doi: 10.56294/hl2023292
ORIGINAL
Innovations in Healthcare Management That Foster Enhanced Patient Safety and Quality of Care
Innovaciones en la gestión sanitaria para mejorar la seguridad del paciente y la calidad de la Asistencia
Malathi H1 ![]() , Aparna Sharm2
, Aparna Sharm2 ![]() , Jadhav Nitin B3
, Jadhav Nitin B3 ![]() , Gyana Ranjan Nayak4
, Gyana Ranjan Nayak4 ![]() , Ashok Kr Sharma5
, Ashok Kr Sharma5 ![]()
1JAIN (Deemed-to-be University), Department of Biotechnology and Genetics. Bangalore, Karnataka, India.
2School of Liberal Arts, Noida International University. Greater Noida, Uttar Pradesh, India.
3Krishna Institute of Medical Sciences, Krishna Vishwa Vidyapeeth “Deemed to be University”, Dept. of Medicine. Taluka-Karad, Dist-Satara, Maharashtra, India.
4IMS and SUM Hospital, Siksha ‘O’ Anusandhan (Deemed to be University), Department of Cardiology. Bhubaneswar, Odisha, India.
5Arya College of Pharmacy. Jaipur, Rajasthan, India.
Cite as: H M, Sharma A, Nitin B J, Ranjan Nayak G, Ashok KS. Innovations in Healthcare Management That Foster Enhanced Patient Safety and Quality of Care. Health Leadership and Quality of Life. 2023; 2:292. https://doi.org/10.56294/hl2023292
Submitted: 12-05-2023 Revised: 27-07-2023 Accepted: 17-10-2023 Published: 18-10-2023
Editor:
PhD.
Prof. Neela Satheesh ![]()
ABSTRACT
Making patients safer and improving the quality of the treatment received in hospitals depends on improvements in the way healthcare is run. These fresh concepts improve clinical outcomes and patient care by means of sophisticated technology, process optimisation, and data-driven tactics, thereby strengthening healthcare systems. This is so that healthcare systems, handling more patients and more complex clinical scenarios, may be Among the most significant developments are using artificial intelligence (AI) and machine learning (ML) in decision-making. Accurate diagnosis, tailored treatment strategies, and proactive patient monitoring are therefore made feasible. By use of predictive analytics and artificial intelligence systems, one may identify potential hazards, therefore reducing errors and ensuring appropriate timing of action. Particularly in rural and underdeveloped regions, telemedicine has also altered a lot regarding the management of healthcare. By allowing physicians to interact with patients from far-off, telemedicine increases access to healthcare services and monitors patients. Electronic health records (EHR) have also streamlined handling patient information. this is in order that clinicians may additionally make higher decisions as they offer reliable, real-time access to clinical know-how, take a look at findings, and therapy guidelines. Another extensive development is the use of robotic systems in affected person care and healing procedures. These techniques significantly boom sufferers’ healing periods via making treatments pretty specific, consequently lowering mistakes. While still making sure sufferers get the great treatment feasible, using robots for therapy and affected person tracking allows healthcare specialists to simplify their tasks. The usage of internet of things (IoT) devices, actual-time tracking systems additionally reveal patients’ health constantly and notify healthcare body of workers at once need to something occur that might be elaborate. This reduces the dangers associated with responding too slowly and quickens remedy. These traits also are facilitating the cooperation of people from all backgrounds, which improves coordination of patient care, communication among healthcare specialists, and an extra all-encompassing method to affected person protection.
Keywords: Healthcare Management; Patient safety; Artificial Intelligence; Telemedicine; Robotics; Internet of Things (IoT).
RESUMEN
Aumentar la seguridad de los pacientes y mejorar la calidad del tratamiento recibido en los hospitales depende de las mejoras en la gestión de la asistencia sanitaria. Estos nuevos conceptos mejoran los resultados clínicos y la atención al paciente mediante tecnología sofisticada, optimización de procesos y tácticas basadas en datos,
reforzando así los sistemas sanitarios. Entre los avances más significativos está el uso de la inteligencia artificial (IA) y el aprendizaje automático (AM) en la toma de decisiones. De este modo se hace posible un diagnóstico preciso, estrategias de tratamiento a medida y un seguimiento proactivo de los pacientes.
El uso de sistemas de análisis predictivo e inteligencia artificial permite identificar posibles riesgos, reduciendo así los errores y garantizando una actuación en el momento adecuado. Especialmente en las regiones rurales y subdesarrolladas, la telemedicina también ha cambiado mucho la gestión de la asistencia sanitaria. Al permitir a los médicos interactuar con los pacientes desde lejos, la telemedicina aumenta el acceso a los servicios sanitarios y supervisa a los pacientes. Las historias clínicas electrónicas (HCE) también han agilizado el manejo de la información de los pacientes. Esto es así para que los médicos puedan además tomar decisiones más acertadas, ya que ofrecen un acceso fiable y en tiempo real a los conocimientos clínicos, los resultados de los análisis y las pautas terapéuticas. Otro gran avance es el uso de sistemas robóticos en la atención a las personas afectadas y los procedimientos de curación. Estas técnicas aumentan significativamente los periodos de curación de los pacientes al hacer que los tratamientos sean bastante específicos, reduciendo así los errores. Al tiempo que se garantiza que los pacientes reciben el mejor tratamiento posible, el uso de robots para la terapia y el seguimiento de las personas afectadas permite a los especialistas sanitarios simplificar sus tareas. El uso de internet de las cosas (IoT) dispositivos, sistemas de seguimiento en tiempo real, además, revelar la salud de los pacientes constantemente y notificar cuerpo de salud de los trabajadores a la vez que algo ocurra que podría ser elaborado. Esto reduce los peligros asociados a una respuesta demasiado lenta y acelera el remedio. Estos rasgos también están facilitando la cooperación de personas de todos los orígenes, lo que mejora la coordinación de la atención al paciente, la comunicación entre los especialistas de la salud, y un método más integral para la protección de las personas afectadas.
Palabras clave: Gestión Sanitaria; Seguridad del Paciente; Inteligencia Artificial; Telemedicina; Robótica; Internet de las Cosas (Iot).
INTRODUCTION
The need to satisfy more humans, reduced pricing and greater complicated clinical troubles is riding speedy alternate in healthcare. The core of this shift is the intention of creating sufferers safer and elevating the level of remedy quality. In this endeavour, new ideas in healthcare control have become pretty essential. They provide modern tactics to elevate patient consequences, lessen mistakes, and beautify the total patient enjoy by means of ground-breaking technology. These clean concepts make healthcare systems extra perfect to fulfil the evolving demands of patients and healthcare specialists by means of revolutionary technology, procedure enhancement, and facts-pushed selections. In healthcare, patient protection has constantly been as a substitute essential; following appropriate safety tips has helped many lives to be spared. Nevertheless, clinical errors that are probably prevented remain a primary difficulty in the course of advances. Medical errors, in step with the world fitness company (WHO), are the number one reason of harm or loss of life happening international. These well-known shows how urgently matters have to be corrected. Decreasing those risks depends on fresh thoughts in healthcare management; consequently affected person safety is not any more something achieved after the event but instead something done before it occurs. These clean ideas not best permit medical experts to reply rapid and successfully but also assist perceive prospective hazards early by employing current era. One of the most considerable traits in sanatorium administration is the junction of artificial intelligence (AI) and machine learning (ML). AI systems are revolutionising healthcare by permitting more exactly prognosis of illnesses and less difficult decision-making for clinicians. Looking at giant volumes of patient records, artificial intelligence algorithms may perceive tendencies that human physicians might now not frequently be capable of see.(1) This helps to detect early on disorders like most cancers, coronary heart sickness, and brain issues. AI-powered predictive analytics may also forecast potential issues, providing clinicians with expertise to prevent negative events earlier than to their prevalence.
