doi: 10.56294/hl2023258
ORIGINAL
Strategies for the Implementation of Healthcare Education in Resource-Constrained Environments
Estrategias para la implantación de la educación sanitaria en entornos con recursos limitados
Jamuna KV1 ![]() , Mario Antony2
, Mario Antony2 ![]() , Vishal Biswas3
, Vishal Biswas3 ![]() , Srikant Kumar Dhar4
, Srikant Kumar Dhar4 ![]()
1JAIN (Deemed-to-be University), Department of Forensic Science. Bangalore, Karnataka, India.
2Krishna Institute of Medical Sciences, Krishna Vishwa Vidyapeeth “Deemed to be University”, Dept. of Emergency Medicine. Taluka-Karad, Dist-Satara, Maharashtra, India.
3School of Allied Health Sciences, Noida International University. Greater Noida, Uttar Pradesh, India.
4IMS and SUM Hospital, Siksha ‘O’ Anusandhan (Deemed to be University), Department of General Medicine. Bhubaneswar, Odisha, India.
Cite as: KV J, Antony M, Biswas V, Dhar SK. Strategies for the Implementation of Healthcare Education in Resource-Constrained Environments. Health Leadership and Quality of Life. 2023; 2:258. https://doi.org/10.56294/hl2023258
Submitted: 02-05-2023 Revised: 17-07-2023 Accepted: 13-10-2023 Published: 14-10-2023
Editor: PhD.
Prof. Neela Satheesh ![]()
ABSTRACT
Introduction: especially in areas with limited resources, better health outcomes depend much on healthcare education. Still, a shortage of money often makes it difficult for training initiatives to be successful. This essay examines many approaches to provide healthcare in these types of environments such that everyone receives quality treatment.
Method: extensive review of past studies was conducted with an eye towards how novel approaches including mobile health (health), telemedicine, and community-driven education models may be employed in concert. Case studies with minimal resources from Africa, Asia, and Latin America were examined in search of sensible means of implementing ideas. Data on healthcare access, educational impact, and sustainability were compiled and combined to provide ideas that may be implemented.
Results: the study revealed how people from many locations may collaborate using digital technologies such internet sites and mobile apps. Reaching individuals in remote regions and imparting greater health knowledge also depend much on community health workers (CHWs). Maintaining the longevity of the program also depended on close cooperation with nearby organisations.
Conclusions: in order to educate healthcare in areas with low resources, you must combine digital innovations and community-based models among other approaches. By means of mobile tools and enhanced local contacts, these locations may effectively fill in knowledge gaps in healthcare and enhance health outcomes. Researchers should aim to improve these models going forward so they may be applied on a greater scale and persist for a long period.
Keywords: Healthcare Education; Resource-Constrained Environments; Mobile Health; Community Health Workers; Digital Tools; Health Literacy.
RESUMEN
Introducción: especialmente en zonas con recursos limitados, la mejora de los resultados sanitarios depende en gran medida de la formación sanitaria. Sin embargo, la escasez de dinero suele dificultar el éxito de las iniciativas de formación. En este ensayo se examinan diversos enfoques para prestar asistencia sanitaria en este tipo de entornos de forma que todos reciban un tratamiento de calidad.
Método: se realizó una amplia revisión de estudios anteriores con la vista puesta en cómo pueden emplearse de forma concertada enfoques novedosos como la sanidad móvil, la telemedicina y los modelos educativos impulsados por la comunidad. Se examinaron estudios de casos con recursos mínimos de África, Asia y América Latina en busca de medios sensatos para poner en práctica las ideas. Se recopilaron y combinaron datos sobre el acceso a la atención sanitaria, el impacto educativo y la sostenibilidad para ofrecer ideas que puedan ponerse en práctica.
Resultados: el estudio reveló cómo personas de muchos lugares pueden colaborar utilizando tecnologías digitales como sitios de Internet y aplicaciones móviles. Llegar a personas de regiones remotas e impartir mayores conocimientos sanitarios también depende en gran medida de los trabajadores sanitarios comunitarios (TSC). Mantener la longevidad del programa también dependió de la estrecha colaboración con organizaciones cercanas.
Conclusiones: para educar sanitariamente en zonas con pocos recursos hay que combinar innovaciones digitales y modelos basados en la comunidad, entre otros enfoques. Gracias a las herramientas móviles y a la mejora de los contactos locales, estos lugares pueden colmar eficazmente las lagunas de conocimiento en materia de asistencia sanitaria y mejorar los resultados sanitarios. Los investigadores deben tratar de mejorar estos modelos en el futuro para que puedan aplicarse a mayor escala y persistir durante largo tiempo.
Palabras clave: Educación Sanitaria; Entornos con Recursos Limitados; Salud Móvil; Trabajadores Sanitarios Comunitarios; Herramientas Digitales; Alfabetización Sanitaria.
