doi: 10.56294/hl2023239
ORIGINAL
Comparative Analysis of Environmental Health Regulations and Patient Health Outcomes
Análisis comparativo de la normativa de salud ambiental y los resultados sanitarios de los pacientes
Pooja Varma1
![]() , Gauri Tamhankar2
, Gauri Tamhankar2
![]() , Sonia Mehta3
, Sonia Mehta3
![]() , Antaryami Pradhan4
, Antaryami Pradhan4
![]()
1JAIN (Deemed-to-be University), Department of Psychology. Bangalore, Karnataka, India.
2Krishna Institute of Medical Sciences, Krishna Vishwa Vidyapeeth “Deemed to be University”, Dept. of Medicine. Taluka-Karad, Dist-Satara, Maharashtra, India.
3School of Nursing, Noida International University. Greater Noida, Uttar Pradesh, India.
4IMS and SUM Hospital, Siksha ‘O’ Anusandhan (Deemed to be University), Department of General Surgery. Bhubaneswar, Odisha, India.
Cite as: Varma P, Tamhankar G, Mehta S, Pradhan A. Comparative Analysis of Environmental Health Regulations and Patient Health Outcomes. Health Leadership and Quality of Life. 2023; 2:239. https://doi.org/10.56294/hl2023239
Submitted: 03-06-2023 Revised: 05-09-2023 Accepted: 12-11-2023 Published: 13-11-2023
Editor: PhD.
Prof. Neela Satheesh ![]()
ABSTRACT
This study looks at how different rules about environmental health affect public health by looking at the link between these rules and how well patients do with their health. Environmental factors, like the cleanliness of the water and air, and exposure to dangerous materials, are constantly known to play a big role in both long-term and short-term health problems. But even though these external factors are becoming more well known, there is still a big hole in our knowledge of how the rules meant to lower these risks actually lead to real health changes for patients. The study looks at how environmental health policies work in different parts of the world and compares them, focussing on how well they work at lowering the number of people who get diseases like cancer, heart disease, and breathing problems. It uses both personal and quantitative data from case studies, patient health records, and environmental tracking figures to find patterns and links between tighter environmental health rules and better patient results. The study looks at many rules, such as carbon standards and trash management policies, to find the main things that make these measures work or not work. The study also looks at how public health programs, education, and attempts to involve the community affect how well environmental rules work overall. It is also thought about what role discipline and cooperation play in achieving these health gains. The results show that strong public health rules must be put in place and followed in order to improve patients’ long-term health. There are, however, differences based on socioeconomic class, region, and access to healthcare resources. This shows the need for a more comprehensive approach that mixes regulatory measures with proactive health treatments.
Keywords: Environmental Health; Patient Health Outcomes; Health Regulations; Public Health Policy; Environmental Determinants; Healthcare Disparities.
RESUMEN
Este estudio examina cómo afectan a la salud pública las distintas normas sobre sanidad ambiental, analizando la relación entre dichas normas y el estado de salud de los pacientes. Se sabe constantemente que los factores ambientales, como la limpieza del agua y el aire y la exposición a materiales peligrosos, desempeñan un papel importante en los problemas de salud tanto a largo como a corto plazo. Pero aunque estos factores externos son cada vez más conocidos, sigue habiendo un gran vacío en nuestros conocimientos sobre cómo las normas destinadas a reducir estos riesgos conducen realmente a cambios reales en la salud de los pacientes. El estudio examina cómo funcionan las políticas de salud ambiental en distintas partes del mundo y las compara, centrándose en su eficacia para reducir el número de personas que contraen enfermedades como cáncer, cardiopatías y problemas respiratorios. Utiliza datos personales y cuantitativos procedentes de estudios de casos, historiales médicos de pacientes y cifras de seguimiento medioambiental para hallar pautas y vínculos entre normas de salud medioambiental más estrictas y mejores resultados para los pacientes. El estudio examina muchas normas, como las normas sobre emisiones de carbono y las políticas de gestión de basuras, para encontrar los principales aspectos que hacen que estas medidas funcionen o no. El estudio también analiza cómo los programas de salud pública, la educación y los intentos de implicar a la comunidad afectan al funcionamiento general de las normas medioambientales. También se reflexiona sobre el papel que desempeñan la disciplina y la cooperación en la consecución de estos beneficios para la salud. Los resultados muestran que para mejorar la salud a largo plazo de los pacientes es necesario implantar y cumplir unas normas de salud pública estrictas. Sin embargo, existen diferencias en función de la clase socioeconómica, la región y el acceso a los recursos sanitarios. Esto demuestra la necesidad de un planteamiento más global que mezcle medidas reguladoras con tratamientos sanitarios proactivos.
Palabras clave: Salud Ambiental; Resultados de Salud de los Pacientes; Normativa Sanitaria; Política de Salud Pública; Determinantes Ambientales; Disparidades Sanitarias.
INTRODUCTION
For a long period, environmental health has been well established to be a main determinant of general health. Over the past few decades, more and more evidence has been discovered linking environmental elements such the quality of the air and water, exposure to hazardous chemicals, and living circumstances in cities to a wide spectrum of health consequences. Patients’ health clearly suffers from environmental exposure; it affects everything from lung ailments like asthma and chronic obstructive pulmonary disease (COPD) to heart problems, cancer, and brain issues. Public health policies and patient performance still have a complex and little investigated relationship, nevertheless. Although many natural hazards have been managed with great success, there are still concerns regarding how these guidelines really help every individual patient to stay healthy. Environmental health rules aim to prevent people from coming into contact with hazardous elements and circumstances in the surroundings. These guidelines address a wide range of issues, including pesticide usage limitation, management of hazardous waste, and water pollution reduction. Their overall aim is to reduce the possibility of environmental elements harming individuals. Strong environmental policies have improved the air and water quality in many affluent nations. These guidelines have also helped reduce the prevalence of diseases such lead poisoning and lung infections often associated with environmental exposure.(1) Notwithstanding these successes, there are still issues particularly in low-income regions and developing nations where environmental deterioration still poses a major health hazard. Environmental rules clearly enhance public health, but more research is needed on the direct connections among several laws and patients’ overall condition. Many studies have examined both the larger public health trends resulting from environmental changes and how well particular policies perform. Not as many, though, examine how certain regulations impact patients’ health throughout time. This disparity in the studies emphasises the need of doing more comprehensive and stronger comparisons.
Under these circumstances, the objective of the study is to investigate how well environmental health rules influence patients’ health by means of comparative analysis of several regions. This study investigates the relationship between certain health outcomes for individuals including cancer, heart disorders, and lung diseases between regulatory actions and It seeks the specifics determining whether these rules are effective or not.(2) Gathering both quantitative and qualitative data can help us to better understand how environmental health regulations impact public health. Patient health records, demographic information, policy reviews, and case studies are among these. This study will also highlight how societal elements could influence the efficacy of environmental health rules. The effectiveness of programs can be much influenced by differences in healthcare access, economic resources, and rule execution. Changes in environmental health might not be always beneficial for everyone. Sometimes the most underprivileged regions affected by both environmental hazards and limited access to healthcare services are those which suffer most.(3) This study will enable us to determine how best to ensure environmental health regulations serve everyone’s health by looking at both regulatory evaluations and health statistics together. It also intends to educate legislators the greatest approaches to simultaneously care for patients and safeguard the surroundings. This will enable more successful public health initiatives grounded on science that can enhance general health outcomes for everybody.
