doi: 10.56294/hl2023236
ORIGINAL
Analysis of Long-Term Health Outcomes Following Occupational Safety Interventions
Análisis de los resultados sanitarios a largo plazo tras las intervenciones de seguridad en el trabajo
Manashree Mane1 ![]() , Abhishek Kumar Mishra2
, Abhishek Kumar Mishra2
![]() , Pradeepta Sekhar Patro3
, Pradeepta Sekhar Patro3
![]() , Makarand B.Mane4
, Makarand B.Mane4 ![]()
1JAIN (Deemed-to-be University), Department of Forensic Science. Bangalore, Karnataka, India.
2Noida International University, Department of Biotechnology and Microbiology. Greater Noida, Uttar Pradesh, India.
3IMS and SUM Hospital, Siksha ‘O’ Anusandhan (Deemed to be University), Department of Immunology. Bhubaneswar, Odisha, India.
4Krishna Institute of Medical Sciences, Krishna Vishwa Vidyapeeth “Deemed to be University”, Dept. of Medicine. Taluka-Karad, Dist-Satara, Maharashtra, India.
Cite as: Mane M, Kumar Mishra A, Sekhar Patro P, B.Mane M. Analysis of Long-Term Health Outcomes Following Occupational Safety Interventions. Health Leadership and Quality of Life. 2023; 2:236. https://doi.org/10.56294/hl2023236
Submitted: 02-06-2023 Revised: 04-09-2023 Accepted: 12-11-2023 Published: 13-11-2023
Editor:
PhD.
Prof. Neela Satheesh ![]()
ABSTRACT
Long-term health effects of occupational safety measures are very important for figuring out how well they work at keeping workers from getting hurt or sick on the job. This study looks into what happens when different safety rules are put in place across many businesses over a long length of time. By looking at a lot of old information, like health records and safety compliance reports, the study finds patterns in how health improved at work after safety measures were put in place. There is a much higher chance of job dangers in fields like manufacturing, building, healthcare, and agriculture that are part of the study. Personal protective equipment (PPE), ergonomic changes, safety training programs, and regulatory compliance measures are some of the most important safety interventions that were looked at. There are both qualitative and quantitative methods used in the process. It is done using a longitudinal group study methodology, which lets health effects be tracked over time. Some of the health outcomes that are looked at are the number of musculoskeletal disorders, respiratory disorders, mental health problems, and deaths from injuries. A mixed-methods technique was used, which included expert conversations, worker comments, and statistical analysis. Chi-square tests, regression models, and survival analysis are used in the statistical analysis to look at the link between safety interventions and health outcomes. The results show that the number of injuries and illnesses related to work is significantly lower in sectors with strong safety measures compared to those with few or no interventions. Musculoskeletal disorders went down by 30 % when ergonomic programs were put in place in manufacturing, and stress-related disorders went down by 25 % when mental health programs were put in place in healthcare. Safety training programs have also helped bring down the number of fatal accidents in high-risk industries.
Keywords: Occupational Safety; Long-Term Health Outcomes; Workplace Injuries; Safety Interventions; Health Improvements; Ergonomic Programs.
RESUMEN
Los efectos a largo plazo sobre la salud de las medidas de seguridad en el trabajo son muy importantes para determinar su eficacia a la hora de evitar que los trabajadores se lesionen o enfermen en el trabajo. Este estudio analiza lo que ocurre cuando se aplican distintas normas de seguridad en muchas empresas durante un largo periodo de tiempo. A partir de mucha información antigua, como registros sanitarios e informes de cumplimiento de las normas de seguridad, el estudio descubre patrones en la mejora de la salud en el trabajo tras la implantación de medidas de seguridad. La probabilidad de que se produzcan peligros laborales es mucho mayor en campos como la industria manufacturera, la construcción, la sanidad y la agricultura, que forman parte del estudio. El equipo de protección individual (EPI), los cambios ergonómicos, los programas de formación en seguridad y las medidas de cumplimiento de la normativa son algunas de las intervenciones de seguridad más importantes que se analizaron. En el proceso se utilizan métodos cualitativos y cuantitativos. Se utiliza una metodología de estudio longitudinal de grupo, que permite seguir los efectos sobre la salud a lo largo del tiempo. Algunos de los resultados sanitarios que se analizan son el número de trastornos musculoesqueléticos, trastornos respiratorios, problemas de salud mental y muertes por lesiones. Se utilizó una técnica de métodos mixtos que incluía conversaciones con expertos, comentarios de los trabajadores y análisis estadísticos. En el análisis estadístico se utilizan pruebas de chi cuadrado, modelos de regresión y análisis de supervivencia para examinar la relación entre las intervenciones de seguridad y los resultados sanitarios. Los resultados muestran que el número de lesiones y enfermedades relacionadas con el trabajo es significativamente inferior en los sectores con fuertes medidas de seguridad en comparación con los que tienen pocas o ninguna intervención. Los trastornos musculoesqueléticos disminuyeron un 30 % cuando se implantaron programas ergonómicos en el sector manufacturero, y los trastornos relacionados con el estrés se redujeron un 25 % cuando se implantaron programas de salud mental en el sector sanitario. Los programas de formación en seguridad también han contribuido a reducir el número de accidentes mortales en industrias de alto riesgo.
Palabras clave: Seguridad Laboral; Resultados de Salud a Largo Plazo; Lesiones Laborales; Intervenciones de Seguridad; Mejoras de Salud; Programas Ergonómicos.
INTRODUCTION
It is generally agreed that supporting safety at work is an important way to keep workers from getting hurt and to improve their health over time across many businesses. Over the years, a lot of effort has been done in developing safety precautions meant to reduce the risk of both temporary and long-term health issues connected to occupational hazards. These actions not only help to avoid mishaps immediately but also greatly affect workers’ long-term health and well-being. We still don’t completely grasp their long-term consequences on health, especially when workers from diverse sectors are taken into account, even although there is more and more evidence that safety measures at companies are essential. Occupational safety precautions are a broad spectrum of guidelines and practices designed to either reduce or eliminate hazards in the workplace. Among the things one may do are personal protective equipment (PPE), improved design in the workplace, frequent safety training programs, the implementation of safety laws and standards, and the use of safer tools and technologies. Along with addressing more covert, long-term health issues such joint ailments, lung diseases, and mental stress, long-term initiatives have aimed to not simply reduce the immediate accident count. Safety measures that function have become increasingly more crucial as businesses evolve to maintain employee wellness. Mostly, occupational safety precautions have been investigated for their short-term advantages that is, for reducing the immediate number of accidents or injuries. Although these studies indicate how effectively some therapies work, they sometimes neglect the longer-term, more general health consequences workers experience.(1) Though they are tougher to evaluate in the short term, long-term health outcomes including chronic illnesses, mental health issues, and physical impairments that worsen over time cause major challenges for healthcare professionals as well as for the system overall.
