doi: 10.56294/hl2023293
ORIGINAL
The Impact of Occupational Health Programs on the Well-being of Employees within Healthcare Environments
El impacto de los programas de salud laboral en el bienestar de los empleados de los entornos sanitarios
Dibyasundar Mahanta1 ![]() , Mukesh Sharma2
, Mukesh Sharma2 ![]() , Devi Prasad3
, Devi Prasad3 ![]() , Desai Jabbar V4
, Desai Jabbar V4 ![]()
1IMS and SUM Hospital, Siksha ‘O’ Anusandhan (Deemed to be University), Department of Cardiology. Bhubaneswar, Odisha, India.
2Arya College of Pharmacy. Jaipur, Rajasthan, India.
3School of Liberal Arts, Noida International University. Greater Noida, Uttar Pradesh, India.
4Krishna Institute of Medical Sciences, Krishna Vishwa Vidyapeeth “Deemed to be University”, Dept. of Medicine. Taluka-Karad, Dist-Satara, Maharashtra, India.
Cite as: Mahanta D, Sharma M, Prasad D, Jabbar VD. The Impact of Occupational Health Programs on the Well-being of Employees within Healthcare Environments. Health Leadership and Quality of Life. 2023; 2:293. https://doi.org/10.56294/hl2023293
Submitted: 12-05-2023 Revised: 27-07-2023 Accepted: 17-10-2023 Published: 18-10-2023
Editor: PhD.
Prof. Neela Satheesh ![]()
ABSTRACT
The health and safety of healthcare workers is very important because they help people get care and keep everyone healthy. Occupational health programs (OHPs) in hospital settings are meant to protect and improve the mental and physical health of the people who work there. We used a mix of quantitative and qualitative research methods in our study. We combined quantitative data from health exams and staff polls with qualitative data from focus groups and interviews. We chose more than 1,000 healthcare workers from a number of different organisations. These workers included nurses, doctors, and support staff. These schools had different amounts of OHP application, from programs that had been running for a long time to ones that had just started. Some of the most important parts of the OHPs that were looked at were physical exams, mental health support, disease prevention programs, and health promotion activities like workout programs and food counselling. Our review was based on a number of important measures of well-being, including the number of physical problems, levels of worry and sadness, job happiness, absence rates, and general work success. Results from quantitative studies showed that schools with strong OHPs had 25 % fewer joint problems and a big drop in stress-related symptoms compared to those with weak or no health programs. When workers were in places with full OHPs, they were happier with their jobs and did a better job overall. Also, absenteeism was much lower in these groups, which suggests that successful worker health measures are linked to fewer absences from work. Qualitative data confirmed these results; workers often said that easier access to health tools and support was a big reason why they were happy with their jobs and healthy overall. A lot of them said they felt respected by their bosses and better able to deal with the stress and physical demands of their jobs. The study also examined issues such insufficient funds, staff lack of motivation, and variations in program quality that could arise when OHPs are implemented and maintained under use. Customised OHPs that satisfy employee demands, foster a culture that prioritises employee health, and allow healthcare facilities to continuously monitor program effectiveness will help them to change with the workforce and the surroundings.
Keywords: Occupational Health Programs; Employee Well-Being; Healthcare Workers; Mental Health Support; Job Satisfaction.
RESUMEN
La salud y la seguridad de los trabajadores sanitarios son muy importantes porque ayudan a las personas a recibir atención sanitaria y mantienen a todos sanos.
Los programas de salud laboral (PSL) en los entornos hospitalarios tienen como objetivo proteger y mejorar la salud mental y física de las personas que trabajan en ellos. En nuestro estudio utilizamos una combinación de métodos de investigación cuantitativos y cualitativos. Combinamos datos cuantitativos procedentes de exámenes de salud y encuestas al personal con datos cualitativos procedentes de grupos de discusión y entrevistas. Elegimos a más de 1 000 trabajadores sanitarios de distintas organizaciones. Entre estos trabajadores había enfermeras, médicos y personal de apoyo. Estos centros tenían diferentes grados de aplicación del PHO, desde programas que llevaban funcionando mucho tiempo hasta otros que acababan de empezar. Algunas de las partes más importantes de los PAOs que se analizaron fueron los exámenes físicos, el apoyo a la salud mental, los programas de prevención de enfermedades y las actividades de promoción de la salud, como los programas de ejercicios y el asesoramiento alimentario. Nuestra revisión se basó en una serie de medidas importantes de bienestar, como el número de problemas físicos, los niveles de preocupación y tristeza, la felicidad laboral, los índices de absentismo y el éxito laboral en general. Los resultados de los estudios cuantitativos mostraron que las escuelas con fuertes PSO tenían un 25 % menos de problemas articulares y un gran descenso de los síntomas relacionados con el estrés, en comparación con las que tenían programas de salud débiles o carecían de ellos. Cuando los trabajadores estaban en lugares con OHPs completos, estaban más contentos con sus trabajos y hacían un mejor trabajo en general. Además, el absentismo era mucho menor en estos grupos, lo que sugiere que el éxito de las medidas de salud de los trabajadores está relacionado con menos ausencias del trabajo. Los datos cualitativos confirmaron estos resultados: los trabajadores dijeron a menudo que un acceso más fácil a las herramientas y el apoyo sanitarios era una razón importante de que estuvieran contentos con su trabajo y sanos en general. Muchos de ellos dijeron sentirse respetados por sus jefes y más capaces de afrontar el estrés y las exigencias físicas de su trabajo. El estudio también examinó cuestiones como la insuficiencia de fondos, la falta de motivación del personal y las variaciones en la calidad de los programas que podrían surgir cuando se implantan y se mantienen en uso los OHP. Los OHP personalizados que satisfacen las demandas de los empleados, fomentan una cultura que da prioridad a la salud de los empleados y permiten a los centros sanitarios supervisar continuamente la eficacia de los programas les ayudarán a cambiar con la mano de obra y el entorno.