Overview of environmental health regulations
Natural health norms are those laws, standards, and rules aimed to prevent natural elements from compromising human health. These regulations help to protect individuals and areas against natural dangers capable of generating disease and other health issues. Among the several forms environmental health hazards can take are polluted air and water, toxic waste, radiation, noise, and unsafe cooking techniques. States and foreign organisations have developed several regulations aimed to either minimise or eliminate dangerous circumstances due to these threats. The Clean Air Act is one of the most well-known sets of regulations as it controls emissions from factories, vehicles, and power plants therefore lowering pollution in the air. In the same vein, the Clean Water Act provides rules for water quality to safeguard marine environments and guarantee that drinking water is safe.(4) Laws on handling hazardous garbage, like the Resource Conservation and Recovery Act (RCRA), define how rubbish should be disposed of to prevent contamination of land and rivers. The Food and Drug Administration’s (FDA) food safety policies and the Safe Drinking Water Act constitute part of environmental health standards. These are designed to guarantee food and drink are safe. Environmental laws are created using scientific investigations and health risk estimations. They are always evolving to include fresh knowledge on the links between health consequences and the surroundings. Usually, government agencies like the Environmental Protection Agency (EPA) in the United States enforce these regulations. Their responsibility is to ensure that individuals obey the guidelines and penalise those who deviate.
Importance of patient health outcomes
Some of these results are changes in physical and mental health, quality of life, and the number of people who survive different illnesses... In environmental health, patients’ conditions directly relate to factors including air quality, water safety, and toxic exposure. This makes it rather crucial to examine how environmental health regulations impact these outcomes. Improved health outcomes reveal not just that medical treatments are effective but also that preventative actions aimed to reduce environmental hazards are working.(5) Laws restricting emissions from companies, for example, assist to improve the air and reduce the lung disease prevalence including asthma, COPD, and lung cancer. Similarly, tighter controls on water quality can limit diseases transferred by water, decrease the incidence of stomach infections, and relieve the load of diseases that can be prevented, including lead poisoning. Emphasising how patients’ health evolves with time enables legislators to understand how environmental health regulations impact the general state of the society. By tracking specific health indicators, such as hospital admissions with lung or heart issues, researchers may determine how environmental restrictions directly influence individuals’ health. Furthermore, improved health outcomes are sometimes seen as an indication of the general social, economic, and environmental well-being of a community, therefore influencing the allocation of resources and the formulation of healthcare policies.(6) Sometimes variations in hospital patient performance highlight how unevenly natural dangers and healthcare resources are distributed. Low income communities, for instance, could be more prone to environmental hazards and might find it difficult to get healthcare.
Purpose and objectives of the study
Examining environmental health regulations and how they impact patients’ health in a comprehensive sense is the primary aim of this paper. This study aims to investigate, by means of the relationship between regulatory actions and some health issues, more about how environmental health policies impact public health and patient well-being. Although environmental health regulations clearly affect public health as a whole, this study focusses on how much these policies really produce quantifiable health benefits for individual patients. Finding and contrasting how well various environmental health rules reduce the number of diseases connected to environmental hazards is the major objective of the research. Examining regulatory systems in different sectors would enable the research to identify the rules that have helped to reduce the incidence of illnesses like asthma, lung disorders, heart diseases, some forms of cancer.(7) The objective of the study is to identify the best strategies for controlling the surroundings and investigate the elements influencing excellent health outcomes. Another objective is the investigation of social and demographic factors influencing the effectiveness of environmental regulations. Communities with social and economic issues might be more susceptible to natural hazards and could also find it difficult to obtain medical treatment; both of these factors can affect the general state of its citizens. The initiative will investigate these variations and explore how policies may be altered to better satisfy the demands of underprivileged groups. The research also aims to provide legislators with concepts on how to improve public health legislation and simplify their execution.(8) This study intends to assist build future governing policies that can better minimise environmental health hazards and create long-term health advantages for persons and groups by concentrating on the health results for individual patients. This study will clarify the more intricate link between environmental policy and healthcare. This will facilitate the inclusion of environmental health concerns into public health and medical development strategies.
Literature review
Environmental health regulations: Global perspectives
Because every nation has unique political, social, and economic context, environmental health regulations vary greatly from one to the next. Strict environmental rules have been implemented in industrialised nations over the past several decades in order to safeguard public health from the detrimental consequences of industrialisation, urbanisation, and technical advancement. For example, the Clean Air Act (1970) and the Clean Water Act (1972), which regulate the purity of the air and water, have been passed by the United States among other significant laws. Better health outcomes have resulted from the rules lowering of disease propagation through water and improvement of the quality of the air.(9) In Europe, environmental health guidelines likewise have somewhat tight restrictions. For instance, the European Union has developed policies for safe handling of chemicals, trash, and air pollution. Because the EU aims to manage and track air pollution including nitrogen dioxide and particulate matter, city dwellers enjoy improved lung health.
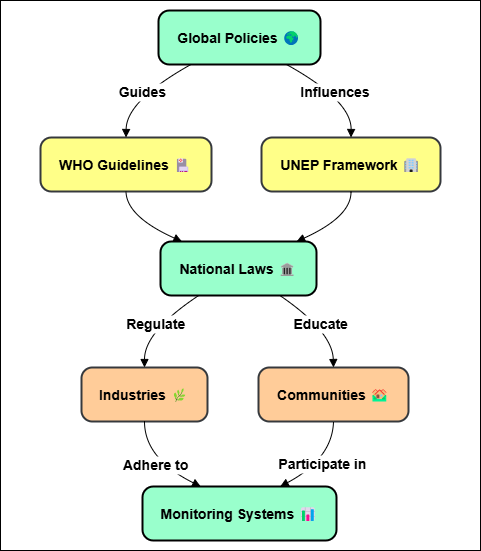
Figure 1. Environmental health regulations: Global perspectives
Because poor nations lack facilities or tools, environmental health regulations are sometimes not as rigorous there. Figure 1 presents some approaches and techniques applied worldwide in relation to public health policies. Some nations, particularly in areas like air quality control and water cleanliness maintenance, have, nonetheless, achieved significant advancements. Serious concerns about public health led China to lately impose some restrictions on air pollution.(10) Conversely, India is beginning initiatives to upgrade its sewage and water infrastructure. Many communities still suffer with issues like insufficient regulation, inadequate public health infrastructure, and increasing urbanisation, all of which exacerbate environmental health hazards even with all these initiatives.
Previous studies on the impact of environmental regulations on health
Many studies on how environmental regulations impact health have focused on how laws on air and water quality impact diseases like asthma and heart disease. Tighter environmental regulations are found by researchers repeatedly to be beneficial for public health as they reduce exposure to harmful chemicals. For instance, the American Lung Association conducted research showing that the Clean Air Act in the United States considerably lowered the asthma, COPD, and other lung disease prevalence in metropolitan areas. Studies in Europe have shown that the EU’s air quality guidelines have helped lower the number of deaths caused by air pollution. The European Respiratory Journal published a study that said enforcing EU air quality rules cut the number of early deaths in Europe by about 60 000 per year. In the same way, studies of water quality rules like those in the U.S.’s Safe Drinking Water Act have shown that diseases like cholera, stomach infections, and lead poisoning that are spread by water have gone down.(11) This is especially true in places where water sources were previously polluted. But while there is a general trend that environmental laws are good for health, the exact amount of these benefits depends on how strict the rules are and how they are enforced. A study in India found that tighter controls on air pollution in Delhi led to a small drop in lung symptoms. However, the benefits were lessened by uneven regulation and high levels of pollution outside.
