doi: 10.56294/hl2023259
ORIGINAL
The Effects of Enhancements in Environmental Health on Pediatric Health Outcomes
Efectos de la mejora de la salud ambiental en los resultados sanitarios pediátricos
Sunil Lawand1 ![]() , Supriya Awasthi2
, Supriya Awasthi2 ![]() , Chandan Das3
, Chandan Das3 ![]() , Malathi H.4
, Malathi H.4 ![]()
1Krishna Institute of Medical Sciences, Krishna Vishwa Vidyapeeth “Deemed to be University”, Dept. of Pediatrics. Taluka-Karad, Dist-Satara, Maharashtra, India.
2School of Allied Health Sciences, Noida International University. Greater Noida, Uttar Pradesh, India.
3IMS and SUM Hospital, Siksha ‘O’ Anusandhan (Deemed to be University), Department of General Medicine. Bhubaneswar, Odisha, India.
4JAIN (Deemed-to-be University), Department of Biotechnology and Genetics. Bangalore, Karnataka, India.
Cite as: Lawand S, Awasthi S, Das C, H M. The Effects of Enhancements in Environmental Health on Pediatric Health Outcomes. Health Leadership and Quality of Life. 2023; 2:259. https://doi.org/10.56294/hl2023259
Submitted: 03-05-2023 Revised: 18-07-2023 Accepted: 13-10-2023 Published: 14-10-2023
Editor: PhD.
Prof. Neela Satheesh ![]()
ABSTRACT
Environmental health has been known for a long time to have a big effect on people’s health, especially when they are young because their bodies are still developing and they are more likely to be affected by environmental stresses. It is possible for improvements in environmental health practices to have a big impact on children’s health by lowering their exposure to environmental risks, making living situations better, and improving their health over time. This study looks into the different ways that changes in environmental health, like better air quality, water cleaning, garbage management, and urban planning, can have direct and secondary effects on the health of children. Children and teens are especially vulnerable to environmental chemicals and dangers because their immune systems are still growing, their metabolisms are faster, and they do things that put them at risk, like spending more time outside and eating with their hands. This is why effective public health campaigns may significantly reduce the prevalence of children suffering with asthma, lung diseases, lead poisoning, and developmental abnormalities. Keeping children healthy and preventing diseases that may be prevented also depends on access to safe living, clean water, and pollution-free surroundings. The paper examines several case studies and actual data from areas where public health guidelines have become somewhat better. Particularly in places with significant pollution, the data reveal a high correlation between environmental health policies and improved health outcomes for children. Better growth and development in children generally, reduced incidence of long-term disorders like asthma, and less hospitalisation resulting from improvements to public health services.
Keywords: Environmental Health; Pediatric Health; Air Quality; Urban Planning; Public Health Interventions.
RESUMEN
Desde hace mucho tiempo se sabe que la salud ambiental tiene un gran efecto en la salud de las personas, especialmente cuando son jóvenes porque sus cuerpos aún se están desarrollando y son más propensos a verse afectados por el estrés ambiental. Es posible que las mejoras en las prácticas de salud ambiental tengan un gran impacto en la salud de los niños al reducir su exposición a los riesgos ambientales, mejorar sus condiciones de vida y mejorar su salud con el tiempo. Este estudio examina las distintas formas en que los cambios en la salud ambiental, como la mejora de la calidad del aire, la limpieza del agua, la gestión de la basura y la planificación urbana, pueden tener efectos directos y secundarios en la salud de los niños. Los niños y los adolescentes son especialmente vulnerables a las sustancias químicas y los peligros ambientales porque su sistema inmunitario aún está creciendo, su metabolismo es más rápido y hacen cosas que los ponen en peligro, como pasar más tiempo al aire libre y comer con las manos. Por eso, unas campañas de salud pública eficaces pueden reducir significativamente la prevalencia de niños que padecen asma, enfermedades pulmonares, intoxicación por plomo y anomalías del desarrollo. Mantener a los niños sanos y prevenir las enfermedades que pueden prevenirse también depende del acceso a una vida segura, agua limpia y un entorno libre de contaminación. El documento examina varios estudios de casos y datos reales de zonas donde las directrices de salud pública han mejorado algo. Especialmente en lugares con una contaminación significativa, los datos revelan una alta correlación entre las políticas de salud ambiental y la mejora de los resultados sanitarios en los niños. Mejor crecimiento y desarrollo de los niños en general, menor incidencia de trastornos a largo plazo como el asma y menos hospitalizaciones gracias a las mejoras de los servicios de salud pública.
Palabras clave: Salud Ambiental; Salud Pediátrica; Calidad del Aire; Planificación Urbana; Intervenciones de Salud Pública.
INTRODUCTION
Particularly for children and other vulnerable populations, environmental health is a really crucial component of public health. Particularly regarding children's health, there has been a lot of attention in the relationship between outside variables and health outcomes in recent years. Children breathe quicker and their bodies are still developing, hence they are more prone to be harmed by environmental hazards. Through their activities—like playing outside and eating with their hands—they are also more likely to come into contact with contaminants. Children's bodies and immune systems are still developing hence toxins and chemicals are also more prone to damage them. This makes it rather crucial to understand how directly changes in public health might affect the health outcomes of children. Environmental health covers a wide spectrum of factors influencing individuals's health, including air and water quality, cleanliness, chemical exposure, noise pollution, rubbish management, and architectural and maintenance practices of cities. Improvements in these areas will help to significantly reduce the likelihood of many health issues affecting youngsters. Reducing dangerous pollutants like nitrogen dioxide (NO2) and particle matter (PM), for instance, can improve the quality of the air and considerably increase its safety for human breathing. This can drastically lower the prevalence of respiratory disorders including bronchitis and asthma among children living in highly polluted metropolitan areas. Similarly, clean drinking water, appropriate garbage disposal, and access to green spaces are all vital for enhancing children's health by minimising their risk of gastrointestinal diseases, not obtaining enough food, and lagging growth. Among the most well-known paediatric disorders influenced by the surroundings is asthma. Environmental elements, particularly in highly polluted areas, have been connected to this long-term long illness.
Children who reside in these areas are more likely to develop asthma or have it worsen, which results in more frequent hospital visits and skipping of classes. Many research have indicated that ensuring the surroundings is safer helps children with asthma avoid issues. Lower asthma rates and milder asthma symptoms have been associated, for instance, with improved air quality and reduced aller exposure. An additional crucial component of public health for children is the consequences of lead poisoning. Children's lead contamination has been connected to issues with their growth, behaviour, and cognition. Blood lead levels have dropped significantly and the long-term consequences of lead exposure have been stopped thanks in great part to environmental health gains—especially stronger regulations on lead in water, homes, and other consumer items.(1) In areas where lead removal campaigns have been implemented, the number of children suffering from lead poisoning and the accompanying health issues has dropped dramatically. Furthermore influencing children's health is the design of cities and the maintenance of residences. The built environment which comprises the quality of dwellings, green spaces, and transportation systems can influence children's mental and physical state. Access to safe parks, schools, and other leisure activities, for example, can inspire individuals to be more active and social, therefore improving their health. Furthermore, the way cities are designed with an eye towards reducing noise pollution and ensuring clean air and water would improve their suitability for children's growing up environment. Like having safe, mild-free homes, housing conditions can also reduce the likelihood of lung issues and other health concerns.(2)
Definition of Environmental Health
Define environmental health. Studies on how the environment influences disease are a component of public health. It looks at and seeks to manage the several man-made and natural objects on the planet that could affect human health. Among these elements are the quality of the air and water, the state of the local cleanliness, the possibility of chemical exposure, noise pollution, waste management, and general living environment safety. Particularly those resulting from environmental responses, environmental health studies how these factors influence the emergence of diseases, accidents, and other health issues. Environmental health encompasses not only the state of the surroundings but also the social, financial, and cultural elements influencing human behaviour. It entails attending to probable hazards such air pollution, contaminated water, harmful chemicals, and hazardous accommodation.(3) Using public health policy, modern technology, and health education helps one to either lower or eliminate these hazards. This will help to make the earth a better and healthier environment for everybody. By means of efforts to enhance environmental health, one can reduce the prevalence of ailments like lung disorders, stomach infections, and lead poisoning resulting from pollution and hazardous living environments. Regarding children's health, environmental health is very crucial. Toxins and pollution in the environment can hurt children more because their immune systems are still growing, their bodies are smaller, and they are exposed to more of them than adults.