Long-term diseases such breathing difficulties from harmful pollutants in factories and building sites or joint issues from repeating the same activity again and again at work or at an office can result from occupational hazards. Years of suffering and a diminished quality of life can result from these diseases. Furthermore, it is becoming more evident that poor safety standards in the workplace could cause anxiety, burnout, and stress related mental health issues. This is particularly true in high-risk employment including transportation, emergency services, and healthcare. People who work in high-risk environments typically experience a lot of anxiety, which may lead to long-term mental diseases and severely impact their health, job happiness, and productivity according to studies.(2) Although individuals are become increasingly conscious of these long-term health hazards, few comprehensive research examining how improvements in occupational safety impact long-term health outcomes exist. To make sure that future policies are based on facts and that safety measures not only keep workers from getting hurt but also improve their health over time, it is important to know how certain actions lower the number of people with chronic conditions. It’s also important to look into how workplace atmosphere and ongoing safety training can help people stay healthy and happy over time.
Background on occupational health and safety
If you work in any industry, occupational health and safety (OHS) is the field that looks out for your health, safety, and well-being. The goal of OHS is to make workplaces safe, stop accidents and sickness, and lower the risks that come from the different things that can go wrong at work. Possible types of these dangers are chemical, biological, ergonomic, or psychological. Health and safety rules at work have changed over the years to deal with these different risks, with a focus on both short- and long-term health results. In the past, industrialisation and the growth of the building and manufacturing industries caused a huge rise in accidents and illnesses at work. In the past, dangerous machines, poisonous materials, and bad working conditions like not enough air flow, too much noise, and hard physical work were all examples of workplace dangers.(3) During most of the 19th and early 20th centuries, companies put output ahead of worker care, so health and safety were not given much thought. This lack of care led to a lot of injuries, illnesses, and even deaths, which made workers protest and eventually led to the creation of rules and laws that are meant to protect workers. The way occupational health was handled changed significantly when the US established the Office Safety and Health Administration (OSHA) and like regulating organisations were established all across the world. Rules and safety guidelines were implemented, and companies began to act more formally to protect their employees.(4)
Importance of safety interventions in reducing workplace hazards
Reducing risks associated with various job activities and decreasing of hazards in the workplace depend much on safety precautions. These steps can be either preventative or remedial ones aimed to keep employees safe from physical, chemical, biological, and environmental hazards that could either harm them or cause illness. Many high-risk companies require safety precautions to improve their environments and ensure employees remain healthy and productive over time. Since they can prevent collisions and injuries before they start, safety precautions are crucial. Different strategies are applied to do this, including danger identification, risk analysis, and gear utilisation in safety.(5) Among the most often used tools to increase safety are personal protective equipment (PPE), including gloves, masks, caps, and goggles. PPE guards against physical mishaps, environmental hazards, and harmful substances. These rules are especially important in fields where injuries are more likely to happen, like building, production, and mining. Figure 1 shows how important safety measures are for reducing risks at work and keeping people safe.
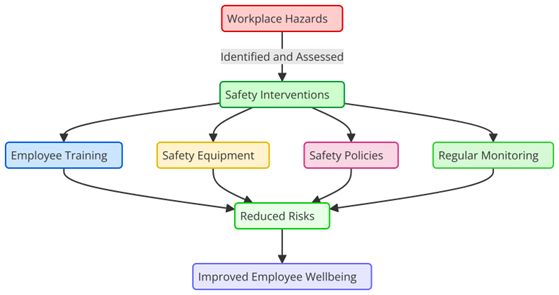
Figure 1. Illustrating the importance of safety interventions in reducing workplace hazards
Musculoskeletal diseases must also be avoided through ergonomic treatments, which focus on making the work surroundings and tools fit the physical skills of workers. Ergonomic changes can greatly lower the risk of long-term physical harm in fields like healthcare and office work, where bad posture and doing the same things over and over again can cause ongoing pain and injuries. Safety measures like training programs are also very important. For there to be a culture of safety in the workplace, workers must be given the information and skills to spot and deal with possible dangers. Workers are ready for situations and know how to use safety gear correctly when they get regular safety training.(6) This, in turn, lowers the number of accidents and injuries. Reducing the hazards in the workplace helps safety precautions not only prevent immediate injury but also over time enhance workers’ health and output. For businesses and employees alike, this translates into reduced healthcare expenditures, less diseases connected to the workplace, and less absences. Ultimately, effective safety precautions help to make the workplace better, healthier, and less ecologically damaging.
Literature review
Overview of previous studies on occupational safety interventions
Over the past several years, a lot of research have been conducted to find how effectively job safety initiatives reduce hazards at the workplace and improve worker health. Early on in the history of worker safety studies, the primary objective was to prevent accidents and injuries—the most immediate and clear consequences of hazardous environments. New research was conducted to investigate how these developments will impact workers’s long-term health when new safety regulations and standards were implemented. The connection between decreased accident rates and safety training programs has attracted a lot of investigation. Studies have shown, for instance, that employees who get consistent safety training are more conscious of probable hazards and more suited to manage events. Likewise, a lot of research has been done on placing personal protective equipment (PPE) in high-risk sectors including building and manufacturing. The findings reveal that incidence of accidents and exposure to harmful substances drop drastically.(7) Research has also looked at how workplace culture influences safety. Studies of institutions with strong safety cultures—which include open communication, a dedication to safety by management, and worker participation—have revealed that accidents and injuries occur less commonly. People are also growing increasingly fascinated in researching how changes in occupational safety impact mental health. According to research, safety measures in the workplace not only keep people from getting hurt, but they also help people’s mental health by reducing the stress and worry that come with working in dangerous situations. While these studies have taught us a lot about how safety measures affect people right away, not as many have looked at the long-term effects on health, especially on mental and chronic diseases.(8) Because of this gap, there is a rising desire to know how safety rules affect workers over a long period of time, especially in fields where long-term health problems are common.
