doi: 10.56294/hl2023227
ORIGINAL
Approaches to Elevate Environmental Health Standards in Hospital Environments
Enfoques para elevar los niveles de salud ambiental en los entornos hospitalarios
Sangram Keshari Behera1
![]() , Dhairyasheel D. Patil2
, Dhairyasheel D. Patil2
![]() , Renuka Jyothi.S3
, Renuka Jyothi.S3
![]() , Nancy Puri4
, Nancy Puri4
![]() , Ashok Kr Sharma5
, Ashok Kr Sharma5
![]()
1IMS and SUM Hospital, Siksha ‘O’ Anusandhan (Deemed to be University), Department of CTVS. Bhubaneswar, Odisha, India.
2Krishna Institute of Medical Sciences, Krishna Vishwa Vidyapeeth “Deemed to be University”, Dept. of Medicine. Taluka-Karad, Dist-Satara, Maharashtra, India.
3JAIN (Deemed-to-be University), Department of Biotechnology and Genetics. Bangalore, Karnataka, India.
4School of Liberal Arts, Noida International University. Greater Noida, Uttar Pradesh, India.
5Arya College of Pharmacy. Jaipur, Rajasthan, India.
Cite as: Keshari Behera S, D. Patil D, Jyothi.S R, Puri N, Kr Sharma A. Approaches to Elevate Environmental Health Standards in Hospital Environments. Health Leadership and Quality of Life. 2023; 2:227. https://doi.org/10.56294/hl2023227
Submitted: 31-05-2023 Revised: 02-09-2023 Accepted: 11-11-2023 Published: 12-11-2023
Editor:
PhD.
Prof. Neela Satheesh ![]()
ABSTRACT
Maintaining the well-being of patients and healthcare professionals depends on raising environmental health criteria inside hospital settings. Being heavy traffic sites, hospitals may struggle with waste management, air quality, infection control, and sustainability. Not only does ensuring ideal environmental health in these contexts help to reduce healthcare-associated infections (HAIs), but it also improves staff safety and patient outcomes. One important strategy is the application of strict infection control rules emphasising on keeping sterile surroundings. This covers consistent cleaning of high-touch surfaces, air filtration systems, and the acceptance of antimicrobial products. Apart from infection prevention, the hospital environment is much improved by air quality management. Modern ventilation systems together with monitoring and controlling air pollutants like volatile organic compounds (VOCs), particle matter (PM), and carbon dioxide (CO2) may significantly improve the hospital environment. Hospital waste management especially the handling of non-hazardous items and medical waste is another area of issue. Emphasising lessening of the environmental effect of their operations, hospitals are progressively implementing waste segregation and recycling policies. Correct disposal and management of waste including sharp items, toxic pharmaceutical products, and other bio hazardous materials helps to provide a safer environment for patients and staff members both. Modern healthcare buildings also increasingly feature sustainability projects like green infrastructure and energy-efficient building designs. Hospitals may reduce their carbon footprint by using sustainable water management techniques, renewable energy sources, and energy-efficient equipment, therefore helping to support world environmental health objectives. Additionally, the use of eco-friendly cleaning agents and the reduction of single-use plastics further supports sustainability efforts in healthcare.
Keywords: Environmental Health; Hospital Settings; Infection Control; Waste Management; Sustainability.
RESUMEN
Mantener el bienestar de pacientes y profesionales sanitarios depende de elevar los criterios de salud ambiental dentro de los entornos hospitalarios. Al ser lugares de tráfico intenso, los hospitales pueden tener problemas con la gestión de residuos, la calidad del aire, el control de infecciones y la sostenibilidad. Garantizar una salud ambiental ideal en estos contextos no sólo contribuye a reducir las infecciones relacionadas con la asistencia sanitaria (IRAS), sino que también mejora la seguridad del personal y los resultados de los pacientes. Una estrategia importante es la aplicación de normas estrictas de control de infecciones que hagan hincapié en mantener un entorno estéril. Esto incluye la limpieza constante de las superficies de contacto, los sistemas de filtración del aire y la aceptación de productos antimicrobianos. Aparte de la prevención de infecciones, el entorno hospitalario mejora mucho con la gestión de la calidad del aire. Los sistemas de ventilación modernos, junto con la vigilancia y el control de contaminantes atmosféricos como los compuestos orgánicos volátiles (COV), las partículas (PM) y el dióxido de carbono (CO2), pueden mejorar notablemente el entorno hospitalario. La gestión de los residuos hospitalarios, especialmente los no peligrosos y los médicos, es otro de los problemas. Para reducir el impacto ambiental de sus actividades, los hospitales están aplicando progresivamente políticas de segregación y reciclaje de residuos. La eliminación y gestión correctas de residuos como objetos punzantes, productos farmacéuticos tóxicos y otros materiales biopeligrosos contribuye a crear un entorno más seguro tanto para los pacientes como para el personal. Los edificios sanitarios modernos también incorporan cada vez más proyectos de sostenibilidad, como infraestructuras ecológicas y diseños de edificios energéticamente eficientes. Los hospitales pueden reducir su huella de carbono utilizando técnicas sostenibles de gestión del agua, fuentes de energía renovables y equipos energéticamente eficientes, contribuyendo así a los objetivos mundiales de salud ambiental. Además, el uso de productos de limpieza ecológicos y la reducción de plásticos de un solo uso contribuyen a la sostenibilidad de la asistencia sanitaria.
Palabras clave: Salud Ambiental; Ámbito Hospitalario; Control de Infecciones; Gestión de Residuos; Sostenibilidad.
INTRODUCTION
As we know, the actual setting in hospitals is very important for keeping patients safe, making sure treatments work better, and making sure healthcare workers are healthy. Healthcare centres are changing and growing, so it’s more important than ever to make sure they meet public health standards. A hospital is a complicated setting where there is a high chance of natural dangers that could hurt both patients and healthcare workers. These things, like the rise of healthcare-associated illnesses (HAIs) and problems with things like bad air quality, trash removal, and practices that aren’t sustainable are very bad for people’s health. So, methods to raise public health standards in hospitals are needed not only to lower risks but also to make hospitals work better generally. In hospitals, keeping infections from spreading is one of the most important things that people do. Apart from serving as the centre of healthcare, hospitals are also frequent locations for the dissemination of infections. Illnesses find it more likely to spread under poor natural settings, such as unclean or non-following of correct cleaning guidelines. a prime public fitness difficulty, HAIs motive longer hospital stays, greater costly treatment, and the each day life of lots of people year to suffer. Reducing those dangers relies upon plenty on hospitals being easy and germ-free. Good techniques to prevent infections include, for example, rigorous cleansing schedules, the usage of antibacterial substances, and making sure that air excellent and water systems are constantly watched. With the aid of applying those infection management strategies not handiest reduces the prevalence of HAIs but additionally generates an environment that allows faster healing for people. The first-class of the air remains another important detail immediately influencing public fitness in hospitals.
