doi: 10.56294/hl2023237
ORIGINAL
Implementing AI-Driven Diagnostic Tools to Improve Quality of Life Assessments
Aplicación de Herramientas de Diagnóstico Basadas en IA para Mejorar las Evaluaciones de la Calidad de Vida
Deepika Sharma1
![]() , Sudhansu Sekhar Patra2
, Sudhansu Sekhar Patra2
![]() , Sujayaraj Samuel Jayakumar3
, Sujayaraj Samuel Jayakumar3
![]() , Vasant Devkar4
, Vasant Devkar4
![]()
1Noida International University, Department of Computer Sciences. Greater Noida, Uttar Pradesh, India.
2IMS and SUM Hospital, Siksha ‘O’ Anusandhan (Deemed to be University), Department of General Surgery. Bhubaneswar, Odisha, India.
3JAIN (Deemed-to-be University), Department of Forensic Science. Bangalore, Karnataka, India.
4Krishna Institute of Medical Sciences, Krishna Vishwa Vidyapeeth “Deemed to be University”, Dept. of Medicine. Taluka-Karad, Dist-Satara, Maharashtra, India.
Cite as: Sharma D, Sekhar Patra S, Sujayaraj SJ, Devkar V. Implementing AI-Driven Diagnostic Tools to Improve Quality of Life Assessments. Health Leadership and Quality of Life. 2023; 2:237. https://doi.org/10.56294/hl2023237
Submitted: 02-06-2023 Revised: 04-09-2023 Accepted: 12-11-2023 Published: 13-11-2023
Editor:
PhD.
Prof. Neela Satheesh ![]()
ABSTRACT
Using artificial intelligence (AI) in the healthcare sector alters doctors’ major decision-making process. Evaluating patients’ quality of life (QoL) is one area where artificial intelligence seems rather promising. Understanding how various illnesses and therapies influence a person’s overall health depends much on quality of life testing. Standard QoL exams, which rely on hand-written assessments and patient comments on their health, have issues like being subjective, biassed, and sluggish when it comes to analyse vast volumes of data. AI-powered testing tools can provide more accurate, quick, scalable methods to evaluate QoL if one is looking for a way around these challenges. This essay examines how artificial intelligence technology could alter the methodology of quality of life surveys. Diagnostics based on artificial intelligence are quite useful. For patient anecdotes, for instance, natural language processing (NLP) may be employed; machine learning techniques can then be used to project QoL values from medical data. AI systems can handle a lot of clinical data including medical records, imaging data, patient-reported results to generate objective, real-time, tailored QoL evaluations consistent and reusable once and again. Furthermore, these instruments can identify early warning indicators of deterioration that would not be evident using more conventional approaches. the usage of several sorts of records sources inclusive of clever tech and cellular fitness apps which increases the accuracy of stories in real time and allows non-stop tracking AI-driven checking out will also be led via This method not handiest courses medical doctors in making better selections however additionally affords people extra manipulate over their fitness, therefore improving their excellent of life over time. The studies additionally addresses moral questions arising from AI-primarily based QoL assessments consisting of data protection, patient permission, and what clinical professionals should do upon assessment of AI outcomes. through discussion of these issues, this take a look at emphasises the need of ensuring that synthetic intelligence generation be applied in a way that complements the interaction among the affected person and company in preference to replaces human know-how.
Keywords: AI-Driven Diagnostics; Quality of Life Assessments; Machine Learning; Patient-Reported Outcomes; Healthcare Innovation.
RESUMEN
El uso de la inteligencia artificial (IA) en el sector sanitario altera el importante proceso de toma de decisiones de los médicos. La evaluación de la calidad de vida (CdV) de los pacientes es un ámbito en el que la inteligencia artificial parece bastante prometedora. Comprender cómo influyen las distintas enfermedades y terapias en la salud general de una persona depende en gran medida de los exámenes de calidad de vida. Los exámenes estándar de calidad de vida, que se basan en evaluaciones escritas a mano y en los comentarios de los pacientes sobre su salud, presentan problemas como la subjetividad, la parcialidad y la lentitud a la hora de analizar grandes volúmenes de datos. Las herramientas de análisis basadas en IA pueden proporcionar métodos más precisos, rápidos y escalables para evaluar la calidad de vida si se busca una forma de superar estos problemas. Este ensayo examina cómo la tecnología de inteligencia artificial podría alterar la metodología de las encuestas de calidad de vida. Los diagnósticos basados en inteligencia artificial son bastante útiles. Para las anécdotas de los pacientes, por ejemplo, se puede emplear el procesamiento del lenguaje natural (PLN); luego se pueden utilizar técnicas de aprendizaje automático para proyectar valores de calidad de vida a partir de datos médicos. Los sistemas de IA pueden manejar gran cantidad de datos clínicos, como historias clínicas, datos de diagnóstico por imagen o resultados notificados por los pacientes, para generar evaluaciones de la calidad de vida objetivas, en tiempo real, adaptadas, coherentes y reutilizables una y otra vez. Además, estos instrumentos pueden identificar los indicadores de alerta temprana de deterioro que no sería evidente el uso de enfoques más convencionales. el uso de varios tipos de fuentes de registros, incluida la tecnología inteligente y aplicaciones de fitness celular que aumenta la precisión de las historias en tiempo real y permite el seguimiento sin parar AI impulsada por la comprobación a cabo también se llevará a través de Este método no cursos handiest médicos en la toma de mejores selecciones, sin embargo, además, ofrece a las personas más manipular sobre su estado físico, por lo tanto, la mejora de su excelente calidad de vida en el tiempo. Los estudios, además, aborda cuestiones morales que surgen de AI-principalmente basado en evaluaciones de calidad de vida que consiste en la protección de datos, el permiso del paciente, y lo que los profesionales clínicos deben hacer tras la evaluación de los resultados de la IA. a través de la discusión de estas cuestiones, este echar un vistazo a hace hincapié en la necesidad de garantizar que la generación de inteligencia sintética se aplica de una manera que complementa la interacción entre la persona afectada y la empresa en lugar de reemplazar a los seres humanos know-how.
