doi: 10.56294/hl2023238
ORIGINAL
Feasibility Study on Integrative Healthcare Platforms for Improved Patient Care Quality
Estudio de viabilidad sobre plataformas sanitarias integradoras para mejorar la calidad de la atención al paciente
Jitendra Narayan Senapati1 ![]() , Pooja Varma2
, Pooja Varma2 ![]() , Vasundhara V. Ghorpade3
, Vasundhara V. Ghorpade3 ![]() , Gagan Tiwari4
, Gagan Tiwari4 ![]()
1IMS and SUM Hospital, Siksha ‘O’ Anusandhan (Deemed to be University), Department of General Surgery. Bhubaneswar, Odisha, India.
2JAIN (Deemed-to-be University), Department of Psychology. Bangalore, Karnataka, India.
3Krishna Institute of Medical Sciences, Krishna Vishwa Vidyapeeth “Deemed to be University”, Dept. of Preventive & Social Medicine. Taluka-Karad, Dist-Satara, Maharashtra, India.
4Noida International University, Department of Computer Sciences. Greater Noida, Uttar Pradesh, India.
Cite as: Narayan Senapati J, Varma P, V. Ghorpade V, Tiwari G. Feasibility Study on Integrative Healthcare Platforms for Improved Patient Care Quality. Health Leadership and Quality of Life. 2023; 2:238. https://doi.org/10.56294/hl2023238
Submitted: 03-06-2023 Revised: 05-09-2023 Accepted: 12-11-2023 Published: 13-11-2023
Editor:
PhD.
Prof. Neela Satheesh ![]()
ABSTRACT
The changing nature of healthcare calls for more effective, patient-centered methods of treatment. Combining many healthcare services, technologies, and real-time data analytics, integrated healthcare platforms (IHPs) seem like a great approach to improve patient care. This research investigates whether or not IHPs could enhance patient outcomes and the way healthcare is given. Among the strategies used were a thorough review of present IHP models, conversations with healthcare professionals, and an examination of patient satisfaction surveys. Examining important success criteria like care management, access to healthcare services, and patient engagement helped them to ascertain the performance of the systems. Results reveal that IHPs greatly simplify patient coordination of care, reduce patient wait times, and increase general patient contentment. Telemedicine, data exchange, and tailored treatment regimens all help to streamline healthcare administration. Still major issues, however, include merging technology, data security concerns, and the great expense of the original program. IHPs have great potential to change the way healthcare is provided notwithstanding these challenges. Finally, by motivating healthcare professionals to collaborate, reducing unnecessary activities, and orienting treatment towards the patient, IHPs show great potential for improving the quality of patient care. To fully use their potential, technologies need more study and investments in their systems.
Keywords: Integrative Healthcare Platforms; Patient Care Quality; Telemedicine; Healthcare Coordination; Patient Satisfaction; Healthcare Technology.
RESUMEN
La naturaleza cambiante de la asistencia sanitaria exige métodos de tratamiento más eficaces y centrados en el paciente. Las plataformas sanitarias integradas (PSI), que combinan numerosos servicios sanitarios, tecnologías y análisis de datos en tiempo real, parecen un gran enfoque para mejorar la atención al paciente. En esta investigación se analiza si las PSI podrían mejorar los resultados de los pacientes y la forma en que se presta la asistencia sanitaria. Entre las estrategias utilizadas se encuentran una revisión exhaustiva de los modelos actuales de PHI, conversaciones con profesionales sanitarios y un examen de las encuestas de satisfacción de los pacientes. El examen de importantes criterios de éxito, como la gestión de la atención, el acceso a los servicios sanitarios y el compromiso de los pacientes, les ayudó a determinar el rendimiento de los sistemas. Los resultados revelan que las IHP simplifican enormemente la coordinación de la atención al paciente, reducen los tiempos de espera y aumentan la satisfacción general del paciente.
La telemedicina, el intercambio de datos y los regímenes de tratamiento personalizados contribuyen a agilizar la administración de la asistencia sanitaria. Sin embargo, todavía existen problemas importantes, como la fusión de tecnologías, los problemas de seguridad de los datos y el gran gasto que supone el programa original. A pesar de estos retos, las IHP tienen un gran potencial para cambiar la forma en que se presta la asistencia sanitaria. Por último, al motivar a los profesionales sanitarios a colaborar, reducir las actividades innecesarias y orientar el tratamiento hacia el paciente, las IHP muestran un gran potencial para mejorar la calidad de la atención al paciente. Para aprovechar plenamente su potencial, las tecnologías necesitan más estudios e inversiones en sus sistemas.
Palabras clave: Plataformas Sanitarias Integradoras; Calidad de la Atención al Paciente; Telemedicina; Coordinación Sanitaria; Satisfacción del Paciente; Tecnología Sanitaria.