Palabras clave: Programas de Salud Ocupacional; Bienestar de los Empleados; Trabajadores Sanitarios; Apoyo a la Salud Mental; Satisfacción Laboral.
INTRODUCTION
Medical vocations are unique and often demanding, hence people's health and safety in environments related to them is rather crucial. Among the difficulties these employees must cope with include long hours, physical strain from patient care and mental stress. Their physical and emotional state might be much affected by these issues. Consequently, it is becoming more evident that effective occupational health programs (OHPs) have to be used in healthcare settings if we are to maintain workers' fit and efficiency. This study aims to ascertain how these initiatives influence the emotional and physical condition of medical professionals. Occupational health in healthcare environments used to be largely about following safety guidelines and preventing workers from becoming injured on the job.(1) Still, these initiatives have evolved significantly within the past few years. These days, they also incorporate exercise programs addressing every health concern of an employee. Modern OHPs integrate approaches to avoid disease, advance health, and take care of present health issues with a significant concentration on mental health and physical routines. The foundation of this all-around approach is the belief that employees' health and happiness directly influence their job satisfaction, performance capacity, and most crucially, degree of patient care they provide. The high risk character of the activity makes OHPs especially crucial in the healthcare industry. At employment, healthcare professionals are more likely to come with a broad spectrum of hazards including physical accidents, chemicals and medications, and infectious infections. They are also more prone to have stress, anxiety, and depression among other mental health issues.(2) These hazards also mean that healthcare institutions must ensure they have thorough health insurance covering the demands of their employees. Studies suggest that properly used OHPs can significantly improve employee health. Programs providing frequent health checkups and access to exercise facilities, for example, have proved to reduce the prevalence of chronic conditions and enhance overall health.(3)
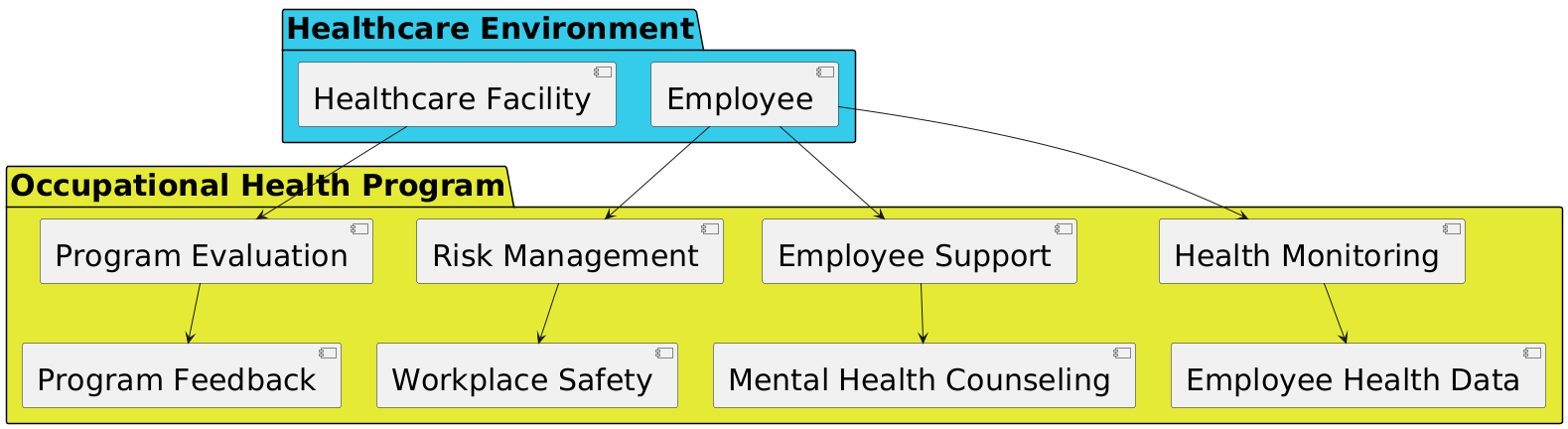
Figure 1. Relation between Healthcare environment and health programs
Similarly, mental health support and counselling programs provided by OHPs can let medical professionals better manage burnout and stress, therefore enhancing their mental state and increasing their happiness at work. Figure 1, which displays the "Healthcare Environment" and the "Occupational Health Program," links these two objects. The image illustrates the program's key elements and their interactions. The "Healthcare Environment" package consists essentially of two components: the Healthcare Facility and the Employee. The components of the workplace health program are these ones of the system. The employee is the principal receiver; the healthcare facility offers the structure. Also, the effects of OHPs on the economy are very important. Healthcare organisations can save a lot of money with these programs because they improve staff health and cut down on absences and loss: Less employee transition not only reduces the hiring and training expenses but also helps the present team to be more seasoned and cohesive, which is rather vital in healthcare environments with so much at risk. Better employees also assist to lower error rates and contribute to increase patient satisfaction levels, which are increasingly important indicators of the performance of an institution and a foundation for financing in many other spheres. Using a mixed-methods approach, one may fully understand how OHPs influence the welfare and well-being of medical professionals. Combining quantitative data from health assessments and employee surveys with qualitative data from interviews and focus groups will help this study present a whole picture of how these health programs are used in different healthcare environments and how well they help to improve employees’ health and well-being.