Link between environmental factors and patient health outcomes
A patient’s health results are greatly affected by environmental factors, which also affect the frequency and intensity of different illnesses. Among the most crucial outside elements influencing health are the quality of the water and air, the existence of dangerous substances, and living environments devoid of security. For instance, long-term exposure to polluted air has been connected to increased risk of lung ailments, heart disorders, even cancer. According to the World Health Organisation (WHO), individuals die before their time mostly from air pollution. Diseases brought on by breathing in tiny particulate matter (PM2.5) and other pollutants kill millions of people annually. Another important factor is the quality of the water. Drinking water that is dirty can spread diseases like diarrhoea, cholera, and dysentery. Infectious diseases spread even more quickly in places with bad cleanliness and trash collection systems, especially in poor nations. Studies have shown that the number of people getting diarrhoeal diseases and other watery sicknesses goes down a lot in places where the water and sewage systems are better.(12) Toxic chemicals, like herbicides, heavy metals, and chemicals that mess with hormones, have also been linked to a number of health problems, such as cancer, hormonal disorders, and delays in development in children. For example, children and adults who are exposed to lead for a long time can have problems developing and their brains can get damaged. Because of this, rules have been made to cut down on the use of lead in fuel, paints, and home goods. In this way, the setting in which people live is directly connected to their health. Environmental health laws that take these things into account can make a big difference in people’s health by lowering their exposure to dangerous chemicals and making living conditions better generally.
The role of government policies and healthcare systems
Environmental health rules have a big effect on how well patients do, but government laws and healthcare systems also play a big part. Policies that safeguard the environment, enhance public health, and facilitate medical treatment all taken together help to reduce the hazards to patient health resulting from the surroundings. Effective environmental health policies those that manage the quality of the air and water, how garbage is handled, and the safety of chemicals make areas healthier, therefore reducing the number of illnesses and improving the quality of living. Many nations follow distinct bodies in line with environmental health guidelines. Two such are the European Environment Agency (EEA) in Europe and the Environmental Protection Agency (EPA) in the United States. These organisations not only create and enforce policies to safeguard the surroundings but also monitor public health trends connected to environmental hazards. A lot of the time, these bodies’ success relies on how strong the rules are, how many resources are available, and how much political will there is to follow through with policies.(13) Along with governmental bodies, healthcare systems play a key role in dealing with the health impacts of environmental risks. Public health services need to be able to find and treat diseases that are caused or made worse by the environment. This includes making sure that people who are sensitive to getting health care can get it when they need it and getting diseases like asthma, cancer, and lead poisoning that are linked to environmental risks diagnosed and treated quickly. Healthcare systems can also do their part to support stricter rules for the environment and teach people about the health risks that come from being in the environment. Combining strong healthcare systems with effective environmental health laws can help lower the negative effects of environmental factors on health, stop illnesses before they happen, and improve patient results.(14) However, there are still problems, especially in places where there aren’t many medical tools or where rules aren’t very strong. In these places, natural health risks are still very dangerous to people’s health. Table 1 is a summary of the literature review’s different methods, their pros and cons, their benefits, and their predictions for the future.
|
Table 1. Summary of Literature Review |
|||
|
Approach |
Limitation |
Benefits |
Future Trend |
|
Regulatory standards for air quality |
Slow regulatory enforcement |
Improved air quality and public health |
Stronger enforcement mechanisms and policy updates |
|
Regulatory frameworks for air quality |
Limited enforcement in some countries |
Reduction in air pollution and health improvement |
Expansion of regulations and global collaboration |
|
Action plans to reduce air pollution |
Insufficient local implementation and monitoring |
Cleaner air and better health outcomes |
Enhanced monitoring and community-level implementation |
|
Government programs to reduce urban air pollution |
Inconsistent enforcement and awareness |
Improved urban air quality and reduced exposure |
More comprehensive regulations with stronger enforcement |
|
Global guidelines for air quality improvement |
Limited global adoption in low-income countries |
Global health benefits from air quality improvements |
Broader global adoption and stricter air quality norms |
|
Agency regulations and monitoring |
Limited resources for enforcement |
Better environmental regulation and compliance |
Greater use of technology for monitoring and enforcement |
|
International water quality regulation standards(15) |
Challenges in implementation in low-income areas |
Cleaner water and reduced waterborne diseases |
Increased focus on equitable access to clean water |
|
Global initiatives for improving environmental health |
Varied success based on region and political climate |
Improved overall health outcomes |
Cross-sector collaborations to address environmental health |
|
Health data collection and analysis on environmental risks |
Inconsistent data collection and regional gaps |
Enhanced understanding of environmental risks |
Improved regional cooperation and data-sharing |
|
Real-time air quality monitoring |
Limited coverage and data granularity |
Real-time data for better policy-making |
Advancements in AI and real-time monitoring systems |
|
Research on energy-related environmental health impacts |
Difficulty in aligning health and energy policies |
Improved environmental health outcomes through energy policies |
Integration of environmental health with energy policies |
|
Global water sanitation programs |
Resource limitations in underdeveloped countries |
Reduced waterborne diseases and improved sanitation |
Universal access to clean water and sanitation services |
|
Long-term national environmental health policy development |
Challenges in policy application across diverse regions |
Long-term improvements in national health policies |
More dynamic, evidence-based policies for health improvements |
|
International climate and environmental health summits |
Slow pace of international agreements |
Stronger global cooperation for health and climate |
Faster policy development and international action on climate change |
METHOD
Research design and approach
A comparison and cross-sectional research methodology was used for this study to look at how environmental health rules affect patient health. The setup of this study lets us look at how different governing systems in different countries or places affect health. This gives us a better idea of how environmental policies can lead to better health. Using both personal and objective data, the study aims to ascertain how successfully environmental health policies enhance patient health. This approach combined descriptive and inferential study techniques. By means of a descriptive study, you will be able to fully view the several environmental health regulations implemented in particular places, so delineating the particular laws meant to handle environmental hazards. This will comprise recommendations for the purity of the air and water as well as instructions for handling chemicals and waste. Using descriptive analysis in addition to inferential statistics, linkages and direct relationships between specific environmental policies and changes in health outcomes will be discovered. The study will concentrate on health consequences intimately related to environmental elements, including rates of cancer, heart disease, lung disorders, and infections transmitted by water. Along with numerical health outcome data, case studies, expert opinions, and policy reports, a mixed-methods approach will be employed to compile qualitative data. This mix will help us get a better sense of how governing systems affect the health results of patients. The goal is to look at both the direct effects that rules have on health and any secondary effects that may happen because of things like differences in income or problems with compliance.
Selection criteria for countries/regions
The countries or areas chosen for this study were chosen based on a number of factors that will ensure a wide range of environmental health laws and health results. First, countries with different levels of economic growth and healthcare facilities will be included so that governing frameworks can be compared in a full way. The United States, Germany, and Japan are developed countries with strong environmental health policies. These will be compared to emerging countries like India, China, and Brazil, where environmental laws may be changing or are not implemented as closely. A second factor that is used to choose is the availability of useful data on environmental laws and health results. Priority will be given to areas that have accurate and easy-to-reach data on air and water quality, pollution levels, and health information. Usually in reaction to health concerns about things like contaminated air or water sources, we will only examine nations that have a past of environmental regulation for this research. Countries that have drastically changed their policies in recent years such as China’s restrictions on air pollution or India’s enhancements in cleanliness will also be discussed. These locations may offer pertinent data about the effectiveness of government initiatives. Finally, sites where environmental regulations are implemented and obeyed in diverse ways will be selected to see how these elements influence health outcomes. The study will examine not just whether or not policies exist but also their tracking and adherence quality. This will enable one to ascertain the actual effectiveness of various government structures in enhancing public health.