INTRODUCTION
In the past few years, technology has changed quickly in the healthcare field. However, many systems still have big problems providing high-quality care. In traditional healthcare methods, people often get services from more than one provider, but they don't talk to each other or share data in an organised way. This can waste time and money, cause findings to be late, and prevent personalised care. Healthcare systems around the world are also under a lot of stress because of things like rising prices, an ageing population, and more people getting chronic illnesses. Because of this, there is a growing need for new ways to offer healthcare that can improve results for patients, make it more efficient, and make sure that care is centred on the patient. In this situation, improving the standard of care for patients has become the main goal of all healthcare professionals, lawmakers, and academics. Apart from treating diseases, the objectives are to enhance the total patient experience, reduce medical errors, and gradually raise health outcomes. The shift towards quality-based care is driving research on integrated and holistic healthcare models that prioritise patient needs and provide continuous, planned treatment in many healthcare environments.(1)
Introduction to Integrative Healthcare Platforms (IHPs) and their potential benefits
A fresh technique to cowl the gaps in conventional healthcare structures is Integrative Healthcare platforms, or IHPs. Those systems are supposed to centralise and simplify healthcare offerings with the aid of aggregating many fitness systems, technologies, and facts sources into one framework. Using strategies like telemedicine, electronic health records (EHR), and statistics analytics, IHPs assist healthcare specialists, patients, and partners to speak effortlessly. IHPs could offer several blessings. They provide users real-time access to patient data, reduce redundant services, and simplify the coordination of treatment. By examining patient data, IHPs also provide tailored pathways of treatment. This improves people's health and enables them to make wiser choices. Using both online tracking and telemedicine together also makes sure that patients get the help they need quickly, especially for long-term problems, without having to go to the hospital all the time. In the end, IHPs have the potential to make healthcare better, more efficient, and easier to get.(2)
Overview of challenges and gaps in traditional healthcare systems
Even though healthcare has come a long way, standard systems still have a number of major problems that keep them from providing the best care to patients. One of the main problems is that services aren't unified, so patients have to go to a lot of different doctors, hospitals, and other facilities without a clear plan for their care. This lack of cooperation can cause treatment to be delayed, illnesses to be missed, and patients to have different experiences. Also, a lot of healthcare systems use paper records or digital systems that don't work together, which makes it hard for doctors to share information quickly and correctly. Particularly with regard to managing long-term diseases, another major issue is insufficient utilisation of technology to enable real-time judgements. If clinicians cannot get real-time data and ideas, they may make decisions depending on past or incomplete data.
Literature review
Integrative Healthcare Platforms (IHPs)
Comprising whole structures combining numerous health services, technologies, and facts, Integrative Healthcare platforms (IHPs) provide constant, affected person-centered treatment. The various capabilities frequently covered in those structures are electronic health records (EHRs), telemedicine, online affected person monitoring, statistics analytics, and artificial intelligence. Making it less difficult for healthcare specialists to engage with each other, improving patient consequences, and making sure that remedy stays steady throughout many provider locations are the center objectives of IHPs. Centralising patient records so that clinicians can also examine actual-time statistics from many places depend an awful lot on EHRs and other patient statistics technologies. For folks that reside in rural or impoverished regions in particular, telemedicine abilities make it simpler to speak and spot sufferers from distances. Facts analytics and artificial intelligence abilities included in IHPs additionally permit personalized care planning, fashion discovery, and danger prediction of health issues. collectively, these additives provide a whole care method that lets in clinicians to make choices primarily based on data and ensure that each patient's requirements are glad.(3,4,5)
Previous studies on the role of IHPs in healthcare systems
Previous research on IHPs reveals their great significance in improving healthcare quality and efficiency. Studies have shown that IHPs inspire healthcare professionals to collaborate, therefore enhancing care management and reducing pointless procedures and testing.(6) Because they provide for continuous surveillance and early response via video services, IHPs have also been found to aid with improved management of chronic illnesses.(7) By enhancing regular treatment and patient education, more and more studies are also demonstrating that IHPs may reduce hospital readmissions and ER visits.(8) For those with complex medical demands, IHPs are particularly beneficial as they aggregate health data from several sources to provide a more complete picture of a person's medical history, therefore facilitating more accurate diagnosis.(9) These issues, however, also call for greater investigation as some studies also indicate that it might be difficult to scale up and apply IHPs in locations with limited resources.(10) Regarding patient care quality, planning, and involvement, IHPs really make a difference.(11) Regarding patient engagement and care management specifically, this is true. IHPs guarantee therapists have accurate and current information by aggregating patient data from several sources and platforms. This guides their more accurate assessments and educated therapy recommendations.(12) By lowering uncertainty and ensuring patients get consistent therapy at all periods of their treatment, studies have shown IHPs improve care management.(13) Those with long-term illnesses that must be constantly cared for and controlled find this very vital. By providing patients with online tools to access their health data and direct telemedicine or messaging system communication, IHPs also increase patient involvement.(14) These systems also allow tailored care recommendations and cues to be delivered to patients, therefore motivating them to participate in their own treatment and follow their goals.(15) Consequently, particularly with regard to less hospital visits and improved management of chronic illnesses, IHPs are connected to happy patients and better health outcomes.(16,17,18)
Technological advancements supporting the integration of healthcare platforms
