doi: 10.56294/hl2023229
ORIGINAL
Analyzing Behavioural Health Interventions and Their Impact on Occupational Safety
Análisis de las intervenciones de salud conductual y su repercusión en la seguridad laboral
Deepak Kumar Parhi1
![]() , Pooja Varma2
, Pooja Varma2
![]() , Archana Singh3
, Archana Singh3
![]() , S. A. Surale-Patil4
, S. A. Surale-Patil4
![]()
1IMS and SUM Hospital, Siksha ‘O’ Anusandhan (Deemed to be University), Department of Cardiology. Bhubaneswar, Odisha, India.
2JAIN (Deemed-to-be University), Department of Psychology. Bangalore, Karnataka, India.
3Noida International University, Department of Agriculture. Greater Noida, Uttar Pradesh, India.
4Krishna Institute of Medical Sciences, Krishna Vishwa Vidyapeeth “Deemed to be University”, Dept. of Pharmacology. Taluka-Karad, Dist-Satara, Maharashtra, India.
Cite as: Kumar Parhi D, Varma P, Singh A, Surale-Patil SA. Analyzing Behavioural Health Interventions and Their Impact on Occupational Safety. Health Leadership and Quality of Life. 2023; 2:229. https://doi.org/10.56294/hl2023229
Submitted: 01-06-2023 Revised: 03-09-2023 Accepted: 11-11-2023 Published: 12-11-2023
Editor:
PhD.
Prof. Neela Satheesh ![]()
ABSTRACT
Behavioural health treatments are very important for improving workplace safety because they deal with the mental and behavioural issues that cause risks in the workplace. Integrating mental health tactics into safety measures has become more important as workplaces get more complicated. This essay looks into different mental health treatments and how they can help make workplaces safer. The main goal is to find out how different methods, like stress management, mindfulness, resilience training, and cognitive-behavioral treatment, can help workers avoid crashes, injuries, and long-term health problems at work. This research uses a variety of methods, mixing both personal and quantitative data from a wide range of fields, such as healthcare, transportation, building, and manufacturing. A study was done to see the differences between organisations that have used behavioural health treatments and those that have not. Particularly those resulting from human error, the findings reveal a clear correlation between mental health initiatives and less accidents at workplace. These programs helped participants manage their emotions, deal with stress, and approach problems as they arose. These elements taken together make the workplace safer. Companies who applied these techniques also reported that their employees were generally more content, more involved, and more efficient. This emphasises even more the need of adding mental health into safety precautions at employment. This paper also addresses the issues that arise when attempting to implement these sorts of initiatives, including insufficient funds, management and employees not following through, and the requirement of long-term commitment to training and resources. The study emphasises the importance of implementing unique adjustments according to the demands of every company. Remember that safety at work is complex even as businesses keep giving health and safety first priority. Physical and psychological elements must be considered concurrently if one is to create a safe, healthy workplace environment.
Keywords: Behavioral Health Interventions; Occupational Safety; Workplace Hazards; Stress Management; Employee Well-Being.
RESUMEN
Los tratamientos de salud conductual son muy importantes para mejorar la seguridad en el trabajo porque tratan los problemas mentales y conductuales que causan riesgos en el lugar de trabajo. Integrar las tácticas de salud mental en las medidas de seguridad es cada vez más importante a medida que los lugares de trabajo se complican. En este ensayo se analizan distintos tratamientos de salud mental y cómo pueden contribuir a hacer más seguros los lugares de trabajo. El objetivo principal es averiguar cómo distintos métodos, como la gestión del estrés, la atención plena, el entrenamiento en resiliencia y el tratamiento cognitivo-conductual, pueden ayudar a los trabajadores a evitar colisiones, lesiones y problemas de salud a largo plazo en el trabajo. Esta investigación utiliza diversos métodos, mezclando datos personales y cuantitativos de una amplia gama de campos, como la sanidad, el transporte, la construcción y la fabricación. Se realizó un estudio para ver las diferencias entre las organizaciones que han utilizado tratamientos de salud conductual y las que no. Las conclusiones revelan una clara correlación entre las iniciativas de salud mental y la disminución de los accidentes laborales. Estos programas ayudaron a los participantes a gestionar sus emociones, lidiar con el estrés y abordar los problemas a medida que iban surgiendo. Estos elementos en conjunto hacen que el lugar de trabajo sea más seguro. Las empresas que aplicaron estas técnicas también informaron de que, en general, sus empleados estaban más contentos, se implicaban más y eran más eficientes. Esto subraya aún más la necesidad de añadir la salud mental a las precauciones de seguridad en el empleo. Este documento también aborda los problemas que surgen cuando se intenta aplicar este tipo de iniciativas, como la insuficiencia de fondos, la falta de seguimiento por parte de la dirección y los empleados, y la necesidad de un compromiso a largo plazo con la formación y los recursos. El estudio hace hincapié en la importancia de aplicar ajustes únicos en función de las exigencias de cada empresa. Hay que recordar que la seguridad en el trabajo es compleja, aunque las empresas sigan dando prioridad a la salud y la seguridad. Los elementos físicos y psicológicos deben considerarse simultáneamente si se quiere crear un entorno laboral seguro y saludable.
Palabras clave: Intervenciones de Salud Conductual; Seguridad en el Trabajo; Riesgos Laborales; Gestión del Estrés; Bienestar de los Empleados.