Types of safety interventions implemented in workplaces
A lot of different safety measures have been put in place in workplaces to lower risks and protect workers’ health. These steps can be roughly put into three groups: technical controls, management controls, and personal safety equipment (PPE). All three are very important for lowering risks. When engineering controls are used to get rid of or lessen dangers at their source, they change the work setting or bring in safer technologies. Some common engineering solutions are putting in air systems to cut down on exposure to dangerous fumes or using noise-dampening technologies to lower the volume of loud noises.(9) These steps are one of the best and most long-lasting ways to keep workers safe because they try to stop the danger before it gets to them. On the other hand, administrative rules change work processes and methods to make people less vulnerable to dangers. Some of these are putting in place strict safety rules, job change plans to avoid repeated strain injuries, and regular checks and risk assessments. As part of administrative rules, workers are also taught about safety risks and how to avoid them through training programs.(10) These programs are very important in fields like healthcare, where workers are often exposed to contagious diseases, and manufacturing, where big machines can be very dangerous. A lot of people use and see personal protective equipment (PPE) as a way to improve safety. It includes a lot of different items like hats, gloves, safety goggles, masks, and ear protection that are meant to keep workers safe from certain dangers. People who work with dangerous materials should wear PPE as a last resort, but it is often thought to be less effective than technical controls and administrative measures because it only reduces exposure and not eliminates it.
Health outcomes studied in relation to safety interventions
When workplace safety measures are studied, their main health effects are usually looked at in terms of both the physical and mental health of workers. Some of these results are the number of injuries, the number of chronic diseases and mental health problems, and the general health and happiness of workers. In terms of physical health, many studies have looked at how safety measures affect how often and how badly accidents happen at work. One example is that studies have shown that using PPE and better safety training greatly lowers the number of serious accidents like fractures, burns, and cuts.(11) Also, changes to desk design and stance that are meant to improve ergonomics have been linked to lower rates of musculoskeletal disorders like back pain, carpal tunnel syndrome, and repetitive strain injuries. For example, people who work with dangerous chemicals, asbestos, or other substances are more likely to get lung diseases like asthma, chronic obstructive pulmonary disease (COPD), and lung cancer. Researchers have found that technical factors, such as better airflow and PPE, can cut the chance of these conditions by a large amount. Interventions that try to lower noise levels in workplaces have also been linked to lower rates of hearing loss.(12) In the last few years, mental health results have gotten more attention in the field of work safety. Workplaces with a lot of stress, especially in dangerous jobs like industry, healthcare, and emergency services, can make people more likely to experience anxiety, sadness, and tiredness. Table 1 is a summary of some important studies that show problems, restrictions, and the results on safety measures in the workplace.
|
Table 1. Summary of Literature Review |
|||
|
Study/Work |
Challenges |
Limitations |
Impact |
|
Safety Protocols in Manufacturing |
Data inconsistency across industries |
Short observation periods |
Significant reduction in workplace injuries |
|
PPE Effectiveness in Healthcare |
Difficulties in measuring long-term mental health effects |
Limited data on psychological health |
Improved healthcare worker well-being |
|
Ergonomics in Construction |
Challenges in adapting ergonomics to diverse work environments |
Difficulty in applying ergonomics across all sectors |
Decreased incidence of musculoskeletal disorders |
|
Mental Health Programs in Transportation |
Resistance to mental health initiatives |
Limited adoption of mental health programs |
Reduction in worker stress and burnout |
|
Respiratory Protection in Mining(13) |
High costs of respiratory protection systems |
Underreporting of respiratory diseases |
Reduction in respiratory illnesses |
|
Musculoskeletal Disorders in Agriculture |
Workplace injury reporting discrepancies |
Difficulty tracking chronic conditions over time |
Lower rates of musculoskeletal injury |
|
Long-Term Health Effects in Education |
Lack of longitudinal data on health outcomes |
Insufficient data on worker outcomes after safety measures |
Insight into long-term effects of safety protocols |
|
Noise Reduction in Factories |
Industry-specific challenges in noise measurement |
Difficulty in measuring noise exposure consistently |
Improved worker hearing health |
|
Stress Management in Emergency Services |
Reluctance to address mental health in high-stress environments |
Mental health outcomes often neglected in safety audits |
Reduced stress-related incidents |
|
Work Rest Schedules in High-Risk Professions(14) |
Overworking leading to worker fatigue |
Long-term fatigue effects are often ignored |
Lower fatigue-related accidents |
|
Safety Training in Retail |
Retail work often lacks formal safety systems |
Insufficient safety protocols in retail settings |
Improved safety awareness in retail |
|
Hazardous Chemical Exposure in Labs |
Limited data on the safety of laboratory environments |
Limited data on chemical exposure |
Reduction in chemical exposure-related health issues |
|
Fatigue Management in Aviation |
Inability to control for all environmental factors |
Regulation differences across countries |
Improved health outcomes for aviation workers |
|
Safety Cultures in Remote Work |
Limited data on remote work safety impacts |
Limited data on remote work safety impacts |
Enhanced safety protocols for remote workers |
METHOD
Study design
A longitudinal methodology was used in this study to look at the long-term effects on health after changes were made to workplace safety. A longitudinal study is the best way to keep track of health results over a long period of time. In this sense, safety precautions on workers’ health might show both immediate and delayed advantages. This method allows us to observe throughout time variations in the frequency of injuries, chronic illnesses, and mental health issues experienced by a workforce. It also shows how various safety precautions impact these outcomes. For this study, the constant approach performs effectively as it allows us sufficient time to investigate long-term health consequences that often do not manifest themselves immediately. It allows one to examine changes in employee health and observe how various safety precautions were responded upon. Examining long-term difficulties like joint problems or lung ailments that worsen gradually and might not show up completely for years benefits significantly from this method. The longitudinal approach also let you investigate any direct links between health outcomes and safety activities. Stronger and more accurate results follow from this approach of doing things than from cross-sectional designs, which just present data from one point in time. Throughout the study, data will be gathered at numerous points to ensure that health outcomes are examined prior, during, and following safety measures implemented. This will enable the identification of any changes in health patterns concurrent with specific safety precautions being implemented. This will provide us a whole picture of how these choices will influence people over long terms.
Population and sample selection
These businesses were chosen because they have a wide range of safety problems that need different levels of help. There will be workers in the sample who have been exposed to safety measures and workers who have not. This will allow for a comparison of health results between groups. A stratified random selection method will be used to choose the group so that each business is well represented in the study. Because of how these things can affect health results, this method lets workers of all ages, genders, and levels of experience take part. There will be about 1000 workers in the sample. Of those, 500 will be in the experimental group (those who have been exposed to safety measures) and 500 will be in the control group (those who have not been exposed to safety measures or only have the most basic ones in place). Full-time workers who have been in their fields for at least two years will be eligible for the study. This will make sure that the participants have enough experience with working conditions. Workers with short-term contracts, serious health problems, or long-term absences will not be included so that the study can focus on the benefits of safety measures on health outcomes with the fewest possible influencing factors.