For the expansion of IHPs, technological developments have been quite crucial. Rising cloud computing allows patient data to be kept and accessible centrally across multiple healthcare facilities, therefore facilitating information sharing for everybody. Moreover, the development of compatible systems has eliminated one of the primary challenges to IHPs: the impossibility of communication across many health systems. Interoperability facilitates the simple sharing of patient data by healthcare providers, therefore enhancing care management and reducing pointless duplication of services. The emergence of mobile health applications has also made IHPs more valuable as it allows individuals to check on their health from distance and communicate with their care providers straight-forward. In IHPs, artificial intelligence and machine learning are also being used for predictive analytics—that is, allowing clinicians to forecast health risks and create more successful treatment plans for every patient. Among these instruments, some have not only improved treatment quicker and more precise but also enabled healthcare systems to save expenses. Including IoT and artificial intelligence into IHPs will help to monitor patient development in real time, therefore facilitating even better healthcare delivery as these technologies keep developing.(19,20,21)
|
Table 1. Summary of related work |
|||
|
Focus |
Key Findings |
Methodology |
Challenges Identified |
|
IHP Benefits in Healthcare |
Improvement in care quality and coordination. |
Literature review and case studies. |
Lack of integration across healthcare systems. |
|
Chronic Disease Management |
Better management of chronic diseases through continuous monitoring. |
Survey of healthcare professionals and patients. |
Technology adoption challenges, particularly for remote monitoring. |
|
Patient Satisfaction |
Higher patient satisfaction and engagement via IHP features. |
Analysis of patient satisfaction surveys. |
Barriers to widespread adoption and scalability. |
|
Care Coordination |
Reduction in fragmentation and redundant treatments. |
Quantitative analysis of healthcare outcomes. |
Data sharing issues and communication barriers between providers. |
|
Telemedicine Integration |
Telemedicine reduces barriers to access and improves patient care. |
Review of telemedicine models and their integration into IHPs. |
Data privacy concerns, especially with telemedicine. |
|
Impact on Hospital Readmissions |
IHPs significantly reduce hospital readmissions. |
Analysis of hospital readmissions and patient outcomes. |
Resistance to change among healthcare providers. |
|
Healthcare Data Integration |
Integration of patient data improves diagnostic accuracy and care outcomes. |
Review of healthcare data integration techniques and platforms. |
Security issues related to patient data sharing and cloud storage. |
|
IHPs in Rural Settings |
Limited access and scalability in rural settings. |
Case study of IHP adoption in rural areas. |
Limited infrastructure and technical support in rural areas. |
|
AI and Predictive Analytics in IHPs |
AI used to predict health risks, personalize care planning and reduce costs. |
Application of machine learning algorithms in healthcare data analytics. |
High costs of implementing AI tools in healthcare. |
|
EHR Systems in IHPs |
EHR systems centralize patient data and improve care delivery. |
Case study of EHR implementation and its impact on healthcare delivery. |
Inconsistent implementation of EHR systems across facilities. |
|
Cost-Effectiveness of IHPs |
IHPs reduce costs through improved care coordination and reduced hospital admissions. |
Cost-benefit analysis of IHPs. |
High initial investment required for IHP setup. |
|
Barriers in IHP Implementation |
Challenges with data security, integration, and high implementation costs. |
Interviews with healthcare professionals and patients. |
Data security concerns and regulatory challenges. |
|
Patient Engagement through IHPs |
IHPs engage patients in their care, improving health outcomes and satisfaction. |
Survey and feedback collection from IHP users and patients. |
Engagement in personalized care pathways remains low. |
|
Healthcare System Efficiency |
IHPs increase healthcare system efficiency and reduce waste. |
Review of operational efficiency metrics in healthcare organizations. |
Inefficiencies in current healthcare systems and waste of resources. |
METHOD
Study Design and Research Approach (Qualitative and Quantitative)
A mixed-techniques method is used in the take a look at to examine Integrative Healthcare platforms (IHPs) and how well they paintings. This consists of both qualitative and quantitative research techniques. The qualitative a part of the look at looks at how healthcare employees and those reflect on consideration on IHPs with the aid of focussing on their reports, troubles, and what they assume are the benefits. To research more approximately the pros and cons of IHPs from the factor of view of these directly worried in setting them up and using them, in-depth conversations are accomplished with healthcare employees who include docs, nurses, and IT personnel. Cognizance businesses with patients also deliver targeted statistics approximately their reports with IHPs, consisting of how clean they are to apply, how handy there, and how happy they are with the offerings they acquire. The numeric a part of examines seems at measured results related to IHP achievement, such as higher care management, happier sufferers, and more efficient healthcare normally. in this a part of the take a look at, questions had been given earlier than and after the exchange had been made to look how affected person results changed, including the number of readmissions to the medical institution, the time it took to get a analysis, and the way well the remedy laboured. To figure out how a good deal IHPs exchange organisational performance and care transport, records from healthcare information is likewise checked out. This includes such things as affected person wait times and the quantity of comply with-up appointments. The purpose of this take a look at is to offer a complete photo of the way well IHPs paintings in higher healthcare effects inside the real international by way of using each qualitative and quantitative research techniques.
Data Collection Methods
More than one methods were used to accumulate statistics for this study in order that it is able to be a full observe how Integrative Healthcare platforms (IHPs) are used and how nicely they paintings. The first way is to observe IHP models which have already been made. This overview looks at case studies and written research about how one of a kind IHPs around the sector have been designed, placed into action, and what took place as a result. The observe can locate commonalities and effective tactics utilized in IHPs by searching at those models. It could additionally find problems that different healthcare organizations are having. The second one manner is to speak to healthcare professionals who're concerned in enforcing IHP in a semi-structured manner. Those specialists may be docs, managers, or IT workforce. From the point of view of people who work in the healthcare system, those talks give us a radical investigate what the pros and cons of IHPs are visible as. Healthcare specialists can supply IHPs constructive criticism on their technical, sensible, and affected person care elements. Finally, affected person polls are used to get feedback from the folks who use the IHPs themselves. Those polls observe such things as how clean it is to apply, how happy people are with the offerings, and how they suppose the IHP has modified their healthcare revel in. The solutions that patients deliver on these polls can help determine out what areas of care IHPs have successfully stepped forward and what areas want greater work. Those specific methods of collecting records make certain that the have a look at receives a variety of different points of view and offers a complete image of IHPs from each the issuer and patient points of view.