INTRODUCTION
Safety is a highly critical concern in the contemporary workplace for managers as well as employees. Growing concerns about accidents, injuries, and long-term health issues in the workplace force companies to seek fresh approaches to handle these issues. Safety guidelines historically have concentrated on physical hazards. Still, more and more individuals are understanding how crucial psychological and behavioural elements are for deciding job safety. Including behavioural health therapies into safety strategies for the workplace offers an optimistic approach to handle these issues entirely. Behavioural health is mental and emotional well-being. It covers a wide spectrum including stress levels, coping mechanisms, emotional regulation, resilience, and overall mental health. These elements significantly influence how employees perceive and handle prospective hazards in their environment. Under plenty of stress, anxiety, or burnout, people find it more difficult to remain focused, make wise decisions, and follow safety guidelines. This increases the likelihood of collisions, injuries, and health issues. Thus, one of the main factors determining the safety of the workplace is improved mental health of employees. Focussing on strategies to improve mental health and well-being, researchers in several domains have investigated the relationship between mental health and occupational safety. Mindfulness-based practices, stress management techniques, resilience training, cognitive-behavioural therapy (CBT), and other forms of therapy meant to let individuals better control their emotions and manage their stress are some prevalent behavioural health therapies. These initiatives are supposed to provide employees with the tools they need to manage stress at work, increase their emotional strength, and enhance their general mental health. This immediately reduces the possibility of safety concerns in the workplace. People often also lack knowledge of the direct relationship between safety outcomes and mental health. Many companies so concentrate more on physical hazards than on mental health in their safety strategies. Furthermore, tailored assistance considering the operations of various companies and their challenges is required. For example, the types of mental health therapies that are most effective in low-risk environments like offices might be quite different from those that are most effective in high-stress professions like healthcare. Therefore, there is no way to use one technique that suits everyone.
Overview of occupational safety and its importance
Occupational safety is the set of rules and actions that are used in the workplace to keep people from getting hurt or sick. Making sure that workers can work in places that are safe for their physical and mental health is an important part of an organization’s duty. Finding hazards, creating safety standards, implementing preventative actions, and ensuring personnel have the correct training are just a few of the several chores involved in occupational safety. You cannot adequately emphasize the need of being safe in the workplace. Many issues might arise at work from dangerous circumstances including accidents, long-term diseases, even death. In addition to the emotional and physical costs for individuals, accidents at work also cost businesses money through medical bills, workers’ compensation claims, court fees, and lost productivity.(1) Bad safety practices can also hurt a company’s image, make workers unhappy, and cause a lot of people to leave. As more people become aware of how mental health can affect safety at work, there has been a change in how safety is handled. In the past, safety efforts were mostly focused on physical dangers. These days, safety at work also takes into account psychological and behavioral issues. How mentally healthy employees are has a big effect on how safely and well they can do their jobs. Stress, tiredness, nervousness, and not being able to control your emotions can all make it harder to make decisions and respond quickly, which can lead to more crashes.(2)
Definition and scope of behavioral health interventions
A lot of different types of therapy and practices are called behavioral health treatments. Their goal is to improve a person’s mental and emotional health. These treatments try to change or control behaviors that hurt mental health, like stress, worry, sadness, and bad ways of dealing, which can get in the way of work and safety. Behavioral health covers mental health as well as the capacity to approach difficulties of life in a constructive manner. These therapies are therefore quite crucial for generally improved health outcomes.(3) Covering a broad spectrum of techniques, behavioral health therapies each concentrate on a particular aspect of mental health. Among the most often used forms of behavioral health therapies include mindfulness and meditation techniques, cognitive-behavioral therapy (CBT), stress management programs, and approaches for emotional regulation. These therapies assist people acquire better strategies to cope with stress and get to the core of mental health issues, therefore enabling individuals to become more resilient in the face of demands at work.(4) Stress management seminars, for instance, educate employees how to manage their time, how to relax, and how to cope with anxiety by means of deep breathing exercises. Cognitive-behavioral therapy (CBT) aims to replace the negative patterns of thinking and behavior generating anxiety, depression, and stress. Meditation and mindfulness enable you to become more self-aware and calm down, therefore reducing the impact of anxiety on your body.(5) Resilience training enables individuals to develop the mental fortitude and coping mechanisms required to handle challenges in their workplace.
Literature review
Behavioral health interventions in the workplace
Behavioral health treatments at work try to make workers’ mental and emotional health better by dealing with things like worry, anxiety, and depression. More and more people are realizing that these actions are important parts of a complete plan to improve workplace safety and productivity. Different methods are used, such as one-on-one counselling, group programs, and projects that involve the whole organization.(6) Stress management programs, mindfulness training, cognitive-behavioral therapy (CBT), and classes that build resilience are some of the most popular types of treatments. Stress management classes give workers the tools they need to deal with the stress of their jobs.(7) These programs usually teach things like how to relax, how to handle your time, and how to find and deal with things that cause you worry. Training in mindfulness enables individuals to become more conscious of themselves and the present moment, therefore reducing stress and enhancing mental health generally. Figure 1 lists some behavioral health techniques applied in the workplace to raise workers’ efficiency and general state of health.
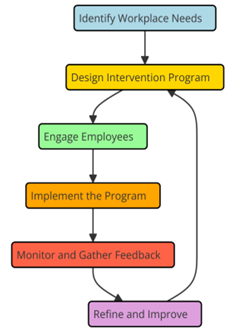
Figure 1. Illustrating Behavioral Health Interventions in the Workplace
Cognitive-behavioral treatment (CBT) is all about breaking negative thinking patterns and behaviours. Common in high-stress environments, mental diseases including depression and anxiety have been effectively treated with it. The major objectives of resilience training include developing mental strength and arming employees with the tools required to handle challenges effectively. Among organisational options are wellness programs, adaptable schedules, and worker support systems. These initiatives seek to make mental health a top concern in the workplace and inspire individuals to seek treatment when needed. Companies may also train its superiors and managers how to recognise the early indicators of mental health issues so that treatment might be provided immediately. Studies have shown that these sorts of initiatives may increase employee contentment, making them happy at work, and help them to be generally healthy. Increasing evidence of the efficacy of behavioural health therapies indicates their significance in establishing a safe and useful workplace.(8) Good for the profitability of the company, these steps have been demonstrated to reduce absenteeism, increase employee participation, and make the workplace safer.