Palabras clave: AI-Driven Diagnostics; Quality of Life Assessments; Machine Learning; Patient-Reported Outcomes; Healthcare Innovation.
INTRODUCTION
Using artificial intelligence (AI) in healthcare to improve measurement and control of a patient’s quality of life (QoL) might represent a significant advance. Broadly speaking, quality of life (QoL) is a person’s general state of health and pleasure encompassing their bodily and psychological condition, social relationships, environment, and so on. Conventional methods of gauging quality of life include judgements based on what others observe, self-reported polls, and physician reviews. These approaches are constrained, nevertheless, by human prejudices, incomplete data, and difficulties with application. Conversely, AI-driven diagnostic technologies can overcome these issues by providing more exact, objective, scalable responses allowing for continuous, real-time measurement of quality of life. More and more artificial intelligence (AI) technologies—particularly natural language processing (NLP) and machine learning (ML)—are being applied in healthcare to enable patients to heal. AI can examine enormous volumes of data from numerous sources—medical records, picture data, smart health devices—for assessments of quality of life. Handling and comprehending this sort of data will enable us to better understand how illnesses, medications, and other interventions impact a patient’s life. By considering the individual characteristics and medical experiences of every patient, AI-powered solutions may also offer tailored assessments. This helps the evaluation process to be more comprehensive and tailored to every individual’s demand.(1) One possible approach to apply artificial intelligence in QoL evaluation is by looking at patient-reported outcomes (PRRs), using NLP techniques. Understanding QoL requires knowledge of PROs as they are direct remarks from patients regarding their health conditions that have not been altered or understood by medical professionals. Usually, though, determining what this data indicates requires hand examination, which takes a lot of time and is prone to error. AI systems can rapidly assess text-based data from patient surveys, professional notes, even social media postings, hence accelerating this procedure.
This technique of evaluating QoL is extra powerful and flexible seeing that artificial intelligence can utilise NLP to find out traits, analyse adjustments for the duration of time, and extract essential insights. The potential of AI-driven monitoring solutions to combine numerous kinds of facts to offer a extra whole image is among their strongest capabilities. actual-time recording of a patient’s critical symptoms, exercising level, and sleep styles the usage of wearable health devices and cell fitness programs permits for this non-stop flow of information facilitates synthetic intelligence structures provide extra flexible and present day checks of a affected person’s satisfactory of life whilst combined with everyday medical records. Small modifications in an affected person’s circumstance that trendy strategies might forget may be picked up with the aid of these AI devices.(2) This permits clinicians to choose interventions, cures, or way of life adjustments for a patient better. Artificial intelligence can also permit early discovery of probable health worries or disorders. Long-term data patterns permit artificial intelligence systems become aware of early caution signals of a declining high-quality of life, such more pain, growing mental issues, or much less physical activity. This preventative technique can permit individuals to be seeking for assistance while wished, therefore stopping most important fitness problems earlier than they begin and hence improving the overall affected person consequences. Although it has a few troubles, artificial intelligence has splendid capacity to enhance best of living rankings. Ethical concerns related to patient privateness, statistics safety, and authorisations have to be considered a good way to guarantee appropriate application of AI technology.
Background of Quality of Life (QoL) Assessments
This approach looks at health from all sides—not only the physical but also the psychological, social, and environmental ones. For a long time, quality of life has been assessed using patient-reported outcome measures (PROMs), like surveys asking patients to describe their feelings, symptoms, and how their diseases influence their life.(3) Clinical investigations, mental health care, cancer treatments, and long-term sickness management now all depend on these tests in great part. From the patient’s point of view, they assist doctors in determining the effectiveness of treatments and provide a more complete picture of how care influences persons outside of simply clinical outcomes. Figure 1 lists the components and procedures applied in evaluation of Quality of Life (QoL) measurements.
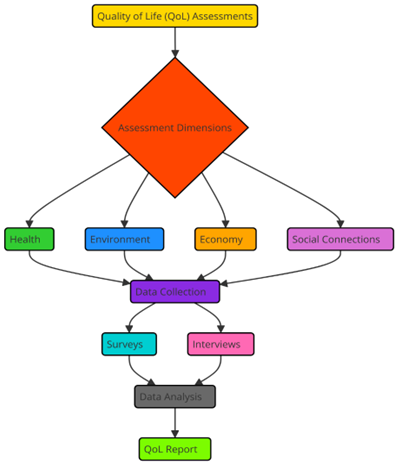
Figure 1. Illustrating Quality of Life (QoL) Assessments
Standard QoL tests, however, might be constrained by factors like biassed interpretation, patient memory problems, and the reality that they are often conducted at one moment in time. As it becoming more evident how crucial it is to continuously monitor patients and evaluate data in real time, healthcare is seeking more dynamic, dependable, objective means of measuring quality of life. In this case, cutting edge technologies like Artificial Intelligence (AI) are very important. They open up new ways to make QoL assessments more accurate and useful by combining many types of data.