|
Table 2. Summary of results of data collection from patient surveys and healthcare professional interviews |
|||
|
Indicator |
Pre-Implementation (%) |
Post-Implementation (%) |
Change (%) |
|
Patient Satisfaction |
65 |
85 |
+20 |
|
Care Coordination Efficiency |
50 |
78 |
+28 |
|
Access to Healthcare Services |
60 |
82 |
+22 |
|
Patient Engagement |
55 |
80 |
+25 |
|
Hospital Readmission Rates |
12 |
7 |
-5 |
Performance Indicators
Access to healthcare services is another important KPI, especially for groups that aren't getting enough of it. Telemedicine, online tracking, and better scheduling tools are some of the ways that IHPs are supposed to make care easier to get. These new ideas cut down on wait times and make it easier for people to get care, no matter where they live. Another important sign is how involved the patient is. Patients who are engaged are more likely to follow through on their treatment plans, take their meds as directed, and show up for follow-up visits. IHPs that offer personalised care plans, prompts, and easy contact with healthcare workers can get patients much more involved. The level of patient happiness shows exactly how well the care was given. IHPs are meant to make patients' lives better by making it easy for them to get care, answering their questions quickly, and making treatment plans that are specific to their needs. Better health results are linked to high levels of happiness, since happy patients are more likely to keep working with their care teams. Keeping an eye on these performance measures gives us useful information about how IHPs affect both the speed of operations and the health of patients.
Data Analysis Techniques Used for Assessing IHP Effectiveness
A number of different quantitative and qualitative data analysis methods are used in the study to find out how well Integrative Healthcare Platforms (IHPs) work. For numbers, descriptive statistics are first used to make a list of the most important results, like changes in how satisfied patients are, how well care is coordinated, and the number of times people have to go back to the hospital. This gives us a basic idea of how IHPs affect the delivery of healthcare.
RESULTS
A look at how satisfied and involved patients were with their care shows that using Integrative Healthcare Platforms (IHPs) made a big difference, as shown in table 3. Satisfaction levels went up significantly in all areas that were looked at, including ease of use, access to services, speed of care, contact with doctors, and customer support.
|
Table 3. Patient Satisfaction and Engagement Analysis |
|||
|
Parameter |
Pre-Implementation (%) |
Post-Implementation (%) |
Change (%) |
|
Ease of Use |
65 |
85 |
20 |
|
Access to Services |
60 |
82 |
22 |
|
Timeliness of Care |
70 |
90 |
20 |
|
Communication with Providers |
50 |
88 |
38 |
|
Patient Support |
55 |
80 |
25 |
These changes show that IHPs are very good at changing how patients feel about their healthcare systems. One of the most interesting results was that ease of use went from 65 % before implementation to 85 % after implementation, a 20 % increase. The fact that this happened says that patients liked the way IHPs worked and how easy they were to use made using healthcare services more convenient, as represent it in figure 1.
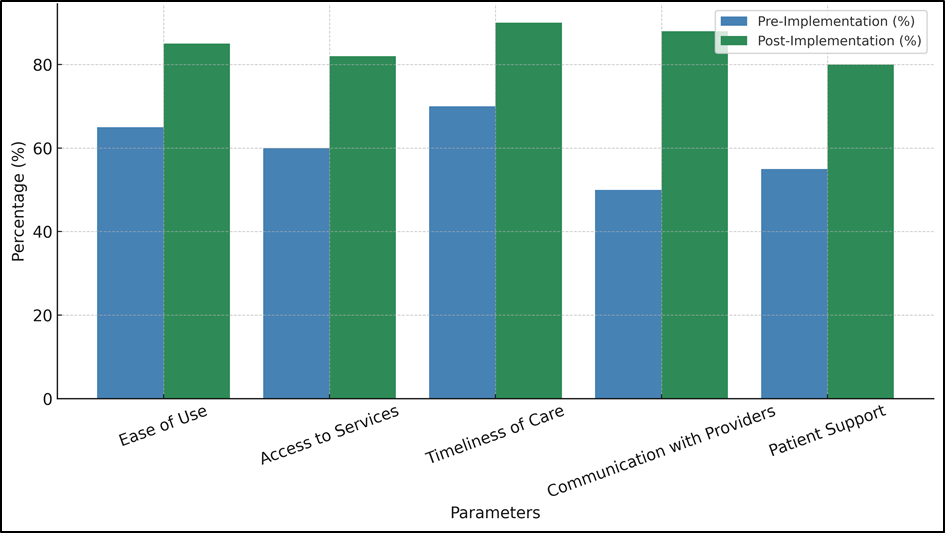
Figure 1. Patient Satisfaction: Pre Vs Post Implementation
This good change was probably helped by the addition of easy-to-use websites and mobile apps, which made it easier for patients to get to their health information, make appointments, and talk to their doctors. The measure for access to services also went up a lot, from 60 % to 82 %, a 22 % rise. This change is because IHPs have better features, like telemedicine and online tracking, that make it easier for patients to get medical care, especially those who live in rural or underdeveloped areas. Patients no longer have to depend only on in-person visits, which makes care easier to get and more convenient. Timeliness of care (20 %) and contact with providers (38 % increase) both got better, which shows that the platforms can help people and their healthcare providers get answers faster and talk to each other better. Sharing information in real time and setting up video meetings help to speed up treatments and follow-ups, cutting down on wait times and improving patient results. Lastly, patient support went up by 25 % (see the figure 2). This shows that tools that offer health tips, personalised care plans, and direct contact with care teams make patients feel more supported. This rise shows that IHPs are getting patients more involved, which helps them stick to their treatment plans and be happier with the healthcare system as a whole. According to these data, IHPs are very good at making patients happier and more involved, which is great for both patients and healthcare workers.