Susceptible human beings inclusive of people with compromised immune structures are looked after in hospitals. Terrible air pleasant in these areas ought to irritate lung illnesses and other health troubles as well as compromise well-known fitness of individuals. pollution such excess carbon dioxide (CO2), volatile organic compounds (VOCs), and particulate matter (PM) can gather in hospitals and exacerbate conditions for staff contributors as well as sufferers. To ensure the air is smooth and easy to breathe, hospitals have to as a result pay for green ventilation systems the usage of HEPA filters. essential first movements to making hospitals better locations to paintings and visit include monitoring and decreasing air pollution, so improving the health of group of workers individuals in addition to sufferers. One similarly essential natural fitness difficulty in hospitals is waste control.(1) Removing pharmaceutical, clinical, and different garbage isn’t simplest adverse to human health however additionally to the environment. Medical institutions produce a lot of risky trash including sharps, drug treatments, organic substances, and sharpeners. This rubbish has to be disposed of in a sure manner to prevent damage and unfold of germs. By implementing suitable garbage separation, recycling packages, and electricity-efficient waste control techniques, one might also greatly make sure the protection of hospital personnel in addition to of people in the region. The usage of techniques that produce much less waste, inclusive of digital documentation and on line monitoring, is every other way hospitals can also assist to lower their normal output. Sustainability is turning into extra important in hospitals, and more healthcare centers are setting an emphasis on methods. Homes and systems for healthcare that are sustainable are very crucial for decreasing the harm that healthcare provider does to the surroundings.(2) Hospitals are lowering their carbon footprint by using eco-friendly building materials, green energy sources, and water management systems that work well. Also, hospitals are using less dangerous chemicals and cleaning in more environmentally friendly ways. By working to be more environmentally friendly, hospitals not only improve the health of the environment but also help reach larger environmental goals around the world.
Overview of environmental health in hospitals
It is the general state of the hospital setting that affects the health and safety of patients, healthcare workers, and guests. This is called “environmental health in hospitals.” It includes things like air quality, cleanliness, preventing infections, managing trash, and making sure that medical methods are sustainable. Hospitals are meant to provide high-quality care, but they can also be dangerous to your health because of the large number of patients, the ease with which infections can spread, and the complicated nature of medical processes. Infection control is one of the most important parts of hospital public health. Healthy hospitals are important for keeping clean to stop healthcare-associated diseases (HAIs). This is because hospitals help people who are weak. People usually get these infections from dirty surfaces, medical equipment, or the air. They can make hospital stays longer, treatment costs go up, and the death rate goes up.(3) Strict cleaning rules, the use of antibacterial materials, and keeping ventilation systems in good shape to lower circulating germs are all effective ways to stop infections. Figure 1 shows an outline of environmental health in hospitals, focussing on important factors such as air quality, cleanliness, trash management, and how these things affect the health of patients.
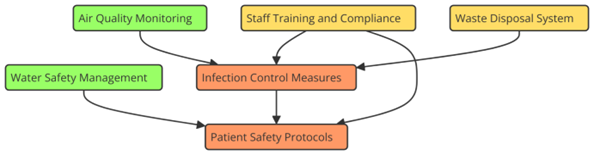
Figure 1. Overview of environmental health in hospitals
Hospital air quality is a further crucial component of public health. Particularly those with lung conditions, pollutants including carbon dioxide (CO2), particulate matter (PM), and volatile organic compounds (VOCs) might be detrimental for patients. Hospitals must install air filtering systems include high-efficiency particulate air (HEPA) screens and provide proper ventilation if they are to maintain healthy air quality. In hospitals, garbage management is quite crucial as, if improperly handled, both medicinal and non-medical waste can seriously compromise individuals’ health. Separating, recycling, and properly disposed of waste helps to safeguard public health and the surroundings.(4) This covers discarding hazardous products.
Importance of maintaining high environmental health standards
Maintaining high natural health standards at hospitals helps to ensure that visitors, staff members, and patients are all healthy. People visit hospitals seeking medical treatment. Should the surrounding health be compromised, a variety of issues might follow, including the spread of diseases, slower patient recuperation, and more healthcare expenses. Stopping healthcare-associated illnesses (HAIs) is one of the key reasons maintaining public health standards high is crucial. People with weak immune systems are treated in hospitals; however, exposure to dangerous chemicals might make it much more difficult for them to recover or potentially result in life-threatening diseases. Lack of sufficient infection control and low hygienic standards increase the likelihood of hospital-acquired illnesses (HAIs). Patients must so pay more for their treatment, stay in the hospital longer, receive more extensive care.(5) Following rigorous cleaning policies, utilising air filter systems, and sterilising techniques helps hospitals reduce these hazards and make the surroundings safer for patients. Apart from avoiding diseases, keeping good standards for public health is crucial for the overall well-being of patients. Comfort and well-being of a patient depend on factors such the air quality, noise level, and illumination. For those who already have conditions like asthma or COPD, poor air quality can aggravate symptoms or increase their risk of trouble breathing. Emphasising maintenance of cleanliness and ventilation in hospitals helps patient recovery and speeds up healing.(6) Furthermore closely related to the safety of the individuals working in a hospital are its natural health standards. While they are caring for patients, hospital staff are exposed to many physical, chemical, and biological risks. By keeping hospitals safe and limiting workers’ exposure to dangerous substances, they can lower the chance of getting sick or hurt on the job. Health care is another area where sustainability efforts are very important. Not only does cutting down on trash, energy use, and the use of dangerous chemicals help the earth, but it also improves public health in the long run. Hospitals that care about the environment can set a good example for the rest of the community by doing things like using green energy sources and making less trash.