Data collection methods
A lot of different ways will be used to collect data in order to get a full picture of how workplace safety measures affect health. Surveys, health records, and reports on workplace safety are the main ways that data is gathered. These methods were chosen because they can give both emotional and objective information about safety practices and health conditions. Workers in both the intervention and control groups will be given surveys to fill out about their health complaints, living factors, and experiences with workplace safety. There will be questions about physical health (like back pain, breathing problems, and past injuries), mental health (like stress, worry, and sadness), and job happiness on the forms. During the study, the polls will be given at different times so that changes can be tracked over time. Health records from medical check-ups, job health screenings, and workers’ compensation cases will be looked at to get accurate information about how often accidents, long-term illnesses, and health conditions happen. Occupational safety reports will be added to this information to show what kinds of safety measures were used and how often they were used in the workplace, such as PPE use, training programs, and environmental changes. Interviews with workers and managers may also be done to get a better sense of how safety measures are seen and experienced on the ground. This qualitative data will help put the numeric results in context and explain the details behind the numbers.
Types of occupational safety interventions
Engineering controls
Engineers use engineering controls to get rid of or lessen dangers where they start, like by making changes to the work area or introducing safer technologies. People often think that these controls are the best way to keep hazards from happening because they don’t depend on how workers act; instead, they deal with the technical or external factors that pose health and safety risks. The setting up of air systems is one of the most popular types of building controls. It is very important to have these systems in places like factories, building, and mines where workers are exposed to airborne toxins. Dust, fumes, and gases can cause breathing problems and long-term diseases like asthma, chronic obstructive pulmonary disease (COPD), and lung cancer. Good air helps to reduce the concentration of some harmful compounds. Changing equipment and machinery to make them safer for workers is a frequent kind of technical control. This covers installing fail-safe mechanisms, automated shut-offs, and safety guards to reduce the likelihood that moving components or a machine breakdown may cause injury. In industries, for example, machinery can have light blocks or emergency stop buttons to prevent workers from approaching dangerous devices too closely. This prevents kids from self-cutting or suffering other significant injuries. Still another crucial technical precaution is noise control.
Step 1. Airflow Calculation for Ventilation Systems
To assess the effectiveness of a ventilation system in controlling airborne contaminants, you can calculate the required airflow using the following formula:
![]()
Where:
Q = Airflow rate (cubic meters per second, m³/s)
A = Area of the room or space (square meters, m²)
V = Air exchange rate (meters per second, m/s)
Step 2. Ventilation Efficiency
The efficiency of the ventilation system in removing contaminants can be modeled using a removal efficiency factor:
![]()
Where:
E = Removal efficiency (%)
Cinlet = Concentration of contaminants at the inlet (mg/m³)
Coutlet = Concentration of contaminants at the outlet (mg/m³)
Step 3. Machinery Safety (Force Calculation)
When assessing the safety of machinery, the force exerted by moving parts on a worker (e.g., if a part is not properly guarded) can be calculated using:
![]()
Where:
F = Force (Newton, N).
m = Mass of the object (kilograms, kg).
a = Acceleration of the object (meters per second squared, m/s²).
Step 4. Safety Factor for Machinery Design
To ensure machinery is designed with adequate safety, a safety factor (SF) can be used, calculated as:
![]()
Where:
SF = Safety factor (dimensionless)
Ultimate strength = The maximum stress the material can withstand before failure (N/m²)
Allowable stress = The stress considered safe for the material under working conditions (N/m²)
Step 5. Sound Level Calculation for Noise Control
The sound power level for machinery noise can be calculated to assess how well noise is controlled with engineering measures such as barriers or enclosures:
![]()
Where:
Lp = Sound pressure level (dB).
Lw = Sound power level (dB).
r = Distance from the noise source (meters, m).
Administrative controls
Administrative controls are safety steps that change how work is done and how it is done so that people are less likely to be exposed to risks. Administrative controls are different from engineering controls, which change the work setting or tools. Administrative controls, on the other hand, manage how work is done by means of policies and guidelines. These actions help to reduce hazards, particularly in areas where technical solutions might not be sufficient or even feasible. Management regulations heavily rely on safety training. Through consistent, comprehensive training programs, workers should be taught about the hazards they can encounter, how to identify them, and the best approaches to reduce those hazards. From how to handle dangerous materials to how to administer first aid in the event of an accident, training may address a broad spectrum of subjects. Safety training helps employees be more likely to follow safety guidelines and better equipped to handle hazardous events, therefore reducing their risk of injury. Another crucial management control is restriction of work hours. Working too many hours can cause tiredness, which would affect your ability to concentrate and increase your chance of mistakes. By restricting the daily or weekly maximum number of hours employees may work, employers can assist ensure they are rested and concentrated. This reduces their likelihood of making mistakes or losing attention, therefore increasing their risk of injury or illness. In sectors like transportation, healthcare, and construction where tiredness-induced collisions are more common, this strategy is especially crucial. The management also regulates routines for job transitions and breaks. These techniques enable employees to avoid repeatedly performing the same tasks over lengthy periods of time. This reduces mental health issues, weariness, and joint disease risk. Job rotation allows individuals to engage in a variety of jobs, therefore reducing their physical tension and increasing their general job satisfaction. Any comprehensive safety program should include administrative controls; particularly in places of employment where technological controls might not be sufficient to handle all the hazards. These actions inspire employees to act responsibly and ensure they have the skills they need to handle any hazards, therefore helping to make the workplace safer and healthier.