Importance of Accurate QoL Evaluations in Healthcare
In healthcare, accurate QoL assessments are very important because they show how diseases and medicines affect patients in ways that go beyond the usual clinical measures. These tests help doctors figure out not only how bad a disease is, but also how it affects the patient’s daily life. This is important for customising treatment plans and making sure patients do better. When managing a chronic disease, for example, patients may not notice any changes in their state right away, but their quality of life (QoL) can get a lot worse. Some illnesses, like arthritis, diabetes, or depression, may not show up as major signs on a medical test, but they can make it very hard to do everyday things, keep relationships, or go to social events. By correctly measuring QoL, healthcare professionals can change how they care for patients, add the right medicines, and make changes to their lifestyles that will improve their general health.(4) Also, correct QoL assessments are very important for figuring out how well treatments work, especially in clinical studies. A treatment may sometimes make clinical signs better, like the size of the tumour or blood pressure, but it doesn’t always make the patient feel like their quality of life is much better. By using correct QoL measures, healthcare systems can make better choices about which medicines will not only help patients but also make their lives better. Accurate QoL data is also needed to make healthcare policies and decide how to use resources. Policymakers use QoL assessments to help them decide how much to spend on healthcare, how to create patient-centered solutions, and how to best use resources for groups of people who need a lot of different kinds of care.(5)
Literature review
Traditional Methods of Quality of Life Assessment
For a protracted length, quality of life (QoL) tests were a staple of healthcare as they offer essential statistics on a patient’s ordinary condition. those assessments was once carried out historically the usage of patient-reported outcome measures (PROMs), that are based questionnaires or surveys asking patients to score their social, mental, and bodily states. Regularly used instruments measuring a vast spectrum of factors, consisting of mental and physical health, social relationships, and environmental factors are the WHOQOL (world health organisation quality of life) and SF-36 (short form-36). Those regular strategies may be carried out in expert settings or as part of studies initiatives; they help one to understand the patient’s attitude approximately their health. Many in cancer, mental health, and continual infection control utilise them to screen affected person development, track treatment efficacy, and study how fitness troubles effect man or woman’s existence at some stage in time.(6) These strategies additionally permit clinicians to comprehend in ways beyond their clinical findings how operations, medicinal drugs, or treatments influence a affected person’s fine of lifestyles. Conversely, the checks and their interpretations commonly rely upon self-stated statistics, which can be distorted through factors like reminiscence bias, social choice bias, or people who conflict with clarity of concept.(7) Moreover, traditional approaches typically only capture QoL at specific times, which make it difficult to see how a patient’s health evolves during course of therapy or illness. More and more individuals believe these approaches are insufficient to provide comprehensive, real-time, objective assessments of QoL, even if they are still quite crucial in healthcare.
Limitations of Current Diagnostic Tools in QoL Evaluations
Patients may either not report their symptoms at all or report them too much because of social pressure, fear of being judged, or just not being able to remember things correctly. This makes the QoL rating process more subjective and biassed, which could change the real picture of the patient’s situation. In addition, standard methods are often rigid and only show QoL at a single point in time. This is a problem for people with diseases that change over time, like cancer, or long-term illnesses, like diabetes, where their quality of life can change a lot. Without constant, real-time tracking, these evaluations might miss important changes in the patient’s mental or physical health, which could cause delays in treatment or changes to care that aren’t as good as they could be.(8) Also, the problems with old tools are worse for some types of patients, like those who have trouble thinking clearly, little kids, or people who speak different languages. For these groups, QoL tests may not be as accurate or reliable as they should be. In these situations, tools like observed assessments or proxy assessments (where a carer or family member reports on the patient’s behalf) are used. However, they are also subject to bias, which makes it harder to get accurate QoL statistics.(9) Conventional approaches also make it more difficult to present a complete, complicated picture of a patient’s health as they often lack advanced analytics or many data sources. This is why healthcare professionals are searching for new, more flexible, objective measures of quality of life that would allow them to circumvent the issues with present approaches.
Advances in AI for Healthcare Diagnostics
Particularly in diagnosing tools and professional decision-making, artificial intelligence (AI) has advanced much in the field of medicine. AI might entirely transform the way Quality of Life (QoL) is measured by making extensive, rapid, and accurate reviews. Since they can examine a lot of data from many sources—including electronic health records (EHRs), medical pictures, smart devices, and patient-reported outcomes (PRRs)—adding machine learning (ML) technologies is a huge leap forward. These AI-powered tools can identify trends and links in data that would be difficult for human physicians to perceive. QoL ratings so are more accurate.(10) Improving QoL ratings depends partly on a component of artificial intelligence known as natural language processing (NLP). By analysing text-based data like patient reports, clinical notes, or even social media postings, NLP algorithms may determine people’s mood, how severe their symptoms are, and other factors influencing quality of life. Not achievable with conventional evaluations conducted at one point in time, this approach allows AI systems provide assessments in real time based on the patient’s condition that can indicate how their health and well-being evolve over time. AI has also made it simpler to design complete diagnosis systems using data from many sources. Personal health devices can monitor, for instance, a person’s vital signs, activity level, sleeping pattern, even indicators of mental health.(11) Combining this information with artificial intelligence techniques helps to provide a more complete picture of the patient’s quality of life (QoL), which can result in more tailored treatment plans and speedier responses. These technologies enable you monitor things constantly, thereby helping you to identify early harm that you would overlook otherwise. Table 2 summarises the methods in the literature research together with their advantages, disadvantages, and shortcomings.