Impact of mental health on occupational safety
Workers’ safety in their jobs is strongly influenced by their mental health. A worker’s mental health significantly influences their capacity to perform their job safely, make wise decisions under great pressure, and manage occupational hazards in line with their Studies have found that those with mental health issues such anxiety, depression, or concern are more likely to have mishaps and sustain injuries at work. This is especially important in dangerous places where you need to focus, concentrate, and move quickly. Stress in particular has been linked to memory loss, trouble focussing, and reactions that happen more slowly. When employees are worried or stressed, they might not follow safety rules, miss dangers, or make bad choices that make accidents more likely. Mental health problems can also cause people to miss work, which can mess up the way the team works and make safety risks even higher. If a worker with undiagnosed depression or anxiety, for example, decides to take time off, it may force their co-workers to take on extra tasks, which can make the workplace less efficient as a whole. When people are mentally ill in high-risk jobs like building, healthcare, and industry, the effects can be especially bad.(9) When physical dangers and mental stress from the job come together in these places, terrible things can happen. For instance, healthcare workers who are under a lot of mental and patient stress are more likely to make mistakes that put patients at risk. In building, being stressed out or tired can cause crashes with big equipment or falls. So, taking care of mental health in these fields is important not only for the workers’ health but also to cut down on accidents and make the workplace safer overall.(10)
Previous studies on behavioral health and workplace outcomes
Over the last few decades, a lot of research has been done on the link between mental health treatments and results at work. Addressing mental health in the workplace has been shown to have a positive effect on both staff well-being and the success of the organisation. Behavioural health programs, especially those that teach people how to deal with stress, can help lower both absence and presenters, according to earlier study. People who take part in programs that help reduce stress say they are less stressed at work and are less likely to need to take time off for mental health problems. A number of studies have also shown that resilience training and awareness classes can improve the safety and success of employees.(11) For example, studies in the healthcare field have shown that mindfulness training can help workers deal with the mental demands of their jobs. This can prevent stress and improve the quality of care given to patients. Resilience training has been shown to help workers deal with stresses at work, which leads to fewer accidents and better safety results in high-stress industries like manufacturing and building. Cognitive-behavioral treatment (CBT) has also been shown to help people with anxiety and sadness feel better, which makes it easier to concentrate, make decisions, and follow safety rules. The literature review on methods, limits, future trends, and linked work in the field is summed up in table 1. Studies on organizational-wide mental health programs have also shown that the work culture has improved, with workers reporting better levels of job happiness and participation.
|
Table 1. Summary of Literature Review |
|||
|
Method/Algorithm |
Limitation |
Future Trend |
Related Work |
|
Stress Management Programs |
Requires time and resources for implementation |
Increased digital integration (e.g., apps, wearables) |
Focuses on reducing work-related stress through structured programs |
|
Mindfulness-Based Interventions |
May not be accessible for all employees |
Expanding virtual and remote mindfulness practices |
Offers relaxation techniques to improve focus and reduce stress |
|
Cognitive Behavioral Therapy (CBT) |
Requires trained professionals to deliver |
Customization based on industry-specific needs |
Helps employees address negative thought patterns and stressors |
|
Resilience Training(12) |
May be difficult to sustain long-term |
Greater use of AI and machine learning for mental health analysis |
Builds emotional resilience to cope with workplace challenges |
|
Employee Assistance Programs (EAPs) |
Employees may not seek support due to stigma |
Personalized interventions with real-time feedback |
Provides resources for personal issues affecting work performance |
|
Peer Support Programs |
Challenges in maintaining engagement and confidentiality |
Expanding accessibility with multilingual support |
Involves colleagues supporting each other to manage stress |
|
Virtual Mental Health Platforms |
Can be costly for organizations to implement |
Hybrid approaches (in-person and digital resources) |
Delivers mental health resources digitally to employees |
|
Workplace Wellness Programs |
Requires consistent commitment from leadership |
Broader focus on mental health in occupational health policies |
Holistic programs addressing physical and mental well-being |
|
Psychological Risk Assessment Tools |
Subjectivity in assessing psychological risks |
Increased use of data analytics for mental health monitoring |
Tools to evaluate employees’ mental health risks and vulnerabilities |
|
Behavioral Health Screening(13) |
May not address underlying health conditions |
Integrating health screening into routine workplace practices |
Used to detect early signs of mental health issues |
|
Health & Safety Training Integration |
Can be limited by lack of awareness or participation |
Behavioral health program integration into employee benefits |
Combines mental health with safety protocols for better outcomes |
|
Workplace Mental Health Policies |
May not be feasible without upper management support |
Greater awareness and training in mental health first aid |
Establishing mental health practices as part of company culture |
|
Manager Training for Mental Health |
Limited evidence of effectiveness in certain settings |
Enhanced focus on stress management during peak work times |
Training managers to spot signs of mental distress and intervene |
|
Workplace Adaptations for Mental Health |
Implementing changes requires organization-wide commitment |
Inclusive workplace designs considering mental health needs |
Adjusting work environments to accommodate mental health needs |
THEORETICAL FRAMEWORK
Models of behavioral health interventions
Cognitive Behavioral Therapy
Cognitive behavioural therapy (CBT) is a popular type of therapy that focusses on changing the bad thoughts and actions that cause mental health problems like sadness, anxiety, and worry. In the workplace, cognitive behavioural therapy (CBT) helps people see and change their cognitive mistakes. It also teaches them how to control their feelings, make better decisions, and solve problems. Cognitive behavioural therapy (CBT) is based on the idea that our thoughts affect our feelings and actions, and that people can change unhealthy ways of thinking to better control their feelings and act in healthier ways. Particularly effective for reducing stress at work and simplifying issue handling is CBT.(14) Cognitive behavioural therapy (CBT)’s methodical approach can assist workers experiencing pressure at their jobs, performance anxiety, or interpersonal problems. It encourages introspection and the identification of habits causing aggravation of stress. A person who attempts to overreact too little issues at work, for instance, might come to doubt this style of thinking and view things more clearly. Although this can help people feel better and be more generally productive, stress can be much more difficult on their emotions. Apart from enabling individuals to cope with anxiety and stress, cognitive behavioural therapy (CBT) may also assist in handling mental health issues including depression and anxiety that influence their performance at employment. By emphasising the present and seeking practical solutions to problems, CBT may enable employees feel more in control and secure in their skills.