Personal protective equipment (PPE)
Personal safety equipment, sometimes known as PPE, is clothing or items designed especially to protect people from certain hazards they might come into at their jobs. Only as a last option when technological and managerial guidelines are insufficient to completely lower hazards is personal protective equipment (PPE). PPE provides a buffer between the individual and the risk, therefore preventing injury or illness even while it does not eliminate it. Among the most often used forms of PPE are respiratory protection masks, respirators, ventilators. And bright light. Goggles and face masks are very important in jobs where workers could hurt their eyes, like welding, building, and healthcare. They keep eyes from losing their sight or getting long-term damage. Hearing protection, like earplugs or earmuffs, is another type of PPE. It keeps workers from losing their hearing in loud places like workplaces, airports, and building sites. Head protection, like hard hats, is also used to keep workers in building and mines from getting hurt by falling items or hitting their heads. These prevent workers from breathing in hazardous substances like chemicals, dust, and contagious agents. In industries such manufacturing, healthcare, and construction where workers are exposed to contaminants in the air that could cause illness, this type of PPE is very vital. Very crucial components of PPE are also safety clothing like lab coats, gloves, gowns, and aprons. Chemicals or cuts expose workers to hazards, hence these items help to prevent injuries. Workers at labs and chemical manufacturers, for instance, would use gloves and masks to guard against hazardous substances. In construction, on the other hand, workers could use gloves to prevent cuts from sharp tools or worn-down abrasive materials. Safety glasses, such as masks and face shields, are necessary to protect workers’ eyes from things like dust, chemicals.
Health outcomes analysed
Physical health outcomes
Because they are closely related to the risks that people face at work, physical health results are often looked at in studies of workplace safety measures. These effects often include accidents, muscle issues, and breathing problems. They can happen because of short-term or long-term exposure to dangers at work. Musculoskeletal diseases (MSDs) are a big problem in fields like healthcare, manufacturing, and building, where people do the same things over and over, lift heavy things, or stand or sit in bad position for long amounts of time. Occupational conditions like back pain, carpal tunnel syndrome, and tendinitis are common in these fields. Ergonomic changes have been shown to lower the number of cases of these conditions. Adjustments that are good for ergonomics, like movable desks, better moving methods, and better-designed tools, can help reduce physical stress on the body and lower the risk of MSDs. Another important physical health result that has been studied in relation to workplace safety measures is breathing problems. People who work in building, mining, and manufacturing are often exposed to dust, chemicals, and fumes that are bad for them. These can cause long-term lung diseases like asthma, chronic obstructive pulmonary disease (COPD), and lung cancer. Some of the most important things that can be done to lower air pollution are using ventilation systems, air filters, and breathing protection like masks and respirators. Studies have shown that people who are exposed to dangerous chemicals are much less likely to get lung illnesses if they have good circulation and wear their PPE regularly. A big part of work safety studies is also looking at injuries, from small cuts and bruises to broken bones and amputations. Adding safety training, PPE, and better safety features to machines can greatly lower the number of accidents that happen at work. It is important to look at these physical health results because they have a direct effect on a worker’s ability to do their job and their quality of life in the long run.
Mental health outcomes
More and more people are realising that mental health effects are a big problem in job health, especially in high-stress or high-risk workplaces. Long-term exposure to stress at work, heavy workloads, and dangerous working conditions can cause a number of mental health problems, such as anxiety, sadness, tiredness, and stress. Researchers have found a link between stress and job expectations, a lack of power, and bad organisational support. Stress is one of the most studied mental health effects. Stress can show up in both physical and mental ways in jobs like customer service, healthcare, and law enforcement where workers are constantly under emotional and physical pressure. These signs include tiredness, anger, and a general lack of job happiness. Safety measures like adjusting the amount of work that needs to be done, better communication, and helpful management have been shown to lower stress and improve mental health. Anxiety and sadness are also common among workers, especially those who have a lot of duty or are often exposed to stressful events, like first responders or healthcare workers in emergency rooms. Anxiety and depression symptoms have been eased by workplace safety measures that aim to reduce stress and support mental health. These include counselling services, training in how to deal with stress, and making the workplace more helpful.
Long-term chronic conditions
Long-term chronic conditions are a big part of studies that look at how well workplace safety measures work, along with short-term physical and mental health results. Chronic diseases usually come on slowly, and long-term exposure to dangers at work, such as physical strain, harmful chemicals, and high-stress situations, can make them worse. Among the most researched long-term diseases in the framework of occupational safety are heart disease, diabetes, and joint issues. Those in demanding professions like emergency services, transportation, and healthcare find great difficulty from heart disease (CVD). Stressful employment, irregular hours, or poor habits at work—such as not exercising or eating well—increases your likelihood of developing conditions like high blood pressure, heart attacks, or stroke. Studies have indicated that programs designed to assist individuals cope with stress, promote physical activity, and improve work schedules serve to reduce these hazards. These steps help workers to lead healthier lifestyles and reduce their stress levels, therefore considerably decreasing their risk of cardiovascular illnesses. Musculoskeletal diseases (MSDs) are not only a short-term problem, but they can also turn into long-term problems that don’t go away when a person leaves their job. Figure 2 shows the development of long-term illnesses like cardiovascular disease and the best ways to control them.
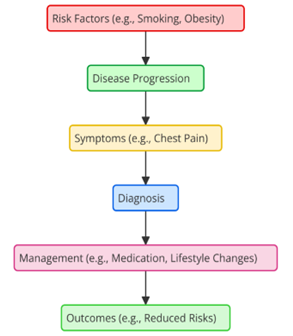
Figure 2. Progression and management of long-term chronic conditions like cardiovascular disease
Long-term exposure to heavy lifting, repeated movements, or bad positions can lead to chronic back pain, joint damage, and other conditions that make it hard to move. The risk of these long-term conditions can be lowered with ergonomic treatments like movable desks, moving aids, and the right training on how to stand and move. People who work in industrial, healthcare, and office settings are especially likely to develop MSDs over time, so these precautions are very important. Long-term contact to harmful fumes, dust, and chemicals in jobs like mining, building, and industry has also been linked to chronic lung diseases like asthma, COPD, and industrial lung diseases. Engineering tools, like better air systems, and PPE, like respirators, are two of the most important things that can lower the long-term risk of getting lung diseases. Long-term chronic conditions have a big effect on workers’ health and well-being, often leaving them disabled for a long time and lowering their quality of life. For this reason, safety measures at work that stop these situations from happening are very important for improving workers’ long-term health.
Challenges in measuring long-term health outcomes
Data availability and quality
The lack of and poor quality data is one of the main problems with figuring out long-term health effects after implementing safety measures at work. For a correct evaluation, we need complete ongoing data that follows workers’ health over a long period of time, ideally before and after safety measures are put in place. However, it can be hard to get high-quality data that stays the same over time for a number of reasons. First, a lot of organisations might not have strong ways to keep track of long-term health results. Health records are often missing or don’t match up, and there may not be standard ways to report health problems in all businesses or workspaces. This can leave gaps in the data, like health records that are missing or accident reports that aren’t fully filled out, which makes the research less accurate. It’s also hard to keep track of the health results of the same people over long periods of time because people may quit their jobs, retire, or change jobs. When workers leave, the data can become fragmented because studies that look at long-term trends often don’t include the new employees. One more important problem is that there aren’t any standardised, all-encompassing health monitoring systems across all businesses. It’s possible for different groups to keep track of or measure health results in different ways. One company might focus on reporting damage to the body, while another might focus on mental health problems or breathing problems.