Importance of Pediatric Health
Paediatric health is an important part of public health that looks after the health and growth of kids from birth to adolescence. This is an important time in life because it's when your body, mind, and emotions all grow quickly. Getting the right care as a kid is important for a healthy growth, avoiding illnesses, and setting the stage for a healthy life. Paediatric health includes a lot of different areas of health, such as diet, immunisations, mental health, long-term diseases, and avoiding injuries. One of the main goals of paediatric health is to keep kids from getting diseases that can be avoided. As shown in figure 1, paediatric health is very important for a child's long-term growth and well-being.
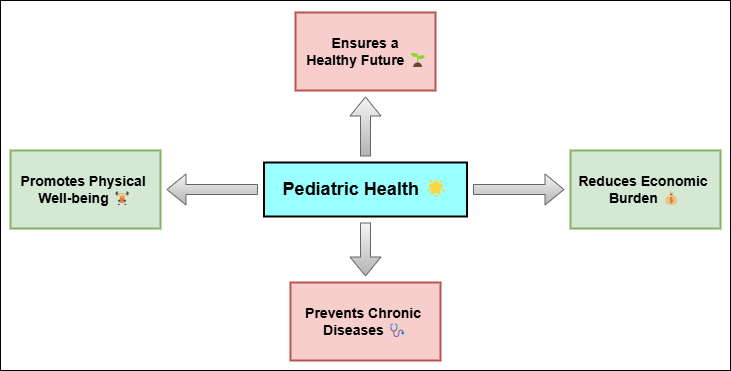
Figure 1. Illustrating the importance of pediatric health
Catching problems early can have a big effect on a child's health over time. Because their bodies and defence systems are still growing, children are more likely to be hurt by biological and external factors than adults. Because of this, they are very likely to get a lot of different diseases, especially ones that are linked to being in the environment. Asthma, developmental delays, lead pollution, and childhood cancers have all been linked to environmental factors. Reducing these risks is very important for improving the health of children. Also, dealing with mental health issues during childhood is very important because stresses and trauma in early life can have long-lasting effects on social and psychological growth. Children's health is important for more than just their physical well-being; it also affects their mental and social growth. Children who grow up in dirty environments or when they come across harmful substances, for instance, may have development gaps that make it more difficult for them to perform in the classroom and among peers.(4) Children's excellent development and growth depend critically on their being able to go to safe locations, eat healthily, and obtain medical attention as needed. This is why the relationship between natural health and kid health is so crucial: we can directly influence children's health and well-being by improving the surroundings.
Purpose and Scope of the Study
The aim of this study is to investigate how improvements in public health impact child health. Children's health can be seriously compromised by environmental hazards, as is widely recognised. Still, there is much more research to be done on the significant part environmental health enhancements play in reducing these risks and enhancing health. This study aims to investigate how various activities aimed to promote environmental health—that includes standards for air quality, water cleaning programs, trash management systems, and urban planning—have resulted in fewer childhood ailments and improved overall health for children. The study examines case studies, present studies, and actual data from locations that have undergone significant modifications to better the quality of their surroundings. Examining these developments will help the research to fully understand how specific health issues in children, including asthma, lead poisoning, behavioural delays, and childhood malignancies, are affected by environmental improvements. Moreover, the study will investigate the more general consequences of these outside developments, including how they impact social well-being, mental health, and brain development.(5) This study aims to identify effective worldwide, regional, and local environmental health solutions that may be used, thereby improving public health policy and practice. It also wants to bring attention to how working together across sectors can lead to better health results for kids. For future work to create laws and programs that protect and improve children's health through public health changes, the study's results could be used as a starting point. In the end, this study wants to add to what is already known about how improving the health of the environment can lower the number of childhood diseases, make homes better, and raise the quality of life for kids all over the world.
Literature Review
Historical Context of Environmental Health Enhancements
In the last 100 years, environmental health improvements have changed a lot. This is because of science study and more people becoming aware of how environmental factors affect health. In the past, environmental health changes were mostly reactive, with the goal of controlling disease outbreaks like cholera and typhoid fever that were caused by dirty circumstances. Early days of environmental health focused mostly on sewage system improvement, clean water provision, and garbage management improvement. These steps helped to drastically lower the infectious illness count among humans. As factories and towns developed quicker, people began to pay greater attention to air pollution around the middle of the 20th century—a growing issue. Rules were created to safeguard the air as people came to see that industry pollution, particle matter, and smoking were detrimental for them. The Clean Air Act came enacted in the United States in 1970. Stricher laws and regulations were implemented in the 1970s to guard the environment against pollution and toxins. Leaded fuel was outlawed, for instance, pesticides were controlled, and mechanisms were set up to monitor the surroundings.(6) Efforts to promote public health in the 1980s and 1990s began to focus on reducing exposure to harmful chemicals and bettering city layouts. These included pushing municipalities to have more green spaces, making it more difficult for companies to dispose of their garbage, and simplifying handling of hazardous items. The expansion of environmental justice organisations revealed how more than others low-income and minority populations suffer from environmental hazards influence. This resulted in more equitable approaches of approaching environmental health policies. Efforts to enhance environmental health nowadays still target issues including equitable treatment of the environment, healthy urban development, and climate change. Thanks to constant research and technological development, monitoring and lowering of environmental hazards may be accomplished more precisely. Particularly for children and other vulnerable populations, this serves to promote public health.
Key Environmental Factors Affecting Pediatric Health
Air Quality
One of the main natural elements influencing youngsters' health is the quality of the air. Because they breathe quicker, have smaller lungs, and are still developing their respiratory systems, children are more prone to be impacted by air pollution.(6) Children exposed to air pollution including ozone, particle matter (PM), nitrogen dioxide (NO2), and sulphur oxide (SO2) suffer from a range of health problems including asthma, coughing, and respiratory diseases. Their lungs also develop incorrectly. Children living in areas with poor air quality are more likely to develop asthma, a condition that can severely affect their life and force frequent hospital visits. Long-term respiratory issues and damage to brain development if breathed in for extended periods of time can result from air pollution. Along with aggravating health issues including allergies, air pollution increases the likelihood of early or low birth weight new-borns for pregnant women. Some measures to help to enhance the quality of the air are cutting automobile and factory emissions, as well as changing to green energy sources. For youngsters, these developments can have significant impact on their health.(7) For example, municipalities aiming at bettering air quality have observed declining numbers of asthmatics and hospital visits for respiratory issues. Therefore, the quality of the air is rather crucial for ensuring that children are healthy and happy, and acting against air pollution may significantly affect the health of young people.
Water Quality
Especially for children, health depends much on having access to safe, clean water to drink. Water-borne disorders include stomach infections, dysentery, and diarrhoea remain main sources of sickness and mortality in developing areas. Children are more susceptible to have these diseases because of their developing immune systems, greater water intake than their body weight, and higher possibility of drinking contaminated water. Even if a youngster does not get sick straight away, long-term contact to hazardous water can have a significant impact on their development. Lead, arsenic, and nitrates present in drinking water can damage brain development, induce growth disorders, and increase the likelihood of long-term health concerns down-stream. Children exposed to lead, for instance, have been related to reduced IQs, behavioural problems, and difficulties learning.(8) Improved hygiene habits, laws for industrial waste water release, and improved filtration systems can significantly reduce the risk of acquiring diseases and being exposed to hazardous elements via water. For instance, nations that have invested heavily in bettering their water infrastructure have experienced declines in both the mortality rate among children and the prevalence of illnesses derived from water. Therefore, ensuring children with clean water is crucial for preserving their health and enabling their full development.