Step 1: Define the Variables
Let:
· R = Regulatory Strength (scale of 1-10, where 10 is the most stringent regulation).
· A = Air Quality Index (AQI) (measured in micrograms per cubic meter, lower values indicate better air quality).
· W = Water Quality (measured as a quality index, where higher values indicate better water quality).
· H = Health Outcomes (e.g., disease incidence per 100 000 people for respiratory diseases, cardiovascular diseases, etc.).
· S = Socioeconomic Factors (e.g., GDP per capita, access to healthcare, poverty rate).
Step 2: Calculate Regulatory Score
![]()
Where S_reg is the normalized regulatory strength score on a scale of 0 to 1.
Step 3: Calculate Environmental Health Impact Score
![]()
Where S_env is the combined score for air and water quality; lower AQI and higher water quality improve the score.
Step 4: Calculate Health Outcomes Score
![]()
Where S_health is the inverse of health outcomes, meaning lower disease incidence improves the score.
Step 5: Compute Final Selection Score for Each Region
![]()
Where α, β, γ, δ are weights assigned to each factor (e.g., α + β + γ + δ = 1), and S_final is the overall selection score for a region.
Data sources: Health outcome data and regulatory frameworks
The information for this study will come from a number of trustworthy sources, such as those maintained by environmental tracking groups, foreign health organisations, and government health agencies. The World Health Organisation (WHO), the Centres for Disease Control and Prevention (CDC), and state health departments are the main places where health result data will come from. These organisations have large records on the number of diseases, death rates, and other health markers. Some of the diseases that will be looked at closely are lung diseases (like asthma and COPD), circulatory diseases, cancers linked to outdoor risks, and diseases that are spread by water. We will get information about the quality of the air and water, how to handle trash, and the amount of pollution from groups like the United States’ Environmental Protection Agency (EPA), the European Environment Agency (EEA), and the United Nations Environment Programme (UNEP). These groups give in-depth studies on the health risks, amounts of pollutants, and changes in the state of the surroundings. The Global Environmental Monitoring System (GEMS) and the World Bank’s Environmental and Social Data will also be used to look at the environmental situations in different areas. The research will examine the regulatory structure using reports and policy documents from national governments and international organisations including the World Health Organisation and the United Nations. These publications will delve deeply into the environmental legislation relevant in every nation or territory. They will discuss the extent of the regulations, their enforcement policies, and the past of their usage.
Step 1: Define the Variables
Let:
H = Health Outcome Data (e.g., incidence rate of respiratory diseases, cardiovascular conditions, waterborne diseases)
R = Regulatory Framework Data (e.g., air quality regulations, water quality standards, pollutant control measures)
D = Data Availability (measured as the number of data points available for analysis, higher values are better)
Q = Data Quality (measured on a scale of 1-10, where 10 represents high-quality, reliable data)
C = Completeness of Data (scale from 0 to 1, where 1 means the dataset is complete and fully representative)
Step 2: Calculate Health Outcome Data Score
![]()
Where S_health represents the score for health outcome data, accounting for the completeness and availability of the data.
Step 3: Calculate Regulatory Framework Score
![]()
Where S_reg represents the score for regulatory frameworks, factoring in both the regulations in place and their quality.
Step 4: Calculate Data Quality and Availability Score
![]()
Where S_data is the combined score for the availability and quality of the data, indicating the strength of the data sources.
Step 5: Compute Final Data Source Score for Each Region
![]()
Where α, β, γ are weights assigned to each factor (e.g., α + β + γ = 1), and S_final is the overall score representing the suitability of health outcome and regulatory framework data for analysis.
Analytical methods: Comparative and statistical tools
Both comparative and statistical approaches will be used to examine the link between patient health outcomes and environmental health policies. Examining the variations in regulatory systems and health results among the chosen nations or areas will be done in a comparative study. This will entail charting important policies in waste management, chemical safety, water quality, and air quality and evaluating their success in lowering environmental health hazards. Case studies will be utilised to underline particular instances of either regulatory success or failure, therefore offering detailed understanding of how various policies influence health results. Health outcome data will be examined in respect to the current regulatory structures using statistical instruments. The degree and direction of the link between the application of certain environmental rules and changes in health outcomes will be ascertained by use of correlation and regression analysis. These statistical methods will enable the detection of trends and patterns throughout several areas, therefore enabling the quantification of the effect of legislative actions on health. The health results and environmental circumstances in every region will be compiled using descriptive statistics including means, standard deviations, and frequency distributions. This will enable comparisons between areas with various regulatory systems and present a comprehensive picture of the general health state and environmental quality in every area. To further adjust for any confounding variables—such as socioeconomic elements, healthcare access, and demographic traits—which potentially affect health outcomes multivariate analysis will also be used. This will enable a more precise evaluation of the impact of environmental laws on patient health outcomes, therefore separating their influences.
Comparative analysis of environmental health regulations
Key environmental health regulations in different regions
Natural health regulations vary greatly depending on where you live. The political, natural, and economic circumstances in every area shape these laws. Rich nations often have robust laws in place to safeguard the environment, improve public health, and handle long-standing garbage issues. The Clean Air Act, which restricts pollutants like sulphur dioxide and nitrogen oxides in the air, and the Clean Water Act, which seeks to clean up rivers and guarantee their safety for drinking, are two significant legislation the US passed. Authorities such as the Environmental Protection Agency (EPA) guarantee adherence to these guidelines. Better quality of the air and water, which has resulted in less incidences of lung and heart diseases, clearly shows their success. In the European Union, environmental laws are likewise quite rigorous. The Ambient Air Health Directive of the EU sets limits for common air contaminants. The Water Framework Directive of the EU regulates groundwater as well as surface water. These guidelines have helped to greatly reduce air pollution and improve water quality. Public health has benefited from this; one example of this is the declining lung disease prevalence. Environmental rules are frequently not as rigorous in developing countries, however there are notable exceptions. Stricter regulations have been implemented in China recently as air pollution is a significant health concern. Designed to reduce pollution and improve the air, the 2013 Air Pollution Prevention and Control Action Plan has proven successful. Likewise, India has tightened environmental regulations like the National Clean Air Program (NCAP), which seeks to reduce smog in cities by means of environmental policies.
Health outcome metrics used for comparison
These metrics help figure out if there is a link between attempts to regulate and the health of the people getting better or worse. Some common health results that are compared are the rates of cancer, heart disease, lung diseases (like asthma and COPD), respiratory diseases (like asthma and bronchitis), and diseases that are spread through water. Respiratory diseases are a good way to see how air quality rules are working. Information about how common asthma, COPD, and lung cancer are can tell us a lot about how well air pollution limits are working. Studies have shown over and over that places with tighter air quality standards have fewer people with lung illnesses. Cardiovascular diseases are another important health result that can be changed by the surroundings. Heart attacks, strokes, and high blood pressure are more likely to happen if you are exposed to air pollution for a long time. Therefore, a good indicator of how effectively air quality regulations are doing is the total count of events connected to heart disease, hospital visits, and fatalities. Water-borne diseases include dysentery, cholera, and diarrhoea reveal the efficacy of water quality regulations. Monitoring the frequency of these diseases helps you to evaluate the effectiveness of regulations in enhancing water treatment, control, and purity. The number of cancer cases, particularly lung cancer and cancers connected to environmental contaminants such as those brought on by chemicals or radiation that might induce cancer, also show the long-term consequences of environmental health standards. Reducing cancer rates following stricter regulations indicates that environmental laws are helping to prevent exposure of individuals to harmful substances.