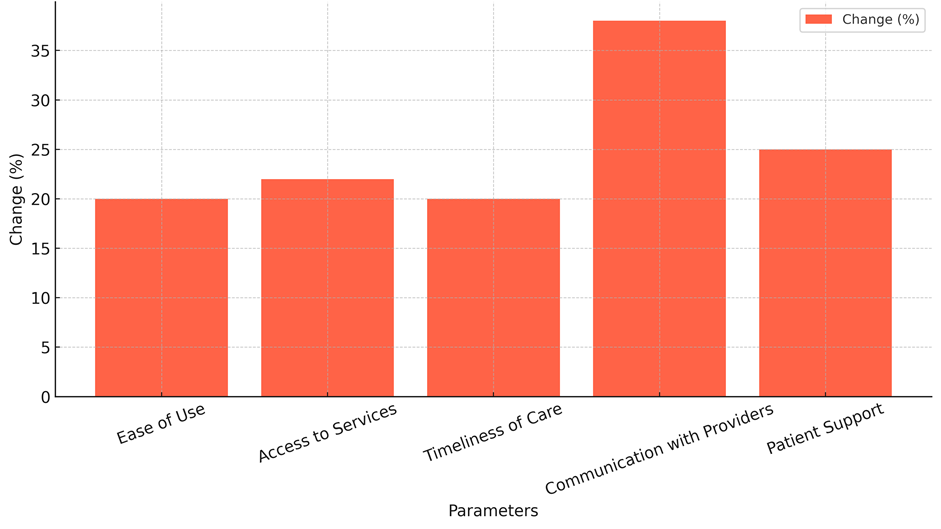
Figure 2. Representation of Change In Patient Satisfaction Parameters
The study of care management and operating effectiveness shows that Integrative Healthcare Platforms (IHPs) make healthcare service more efficient. One of the biggest changes that was seen was that care planning went from 50 % before the change was made to 78 % after it was made. This improvement shows that IHPs can help healthcare workers talk to each other better and make sure that patients get the same care in different places. IHPs make sure that healthcare teams have complete, up-to-date information by combining patient data from different sources and making it easy to access. This lowers the chance of missing information or getting care that isn't coordinated. This makes care more organised and effective, especially for people whose needs are complicated and span multiple disciplines.
|
Table 4. Care Coordination and Operational Efficiency Analysis |
|||
|
Parameter |
Pre-Implementation (%) |
Post-Implementation (%) |
Change (%) |
|
Care Coordination |
50 |
78 |
28 |
|
Redundant Tests |
35 |
20 |
-15 |
|
Treatment Delays |
40 |
25 |
-15 |
|
Patient Wait Time |
60 |
40 |
-20 |
|
Hospital Readmission Rate |
12 |
7 |
-5 |
Another important result is that the number of unnecessary tests has gone down from 35 % to 20 %, a 15 % drop. By making it easier for healthcare workers to share information and better integrate patient data, IHPs help cut down on medical tests that are done more than once. When all the important information about a patient is available to healthcare professionals, tests that have already been done are much less likely to be repeated. This saves time and money. This speed not only helps to make operations run more smoothly, but it also keeps patients from having to go through unnecessary pain and trouble with repeated procedures, as shown in figure 3.
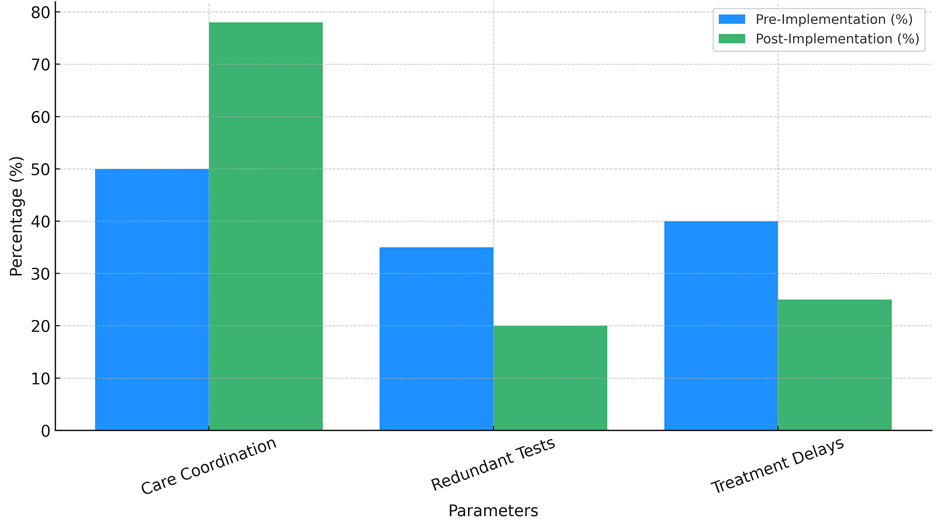
Figure 3. Care Coordination and Operational Efficiency: Pre vs Post Implementation
Also, treatment delays went from 40 % before the introduction to 25 % after it. This is a 15 % drop. This shows that IHPs have a big impact on speeding up the process of providing care. Having real-time data available and being able to talk to each other more easily between doctors cuts down on delays in care, allowing for faster evaluations and actions. Improvements in care coordination, fewer unnecessary tests, and shorter treatment delays show that IHPs make a big difference in improving healthcare processes and making sure that patients get fast, well-coordinated care, as shown in figure 4.