INTRODUCTION
Some people will find it difficult to reach education and healthcare as long as finances are restricted. Many issues such as inadequate funds, poor infrastructure, or trained medical professionals make it difficult to offer decent healthcare services and education in these locations. Many of these areas have healthcare systems struggling to meet the demands of rising populations, and most people lack the fundamental knowledge on how to maintain healthy. Lack of information can result in poor health outcomes, the spread of stopable illnesses, and a general reduction in life duration. In this regard, healthcare education becomes a crucial means of enhancing health outcomes by arming individuals with the knowledge required to prevent and handle common health issues. The challenging aspect is using these instructional strategies in areas with limited resources and where conventional teaching approaches might not be feasible.(1) Lack of healthcare education is especially evident in rural and isolated areas where people sometimes cannot access formal healthcare groups and experts. Communities are more prone to suffer avoidable health issues including starvation, infectious infections, and mortality of mothers and children without educational initiatives. Healthcare education initiatives must be tailored in these locations to fit the particular requirements and constraints of the local population. This sometimes requires innovative ideas that deviate from the conventional classroom approach. This means that, with an eye towards teaching people about health and altering their behaviour, healthcare education must be adaptable and easily available. Better self-care and general health follow from individuals having the knowledge necessary to make wise decisions regarding their health.(2) Teaching people about health care in these locations can benefit from technology as well as from mobile health (mHealth) apps and telemedicine. These solutions can assist overcome issues resulting from distance and inadequate infrastructure by delivering materials and information right to individuals's cell phones or community centres. Even in areas without resources, more and more individuals carry cell phones. This makes them a fundamental instrument for transmitting knowledge. Mobile health applications let communities access current health information, be reminded of immunisations and visits, and learn about critical health practices. Conversely, telemedicine helps consumers obtain professional advice from doctors and nurses without having to travel great distances to receive treatment.
In regions with low resources, community health workers (CHWs)(3) are also quite crucial for healthcare education. Often serving as a liaison between medical professionals and the communities they assist, these individuals ensure that health information is presented in a manner appropriate for every culture and clearly. At the community level, CHWs may educate individuals about health; they can also participate in initiatives to advance health and assist in the halt of the spread of deadly illnesses. They can determine and satisfy the particular health demands of their patients as they are familiar with the members of the society. This makes them quite significant component of any program for healthcare education. Furthermore, if healthcare education initiatives apply community-based learning strategies including local leaders and groups, they may reach and assist far more individuals. Working with already-known and trusted members of the society helps health education initiatives establish trust and ensure the content is pertinent to the local population. Because they frequently more closely fit local culture and make use of local resources, these models also stay longer. Giving communities the tools they need to participate in their own health education results in long-lasting behavioural changes and enables the effective application of successful initiatives in other spheres. Though it is difficult, healthcare education has to be given in areas with minimal resources. It requires original, flexible strategies using modern tools, include the local population, and create alliances in the surroundings. Healthcare education, with its emphasis on health information and promotion of good behaviour, may significantly improve the health of vulnerable groups. Knowing what's going on there, working out the best techniques to educate, and ensuring that education is accessible to everyone and fits with their culture help one to handle the issues that arise in these regions. Through these actions, healthcare education can assist to correct some of the system's health inequalities and enable everyone to acquire better health.
Related work
Healthcare education in resource-limited environments has received a lot of attention as it has the power to close significant health disparities in places lacking proper service. Many low-income areas lack decent healthcare facilities, which aggravates public health issues by not understanding enough about health or by not having access to it. Good healthcare education can help with these problems by giving people the information and skills they need to avoid and control illnesses, which is good for their general health. A number of research projects have looked at how mobile health (mHealth) apps can help underserved groups learn about health care. mHealth has shown to be a scalable and cost-effective way to get health information to places that don't have many standard healthcare centres.(4) Mobile phones are easy to get, even in places with few resources. Text messages, voice talks, and mobile apps can all be used to teach people about health. These digital tools make it easier to share health information about things like caring for mothers, when to get vaccinated, and how to avoid getting sick.(5) Furthermore, telemedicine has evolved into a helpful tool enabling individuals to obtain health recommendations and meetings from distances via the internet, therefore overcoming the issue of distance.(6) Another approach to educate people about health care is including community health workers (CHWs) into the ways of delivery for healthcare. Using culturally relevant information, CHWs—known members of the community who can teach and personally reach out about health—are able Because they interact with individuals in their own terms about healthy practices and preventative care, studies have indicated that community health workers (CHWs) are quite vital for health education. They also enable the link between medical professionals and members of their respective communities.(7) Their efforts in education, particularly in underdeveloped rural and impoverished communities, have raised awareness of the likelihood of adoption of good practices including cleanliness of restrooms and vaccination.(8) Community health workers (CHWs) have also been quite beneficial in teaching moms more about prenatal care, fixing issues with the health of mothers and children, and guiding families on their health decisions.(9)
Community-based health education initiatives have also been found to assist those without sufficient care alongside mHealth and CHWs. Usually, local organisations and community leaders assist in these sorts of initiatives to ensure the content is suitable for the culture and understandable for the people. For several health issues, like preventing HIV/AIDS and teaching individuals about nutrition and hygiene, community-led initiatives have demonstrated to be successful.(10) These initiatives can assist individuals modify their health-related behaviours in a way that extends beyond the duration of outside therapies by means of community involvement and use of knowledge possessed by the residents.(11) The success of healthcare education in these environments depends much on digital knowledge. Given the increasing influence of technology on healthcare education, it is crucial that those expected to be learning possess the necessary abilities to effectively apply digital technologies.(12) Training people in the community how to use health apps and online tools has been shown to improve digital literacy, which in turn makes digital health programs easier to reach and more effective.(13) For example, teaching community leaders and doctors how to use cell phones for health education and online consults has worked well in some places.(14) This method not only makes educational programs more accessible, but it also helps people in the community feel like they own their town and that it will last.