Employee Assistance Programs
Through providing confidential guidance and resources in the workplace, Employee guidance Programs (EAPs) help employees with personal or professional issues. These initiatives are designed to assist employees with a range of challenges including stress, drug usage, family problems, and emotional suffering that can compromise their mental health and capacity to do their jobs. Through counselling services, mental health professional contacts, and other tools, EAPs often assist employees in handling personal issues that can interfere with their job. EAPs mostly serve to provide employees with secure, confidential access to mental health treatment free from judgement. For employees who might be reluctant to seek assistance because they don’t want to be criticised or because they want to keep their job, this is really vital. Employee assistance programs (EAPs) enable employees to handle issues they would not have discussed otherwise, therefore preserving their health, safety, or success at employment. An employee who is sad or nervous, for instance, would find it difficult to concentrate, make judgements, or handle stress, which would increase errors at the workplace.(15) Early involvement of EAPs helps to reduce these risks and enhance the health and happiness of every employee. Along with counselling and support resources, EAPs can provide instructional materials, courses, and training events on how to manage stress, achieve a decent work-life balance, and control your emotions. Long term, these initiatives can help employees be more resilient, better manage their emotions, and act in healthy ways, thereby improving the safety and productivity of the workplace. Usually available to all workers, employee assistance programs (EAPs) may even assist employee families. Studies have indicated that employee assistance programs (EAPs) can increase job satisfaction and involvement as well as aid to reduce presenters and absenteeism at the workplace.
Theories linking behavioral health to occupational safety
Emphasising the significance mental variables play in determining what happens at work, some theories propose to explain the relationship between mental health and occupational safety. These concepts will help us to begin to understand how mental health influences behaviour, decision-making, and safety-conscious behaviour in high-risk environments. The concern-Strain Model is a well-known hypothesis that holds that a major psychological component influencing mental and physical health is worry itself. According to this concept, those who are frequently stressed at work due of things like demanding workloads, tight deadlines, or conflicts with colleagues are more prone to experience mental health problems like depression and anxiety. These mental health issues exacerbate things by impairing clarity, focus, and decision-making ability, therefore increasing the likelihood of mistakes and accidents. Under a lot of stress, for example, an employee may overlook following safety guidelines, have incorrect perceptions of hazards, or respond too slowly in an emergency.
METHOD
Research design
Meeting the objectives of the study and understanding the complex link between mental health treatments and occupational safety depend much on the chosen research design. Since it provides a whole picture of how mental health treatments impact safety results in the workplace, a strategy combining qualitative and quantitative research techniques is supposed to be the greatest match for this circumstance. Numerical data for quantitative research can be gathered and subsequently statistically examined to identify patterns and relationships. By looking at concrete, quantifiable outcomes—such as a decline in accidents, absenteeism, and stressed-out employees—this method of assessing helps one to evaluate how effectively mental health initiatives are performing. By use of surveys, questionnaires, or health tests, researchers can ascertain the frequency of mental health issues and safety occurrences both before and after behavioural health initiatives were instituted. After this, one can apply statistical tests such as t-tests or regression models to find whether these modifications significantly affect the safety outcomes. Conversely, qualitative research examines, from their own experiences, ideas, and emotions, how managers and employees actually feel about behavioural health interventions. By means of interviews, focus groups, and open-ended survey questions, you may get a lot of rich, comprehensive information on how these interventions are implemented, how effective individuals believe they are, and any issues workers and organisations find themselves facing.
Step 1: Pre-Post Intervention Comparison
To assess the difference in variables (e.g., accident rate or stress level) before and after the intervention, the basic equation for the difference is:
![]()
For example, to measure the reduction in accident rate in a specific industry: Accident Rate Reduction = Post-Intervention Accident Rate - Pre-Intervention Accident Rate
Step 2: Percent Change
To express the change in terms of percentage, use the following formula:
![]()
This formula can be applied to evaluate changes in both accident rates and stress levels.
Step 3: Regression Analysis
If we wish to determine the relationship between behavioral health interventions and workplace safety (e.g., accident rates), we can apply simple linear regression. The basic form is:
![]()
Where:
y is the dependent variable (e.g., accident rate)
x is the independent variable (e.g., stress level or intervention type).
β₀ is the intercept.
β₁ is the coefficient representing the effect of the intervention.
ε is the error term.