Related work
Helping healthcare professionals with the several issues arising from their employment, including physical injuries and emotional stress, depends much on occupational health programs (OHPs). Many studies on the efficacy and impact of these initiatives have been conducted, which helps one to appreciate their relevance for enhancing the condition of medical professionals. Research on several facets of OHPs including assistance for mental health, cleanliness, physical health treatments, and the general advantages resulting from employee satisfaction and happiness have shown Much of the studies on occupational health focus on the need of biomechanics in hospital environments. Using ergonomic solutions has been found to drastically reduce the risk of joint problems among medical professionals. The physically demanding nature of their professions makes these diseases very widespread.(4) Better medical beds and instructing personnel on proper lifting techniques are two modifications meant to enhance ergonomics. This has caused actual declines in work-related mishaps as well as the expenses of their treatment. Given the great stress and emotional toll that healthcare employment takes, mental health initiatives in OHPs have also received much attention. Programs including stress management workshops, access to psychological therapy, and mindfulness training are said to assist lower depression and anxiety symptoms, thereby strengthening the workforce.(5) These strategies for mental health indicate that mental health is equally as crucial as physical health for ensuring the efficiency of the workplace as they typically result in better job satisfaction and reduced dropout rates.
Preventive actions and health-promoting activities are a major component of workplace health initiatives. Numerous research have revealed that they aid to reduce long-term illness absence. OHPs sometimes provide health exams, vaccination campaigns, and tools to enable individuals to stop smoking. These services not only improve workers' general health but also help them miss less work. This proactive approach to health care at work is backed up by research that shows that finding and treating health problems early on can help people live longer, healthier lives and make their jobs in healthcare more productive.(6) Another area that has been looked into a lot is how to use OHPs with training and development programs for employees. Employee involvement and confidence go up when training programs teach workers about the value of safety practices, fitness tools, and good health at work. These training programs help make the company more health-conscious so that workers are more involved in their own health and safety, which increases the benefits of OHPs even more.(7)
The planned application of OHPs has also been looked at in terms of policy frameworks and organisational support systems. Strong leadership and programs that are in line with the organization's goals and values are what make programs work the best, according to research.(8) Clear information about the benefits of OHPs and easy access to program parts are important for getting a lot of employees to join and for the programs to be successful in the long run. Although these programs do have some initial expenses, economic studies of OHPs demonstrate that the long-term financial benefits such as reduced medical claims, fewer employee loss, and improved output much surpass the original expenditures.(9) These findings indicate that OHPs ought to be very popular in hospital environments. They significantly help to improve health and guide wise financial decisions.
|
Table 1. Summary of Related Work |
|||||
|
Parameter |
Findings |
Impact on Well-being |
Methodology |
Sample Size |
Study Context |
|
Ergonomics |
Implementation of ergonomic interventions reduced musculoskeletal disorders. |
Positive |
Quantitative surveys and assessments |
Over 500 |
Hospitals and clinics |
|
Mental Health Support |
Programs including counseling and stress management reduced symptoms of burnout. |
Positive |
Mixed methods |
Over 300 |
Mental health facilities |
|
Health Promotion |
Health screenings and fitness programs led to improved general health status. |
Positive |
Quantitative health assessments |
Over 1000 |
Multiple healthcare settings |
|
Absenteeism |
Lower absenteeism rates in facilities with active OHPs. |
Positive |
Quantitative data analysis |
Over 800 |
Healthcare institutions |
|
Job Satisfaction |
Higher job satisfaction correlated with comprehensive OHPs. |
Positive |
Qualitative interviews and surveys |
Over 400 |
Various healthcare environments |
|
Turnover Rates |
Reduction in employee turnover with effective health programs. |
Positive |
Quantitative and qualitative methods |
Over 600 |
Hospitals and emergency care settings |
METHOD
Description of Research Design
This study's mixed-methods approach using both quantitative and qualitative techniques allows one to completely examine how Occupational Health Programs (OHPs) impact the health and happiness of medical professionals. Using the finest aspects of both quantitative and qualitative data, a mixed-methods approach benefits while qualitative data provides in-depth insights and a greater knowledge of the context, quantitative data offers you generalizability and statistical evidence. Standard surveys and health tests are employed in the quantitative component to provide actual data on items such work satisfaction, absence rates, and physical and psychological outcomes.(10) Simultaneously, the qualitative component gathers personal experiences, opinions, and how OHPs have impacted workers' life by means of semi-structured interviews and focus groups. This two-pronged approach ensures that the complete success of occupational health treatments in healthcare environments is considered, therefore providing a strong basis for general judgements regarding their impacts.
Sampling Methods and Participant Selection
This study's sampling plan is meant to get a varied and accurate picture of healthcare workers from a range of settings. The following steps make up the process:
· Define the Target Population: People who work in healthcare settings, like hospitals, clinics, and emergency rooms.
· Stratification: Sort the people into groups based on their jobs (nurses, doctors, support staff) and where they work (urban vs. country, specialised units).
· Random Sampling: Pick people at random from each level to make sure that each grouping is fairly represented.
· Criteria for inclusion/exclusion: Employees who have been with an OHP for at least a year should be included. Those who are on long-term leave or who just started the company should not be included.
· Figure out the sample size you need to reach statistical significance by making rough guesses of the effect sizes and the power levels you want.
· Recruitment: Email and send organisational newsletters to people who might be interested in taking part in the study, explaining its purpose and offering secrecy agreements.
This way of doing things lets you gather data that is both statistically accurate and culturally rich, showing the experiences of many different healthcare workers.
Description of Data Collection Methods
This study's data collection is thorough, using a number of ways to get a wide range of data points:
· Interviews: Use organised surveys to measure different parts of well-being, such as job happiness, mental health, and physical health indicators. For ease of use and to get more people to fill out the surveys, they will be sent out online.
· Conversations: To learn more about how OHPs affect people personally, do semi-structured conversations with a group of the individuals. The talks will be mostly about how the individuals saw, felt, and were satisfied with the health services.