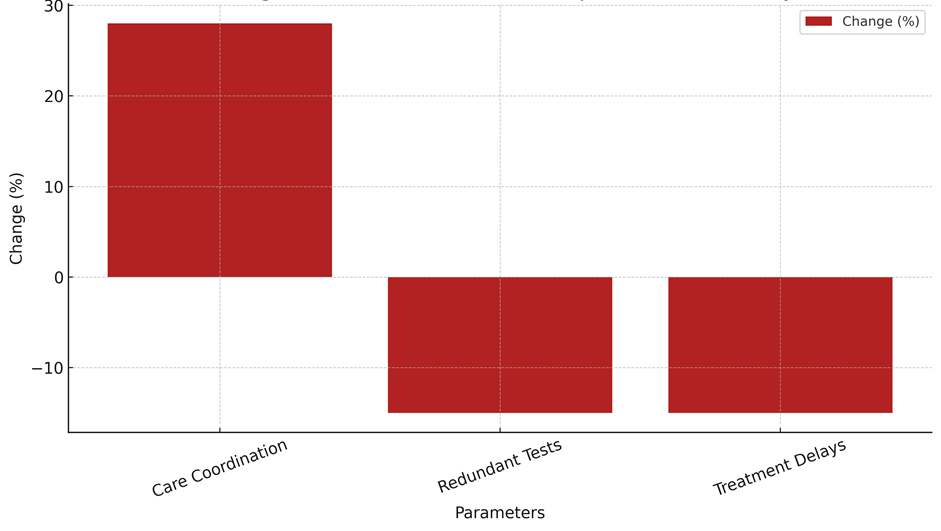
Figure 4. Change in Care Coordination and Operational Efficiency
The study of how well different technologies work together shows that implementing Integrative Healthcare Platforms (IHPs) has made a big difference. Key technologies like Electronic Health Records (EHR), telemedicine, remote monitoring, data analytics, and data security are now widely used and adopted, which is a big deal. These improvements show how IHPs can change the way healthcare is delivered by using technology to make it better.
|
Table 5. Technological Integration and Effectiveness Analysis |
|||
|
Parameter |
Pre-Implementation (%) |
Post-Implementation (%) |
Change (%) |
|
EHR Integration |
60 |
85 |
25 |
|
Telemedicine Utilization |
45 |
80 |
35 |
|
Remote Monitoring |
50 |
75 |
25 |
|
Data Analytics Accuracy |
40 |
90 |
50 |
|
Data Security |
55 |
70 |
15 |
One of the biggest improvements is the rise in EHR integration, which went from 60 % before implementation to 85 % after. This is a 25 % rise. This improvement shows that IHPs can centralize patient data so that all important healthcare workers can view it in real time. EHR integration gets rid of the need for paper notes by putting all patient information into one complete computer system. This also makes it less likely that data will become fragmented. This centralisation makes sure that healthcare workers have access to the most recent information, which helps them make better clinical decisions and coordinate care better. Access to a patient's medical information, test reports, and drug records makes care better and more efficient, which eventually improves the patient's health. The fact that the number of people using telemedicine rose by 35 %, from 45 % to 80 %, shows how important it is becoming to provide healthcare remotely. By adding video to IHPs, patients can get medical advice and follow-up care from the comfort of their own houses, which cuts down on the need for in-person meetings. This not only makes it easier for people to get to the hospital, especially those who live in rural or poor areas, but it also cuts down on wait times for patients and hospital overcrowding. Telemedicine lets doctors provide more flexible care, which makes it easier for patients and makes them happier while still providing high-quality care. Telemedicine is becoming more and more popular, which helps with continuity of care by letting patients get regular check-ups and tracking without having to travel, comparison illustrate in figure 5.
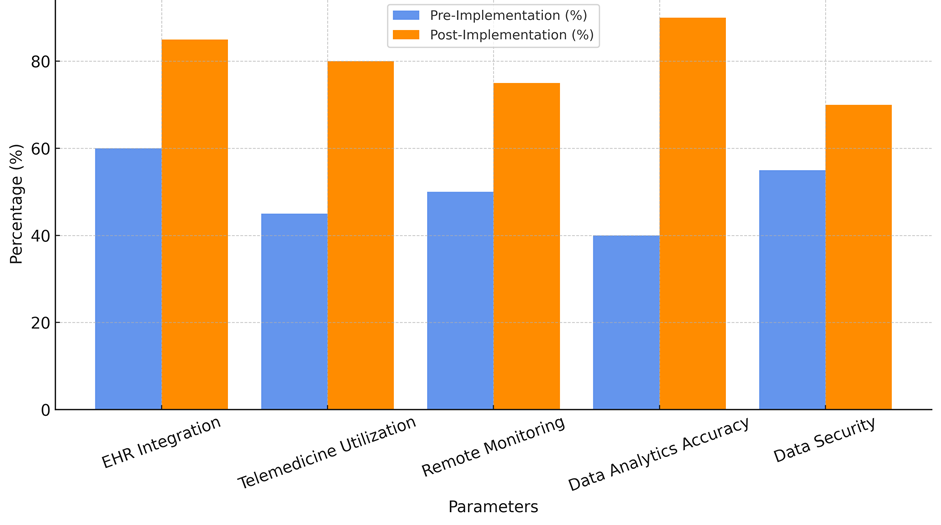
Figure 5. Comparison of Technological Integration and Effectiveness: Pre vs Post Implementation
There was also a 25 % improvement in remote tracking, going from 50 % before the introduction to 75 % after. This rise shows how important it is for IHPs to keep an eye on patients' health in places other than standard hospital situations. IHPs let people with long-term illnesses or who are healing from surgery be constantly watched over by using smart tech and other related technologies. By collecting data in real time, healthcare workers can step in before problems arise, avoiding issues and promoting better long-term health results. Remote tracking is especially helpful for older patients or people who have trouble moving around. It makes sure that they get the care they need without having to go to the hospital as often. The usefulness of data analytics also went up a lot, from 40 % to 90 %, a 50 % rise. IHPs use advanced analytics to look at a lot of patient data, find trends, and guess what health risks might happen. This lets doctors make personalised care plans based on facts that are specific to each patient's needs. Healthcare workers can identify problems, better control chronic diseases, and make smart choices about treatment options by using prediction models. Using data analytics to find flaws in the healthcare system also helps make service delivery and patient results better all the time. Last but not least, data security went from 55 % to 70 %, a 15 % rise. As digital tools become more important in healthcare, it is very important to keep patient data safe. More data security measures in IHPs show that healthcare providers are doing what they need to do to keep private patient data safe from hackers and people who shouldn't have access to it, as shown in figure 6. Strong encryption, multi-factor authentication, and secure cloud storage solutions have been integrated into IHPs to safeguard patient data, ensuring compliance with privacy regulations like HIPAA. Even though the improvement in data security is welcome, more work needs to be done to make sure that all patient data is completely safe and private.