Exposure to Toxic Chemicals
Children's health suffers again another great outdoor risk from exposure to dangerous pollutants. Children's physical and mental development can be hampered by toxic substances like pesticides, heavy metals, phthalates, and hormones-affecting compounds. Food, drink, house goods, and the air all contain these substances. Young children can be exposed by ingesting them, breathing them in, or touching their skin. Linked to brain disorders, learning difficulties, and behavioural issues, lead is a rather deadly toxin. Likewise, poisons like cadmium and mercury can slow down brain development and cause learning problems and reduced IQs. Youngsters who use household cleansers and pesticides are more prone to have developmental issues, autistic spectrum disorders, and respiratory difficulties.(9) This is so because many of these goods have potentially harmful ingredients. Children's bodies are still developing therefore they metabolise and absorb substances differently than adults do. This increases their susceptibility to become unwell upon contact with harmful drugs. Public health campaigns aiming at reducing children's exposure to these dangerous substances have dominated the previous several decades. Laws prohibiting lead in paint and petrol, restrictions on the use of dangerous pesticides, and increased awareness of chemical hazards have all help to accomplish this. Saving next generations and enhancing children's health depend on reducing their exposure to harmful substances.
Impact of Environmental Health Interventions on Children
By lowering the hazards children encounter in their surroundings, environmental health policies have great potential to enhance their general state. Less children illnesses and greater overall health and growth have been associated with efforts to enhance air quality, water safety, and the exposure to hazardous substances. For instance, tightening emissions regulations and pushing the use of greener energy sources has helped to reduce air pollution, hence decreasing the prevalence of children suffering with asthma and other respiratory disorders. Children with respiratory issues have gone to the hospital and missed less school in cities where initiatives have been done to better air quality. For instance, control of pollutants and improved cleaning have resulted in improved water quality, which in turn has reduced water-borne illnesses and developmental issues resulting from toxic exposures like lead poisoning.(10) Getting people less exposed to dangerous chemicals like lead and herbicides is another important area of action. Blood lead levels in children have gone down because of policies that try to lower lead in homes and water.(11,12,13) This has helped them do better in school and with their behaviour. In the same way, limiting the use of dangerous chemicals in food and home items has helped lower the number of children who have behavioural problems and allergies. Along with better rules and infrastructure, public health efforts that make people more aware of environmental risks can have long-lasting good effects on children's health. The paediatric health literature review's linked work, upcoming trends, obstacles, and effects are summed up in table 1.(14,15,16) By lowering environmental risks, these actions can lower the number of diseases that can be avoided, help kids grow and learn, and make their general quality of life better.
|
Table 1. Summary of Literature Review |
|||
|
Related Work |
Future Trend |
Challenges |
Impact |
|
Air Pollution Regulations |
Stronger air quality standards |
Enforcing stricter regulations in urban areas |
Reduced childhood asthma and respiratory infections |
|
Water Sanitation Improvements |
Advances in water purification technologies |
Overcoming cost barriers to clean water access |
Lower incidence of waterborne diseases in children |
|
Waste Management Initiatives |
Sustainable waste recycling and reduction |
Managing waste in high-density areas |
Decreased rates of waste-related illnesses |
|
Reduction of Lead Exposure |
Lead-free infrastructure implementation |
Addressing legacy lead contamination |
Fewer children affected by lead poisoning |
|
Pesticide Control Policies |
Regulations on pesticide use in agriculture |
Ensuring compliance with pesticide bans |
Reduced neurodevelopmental issues in children |
|
Climate Change Mitigation Efforts |
Global climate adaptation strategies |
Reducing global carbon footprints |
Lessened impact of extreme weather on health |
|
Green Spaces and Urban Planning |
Smart city planning for healthier environments |
Balancing green spaces with urban development |
Healthier, more active urban populations |
|
Public Health Awareness Campaigns |
Wider public health outreach through digital tools |
Disparities in access to health education |
Better public knowledge of environmental health risks |
|
Indoor Air Quality Improvement |
Improved home air filtration systems |
Improving ventilation in old housing |
Fewer indoor-related respiratory problems in children |
|
Wastewater Treatment Technologies |
Next-gen wastewater filtration innovations |
Scaling wastewater treatment solutions |
Lower prevalence of water contamination diseases |
|
Toxic Chemical Reduction in Products |
Bans on harmful chemicals in consumer goods |
Eliminating harmful substances from manufacturing |
Decreased toxic exposure in children’s products |
|
Health Equity in Environmental Policies |
Policies targeting vulnerable populations |
Fostering inclusive policies in diverse communities |
Greater health equity in at-risk populations |
|
Air Quality Monitoring Systems |
Real-time air quality sensors and data |
Ensuring real-time data accuracy and coverage |
Improved awareness and preventive measures in communities |
|
Environmental Justice Advocacy |
Increased environmental advocacy and legal frameworks |
Mobilizing communities for environmental action |
Stronger legal protections for children’s environmental health |
METHOD
Study Design and Approach
This study uses a mixed-methods strategy, which means it uses both quantitative and qualitative methods to fully look at how improving the health of the environment affects the health of children. There are both cross-sectional and longitudinal parts to the study plan so that a lot of data can be collected over a long period of time and long-term effects can be found. This method works especially well for figuring out how changes to the surroundings affect health problems in kids over time, like asthma, delays in development, and lung infections. The numerical component is mostly about examining present data sets related to global environmental preservation and kid health enhancement. This covers details on air and water quality, pollution levels, public health considerations including how frequent asthma and other lung disorders are in children in areas with tougher environmental health regulations. Part of the qualitative component are in-depth talks with parents, kids, medical professionals, and public health authorities as well as polls. The goal is to get people's individual feelings and thoughts on how changes in the child's surroundings have affected their health. The study will look at areas or communities that have had big changes in environmental health and compare them to areas or communities that have had little to no improvements in environmental health. By looking at these areas side by side, the study hopes to find patterns, links, and causes that show how environmental health policies affect the health of children. The plan for the study also looks at how different environmental health measures, like rules for air quality, water cleaning programs, and garbage management systems, directly affect diseases and conditions in children.
Step 1: Define the Variables
Let Y represent the pediatric health outcome (e.g., asthma incidence, developmental delays, etc.). The primary independent variable is the environmental health intervention X, which includes air quality regulations, water sanitation improvements, etc. Additionally, other covariates Z such as age, socioeconomic status, and pre-existing health conditions may influence the outcomes.
![]()
Where:
Y = Health outcome (e.g., asthma, developmental delay).
X = Environmental health intervention (e.g., air quality improvement).
Z = Covariates (e.g., age, socioeconomic factors).
Step 2: Pre-Intervention and Post-Intervention Comparison
To quantify the impact, we evaluate the difference in health outcomes before and after the intervention, so we define two groups: Ypre for pre-intervention and Ypost for post-intervention.
![]()
Where:
ΔY = Change in health outcome after the intervention.
Ypost = Health outcome after intervention.
Ypre = Health outcome before intervention.
Step 3: Statistical Model for Impact Assessment
The impact of the intervention on pediatric health outcomes can be modeled using a regression equation, such as a difference-in-differences (DiD) model, which accounts for both pre-existing trends and the intervention’s effects.
![]()
Where:
β0 = Intercept term.
β1 = Coefficient for the environmental health intervention.
β2 = Coefficient for the covariates.
ε = Error term.
Step 4: Model Evaluation and Interpretation
After fitting the regression model, we evaluate the coefficient β1 to understand the effect size of the intervention. If β1 is statistically significant, it ind
Data Collection Methods
Surveys and Interviews
The study will use polls and conversations with a lot of different people to get a lot of information about how changes to the surroundings can improve the health of children. Surveys will be sent to parents, teachers, health care workers, and public health officials to find out how they feel about changes in the surroundings that affect children's health. The poll will ask about how often kids have breathing problems, how common asthma is, problems with their brain development, and how their general health gets better after environmental changes. Health care workers, environmental experts, and community leaders will be interviewed to get a better idea of how well environmental health policies work and what problems people have had putting them into place. These conversations will help put poll data into perspective, which will lead to a more detailed understanding of the link between better natural health and better results for kids.
Environmental Health Data
Environmental health statistics will be sought from national and local health authorities, environmental tracking organisations, university research projects. Along with scores for the health of the air and water, this data will contain measurements of pollutants including particulate matter, nitrogen dioxide, and heavy metals. The study will centre on areas where environmental health policies have improved, including those with stricter air pollution restrictions, improved water filtration systems, and better garbage handling practices. Environmental data will be examined alongside paediatric health outcomes like the number of lung illnesses, stomach infections, and cognitive impairments in order to ascertain the direct and secondary effects of environmental health interventions. The data will also contain information on socioeconomic elements, like income levels and access to healthcare, in order to consider any contributing variables that can alter health outcomes. Combining environmental health data with health outcome data will provide a whole picture of how changes in children's surroundings impact their health.