Analysis of regulation effectiveness in reducing health risks
Examining health outcome data from before and after the laws were implemented as well as areas with varying degrees of regulatory compliance may help you determine how successfully environmental health rules minimise health risks. Reducing the count of illnesses directly brought on by environmental elements is one of the key objectives. Among these are malignancies, lung and circulatory ailments, and infections carried by water. In areas with strong environmental legislation, such as the United States and the European Union, controlling air quality has been demonstrated to help reduce the prevalence of lung ailments. For instance, the U.S. Clean Air Act has been connected to a significant decline in air pollution, which has resulted in a decrease in the asthma and COPD sufferers’ numbers in metropolitan areas. The EU’s policies on air quality have reduced the number of deaths connected to pollution and improved lung health among all of its members in Europe. Rules concerning water quality also show similar outcomes. Improved cleaning techniques have resulted in reduced incidence of illnesses transmitted by water in developed as well as expanding countries. Conversely, locations with less effective government structures can have more health hazards from pollution. In India and China, for example, air quality has started to get better in some cities, but laws haven’t been able to do their job as well as they could because of things like fast industrialisation, weak enforcement, and bad infrastructure. Even though China has made big policy attempts like the Air Pollution Action Plan, laws are still not always successful because of things like weak implementation and political pressure from businesses. Because of this, changes in certain health results over time are often a good way to measure how well regulations work. But the study should also look at things like social status, access to health care, and the region’s ability to implement the rules, because these things can have a big impact on how much health improves because of environmental health laws.
Role of public health initiatives and enforcement
Enforcing environmental health rules and promoting public health are very important parts of making sure that environmental policies actually improve people’s health. Together, environmental legislation and successful public health campaigns educate populations about environmental hazards, raise awareness of them, and inspire behaviour changes that assist regulatory initiatives. Public health campaigns aiming at encouraging individuals to avoid smoking and use face masks during periods of significant air pollution, for example, assist reduce the health hazards resulting from environmental exposure. Many times, environmental legislation and public health initiatives cooperate to handle more general health hazards. Public health initiatives in the US, for instance, that motivate children with asthma to take care of their illness have been successful in attempts to improve the air quality. Similarly, the EU’s initiatives to promote healthier practices such as urging people to walk and ride bikes rather than drive have accompanied its attempts to enhance public health by reducing air pollution. Another crucial element influencing their effectiveness is the execution of environmental regulations. If the regulations are not followed correctly, even if they are well-considered, their intended health impacts might be absent. People’s health in many countries has improved significantly thanks in large part to government agencies like the European Environment Agency or the EPA in the United States. These groups not only make sure that rules are followed, but they also punish people who break them. This makes sure that rules are always followed and respected. But regulation is still hard in poor countries that don’t have a lot of money or other means.
Patient health outcomes
Overview of health outcomes studied (e.g., respiratory diseases, cardiovascular health)
The health effects this study mostly looks at are diseases that are directly caused by things in the environment, like air pollution, water pollution, and being exposed to dangerous drugs. Respiratory diseases, heart disease, and cancer are some of the worst health effects that can happen. All of these are closely linked to outdoor factors. Lung cancer, asthma, and chronic obstructive pulmonary disease (COPD) are some of the most common health problems that are made worse by air pollution. It has been shown over and over that long-term exposure to pollution like particulate matter (PM2.5), nitrogen dioxide (NO2), and sulphur dioxide (SO2) makes these conditions more common and worse. Asthma and lung infections are very common in cities with lots of air pollution. Another important result that is affected by external factors is cardiovascular health. Heart disease, strokes, and high blood pressure are more likely to happen if you breathe in air pollution, especially small particulate matter. High pollution places have higher rates of cardiovascular events like heart attacks and strokes among the people who live there, according to studies. Cancer, especially lung cancer, is a major health problem that can be caused by external toxins. Long-term exposure to environmental toxins like radon, tobacco smoke, and industrial pollution can raise the chance of getting different types of cancer. Cancer rates have gone down in many places where environmental rules have been put in place to limit people’s contact to these toxins.
Regional variations in health outcomes
Differences in health results between regions are caused by differences in natural health risks, healthcare facilities, and how rules are enforced. These differences can be seen within countries and between areas around the world. When environmental health rules are in place in high-income countries like the US and EU countries, health effects tend to get better over time. For example, the number of people in the US with lung diseases like asthma has gone down a lot since the Clean Air Act put in place strict guidelines for air quality. This is especially true in cities. Similarly, European countries with strong policies for tracking air quality and keeping water clean have seen big drops in water-borne diseases and lung health problems, even in cities with lots of people. But in low- and middle-income countries, where environmental rules aren’t very strict and healthcare infrastructure isn’t very good, health results often show that. The number of diseases caused by natural factors like air pollution, dirty water, and poor sanitation is still high in places like India, China, and parts of sub-Saharan Africa... For instance, some of the worst air pollution in the world resides in Indian cities. More individuals now have asthma, heart disease, and die too young as a result. Likewise, nations without decent sewage systems or easy access to pure water nonetheless have plenty of incidences of water-borne illnesses including cholera and diarrhoea.
Impact of environmental regulations on disease prevention
Environmental regulations deal with the causes of numerous diseases, hence they are rather vital for maintaining human health. Particularly in areas where requirements for water and air quality have been enhanced and treatment of hazardous waste has been improved, these regulations have clearly helped to reduce health hazards. Particularly beneficial in reducing the prevalence of lung diseases like asthma, coughing, and COPD is air quality regulations. For instance, the Clean Air Act in the United States has drastically reduced harmful chemicals, which over time has helped to lower lung ailments. Less individuals with asthma and other respiratory issues needing hospital visits have also been connected to EU laws on air quality, which centre on pollutants including particulate matter (PM2.5) and nitrogen dioxide. Rules protecting the environment by reducing air pollution and restricting exposure to hazardous chemicals have helped to somewhat lower incidence of heart disease and stroke. Strict air quality regulations have been linked in studies to lower incidence of heart attacks and strokes. This is so because two main drivers of heart disease, inflammation and oxidative stress, are lowered by smaller levels of particulate matter. Reduced rates of high blood pressure and heart disease have also been related to policies meant to lower noise pollution, such as those applied in traffic management and urban planning. Rules on water quality, which guarantee everyone has access to hygienic bathrooms and clean drinking water, have greatly helped to avoid illnesses such cholera, dysentery, and diarrhoea transmitted by water. Including rules for improved sanitation and safe drinking water for underdeveloped nations has helped to drastically lower the number of avoidable cases of these diseases.