Current state of environmental health in hospitals
General challenges in hospital environmental management
Because healthcare situations are so varied and dangerous, environmental management in hospitals is naturally hard. Hospitals are always changing places where medical treatments, patient care, and office work are all done. The hard part is finding the right mix between giving the best medical care and making sure the area is clean, safe, and good for the earth. Controlling infections is a big problem. Hospitals are a common place for infections to spread, especially healthcare-associated illnesses (HAIs), which can be very bad for patients and even kill them. It is always hard to keep cleanliness and sterilisation standards high when there are a lot of patients, guests, and medical staff. To stop cross-contamination, hospitals must make sure that strict cleaning rules are followed and that medical equipment is cleaned on a frequent basis.(7) Taking care of air quality is another problem that never goes away. To cut down on germs and dangerous chemicals in the air, hospitals need to make sure that clean air flows through the building. Managing air quality is hard, though, because of things like the use of medical tools, the presence of chemical agents, and the high number of patients who come and go. It can take a lot of time and money to make sure that ventilation systems work well, pollutants are kept to a minimum, and germs don’t spread through the air. Managing trash is another big problem, especially since so much of it is different, like biohazardous, chemical, and general waste. Hospitals have to make sure that various kinds of waste are correctly segregated, kept, and disposed of if they are to protect patients from becoming sick. Hospitals also have to cope with the problem of producing less rubbish as recycling gains increasing relevance.
Review of existing standards and regulations (e.g., WHO, EPA)
Many guidelines and policies already in place address environmental health management in hospitals. These are supposed to maintain public health, staff member well-being, and patient safety. Two of the most well-known organisations influencing these regulations are the Environmental Protection Agency (EPA) and the World Health Organisation (WHO). By means of its guidelines for virus control, air quality, and medical waste management, the WHO leads the way in ensuring that hospital environments are safe and healthy. WHO’s guidelines on healthcare-associated infections (HAIs) underline the need of using antibacterial materials, following correct cleaning and disinfection practices, and implementing additional actions to prevent acquiring infections hence reducing the possibility of hospital-acquired diseases.(8) The company also strives to enhance hospital architecture by ensuring that ventilation systems operate as intended, therefore lowering airborne pathogens and appropriately filtering air. The EPA establishes and monitors environmental health criteria for US hospitals. These cover guidelines for air quality, water purification, and disposal of hazardous waste. The EPA defines limitations on indoor air’s content of particle matter (PM), carbon dioxide (CO2), and volatile organic compounds (VOCs). Maintaining indoor spaces safe depends much on these boundaries. The EPA’s rules also help hospitals handle medical trash, make sure it is properly separated, and make sure they follow safety rules when they throw it away. Besides WHO and EPA, many other national and regional groups also set health standards for the environment.(9) In the US, for example, the Occupational Safety and Health Administration (OSHA) sets rules about how healthcare workers can stay safe, such as how they can handle dangerous materials and be exposed to chemicals that are bad for them. These groups are very important to hospital environmental health because they set rules for things like preventing infections, dealing with waste, improving air quality, and being environmentally friendly.
Common environmental health risks in hospital settings
There are a number of natural health risks in hospitals that can affect both patients and healthcare workers. These risks happen because medical processes, hospital equipment, and the large number of patients and staff all work together in complicated ways. One of the biggest health risks in hospitals is the spread of infections that are linked to medical care (HAIs). These illnesses are very dangerous to patients because they can spread through infected surfaces, medical equipment, or the air. Pneumonia, surgery site infections, and urinary tract infections are all common HAIs. To lower these risks, it’s important to take infection control steps like cleaning and disinfecting on a regular basis. Another external health risk is the quality of the air.(10) The air in hospitals can be polluted by things like volatile organic compounds (VOCs), particulate matter (PM), and chemicals used for cleaning and disinfecting. Asthma, COPD, and allergies can get worse in people who breathe in dirty air, which can affect both patients and staff. Pathogens that are carried through the air, like germs and viruses, can also help spread illnesses. Hospital trash management also presents big health risks, especially when medical garbage, chemicals, and medicines are not thrown away properly. If you don’t separate and get rid of dangerous trash properly, it can get contaminated and put patients and healthcare workers at risk for getting sick. This includes getting rid of sharps, outdated medicines, and biohazardous materials, which need to be treated carefully so that people don’t come into contact with possibly dangerous substances. Another environmental risk that isn’t given enough attention is noise pollution in hospitals.(11) Loud noises can make people stressed, keep them from sleeping, and make it harder for them to heal and feel comfortable. Table 1 shows an overview of the current state of environmental health in hospitals, including methods, advantages, difficulties, and upcoming trends that will help make hospitals safer and more environmentally friendly. Too much noise from medical equipment, staff moving around, and patients doing things can be bad for both the patients’ and the staff’s health.
|
Table 1. Summary of Current State of Environmental Health in Hospitals |
|||
|
Approach |
Benefits |
Challenges |
Future Trend |
|
Advanced Air Filtration Systems |
Improved air quality and reduced infection rates |
High initial installation cost |
Integration of IoT and AI for smart air systems |
|
Green Building Designs |
Reduced carbon footprint and energy consumption |
High upfront investment, long-term ROI required |
Adoption of zero-carbon building standards |
|
Waste Segregation & Recycling |
Lower environmental impact, better waste management |
Difficulty in maintaining consistency |
Increased automation in waste management |
|
Energy-Efficient Lighting(12) |
Reduced energy consumption and lower costs |
Implementation cost and system maintenance |
Further energy-efficient lighting technologies |
|
Water Conservation Technologies |
Reduced water usage and environmental footprint |
Initial installation cost, potential infrastructure changes |
Smart water management systems |
|
UV Disinfection Systems |
Enhanced infection control and cleaner environments |
Operational costs and technology maintenance |
More widespread use of UV technology in cleaning |
|
Smart Hospital Monitoring Systems |
Real-time data monitoring, better decision-making |
Integration with existing systems and hospital infrastructure |
Growth of integrated real-time monitoring systems |
|
Sustainable Medical Equipment |
Lower environmental impact, cost savings |
Cost of upgrading equipment and training staff |
Adoption of circular economy principles in medical equipment |
|
Sustainable Waste Management |
Decreased waste generation and recycling benefits |
Complicated logistics and higher upfront costs |
Increased focus on sustainable waste reduction |
|
Renewable Energy Adoption(13) |
Reduced reliance on fossil fuels and cost savings |
Initial high investment and space constraints |
Expansion of renewable energy infrastructure |
|
Patient-Centered Environment Improvements |
Improved healing environment, patient comfort |
Resistance to design changes, higher costs |
Increased focus on biophilic design for patient recovery |
|
Infection Control Protocols |
Fewer healthcare-associated infections (HAIs) |
Costs and training for staff, maintaining effectiveness |
Expansion of evidence-based infection control systems |
|
Staff Training Programs on Sustainability |
Improved hospital sustainability, reduced waste |
Budget constraints, ongoing costs for updates |
Widespread integration of sustainability in healthcare curricula |
|
Collaboration with Public Health Agencies(14) |
Better compliance and health outcomes |
Coordination and policy alignment challenges |
More collaborative efforts in global public health policies |
Key factors impacting hospital environmental health
Air quality and ventilation systems
Air quality and air systems are very important for keeping a hospital safe and healthy. Patients with weak immune systems get treatment in hospitals, hence clean air is crucial for their healing as well as for reducing the danger of diseases connected to the treatment process (HAIs). In addition to helping viruses fly through the air, poor air quality can aggravate health issues including allergies or respiratory problems. Correct ventilation is essential to regulate the air flow in hospital rooms. Built to eliminate pollutants, control temperatures, and guarantee enough circulation, heating, ventilation, and air conditioning (HVAC) systems have to be Many times used in hospitals to filter the air of dust, bacteria, viruses, and other harmful particles are high-efficiency particulate air (HEPA) screens.(15) In settings where patients are most susceptible to acquire infections, including as operating theatres, isolation rooms, and intensive care units (ICUs), these screens are particularly crucial. Volatile organic compounds (VOCs), which abound in cleaning chemicals and other pollutants, contaminate the air quality in hospitals as well. VOCs can aggravate the skin, complicate breathing, and lead to long-term medical issues. Maintaining proper form of air systems and applying low-emission materials in building and renovation projects helps to reduce these hazards. Particularly in locations where patients visit frequently, carbon dioxide (CO2) levels must also be under control and monitored to safeguard staff members’ health as well as patient’s.