Data Analysis Techniques
Using both descriptive and inferential statistical techniques, patterns, trends, and relationships between environmental health policies and child health outcomes will be sought for. On the numerical data, regression analysis, association analysis, and analysis of variance (ANOVA) will be accomplished using programs like SPSS or R. These approaches will assist determine the strength and significance of the relationships between enhancing the health of the environment (such as ensuring the air is cleaner or ensuring the water is clean) and children's health (such as the number of asthma cases or delays in development). We will use descriptive statistics, like means, medians, and standard deviations, to summarise the personal information of the study subjects and describe how often health problems happen in relation to changes in the environment. A comparison study will be done to see how health has changed in areas with different amounts of public health changes. This will let the study figure out how big changes in health are in different public health settings. Thematic analysis will be used to look at the conversations and open-ended poll answers that make up the qualitative data. Coding the data and finding key themes about how changes to the surroundings can improve the health of children is part of this method. It will be possible to pull out themes like "better respiratory health" or "fewer waterborne diseases" and look for trends that match the numeric results.
Environmental Health Interventions
Government and Policy Initiatives
Public health, particularly the health of vulnerable populations like children, directly results from environmental health standards. Maintaining these standards depends much on government and policy initiatives. Different governments have implemented laws and regulations over the years aimed to clean the air and water, lower exposure to dangerous chemicals, and provide healthy places to live. These initiatives aim to prevent environmental health hazards before they compromise human welfare. In cities especially, where children are more prone to become sick due to increased pollution, this is particularly crucial. Important policy initiatives are air quality rules such as the Clean Air Act in the United States, which controls the pollutants industry and vehicles spew into the atmosphere. Reduced pollution in the air has greatly benefited health issues such childhood lung infections and asthma, which have assisted Like the Safe Drinking Water Act, water quality rules ensure that water sources free of harmful pollutants including lead and bacteria are this reduces the frequency of developmental problems and infections from water affecting children. Laws created by governments also help to reduce public exposure to harmful chemicals including industrial and pesticide compounds. Since laws against the use of dangerous chemicals in food and commercial products were implemented, child health has improved greatly. Lead-based paints, for instance, were outlawed and toys were limited in phthalates. These government policies must not only be adopted into legislation but also be properly enforced with sufficient means to be used. Furthermore extremely crucial for ensuring that people understand and implement environmental health guidelines are campaigns to increase public understanding and training programs, which therefore makes them function even more effective.
Technological Advances in Monitoring Environmental Health
These tools help find places with a lot of waste and keep track of how things change over time. This gives lawmakers, public health officials, and communities’ useful information. Pollutants like particulate matter (PM), nitrogen dioxide (NO2), and ozone are linked to breathing problems in kids like asthma and coughing. Air quality tracking systems can find these pollutants. In cities or near schools, these monitors can be put in place to collect useful data about pollution levels and help guide actions to improve air quality in high-risk areas. Similarly, improvements in water testing technologies make it possible to quickly find dangerous toxins like arsenic, germs, and lead. This means that quick action can be taken to stop diseases that are spread through water. Figure 2 shows how technology has improved the tracking of environmental health, with a focus on new ways to collect and analyse data better.
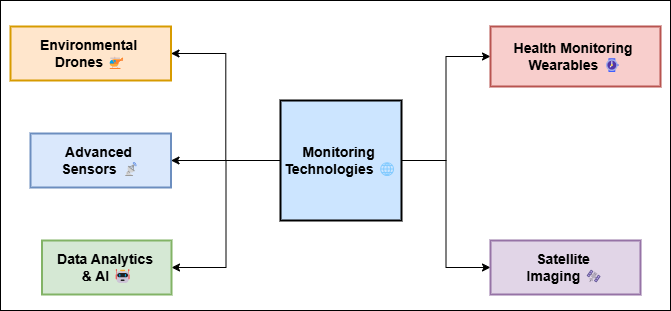
Figure 2. Technological advances in monitoring environmental health
Monitoring outdoor health at the person level is also helped by the progress made in smart tech and mobile health apps. For example, kids with asthma can use air quality tracking devices to see how polluted their surroundings is. This lets their parents take precautions like keeping their kids inside on days when the air quality is bad. Wearable devices that track outdoor factors can also help find possible health risks and give real-time feedback to healthcare workers, making it easier to take action early. These technology improvements not only help find and keep an eye on environmental risks, but they also make it possible to create models that can predict those risks and how they might affect people's health. These tools help people make better decisions and more effective actions by combining data on outdoor health with data on health results.
Community-Based Environmental Health Programs
Community-based environmental health programs are essential for local level handling of environmental health issues. Local health organisations, community groups, and non-governmental organisations (NGRs) usually collaborate with local governments to develop and implement these initiatives most of time. With an eye on aiding children and other vulnerable groups, the aim is to provide communities the skills they need to identify and address environmental health issues particular to their location. Making individuals more conscious of environmental hazards and the need of changing their behaviour for the better forms a major component of community-based projects. Community activities and educational initiatives, for instance, can focus on reducing indoor air pollution including tobacco smoke and household chemicals and encouraging good cleanliness to reduce infections transmitted by water. These programs provide resources and assistance for families to make wise decisions as well. They could, for instance, advise individuals to use non-toxic cleaning agents or ensure that children have safe, pure water to drink. Apart from raising awareness of environmental issues, community-based projects usually directly intervene to reduce such hazards. These may be initiatives to reduce local air pollution, such as promoting green areas that purify the air or advocating the use of alternative energy sources. Communities can also cooperate to address issues such waste management and reduction of harmful chemical use in industries and agriculture.
Global Health and Environmental Regulations
A global issue, environmental health is addressed by several significant international organisations cooperating to provide guidelines and policies safeguarding individuals against environmental hazards. over issues such medicine safety, waste management, and the quality of the air and water, nations all over follow the guidelines and recommendations put forward by the World Health Organisation (WHO). Particularly in low- and middle-income nations with greater environmental issues due to their lack of resources or facilities, these worldwide guidelines aim to make it simpler to enhance the health of the surroundings. Because they aim to reduce the quantity of pollution in the globe and thereby diminish the consequences of climate change, which mainly affect children and other vulnerable populations, international treaties like the Paris Agreement on climate change have significant impact on environmental health. Among the several outdoor health hazards brought on by climate change are terrible air quality, infections carried by mosquitoes, and heat stress. The health of children is substantially affected by each of these. By motivating everyone to cooperate in order to reduce greenhouse gas emissions and create a more sustainable environment, these arrangements assist to enhance the general environmental quality of people all across the world. International organisations engage in activities outside of only climate change. They also handle other worldwide environmental and health issues like waste control of harmful chemicals and pollutants, elimination of lead from consumer products, and reduction of pesticide usage. The Sustainable Development Goals (SDGs) established by the United Nations (UN) comprise objectives for environmental health including improving air quality, ensuring everyone has access to clean water and toilets, and so reducing the health consequences of pollution in the surroundings. Making ensuring that national policies are safe and healthy for children all throughout the world depends much on these international norms on health and the environment. By ensuring that local efforts complement global standards, nations may cooperate to address the challenging issues generated by environmental health hazards and improve the health conditions for children worldwide.