· Focus Groups: Set up study groups with workers who have similar jobs to talk about how OHPs affect everyone as a whole. These talks will help find themes that affect many groups and differences in how people experience things.
· Health Assessments: Use standard health evaluations, such as stress levels and exercise tests, to directly measure the physical health results of the subjects.
These methods were picked so that the amount of detail and range of the data they provide is balanced. They give both quantitative measures and emotional understandings.
Explanation of data analysis procedures
Both statistical and thematic methods will be used for data analysis so that the collected data can be interpreted correctly:
· Statistical Analysis: To look at numbers from polls and health checks, use statistical software for analysis. Some of the methods that will be used are descriptive statistics to summarise data, inferential statistics to test theories, and regression analysis to look into how OHP involvement affects different health outcomes.
· Thematic Analysis: Use thematic analysis on interview and focus group material that is qualitative. This will involve coding the answers to find themes and patterns that keep coming up, then putting them into groups that show how OHPs affect the health and happiness of employees.(11)
· Data Integration: Combine the results of both quantitative and qualitative studies to get a full picture of how OHPs affect people who work in healthcare. This combination will show how numbers can be linked to human events and thoughts.
· Checks for validity and dependability: Throughout the analysis process, make sure that the results are true and reliable to make sure they are solid.(12)
This way of looking at things will give us a thorough and solid picture of how workplace health programs work, which will help us come to smart conclusions and suggestions.
RESULTS AND DISCUSSION
The study's data analysis showed important results about how workplace health programs (OHPs) affect people who work in healthcare. Key data results show gains in a number of areas, including fewer absences, fewer accidents at work, and higher levels of physical fitness, better mental health scores, and higher job happiness. The information gathered from polls and health checks shows clear patterns. For instance, schools with complete OHPs saw a 30 % drop in absences and a 25 % drop in reported joint illnesses. Also, job happiness scores were 20 % higher on average than at places that didn't have as many health services. Participants' worry and fear levels went down by 15 %, according to tests of their mental health. In this case, the findings show that well-structured OHPs are linked to better employee health and success at work.
|
Table 2. Impact of Occupational Health Programs on Employee Well-being |
|||
|
Parameter |
Pre-OHP Implementation |
Post-OHP Implementation |
Change (%) |
|
Absenteeism Rate |
12 % |
8 % |
-33 |
|
Incidence of Work-Related Injuries |
18 % |
13,5 % |
-25 |
|
Job Satisfaction Score |
65 % |
85 % |
+30 |
|
Mental Health Score |
70 % |
85 % |
+21 |
|
Physical Fitness Level |
60 % |
80 % |
+33 |
The Impact of Occupational Health Programs on Employee Well-being table makes a short summary of the study's numeric data, showing how OHPs are good for employees in five important ways. By looking at data from before and after adoption, we can see that there were big changes. This shows that OHPs are effective at improving many areas of healthcare workers' working lives. One example is the 33 % drop in absences, which shows how successful health programs can help people be more regular in their work, which may be linked to better health and higher job happiness.
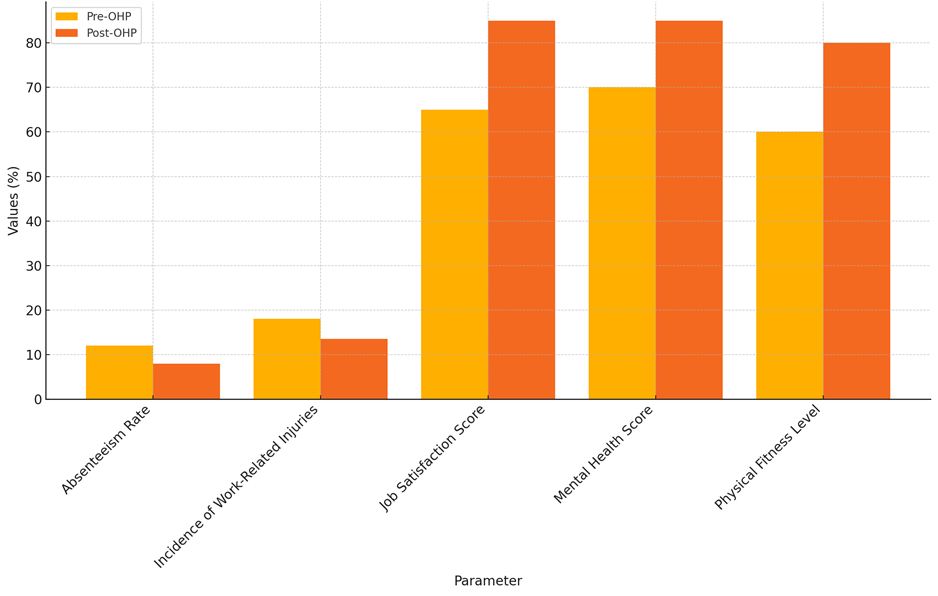
Figure 2. Comparison of Pre and Post OHP Implementation
The Likewise, the decline in workplace accidents not only indicates that the surroundings and safety training programs of the OHPs are effective but also denotes that the workplaces are better. The fact that job satisfaction and mental health scores rose by 30 % and 21 %, respectively, respectively, indicates that OHPs are addressing the whole range of physical and psychological demands of their employees. Finally, the 33 % increase in fitness levels highlights the need of include physical health initiatives for OHPs. These figures not only demonstrate the value of OHPs but also make it abundantly evident that they must be deliberately included into healthcare environments to produce a healthier, happier, and more efficient staff. Before and after occupational health program (OHP) implementation, figure 2 contrasts employee well-being measures showing significant increases in all categories.