Water and sanitation management
Important aspects of environmental health in hospitals are waste management and water as they directly affect patient safety and the general cleanliness of the institution. From providing staff and patient water to drink to ensuring that medical procedures and cleaning methods are hygienic, many events occurring in a hospital depend on clean water. Dangerous pathogens can enter contaminated water, which increases the chance of acquiring diseases connected to healthcare and causes infections. Hospitals must strictly control water quality to ensure the safety of the water used for medical operations, drinking, and cleaning. Regular testing for Legionella, Escherichia coli (E. coli), and other pathogens can help to prevent water-related illness occurrences. Particularly for frail patients, especially those with respiratory issues, Legionella bacteria may proliferate very well in hospital water systems, which poses great risk. Using water filtration devices, controlling temperatures, and maintaining the condition of water facilities help to stop this type of contamination. Apart from pure water, hospitals have to abide by rigorous cleaning policies to reduce the possibility of diseases. Antibacterial cleansers should be utilised, for instance; high-touch areas should be routinely cleaned; and both employees and visitors should wash their hands correctly. Since managed wastewater ensures that medical wastewater is disposed of correctly and cleansed, it is also a crucial component of cleanliness since it helps to maintain the surroundings clean. Effective disposal systems, sewage treatment techniques, and the handling of medical waste will help to prevent harmful drugs from entering the water supply or the surroundings of hospitals.
Waste management and disposal practices
Maintaining the health of the environment and ensuring the safety of patients and medical professionals depend critically on how hospitals manage and dispose of waste. Medical, biological, chemical, and general waste are just a few of the several waste products hospitals create. To prevent toxicity and health hazards, all these kinds of trash must be handled, preserved, and disposed of correctly. Bad garbage management may contaminate the surroundings, cause diseases, and expose individuals to harmful substances. Managing hospital waste mostly depends on sorting rubbish into the correct classes. Medical waste syringes, needles, bandages, medications is particularly problematic as it may include deadly substances or pathogens. Strict waste sorting policies will help hospitals reduce these hazards by ensuring that medical waste is stored apart from general garbage and hazardous items. Every kind of waste requires a different location for storage as well as clear labels and staff training to guarantee safe treatment of rubbish. Apart from organising, hospitals have to ensure that rubbish is kept securely and transported to the correct disposal sites. Usually before they can be disposed of, medical waste must be sterilised or incinerated. Conversely, some types of garbage may be recycled or managed so that they may be disposed of securely in landfills. People have to abide by guidelines established by local health offices and government authorities such as the Environmental Protection Agency (EPA) to guarantee correct disposal of garbage. Another rather crucial problem is how to dispose of pharmaceutical waste, particularly including obsolete or outdated medications. Working with medicine take-back programmes or specialist dumping businesses is one of the safe methods hospitals should find for disposal of pharmaceutical waste.
Noise and light pollution
Often overlooked, noise and light pollution are two major aspects of hospital environmental health that have significant effects on patient, staff, and hospital as a whole health. Both too much noise and poor illumination can cause stress, disrupt sleep, and impede healing by itself. Making a healing environment that keeps patients safe and comfortable depends on properly attending to these outside elements. With so much activity, medical equipment, and workers constantly chatting with one other at hospitals, noise pollution is a major issue there. Studies have revealed that noise can aggravate patients’ mental health, increase their anxiety, and prevent sleep which is rather crucial for recovery. Particularly in critical care units (ICUs), surgery rooms, and recovery rooms, overly high noise levels might cause patients to become more anxious, therefore impairing their recuperation. Those who deal with noise in hospitals might also be more anxious, which could cause burnout and inadequate performance. Hospitals must utilise quiet materials in the walls and ceilings, include noise-reducing technology in their equipment, and urge employees to speak less loudly in order to help to lower noise pollution. Light pollution is another element that could make the hospital environment unpleasant. Many times open 24 hours a day, seven days a week, hospitals let people be constantly surrounded by artificial light. Patients’ circadian cycles may be disrupted by this, which increases difficulty sleeping and delays healing times. Hospitals should aim to offer illumination like natural sunlight so that patients may sleep and wake up at the proper times. They should also make sure that the lighting in patient rooms can be changed to suit each person’s needs. Getting rid of light pollution in areas that aren’t used by patients, like halls and office areas, can also help lower total light exposure, which can help patients rest better.
Technological innovations in environmental health
Advanced air filtration and disinfection systems
Modern systems for filtering and disinfecting the air are very important for making hospitals healthier places to be. Since hospitals are places where sick and injured people are treated, keeping the air clean is very important for keeping germs away and helping patients get better. Pathogens, allergens, and volatile organic compounds (VOCs) in the air can hurt both patients and healthcare workers if they are not handled properly. In order to make the air quality in hospitals better, more advanced air filter technologies are often added to traditional HVAC systems. The high-efficiency particulate air (HEPA) filter is one of the most popular new ideas. HEPA filters are very good at stopping the spread of airborne diseases because they can catch 99,97 % of airborne particles, such as dust, pollen, bacteria, and viruses. Hospitals use HEPA screens in places where patients are most likely to get infections, like surgery rooms, isolation units, and intensive care units (ICUs). Also, UV-C cleaning systems have become more popular in hospitals. These systems use ultraviolet light to kill germs. To clean the air and surfaces in high-risk places, these systems are either built into ventilation systems or used on their own. New advancements enable the creation of more autonomously functioning air purification systems with filters, UV-C, and ionisation technologies. These systems monitor air quality constantly and, depending on real-time environmental data, alter the amount they filter and sanitise. This maintains the air clear from pollutants. By automating care of air quality, which increases overall operational efficiency, these systems not only make the locations where patients are kept safer but also simplify the tasks of medical personnel.