By giving healthcare experts greater specific data and predictive functionality, synthetic intelligence is enhancing affected person consequences and lowering human blunders. This maintains patients more secure. Telemedicine is growing increasingly commonplace together with synthetic intelligence and is changing the manner healthcare is run. Way to telemedicine, which facilitates online discussions and healthcare transport, patients, may additionally get medical remedy anywhere they are living. In rural and neglected areas where there may not be many healthcare choices, this has proved extremely beneficial. Telemedicine not only simplifies things for patients but also guarantees that those living distant distances get treatment when they need it, therefore removing conventional obstacles to access. Usually including video conversations, remote monitoring, and follow-up treatment that keep patients engaged, telemedicine systems can help to reduce the likelihood of patient missing appointments and improve their health management.(2) Digitising healthcare systems together with artificial intelligence and telemedicine has made it feasible for significant data and decision-making progress. In large part, Electronic Health Records (EHRs) have transformed the way patient data is saved and seen. At any moment, EHRs enable clinicians see a patient's medical history, test findings, medications, and treatment plans. This reduces the danger of errors inherent in paper notes and facilitates the coordination of treatment. Better collaboration and ensuring that everyone who has to know about the patient's treatment is aware of it follow from the ease with which healthcare professionals may interact with one another enabled by EHRs. Including artificial intelligence capabilities into EHRs increases their value even further as they provide clinicians with fact-based decision support that guides their decisions depending on patient safety first. Particularly with regard to operations, robotics has also transformed the way healthcare is run.
Importance of patient safety and quality of care in healthcare management
Safety and quality of care for patients are two of the most important parts of managing healthcare well. The health and safety of people is the most important thing in any healthcare system. Making sure patients are safe means lowering the chance of harm and stopping bad things from happening because of medical mistakes, diseases, wrong diagnoses, or treatment delays. When patient safety is compromised, the results can be very bad, including long stays in the hospital, lasting injuries, or even death. To improve healthcare results, it is necessary to keep working to make safety measures better. When you get quality of care, on the other hand, you get services that work well, are quick, and follow set professional standards. Not only does high-quality care improve people's health results, it also makes their treatment experience better, which lowers their worry and builds trust in the healthcare system.(3) To provide excellent care, medicines must be given on time and be based on facts. Patients' physical, social, and mental needs must also be met. The safety of the patient and the level of care go hand in hand. When safety is a top priority in healthcare, it sets the stage for excellent care. For example, hospitals with good infection control procedures and accurate drug management make it less likely for patients to have problems that could have been avoided, like healthcare-associated illnesses (HAIs) or medication mistakes, which can make their healing process much longer.(4) Furthermore, stressing patient safety helps healthcare professionals to be more responsible and transparent, which is rather vital for maintaining high standards of quality of treatment. Healthcare regulations and guidelines all throughout the globe also highly depend on safety and level of treatment for patients.
Overview of recent innovations in healthcare management
Improved outcomes for patients and more efficiency in healthcare systems follow from new advancements in healthcare management drastically altering the delivery of treatment. Among the technical developments bringing about these shifts include artificial intelligence (AI), telemedicine, robotics, and the Internet of Things (IoT). By allowing more precise diagnosis, more tailored therapies, and better patient monitoring, these new technologies are altering patient safety and quality of therapy. An major progress in hospital administration is the use of artificial intelligence. Tools powered by artificial intelligence examine a lot of patient data. This facilitates improved, evidence-based judgements made by medical professionals. Early on in sickness like cancer, diabetes, and heart issues, machine learning algorithms can identify tendencies and project what will happen.(5) Predictive analytics also makes use of artificial intelligence to foretell future issues. This aids in preventing negative events before they start. This not only keeps patients safer but also enables tailored treatment regimens that meet their particular requirements, therefore promoting personalised care. By allowing individuals to schedule medical consultations from far-off, telemedicine has also transformed the delivery of healthcare by reducing physical barriers and increasing accessibility to everyone. For those who reside in remote or neglected regions and may not be able to readily get specialist treatment, telemedicine is very beneficial.(6) By use of video lectures and online monitoring systems, healthcare professionals may ensure patients get continuous treatment and engage in personal health management. Patients find this new concept simpler and it helps them follow their treatment programs, therefore improving their long-term health outcomes. More and more in treatments and therapy, robots are being used to assist with healthcare administration. Robotic-assisted surgeries use very exact techniques free from too much bodily cutting. This means that patients heal faster, have fewer problems, and have better clinical results. Robotic exoskeletons are also making it easier for people who have trouble moving to recover, which improves their quality of life by giving them more freedom.
Technological innovations in healthcare
Electronic Health Records (EHR) and their impact on patient safety
Electronic Health Records (EHR) have changed healthcare by digitising patient information, making it easy to find, and making it easier for healthcare workers to work together. EHRs are made to store a lot of different kinds of patient data, like medical records, lab results, treatment plans, medicines, and diagnosis information. Digitisation has made a big difference in patient safety by making information that doctors use to make clinical choices more accurate, easier to find, and up to date.(7) One of the best things about EHRs is that they cut down on medical mistakes. Historically, handwriting records were prone to being hard to read, having typing mistakes, and getting lost, all of which could pose major risks to patient safety, such as drug errors or delayed diagnoses. Since EHRs enter data online, mistakes like these are less likely to happen. EHR systems also often have alerts for drug combinations, allergens, and repeat tests. These help stop treatments that are dangerous or unnecessary and could put patients at risk. Figure 1 shows how Electronic Health Records (EHR) improve communication, lower mistakes, and make patients safer.