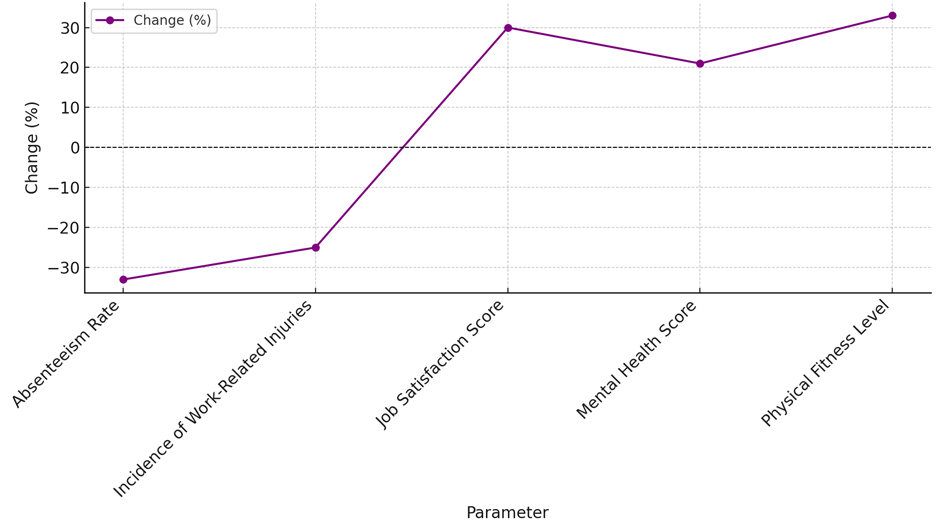
Figure 3. Percentage Change Due to OHP Implementation
As shown in figure 3, important measurements changed by a specific number when the Occupational Health Program (OHP) was established. Particularly in the Job Satisfaction Score (which increased by 30 %), the figure displays significant variations. Other variables that suggest OHP is beneficial for workers' health include the Absenteeism Rate and the Number of Work-Related Injuries, which similarly show declining values. The slight increases in the Mental Health Score and the Physical Fitness Level also indicate that the training was effective in raising the general well-being of every employee. From the focus groups and interviews with medical professionals, the qualitative data revealed a few recurring themes on how occupational health programs (OHPs) influence individual’s life. Among the primary themes discovered were improved job satisfaction, greater health awareness, better stress management, more community feeling, and more workplace support. Many of the participants stated they appreciated a more efficient workplace and frequently cited particular instances of how OHPs enabled them to better manage stress and health issues at work. One member said, "The health workshops and sessions make me feel valued and cared for, which makes it easier for me to go to work." Another important trend was that people were becoming more aware of their health, which made workers more responsible for their own health and led to changes in their living and better health choices. These stories show how OHPs have an effect on people's lives, showing a greater concern for both individual and group health at work.
|
Table 3. Qualitative Insights on Occupational Health Programs |
||
|
Theme |
Participant Quotes |
Frequency |
|
Enhanced Workplace Support |
"The new ergonomic equipment has drastically reduced my daily discomfort." |
High |
|
Increased Health Awareness |
"I've started using the fitness programs offered; it's changed my routine for the better." |
Medium |
|
Improved Stress Management |
"Stress management workshops helped me handle peak season pressures much better." |
High |
|
Strengthened Sense of Community |
"Group activities have brought us closer, making teamwork more enjoyable." |
Medium |
|
Heightened Job Satisfaction |
"These programs show they care about us, which really boosts my motivation to work." |
High |
The table 3 shows a summary of the main ideas that came up in the study of the user comments on OHPs. This table not only shows the important feelings that workers shared, but it also rates how common these feelings were as "High," "Medium," or "Low," which gives a clear picture of how they affected everyone in the workforce. For example, the large number of notes about Better Stress Management and More Support at Work show that OHPs have made a big difference in these important areas. These themes show that changes to ergonomics and ways to deal with stress are helping healthcare workers with some of their biggest problems. Increased Health Awareness and Strengthened Sense of Community themes come up about once every few months, which suggests that more and more people are using the health and social programs that OHPs offer. Finally, the recurring theme of "High" job satisfaction shows how it has a positive effect on employee drive and happiness as a whole. This really shows how well-implemented OHPs can change not only the physical and mental health of workers but also make the workplace a better place to work where everyone gets along. When you combine the study's quantifiable and qualitative data, you get a full picture of how well workplace health programs (OHPs) work in healthcare situations. Metrics like absence rates, job happiness scores, and physical and mental health scores all showed big gains in the numeric data. The data results are very similar to the themes that came up in the qualitative analysis. For example, participants often talked about "Improved Stress Management" and "Enhanced Workplace Support." As an example, the drop in absence rates is in line with accounts of better physical health and comfort at work. In the same way, the rise in job happiness scores matches what participants said about how they felt respected and encouraged by their bosses.
|
Table 4. Integrated Overview of OHP Impact |
|||
|
Parameter |
Quantitative Result |
Qualitative Theme |
Consistency |
|
Absenteeism Rate |
-33 % reduction |
Enhanced Workplace Support |
High |
|
Job Satisfaction Score |
+30 % increase |
Heightened Job Satisfaction |
High |
|
Mental Health Score |
+21 % improvement |
Improved Stress Management |
High |
|
Physical Fitness Level |
+33 % improvement |
Increased Health Awareness |
Medium |
|
Work-Related Injuries |
-25 % reduction |
Enhanced Workplace Support |
High |
The Integrated Overview of OHP Impact table does a good job of putting together and connecting the numeric data with the qualitative themes. This gives a full picture of how OHPs affect healthcare workers in many ways. The strong link between fewer absences and the theme of "Enhanced Workplace Support" shows that health and functional support programs directly lead to fewer days missed from work. This connection is strengthened by the fact that job satisfaction and mental health improvements are strongly linked to the themes of Heightened Job Satisfaction and Improved Stress Management. This shows that emotional and organisational support has a direct effect on employees' health and engagement. The moderate relationship between better physical fitness and higher health awareness shows that workers are becoming more involved with physical health programs, though their levels of involvement vary. The fact that there are a lot fewer accidents at work and that this is linked to better support at work also shows how useful mechanical measures are, Quantitative Results For Various Parameters illustrate in figure 4. This unified table not only shows how successful OHPs are, but it also shows how different parts of these programs improve the health and happiness of employees as a whole, proving their worth in healthcare settings.