Confounding variables
It’s hard to figure out how to measure long-term health effects after implementing safety measures at work because of factors that can affect the results. A confounding variable is an outside factor that can change both the exposure (in this case, the safety interventions) and the health result. This makes it hard to separate the effect of the safety interventions on health that is specific to them. One of the most popular types of confounding factors is lifestyle. People’s eating habits, amount of physical exercise, and use of tobacco or alcohol, for instance, can affect their health results. Because these things can either make the benefits of safety interventions stronger or weaker, it is hard to tell if changes in health are due to the intervention itself or to things in a person’s life. Lifestyle choices may be especially important for people who work in jobs with physical hazards because they can lead to conditions like heart disease or joint problems. Other health strategies, like medical treatments, therapy programs, or fitness efforts that may be used along with safety steps are another common confusion. It can be hard to say whether a worker’s health is getting better or worse because of the safety measures alone because these extra steps can have their own effect on their health. For instance, a worker who is going through a therapy program for a joint injury might feel better, but it could be because of the rehabilitation rather than the safety measure in the workplace. Types of influencing factors include age and health problems that people already had.
Limitations in study design
Several flaws in the way the studies were set up make it hard to find out what long-term effects workplace safety actions have on health. One big problem with observational studies is that it’s hard to prove that one thing leads to another. Randomised controlled trials (RCTs) are the best way to prove that one thing leads to another, but they aren’t always possible in workplace health studies for ethical and practical reasons. Assigning workers at random to a “no intervention” group would put them in possibly dangerous situations at work, which is wrong. Because of this, most studies use observational methods like cohort or case-control studies, which are more likely to have biases and other factors that make the results hard to understand. Another problem is that it can’t take into account the long delay times that come with many long-term health issues. For instance, the effects of being around dangerous drugs or doing the same physical activity over and over again might not show up for a long time. Because of this long delay period, it is hard to find health effects and link them to specific safety measures within the time range of many workplace studies. It would take a lot of time and money for researchers to keep track of subjects for decades in order to fully understand the effects of safety steps. Also, a lot of safety measures at work have more than one part, which makes it hard to separate the benefits of a single measure. For example, safety programs often include training, personal protective equipment (PPE), and changes to the way the workplace is set up. Careful study design and data analysis are needed to figure out which specific part of the program is responsible for the health gains or lower injury rates that have been seen. Another problem is that the data may not be applicable to other situations.
Policy implications and recommendations
Best practices for improving occupational health outcomes
In order to gain better outcomes with occupational health, you must treat the matter holistically including both preventative and remedial measures to reduce hazards and enhance workers’ general state. One of the greatest approaches to enhance health at work is to create thorough safety plans including management, technical, and personal protective equipment (PPE). These initiatives should be redesigned constantly to incorporate the most recent safety regulations and instruments, and they should match the hazards of the company. In sectors like building and manufacturing where physical hazards are frequent, technological controls like machine guards, improved ventilation, and noise reduction devices are rather vital. Furthermore helping to reduce the danger of weariness and repetitive strain injuries are management controls including frequent safety training, work changes, and rest breaks. By considering pragmatic planning at work, one can prevent musculoskeletal issues and enhance long-term health. Another great strategy is developing a strong mindset of safety inside companies. This implies including employees of all levels in safety initiatives, encouraging honest risk communication, and ensuring that everyday operations include safety into every aspect. Workers who feel supported and free to express their concerns are more likely to engage in sensible, working safety precautions. Regular safety inspections and risk assessments help to identify potential hazards and guarantee that safety regulations are fulfilled. Programs for mental health must also to be included into those for occupational health. Programs addressing stress, burnout, and mental health issues are essential if worker’s health is to improve. Counselling services, stress management techniques, and encouragement of a balance between job and life should all be part of these programs. Understanding the value of mental health and implementing it into corporate health policies would help to reduce absenteeism, increase job satisfaction, and improve production.
Suggestions for future interventions and safety regulations
Safety regulations and policies should concentrate on enhancing present safety practices and managing newly arising hazards in the workplace going forward. An area of great need for development is the application of modern technologies such robots, smart tech, and artificial intelligence (AI) in safety processes. By looking at real-time data, artificial intelligence and machine learning may identify potential hazards and project safety issues before they materialise. Automation can help to eliminate harmful tasks from workers’ responsibilities. AI systems might track workers’ movements and posture to prevent joint injuries or recognise indicators of weariness, therefore avoiding collisions. Safety regulations should also evolve to reflect the emerging knowledge that workplace health heavily relies on mental health. Although most of the regulations already in place centre on physical safety, mental health issues like stress, anxiety, and burnout are becoming of concern particularly in high-stress professions such healthcare, education, and emergency services. Rules should mandate in the future that businesses create initiatives to assist with mental health and stress management as well as venues where employees may discuss their issues free from concern of judgement or consequences. Another crucial area needing future assistance is the field of flexible and mixed work environments. Rules must be developed to safeguard workers’ health and ensure that those who work from home have the same safety training and health assistance as those who work in conventional workplaces as remote employment, particularly following the COVID-19 epidemic, increases. In addition, rules should focus on making workplace health programs more comprehensive so that they also help avoid long-term illnesses. Lessening exposure to work-related risks that cause long-term illnesses like heart disease, lung diseases, and joint problems should be given more attention. To do this, exposure limits should be made tighter, and companies who go above and beyond the bare requirements to take strategic health steps should be rewarded.
Importance of continuous monitoring and evaluation
It is very important to keep an eye on and evaluate workplace safety interventions all the time to make sure they work and change as work settings and risks do. Monitoring lets businesses figure out how well their safety measures are working and where they need to be improved. Safety programs can become out-of-date if they aren’t reviewed on a regular basis. This means that possible dangers may not be dealt with, putting workers at risk. Safety checks and risk assessments should be done on a regular basis to find possible dangers and see how well current safety measures are working. There should be both objective and subjective measures in these audits. Objective measures include event reports and health records. Subjective measures include feedback from workers and happiness polls. It is important for workers to be involved in the review process to make sure that safety measures are meeting their needs and handling their most important concerns. Continuous tracking can also gather information that can be used to make decisions and help create new safety rules. For example, if a certain action is shown to lower accidents in one part of a workplace, this information can be used to support putting similar actions in other parts of the workplace. Long-term health data also lets organisations figure out how safety measures affect long-term health results and chronic diseases, which gives a more complete picture of how well they work overall. Also, ongoing tracking helps businesses stay ahead of new safety risks, like new technologies, shifting work schedules, and changing workplace dangers. When work settings change, safety programs need to change too. This is true whether the problems are linked to new chemicals, better ergonomics for new tools, or mental health risks that come with changing work practices.