|
Table 1. Summary of Literature Review |
|||
|
Algorithm |
Benefits |
Challenges |
Limitations |
|
Random Forest |
Handles complex data with high accuracy |
Requires large datasets for optimal performance |
Hard to interpret and explain |
|
Support Vector Machine (SVM) |
Good for binary classification |
Sensitive to feature scaling |
Prone to overfitting with small datasets |
|
k-Nearest Neighbors (k-NN) |
Simple and efficient for smaller datasets |
Not ideal for high-dimensional data |
May not capture complex relationships |
|
Convolutional Neural Networks (CNN)(12) |
Excellent for image-based QoL data |
Requires large datasets and computational power |
Requires large labeled datasets |
|
Recurrent Neural Networks (RNN) |
Effective for sequential data like time-series |
Requires significant computational resources |
Complex and difficult to train |
|
Natural Language Processing (NLP) |
Analyzes unstructured text for sentiment and patterns |
Requires clean and accurate textual data |
Relies heavily on pre-processing of data |
|
Deep Neural Networks (DNN) |
Highly flexible and adaptable |
Requires large amounts of training data |
Hard to interpret results |
|
Logistic Regression |
Interpretable and easy to implement |
Less flexible with non-linear data |
Can be less accurate with large feature sets |
|
Decision Trees |
Fast and efficient for classification tasks |
Overfitting with small datasets |
Not ideal for large datasets |
|
Naive Bayes |
Simple probabilistic model |
Less effective with highly imbalanced data |
Requires feature engineering |
|
XGBoost(13) |
High accuracy and robust performance |
Sensitive to noisy data |
Computationally expensive |
|
Gradient Boosting Machine (GBM) |
Handles non-linear data with flexibility |
Computationally expensive |
Not ideal for highly complex tasks |
|
Linear Regression |
Easy to interpret and understand |
Linear model, struggles with complex relationships |
May not capture all the important features |
|
Principal Component Analysis (PCA) |
Reduces data dimensionality for easier analysis |
Loss of information when reducing dimensionality |
Not ideal for highly complex tasks |
AI technologies in diagnostics
Machine Learning and Deep Learning Approaches
Two key artificial intelligence (AI) technologies that have greatly improved healthcare diagnostics are machine learning (ML) and deep learning (DL). Methods allowing computers to learn from data and improve over time without clear programming to accomplish so are known as ML. Using neural networks with multiple layers, DL is a subfield of machine learning that investigates intricate trends in large datasets. These technologies are applied in healthcare research based on real-time and past data to estimate illness progression, identify anomalies, and create individualised treatment regimens. Support vector machines (SVM), random forests, and k-nearest neighbours (k-NN) have been used to project patient outcomes by means of clinical data using machine learning techniques. Looking at complex medical data including imaging data and electronic health records (EHRs), these algorithms can identify trends suggesting a certain diagnosis or health course.(14) By learning from image data such as mammograms or CT scans and calculating how probable it is that the tissue is dangerous based on patterns people might not be able to perceive, ML models can discover early-stage cancer. Deep learning approaches especially convolutional neural networks (CNNs) have been quite successful in medical image analysis. CNNs are designed to operate with images and other data having a grid-like arrangement.
Step 1: Define the Problem and Data Representation
The first step involves defining the problem and preparing the data for analysis. In ML and DL, this is represented as:
![]()
Where:
xi represents the input features (data points).
yi represents the output or labels.
Step 2: Model Selection
Select a model (ML or DL algorithm). For example, in supervised learning, the goal is to learn a function f(x) that maps inputs to outputs:
![]()
Where:
f(x) is the function learned by the model.
ε is the error term or noise.
Step 3: Loss Function Definition
The loss function measures how well the model performs. For example, the mean squared error (MSE) for regression problems:
![]()
Where:
yi is the true label.
f(xi) is the predicted value.
n is the number of data points.
Step 4: Optimization
To minimize the loss function, optimization techniques like gradient descent are used:
![]()
Where:
θ are the model parameters (weights).
α is the learning rate.
∇θ L(θ) is the gradient of the loss function with respect to the parameters.
Step 5: Model Training
In ML and DL, training is the process of adjusting the model parameters to minimize the loss. The parameters θ are updated iteratively through optimization. In Deep Learning, this step involves updating weights in neural networks:
![]()
Where:
W represents weights.
x is the input vector.
b is the bias.
σ is the activation function (e.g., ReLU, Sigmoid).
Step 6: Evaluation and Prediction
After training the model, it is evaluated using a test set. Predictions are made by applying the learned function to new data:
![]()
Where:
ŷ is the predicted output for new input xnew.
Wfinal and b are the learned parameters after training.
Natural Language Processing for Patient Feedback
Natural language processing (NLP) is yet another moniker for artificial intelligence. NLP explores how human languages and computers could cooperate. An integral component of gauging quality of life (QoL) and monitoring patient behaviour, NLP is increasingly applied in healthcare to read and comprehend patient input. Surveys, interviews, or written reports—all of which include patient comments—can reveal a great deal about a patient’s health, symptoms, mental health, and treatment satisfaction. By use of NLP techniques, healthcare personnel may digest comments and increase their knowledge of the circumstances of their patients, therefore enabling better decisions. NLP helps one to examine both structured and unstructured patient feedback. This covers professional notes, responses to patient-reported outcome measures (PROMs), and even free-text notes from electronic health records (EHRs).(15) Patients could, for instance, jot free-form notes about their symptoms, concerns, or changes in their condition. This generates a lot of untamed data that has to be controlled. Two NLP techniques called named entity recognition (NER) and mood analysis enable one to extract relevant information from this arbitrary input. Processing and comprehension so proceed faster. For example, even if patients use odd or strange language, NLP may identify some indicators of emotional anguish in their remarks. By analysing a patient’s tone of speech, NLP can determine if they are discussing happiness, pain, or concern.