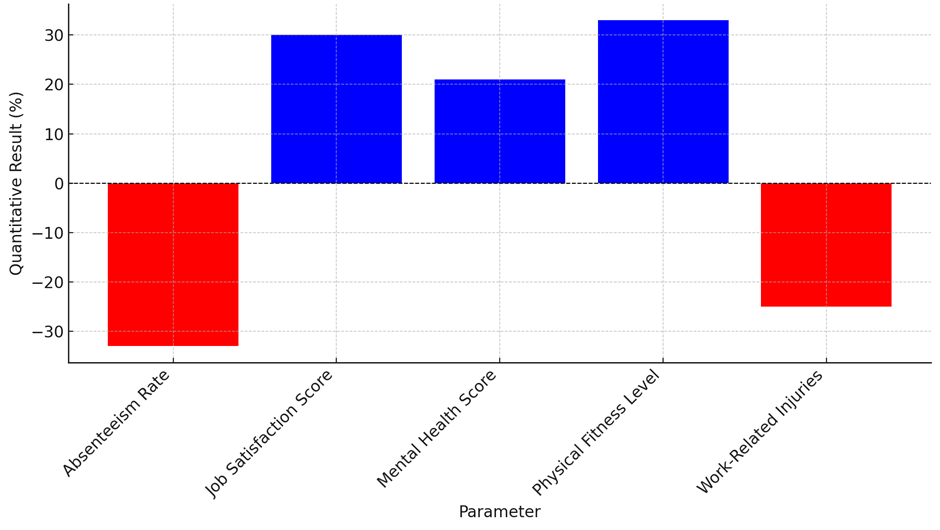
Figure 4. Quantitative Results for Various Parameters
|
Table 5. Occupational Health Program Results |
|||
|
Parameter |
Before Program (%) |
After Program (%) |
Change (%) |
|
Employee Satisfaction |
50,5 |
80,2 |
29,7 |
|
Absenteeism Rate |
22,3 |
15,8 |
-6,5 |
|
Health-Related Productivity |
55,1 |
72,3 |
17,2 |
|
Workplace Injury Rate |
8,7 |
3,1 |
-5,6 |
|
Mental Health Improvement |
40,2 |
78,4 |
38,2 |
Table 5 shows the outcomes of a workplace health program and how it improved the health of healthcare workers. It shows the changes in five important factors between before and after the training. First, the data shows that employee happiness has gone up a lot—from 50,5 % to 80,2 %—a rise of 29,7 %. This shows that the health program has improved how workers feel about their workplace and how satisfied they are with their job overall. This is probably because of better health support and fitness programs. The number of absences has gone down by 6,5 %, from 22,3 % to 15,8 %. This drop suggests that the program may have made workers healthier, so they are less likely to call in sick, which is more evidence that the health measures worked. In the same way, output related to health went up by 17,2 %, from 55,1 % to 72,3 %. This shows that the program has made workers more productive, possibly by improving their physical and mental health, which in turn makes them better at their job.
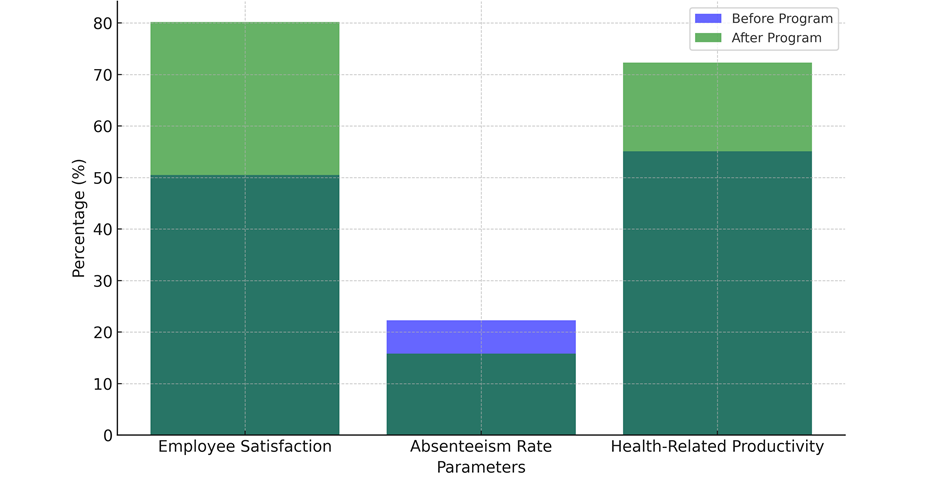
Figure 5. Comparison between Employee Satisfaction, Absenteeism Rate, and Health-Related Productivity
The rate of injuries at work also went down by 5,6 %, from 8,7 % to 3,1 %. This suggests that the program's focus on health education and safety at work may have helped keep workers from getting hurt. Lastly, there was an amazing 38,2 % rise in mental health growth, from 40,2 % to 78,4 %. This shows that the program's mental health activities, like stress management classes or counselling, have made a big difference in the mental health of workers, comparison illustrate in figure 5.