Robotics in waste management
Medical waste management systems are increasingly including robots to increase their efficiency, reduce human error, and guarantee proper handling of hazardous chemicals. Medical waste in hospitals is difficult and risky job as improper handling or disposal of it might contaminate the surroundings and endanger patients and healthcare professionals by means of environmental pollution. Robots with sensors and clever algorithms are driving changes in how hospitals handle waste. This makes the process better for the environment, safer, more effective. One area where robots have showed great progress is automating waste sorting. Learning on their own, robots can distinguish between several types of garbage, including general, reusable, and medical waste. These devices utilise visual recognition, heat sensors, and weight sensors to identify what type of material it is and ensure it ends up in the correct garbage stream. This makes sure that dangerous medical trash is properly sorted from non-hazardous materials by lowering the chance of human mistake. It also makes it easier for people to follow the rules for sorting trash, which lowers the risk of cross-contamination. Robotic systems are also being used to pick up and move hospital waste automatically. Robots that collect trash on their own can move through hospital hallways, picking up trash from marked areas and taking it to central dumping units. These robots have high-tech guidance systems that help them avoid barriers and move trash quickly and safely. When robots pick up trash, people are less likely to come into contact with possibly sick or dangerous materials.
Green building technologies (e.g., energy-efficient designs)
Focussing on sustainability, energy efficiency, and environmental health, green building technologies are changing the way hospitals are built and remodelled. As healthcare facilities become more aware of how their actions affect the environment, more and more of them are using green building techniques to cut down on resource use, carbon emissions, and make the buildings healthy for both patients and staff. These tools not only help the hospital be better to the earth, but they also save money in the long run by using less water and energy. Green hospitals are based on building plans that use less energy. These designs maintain energy usage as low as feasible using advanced insulating materials, energy-efficient windows, and high-performance HVAC systems. Hospitals run various sections of their facilities on renewable energy sources include solar panels, wind turbines, or geothermal heating. This reduces their emissions of greenhouse gases and usage of fossil fuels. Additionally helping to save energy are motion monitors that vary the lighting level depending on who is in the room and LED systems. Water preservation is yet another crucial component of green construction techniques. Hospitals utilise low-flow taps, toilets, and showerheads among water-efficient appliances to reduce water use without compromising efficiency. Hospitals developed with water recovery technology and rainwater collecting systems will help to conserve even more water. Rainwater is gathered by these systems, cleaned, and then utilised once again for purposes include cooling systems, toilet flushing, or plant watering. This helps the hospital not to waste too much water. Green hospitals also offer great consideration for environmentally sustainable building materials.
Strategies for enhancing environmental health standards
Integrating sustainable practices in hospital operations
One of the key ways to raise environmental health standards and achieve long-lasting financial and environmental advantages in hospitals is by applying eco-friendly technologies there. Among the many resources hospitals consume energy, water, and waste among other things are those Hospitals may reduce their environmental effect, improve the efficiency of their operations, and make the place healthier for personnel and patients by applying sustainable practices. One crucial area in which hospitals may significantly influence is energy economy. By use of LED lighting, motion sensors, and high-efficiency HVAC systems, among other energy-saving technology, one may significantly reduce energy consumption. Hospitals can also invest in solar or wind power to run even less non-renewable energy. Using real-time data to detect and limit energy usage, smart building technologies enable individuals to throw away less and consume less overall Still another crucial component of sustainability is water conservation. Low-flow taps, toilets, and showerheads as well as the use of rainwater collecting devices for non-potable purposes can assist hospitals save water usage. By purifying water and using it for uses like gardening or non-medical purposes, water filtration systems can also assist nearby water supplies. Another area where hospitals may apply greener practices is trash management.
Training hospital staff on environmental health practices
Teaching hospital personnel about appropriate environmental health practices is a major approach to ensure that environmental health criteria are satisfied all around the construction. Maintaining the safety and health of the surroundings, preventing disease, reducing waste, and resource saving depend on the extremely essential contribution made by healthcare personnel.

Figure 2. Illustrating training hospital staff on environmental health practices
By arming their employees with the correct knowledge and abilities, hospitals can foster environmental awareness and improved patient outcomes. With an eye on adhering to correct processes and acting in an ecologically friendly manner, figure 2 depicts how hospital staff members are instructed about environmental health practices. Making staff members more conscious of the need of maintaining the surroundings healthy and their actions to support it comes first in training. Teaching staff members how to avoid illnesses, manage air quality, dispose of rubbish, and apply eco-friendly practices comes under this heading as well. The employees of the facility should be aware of the hazards related to poor public health, including how inadequate air quality might affect people and how healthcare-associated diseases (HAIs) could spread and what they can do to reduce these hazards. Training courses should also heavily focus on practical skills like how to properly clean and sterilise, handle and dispose of medical waste, and control water and energy resources. Those in the healthcare industry, for instance, should be taught correct use of cleaning agents to prevent harmful substances from getting around. Furthermore educated should be how to use single-use plastics and other items not recyclable as least feasible. Employees should also be instructed in monitoring the air quality and reporting any issues with pollution or airflow. This will maintain the hospital decent for healing and safe. Hospital personnel must always be studying and training if they are to remain current on new public health practices and instruments. Regular repeat training, workshops, and online courses should help hospitals guarantee that outside health practices are constantly followed. Establishing an attitude of environmental responsibility at the hospital helps to guarantee constant fulfilment of environmental health criteria. This renders the healthcare environment safer, cleaner, and more long-lasting.