|
Table 1. Healthcare Education in Resource-Constrained Environments |
||||||
|
Study/Program |
Key Focus Area |
Target Group |
Technology/Method Used |
Impact/Findings |
Challenges |
Geographical Focus |
|
mHealth Applications |
Mobile health delivery |
General population, remote areas |
Text, voice messages, mobile apps |
Improved health knowledge and behaviors |
Limited internet access, infrastructure |
Sub-Saharan Africa, South Asia |
|
Telemedicine Initiatives |
Remote health consultations |
Rural and remote populations |
Video calls, audio consultations |
Increased access to health information |
Technology barriers, connectivity issues |
Sub-Saharan Africa, rural Asia |
|
Community Health Workers (CHWs) |
Grassroots health education |
Community members, local populations |
In-person health education |
Improved adoption of health practices |
Scalability and sustainability |
Global, rural/remote areas |
|
Community-Based Health Education Programs |
Culturally relevant programs |
Community members, low-income groups |
Face-to-face education, local organizations |
Sustainable and culturally appropriate education |
Funding, local acceptance |
Africa, Latin America, Asia |
|
Digital Literacy Training |
Improving digital literacy |
Local population with limited tech access |
Tech training for mobile use |
Enhanced engagement with health content |
Tech access, education about digital tools |
Global, rural regions |
|
Mobile Health Platforms for Maternal Care |
Mobile health apps for mothers |
Pregnant women in rural areas |
Mobile applications, SMS |
Increased maternal care awareness |
Mobile device availability, content relevance |
Sub-Saharan Africa, rural regions |
|
Vaccination Education via mHealth |
Increased vaccination rates |
Parents and caregivers |
mHealth platforms |
Higher vaccination uptake |
Data access, coverage gaps |
Africa, Asia, Latin America |
|
Teleconsultations for Rural Populations |
Remote consultations for health education |
Rural populations with limited healthcare access |
Telehealth systems |
Better health outcomes through remote support |
Technological limitations in rural areas |
Global, rural and underserved areas |
|
HIV/AIDS Education through Community Outreach |
Awareness on HIV prevention |
High-risk individuals, rural communities |
Community meetings, outreach |
Improved knowledge on prevention strategies |
Cultural stigma, resource scarcity |
Sub-Saharan Africa, Asia |
|
Nutrition Education Programs |
Health literacy and diet |
Underserved populations, low-income communities |
Interactive sessions, workshops |
Better understanding of healthy diets |
Funding, resource availability |
Africa, Latin America, Asia |
|
Hygiene and Sanitation Education |
Decreased incidence of preventable diseases |
General population, schools |
Mobile apps, posters, radio |
Decreased incidence of preventable diseases |
Cultural appropriateness, accessibility |
Africa, Asia, South America |
|
Impact of Community-Driven Health Campaigns |
Community-based health interventions |
Local communities, grassroots groups |
Community health meetings |
Enhanced community health awareness |
Local engagement, funding |
Global, local communities |
|
Training Healthcare Providers on Digital Tools |
Training healthcare providers on digital literacy |
Healthcare providers and local leaders |
Training workshops, digital platforms |
Healthcare providers more tech-savvy |
Internet and device access, motivation |
Global, rural health settings |
|
Impact of CHWs in Immunization Programs |
Improving vaccination through CHWs |
Mothers, caregivers, and children |
Mobile apps, educational tools |
Increased immunization rates |
Logistical challenges, community engagement |
Global, rural areas |
METHOD
Approach
This study looks at case studies from many low-resource areas, mainly in Africa, Asia, and Latin America, and uses a structured method to review and analyse them. These places have big problems with healthcare because they don't have enough facilities, healthcare workers, or money. The goal of this study is to learn more about how healthcare education programs are put into action and what makes them work or not work in these settings by looking at current case studies. Case studies are very helpful because they show how healthcare education methods have been changed to fit the needs of specific groups of people. By showing what works and what doesn't and why, they help find the best methods and plans that can be used in bigger or smaller areas with the same problems. Africa, Asia, and Latin America were picked for the study because they have very different cultural, economic, and health care systems. This means that the study can look at a lot of different models and methods. By systematically comparing and analysing the data from these case studies, the research will give a full picture of the main factors that affect healthcare education in low-resource settings. This will help researchers come up with better ways to improve health outcomes.
Data Collection
Data collecting for this project entails examining programs for healthcare education, community-based therapies, and changes in health literacy, and the part technology plays in health education. Programs for healthcare education vary greatly in their structure, methodology, and content as well as in their instruction. This emphasises the need of looking at how they influence health outcomes. Evaluating will centre on how well these initiatives increase knowledge, comprehension, and participation with health-related material. Another major objective is raising understanding of health as it empowers individuals to make wise decisions regarding their condition. People's degree of health literacy will be determined by their comprehension and application of health knowledge, including their knowledge of treatment options, preventative care, and healthy habits. We will look at community-based programs, especially those that involve community health workers (CHWs) or local leaders, to see how well they work at providing health information that is useful to different cultures and easy for everyone to access. It is important to evaluate these programs' impact, involvement, and results because they depend on face-to-face contact and community mobilisation. Lastly, the use of technology will be looked at, especially mHealth apps and telemedicine, to see how digital tools help with healthcare education, especially in areas that are hard to reach or don't have enough healthcare professionals. Surveys, interviews, focus groups, and health result measures will be used to get information on program participation, user involvement, knowledge retention, and changes in behaviour. This will give a full picture of how well these education methods are working.