Computer Vision for Health Monitoring
Driven by CV, computer programs in X-rays, MRIs, CT scans, and other imaging modalities search for issues like infections, fractured bones, or tumours. Particularly in more complex or delicate instances, these systems can identify trends and nuances in the images that could be difficult for a clinician to perceive. Among other things, early indicators of lung cancer in chest X-rays, skin lesions for melanoma diagnosis, and eye pictures for diabetic retinopathy have been found effectively using CV algorithms. Computer vision is being used more and more in patient tracking tools, along with medical images.(16) With the help of cams or wearing tech, CV can keep an eye on a patient’s movement, stance, facial expressions, and even vital signs like heart rate and breathing rate. This constant tracking lets doctors check on a patient’s state in real time, which is especially helpful for people who have long-term illnesses, are recovering from surgery, or are older and may fall or lose their memory.(17)
Integration of AI in Real-Time Diagnostics
Using artificial intelligence (AI) in real-time testing is changing how doctors check on, treat, and keep an eye on their patients. Traditional medical methods, which often involve looking back at patient data, can’t always give you new information right away, which is especially true in emergency or fast-paced situations. Conversely, artificial intelligence technologies machine learning, deep learning, computer vision, and so on allow healthcare systems to make decisions instantly depending on real-time input from various sources. Real-time diagnostics are quite useful in settings like emergency rooms, intensive care units (ICUs), and during surgery when fast diagnosis of a patient is crucial for wise treatment decisions. AI-powered devices, for instance, can also continuously monitor a patient’s essential signs and symptoms coronary heart rate, blood stress, oxygen stages, and respiratory price and provide actual-time alerts to medical professionals should they hit upon any issues or symptoms of worsening. This preventive technique permits clinicians to interfere rapidly, consequently stopping problems earlier than they start and for this reason enhancing patient results. AI structures can accomplish greater than only monitor essential signs. They also can take a look at clinical image facts including dynamic scans or real-time video feeds. This link allows one to hold monitoring problems like strokes, traumas, or cardiac occasions whilst rapid clinical response is rather critical. AI can quick locate and look at sizable clinical photo factors as cancers, haemorrhages, or blockages and provide us precious records to allow quick reaction. By integrating records from several assets together with electronic health records (EHRs), the affected person’s historical past, smart era, and the surroundings adding artificial intelligence to real-time examinations also helps individuals make better decisions.(18)
Developing ai-driven diagnostic tools for qol assessments
Data Collection and Sources for QoL Assessments
Important clinical data from EHRs a patient’s medical history, treatment plans, diagnostic counts that enable clinicians determine a patient’s actual degree of illness aid them Patient-reported outcome measures (PROMs), which might be official questionnaires or interviews, are yet another crucial source of data. Patients give opinion information about their physical and mental health, emotional well-being, social functioning, and quality of life as a whole using these tools. There is a chance that these self-reported measures are biassed or inconsistent, but they are still useful because they show how the patient actually feels about their health state. Wearable tech, like fitness apps and health monitors, can constantly and real-timely record a person’s heart rate, exercise levels, sleep patterns, and other important body functions. This changing information is very helpful for keeping track of changes in QoL over time, like how mobile you are or how well you sleep, which could be caused by treatment or the disease getting worse. Mobile health apps and social media sites have also become useful tools for gathering information about patients’ emotional and mental health.(19)
AI Model Selection and Training
Choosing and teaching the correct AI model is absolutely crucial for developing diagnostic tools to evaluate Quality of Life (QoL). The artificial intelligence model must be capable of handling all the many types of patient data. This can encompass free-text patient comments and healthcare records as well as organised and unstructured data. Machine learning (ML) and deep learning (DL) models are used for those types of tasks. The version to use depends at the information and the goals of the research. a few of the most usually used machine mastering models in established information are assist vector machines (SVM), random forests, and logistic regression. This covers polls and EHRs. Those models are in reality splendid at figuring out or forecasting QoL outcomes primarily based on historic information. They can let you know, as an example, how a given medication might impact a patient’s pleasant of existence or degree of happiness. These models provide insightful analysis of crucial factors influencing pleasant of residing and are easier to comprehend. This qualifies them for instances when readability and comprehension are crucial. RNNs are quite awesome, for example, at processing repeated information from clever devices or monitoring critical symptoms over time. These models may additionally reveal modifications in best of existence over the years, simply as early caution signals indicate a patient’s circumstance is worsening. Natural language processing (NLP) techniques such temper evaluation and emotion recognition which assist to use textual content statistics to study patient intellectual fitness can also be used the use of deep learning models.(20)
Applications of ai in qol assessments
Mental Health Monitoring and Evaluation
In the realm of mental health tracking and review, artificial intelligence (AI) has advanced quite a distance. It currently provides nurses and doctors with powerful instruments for assessing the quality of life (QoL) of those suffering with mental health issues. Common approaches to check on someone’s mental health are self-reported questionnaires or in-person meetings, although they could not entirely depict the patient’s mental state or mood fluctuations. By combining data from multiple sources patient polls, electronic health records (EHRs), even social media or mobile apps to provide fuller and accurate information regarding mental health, artificial intelligence can assist get past these issues. Among the most crucial artificial intelligence techniques applied in monitoring mental health is natural language processing (NLP). Figure 2 provides mental health testing instrument and technique viewing, evaluation, and application guidelines.
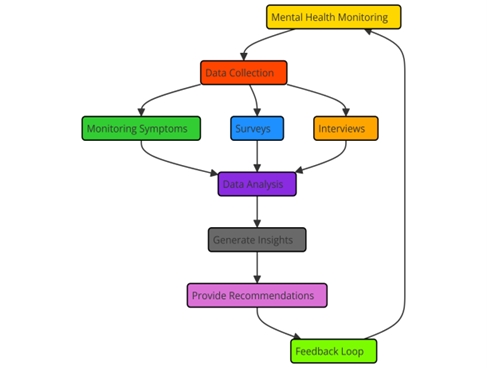
Figure 2. Illustrating Mental Health Monitoring and Evaluation
NLP can, for instance, scan text messages and indicate whether someone is unhappy, nervous, or contemplating suicide. This allows medical professionals assist patients sooner and provides real-time feedback to them. Often connected to mental health issues, wearable sensors controlled by artificial intelligence may also monitor physical activities, sleep patterns, and body indicators including heart rate. These devices help clinicians monitor concern, anxiety, or sad episodes in real time by providing continuous information on a patient’s physical and mental health. By aggregating data from several sources and applying machine learning algorithms, artificial intelligence can assist clinicians in determining a patient’s mental state. This allows data-based decisions on treatment and care for clinicians. Furthermore speedier and more accurate mental health tests can be created using artificial intelligence.