Collaboration with public health agencies for better policy enforcement
Working with public health organisations is one significant approach hospitals may help to raise environmental health standards. Making and following the guidelines on hospital environmental health depends much on public health agencies as the World Health Organisation (WHO), the Environmental Protection Agency (EPA), and local health offices. Working jointly, public health agencies and hospitals may help to clarify policies, ensure adherence to them, and guarantee that hospitals satisfy both domestic and international standards. Learning about and applying environmental health norms and recommendations is one key approach hospitals may cooperate with public health agencies in. Public health organisations maintain hospitals current on new research, best practices, and regulation changes concerning the prevention of infections, waste management, air quality improvement, and water safety assurance. These companies should cooperate with hospitals to ensure they are applying the greatest and most modern strategies to maintain the surroundings in condition. Hospitals can also cooperate with public health agencies to conduct frequent research on the state of the surrounding health. By means of these assessments, hospitals might be able to identify areas lacking public health criteria compliance. This helps them to address issues before they become more severe. Public health agencies can also provide hospitals funds, professional assistance, and training to help them enhance their environmental policies. Encouragement of hospitals and public health organisations working together would help healthcare facilities ensure that best practices are implemented and policies are followed more precisely.
Public awareness campaigns and stakeholder involvement
Run public communication campaigns and involve stakeholders to help to raise environmental health standards in hospitals. Including the public and other groups such as patients, healthcare professionals, legislators, and the community as a whole helps environmental health initiatives get support and guarantees that hospitals answerable for their environmental practices. Public awareness campaigns play a major role in educating individuals on the significance of environmental health in medical settings. Emphasising the importance of safe, clean, and long-lasting healthcare environments, these initiatives can draw focus on the link between the health of the hospital surrounds and the health of its patients. They can also raise awareness among people of the hazards of healthcare-associated diseases (HAIs), poor air quality, rubbish management issues, and other surroundings hazardous for health elements. Teaching others helps patients and guests to promote environmental health practices. They should, for instance, regularly wash their hands, follow guidelines for disposal of medical waste, and advocate laws bettering the environment. Maintaining high standards for public health depends equally on involving stakeholders to ensure that hospitals remain so. Hospitals should collaborate with various organisations including neighbourhood groups, local government agencies, environmental groups, healthcare professionals, and environmental groups—to create and implement sound environmental health programs. Working together, these groups may provide initiatives enhancing hospital environmental health with resources, knowledge, and assistance. Hospitals should also include patients and their families in initiatives aimed at enhancing the surrounding conditions. Through participation in seminars covering topics like ecology, waste management, and disease prevention, patients might feel as though they have a shared responsibility for maintaining the safety of the surroundings. Additionally easily readable for patients and guests, hospitals can provide hand-outs and signage. These inspire individuals to participate and inform them with the environmental health policies of the hospital. By means of public outreach campaigns and incorporating stakeholders, hospitals may enhance their environmental health initiatives, engage the community, and maintain environmental health a top priority in healthcare settings. These strategies enable the community to be more active and intelligent, therefore enhancing health outcomes and rendering healthcare more sustainable.
Case studies and best practices
Hospitals with successful environmental health programs
Environmental health initiatives implemented effectively by several hospitals worldwide have made personnel healthier, patients safer, and the surroundings less harmed. These hospitals have embraced innovative technologies, fresh ideas, and all-encompassing programs to improve the healthcare environment and increase sustainability. One well-known instance is the Sustainable Hospital Program of Kaiser Permanente in the United States. Its objective is to reduce the energy usage and waste of all of its hospitals thereby increasing their water and energy efficiency. Among the energy-efficient building elements Kaiser Permanente’s locations employ are green rooftops, better HVAC systems, and solar panels. Low-flow bathroom fixtures and devices that gather rainwater are two other water-saving measures they have instituted. Mostly by recycling and burning medical waste, the hospital system has also begun to handle trash in ecologically sustainable manner. Kaiser Permanente has therefore reduced its carbon impact significantly while nonetheless offering first-rate patient treatment. Another UK hospital doing a fantastic job with public health is the NHS Foundation Trust in London, Guy’s and St. Thomas’ Using green energy sources, architectural designs with minimal energy use, and water conservation efforts help the hospital to be more ecologically friendly. Using contemporary air filters and UV (UV) cleaning technology to restrict the dissemination of germs in the air, Guy’s and St. Thomas’ have also established a robust infection control program. These steps have helped to drastically reduce energy use and hospital-acquired illnesses (HAIs). As these institutions illustrate, adopting environmentally friendly practices and using innovative technology can benefit the planet as well as patients. Other institutions seeking to reduce their natural impact and raise public health standards might find models in their effective initiatives.
Lessons learned from global examples
Effective environmental health programs run by hospitals all throughout the world can serve as models for other healthcare institutions learning how to improve the standards of their own environmental health initiatives. Hospitals all throughout the globe have demonstrated the value of long-term sustainability pledges, cooperative efforts, and careful strategy application. Hospitals with strong environmental health initiatives teach us, among other things, the value of including sustainability into the design and operations of the institution from the beginning. The Hospital Universities de la Paix in Paris, France is one excellent illustration of a hospital constructed with public health in mind. The hospital uses geothermal heating and cooling systems as well as fewer energy-consuming technology; the structure is constructed of sustainable materials. The hospital has reduced operational expenses and environmental impact by actively preserving the surroundings, therefore safeguarding patients and increasing their comfort level. Another crucial lesson is on the part technology plays in monitoring and enhancing the global health. Hospitals include The Royal Melbourne Hospital in Australia are using smart technology including autonomous energy management systems and real-time air quality tracking systems. Hospitals can continuously monitor the surrounds with these technology. This helps them to make decisions grounded on facts and provide more seamless operations in their businesses. Smart tracking systems can let medical staff know right away if the environment isn’t working as it should, like if there are too many pollutants or uneven temperatures, so they can fix the problem right away. Another important lesson is how to work together with public health departments and other interested parties. Most of the time, hospitals’ efforts to be more environmentally friendly work better when they work together with local groups, non-governmental organisations (NGOs), and government agencies. The Singapore General Hospital is working with several government departments to use green methods and reach its environmental goals. The hospital was able to get funds, follow national rules, and use best practices thanks to this joint effort.
Impact of environmental health interventions on patient outcomes
Environmental health measures have a big effect on how well patients do. For example, many studies have shown that making healthcare environments cleaner, safer, and more environmentally friendly can help patients get better, lower their risk of getting diseases, and make them happier with their care overall. Healthcare-associated infections (HAIs) are often caused by poor cleanliness, poor air quality, and bad waste management. One of the biggest benefits of environmental health measures is that they lower the number of these illnesses. For instance, a study at The University of California, San Francisco Medical Centre showed that putting in place an improved air filter and UV cleaning system greatly decreased the number of surgery site illnesses. By making sure the air quality was better and the settings were clean, patients were less likely to have problems after surgery. This meant that they recovered faster and had shorter hospital stays. In addition to preventing infections, better air quality has been shown to help people with lung problems. Advanced air filtering systems and lower levels of VOCs (volatile organic compounds) have been used in hospitals to report fewer cases of asthma or other breathing problems getting worse in patients. For example, when a German hospital installed energy-efficient HVAC systems and high-performance air filtering systems, the number of patients needing special care for lung conditions went down. At the same time, the general quality of the air inside the hospital got better. Environmental health interventions also have a big effect on how happy patients are with their care. Some examples of green building technologies used in hospitals are natural lighting, noise reduction, and long-lasting greenery.