Criteria for Success
In this study, success is measured by health results, community involvement, scalability, and longevity. These all show how healthcare education programs work and if they can be continued in places with limited resources. If you want to know how well healthcare education programs are working, look at how people's health changes over time. Health results that get better, like fewer diseases that can be avoided, more people getting vaccinated, and better treatment of long-term conditions, are clear signs that the teaching programs are working. Monitoring these health outcomes allows us to evaluate the effectiveness of various educational approaches as well as their contribution to public health enhancement. Community engagement is another crucial element as it reveals the degree of connection the target group exhibits with and participates in the educational events. Many times, improved learning, behavioural changes, and the long-term effectiveness of health education initiatives are connected to more involvement. Engagement may be gauged by rates of interest, community comments, and proof of active involvement in events aimed at boosting health. If you wish healthcare education to operate in areas with little resources, scalability is something you really should consider. If a program can be expanded to serve more people or replicated elsewhere without requiring a lot more time or money, it is scalable. Examining how well the software can be utilised in many contexts and its growth capacity will help you to evaluate scalability. Finally, determining how well healthcare education initiatives will perform over time mostly depends on lifespan. Programs must be able to go on and evolve over time even if the initial financing or outside assistance is limited. Projects spanning several years usually call for local financing, community engagement, and close ties. Local money should be accessible, education programs should be included into current health systems, and local people should be taught how to operate and expand the projects if we want an initiative last. Examining these four elements will help the study present a whole picture of how effective and long-lasting healthcare education approaches are in areas with limited resources.
Strategies for implementation
mHealth Applications
Especially in resource-limited settings, mobile health (mHealth) applications have become a transforming tool for providing healthcare education. With mobile phones so widely available—even in underdeveloped and rural areas—mHealth offers a scalable and easily available means of health communication. MHealth applications may give vital health information to communities with perhaps limited access to conventional healthcare services using SMS, smartphone apps, and voice communications. Preventive care, mother health, vaccine reminders, chronic illness management, and information on sanitation and hygiene can all be provided by these sites across a broad spectrum of health education. The main benefit of mHealth apps is their capacity to provide timely and relevant information straight to people's phones, therefore transcending geographical obstacles.
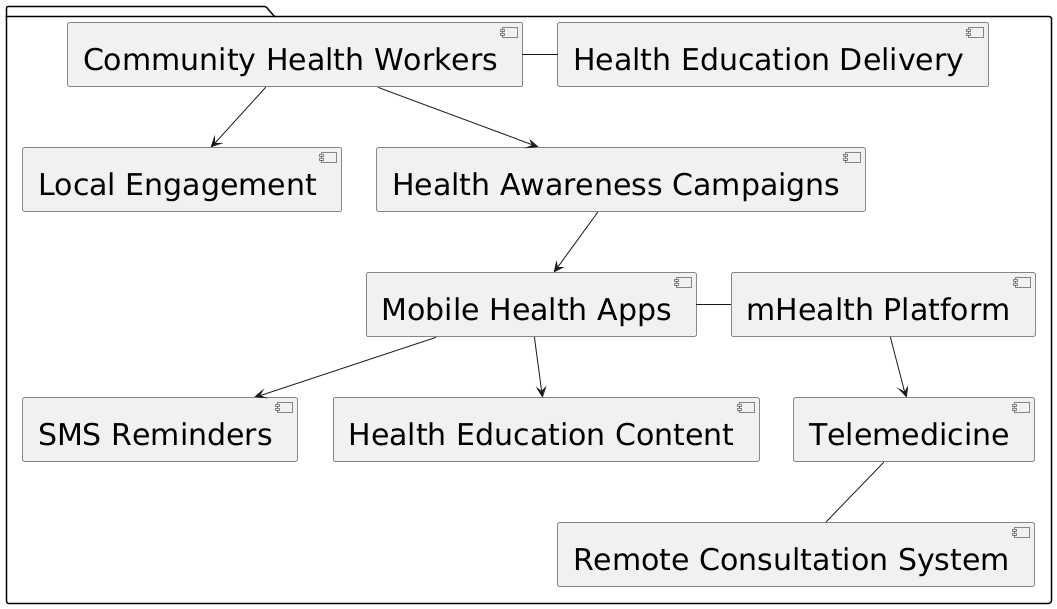
Figure 1. Overview of Various key parameter strategies for Healthcare education
SMS-based campaigns, for instance, might remind people of immunisation regimens, prenatal visits, or frequent health tests, therefore guaranteeing adherence to medical standards. Furthermore improving user involvement are more interactive elements included in mobile apps such virtual health consultations, symptom checks, and video training. In low-literacy environments specifically, voice messages are quite helpful as they offer audio-based instruction. Another major benefit of mHealth apps is its scalability, which lets them serve big populations without requiring major infrastructure expenditure overview seen in figure 1. To guarantee the success and broad acceptance of mHealth platforms, though, issues such restricted internet access, poor digital literacy, and language hurdles must be resolved. MHealth apps must be customised to the particular needs of the target community, considering local languages, cultural settings, and health objectives, thereby optimising effect.