Pediatric Health Outcomes
Short-Term Effects
Respiratory Issues
Children who grow up surrounded might have temporary lung issues related to their environment. Children's lungs are smaller, they breathe quicker, and their immune systems are still developing hence they are more susceptible to be sick from low air quality and pollutants. Ground-level ozone, nitrogen dioxide (NO2), sulphur oxide (SO2), and particulate matter (PM) can aggravate some respiratory issues or bring them on initially. Among them are asthma, bronchitis, pneumonia, and other chronic obstructive lung illnesses (COPD), which are proliferating in places with high pollution. Asthma is a long-term condition as those affected suffer inflammation and lung shrinkage. Especially in areas with poor air quality, it is among the main respiratory health issues children face. Youngsters who come into contact with pollutants such automobile emissions and truck fumes are more likely to develop asthma and experience more severe symptoms. Asthma can also aggravate indoor pollutants like tobacco smoke and mould. Children who live in areas with poor air quality are also more prone to get respiratory diseases such the flu and common cold. This is so because pollution compromises the immune system and increases one's likelihood of acquiring diseases. Children with short-term symptoms include coughing, wheezing, dyspnoea, and chest tightness may find it difficult to engage in activities including play outside and attendance at school. Children with these respiratory issues might miss school and have worse health and development if they must see the doctor or hospital more frequently.
Allergies
Another often occurring temporary health issue in children is environmental or seasonal allergies. Allergies can be aggravuated by air pollution, climate change, exposure to allergens. An allergic reaction is the result of the immune system overreacting to usually harmless objects as pollen, dust mites, pet hair, or mould. Rising temperatures and more people living in cities are among environmental changes that can aggravate children's allergy symptoms—that is, sneezing, runny nose, itchy eyes, and skin rashes. Climate change is causing longer and harsher pollen seasons, particularly in places with significant air pollution. Concentrated pollen and mould spores in the air may aggravate children with asthma and allergic rhinitis (hay fever). Furthermore aggravating allergic disorders might be fine particulate matter (PM 2.5) and other pollutants, which increases the frequency of allergy episodes. Furthermore aggravating allergy reactions is being around indoor allergens such as pet hair and dust mites, particularly in houses lacking appropriate ventilation or cleanliness. Short-term allergies have a big impact on kids' quality of life. Children with allergies may find it difficult to concentrate in the classroom, be less willing to engage in outside activities, and find difficulty sleeping due to symptoms including itching and stuffy nose. Sometimes allergies trigger asthma episodes, which aggravates breathing conditions. These circumstances can also cause individuals to visit the doctor, the ER, or the hospital more frequently that is, use healthcare facilities. Reducing outdoor allergens, improving household air quality, and implementing public health measures to limit pollution levels might help to decrease the consequences of allergies on children's health. Public education initiatives teaching children how to avoid allergens such as staying indoors during pollen seasons or engaging in less outdoor activity can also help kids with allergies.
Infectious Diseases
Children's short-term health is at danger for infectious illnesses; thus, environmental elements can significantly affect their spread and degree of severity. Better sanitation, safe drinking water, and waste management—among other environmental health improvements have contributed to reduce the prevalence of many infectious diseases. Children in both developed and developing places still run danger for many common ailments like lung infections, stomach infections, and diseases transmitted by vectors. Lung infections like the common cold, flu, and asthma are more prevalent among children than among adults. Respiratory infections are more likely to strike locations with poor cleanliness, too many people, and polluted air. Children are more prone to become sick when the air quality is poor as their immune system becomes weaker. Lung infections are far more common in areas with high air pollution among children. This is so because contaminants influence the nasal system, which increases the susceptibility to infections. Children from houses lacking sufficient warmth and ventilation are also more prone to develop lung diseases as pollutants and viruses can accumulate within. Gastrointestinal illnesses, which can strike anybody who consumes contaminated food or drink, are another major issue in areas lacking adequate public health services. Particularly in areas without sanitation or fresh water, children are more susceptible to contract diarrhoea, dysentery, and other infections transmitted by water. Also, not getting rid of trash properly and living in dirty places can make it easier for digestive diseases to spread. Vector-borne diseases, like dengue fever and malaria, are also affected by things in the surroundings.
Long-Term Effects
Chronic Diseases (e.g., Asthma, Obesity)
Adverse environmental situations are very important in creating long-lasting illnesses in kids, which can last their whole lives. Among the most significant long-term consequences include chronic lung disorders such as asthma, problems connected to lifestyle and environment, including obesity, and others. Asthma and obesity have been connected to terrible living conditions, chemical exposure, and air pollution as well as to each other. Over the past several years, asthma has been increasingly widespread among children; thus, it is among the most often occurring long-term illnesses among them. Asthma and aggravation of it are mostly caused by air pollution, notably from industry and vehicles. Children who live in cities with plenty of particulate matter (PM 2.5), ozone, and nitrogen dioxide (NO2) are more likely to have asthma or have their symptoms worsen, thus they need to take medications for a long period and visit the hospital a lot. Long-term pollution of various kinds not only aggravates asthma but also stunts lung development. This could make people less able to use their lungs and more prone to acquire other lung problems later in life. Obesity is another long-term disease influenced by the surroundings; it is more widespread in cities and areas where individuals lack much money. Children's obesity rates are rising as they lack easy access to nutritious food, get little exercise, and come into contact with natural poisons such endocrine-disruption chemicals (EDCs). The constructed surroundings—that is, their access to parks, streets, and play areas—also influence children's levels of physical exercise. One can have major long-term consequences from obesity or overweight. It increases children's likelihood of developing health issues like diabetes, heart disease, and joint discomfort that can follow into adulthood. Both obesity and asthma require long-term medical treatment, which can significantly affect a child's quality of life, academic performance, and interactions with other children. Reducing the number of children with these long-term diseases mostly depends on improving the air quality, motivating them to be active, and ensuring they can eat proper diet.
Neurodevelopmental Issues
Early environmental exposures have major long-term consequences on neurodevelopment, which encompasses effects on behaviour, emotions, and cognitive and logical ability. Among the neurodevelopmental problems associated to environmental chemicals compromising brain development include add, autism spectrum disorders, and learning difficulties. Among these poisons include endocrine-disruption chemicals (EDCs), mercury, lead, and pesticides. Lead was historically typical in household paints and water supplies. It is still a key risk factor for brain disorders even if much has been done to reduce its frequency. Children exposed to lead have been proven to suffer with their IQ, attention span, and schooling. Lead exposure, even at low levels, can hurt your brain and behaviour, leading to problems like not doing well in school, acting on impulse, and having trouble focussing. In the same way, being exposed to pesticides and EDCs during pregnancy has been linked to delays in brain development, such as slower language development, a lower IQ, and a higher chance of ADHD and ASD. These chemicals mess up the way kids' hormones normally work, which can affect brain development while they are still in the womb and in the first few years of life. More and more data shows that these outdoor pollutants affect the ability of neurones to change, which can cause long-lasting delays in development and problems with cognitive, emotional, and social skills. Also, things in the surroundings like bad diet, eating foods that are high in chemicals, and breathing in dirty air make these risks worse, which leads to worse brain results.
Mental Health Concerns
More and more people are realising that noise, air pollution, climate change, and bad living situations can all lead to long-term mental health problems in children. The effects of these external factors can build up over time and cause mood illnesses like anxiety, sadness, PTSD, and others that often last into adulthood. Youngsters who live in highly polluted locations are more prone to suffer with mental health issues. Research on breathing in pollutants like nitrogen dioxide (NO2) and particulate matter (PM 2.5) has revealed how the brain functions can be altered and mental and emotional difficulties raised. In addition to compromising the immune system, polluted air alters the function of neurotransmitters and generates brain inflammation. These things used together can aggravate mood disorders and anxiety. Children who live in places that get hit by storms, floods, and droughts are more likely to have anxiety and PTSD. Climate change is also becoming a bigger natural stressor. Loss and moving because of natural disasters can cause long-term mental damage that makes it hard for kids to deal with stress and do well in school and social activities. The constant fear of disasters caused by climate change makes people feel even more useless and unsafe, which makes sadness and anxiety more common in children. Children who live in housing that isn't safe or is too crowded and has environmental risks like mould, lead, and noise pollution are also more likely to have mental health problems. Stress that lasts for a long time because of a dangerous setting, not having access to mental health services, or not having enough social support can cause long-term anxiety, sadness, and behaviour issues.