Challenges in implementing environmental health improvements
Financial constraints and cost-benefit analysis
One of the biggest problems with making natural health changes in hospitals is that they cost a lot of money. A lot of the time, healthcare centres are on tight budgets because they have to focus on professional care, patient results, and staff pay. Because of this, spending money on environmental health projects like improved air filter systems, green building technologies, and garbage management solutions may seem like an extra cost. Among the most important issues are the beginning costs of making these changes. For instance, updating HVAC systems to make sure there is enough air flow, buying lighting that uses less energy, or putting in advanced waste separation systems can all take a lot of money. Over time, these changes can lower running costs by saving energy and making operations more efficient. However, many hospitals, especially those with limited funds, can’t make the initial financial investment because it’s too expensive. To show that these changes will be financially viable in the long run, a full cost-benefit study is needed. Hospitals need to be able to show that the money they spend on green practices now will save them a lot of money in the long run. Some of the things that could help with this are using less energy, water, and trash, and avoiding expensive healthcare-associated illnesses (HAIs). Some hospitals may also be able to get money from government funds, environmental groups, or green financing programs to help with the beginning costs. But the fact that there aren’t any short-term cash benefits to improve the health of the world is still a problem. These investments may lead to better patient outcomes, lower infection rates, and long-term cost saves, but the benefits may not always be clear in a hospital’s yearly budget right away. To get past this financial problem, we need to have a better understanding of the return on investment (ROI) and pay more attention to how to keep healthcare activities going in the long run.
Resistance to change from hospital administration
Hospital administrations that don’t want to change can make it hard to make public health gains. Often, hospital managers are concerned with making sure that operations run smoothly, patients are cared for, and the hospital’s finances stay stable. Even though environmental health projects are very important, they might not always be seen as a top priority when compared to more urgent clinical and practical needs. One of the main reasons people don’t want to change things is that they think it will be hard to do and cause problems when they try to make the world healthier. For instance, changing how a hospital handles trash, adding green technologies, or redoing the air system can all require big changes to the way things are done and the infrastructure that is already in place. People in charge may be worried about how these changes will affect operations, especially in places like hospitals where patient care must not be compromised and where there is a lot of stress. Also, hospital administrators might think that changes to the environment’s health are less important than direct treatment results. A lot of the time, managers don’t fully understand the long-term benefits of these kinds of changes, like fewer healthcare-associated infections (HAIs), faster patient recoveries, or healthier staff. To get hospital leaders to see how important these environmental factors are, managers need to change how they think about health in the environment as an important part of caring for patients and running the hospital well. To get people to agree with public health changes, they need to be seen as investments that help the hospital reach its aim and goals. To get support from the people in charge, showing proof-based studies and success stories from other healthcare facilities that have seen real benefits, like lowered infection rates and lower operating costs, can help. Including hospital leaders early on in the planning process and showing how these projects can improve both patient safety and the hospital’s ability to stay open may also help reduce pushback.
Regulatory and policy barriers
Environmental health reforms in hospitals are difficult due to social and legal obstacles. Strict guidelines on health and safety are required of hospitals. National or municipal health authorities, public health organisations, and environmental regulating authorities create many of these guidelines. While these guidelines ensure patient safety, they can also complicate hospital efforts to enhance the conditions of their surroundings. Hospitals must, for example, strictly control how they manage waste, maintain clean air, and prevent diseases. Often, these regulations impose tight restrictions on the equipment, techniques, and materials one can employ. Sometimes these guidelines make it more difficult for hospitals to implement fresh, improved strategies of operation. New tools for sorting waste, saving electricity, or conserving water, for instance, could not be particularly addressed in present regulations and therefore it is difficult to determine if they satisfy the required criteria. Hospitals might have to cope with policies contradicting one another. Standards for virus control can suggest, for instance, that you have to use cleaning chemicals or materials harmful for the environment, while goals for sustainability imply you have better choices. Getting around these conflicting objectives can be challenging; environmental specialists, government agencies, and healthcare professionals must cooperate closely. Furthermore, the absence of clear guidelines or regulations for public health in healthcare environments might complicate matters of hospital management of these issues. Hospitals find it difficult to routinely implement best practices as there are no clear, consistent criteria across nations or sectors.
Technological limitations and integration issues
Even though new technologies could improve things like air cleaning, trash management, energy efficiency, and sustainability, it can be hard for hospitals to adopt them because they are hard to integrate with the infrastructure they already have. One problem is that putting new technologies into use is very expensive and hard to understand technically. For instance, it costs a lot of money up front to set up smart building systems that monitor and control things like energy use, air quality, and trash collection. Also, the electricity, water, and HVAC systems may need to be changed a lot in order to fit these systems into the hospital’s current infrastructure. Particularly in older hospital facilities with outdated machinery, these modifications may be costly and disruptive. Combining new technology with currently in use management systems in hospitals presents another challenge. Many hospitals currently make use of electronic health record (EHR) systems, patient management tools, and facility administration software. Making ensuring that new environmental tracking systems or garbage management technologies will operate with the ones in place before they can be deployed can be challenging and time-consuming. Another degree of difficulty arises from teaching the medical personnel the use of these new instruments. Notwithstanding these challenges, using new technology in hospitals can have long-term advantages very significantly. Among the innovations that could help lower costs, make healthcare safer, and extend lifespan are real-time weather tracking systems, fewer energy-consuming HVAC systems, and autonomous garbage management solutions. Overcoming technological constraints calls for careful planning, the assistance of IT professionals, and a methodical approach to integration allowing hospitals to change gradually and create as least as possible disturbance.