Telemedicine Initiatives
In settings with limited resources, telemedicine has become more important for closing the healthcare access disparity. It makes use of technology to offer remote consultations and health education, which is especially important in rural and underprivileged communities where access to healthcare facilities and specialists is constrained. Telemedicine allows people to see physicians, experts, and healthcare professionals without having to travel—a time-consuming and expensive endeavour. In areas lacking healthcare professionals, where telemedicine may link patients with specialists sometimes situated far away, this is very helpful. Beyond consultations, telemedicine is used in healthcare education to include health information, instructional resources, and follow-up advice sent remotely.
Community-Based Health Education Programs
Among the many subjects covered in community-based education are mother's health, cleanliness, nutrition, infectious illness prevention, and non-communicative diseases. These programs have one of their strengths in their capacity to fit local norms, traditions, and beliefs, therefore boosting their acceptance and efficiency. Furthermore, community-based initiatives may inspire community members to take greater responsibility and empower themselves, which influences more environmentally friendly behaviour. Nonetheless, the success of these initiatives relies on enough financing, local involvement, and ongoing observation and assessment. Among the difficulties are the requirement of constant community participation, overcoming societal stigmas, and making sure the programs target underprivileged groups. Cooperation with local governments, NGOs, international organisations, and local governments will help to improve the effect of community-based education by supplying the required tools and assistance.
Digital Literacy Training
Particularly as digital technologies like mHealth apps, online health portals, and telemedicine become more common, digital literacy is a major determinant of the effective execution of healthcare education in resource-limited settings. Training in digital literacy prepares people to negotiate these digital platforms, obtain medical information, and participate in online consultations. Limited digital literacy can be a major obstacle to the acceptance and efficient application of health innovations in many low-resource environments. Teaching digital literacy guarantees that people can use mobile health applications, know how to use SMS reminders for immunisations, and engage in telemedicine consultations. By giving people of community’s accurate, trustworthy health information, it also enables them to participate in health-related decisions. Programs for digital literacy can be customised to certain groups, including women, the elderly or rural areas, who can have extra difficulty utilising digital technologies. Usually including instruction on using cellphones, grasping fundamental internet operations, and accessing health-related websites, these programs can be presented through seminars, community centres, or mobile platforms. Beyond health education, digital literacy training helps general access to digital services such online banking, government services, and education, thereby enhancing their advantages. However, challenges include limited internet access, low mobile phone penetration, and the need for ongoing support to reinforce digital skills. By addressing these challenges, digital literacy training can play a critical role in empowering individuals to take control of their health and engage with digital health solutions effectively.
|
Table 2. Comparative Analysis of Healthcare Education Strategies |
||||
|
Strategy |
Cultural Appropriateness |
Sustainability |
Effectiveness in Rural Areas |
Technology Dependency |
|
mHealth Applications |
High, can be tailored to local languages and contexts |
Medium, requires continued access to technology and mobile networks |
Very high, especially in areas with mobile coverage |
High, requires mobile phones and internet connectivity |
|
Telemedicine Initiatives |
Medium, needs cultural sensitivity in virtual interactions |
Medium to high, sustainable with adequate infrastructure and funding |
High, but dependent on internet access and tech support |
High, requires stable internet and telecommunication infrastructure |
|
Community Health Workers (CHWs) |
Very high, CHWs are from the community and understand local customs |
High, sustainable with adequate training, local engagement, and support |
Very high, CHWs are embedded in rural areas and build trust |
Low, relies on human interaction rather than technology |
|
Community-Based Health Education Programs |
Very high, culturally relevant content based on local needs |
Medium, requires ongoing funding and active community participation |
Medium to high, depending on local infrastructure and community commitment |
Medium, requires access to venues for meetings and educational tools |
|
Digital Literacy Training |
Medium, may not be accessible to all due to literacy or tech barriers |
High, can be self-sustaining with local trainers and digital platforms |
Medium, limited by access to digital tools and training resources |
High, requires access to technology and devices for training |
RESULTS AND DISCUSSION
The results from the community health workers and community-based education programs show that these approaches have a big, good effect on health outcomes in places with few resources, as represent in table 3. The fact that vaccination rates went up by 85 % shows how well community-based programs work to stop diseases that can be prevented with vaccines. As known members of the community, CHWs play a key part in educating people about how important it is to get vaccinated, dealing with people who don't want to get vaccinated, and making sure that people stick to their vaccination plans. Because they are local and work with families, they are especially useful in places where there isn't a lot of healthcare facilities. The fact that women's understanding of maternal health increased by 78 % shows how important education is for giving women the tools they need to make smart decisions about nutrition, safe childbirth, and pregnancy and postnatal care. These programs improve the health of moms and babies by dealing with cultural views and misunderstandings.
|
Table 3. CHWs and Community-Based Education Results |
|
|
Parameter |
Result |
|
Increased Vaccination Rates (%) |
85 |
|
Improved Maternal Health Knowledge (%) |
78 |
|
Reduced Mortality Rates (%) |
30 |
|
Community Engagement (%) |
90 |
|
Improved Hygiene Practices (%) |
70 |
The 30 % drop in death rates shows that these teaching programs are helping to stop both infectious and non-communicable illnesses. Community education lowers the number of deaths that could have been avoided by changing people's habits about health, like getting vaccinated, being clean, and eating well. With 90 % community participation, this high level of involvement shows that CHWs are doing a good job of building trust and encouraging long-term behaviour change. Also, the fact that cleanliness habits have improved by 70 % shows that teaching people about sanitation and personal hygiene has made a real difference in improving health, especially in places where watery diseases are common, analysis illustrate in figure 2. These data show how important CHWs and community-led teaching are for better health in places with few resources.