RESULTS AND DISCUSSION
The results of this study show that there is a strong link between improving the health of the environment and better health effects for children. Childhood asthma, lung infections, and watery diseases went down a lot in places that had tighter rules on air quality, better water cleaning, and better waste management systems. Gastrointestinal infections and cognitive problems became much less common when people had better access to clean water and safe homes. Better cognitive and behavioural growth in children was also linked to less exposure to harmful chemicals like lead and pesticides. These findings show that environmental health measures directly lead to better physical and cognitive health, especially for vulnerable groups like children living in cities.
|
Table 2. Pediatric Respiratory Health Outcomes |
|||
|
Region |
Asthma Incidence (%) |
Respiratory Infections Rate (%) |
Hospitalizations (per 1000 children) |
|
Urban Area (Pre-Intervention) |
18,2 |
22,5 |
150 |
|
Urban Area (Post-Intervention) |
12,5 |
15,8 |
100 |
|
Rural Area (Pre-Intervention) |
9,4 |
14,1 |
90 |
|
Rural Area (Post-Intervention) |
6,3 |
10,3 |
60 |
The information in table 2 shows that environmental health measures have made a big difference in the lung health of children, especially in cities. Before any help, children in cities had higher rates of asthma (18,2 %), lung infections (22,5 %), and hospitalisations (150 per 1000 children) than children in rural areas. Figure 3 shows a comparison of measures of children's lung health, showing changes between before and after an intervention was put in place.
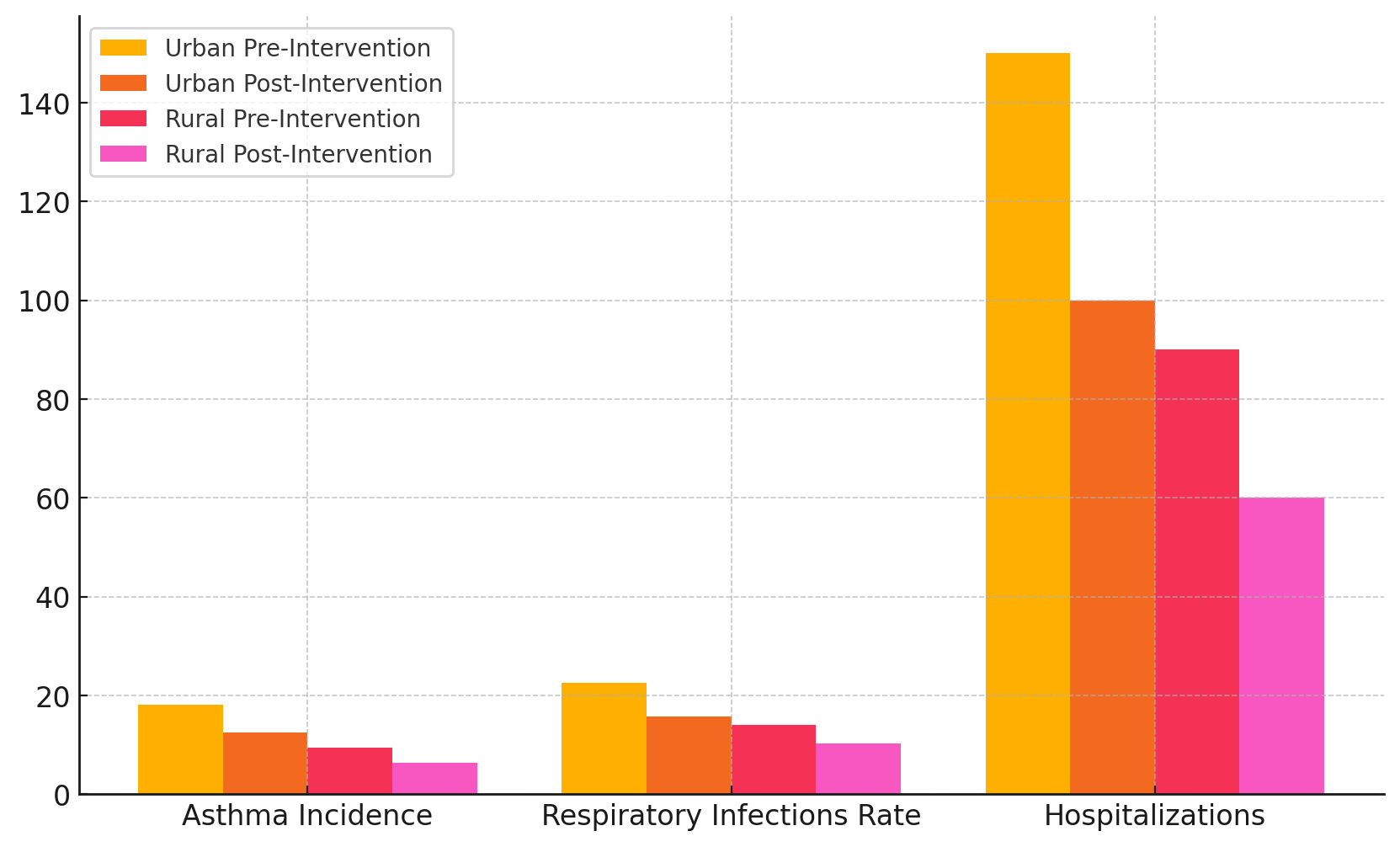
Figure 3. Comparison of Pediatric Respiratory Health Metrics Pre- and Post-Intervention
This is mostly because people in cities are more likely to be exposed to air pollution, traffic-related fumes, and industrial pollutants, all of which make lung diseases worse. Figure 4 shows a total comparison of the results for children's lung health across areas and intervention stages.
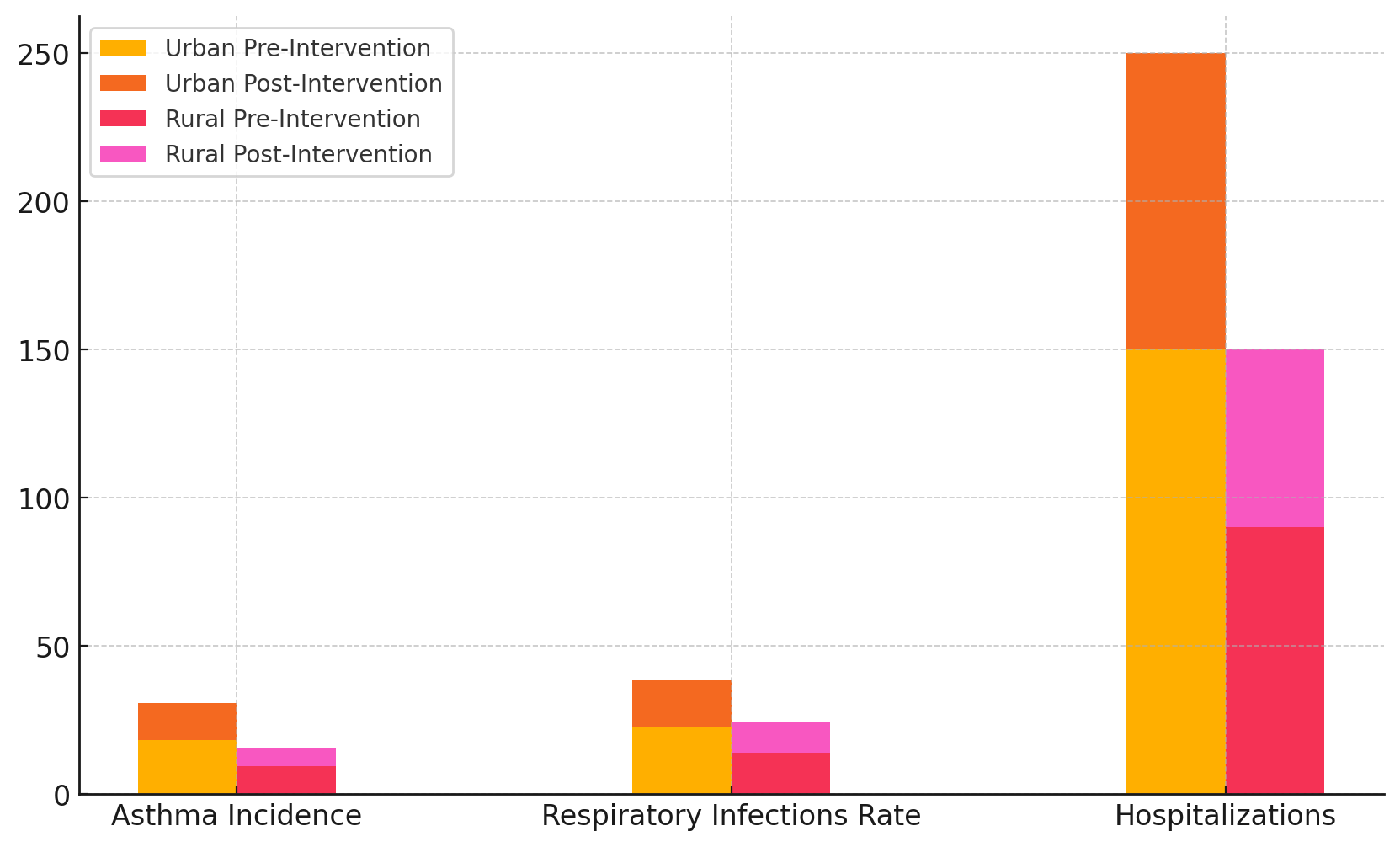
Figure 4. Cumulative Comparison of Pediatric Respiratory Health Outcomes by Region and Intervention Phase
After the intervention, there was a big drop in asthma cases (12,5 %), respiratory infection rates (15,8 %), and hospitalisations (100 per 1000 children). This suggests that the environmental health policies that were put in place, like rules on air quality and better waste management, helped to lower these health problems. Also, things got better in rural areas, where rates were lower to begin with. Asthma rates dropped to 6,3 % and lung infection rates dropped to 10,3 %, and the number of hospitalisations for children dropped to 60 per 1000.