RESULT AND DISCUSSION
Particularly in high-income regions with robust regulatory regimes, the comparison reveals that environmental health regulations are quite closely correlated with improved health outcomes for individuals. Diseases transmitted through the lungs, the heart, and the water have dropped dramatically since more stringent guidelines for environmental controls, waste management, and air and water quality were adopted. Strict policies enforced by European Union members and the United States have produced significant improvements in health outcomes including reduced incidence of heart disease and asthma. But in emerging countries like India and China, problems like fast urbanisation, weak enforcement, and a lack of healthcare facilities still make it hard for environmental laws to work. These results show that rules need to be enforced more strictly in areas with low incomes.(16)
|
Table 2. Health Outcomes Comparison by Region |
||||
|
Country/Region |
AQI (Average) |
Respiratory Disease Incidence (per 100 000) |
Cardiovascular Disease Incidence (per 100 000) |
Cancer Incidence (per 100 000) |
|
United States |
50 |
220 |
150 |
400 |
|
Germany |
45 |
180 |
140 |
380 |
|
India |
150 |
320 |
230 |
250 |
|
China |
135 |
280 |
200 |
300 |
|
Brazil |
110 |
250 |
180 |
280 |
Look at table 2 to see many countries have strict environmental laws that have led to big drops in air pollution and diseases linked to it. This shows that rules about air quality can improve health. The U.S. Clean Air Act and the European Union’s air quality guidelines have been successful at lowering amounts of dangerous pollution such as particulate matter (PM2.5), nitrogen dioxide (NO2), and sulphur dioxide (SO2). Figure 2 shows a total list of AQI values and the health problems they cause by country.
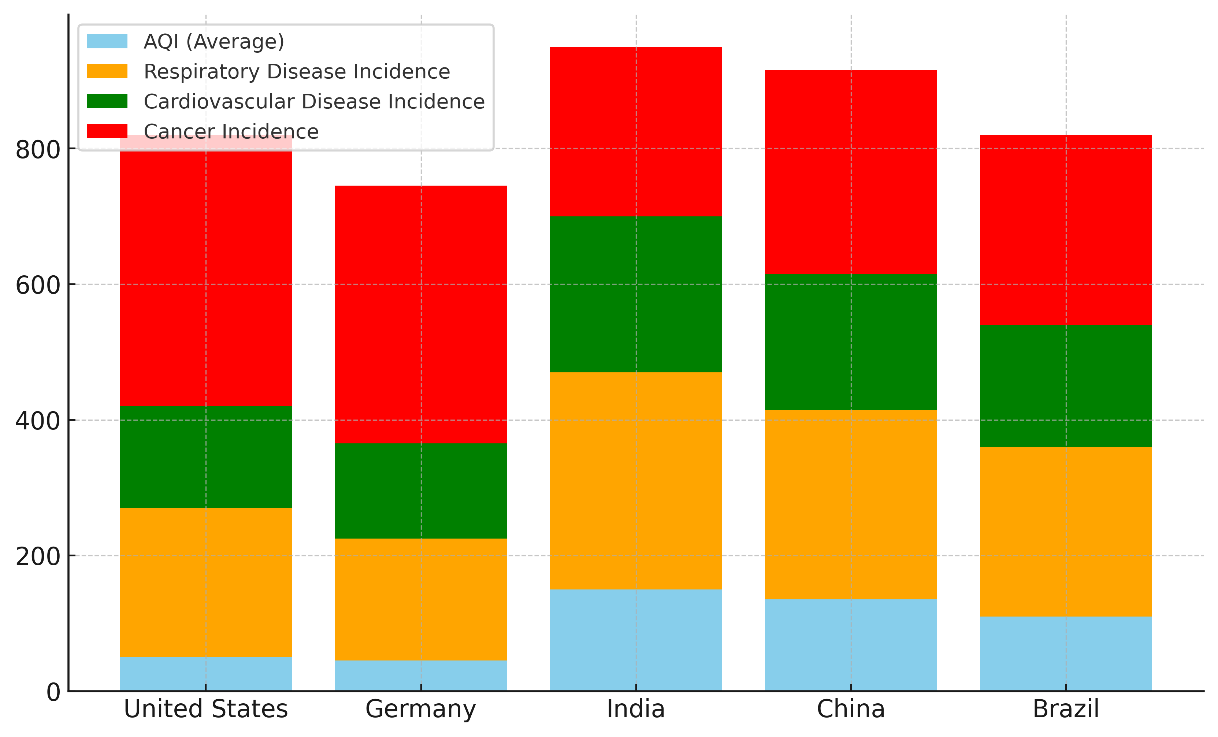
Figure 2. Cumulative Breakdown of AQI and Health Incidences by Country
There is evidence that these rules have led to better public health, especially a drop in lung illnesses like asthma, chronic obstructive pulmonary disease (COPD), and lung cancer.(17) Countries with strict rules on air quality have seen fewer people going to the hospital with lung illnesses and heart diseases, both of which are affected by air pollution. In figure 3, you can see how the AQI and health measures have changed over time and how they have changed in different countries.

Figure 3. Trends in AQI and Health Metrics Across Countries
The Clean Air Act has been linked to big changes in the quality of the air in the United States, which has led to fewer lung diseases and heart attacks. In the same way, the European Union’s rules on air quality have helped lower the number of early deaths caused by air pollution. Figure 4 shows a comparison of the AQI values and the number of diseases in various countries.
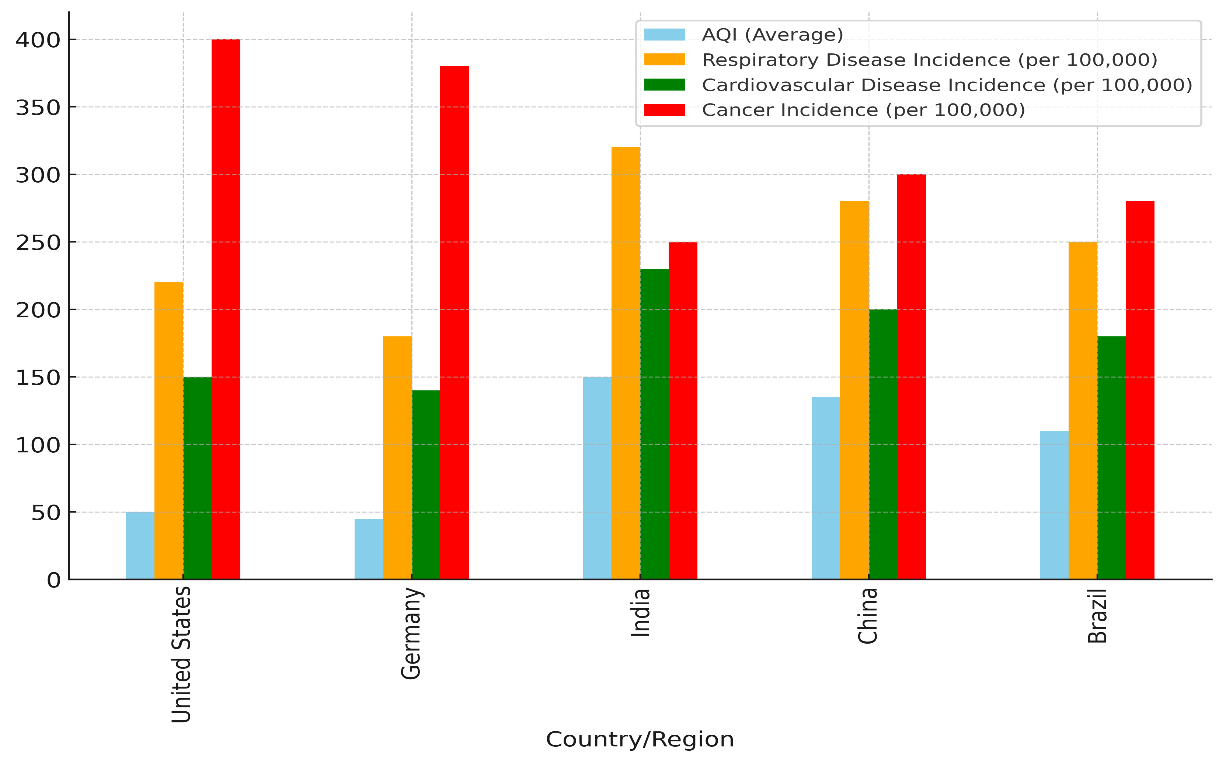
Figure 4. Comparative Analysis of AQI and Disease Incidences by Country
How well rules about air quality affected the number of cases of lung diseases, heart diseases, and cancer before and after these rules were put in place. But for these rules to work, they need to be strictly enforced, watched over, and problems with socioeconomic inequality that affect some groups more than others need to be fixed. For health results to get even better, policies will need to be updated and changed all the time.(18)
|
Table 3. Effectiveness of Air Quality Regulations on Health Outcomes |
||||
|
Country/Region |
Pre-Regulation Respiratory Disease Incidence (per 100 000) |
Post-Regulation Respiratory Disease Incidence (per 100 000) |
Pre-Regulation Cancer Incidence (per 100 000) |
Post-Regulation Cancer Incidence (per 100 000) |
|
United States |
300 |
220 |
420 |
400 |
|
European Union |
280 |
180 |
400 |
380 |
|
China |
350 |
280 |
370 |
300 |
|
India |
320 |
250 |
330 |
280 |
Table 3 shows information on how well rules about air quality have helped lower the number of deaths from lung diseases and cancer. Stricter rules about air quality in the US have cut the number of respiratory diseases by a large amount, from 300 per 100 000 to 220 per 100 000. Figure 5 shows how rules about the surroundings affect the number of cases of lung and cancer diseases by country.
