartz, H.; Marushka, L.; Chan, H.M.; Batal, M.; Sadik, T.; Ing, A.; Fediuk, K.; Tikhonov, C. Pharmaceuticals in source waters of 95 First Nations in Canada. Can. J. Public Health 2021, 112, 133–153.
FINANCING
The authors did not receive financing for the development of this research.
CONFLICT OF INTEREST
The authors declare that there is no conflict of interest.
AUTHORSHIP CONTRIBUTION
Data curation: Abhijeet Nashte, Shankar Lal Soni, Manashree Mane, Sudesh Sangwan, Rajendra Prasad Satapathy.
Formal analysis: Abhijeet Nashte, Shankar Lal Soni, Manashree Mane, Sudesh Sangwan, Rajendra Prasad Satapathy.
Methodology: Abhijeet Nashte, Shankar Lal Soni, Manashree Mane, Sudesh Sangwan, Rajendra Prasad Satapathy.
Supervision: Abhijeet Nashte, Shankar Lal Soni, Manashree Mane, Sudesh Sangwan, Rajendra Prasad Satapathy.
Drafting - original draft: Abhijeet Nashte, Shankar Lal Soni, Manashree Mane, Sudesh Sangwan, Rajendra Prasad Satapathy.
Writing - proofreading and editing: Abhijeet Nashte, Shankar Lal Soni, Manashree Mane, Sudesh Sangwan, Rajendra Prasad Satapathy.