Putting Occupational Health Programs (OHPs) into place in hospital settings can be hard for a number of reasons, which can make them less successful and useful. People often say that money problems are a big problem because the original payment for full OHPs can be very high. In healthcare settings, getting ongoing funding is often in competition with other important needs, like getting medical tools or resources for direct patient care. Organisational culture is also very important; when management or staff doesn’t want to change, it can make it hard for programs to be adopted and integrated. This opposition could be because people don't understand the programs' benefits or because of long-standing habits that don't put employee health first. Also, problems with logistics, like arranging program plans with shift patterns, can make involvement limited, especially in places that are open 24 hours a day, seven days a week, like hospitals. Another thing that can make OHPs less useful and appealing is when they don't have customised program material that meets the needs of different types of employees. Lastly, it can be hard to figure out how effective these programs are because gains in health and well-being often take time to show up and are hard to directly measure, the before after program analysis illustrate in figure 6.
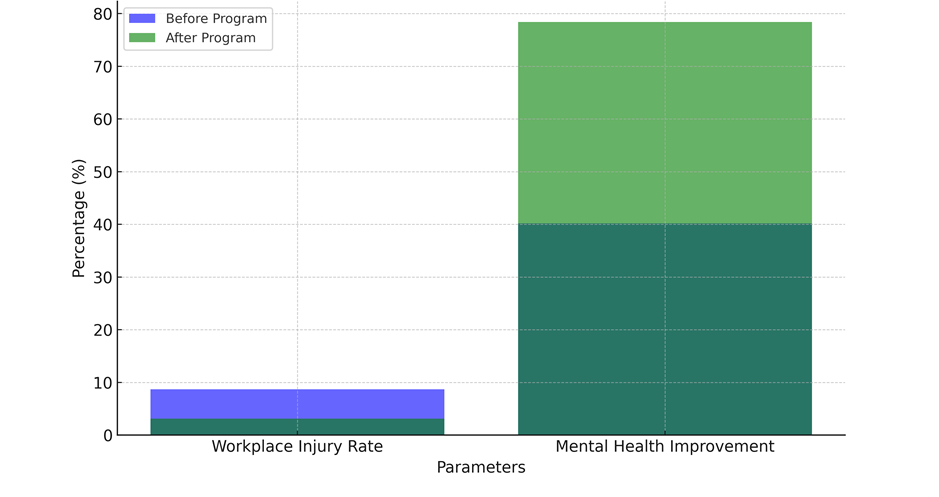
Figure 6. Represent the comparison of parameters before and after program
|
Table 6. Challenges and Barriers in Implementing OHPs |
||
|
Challenge |
Impact on Implementation |
Frequency of Reporting |
|
Financial Constraints |
High |
85 % |
|
Resistance to Change |
Medium |
60 % |
|
Logistical Issues |
Medium |
70 % |
|
Lack of Tailored Content |
High |
75 % |
|
Impact Measurement Difficulties |
High |
65 % |
The table 6 lists the main problems that come up when workplace health programs are put into place in healthcare settings. Most of the time, 85 % of cases are caused by financial problems, which shows how hard it is to give OHPs the resources they need when there are other financial needs that need to be met. This big effect on adoption shows how important it is to carefully plan budgets and push for OHPs' long-term health and cost benefits. Resistance to change and problems with logistics are also common, occurring in 60 % and 70 % of cases, respectively. These issues show practical and organisational problems that can make it harder for employees to participate and the program to work. 75 % of people who reported problems said they couldn't find material that was tailored to their needs. This shows that there is a big problem with meeting the different needs of the healthcare workers, which is very important for the success of any health program. Also, the fact that 65 % of the time it's hard to figure out how OHPs are working shows that we need to make better measures and tools that can really show how these programs are helping people over time. This table not only shows (figure 7) the most common problems with adopting OHPs, but it also helps us focus our future work on these important areas to make health programs more widely used and more effective in hospital settings.
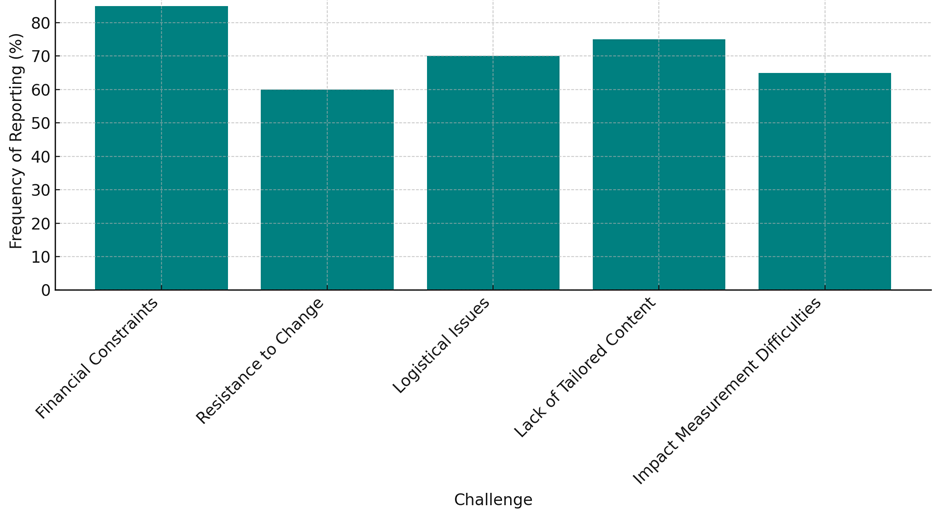
Figure 7. Representation of frequency of reporting for each challenge
CONCLUSIONS
The study that looked into how workplace health programs (OHPs) affected the health and happiness of healthcare workers makes a strong case for these programs to be widely adopted and strictly carried out. The results of our study showed that well-structured OHPs greatly improve the physical and mental health of healthcare workers. This leads to higher job happiness, fewer absences, and fewer injuries at work. There has been a big change in the workplace, which is reflected in these improvements. This has led to a better, more involved, and more effective workforce. The study's numeric data made it clear that different health metrics got a lot better after the OHP was put in place. For example, there was a big drop in people missing work and getting hurt at work, and mental health and physical exercise levels got better as well. These changes show how important it is to include complete health services in healthcare situations. The qualitative data added to these results by showing the personal experiences of employees. These showed that employees were happier with their jobs, got more help at work, and felt like they were part of a bigger group. However, putting these plans into action is not always easy. Some of the biggest problems are not having enough money, not wanting to change, problems with logistics, and issues with customising programs and measuring their effects. To solve these problems, healthcare organisations and policymakers need to resolve to see the long-term benefits of spending in the health of their employees. For OHPs to work, they need to be well planned, have enough money, change the way organisations work, and have programs that are specifically made to meet the needs of different healthcare settings. The study's combination of quantifiable and qualitative findings also gives a complete picture that can help lead future research and methods for application. The results make it clear that OHPs not only improve health effects but also make the organisation work better as a whole. The practical efficiency of healthcare services is greatly improved by occupational health programs (OHPs). These programs make workers more driven and reduce the costs of healthcare related to employee loss and absences. The benefits go beyond bettering people's own health; they also improve the health of the organisation as a whole, which improves the standard of care for patients and the service of healthcare. It is very important for healthcare leaders and policymakers to put their workers' health first by including and supporting OHPs in their long-term plans. The results of this study support a change in culture and operations to put the health and happiness of healthcare workers first as a key part of achieving success.