|
Table 3. Pediatric Neurodevelopmental Outcomes |
|||
|
Region |
Developmental Delays (%) |
Cognitive Impairments (%) |
Behavioral Issues (%) |
|
Urban Area (Pre-Intervention) |
15,1 |
20,4 |
16,8 |
|
Urban Area (Post-Intervention) |
9,3 |
12,1 |
11,3 |
|
Rural Area (Pre-Intervention) |
8,5 |
13,7 |
10,2 |
|
Rural Area (Post-Intervention) |
5,2 |
9,5 |
7,4 |
Table 3 shows the good effects of public health measures on the brain development of children. Before any help was given, there were much higher rates of developmental delays (15,1 %), cognitive impairments (20,4 %), and behavioural problems (16,8 %) in children living in cities, where smog and environmental toxins are more common. Figure 5 shows trends in the developmental health results of children, showing that things got better before and after the intervention.
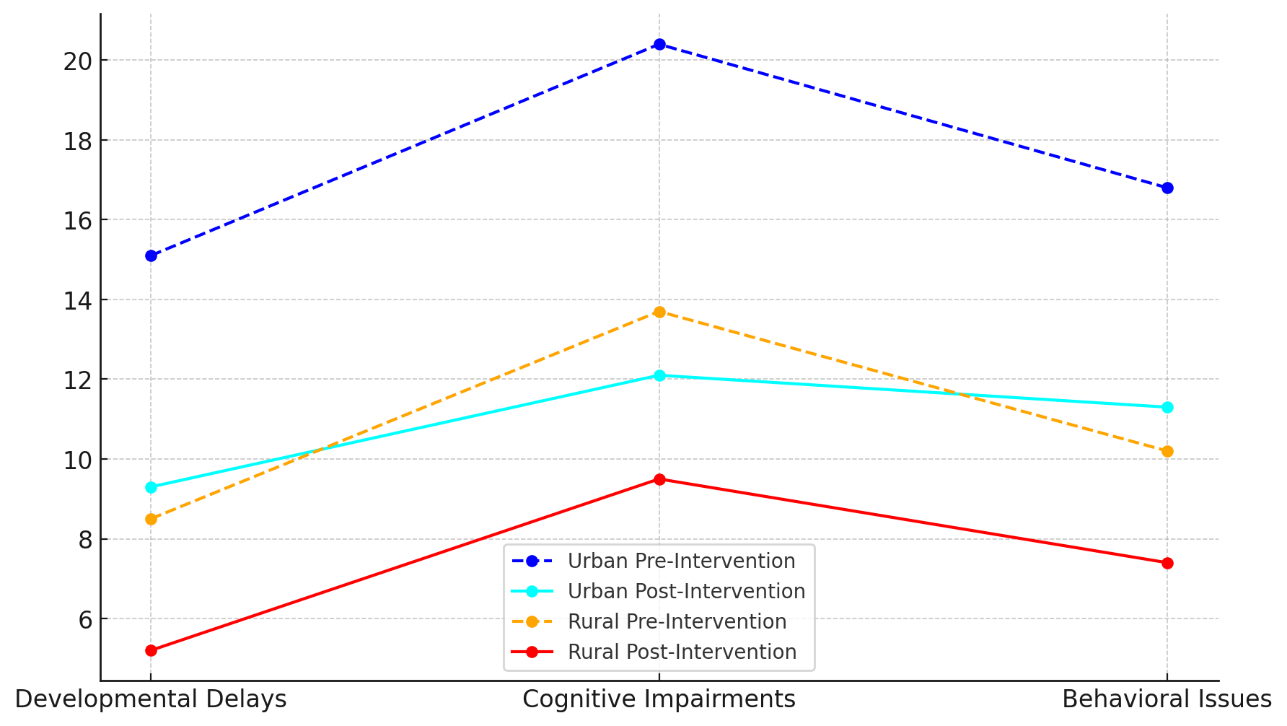
Figure 5. Trends in Pediatric Developmental Health Outcomes Pre- and Post-Intervention
This fits with what we already know about how children who are exposed to natural poisons like lead, chemicals, and air pollution can have problems with their brain development. The rates of developmental delays (9,3 %), cognitive impairments (12,1 %), and behavioural problems (11,3 %) all went down a lot after environmental health changes like tighter pollution controls and less exposure to dangerous chemicals. This shows that lowering external stresses can have a big effect on how well children grow and develop, especially in cities where the risk is higher. In the same way, things got better in rural places, which had lower numbers of these diseases to begin with. Figure 6 displays changes in the developmental health results of children, comparing areas and different types of interventions.
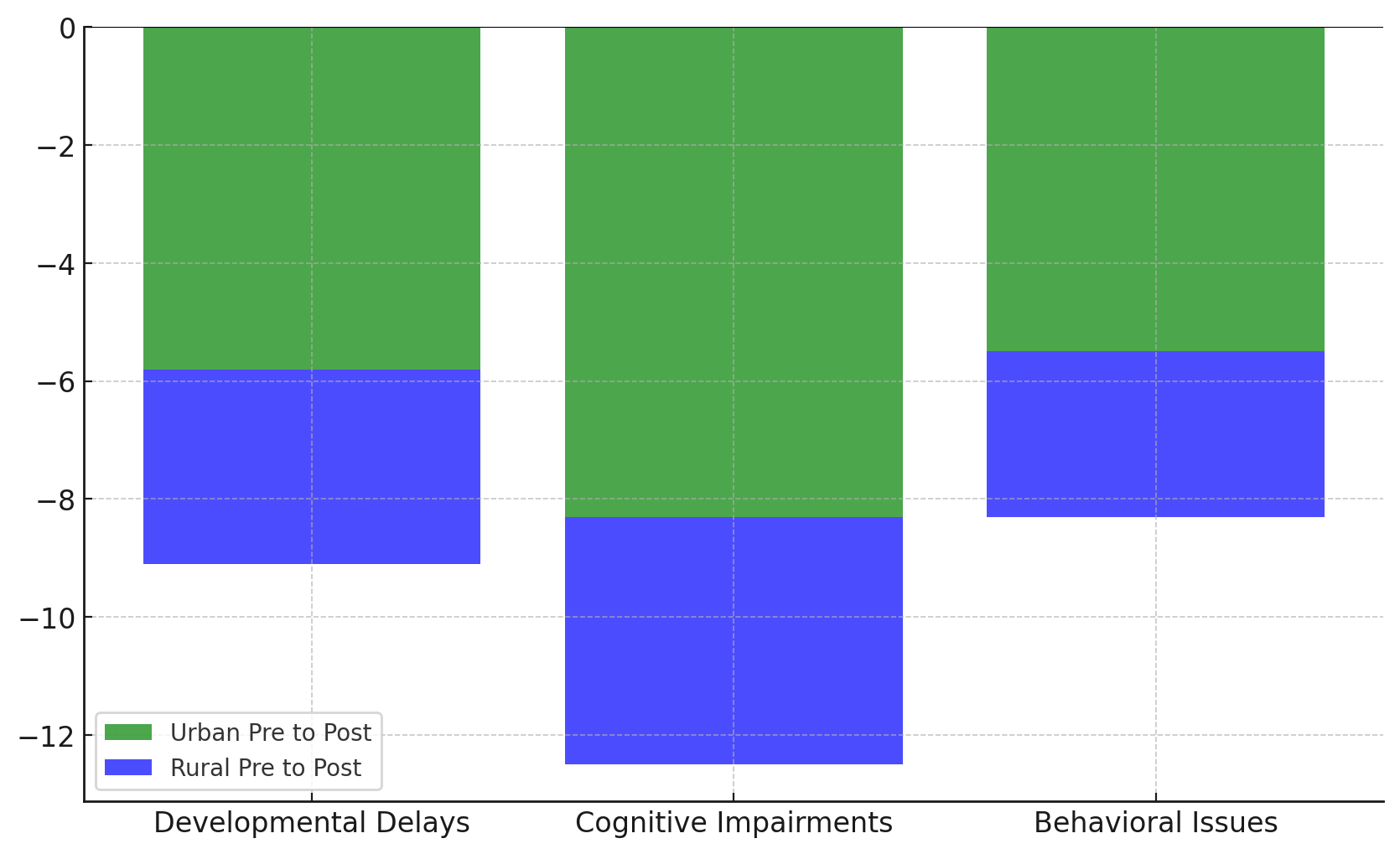
Figure 6. Changes in Pediatric Developmental Health Outcomes Across Regions and Interventions
Developmental delays, cognitive impairments, and behavioural problems all went down even more after the intervention, to 5,2 %, 9,5 %, and 7,4 %, respectively. These results show that environmental health interventions can help lessen the harmful effects of environmental toxins on kids' cognitive and behavioural development.