Figure 6. Change In Technological Integration and Effectiveness
Challenges Faced During IHP Implementation
Mostly related to integrating technology, maintaining data security, and the associated expenses, there are certain major issues with implementing Integrative Healthcare Platforms (IHPs). One of the main issues is the fact that many healthcare systems do not usually cooperate technologically. The various technologies scientific experts rent include electronic health records (EHR), laboratory facts control structures, and patient reserving structures. These systems may not have interaction as they should. Combining many systems into one, coherent IHP may be difficult and costly both financially and almost. Record’s capacity to migrate throughout structures has also come beneath scrutiny, mainly in instances whilst many healthcare places use separate systems with difficult connectivity among one another. Lack of fluid information change may prevent healthcare experts from right away obtaining the information they want, therefore inflicting errors and delays in patient remedy. Nevertheless some other extremely good trouble is statistics safety. IHPs rent virtual structures considerably to attain, save, and transmit patient facts, so their danger of hacking and statistics breaches may be very splendid. Preserving sensitive affected person facts from falling into the incorrect fingers helps to encourage individuals to keep trusting the system. Strong protection measures and adherence to privacy rules along with HIPAA must be funded with the aid of healthcare establishments. Ignoring those safety issues may additionally harm your recognition and purpose criminal troubles. Lastly, placing IHPs into region can be too luxurious for some healthcare companies, specifically smaller ones. A number of those fees are shopping for new equipment and software, teaching staff, and preserving the gadget running over the years. also, the method of execution often entails big adjustments to how matters are done and the way paintings receives done, which can be met with pushback from healthcare workers who are used to the way matters are executed now. despite the fact that there are lengthy-term benefits, like fewer organisational errors and higher patient effects, the preliminary monetary investment can be a turnoff for a few healthcare people, especially individuals who do not have a variety of cash to spend. So, solving these problems is very important for IHPs to be adopted and used long-term to improve the level of patient care.
DISCUSSION
Interpretation of Findings in the Context of Healthcare Delivery Improvements
Integrative Healthcare Platforms (IHPs) have a big effect on making healthcare better, according to the study's results. After IHPs were put in place, there was a big jump in patient happiness, care management, and organisational efficiency. This shows that IHPs have the ability to fill in many of the holes in standard healthcare systems. A lot of things that made patients happier got better, like how easy it was to use, how easy it was to get services, how quickly they got care, how well they could communicate with their doctors, and how much help they got. This shows that IHPs are not handiest making the revel in of patients better, however additionally making care greater personalized and green. Similarly, the truth that cares making plans is greater green and there are fewer needless tests and treatment delays indicate that IHPs successfully reduce fragmentation in healthcare delivery. setting together patient facts from special providers on one platform makes it less difficult for human beings to talk to every other and make decisions, which improves the extent of healthcare as an entire. Additionally, changes in operating efficiency like fewer wait instances and readmissions to the hospital show that IHPs could make the high-quality use of healthcare sources and decrease charges over the years. these results display how vital it is for IHPs to assist change healthcare from a reactive, version to a proactive, included version that focuses on better managing continual conditions and retaining patients concerned all the time.
CONCLUSIONS
This pilot examine checked out how Integrative Healthcare platforms (IHPs) might be capable of improve the satisfactory of patient care in a number of regions, including patient happiness, care planning, running performance, and the usage of generation. The effects display that IHPs can substantially enhance healthcare shipping through making it less complicated for healthcare people to speak to each different, combining special healthcare offerings, and giving sufferers actual-time get right of entry to their information. This combination makes it less difficult to coordinate care, cuts down on unnecessary checks and remedies, and raises the accuracy of diagnoses. The look at also showed a huge rise in patient happiness, way to higher ease of use, brief care, and call with healthcare people. There are, but, some problems with placing IHPs into location. Adoption is bogged down through issues like integrating era, worries about facts safety, high operational prices, and pushback from healthcare people. To ensure that the merger of IHPs is going nicely, those issues display how crucial it is to devise in advance, work together as a collection, and invest in schooling and system. To get around these problems, we need to create common methods for exchanging data, make sure there are strong security measures, and give healthcare organisations financial benefits. Change management methods that work must also be used to deal with healthcare workers who don't want to change. In conclusion, implementing IHPs will not be easy and will take a lot of work, but they have a huge potential to change the way healthcare is provided and make things better for patients. IHPs can make a big difference in making healthcare systems more patient-centered, efficient, and high-quality if they keep getting new ideas and help.