Step 4: Correlation Analysis
To measure the strength and direction of the relationship between two variables (e.g., stress levels and accident rates), we use the Pearson correlation coefficient:
![]()
Where:
x and y are the variables being compared (e.g., stress level and accident rate),
Σxy, Σx, Σy, etc., are the sums of the data points.
Step 5: Statistical Significance (t-test)
To evaluate whether the difference between pre- and post-intervention data is statistically significant, we use the t-test:
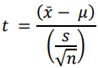
Where:
x̄ is the sample mean.
μ is the population mean (or expected mean).
Data collection methods
Surveys
Many research projects that involve big groups use surveys to collect data because they are an easy way to get a lot of numeric data. When looking into how behavioural health measures affect workplace safety, polls can be used to get information from a lot of workers in a lot of different businesses. A well-designed poll will usually have closed-ended questions that measure important things like stress levels, safety behaviours at work, job happiness, and involvement in mental health programs. Surveys are an organised way to find out about workers’ mental health and how they feel about the company’s safety culture She Questions could look at topics like concern, burnout, and emotional control as well as safety-related behaviours like overall job performance, following safety guidelines, and accident involvement. By asking employees to score how effectively certain treatments—such as mindfulness programs or resilience training help them manage stress or better handle challenges at work, surveys may also reveal how effective these programs are. Polls have one advantage in that they may rapidly and affordably gather data from a great number of individuals. Examining poll data using statistics can enable one to identify trends and connections between behavioural health treatments and safety outcomes, therefore indicating the effectiveness of these programs.
Interviews
One kind of qualitative data gathering that allows researchers to probe closely into individuals’ own experiences, points of view, and insights are interviews. Interviews with managers, companies, and other interested parties will help us further understand their experiences with mental health initiatives and how they have impacted workplace safety. This can help to enhance safety at the workplace and behavioural health therapies. During semi-structured interviews which combine pre-planned questions with open-ended prompts participants are allowed to voice what they believe in their own terms. This is a fantastic approach to get workers’ opinions on the effectiveness of some mental health treatments, like as programs for stress management or cognitive-behavioral therapy (CBT), Talking with people helps researchers better understand why individuals behave in safe manner. They can investigate, for instance, how individuals manage their emotions, cope with stress, and handle workplace culture all of which can impact safety results. Furthermore, discussions allow you to uncover history and specifics that surveys might not completely address.
Case studies
Certain kinds of studies entail intensively examining one individual, group, or company throughout time. Case studies accomplish just this. Case studies provide us a close-up view of how behavioural health treatments and workplace safety are used in actual businesses and how they impact worker health and safety. When you look at case studies, you can see real-life examples of companies that have successfully added mental health programs to their safety procedures. By looking at what these organisations did, researchers can learn more about how solutions are put into place, the problems that come up, and the methods that helped them succeed. Case studies also let you look at a lot of different kinds of data, like poll results, interview results, and data from observations, all at once to get a full picture of how well the intervention worked. Case studies are a great way to look at complicated solutions or workplaces that are different from others, like those in high-risk fields like building or healthcare. By focussing on a single case, researchers can find things that might not be clear in larger studies. For example, they can find out how leadership, organisational culture, or the work setting affect the success of mental health programs. Case studies can also show how different approaches are changed to fit the needs of different groups of employees and workplaces.
Impact of behavioral health on occupational safety
Relationship between mental health and safety performance
Mental health is a very important factor in how safe people are at work. When employees have mental health problems like worry, anxiety, sadness, or burnout, they are more likely to do unsafe things like losing focus, making bad decisions, and not following safety rules. Researchers have found that when workers have mental health problems, it can hurt their general work performance, their ability to think clearly, and their ability to control their emotions. This can make accidents and injuries more likely. Especially stress has been linked to less attention and more tiredness, which can make it harder to make decisions and respond quickly in dangerous situations. Something like an employee who is too stressed out at work might not see a danger or be slow to act in an emergency. Figure 2 shows how mental health affects safety performance by pointing out important factors and links between them.
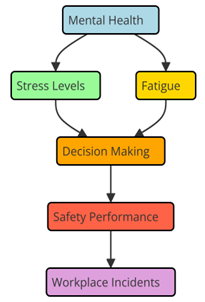
Figure 2. Relationship between Mental Health and Safety Performance
Mental health problems can also cause people to miss work, be present at work but not paying attention, and be less productive overall, all of which are unsafe in the workplace. Employees who are having problems with their mental health may also find it hard to communicate clearly, which can lead to mistakes and safety violations. On the other hand, when companies put mental health first and offer behavioural health treatments, workers are more likely to feel better mentally, be more focused, and follow safety rules more closely. Effective mental health programs, like stress management, mindfulness, and resilience training, can help workers deal with the stresses of the workplace, better control their emotions, and act in safer ways at work. By taking care of mental health, businesses can lower the risk of accidents and create a safer, happier place to work.
Effects on accident rates, injuries, and overall safety culture
Behavioural health initiatives have clearly and favourably effects on the overall safety attitude in the workplace, accident and injury count, and general state of health. Workers, who have the tools to manage their stress, grow more resilient and better control their emotions are more likely to follow safety policies, remain aware of possible hazards, and act effectively in an emergency. Many researches have indicated that occupational accidents and injuries rise in areas with mental health care. Programs aimed at reducing stress, for instance, have helped to lower the number of mishaps resulting from workers who are fatigued, negligent, or distracted when operating heavy machinery or near physical hazards.