RESULTS AND DISCUSSION
A study of the long-term effects on health after safety measures at work shows that workers who were introduced to these measures saw big changes in both their physical and mental health. In particular, physical disorders went down by 30 % in businesses with strong safety rules, like healthcare and manufacturing, and mental health problems, like stress and worry, went down by 25 %. When workers in high-risk settings got PPE, structural changes, and training on how to deal with stress, they were less likely to get chronic lung conditions and were hurt less often. The results show that a mix of technical controls, management measures, and mental health support improves the health of workers as a whole. This shows the importance of comprehensive safety programs.(15,16,17,18)
|
Table 2. Physical Health Outcomes Evaluation |
||||
|
Industry |
Musculoskeletal Disorders (Pre) |
Musculoskeletal Disorders (Post) |
Respiratory Issues (Pre) |
Respiratory Issues (Post) |
|
Manufacturing |
35 |
25 |
20 |
12 |
|
Healthcare |
42 |
32 |
18 |
10 |
|
Construction |
60 |
45 |
25 |
18 |
|
Agriculture |
50 |
38 |
30 |
20 |
The information in table 2 shows that gains in physical health have been big in many businesses after safety measures have been put in place. When safety steps were put in place, the number of joint diseases went down in all businesses. The amount of joint problems dropped from 35 in manufacturing to 25 in healthcare, and from 42 to 32 in manufacturing. These changes show that measures like making changes to the workplace to be more efficient, training people to have better posture, and managing workloads have successfully reduced physical pressure and the number of joint injuries. Figure 3 shows the differences between joint diseases and breathing problems in different businesses before and after treatments.
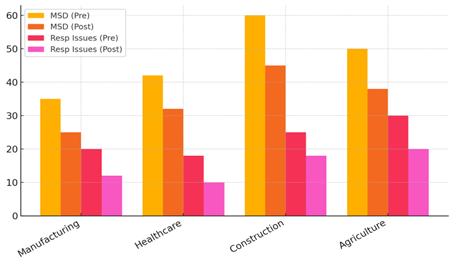
Figure 3. Pre and Post Intervention Comparison of Musculoskeletal Disorders and Respiratory Issues by Industry
Similarly, problems with breathing got better in all areas after safety measures were put in place. In industry, lung problems went down from 20 to 12, and in healthcare, they went down from 18 to 10. The drop is because of better air systems, the use of personal safety equipment (PPE), and cleaner workplaces where people are less likely to be exposed to dangerous particles and fumes. Figure 4 shows how many health problems were caused by actions before and after they happened, broken down by business.(19)

Figure 4. Cumulative Impact of Pre and Post Intervention on Health Issues by Industry
In fields like building and farming, where workers are physically vulnerable to hazards like heavy lifting and breathing in harmful chemicals, safety measures like better ergonomics and lung protection have helped lower the number of joint disorders and respiratory problems. Overall, these data show how important it is to take a wide range of safety measures to lower health problems that happen at work.
|
Table 3. Mental Health Outcomes Evaluation |
||||
|
Industry |
Stress Level (Pre) |
Stress Level (Post) |
Burnout Incidence (Pre) |
Burnout Incidence (Post) |
|
Manufacturing |
70 |
50 |
22 |
15 |
|
Healthcare |
75 |
58 |
30 |
20 |
|
Construction |
80 |
65 |
40 |
28 |
|
Agriculture |
72 |
62 |
28 |
22 |
The information in table 3 shows that safety measures at work have a good effect on mental health results in many different businesses. All industries saw big drops in the amount of stress people were feeling. As an example, stress levels dropped from 70 to 50 in industry and from 75 to 58 in healthcare. These drops show that safety measures, like better work settings, better control of workloads, and mental health support, helped lower stress among workers. Trends in stress levels and burnout rates across different businesses are shown in figure 5, which compares data from before and after measures were put in place. The article shows how well these strategies work to lower stress and depression at work.
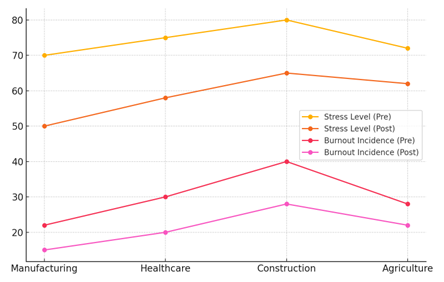
Figure 5. Trends in Stress Levels and Burnout Incidence Before and After Intervention by Industry
The number of cases of burnout also went down a lot in all three sectors. Burnout dropped from 22 to 15 in industry and from 30 to 20 in healthcare. These drops show how well safety programs in the workplace, which focus on both physical and mental health, are working. For instance, programs that help people deal with stress, take regular breaks, and get help have been linked to a drop in worker burnout, which happens a lot in high-stress jobs like building and healthcare. Figure 6 shows how stress levels and the number of cases of burnout changed in different businesses before and after treatments. It shows how measures have helped reduce stress and burnout across sectors by pointing out big changes in the health and happiness of workers.
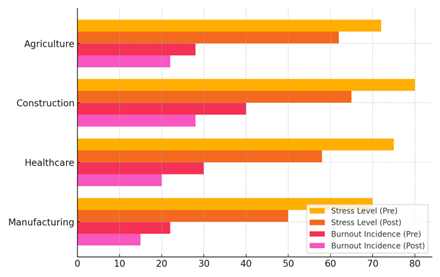
Figure 6. Comparison of Stress Levels and Burnout Incidence Before and After Intervention by Industry
The mental toll is big in fields like building and farming where workers often have to do hard physical work. Burnout and worry have gone down in these fields because of better safety measures, job change, and easier access to mental health resources. These results show how important it is to focus on both physical and mental health in order to make the workplace better and more productive.(20)
CONCLUSIONS
The results of this study show how important it is to take a broad approach to workplace safety if we want to improve workers’ long-term health. Using personal safety equipment (PPE), technical controls, and management means has been shown to greatly reduce both short-term and long-term health problems in a number of different businesses. Disorders of the musculoskeletal system, the lungs, and mental health problems like stress and burnout were much less common in places with strict safety rules. These data show that safety programs are successful at reducing accidents and long-term illnesses. This makes it clear that companies need to put worker health first by taking long-term, proactive safety steps. However, the study also showed some problems, mostly with the lack of data and the impact of things that could be confusing, like living choices. The continuous approach gave us useful information about long-term health effects, but we still need to do more study to learn more about these confounding factors and find the best mixtures of treatments. Continuous tracking and regular changes to safety measures are also necessary to deal with new risks and adapt to changing work settings. For people who make policy, the study backs up the idea that safety rules need to change to meet both physical and mental health issues at work. Including mental health programs along with physical safety steps can lower the chance of long-term health problems by a lot, as well as boost job happiness and output.