Chronic Disease Management
Managing chronic diseases with artificial intelligence has demonstrated great potential for improving the quality of life (QoL) of persons with diabetes, heart disease, and long-term lung issues. Treating chronic illnesses used to require routinely monitoring symptoms, living circumstances, and treatment compliance in the past. People found it difficult to do on their own and this took a lot of time. Conversely, artificial intelligence-powered solutions can streamline many aspects of treating chronic conditions. This helps one to see a patient’s condition in real time and provide them more individualised treatment. Combining data from sensors and smart devices tracking important indications such heart rate, blood pressure, glucose levels, and oxygen intake helps artificial intelligence be used primarily to assist control chronic conditions. Looking at this data, machine learning algorithms may identify trends, project future issues, and notify physicians and patients when any of the health variables fall short. By examining a diabetic patient’s glucose level, activity level, and food intake, artificial intelligence may, for instance, predict when they will experience hypoglycaemia. This allows doctors to act fast before the patient’s blood sugar dangerously drops. Because they provide patients tailored information on how to modify their lifestyle, take their prescriptions as advised, and track their symptoms, mobile health applications using artificial intelligence are also quite beneficial for managing long-term diseases. These applications’ machine learning systems examine data about every patient, including their level of activity, sleep quality, and prescription use, to provide tailored recommendations and cues meant to assist raise their quality of life.
Elderly Care and Mobility Assessments
Care for the elderly and studies of their movement are important parts of healthcare for ageing populations because they have a direct effect on the freedom and quality of life (QoL) of older people. More and more, AI is being used to track and evaluate the health, movement, and well-being of older people. This helps doctors better treat diseases related to getting older and makes the lives of senior citizens better. As the world’s population ages, AI-powered tools provide a flexible and effective way to meet the needs of older people, especially those who have trouble moving around or are more likely to fall. Wearable monitors and gadgets with AI are often used to keep track of an older person’s exercise level, stance, walking, and other signs of mobility. Machine learning systems can look at the data that these devices collect in real time to find early signs of declining movement or other health problems. For instance, AI systems can spot changes in the way a person walks that could mean they are more likely to fall or are losing their strength, which are familiar worries among older people. If healthcare professionals notice these changes early, they can help avoid accidents and improve quality of life by using focused physical therapy, movement aids, or changes to the surroundings. Monitoring brain ability is another important way that AI is used to care for the old. Alzheimer’s disease, dementia, and other forms of cognitive loss can make it harder for people to handle their daily tasks and stay independent. Voice recognition, speech analysis, and face recognition are all AI-powered tools that can keep an eye on cognitive health by noticing changes in speech patterns, facial expressions, or social interactions. These changes are often early signs of cognitive damage.
Future directions
Potential for AI to Revolutionize QoL Assessments
Artificial intelligence (AI) has great power to influence quality of life (QoL) assessments made by medical practitioners. Reviews are more accurate, dynamic, and personalised as artificial intelligence technologies significantly enhance how QoL is assessed, interpreted, and used in clinical settings. Conventional measurements of quality of life (QoL) can rely on frequent self-reports, polls, or conversations, which could not reflect how a patient’s health is evolving in real time. By continuously examining data from multiple sources including smart tech, electronic health records (EHRs), and patient-reported outcomes (PRRs)—AI can gain a complete and current picture of a patient’s health, thereby overcoming these issues. Using artificial intelligence in QoL testing is one of the nicest things about it as it can mix several types of data, including clinical data, psychological tests, and living elements. Machine learning applications allow one to examine this data and identify trends and patterns human physicians might overlook. AI can identify changes in a patient’s mental state, physical mobility, or social contacts that they might not be vocal about. This helps clinicians see more fully how a condition or therapy is compromising a patient’s quality of life. AI might also help to make it simpler to customise QoL assessments to every individual. Looking at large collections of patient data, artificial intelligence may create tailored QoL profiles for every patient. These profiles consider age, gender, treatment history, and other health issues the individual could have.
Integration with Wearable Devices and IoT
Combining artificial intelligence with smart technology and the Internet of Things (IoT) will fundamentally alter how healthcare monitors and gauges Quality of Life (QoL). Like fitness trackers, smart watches, and health monitoring devices, wearable gear may compile real-time data on your heart rate, exercise level, sleep quality, and even stress level. IoT devices link portable technology to medical instruments and healthcare infrastructure, therefore facilitating even more possibilities. This allows one to constantly monitor the state of a patient. AI can make smart devices more valuable by analysing the data smart tech gathers and providing us with pertinent knowledge. Machine learning algorithms, for example, can examine real-time wearable’s data to identify trends indicating changes in a patient’s health, such as a decline in activity or a heart rate that varies nonlinearly. These revelations can help one evaluate a patient’s quality of life (QoL), identify probable medical issues early on, and provide tailored therapies meant to enhance outcomes in health. Using AI, smart tech, and the internet of things (IoT) in quality of life assessments is one of the nicest things about it since it allows you to constantly monitor patients instead of just checking in on them every so frequently. Particularly for those with long-term diseases or undergoing long-term therapy, this continuous monitoring can provide a more accurate and real-time picture of a patient’s health and quality of life.
RESULT AND DISCUSSION
Using AI-powered diagnostic tools in Quality of Life (QoL) evaluations results testing far more accurately and quickly. From electronic health records to patient surveys to real-time data from smart technology, artificial intelligence systems can examine several types of data. They do this by using machine learning techniques and natural language processing. These systems give constant, changing information about a patient’s mental and physical health, which lets doctors find health problems or falls early.
|
Table 2. Comparison of Evaluation Parameters: Traditional vs AI-Driven Methods |
||
|
Parameter |
Traditional Method |
AI-Driven Method |
|
Accuracy (%) |
78,5 |
92,3 |
|
Sensitivity (%) |
74,3 |
89,7 |
|
Specificity (%) |
82,1 |
94,5 |
|
Precision (%) |
76,4 |
91,2 |
|
Recall (%) |
73,9 |
88,3 |
Table 2 compares the rating factors of standard methods and methods that are driven by AI. This shows how far AI has come in improving Quality of Life (QoL) measures. When it comes to accuracy, AI-driven ways are much better than standard ones, going from 78,5 % to 92,3 %. Figure 3 shows the main differences between standard methods and AI-driven techniques by comparing success measures.