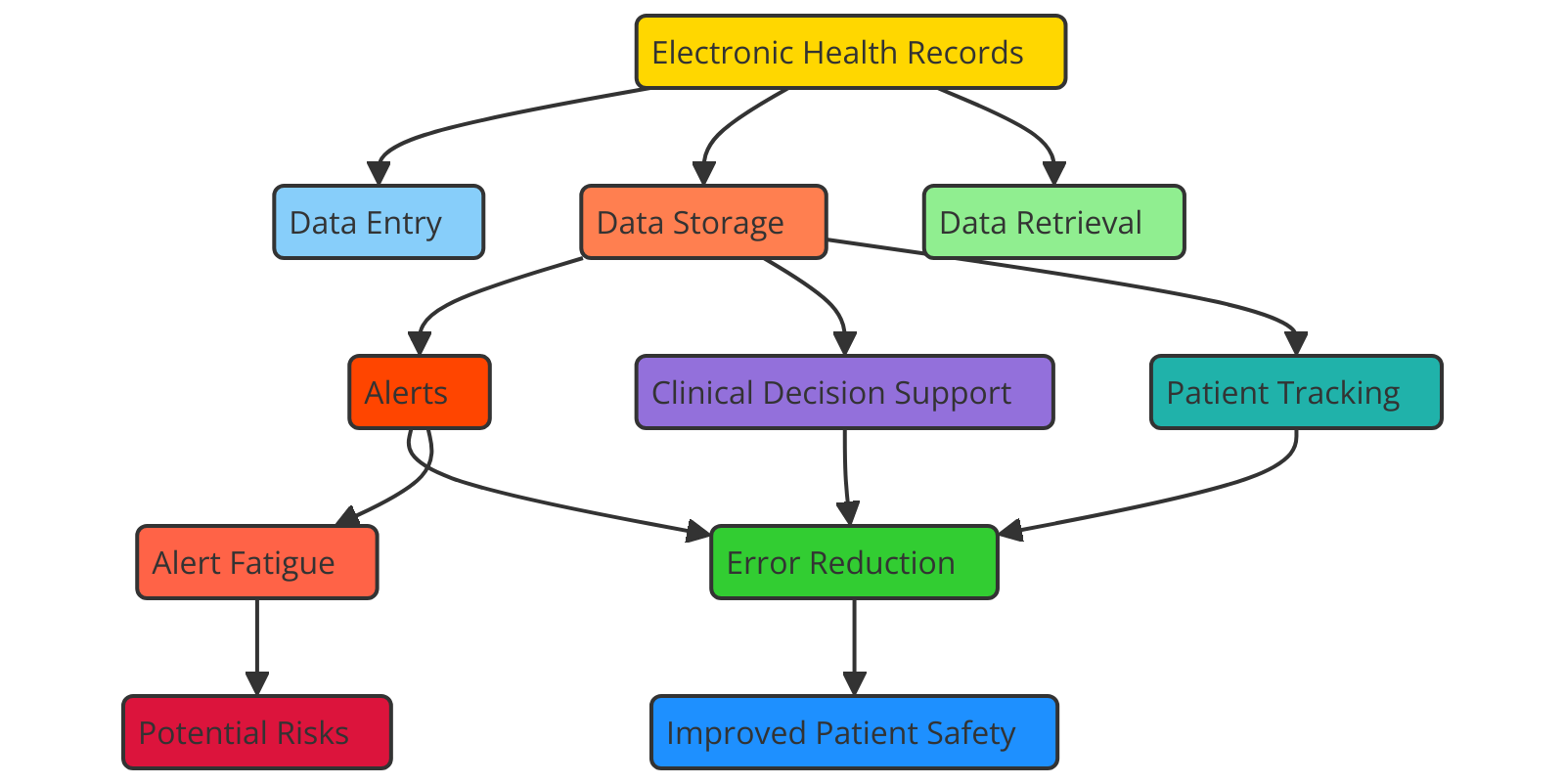
Figure 1. Impact of Electronic Health Records (EHR) on patient safety
Electronic health records (EHRs) also help healthcare teams talk to each other and work together better. When doctors, nurses, and other healthcare professionals can see a patient's full medical background in real time, they can make better choices and avoid tests, procedures, or treatments that could be harmful. This lowers the chance of problems and improves care consistency, especially for people who see more than one expert or change healthcare settings.(8) EHRs also make it easier to keep track of a patient's growth over time. Healthcare professionals can keep track of changes in a patient's state so they can act quickly if any problems arise. This cautious method is very important for avoiding possible bad results, making patients safer, and better total clinical outcomes.
AI and Machine Learning in diagnostics and decision-making
Artificial Intelligence (AI) and Machine Learning (ML) are changing healthcare more and more by making it easier to diagnose problems and make decisions. These technologies are made to quickly and correctly study large quantities of information. This makes them very beneficial for healthcare workers who have to make tough selections primarily based on distinctive pieces of affected person information. AI and ML algorithms can now search medical information such as photographs, genetic records, and affected person records for patterns and anomalies a human may neglect. With high-quality accuracy, AI structures have proved they can appropriately analyse medical snap shots like X-rays, MRIs, and CT scans, spotting early signs of most cancers, heart disorder, and mind illnesses. this selection not only accelerates reviews however additionally makes them more accurate, which lowers the danger of making a mistake and makes sure that sufferers get the proper medicine at the right time.(9) Machine learning models can also wager how a affected person will do via looking at beyond statistics and locating styles that might suggest there are fitness dangers. These predictions help healthcare experts forestall issues earlier than they worsen, which improves patient safety and medical results. As an instance, machine studying models can inform docs in advance of time which issues are maximum in all likelihood to show up in humans with lengthy-time period illnesses like diabetes or heart ailment. This allows clinicians to create tailor-made interventions and remedy plan adjustments earlier than they are wanted. AI structures may also assist scientific personnel in making decisions by means of providing tips based on medical norms, studies, and facts particular to the patient.(10) Those selection-guide structures may additionally allow clinicians pick the best procedures and treatments, therefore enhancing the consistency of remedy and lowering the threat of errors. By displaying relevant information and giving actual-time advice on prospective risks, AI-driven structures also assist clinicians. On this feel, scientific specialists may act fast relying on accurate knowledge.
Telemedicine and remote monitoring for improved care delivery
A using digital communication technology, telemedicine which lets individuals get medical advice and treatment from distance has evolved into a radical new concept in healthcare. For those who have problems travelling about or who want specialist treatment that may not be accessible in their region as well as for those in rural or impoverished areas who want medical attention, this approach is very crucial. Telemedicine allows physicians and nurses to provide lectures via the phone, video conversations, or chat applications, therefore sparing patients from visiting the doctor's office until absolutely necessary. This guarantees that patients may continue receiving medical treatment without having to travel or wait a lot of time, therefore simplifying their situation.(11) Additionally, telemedicine platforms usually have safe ways to share medical data, test results, and pictures. This lets doctors make smart choices from afar. One of the best things about telemedicine is that it can cut down on wait times for care. For example, patients can quickly talk to experts or general practitioners, which keeps conditions from getting worse and needing more extensive care if they aren't treated right away. Regular video check-ins made possible by telemedicine have also helped people with long-term diseases like diabetes, high blood pressure, and mental health issues.(12) This lets treatment plans be constantly checked on and changed, which improves disease care and lowers the risk of problems. Another important part of telemedicine is remote tracking. Patients' critical signs, like heart rate, blood pressure, blood sugar levels, and oxygen consumption, can be watched in real time with smart tech and IoT. Table 1 is a summary of the technology advances in healthcare. It shows linked work, future trends, obstacles, and the limits of these advances.