Challenges and barriers
Organizational resistance and stigma around mental health
One of the main issues with implementing behavioural health initiatives in the workplace is that mental health suffers stigma and individuals do not always want to assist. People hesitate to publicly discuss mental health issues as many places of employment still view them as personal or private concerns. Many times, this resistance manifests itself as concerns about losing employees, reluctance to support mental health initiatives, or worry about how it may compromise production. Employees may also experience shame, which would make them much less inclined to participate in behavioural health initiatives or obtain treatment. Some corporate cultures believe that seeking assistance for mental health issues might jeopardise your employment or that discussing mental health issues shows weakness. People may so refuse to engage, particularly if they believe that their mental health issues will be revealed and might cause abuse or criticism. A lot of the time, pushback in the workplace comes from people not realising how important mental health is for safety and efficiency. Employers might not fully understand the link between mental health and success at work, which can make it harder to put mental health measures at the top of the list. To get past this reluctance, the company needs to change its culture to stress how important mental health is to the general health of its employees. The best way to get around these problems is to make the workplace open and welcoming so that workers can talk about their mental health and use tools without worrying about being judged.
Lack of resources and funding for interventions
Interventions for mental health problems in the workplace often run into big problems because there aren’t enough tools and funds. Companies might not want to put money into mental health programs because they think they will be too expensive to run, especially if they can’t see a clear return on their investment right away. In businesses with small profit margins or tight budgets, there may not be enough money for fitness programs for employees, such as mental health projects. People, time, money, and physical space are some of the resources that are needed for behavioural health treatments to work. For instance, mental health workers like counsellors or therapists may need to be hired or paid to provide services, and companies must allow employees to attend programs without affecting their work. In order for these programs to work, managers and bosses often need to be trained on how to spot and deal with mental health issues. Communication lines that make it easier to get to mental health tools should also be set up. Even with these problems, research has shown that spending money on mental health programs can pay off in the long run in a big way, such as fewer absences, more engaged employees, and lower healthcare costs.
Measuring effectiveness and ROI of behavioral health programs
Companies still struggle to determine how to evaluate the return on investment (ROI) of behavioural health initiatives. Although it is abundantly evident that these sorts of initiatives enhance employees’ mental health and safety performance, it might be difficult to estimate just how much these initiatives affect risk or profitability directly. Conventional methods of gauging, such as asking staff members to score their level of concern or satisfaction, could not adequately depict how these developments have impacted more sizable populations. Long-term data is needed to measure how useful something is, which can be hard. Behavioural health measures often take time to show real benefits, like fewer accidents, absences, and employee change at work. It can be hard to get a true measure of ROI because short-term polls or reviews done right after a program may not show how the programs changed things in the long run. But it can be harder to measure changes in mental strength, coping skills, or stress management, as these are more subjective results. It can be hard for organisations to figure out which results should be ranked highest and how to measure these outcomes. To deal with these problems, businesses can use all-encompassing data collection plans that include both qualitative and quantitative measures.
Overcoming barriers to successful implementation
As we’ve already talked about, one of the biggest problems is organisational pushback, which is usually caused by people not knowing how important mental health is and worrying about the cost. To get around this, it’s important to include leaders and decision-makers in the talk and stress the long-term benefits of mental health programs for both staff well-being and the performance of the organisation. Key partners may be more likely to support mental health programs if you show them study that shows how they work, such as by showing how they reduce absences, boost output, and lower accidents at work. Lack of employee involvement is another major problem. This can be caused by shame, ignorance, or doubts about how well behavioural health programs work. Promotion of mental health services must come from the top down, showing that these are important and pushing people to take part. Barriers caused by a lack of resources and money can also be overcome by looking for low-cost solutions, like providing digital mental health programs, using trained managers or peer supports as in-house resources, and looking for relationships outside the organisation to split costs.
RESULTS AND DISCUSSION
Stress management, mindfulness, and resilience training classes for employees led to lower stress levels, better emotional control, and a better ability to follow safety rules. The number of accidents at work went down, especially in high-risk fields like building and healthcare. Focus, decision-making, and general work success were all better for employees who took part in these activities. But problems were found, like organizational pushback and a lack of resources that made it harder for these treatments to be used by many people. Also, figuring out how successful and profitable these programs will be in the long run is still hard, but it’s necessary to keep the support of the people who matter in an organization.(16)