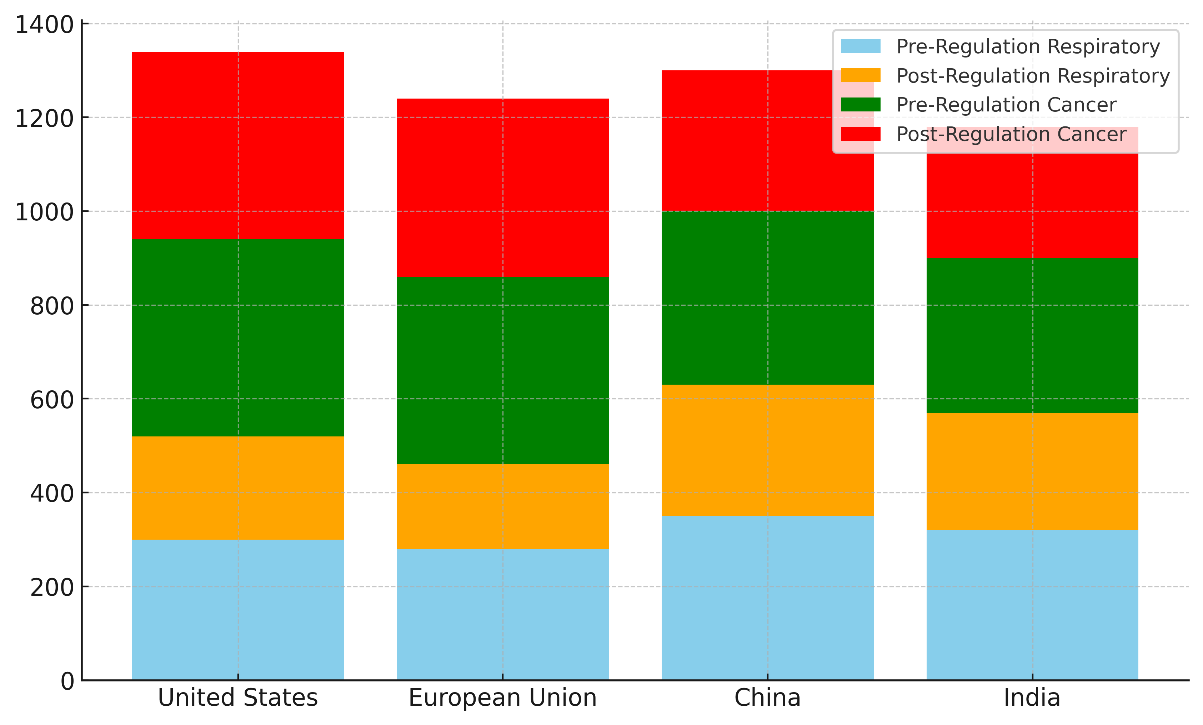
Figure 5. Impact of Regulations on Respiratory and Cancer Disease Incidences by Country
They have also cut the number of cancers by a small amount, from 420 per 100 000 to 400 per 100 000. The good effects of the Clean Air Act can be seen in this improvement. The Act helped lower harmful pollutants like nitrogen dioxide and particulate matter.(19) Even stronger effects of air quality rules can be seen in the European Union, where the number of cases of respiratory diseases dropped from 280 per 100 000 to 180 per 100 000 and the number of cases of cancer dropped from 400 per 100 000 to 380 per 100 000. These gains have been helped by the EU’s strict rules on air pollution, especially when it comes to particulate matter. Figure 6 shows differences between countries by comparing health incidents that happened before and after laws.