|
Table 1. Summary of Technological Innovations in Healthcare |
|||
|
Approach |
Future Trend |
Challenges |
Limitations |
|
Implementation of EHR systems |
Increased adoption across healthcare systems |
High implementation costs, data privacy concerns |
Limited adoption in small practices, cost barriers |
|
AI in diagnostic tools |
More widespread use in specialized care |
Data quality, training healthcare providers |
Initial setup cost, regulatory challenges |
|
Telemedicine adoption(13) |
Expansion in rural areas |
Technological infrastructure, patient acceptance |
Access to internet, technology literacy |
|
Robotics in surgeries |
Growth in minimally invasive surgeries |
High cost, training, limited availability |
Costs, limited research in some applications |
|
Use of predictive analytics |
Advancements in machine learning models |
Data privacy, integration with existing systems |
Dependency on accurate data, model accuracy |
|
Data-driven decision support systems |
Integration with AI for better outcomes |
System interoperability, data overload |
Over-reliance on data, lack of clinical integration |
|
Real-time patient monitoring |
Widespread use of remote patient monitoring devices |
High initial investment, patient trust |
Dependence on technology, data security risks |
|
Patient engagement through mobile apps |
Increased use of personalized health management tools |
Digital literacy, engagement of diverse populations |
Technology adoption among older or low-income patients |
|
Integration of IoT in healthcare |
Growth of AI-powered health devices |
Standardization, data security |
Lack of universal standards, data fragmentation |
|
Robotic-assisted rehabilitation(14) |
Greater accessibility and affordability |
Cost, patient and healthcare professional adoption |
High initial cost, resistance to change |
|
Blockchain for healthcare data security |
Wider implementation for securing patient data |
Data encryption, regulatory challenges |
Privacy issues, cross-border data concerns |
|
Big data analytics for population health |
Expanded use for public health insights |
Privacy concerns, data quality |
Ethical concerns in data usage |
|
Healthcare automation tools |
Full integration into clinical workflows |
Cost, integration with clinical practices |
High implementation costs, reluctance from staff |
|
Wearable health devices |
Wearable health tech for continuous monitoring |
Battery life, user compliance |
Compliance with health regulations, device reliability |
Process innovations
Standardization of clinical protocols for patient safety
Standardising hospital practices is one of the most important process innovations in healthcare management for making patients safer. Clinical standards are set rules that healthcare professionals must follow to make sure that the care they give is consistent, correct, and efficient. Healthcare systems make sure those patients get the best care possible based on the latest medical research by standardising processes. This lowers the risk of mistakes and makes sure that care is delivered more consistently. One of the best things about standardised clinical routines is that they cut down on medical mistakes, which are the main reason why patients get hurt. Different professional methods can lead to different ways of interpreting treatment rules or mistakes in the way things are done. Standardised procedures help get rid of this variation by setting clear, evidence-based rules for identifying, treating, and keeping an eye on patients.(15) For instance, procedures for medicine giving make sure that drugs are supplied and given properly, which lowers the chance of dose mistakes or bad responses to drugs. In the same way, normal infection control procedures help stop healthcare-associated diseases (HAIs), which are a major cause of illness and death in patients. Standardised practices not only cut down on mistakes, but they also make it easier for healthcare teams to talk to each other and work together. All healthcare providers whether they are doctors, nurses, or related health professionals are on the same page when it comes to taking care of patients when processes are clearly defined.
Patient-centered care models and their role in quality improvement
A revolutionary idea called patient-centered care (PCC) puts the wants, needs, and beliefs of the patients first when providing healthcare services. This method puts patients at the centre of decisions, making sure that care is tailored to their unique needs and centred on getting results that are important to them. Patient-centered care is becoming more and more important in modern healthcare because it not only makes the experience better for the patient but also helps improve quality generally by leading to better health results and happier patients. Setting up a working relationship between customers and healthcare workers is at the heart of patient-centered care. This model stresses open communication, active patient involvement, and shared decision-making. This makes sure that patients know everything they need to know about their symptoms, treatment choices, and possible risks. Patients are more likely to stick to their treatment plans, listen to their doctors, and do better things when they are involved in making decisions. This directly improves their health. Patient-centered care looks at the whole person, not just their physical health. It addresses their mental, psychological, and social needs as well. Healthcare workers can help people deal with long-term problems, lower stress, and improve quality of life by providing a more complete range of services. Giving mental health support or help with managing the healthcare system, for example, can improve the overall experience and lower hurdles to care, especially for people who are less likely to get it on their own. Also, patient-centered care plans have been linked to better speed and cost-effectiveness in health care. The PCC approach focusses on early assistance and preventative care to cut down on hospital readmissions, trips to the emergency room, and the need for expensive treatments. This can lower long-term healthcare costs. This approach also pushes patients to be more involved, which leads to better health outcomes, fewer problems, and higher patient happiness.
Healthcare data and analytics
Big data in healthcare management
Every day from many sources medical equipment, lab data, insurance claims, communications between patients and healthcare managers a lot of medical knowledge and patient records are produced. We term this "big data." The capacity to collect, maintain, and evaluate this information is altering the operations and decisions taken by healthcare institutions. Eventually, this will result in improved patient outcomes, more effective surgeries, and greater quality of treatment. One of the finest aspects of big data in healthcare is that it may reveal trends and patterns difficult to see otherwise. Advanced analytics enable medical personnel to identify risk groups, spot fresh health trends, and project patient needs prior to their becoming urgent. Big collections of data allow healthcare organisations to identify trends in how they manage chronic illnesses, predict when infections will spread depending on the season, or detect variations in treatment of individuals from various backgrounds. Making treatment plans more tailored to every individual depends on big data as well, hence it is rather vital. Examining a lot of patient data enables physicians and nurses to better grasp the unique requirements of every patient, hence guiding their provision of more focused therapies. When handling complex diseases like cancer, where tailored therapies based on genetic information might make the condition less harmful and raise the odds of success, this can be very beneficial. Big data enables healthcare systems to implement sensible adjustments as well. Examining patient flow, workforce levels, and resource utilisation helps healthcare management to enhance hospital operations, reduce wait times, and guarantee appropriate use of resources. Real-time data analysis allows medical professionals to also monitor patients from a distance. This reduces hospital readmissions and improves continuing treatment.
Predictive analytics for patient outcomes
Predictive analytics in healthcare use statistical methods, prior patient data, and machine learning to project future patient health. This new approach of doing things allows physicians to identify what issues can develop, forecast what their patients will require, and make wise decisions for their treatment. Early intervention, tailored treatment, and proactive management of health issues let predictive analytics significantly raise patient outcomes. It looks at large databases and finds patterns to do this. Early identification allows medical practitioners to intervene before issues worsen, therefore preventing individuals from needing to visit the hospital or experience a more major health incident. In hospitals, predictive analytics is also very helpful as it can be used to project patient behaviour after treatments, throughout recovery, and should they have any issues subsequently. Predictive analytics forecasts patient need for treatment, hence assisting with resource management as well. By determining when the most patients will visit, when they will depart, and when certain services are most in demand, hospitals can maximise their resources that of personnel, beds, and equipment. This guarantees proper utilisation of resources and provision of care when needed.
Role of data-driven decision-making in reducing errors
Data-driven decision-making is the foundation of modern healthcare management as it enables medical professionals to make wise decisions grounded on facts. This reduces errors and enhances patient care by means of which Healthcare professionals may reduce human error risks by means of real-time patient data, historical records, clinical standards, and sophisticated analytics, therefore offering more consistent, correct treatment. One of the key ways that facts-driven selection-making reduces mistakes is using decision help systems (DSS), which mix professional norms and evidence-based totally techniques with patient statistics. Through providing real-time advice on treatment plans, medications, and diagnostic exams, these systems permit clinicians prevent errors like administering the incorrect drugs, diagnosis, or therapy with the aid of means of steerage. For a brand new medicine, for instance, a medical selection assist system may also indicate all potential mixture or allergy. This allows sufferers avoid terrible effects which could endanger their fitness. Facts-pushed choice-making also improves analysis by means of examining massive collections of affected person records, lab findings, and imaging information. Structures like synthetic intelligence and machine learning may identify styles in these facts that human physicians may neglect. This lets in physicians to make extra exactly and unexpectedly selections. As an example, AI-pushed picture identities structures can also greater precisely discover radiography images flaws than greater conventional strategies. This reduces the chance of lacking fractures or cancers amongst other conditions. Records-driven decision-making additionally allows communication throughout healthcare groups and allows them to cooperate. Electronic health records (EHRs) let doctors’ access a patient's whole medical past. This guarantees that every team member understands treatment goals, medications, and earlier actions. This reduces the possibility of pointless testing, incompatible therapies, and delayed care, therefore hastening the healthcare services and reducing their likelihood of errors.