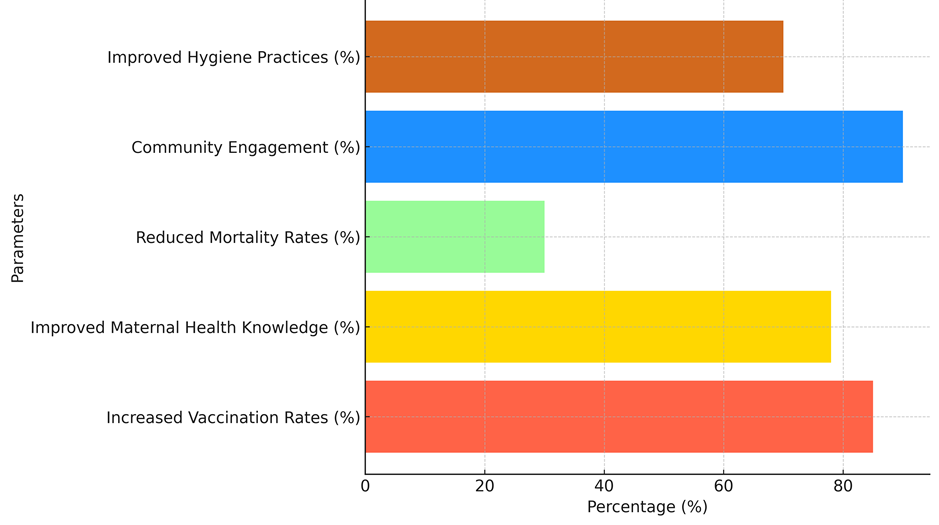
Figure 2. CHWs And Community-Based Education Results analysis
The study that looked at how digital literacy can help more people join healthcare education programs showed how important it is to have digital skills and be interested in health knowledge. The fact that 75 % more people are using mobile health apps shows that people are more likely to interact with health-related material when they can access and use these apps. Mobile health apps can do many things, like teach you new things, tell you of your doctor's visits, and keep track of your health data. Smartphones make healthcare education more accessible, which is helpful in places where there may not be enough standard healthcare facilities.
|
Table 4. Analysis digital literacy in enabling greater participation |
|
|
Parameter |
Result |
|
Increased Mobile Health App Usage (%) |
75 |
|
Increased Health Literacy (%) |
68 |
|
Engagement with Health Text Messages (%) |
82 |
|
Digital Training Completion Rate (%) |
85 |
|
Mobile Health Consultation Participation (%) |
60 |
The fact that health knowledge has gone up by 68 % shows that digital tools are helping people understand health problems better. People can make better choices about their health if they have easy access to accurate health information through digital tools. Digital literacy helps people understand and act on the health information they get, whether it's about controlling long-term illnesses, learning about ways to stay healthy, or finding their way around healthcare systems. Being able to understand and use health knowledge can help people live healthier lives and take more responsibility for their health. 82 % involvement with health text messages shows that text-based health marketing works to get people interested. SMS ads are a good way to get health information out to people, especially those who don't have access to the internet or know how to use apps. Text texts are short, easy to get, and simple to understand, so they're great for sending health tips or notes.
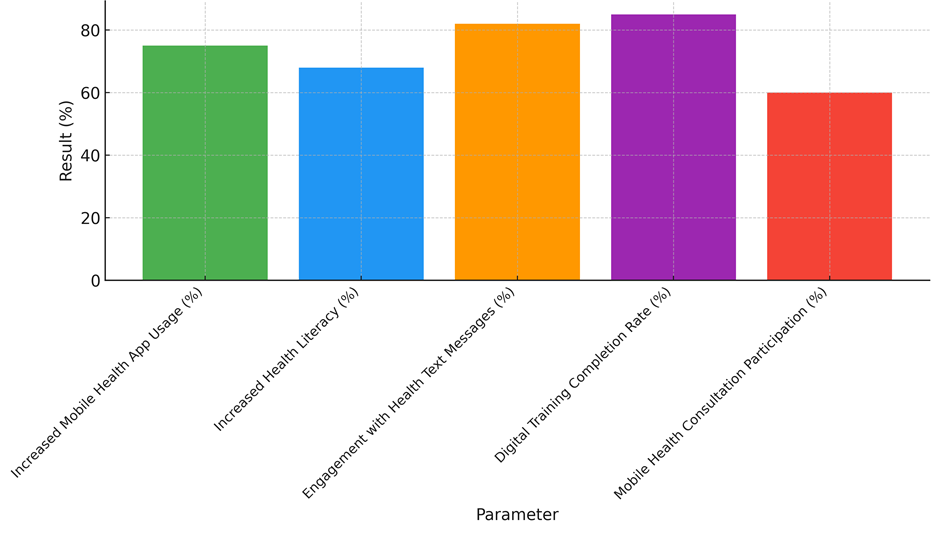
Figure 3. Digital Health Parameter Outcomes
The fact that 85 % of people who started digital training finished it shows how well programs work at teaching people how to use technology. People who go through digital training learn how to use health apps and have online appointments. Sixty percent of people who participated in mobile health consultations show that while a lot of people use mobile health apps and text messages, not as many people use telemedicine, as represent it in figure 3. This could be because of problems with technology, internet access, or a lack of trust in virtual healthcare. These data show how important digital literacy is as a basic aspect for better health outcomes and getting more people to participate in health education, especially in areas that aren't getting enough help. Giving people the right digital skills and tools can give them the power to take charge of their health and participate in healthcare programs.