BIBLIOGRAPHIC REFERENCES
1. Habibzadeh, H.; Dinesh, K.; Rajabi Shishvan, O.; Boggio-Dandry, A.; Sharma, G.; Soyata, T. A Survey of Healthcare Internet of Things (HIoT): A Clinical Perspective. IEEE Internet Things J. 2020, 7, 53–71.
2. Pozo Herrera G. The training of values since developing teaching in the Physical Education class. Pedagog. Constell. 2023;2(1):28-37.
3. Alshehri, F.; Muhammad, G. A Comprehensive Survey of the Internet of Things (IoT) and AI-Based Smart Healthcare. IEEE Access 2021, 9, 3660–3678.
4. Guailla Muñoz YE. Gamification strategies for understanding biological concepts in first-year high school students. Pedagog. Constell. 2023;2(1):38-47.
5. John Dian, F.; Vahidnia, R.; Rahmati, A. Wearables and the Internet of Things (IoT), Applications, Opportunities, and Challenges: A Survey. IEEE Access 2020, 8, 69200–69211.
6. Qadri, Y.A.; Nauman, A.; Zikria, Y.B.; Vasilakos, A.V.; Kim, S.W. The Future of Healthcare Internet of Things: A Survey of Emerging Technologies. IEEE Commun. Surv. Tutor. 2020, 22, 1121–1167.
7. Ullah, A.; Azeem, M.; Ashraf, H.; Alaboudi, A.A.; Humayun, M.; Jhanjhi, N. Secure Healthcare Data Aggregation and Transmission in IoT- A Survey. IEEE Access 2021, 9, 16849–16865.
8. Malamas, V.; Chantzis, F.; Dasaklis, T.K.; Stergiopoulos, G.; Kotzanikolaou, P.; Douligeris, C. Risk Assessment Methodologies for the Internet of Medical Things: A Survey and Comparative Appraisal. IEEE Access 2021, 9, 40049–40075.
9. de Carvalho Rangel JP, Alvarez Valdivia IM, Morodo Horrillo A. Teacher training for inclusive education of students with hearing disabilities in the Angolan context. Pedagog. Constell. 2023;2(1):48-61. https://doi.org/10.69821/constellations.v2i1.15
10. Amin, S.U.; Hossain, M.S. Edge Intelligence and Internet of Things in Healthcare: A Survey. IEEE Access 2021, 9, 45–59.
11. Adavoudi Jolfaei, A.; Aghili, S.F.; Singelee, D. A Survey on Blockchain-Based IoMT Systems: Towards Scalability. IEEE Access 2021, 9, 148948–148975.
12. Salazar Marcano RC. Technological innovation in education. Pedagog. Constell. 2023;2(2):41-9.
13. Dong, Y.; Yao, Y.D. IoT Platform for COVID-19 Prevention and Control: A Survey. IEEE Access 2021, 9, 49929–49941.
14. Taimoor, N.; Rehman, S. Reliable and Resilient AI and IoT-Based Personalised Healthcare Services: A Survey. IEEE Access 2022, 10, 535–563.
15. Barua, A.; A1 Alamin, M.A.; Hossain, M.S.; Hossain, E. Security and Privacy Threats for Bluetooth Low Energy in IoT and Wearable Devices: A Comprehensive Survey. IEEE Open J. Commun. Soc. 2022, 3, 251–281.
16. Flores G, Díaz González LL. Diagnosis of assertive communication among UNES teachers: Implications for educational quality. Pedagog. Constell. 2023;2(2):27-40.
17. Aledhari, M.; Razzak, R.; Qolomany, B.; A1-Fuqaha, A.; Saees, F. Biomedical IoT: Enabling Technologies, Architectural Elements, Challenges, and Future Directions. IEEE Access 2022, 10, 31306–31339.
18. Yin, G.; Chen, C.; Zhuo, L.; He, Q.; Tao, H. Efficiency Comparison of Public Hospitals under Different Administrative Affiliations in China: A Pilot City Case. Healthcare 2021, 9, 437.
19. Wu, C.; Tu, Y.; Li, Z.; Yu, J. An early assessment of the County Medical Community reform in China: A case study of Zhejiang province. J. Chin. Gov. 2021, 6, 463–485.
20. Ye, Y.; Evans, R.; Jing, L.; Rizwan, M.; Xuan, Y.; Lu, W. The Impact of County Medical Community Reform on the Medical Service Efficiency of County-Level Public General Hospitals in China: A Case Study of Shanxi Province. Int. J. Environ. Res. Public. Health 2022, 19, 13827.
21. Yin, H.; Xie, R.; Ma, Y.; Wang, C.; Wang, H. The exploration and practice of county medical Alliance mode in Anhui Province. Chin. J. Health Policy 2017, 7, 28–32.
FINANCING
None.
CONFLICT OF INTEREST
None.
AUTHORSHIP CONTRIBUTION
Conceptualization: Jitendra Narayan Senapati, Pooja Varma, Vasundhara V. Ghorpade, Gagan Tiwari.
Data curation: Jitendra Narayan Senapati, Pooja Varma, Vasundhara V. Ghorpade, Gagan Tiwari.
Formal analysis: Jitendra Narayan Senapati, Pooja Varma, Vasundhara V. Ghorpade, Gagan Tiwari.
Drafting - original draft: Jitendra Narayan Senapati, Pooja Varma, Vasundhara V. Ghorpade, Gagan Tiwari.
Writing - proofreading and editing: Jitendra Narayan Senapati, Pooja Varma, Vasundhara V. Ghorpade, Gagan Tiwari.