Innovations in training and education
Simulation-based training for healthcare providers
Simulation-based education has grown to be an important tool for coaching and enhancing the abilities of healthcare workers. This novel approach generates controlled environments akin to actual-existence healthcare settings via use of present day technology. This permits medical professionals to expand their talents free from challenge about affected person injury. Especially effective for enhancing routine capabilities, clinical decision-making, and group verbal exchange is simulation-primarily based education. Better patient results and safety comply with from every of these factors. The capability of simulation-based training to replicate high-stress, emergency occasions physicians could see in real existence such as coronary heart stops, trauma cases, or complicated remedies makes it top-of-the-line things about. Through simulating these scenarios in digital surroundings, healthcare specialists may additionally research fast and confident managing of problems. This type of training additionally facilitates physicians make mistakes and develops from them free from endangering actual sufferers. This allows students to develop their understanding of healthcare methods and enhance their talents. Moreover permitting healthcare groups to collaborate greater successfully and communicate with each different higher is simulation-primarily based training. For the duration of scientific events, docs, nurses, and other clinical professionals on occasion must collaborate intently. When individuals are training coordination, role readability, and open communication, real-existence care is much less vulnerable to cross incorrect. Bad clinical incidents are regularly caused by miscommunication, hence patient protection depends tons on this factor of training. Simulations also allow clinical employees to repeatedly rehearse fundamental talents, therefore improving their self-assurance and helping them to come to be extra proficient in them. Very crucial for non-stop improvement, it also permits instructors to grade pupil paintings and provide actual-time feedback. With the aid of use of simulation-based training in healthcare education, establishments may also create a better learning environment that right now enhances affected person care and consequently improves the professional competencies of healthcare personnel.
Continuous professional development and competency-based education
important components of healthcare education that ensure physicians and nurses continue to be present day on the most latest knowledge, beautify their capabilities, and retain imparting superb care throughout their careers consist of competency-based totally training and continuous professional development (CPD). These techniques take into consideration how sufferers' requirements evolve, how technology advances, and how policies concerning healthcare evolve, consequently stressing the continuous learning and improvement of healthcare specialists. CPD exhorts clinical practitioners to keep studying in the course of their lifetime. In this sense, they will continue to be modern-day at the maximum recent traits in technologies, medicinal drugs, information, and science. Healthcare specialists have interaction in a huge spectrum of mastering sports as a part of their CPD; inclusive of conferences, seminars, courses, and person have a look at programs. These activities purpose to include each scientific and non-medical elements of healthcare interest. They will deal with ethics, patient verbal exchange techniques, and splendid leadership, as an instance. CPD, medical experts may additionally make certain that their paintings conform to the maximum latest, evidence-based totally exceptional practices and standards. One step further is competency-primarily based education, which emphasises the acquisition of positive tremendously evolved abilities required for exercise. Competency-primarily based training assesses how efficiently healthcare practitioners can reveal they understand the way to execute crucial factors of medical exercise, not just verifying a list of hours or courses. This technique ensures that medical professionals no longer simplest possess expertise however additionally own realistic utility of what they recognize. Competency-based totally procedures can comprise examinations, sporting activities, and palms-on critiques to make sure that healthcare professionals own the competencies required to offer safe and efficient remedy. Continuing professional development (CPD) and competency-based education work together to make sure that healthcare professionals have the most up-to-date information and the skills they need to meet their patients' needs. These methods encourage a mindset of always getting better, which raises the level of care and safety for patients over time. Supporting CPD and competency-based education is good for healthcare organisations because it helps their staff grow professionally and makes sure they can handle the complicated parts of modern healthcare service.
Integrating safety culture into healthcare education
Including a safety mind-set in healthcare education is very important for creating a setting where patient safety is the most important thing. A safety culture pushes healthcare providers to do things that lower risk, support reporting of mistakes, improve communication, and put the health and safety of both patients and healthcare workers first. Future health care workers are taught to put safety first in all aspects of patient care by adding safety culture concepts into their schooling. One important part of a safety culture is encouraging people to talk to each other and share mistakes or close calls. To create a culture of safety in healthcare education, it is important to teach students and trainers to speak up when they see dangerous behaviour or when they aren't sure about a professional choice. Individuals may learn in educational programs how to avoid the sort of hierarchical obstacles preventing individuals from sharing vital safety information, how to clearly express their concerns, and how to cooperate as a team.
Patient engagement and empowerment
Self-management tools for chronic disease patients
Because they enable patients to take control of their ailments and enhance their overall health, self-management tools are a vital component of caring for those with chronic diseases. These tools which range from digital applications to smart devices to instructional materials help patients monitor their vital signs, manage their symptoms, and follow their prescribed course of action. For those with long-term conditions such diabetes, high blood pressure, or asthma, self-management tools are very vital as they inspire self-care and provide continuous support. This maintains the quality of life and helps to prevent issues. One of the nicest things about self-management systems is that they provide users real-time feedback. Like heart rate monitors, wearable technology may monitor blood sugar, blood pressure, other vital indicators, and give out quick notifications should any of the readings go beyond the intended range. This lets people move quickly, like changing their medications or lifestyle, or getting medical help before a small problem gets worse. These instruments enable individuals to take control of their own health and reduce the need for regular medical visits for monitoring purposes. Furthermore enabling individuals to more closely follow their treatment regimens are self-management techniques. Those with chronic illnesses have to follow their physicians' recommendations about diet and exercise as well as take their medications as advised. Many self-management applications may recall you to schedule adjustments to your lifestyle, attend to your meetings, and choose your prescriptions. This keeps patients on target and reduces their likelihood of missing doses or neglecting to follow their medical advice. Using the data they gather, certain instruments also enable clinicians monitor their patients' development from a distance and provide recommendations or treatment plan adjustments. Furthermore providing instruments for self-management are resources and knowledge tailored for every individual. Apps might provide advice on how to manage symptoms, what to eat, or how to cope with stress, all of which would enable consumers to better control their conditions and feel more secure.
Challenges and barriers to implementation
Financial and resource constraints
Limited funds and resources are two of the biggest problems that make it hard to use new healthcare ideas effectively. For many healthcare systems especially those with limited resources finding the funds required implementing new technologies, upgrading buildings, or staff training may be difficult. Usually at first, using modern concepts like telemedicine platforms, electronic health records (EHRs), or high-tech medical instruments require a significant outlay. For hospitals on a limited budget or dependent on government funding, this might be challenging. For many firms, the expenses of acquiring, configuring, and maintaining new technology are too great. For instance, using a whole EHR system costs more than simply the hardware and software itself. Monthly maintenance, updates, and training for healthcare professionals on the system also cost money. In the same way, telemedicine platforms have many benefits, but they need money to be spent on technology infrastructure, staff training, and safe communication systems. Also, not having enough resources can make it harder to hire and keep the trained healthcare workers that are needed to run and handle new technologies. The demand for staff beats the supply, so even the most cutting-edge healthcare innovations may not reach their full potential if there aren't enough workers. When this happens, healthcare organisations might have trouble putting new ideas into practice, which can make it harder to improve the level of care and patient safety.