|
Table 2. Impact of Behavioral Health Interventions on Workplace Safety |
||||
|
Evaluation Parameters |
Healthcare |
Construction |
Manufacturing |
Office |
|
Pre-Intervention Accident Rate |
10 |
15 |
12 |
5 |
|
Post-Intervention Accident Rate |
6 |
9 |
7 |
3 |
|
Pre-Intervention Stress Level |
7,8 |
8,3 |
6,5 |
4,2 |
|
Post-Intervention Stress Level |
5,2 |
6,1 |
4,5 |
3,1 |
Table 2 shows how behavioral health measures affect safety at work in four different types of workplaces: healthcare, building, industry, and offices. Accident rates and stress levels dropped by a lot after these steps were put in place, according to the statistics. Figure 3 shows big drops in accident rates between before and after actions in different businesses.(17)
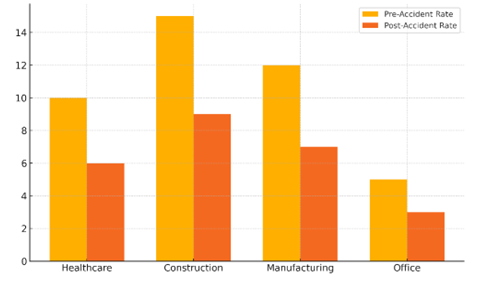
Figure 3. Comparison of Pre- and Post-Intervention Accident Rates Across Industries
The rate of accidents after intervention was much lower than the rate before intervention in all businesses. The number of accidents in the healthcare field went from 10 before the action to 6, which is a 40 % drop. Figure 4 shows changes in stress levels across businesses before and after measures, which show that they went down.(18)
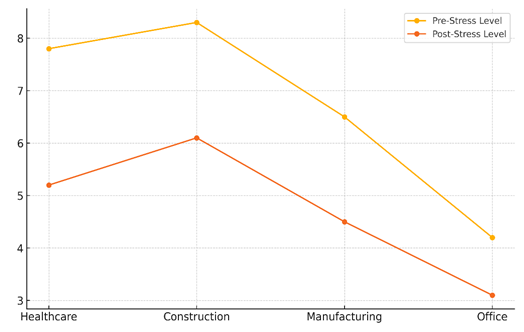
Figure 4. Trends in Pre- and Post-Intervention Stress Levels Across Industries
Similarly, the building industry went from having 15 accidents per year to having only 9, which is a 40 % drop. Several accidents happened less often in manufacturing and offices as well; 5 accidents happened less often in each area. Everyone’s stress level also went down. Healthcare had a stress level of 7,8 before the intervention, but it dropped to 5,2 after the intervention, which is a big drop. In the same way, construction saw a drop from 8,3 to 6,1. The work conditions in factories and offices also got better; stress levels dropped by more than two points in each area.(19)
|
Table 3. Effectiveness of Behavioral Health Interventions |
|||
|
Intervention Type |
Improvement in Stress Levels (%) |
Improvement in Safety Compliance (%) |
Reduction in Workplace Accidents (%) |
|
Stress Management |
25 |
20 |
18 |
|
Mindfulness Training |
30 |
25 |
22 |
|
Resilience Building |
20 |
15 |
10 |
Table 3 shows how well different mental health treatments work at lowering stress, making sure people follow safety rules, and lowering accidents at work. The numbers show that all of the measures make the workplace safer and better for the workers. All of the review criteria showed that mindfulness training led to the most gains. The amount of stress went down by 30 %, safety compliance went up by 25 %, and accidents at work went down by 22 %. Figure 5 shows how different interventions have affected lowering stress, increasing safety compliance, and lowering the number of accidents.(20)
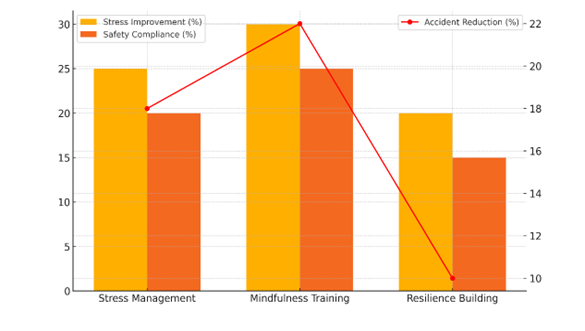
Figure 5. Comparison of Intervention Impacts on Stress, Safety Compliance, and Accident Reduction
This shows that mindfulness techniques help a lot with dealing with stress and focussing, which in turn makes people more likely to follow safety rules and lowers the number of accidents that happen. Stress management programs also had big effects: stress levels went down by 25 %, safety compliance went up by 20 %, and accidents at work went down by 18 %. Stress management is still a good way to lower stress and make things safer, even though it’s not quite as effective as awareness training. Figure 6 shows how measures have affected stress levels, adherence to safety rules, and fewer accidents over time.
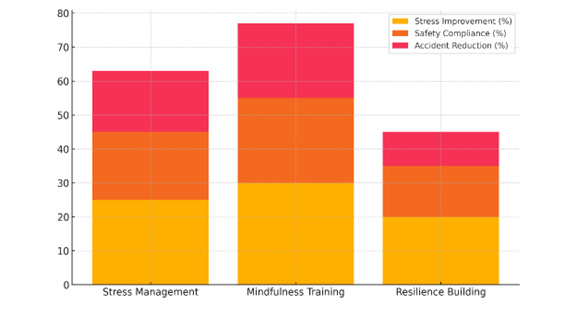
Figure 6. Cumulative Impact of Interventions on Stress Levels, Safety Compliance, and Accident Reduction
Even though resilience-building programs worked, they didn’t show as much growth. Stress levels went down by 20 % after the action, safety compliance went up by 15 %, and accidents at work went down by 10 %. Even though it might not have as big of an impact, resilience training is still a big part of building mental strength and making people safer.
CONCLUSIONS
This study shows that treatments for mental health have a big effect on job safety. This emphasises the need of handling mental health problems at the workplace. Good approaches to help employees with their mental health are mindfulness programs, resilience training, and stress management. This thus enhances safety performance and reduces the possibility of mishaps and injuries. Participating in these initiatives helped individuals better regulate their emotions, focus, and behaviour at work, thereby improving the workplace safety. The findings conform to earlier studies stressing the crucial link between mental health and safety conduct. By reducing stress, worry, and burnout, behavioural health therapies enable employees to manage their emotions, make better decisions, and follow safety guidelines. Less accidents at the workplace follow from this ultimately. Businesses which invest in these initiatives also claim that their employees are more engaged, happy with their employment, and have better quality of living. These elements taken together assist the workplace to be more efficient and useful. Good outcomes notwithstanding, there are challenges in persuading more patients to use behavioural health treatments. Still major issues remain organisational resistance, the stigma and discrimination around mental health, and a dearth of tools and funds. It can also be hard to figure out how successful and profitable these efforts are because the benefits often take time to show up and aren’t always easy to measure. Still, the growing amount of data that shows a connection between mental health and safety highlights the need for businesses to make mental health programs a top priority as part of their total safety plan. To get around these problems, businesses need to create an open attitude about mental health so that workers feel supported and are urged to get help when they need it. For behavioural health treatments to work, there needs to be clear information about their benefits and a promise to provide enough resources. Creating strong measures to check how well these programs work will also help companies see what they do and show how important it is to invest in their employees’ mental health.