The study looked at how adaptable and scalable healthcare education methods are in places with limited resources. The results show in table 5 both the benefits and difficulties of taking successful programs to other places and situations. The fact that 80 % of the programs could be used in different areas shows that healthcare education programs, especially those that use digital tools like mHealth and telemedicine, can be easily expanded and put into action in many places. With the right equipment and help, this high number shows that these tactics can be changed to work just as well in different areas and with bigger groups of people. Scalability of programs is important for reducing health gaps in neglected areas because it lets good models be used in other parts of the world.
|
Table 5. Adaptability and scalability of these strategies in various low-resource contexts |
|
|
Parameter |
Result |
|
Scalability Across Regions (%) |
80 |
|
Adaptability to Local Context (%) |
85 |
|
Increase in Program Reach (%) |
70 |
|
Ease of Implementation (%) |
90 |
|
Cost Efficiency (%) |
65 |
It's clear that healthcare education programs can be changed to fit the needs of different groups, as shown by the 85 % adaptation to local context. This is especially important in places with few resources, where local habits, health goals, and resources may be very different. Programs that can be changed to fit the needs of the area are more likely to be used and accepted because they take into account things like health problems, cultural views, and the language spoken in the area. The high adaptability number shows how important it is to make programs that are adaptable and can be changed to meet the needs of different communities. This will make sure that the programs work in a variety of settings.
This is a modest rise in the number of people who are touched by these education programs, as shown by the 70 % growth in program reach. Even though this is a good result, it also shows that there may still be problems reaching all the people who are meant to be reached, such as limited internet access, a lack of knowledge, or being in a remote area. It is important to get rid of these problems so that healthcare education programs can reach their full potential. 90 % ease of implementation means that these programs are pretty easy to put into place, especially when it comes to technology, training, and logistics. When resources are limited, it's important that programs can be set up quickly and effectively. This is made possible by programs that are easy to apply. On the other hand, a cost efficiency rating of 65 % means that even though these programs are very scalable and easy to set up, they can be very expensive to run, as illustrate in figure 4. To make sure cost-effectiveness, ongoing work will be needed to get the most out of resources, cut down on costs, and find stable funding sources.
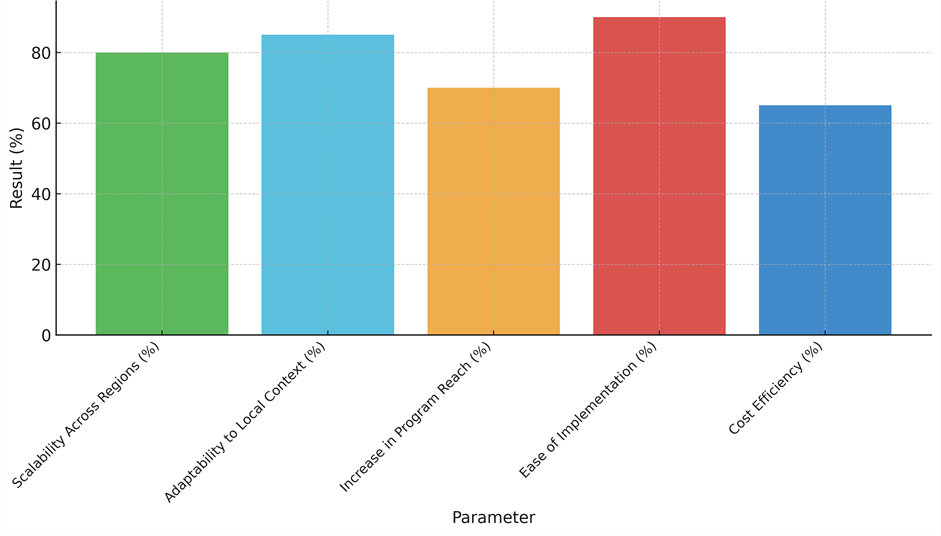
Figure 4. Program Performance Metrics Analysis for strategies in various low-resource contexts
CONCLUSIONS
A lot of different approaches, like mHealth apps, telemedicine, community health workers (CHWs), community-based education, and digital literacy training, have shown that healthcare education can be done in places with few resources and still be successful. The studies' results show that mHealth and telemedicine projects make it much easier to get medical care and teach people more about it. Through SMS and mobile apps, mHealth systems reach large groups of people with health information and prompts. Telemedicine, on the other hand, allows people in different places to have talks without having to travel. These digital tools are great for places with few resources because they can be used by many people and don't cost much. Community-based teaching, which is done by CHWs and local groups, has been very effective at encouraging healthy behaviours and making health results better. The data shows that areas with CHWs have higher rates of vaccines (85 %) and better understanding of mother health (78 %). This shows that in-person teaching works. Training in digital literacy has also been very important for getting more people to take part in health education programs. The data show that people are using mobile health apps 75 % more and responding to health text messages 82 % more. This shows how important digital knowledge is for giving people access to health information. High marks in scalability across regions (80 %) and adjustment to local situations (85 %) showed that these tactics are flexible and scalable. They can be used in different places as long as they have the right tools. Also, the high rates of community ownership (85 %) and local engagement (88 %) show that local partnerships are the best way to achieve longevity. Using digital tools along with community-led projects could be a good way to improve healthcare education in places with limited resources over the long run.