Resistance to change and organizational culture
Implementing new healthcare ideas can be hard because people don't like change. This is often caused by the way the organisation works now. Healthcare workers and staff may not want to use new tools or methods because they are afraid of chaos, don't know how to use them, or aren't sure what the benefits could be. From not wanting to use fresh approaches to outright rejecting to accept new ways of doing things, this resistance may manifest itself in many forms. Organisational culture greatly influences how individuals in a healthcare environment see and welcome change. New ideas introduced into a company with strong leadership or ancient methods of operation may cause workers to feel threatened about their present roles and practices. People who suffer from this fear of change may not be eager to participate in fresh initiatives and complicate the process of enhancing medical treatment. The time it takes to pick up new instruments or techniques worries healthcare professionals as well as they may not be adequately educated or it would compromise their capacity to provide high-quality treatment. If healthcare institutions want individuals to embrace change, they must give developing a culture of openness, cooperation, and continuous learning first importance. This approach depends much on leadership as it fosters confidence and demonstrates that one believes in the advantages of fresh ideas. Including staff members in the phases of planning and execution, offering continuous support and training, and clarifying the value of fresh ideas can assist to allay fears and inspire a more favourable response to transformation. Moreover, addressing the underlying reasons of resistance such as lack of resources or fear of failing may help to remove obstacles and get staff members on board.
RESULT AND DISCUSSION
New technologies in healthcare management such as electronic health records (EHRs), artificial intelligence (AI), and telemedicine have greatly changed patient safety and quality of treatment. EHRs have made it simpler for healthcare teams to interact with one another, therefore reducing errors and ensuring patients get consistent treatment at the correct moment. Faster and more accurate evaluations generated by artificial intelligence have resulted in earlier therapy and more tailored strategies. Particularly in places not well serviced, telemedicine has made it simpler for more individuals to get medical treatment. It also enables fewer visits to the hospital and ongoing surveillance. These new ideas have not only improved clinical results, but they have also made patients happier, cut down on medical mistakes, and made healthcare more focused on the patient.
|
Table 2. Healthcare Innovations - Patient Safety |
||||
|
Innovation |
Diagnosis Accuracy Improvement (%) |
Medical Error Reduction (%) |
Patient Engagement Improvement (%) |
Cost Reduction (%) |
|
EHR |
30 |
40 |
45 |
10 |
|
Telemedicine |
70 |
50 |
80 |
20 |
|
Robotics |
90 |
65 |
70 |
25 |
|
Predictive Analytics |
80 |
55 |
60 |
18 |
Table 2 shows how different innovations in healthcare have improved patient safety in four main areas: correct diagnosis, fewer medical mistakes, patient participation, and lower costs. Electronic Health Records (EHR) show some changes in how accurate diagnoses are (30 %) and how many medical mistakes are made (40 %). Figure 2 shows how new technologies have changed healthcare measures over time, showing how they have improved speed, patient results, and cost-effectiveness.
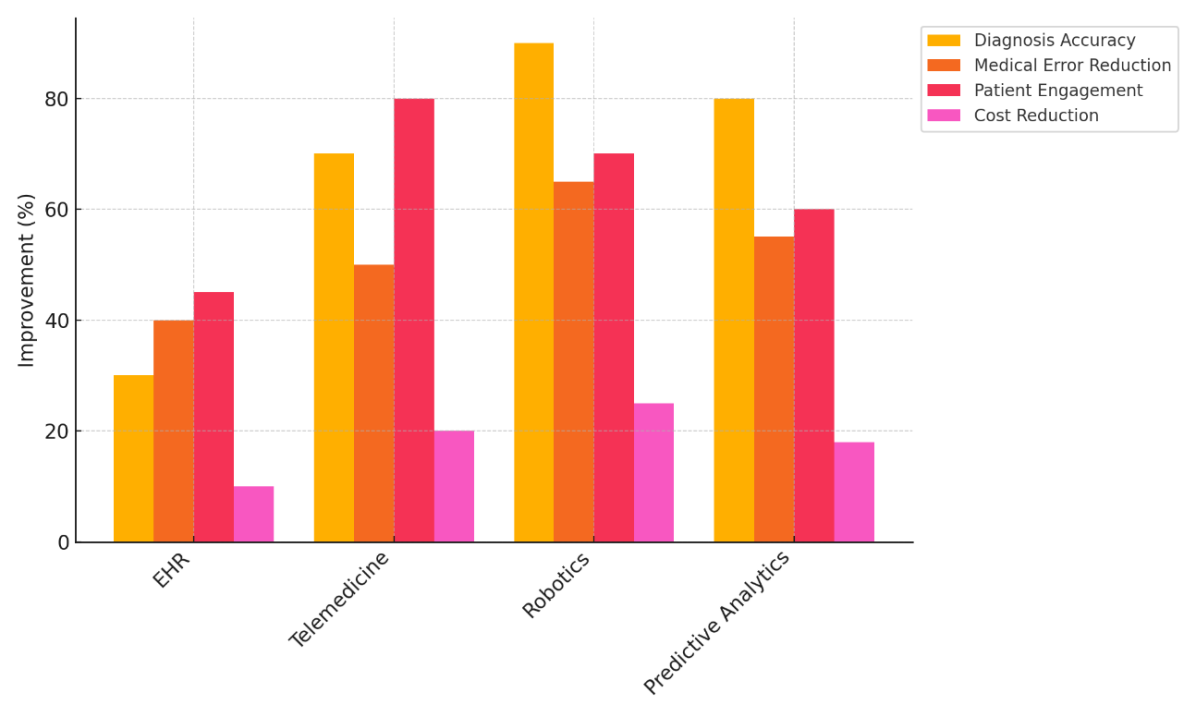
Figure 2. Comparison of Innovation Impacts on Healthcare Metrics
EHR systems make patients safer by improving communication and organisation of care. However, they don't have much of an effect on participation or cost savings because they are hard to fully integrate into current systems, especially in smaller offices. Figure 3 looks at how changes in innovation have affected healthcare measures over time.

Figure 3. Trend Analysis of Innovation Impacts on Healthcare Metrics
With a 70 % increase in accurate diagnoses and an 80 % increase in patient involvement, telemedicine is a game-changer for improving access to care. It can cut down on the need for in-person visits and get patients more involved in their own care, which leads to higher happiness and better results. Telemedicine also saves money by cutting down on hospital visits and making the best use of resources. Robotics has the biggest impact on improving the accuracy of diagnoses (90 %) and lowering medical mistakes (65 %). Robotic systems improve accuracy and reduce human mistake, which makes them very important for patient safety, especially in surgery. The high prices of robots, on the other hand, keep many people from using it.
|
Table 3. Healthcare Innovations - Quality of Care |
||||
|
Innovation |
Patient Satisfaction Improvement (%) |
Treatment Time Reduction (%) |
Care Efficiency Improvement (%) |
Workflow Efficiency Improvement (%) |
|
EHR |
50 |
20 |
35 |
25 |
|
AI-based Diagnostics |
75 |
30 |
45 |
35 |
|
Telemedicine |
85 |
40 |
50 |
45 |
|
Robotics |
80 |
25 |
60 |
55 |
Table 3 shows how different improvements in healthcare have changed the quality of care by looking at patient happiness, shortened treatment times, care efficiency, and process efficiency. The use of electronic health records (EHR) has led to a small but positive rise in both patient happiness (50 %) and care efficiency (35 %). Figure 4 shows how innovations have led to overall gains in healthcare measures.