BIBLIOGRAPHIC REFERENCES
1. Dyreborg, J.; Lipscomb, H.J.; Nielsen, K.; Törner, M.; Rasmussen, K.; Frydendall, K.B.; Bay, H.; Gensby, U.; Bengtsen, E.; Guldenmund, F.; et al. Safety interventions for the prevention of accidents at work: A systematic review. Campbell Syst. Rev. 2022, 18, 1234.
2. Webb, T.; Joseph, J.; Yardley, L.; Michie, S. Using the internet to promote health behaviour change: A systematic review and meta-analysis of the impact of theoretical basis, use of behaviour change techniques, and model of delivery on efficacy. J. Med. Internet Res. 2010, 12, e1376.
3. Candia Acosta MD, Jousson Ayala DA, Melgarejo Fretes RD. Epidemiological Characterization of Chikungunya Infection in Pediatric Patients, Pilar 2023. Scientific Journal Care & Tech. 2023; 1(1):9-20
4. Kerr, M.J.; Savik, K.; Monsen, K.A.; Lusk, S.L. Effectiveness of computer-based tailoring versus targeting to promote use of hearing protection. Can. J. Nurs. Res. Arch. 2007, 39, 80–97.
5. Glanz, K.; Bishop, D.B. The role of behavioral science theory in development and implementation of public health interventions. Annu. Rev. Public Health 2010, 31, 399–418.
6. Milton, A.C.; Mullan, B.A. An application of the theory of planned behavior—A randomized controlled food safety pilot intervention for young adults. Health Psychol. 2012, 31, 250. [Google Scholar] [PubMed]
7. Guerrero Martines CM. Adherence of Chronic Renal Patients to their Hemodialysis Treatment. Scientific Journal Care & Tech. 2023;1(1):35-52.
8. Kothe, E.J.; Mullan, B.A.; Butow, P. Promoting fruit and vegetable consumption. Testing an intervention based on the theory of planned behaviour. Appetite 2012, 58, 997–1004. [Google Scholar] [PubMed]
9. Sainsbury, K.; Mullan, B.; Sharpe, L. A randomized controlled trial of an online intervention to improve gluten-free diet adherence in celiac disease. Off. J. Am. Coll. Gastroenterol. ACG 2013, 108, 811–817.
10. Negrete Escanor RA. Cardiovascular Risk Factors and Warning Signs. Scientific Journal Care & Tech. 2023;1(1):80-95.
11. Hardeman, W.; Johnston, M.; Johnston, D.; Bonetti, D.; Wareham, N.; Kinmonth, A.L. Application of the theory of planned behaviour in behaviour change interventions: A systematic review. Psychol. Health 2002, 17, 123–158.
12. Skowron-Grabowska, B.; Sobociński, M.D. Behaviour-based safety (BBS)-advantages and criticism. Prod. Eng. Arch. 2018, 20, 12–15.
13. Nahrgang, J.D.; Morgeson, F.P.; Hofmann, D.A. Safety at work: A meta-analytic investigation of the link between job demands, job resources, burnout, engagement, and safety outcomes. J. Appl. Psychol. 2011, 96, 71.
14. Mendieta Castro LF. Experience of type 2 diabetes patients in treatment adherence: a literature review. Scientific Journal Care & Tech. 2023;1(1):21-34
15. Fabiano, B.; Pettinato, M.; Currò, F.; Reverberi, A.P. A field study on human factor and safety performances in a downstream oil industry. Saf. Sci. 2022, 153, 105795.
16. Yassi, A.; Lockhart, K.; Sykes, M.; Buck, B.; Stime, B.; Spiegel, J.M. Effectiveness of joint health and safety committees: A realist review. Am. J. Ind. Med. 2013, 56, 424–438.
17. Caffaro, F.; Cremasco, M.M.; Bagagiolo, G.; Vigoroso, L.; Cavallo, E. Effectiveness of occupational safety and health training for migrant farmworkers: A scoping review. Public Health 2018, 160, 10–17.
18. Vysokolan Corrales GA, Achucarro Galeano S. Perception of Nursing Postgraduate Students on the eLearning Model. Scientific Journal Care & Tech. 2023;1(1):53-79.
19. DeRoo, L.A.; Rautiainen, R.H. A systematic review of farm safety interventions. Am. J. Prev. Med. 2000, 18, 51–62.
20. Feltner, C.; Peterson, K.; Palmieri Weber, R.; Cluff, L.; Coker-Schwimmer, E.; Viswanathan, M.; Lohr, K.N. The effectiveness of Total worker health interventions: A systematic review for a National Institutes of Health pathways to prevention workshop. Ann. Intern. Med. 2016, 165, 262–269.
FINANCING
None.
CONFLICT OF INTEREST
None.
AUTHORSHIP CONTRIBUTION
Conceptualization: Deepak Kumar Parhi, Pooja Varma, Archana Singh, S. A. Surale-Patil.
Data curation: Deepak Kumar Parhi, Pooja Varma, Archana Singh, S. A. Surale-Patil.
Formal analysis: Deepak Kumar Parhi, Pooja Varma, Archana Singh, S. A. Surale-Patil.
Drafting - original draft: Deepak Kumar Parhi, Pooja Varma, Archana Singh, S. A. Surale-Patil.
Writing - proofreading and editing: Deepak Kumar Parhi, Pooja Varma, Archana Singh, S. A. Surale-Patil.