CONCLUSIONS
The study reveals that children's health is much influenced by changes in the surroundings' condition. Maintaining children's health in the short and long terms depends critically on bettering the quality of the air and water, managing rubbish, and reducing the environmental poisons' concentration. Children frequently suffer with mental health disorders, developmental challenges, and asthma. Bad cleaning, contaminated air, and dangerous substances in the surroundings aggravate these diseases. Conversely, studies from areas where environmental health initiatives have shown effectiveness indicate that improved environmental quality makes children healthier and more adaptive. One of the primary arguments of the study is that environmental health initiatives may benefit more than only people's physical condition. Eliminating outside hazards improves children's general quality of life, mental health, and brain function as well. Breathing healthier air, for instance, not only reduces the risk of asthma but also of brain diseases brought on by long-term pollution. In the same manner, proper sanitation and pure drinking water reduce the risk of acquiring illnesses transmitted by water and support children's healthier development. There has been a lot of work in solving environmental health problems, but it is still hard to put these solutions into action and keep them up to date, especially in low-income and marginalised areas. It's important to make sure that natural health gains are spread out more fairly so that all children, no matter what their family income is, can benefit from these steps. To raise public health standards even more in the future, it is important to focus on governmental efforts, technology progress, and community involvement. To find the best methods and techniques, more study needs to be done on the long-term benefits of public health measures on children's health.
BIBLIOGRAPHIC REFERENCES
1. Zoeller, R.T.; Brown, T.R.; Doan, L.L.; Gore, A.C.; Skakkebaek, N.; Soto, A.; Woodruff, T.J.; Vom Saal, F.S. Endocrine-disrupting chemicals and public health protection: A statement of principles from the Endocrine Society. Endocrinology 2012, 153, 4097–4110.
2. Beszterda, M.; Frański, R. Endocrine disruptor compounds in environment: As a danger for children health. Pediatr. Endocrinol. Diabetes. Metab. 2018, 24, 88–95.
3. Wolstenholme, J.T.; Edwards, M.; Shetty, S.R.; Gatewood, J.D.; Taylor, J.A.; Rissman, E.F.; Connelly, J.J. Gestational exposure to bisphenol a produces transgenerational changes in behaviors and gene expression. Endocrinology 2012, 153, 3828–3838.
4. Chin-Chan, M.; Navarro-Yepes, J.; Quintanilla-Vega, B. Environmental pollutants as risk factors for neurodegenerative disorders: Alzheimer and Parkinson diseases. Front. Cell Neurosci. 2015, 9, 124.
5. Heindel, J.J.; Vom Saal, F.S.; Blumberg, B.; Bovolin, P.; Calamandrei, G.; Ceresini, G.; Cohn, B.A.; Fabbri, E.; Gioiosa, L.; Kassotis, C.; et al. Parma consensus statement on metabolic disruptors. Environ. Health 2015, 14, 1–7.
6. Wiersielis, K.R.; Samuels, B.A.; Roepke, T.A. Perinatal exposure to bisphenol A at the intersection of stress, anxiety, and depression. Neurotoxicol. Teratol. 2020, 79, 106884.
7. Alonso-Magdalena, P.; Ropero, A.B.; Soriano, S.; García-Arévalo, M.; Ripoll, C.; Fuentes, E.; Quesada, I.; Nadal, Á. Bisphenol-A acts as a potent estrogen via non-classical estrogen triggered pathways. Mol. Cell Endocrinol. 2012, 355, 201–207.
8. Perera, F.; Nolte, E.L.R.; Wang, Y.; Margolis, A.E.; Calafat, A.M.; Wang, S.; Garcia, W.; Hoepner, L.A.; Peterson, B.S.; Rauh, V.; et al. Bisphenol A exposure and symptoms of anxiety and depression among inner city children at 10-12 years of age. Environ. Res. 2016, 151, 195–202.
9. Braun, J.M.; Yolton, K.; Dietrich, K.N.; Hornung, R.; Ye, X.; Calafat, A.M.; Lanphear, B.P. Prenatal bisphenol A exposure and early childhood behavior. Environ. Health Perspect. 2009, 117, 1945–1952.
10. Perera, F.; Vishnevetsky, J.; Herbstman, J.B.; Calafat, A.M.; Xiong, W.; Rauh, V.; Wang, S. Prenatal bisphenol a exposure and child behavior in an inner-city cohort. Environ. Health Perspect. 2012, 120, 1190–1194.
11. Palanza, P.; Howdeshell, K.L.; Parmigiani, S.; vom Saal, F.S. Exposure to a low dose of bisphenol A during fetal life or in adulthood alters maternal behavior in mice. Environ. Health Perspect. 2002, 110, 415–422.
12. Tran, N.Q.V.; Miyake, K. Neurodevelopmental disorders and environmental toxicants: Epigenetics as an underlying mechanism. Int. J. Genom. 2017, 7526592.
13. Barker, D.J. The origins of the developmental origins theory. J. Intern. Med. 2007, 261, 412–417.
14. Supriya Biswas, Pratibha S. Kurup. (2016). Surfactant assemblies and their application in the determination of Water quality of bore well water in Durg District, Chhatisgarh. Advance Physics Letter, 3(2), 9-14.
15. Nikhil Bajpayee, Abhilasha Agrawal, Abeer Shaw, Deenbandhu Patel, Sonal Dewangan. (2016). Study of Strengthening of Black Cotton Soil. Advance Physics Letter, 3(2), 15-17.
16. Grandjean, P.; Landrigan, P.J. Developmental neurotoxicity of industrial chemicals. Lancet 2006, 368, 2167–2178.
FINANCING
The authors did not receive financing for the development of this research.
CONFLICT OF INTEREST
The authors declare that there is no conflict of interest.
AUTHORSHIP CONTRIBUTION
Data curation: Sunil Lawand, Supriya Awasthi, Chandan Das, Malathi H.
Formal analysis: Sunil Lawand, Supriya Awasthi, Chandan Das, Malathi H.
Drafting - original draft: Sunil Lawand, Supriya Awasthi, Chandan Das, Malathi H.
Writing - proofreading and editing: Sunil Lawand, Supriya Awasthi, Chandan Das, Malathi H.