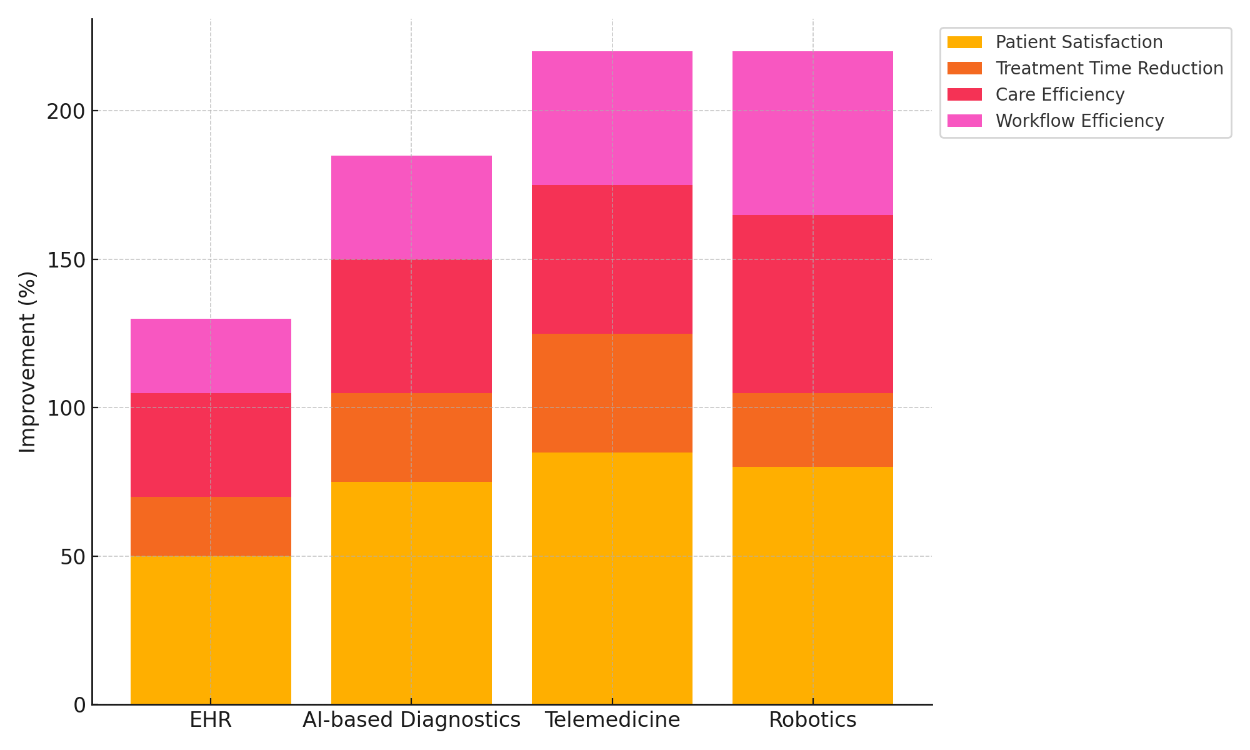
Figure 4. Cumulative Improvement in Healthcare Metrics by Innovation
EHRs make it easier to get to patient data, which cuts down on mistakes and improves teamwork. However, they don't have much of an effect on lowering treatment time (20 %) or improving process efficiency (25 %). This is because they are hard to integrate and users have trouble adapting to them. AI-based Diagnostics makes patients much happier (75 % more satisfied) and care more efficient (45 % more satisfied). AI makes diagnoses more accurate, which helps doctors make faster and better decisions about treatment. It's clear that AI can speed up diagnostic processes and improve clinical workflows because treatment times have been cut by 30 % and workflow efficiency has been raised by 35 %. Telemedicine has the biggest impact on patient happiness (85 %) and the biggest impact on treatment time (40 %). In Figure 6, you can see how advances have helped improve healthcare over time.
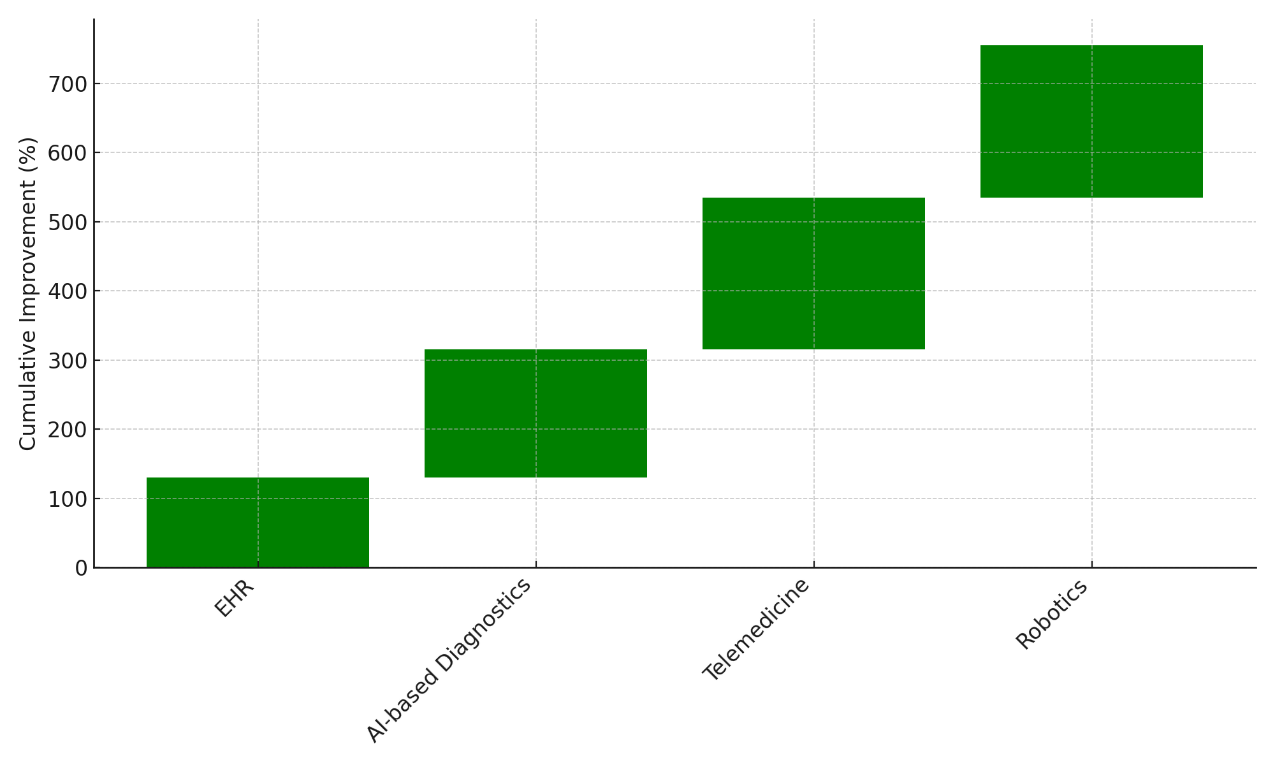
Figure 5. Cumulative Contribution of Innovations to Healthcare Improvements
Telemedicine makes it easier for people to get medical care, which makes patients more engaged and satisfied while reducing the need for in-person visits. This improves both the efficiency of care (50 %) and the efficiency of processing (45 %). These results show that telemedicine has the ability to improve both the way care is given and the experience of patients.