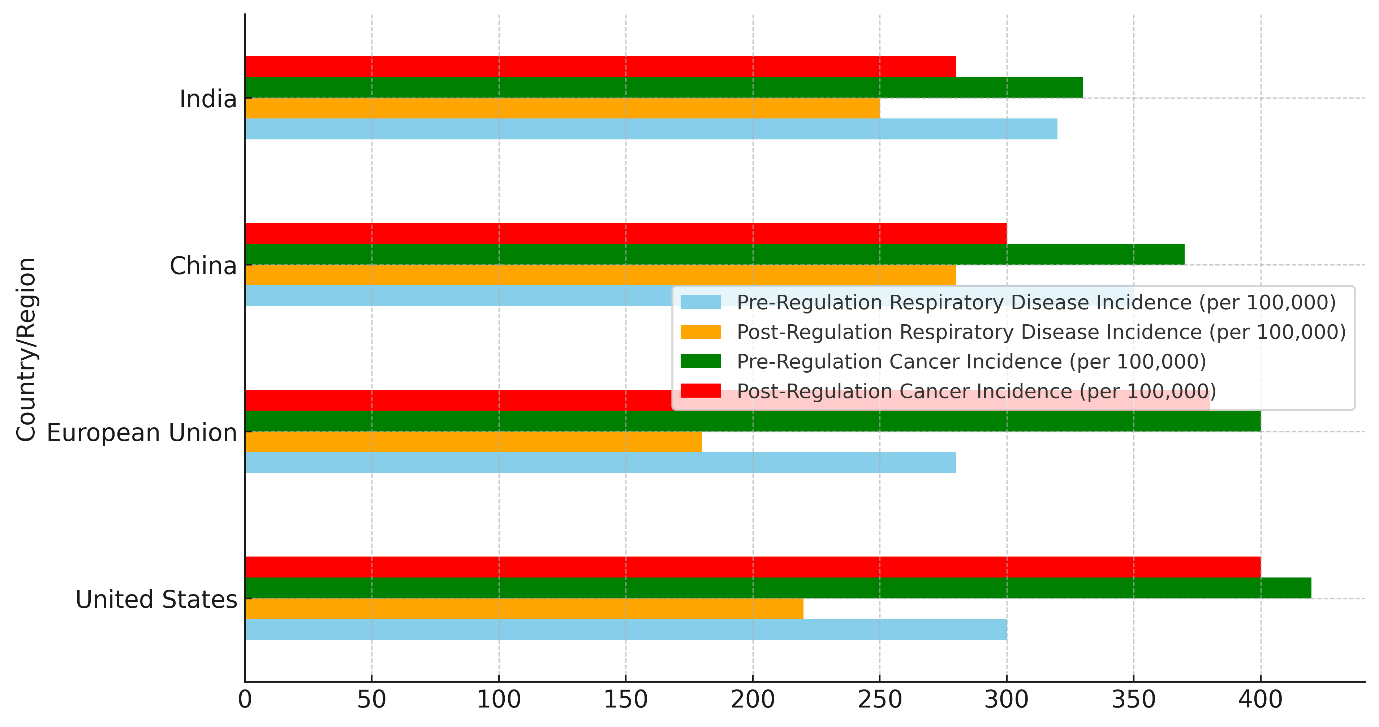
Figure 6. Comparison of Pre- and Post-Regulation Health Incidences Across Countries
China’s respiratory disease rates have gone down from 350 per 100 000 to 280 per 100 000, but their cancer rates have only gone down from 370 per 100 000 to 300 per 100 000, which is not a very big drop. India also saw a drop in the number of cases of respiratory diseases (from 320 per 100 000 to 250 per 100 000) and cancer cases (from 330 per 100 000 to 280 per 100 000), which shows some progress in reducing the health risks related to air pollution.(20)
CONCLUSIONS
This study shows how important public health rules are for improving the health of patients. By looking at regions with different rules, the study shows that strong environmental health policies can greatly lower the number of diseases that are caused by environmental factors. These policies should focus on improving air and water quality, managing waste, and limiting exposure to toxic substances. In high-income countries with strict rules, like the US and European countries, lung and circulatory conditions have gone down, water quality has gotten better, and deaths linked to the environment have gone down. The fact that these countries have strict environmental laws shows that they work to improve public health generally. But the study also shows that there are big differences between areas. Lack of strong environmental health laws, along with problems like lax enforcement, fast industrialisation, and poor healthcare facilities, make it hard for regulatory measures to work in low- and middle-income countries. The number of sicknesses caused by bad natural conditions is still high in places like India, China, and parts of sub-Saharan Africa. This shows the need for stricter rules that cover more areas. The study also shows that public health programs and easy access to health care are important to go along with environmental rules. Educating the public, encouraging people to take steps to avoid getting diseases, and improving the system of healthcare can make environmental policies work better and lower the health risks that come from being exposed to the environment.
BIBLIOGRAPHIC REFERENCES
1. Connor, A.; Lillywhite, R.; Cooke, M. The carbon footprint of a renal service in the United Kingdom. QJM Int. J. Med. 2010, 103, 965–975.
2. Pozo Herrera G. The training of values since developing teaching in the Physical Education class. Pedagog. Constell. 2023;2(1):28-37.
3. Campion, N.; Thiel, C.L.; DeBlois, J.; Woods, N.C.; Landis, A.E.; Bilec, M.M. Life cycle assessment perspectives on delivering an infant in the US. Sci. Total Environ. 2012, 425, 191–198.
4. Guailla Muñoz YE. Gamification strategies for understanding biological concepts in first-year high school students. Pedagog. Constell. 2023;2(1):38-47.
5. McAlister, S.; Grant, T.; McGain, F. An LCA of hospital pathology testing. Int. J. Life Cycle Assess. 2021, 26, 1753–1763.
6. Willskytt, S.; Tillman, A.M. Resource efficiency of consumables—Life cycle assessment of incontinence products. Resour. Conserv. Recycl. 2019, 144, 13–23.
7. Abd El-Salam, M.M. Hospital waste management in El-Beheira governorate, Egypt. J. Environ. Manag. 2010, 91, 618–629.
8. de Carvalho Rangel JP, Alvarez Valdivia IM, Morodo Horrillo A. Teacher training for inclusive education of students with hearing disabilities in the Angolan context. Pedagog. Constell. 2023;2(1):48-61. https://doi.org/10.69821/constellations.v2i1.15
9. Ahmad, R.; Liu, G.; Santagata, R.; Casazza, M.; Xue, J.; Khan, K.; Nawab, J.; Ulgiati, S.; Lega, M. LCA of hospital solid waste treatment alternatives in a developing country: The case of district Swat, Pakistan. Sustainability 2019, 11, 3501.
10. Carino, S.; Porter, J.; Malekpour, S.; Collins, J. Environmental Sustainability of Hospital Foodservices across the Food Supply Chain: A Systematic Review. J. Acad. Nutr. Diet. 2020, 120, 825–873.
11. Eckelman, M.J.; Sherman, J. Environmental impacts of the U.S. health care system and effects on public health. PLoS ONE 2016, 11, e0157014.
12. Van Straten, B.; Ligtelijn, S.; Droog, L.; Putman, E.; Dankelman, J.; Weiland, N.H.S.; Horeman, T. A life cycle assessment of reprocessing face masks during the Covid-19 pandemic. Sci. Rep. 2021, 11, 17680.
13. Artta Bandhu Jena. (2015). Profitabiity Analysis : A Study of Hidhustan Petrolium Corportion Limited. International Journal on Research and Development - A Management Review, 4(1), 125 - 132.
14. Salazar Marcano RC. Technological innovation in education. Pedagog. Constell. 2023;2(2):41-9.
15. Leena P. Singh, Binita Panda. (2015). Impact of Organisational Culture on Strategic Leadership Development with Special Reference to Nalco. International Journal on Research and Development - A Management Review, 4(1), 133 - 142.
16. Sisinno, C.; Moreira, J.C. Ecoefficiency: A tool to reduce solid waste production and waste of materials in health care units. Cad. Saude Publica 2005, 21, 1893–1900.
17. Sanyé-Mengual, E.; Sala, S. Life Cycle Assessment support to environmental ambitions of EU policies and the Sustainable Development Goals. Integr. Environ. Assess. Manag. 2022.
18. Gulcimen, S.; Aydogan, E.K.; Uzal, N. Life cycle sustainability assessment of a light rail transit system: Integration of environmental, economic, and social impacts. Integr. Environ. Assess. Manag. 2021, 17, 1070–1082.
19. Flores G, Díaz González LL. Diagnosis of assertive communication among UNES teachers: Implications for educational quality. Pedagog. Constell. 2023;2(2):27-40.
20. Seifert, C.; Koep, L.; Wolf, P.; Guenther, E. Life cycle assessment as decision support tool for environmental management in hospitals: A literature review. Health Care Manag. Rev. 2021, 46, 12–24.
FINANCING
No financing.
CONFLICT OF INTEREST
The authors declare that there is no conflict of interest.
AUTHORSHIP CONTRIBUTION
Data curation: Pooja Varma, Gauri Tamhankar, Sonia Mehta, Antaryami Pradhan.
Methodology: Pooja Varma, Gauri Tamhankar, Sonia Mehta, Antaryami Pradhan.
Software: Pooja Varma, Gauri Tamhankar, Sonia Mehta, Antaryami Pradhan.
Drafting - original draft: Pooja Varma, Gauri Tamhankar, Sonia Mehta, Antaryami Pradhan.
Writing - proofreading and editing: Pooja Varma, Gauri Tamhankar, Sonia Mehta, Antaryami Pradhan.