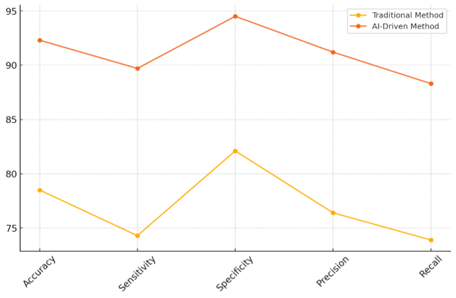
Figure 3. Performance Metrics Comparison Between Traditional and AI-Driven Methods
This rise shows that AI systems can better study and guess what will happen, which lowers the mistakes that come from human judgement and bias. Also, sensitivity, which is a measure of the true positive rate, goes from 74,3 % with old-fashioned ways to 89,7 % with AI-powered tools, which is a huge jump. Figure 4 shows how well standard methods and AI-driven techniques work by comparing success measures.

Figure 4. Comparison of Performance Metrics for Traditional vs. AI-Driven Methods
This means that AI is better at finding related health situations, which is important for getting help right away. On the other hand, precision, or the ability to correctly find false positives, also gets a lot better with AI, going from 82,1 % to 94,5 %. This shows that AI tools are better at telling the difference between people who need medical help and those who don’t, which lowers the number of fake alarms. Both precision and recall are getting better, which means that AI methods are better at finding relevant cases (precision) and remembering all of them (recall). Overall, these data show that AI-driven methods are more efficient and effective than standard methods at giving more accurate, fast, and reliable QoL ratings.
|
Table 3. Additional Evaluation Parameters: Traditional vs AI-Driven Methods |
||
|
Parameter |
Traditional Method |
AI-Driven Method |
|
F1 Score |
0,82 |
0,95 |
|
AUC Score |
0,85 |
0,97 |
|
Processing Time (s) |
120 |
35 |
|
Patient Satisfaction (%) |
74,5 |
89,4 |
|
QoL Improvement (%) |
21,3 |
45,2 |
In table 3, we compare more evaluation factors between traditional methods and methods that are driven by AI. This shows how AI can help with Quality of Life (QoL) assessments. The F1 score, which is a balance between accuracy and recall, shows a big improvement with AI. It went from 0,82 in traditional methods to 0,95 in methods that use AI. While reducing false positives and negatives, this improvement shows that AI tools are better at finding relevant cases and providing more reliable results. The AUC score, which shows how well the model can tell the difference between good and bad outcomes, also goes up a lot, from 0,85 to 0,97. Figure 5 shows how standard and AI-driven methods compare in terms of different success measures.
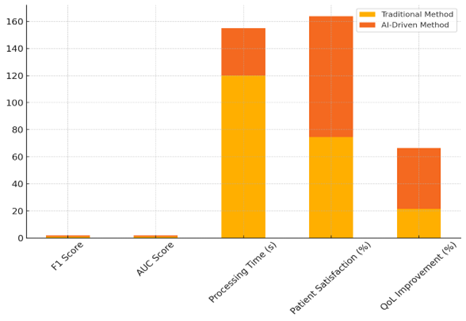
Figure 5. Comparative Contribution of Traditional and AI-Driven Methods Across Metrics
This shows that AI methods are better at predicting different patient conditions, which helps doctors make better decisions and help them faster. Processing time is also much faster with AI-driven methods; it goes from 120 seconds with standard methods to just 35 seconds. Figure 6 shows how AI-driven methods have a bigger effect than standard methods across all measures.

Figure 6. Incremental Impact of AI-Driven Methods Over Traditional Methods
This huge drop in the number of tasks makes AI tools more useful, as it speeds up evaluations and clinical decisions. AI-driven methods also lead to much better patient happiness and quality of life improvement. Patient satisfaction goes from 74,5 % to 89,4 %, and QoL improvement goes from 21,3 % to 45,2 %.
CONCLUSIONS
AI-powered testing tools might alter the measurement of Quality of Life (QoL) in the medical field. Using a range of data sources including electronic health records, smart devices, and patient-reported results AI systems provide a more consistent, continuous, and tailored approach to monitor a patient’s health. These instruments help one to recognise little changes in health, identify fresh issues before they become worse, and make better decisions on treatment and remedies. Using artificial intelligence is one of the nicest things about it as it allows one to monitor individuals in real time and present a whole picture of their condition. Using machine learning and natural language processing, AI systems may examine patient data from several angles that of social, mental, and physical, among others. This helps them to create better plans of action for every patient. Particularly for patients with long-term diseases or who are undergoing complex therapies, this continuous feedback mechanism guarantees that activities occur at the appropriate moment and that outcomes are better. AI-powered technologies allow care be proactive and start early by predicting issues or declines in quality of life. But there are problems with using AI-based testing tools, such as worries about data safety, the need to connect them to current healthcare systems, and the need for large datasets that make sure the models can be used in other situations and are correct. Making sure that data is safe and that rules like HIPAA and GDPR are followed is very important for keeping patients’ trust and privacy. Also, AI tools need to be easily integrated into healthcare processes so that there are no interruptions and professional decision-making is more efficient.
BIBLIOGRAPHIC REFERENCES
1. Veta, M.; van Diest, P.J.; Willems, S.M.; Wang, H.; Madabhushi, A.; Cruz-Roa, A.; Gonzalez, F.; Larsen, A.B.L.; Vestergaard, J.S.; Dahl, A.B.; et al. Assessment of algorithms for mitosis detection in breast cancer histopathology images. Med. Image Anal. 2015, 20, 237–248.
2. Vysokolan Corrales GA, Achucarro Galeano S. Perception of Nursing Postgraduate Students on the eLearning Model. Scientific Journal Care & Tech. 2023;1(1):53-79.
3. Swiderska-Chadaj, Z.; Pinckaers, H.; van Rijthoven, M.; Balkenhol, M.; Melnikova, M.; Geessink, O.; Manson, Q.; Sherman, M.; Polonia, A.; Parry, J.; et al. Learning to detect lymphocytes in immunohistochemistry with deep learning. Med. Image Anal. 2019, 58, 101547.