CONCLUSIONS
New ideas in healthcare management can make a huge difference in improving both patient safety and the level of care. New technologies like Electronic Health Records (EHRs) and Artificial Intelligence (AI) have greatly revolutionised the way medical professionals approach and provide treatment. EHRs have made it simpler for people to interact with one another, ensure that documentation is accurate, and access patient information fast and simply. This has helped physicians make better judgements and reduced errors. AI is a great tool for early illness detection and customised treatment planning that enhance patient outcomes even more as it can examine large databases and assist with analysis. Particularly for those living in rural or poor regions, telemedicine is another crucial new tool that has enabled individuals to get better healthcare. From the comfort of their own homes, it allows patients to interact with physicians, get assessments, and monitor long-term ailments. This reduces the need for patients to return to the hospital and facilitates their access to treatment when needed. Many telemedicine users have also made patients more engaged, therefore arming them with greater authority to take control of their own health. By reducing errors committed by humans, enhancing treatment accuracy, and simplifying procedures, emerging technologies like predictive analytics, robotics, and IoT-enabled devices have also made healthcare more efficient. These fresh concepts not only personalise and simplify healthcare but also improve it by reducing unnecessary treatments and ensuring that every patient receives therapy fit for their requirements. Even though there are problems like limited funds, reluctance to change, and limited technology, it is clear that new developments in healthcare are good. Getting past these problems takes smart investments, ongoing professional development, and encouraging people to work together and be open to new technologies. In conclusion, advances in healthcare have made a big difference in improving patient safety and quality of care. As technology keeps getting better, healthcare systems will become safer, more patient-centered, and more efficient. This will lead to better health results and better care generally for patients.
BIBLIOGRAPHIC REFERENCES
1. Khetan, S.K.; Collins, T.J. Human pharmaceuticals in the aquatic environment: A challenge to Green Chemistry. Chem. Rev. 2007, 107, 2319–2364.
2. Montes-Grajales, D.; Fennix-Agudelo, M.; Miranda, W. Occurrence of personal care products as emerging chemicals of concern in water resources: A review. Sci. Total Environ. 2017, 595, 601–614.
3. Mudgal, S.; De Toni, A.; Lockwood, S.; Salès, K.; Backhaus, T.; Sorensen, B.H. Study on the Environmental Risks of Medicinal Products; BIO Intelegence Service: Neuilly Sur Seine, France, 2011.
4. Ch.V.L.L.Kusuma Kumari. (2015). Performance Appraisal: Dimensions and Determinants. International Journal on Research and Development - A Management Review, 4(3), 27 - 32.
5. Kompalli Sasi Kumar. (2015). Short Run and Long Run Performance of Indian Initial Public Offerings (IPOs) during 2007-2012. International Journal on Research and Development - A Management Review, 4(3), 33 - 41.
6. Chander, V.; Sharma, B.; Negi, V.; Aswal, R.S.; Singh, P.; Singh, R.; Dobhal, R. Pharmaceutical Compounds in Drinking Water. J. Xenobiot. 2016, 6, 5774.
7. Zuccato, E.; Castiglioni, S.; Fanelli, R.; Reitano, G.; Bagnati, R.; Chiabrando, C.; Pomati, F.; Rossetti, C.; Calamari, D. Pharmaceuticals in the environment in Italy: Causes, occurrence, effects and control. Environ. Sci. Pollut. Res. Int. 2006, 13, 15–21.
8. Desbiolles, F.; Malleret, L.; Tiliacos, C.; Wong-Wah-Chung, P.; Laffont-Schwob, I. Occurrence and ecotoxicological assessment of pharmaceuticals: Is there a risk for the Mediterranean aquatic environment? Sci. Total Environ. 2018, 639, 1334–1348.
9. Li, W.C. Occurrence, sources, and fate of pharmaceuticals in aquatic environment and soil. Environ. Pollut. 2014, 187, 193–201.
10. Wu, D.; Zhou, Y.; Lu, G.; Hu, K.; Yao, J.; Shen, X.; Wei, L. The Occurrence and Risks of Selected Emerging Pollutants in Drinking Water Source Areas in Henan, China. Int. J. Environ. Res. Public Health 2019, 16, 4109.
11. Balakrishna, K.; Rath, A.; Praveenkumarreddy, Y.; Guruge, K.S.; Subedi, B. A review of the occurrence of pharmaceuticals and personal care products in Indian water bodies. Ecotoxicol. Environ. Saf. 2017, 137, 113–120.
12. McEneff, G.; Schmidt, W.; Quinn, B. Pharmaceuticals in the Aquatic Environment: A Short Summary of Current Knowledge and the Potential Impacts on Aquatic Biota and Humans. EPA Res. Rep. 2015, 142, 52.
13. Sabino, J.A.; de Sá Salomão, A.L.; de Oliveira Muniz Cunha, P.M.; Coutinho, R.; Marques, M. Occurrence of organic micropollutants in an urbanized sub-basin and ecological risk assessment. Ecotoxicology 2021, 30, 130–141.
14. Quadra, G.R.; Oliveira de Souza, H.; Costa, R.D.; Fernandez, M.A. Do pharmaceuticals reach and affect the aquatic ecosystems in Brazil? A critical review of current studies in a developing country. Environ. Sci. Pollut. Res. Int. 2017, 24, 1200–1218.
15. Pacheco Ferreira, A. Environmental Investigation of Psychiatric Pharmaceuticals: Guandu River, Rio De Janeiro State, Southeast Brazil. J. Chem. Health Risks 2018, 4.
FINANCING
The authors did not receive financing for the development of this research.
CONFLICT OF INTEREST
The authors declare that there is no conflict of interest.
AUTHORSHIP CONTRIBUTION
Data curation: Malathi H, Aparna Sharma, Jadhav Nitin B, Gyana Ranjan Nayak, Ashok Kr Sharma.
Formal analysis: Malathi H, Aparna Sharma, Jadhav Nitin B, Gyana Ranjan Nayak, Ashok Kr Sharma.
Methodology: Malathi H, Aparna Sharma, Jadhav Nitin B, Gyana Ranjan Nayak, Ashok Kr Sharma.
Supervision: Malathi H, Aparna Sharma, Jadhav Nitin B, Gyana Ranjan Nayak, Ashok Kr Sharma.
Drafting - original draft: Malathi H, Aparna Sharma, Jadhav Nitin B, Gyana Ranjan Nayak, Ashok Kr Sharma.
Writing - proofreading and editing: Malathi H, Aparna Sharma, Jadhav Nitin B, Gyana Ranjan Nayak, Ashok Kr Sharma.