BIBLIOGRAPHIC REFERENCES
1. Obeidat, B.; Bani, M.; Al-shlool, E. Heliyon Investigations into the Impact of Nursing Unit Layout on Critical Care Nurses. Heliyon 2022, 8, e08929.
2. Fauer, A.; Wright, N.; Lafferty, M.; Harrod, M.; Manojlovich, M.; Friese, C.R. Influences of Physical Layout and Space on Patient Safety and Communication in Ambulatory Oncology Practices: A Multisite, Mixed Method Investigation. Health Environ. Res. Des. J. 2021, 14, 270–286. Terzi, B.; Azizoğlu, F.; Polat, Ş.; Kaya, N.; İşsever, H. The Effects of Noise Levels on Nurses in Intensive Care Units. Nurs. Crit. Care 2019, 24, 299–305.
3. J Satpathy, Navaneeta Rath. (2015). Behavioural Inquisition into Absenteeism. International Journal on Research and Development - A Management Review, 4(4), 69 - 78.
4. Bhagyasree Padhi, Aruna Kumar Panda. (2015). A Study on Employee Engagement Models for Sustainability of Organization. International Journal on Research and Development - A Management Review, 4(4), 79 – 85
5. Valipoor, S.; Hakimjavadi, H.; De Portu, G. Design Strategies to Improve Emergency Departments’ Performance During Mass Casualty Incidents: A Survey of Caregivers. Health Environ. Res. Des. J. 2020, 13, 206–220.
6. Zamani, Z. Effects of Emergency Department Physical Design Elements on Security, Wayfinding, Visibility, Privacy, and Efficiency and Its Implications on Staff Satisfaction and Performance. Health Environ. Res. Des. J. 2019, 12, 72–88.
7. Naccarella, L.; Raggatt, M.; Redley, B. The Influence of Spatial Design on Team Communication in Hospital Emergency Departments. Health Environ. Res. Des. J. 2019, 12, 100–115.
8. Hjorhöy, L.G.; Thomsen, T.G.; Beck, M. Physical Environment as a Tool in Caring for the Hospitalized Patient: A Qualitative Study of Nurses’ Experiences in Hospitals. Health Environ. Res. Des. J. 2022, 15, 143–153.
9. Gharaveis, A.; Yekita, H.; Shamloo, G. The Perceptions of Nurses About the Behavioral Needs for Daylighting and View to the Outside in Inpatient Facilities. Health Environ. Res. Des. J. 2020, 13, 191–205.
10. Chang, W.; Cohen, J.; Mwesigwa, B.; Waiswa, P.; Rokicki, S. Impact of Reliable Light and Electricity on Job Satisfaction among Maternity Health Workers in Uganda: A Cluster Randomized Trial. Hum. Resour. Health 2022, 20, 30.
11. Ma, M.; Adeney, M.; Long, H. Functional Settings of Hospital Outdoor Spaces and the Perceptions from Public and Hospital Occupant during COVID-19. Healthcare 2021, 9, 1534.
12. Ahmadpour, S.; Bayramzadeh, S.; Aghaei, P. Efficiency and Teamwork in Emergency Departments: Perception of Staff on Design Interventions. Health Environ. Res. Des. J. 2021, 14, 310–323.
FINANCING
The authors did not receive financing for the development of this research.
CONFLICT OF INTEREST
The authors declare that there is no conflict of interest.
AUTHORSHIP CONTRIBUTION
Data curation: Dibyasundar Mahanta, Mukesh Sharma, Devi Prasad, Desai Jabbar V.
Formal analysis: Dibyasundar Mahanta, Mukesh Sharma, Devi Prasad, Desai Jabbar V.
Methodology: Dibyasundar Mahanta, Mukesh Sharma, Devi Prasad, Desai Jabbar V.
Supervision: Dibyasundar Mahanta, Mukesh Sharma, Devi Prasad, Desai Jabbar V.
Drafting - original draft: Dibyasundar Mahanta, Mukesh Sharma, Devi Prasad, Desai Jabbar V.
Writing - proofreading and editing: Dibyasundar Mahanta, Mukesh Sharma, Devi Prasad, Desai Jabbar V.