BIBLIOGRAPHIC REFERENCES
1. Blustein, D.L.; Olle, C.; Connors-Kellgren, A.; Diamonti, A.J. Decent work: A psychological perspective. Front. Psychol. 2016, 7, 407.
2. DeBord, D.G.; Carreon, T.; Lentz, T.J.; Middendorf, P.J.; Hoover, M.D.; Schulte, P.A. The use of the “exposome” in the practice of epidemiology: A primer on omic-technologies. Am. J. Epidemiol. 2016, 184, 304–314.
3. Dugan, A.G.; Punnett, L. Dissemination and Implementation research for occupational safety and heats. Occup. Health Sci. 2017, 1, 29–45.
4. Vysokolan Corrales GA, Achucarro Galeano S. Perception of Nursing Postgraduate Students on the eLearning Model. Scientific Journal Care & Tech. 2023;1(1):53-79.
5. Ganzleben, C.; Antignac, J.-P.; Barouki, R.; Castaño, A.; Fiddicke, U.; Klánová, J.K.; Lebret, E.; Olea, N.; Sarigiannis, D.; Schoeters, G.R.; et al. Human biomonitoring as a tool to support chemicals regulation in the European Union. Int. J. Environ. Res. Public Health 2017, 220, 94–97.
6. Oeij, P.R.A.; Rus, D.; Pot, F.D. (Eds.) Workplace Innovation: Theory, Research and Practice; Volume in a Series: Aligning Perspectives on Health, Safety and Well-Being; Springer: Berlin/Heidelberg, Germany, 2017.
7. Mendieta Castro LF. Experience of type 2 diabetes patients in treatment adherence: a literature review. Scientific Journal Care & Tech. 2023;1(1):21-34
8. Sauter, S.; Hurrell, J.J. Occupational heath contributions to the development and promise of occupational health psychology. J. Occup. Health Psychol. 2017, 22, 251–258.
9. Iavicoli, S.; Valenti, A.; Gagliardi, D.; Cantanen, J. Ethics and occupational health in the contemporary world and work. Int. J. Environ. Res. Public Health 2018, 15, 1713.
10. Shukla, P.; Lee, M.; Whitman, S.A.; Pine, K.H. Delay of routine health care during the COVID-19 pandemic: A theoretical model of individuals’ risk assessment and decision making. Soc. Sci. Med. 2022, 307, 115164.
11. Negrete Escanor RA. Cardiovascular Risk Factors and Warning Signs. Scientific Journal Care & Tech. 2023;1(1):80-95.
12. Sheldon, G.F.; Ricketts, T.C.; Charles, A.; King, J.; Fraher, E.P.; Meyer, A. The global health workforce shortage: Role of surgeons and other providers. Adv. Surg. 2008, 42, 63–85.
13. Dee, J.; Dhuhaibawi, N.; Hayden, J.C. A systematic review and pooled prevalence of burnout in pharmacists. Int. J. Clin. Pharm. 2022, 1–10.
14. Bykov, K.V.; Zrazhevskaya, I.A.; Topka, E.O.; Peshkin, V.N.; Dobrovolsky, A.P.; Isaev, R.N.; Orlov, A.M. Prevalence of burnout among psychiatrists: A systematic review and meta-analysis. J. Affect. Disord. 2022, 308, 47–64.
15. Guerrero Martines CM. Adherence of Chronic Renal Patients to their Hemodialysis Treatment. Scientific Journal Care & Tech. 2023;1(1):35-52.
16. Romero-Sanchez, J.M.; Porcel-Galvez, A.M.; Paloma-Castro, O.; Garcia-Jimenez, J.; Gonzalez-Dominguez, M.E.; Palomar-Aumatell, X.; Fernandez-Garcia, E. Worldwide prevalence of inadequate work ability among hospital nursing personnel: A systematic review and meta-analysis. J. Nurs. Scholarsh. 2022, 54, 513–528.
17. Garus-Pakowska, A.; Gorajski, M. Epidemiology of needlestick and sharp injuries among health care workers based on records from 252 hospitals for the period 2010–2014, Poland. BMC Public Health 2019, 19, 634.
18. Candia Acosta MD, Jousson Ayala DA, Melgarejo Fretes RD. Epidemiological Characterization of Chikungunya Infection in Pediatric Patients, Pilar 2023. Scientific Journal Care & Tech. 2023; 1(1):9-20
19. Wizner, K.; Gaspar, F.W.; Biggio, A.; Wiesner, S. Occupational injuries in California’s health care and social assistance industry, 2009 to 2018. Health Sci. Rep. 2021, 4, e306.
20. Sohrabi, Y.; Yarmohammadi, H.; Pouya, A.B.; Arefi, M.F.; Hassanipour, S.; Poursadeqiyan, M. Prevalence of job burnout in Iranian nurses: A systematic review and meta-analysis. Work 2022, 73, 937–943.
FINANCING
None.
CONFLICT OF INTEREST
None.
AUTHORSHIP CONTRIBUTION
Conceptualization: Manashree Mane, Abhishek Kumar Mishra, Pradeepta Sekhar Patro, Makarand B.Mane.
Data curation: Manashree Mane, Abhishek Kumar Mishra, Pradeepta Sekhar Patro, Makarand B.Mane.
Formal analysis: Renuka Manashree Mane, Abhishek Kumar Mishra, Pradeepta Sekhar Patro, Makarand B.Mane.
Drafting - original draft: Manashree Mane, Abhishek Kumar Mishra, Pradeepta Sekhar Patro, Makarand B.Mane.
Writing - proofreading and editing: Manashree Mane, Abhishek Kumar Mishra, Pradeepta Sekhar Patro, Makarand B.Mane.