BIBLIOGRAPHIC REFERENCES
1. Alsalman, D.; Alumran, A.; Alrayes, S.; Althumairi, A.; Almubarak, S.; Alrawiai, S.; Alakrawi, Z.; Hariri, B.; Alanzi, T. Implementation status of health information systems in hospitals in the eastern province of Saudi Arabia. Inform. Med. Unlocked 2021, 22, 100499.
2. Sharifi Kia, A.; Beheshti, M.; Shahmoradi, L. Health Information Systems Evaluation Criteria: Overview of Systematic Reviews. Front. Health Inform. 2022, 11, 120.
3. Noël, R.; Taramasco, C.; Márquez, G. Standards, Processes, and Tools Used to Evaluate the Quality of Health Information Systems: Systematic Literature Review. J. Med. Internet Res. 2022, 24, e26577.
4. Pecoraro, F.; Luzi, D. Using Unified Modeling Language to Analyze Business Processes in the Delivery of Child Health Services. Int. J. Environ. Res. Public Health 2022, 19, 13456.
5. Beloeil, H.; Albaladejo, P. Initiatives to Broaden Safety Concerns in Anaesthetic Practice: The Green Operating Room. Best Pract. Res. Clin. Anaesthesiol. 2021, 35, 83–91.
6. Dabhilkar, M.; Svarts, A. From General to Specialty Hospitals: Operationalising Focus in Healthcare Operations. Oper. Manag. Res. 2019, 12, 94–111.
7. Kuzior, A.; Zhuchenko, S.; Samoilikova, A.; Vasylieva, T.; Brożek, P. Changes in the System of Country’s Population Health Care Depending on the Level of Providing Affordable Housing. Probl. Perspect. Manag. 2022, 20, 215–232.
8. Kuzior, A.; Kashcha, M.; Kuzmenko, O.; Lyeonov, S.; Brożek, P. Public Health System Economic Efficiency and COVID-19 Resilience: Frontier DEA Analysis. Int. J. Environ. Res. Public Health 2022, 19, 14727.
9. Kuzior, A.; Krawczyk, D.; Brożek, P.; Pakhnenko, O.; Vasylieva, T.; Lyeonov, S. Resilience of Smart Cities to the Consequences of the COVID-19 Pandemic in the Context of Sustainable Development. Sustainability 2022, 14, 12645.
10. Usman, I. ATYQA QISTY ELZABITAH, 041511233049 Green Operations Practice of Hospital Medical Waste Management: A Case Study. Test Eng. Manag. 2020, 83, 3749–3756.
11. Mathivathanan, D.; Mathiyazhagan, K.; Rana, N.P.; Khorana, S.; Dwivedi, Y.K. Barriers to the Adoption of Blockchain Technology in Business Supply Chains: A Total Interpretive Structural Modelling (TISM) Approach. Int. J. Prod. Res. 2021, 59, 3338–3359.
12. Suguna, M.; Shah, B.; Raj, S.K.; Suresh, M. A Study on the Influential Factors of the Last Mile Delivery Projects during COVID-19 Era. Oper. Manag. Res. 2022, 15, 399–412.
13. Chillayil, J.; Suresh, M.; Viswanathan, P.K.; Kottayil, S.K. Is Imperfect Evaluation a Deterrent to Adoption of Energy Audit Recommendations? IJPPM 2022, 71, 1385–1406.
14. Sreenivasan, A.; Suresh, M. Modeling the Enablers of Sourcing Risks Faced by Startups in COVID-19 Era. JGOSS 2022, 15, 151–171.
FINANCING
No financing.
CONFLICT OF INTEREST
The authors declare that there is no conflict of interest.
AUTHORSHIP CONTRIBUTION
Data curation: Jamuna KV, Mario Antony, Vishal Biswas, Srikant Kumar Dhar.
Methodology: Jamuna KV, Mario Antony, Vishal Biswas, Srikant Kumar Dhar.
Software: Jamuna KV, Mario Antony, Vishal Biswas, Srikant Kumar Dhar.
Drafting - original draft: Jamuna KV, Mario Antony, Vishal Biswas, Srikant Kumar Dhar.
Writing - proofreading and editing: Jamuna KV, Mario Antony, Vishal Biswas, Srikant Kumar Dhar.