4. Mendieta Castro LF. Experience of type 2 diabetes patients in treatment adherence: a literature review. Scientific Journal Care & Tech. 2023;1(1):21-34
5. Bulten, W.; Pinckaers, H.; van Boven, H.; Vink, R.; de Bel, T.; van Ginneken, B.; van der Laak, J.; Hulsbergen-van de Kaa, C.; Litjens, G. Automated deep-learning system for Gleason grading of prostate cancer using biopsies: A diagnostic study. Lancet Oncol. 2020, 21, 233–241.
6. Negrete Escanor RA. Cardiovascular Risk Factors and Warning Signs. Scientific Journal Care & Tech. 2023;1(1):80-95.
7. Raciti, P.; Sue, J.; Ceballos, R.; Godrich, R.; Kunz, J.D.; Kapur, S.; Reuter, V.; Grady, L.; Kanan, C.; Klimstra, D.S. Novel artificial intelligence system increases the detection of prostate cancer in whole slide images of core needle biopsies. Mod. Pathol. 2020, 33, 2058–2066.
8. Guerrero Martines CM. Adherence of Chronic Renal Patients to their Hemodialysis Treatment. Scientific Journal Care & Tech. 2023;1(1):35-52.
9. Ch.V.L.L.Kusuma Kumari. (2015). Performance Appraisal: Dimensions and Determinants. International Journal on Research and Development - A Management Review, 4(3), 27 - 32.
10. Kompalli Sasi Kumar. (2015). Short Run and Long Run Performance of Indian Initial Public Offerings (IPOs) during 2007-2012. International Journal on Research and Development - A Management Review, 4(3), 33 - 41.
11. Van Dooijeweert, C.; van Diest, P.J.; Willems, S.M.; Kuijpers, C.C.H.J.; Overbeek, L.I.H.; Deckers, I.A.G. Significant inter- and intra-laboratory variation in grading of ductal carcinoma in situ of the breast: A nationwide study of 4901 patients in the Netherlands. Breast Cancer Res. Treat. 2019, 174, 479–488.
12. Candia Acosta MD, Jousson Ayala DA, Melgarejo Fretes RD. Epidemiological Characterization of Chikungunya Infection in Pediatric Patients, Pilar 2023. Scientific Journal Care & Tech. 2023; 1(1):9-20
13. Kuijpers, C.C.H.J.; Sluijter, C.E.; von der Thüsen, J.H.; Grünberg, K.; van Oijen, M.G.H.; van Diest, P.J.; Jiwa, M.; Nagtegaal, I.D.; Overbeek, L.I.H.; Willems, S.M. Interlaboratory variability in the grading of dysplasia in a nationwide cohort of colorectal adenomas. Histopathology 2016, 69, 187–197.
14. Kuijpers, C.C.H.J.; Sluijter, C.E.; von der Thüsen, J.H.; Grünberg, K.; van Oijen, M.G.H.; van Diest, P.J.; Jiwa, M.; Nagtegaal, I.D.; Overbeek, L.I.H.; Willems, S.M. Interlaboratory variability in the histologic grading of colorectal adenocarcinomas in a nationwide cohort. Am. J. Surg. Pathol. 2016, 40, 1100–1108.
15. Baeten, I.G.T.; Hoogendam, J.P.; Jonges, G.N.; Jürgenliemk-Schulz, I.M.; Braat, A.J.A.T.; van Diest, P.J.; Gerestein, G.; Zweemer, R.P. Value of routine cytokeratin immunohistochemistry in detecting low volume disease in cervical cancer. Gynecol. Oncol. 2022.
16. Epstein, J.I.; Egevad, L.; Humphrey, P.A.; Montironi, R. Best Practices Recommendations in the Application of Immunohistochemistry in the Prostate. Am. J. Surg. Pathol. 2014, 38, e6–e19.
17. Schnog, J.J.B.; Samson, M.J.; Gans, R.O.B.; Duits, A.J. An urgent call to raise the bar in oncology. Br. J. Cancer. 2021, 125, 1477–1485.
18. Yue, M.; Zhang, J.; Wang, X.; Yan, K.; Cai, L.; Tian, K.; Niu, S.; Han, X.; Yu, Y.; Huang, J.; et al. Can AI-assisted microscope facilitate breast HER2 interpretation? A multi-institutional ring study. Virchows Arch. 2021, 479, 443–449.
19. Polesie, S.; McKee, P.H.; Gardner, J.M.; Gillstedt, M.; Siarov, J.; Neittaanmäki, N.; Paoli, J. Attitudes Toward Artificial Intelligence Within Dermatopathology: An International Online Survey. Front. Med. 2020, 7, 1–9.
20. Forcier, M.B.; Gallois, H.; Mullan, S.; Joly, Y. Integrating artificial intelligence into health care through data access: Can the GDPR act as a beacon for policymakers? J. Law Biosci. 2019, 6, 317–335.
21. Sculley, D.; Holt, G.; Golovin, D.; Davydov, E.; Phillips, T.; Ebner, D.; Chaudhary, V.; Young, M.; Crespo, J.; Dennison, D. Hidden technical debt in machine learning systems. Adv. Neural Inf. Process. Syst. 2015, 28, 2503–2511.
FINANCING
None.
CONFLICT OF INTEREST
None.
AUTHORSHIP CONTRIBUTION
Conceptualization: Deepika Sharma, Sudhansu Sekhar Patra, Sujayaraj Samuel Jayakumar, Vasant Devkar.
Data curation: Deepika Sharma, Sudhansu Sekhar Patra, Sujayaraj Samuel Jayakumar, Vasant Devkar.
Formal analysis: Deepika Sharma, Sudhansu Sekhar Patra, Sujayaraj Samuel Jayakumar, Vasant Devkar.
Drafting - original draft: Deepika Sharma, Sudhansu Sekhar Patra, Sujayaraj Samuel Jayakumar, Vasant Devkar.
Writing - proofreading and editing: Deepika Sharma, Sudhansu Sekhar Patra, Sujayaraj Samuel Jayakumar, Vasant Devkar.