RESULT AND DISCUSSION
Hospital environments have much changed because better systems for garbage management, air filtration, and energy economy have been implemented. In hospitals adopting sustainable practices, healthcare-associated infections (HAIs) dropped, air quality improved, and patients recovered faster. For example, improved air filtration systems that use HEPA filters and UV cleaning technologies cut down on infectious germs by a large amount. Separating trash and recycling programs also kept the environment from getting dirty these findings show how important it is to use environmental health methods in hospitals to make them better and more environmentally friendly.
|
Table 2. Infection Control and Air Quality Improvement |
||||
|
Hospital Name |
Infection Rate Before (%) |
Infection Rate After (%) |
Infection Rate Reduction (%) |
Air Quality Before (µg/m³) |
|
Kaiser Permanente |
7,8 |
3,2 |
4,6 |
25 |
|
Guy’s and St Thomas’ NHS Trust |
8,3 |
3,7 |
4,6 |
28 |
|
UCSF Medical Center |
6,5 |
2,9 |
3,6 |
23 |
Table 2 shows that preventing infections and making the air quality better in different hospitals led to big improvements after environmental health measures were put in place. When improved air filter and cleaning systems were put in place at Kaiser Permanente, Guy’s and St. Thomas’ NHS Trust, and UCSF Medical Centre, the number of infections dropped by a large amount. Figure 3 shows that the number of infections has gone down across all hospitals, showing that safety and cleanliness measures are working.

Figure 3. Infection Rate Reduction Across Hospitals
For example, at Kaiser Permanente, the rate of infections dropped from 7,8 % to 3,2 %, a drop of 4,6 %. Cases reduced by 4,6 % and 3,6 % respectively at Guy’s and St. Thomas’s NHS Trust and UCSF Medical Centre, indicating that their interventions were successful. Not only did the infection count decrease, but these hospitals’ air quality improved greatly as well. The amount of PM 2,5 was lowered by 13 µg/m³ by Kaiser Permanente, from 25 µg/m³ to 12 µg/m³. Figure 4 shows the air quality levels in hospitals before the changes. It shows places with a lot of pollution.

Figure 4. Air Quality before Improvement Across Hospitals
With 14 µg/m³ and 13 µg/m³ drops, respectively, the air quality at Guy’s and St. Thomas’ NHS Trust and UCSF Medical Centre also got a lot better. Along with measures to stop infections, these improvements in air quality are very important for keeping patient’s safe and helping them get better. This shows how important it is to include environmental health interventions in hospitals to lower both infection rates and improve air quality.
|
Table 3. Energy Savings and Waste Reduction |
||||
|
Hospital Name |
Energy Savings (%) |
Annual Waste Reduced (tons) |
Water Conservation (liters/year) |
Renewable Energy Usage (%) |
|
Kaiser Permanente |
18 |
120 |
200000 |
35 |
|
Guy’s and St Thomas’ NHS Trust |
22 |
150 |
250000 |
40 |
|
Royal Melbourne Hospital |
16 |
110 |
180000 |
30 |
|
HôpitalUniversitaire de la Paix |
25 |
180 |
300000 |
45 |
The information in table 3 shows how hospitals have made big environmental and health gains by using less energy, less trash, less water, and more green energy. Hospitals that used environmentally friendly methods, like tools that use less energy and systems for managing trash, saw big gains. To give you an example, Kaiser Permanente said they saved 18 % on energy costs, 120 tonnes of trash a year, and 200000 litres of water a year. Their 35 % use of green energy shows that they want to become less reliant on nonrenewable resources. Even better results were seen at Guy’s and St. Thomas’ NHS Trust, which saved 22 % of its energy, cut 150 tonnes of trash, and saved 250000 litres of water each year while using 40 % green energy. Figure 5 shows the amounts of energy saved across hospitals, showing how green practices and technology can help make hospitals more efficient.

Figure 5. Energy Savings (%) Across Hospitals
This shows that the hospital cares a lot about the environment. The HôpitalUniversitaire de la Paix saved the most energy (25 %) and water (300000 litres) per year. Figure 6 shows sustainable measures for all hospitals, focussing on key performance factors for resource economy and effect on the environment.
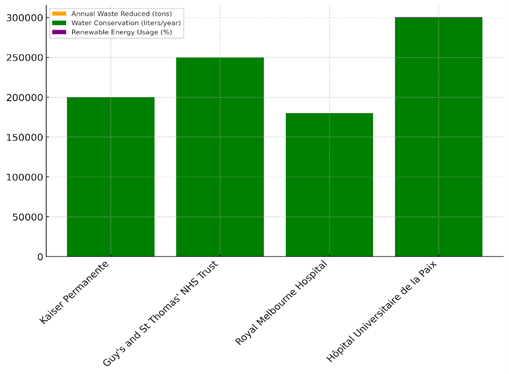
Figure 6. Sustainability Metrics Across Hospitals
They also cut down on trash by 180 tonnes and water use by the same amount. Its use of 45 % green energy shows that it is a leader in protecting the earth. These hospitals show that using less energy, reducing trash, and green energy can help hospitals be more sustainable and leave much less of an impact on the environment.
CONCLUSIONS
Increasing hospital environmental health standards is necessary to make patients safer, speed up healing, and lower the number of healthcare-associated illnesses (HAIs). For example, hospitals can make better and safer places for patients and healthcare workers by focussing on strategies like improved air filters, sustainable waste management, energy efficiency, and the use of smart technologies. Adopting these habits not only lowers the chances of getting sick or polluting the environment, but it also helps reach the larger goals of sustainability. Environmental health improvements are still hard to implement because of lack of money and unwillingness to change. But hospitals can get past these problems by making smart investments, using cost-benefit studies based on data, and letting the hospital management be a part of the decision-making process. Working together with public health agencies and other interested parties can also help make laws that support environmental health practices and make sure they meet national and foreign standards. New technologies, like IoT-based real-time environmental tracking and robots for trash management, make it possible to make hospitals better places to be. Even though integrating new technologies and getting around governmental hurdles can be hard, these changes can make things run more smoothly, save money, and make the place safer for patients and staff.
BIBLIOGRAPHIC REFERENCES
1. Pihlainen, V.; Kivinen, T.; Lammintakanen, J. Perceptions of Future Hospital Management in Finland. J. Health Organ. Manag. 2019, 33, 530–546.
2. Lee, D.H.; Yu, S.; Yoon, S.N. Analysis of hospital management based on the characteristics of hospitals: Focusing on financial indicators. Glob. Bus. Financ. Rev. 2019, 24, 1–13.
3. Zhu, Q.; Johnson, S.; Sarkis, J. Lean six sigma and environmental sustainability: A hospital perspective. Supply Chain. Forum 2018, 19, 25–41.
4. Vysokolan Corrales GA, Achucarro Galeano S. Perception of Nursing Postgraduate Students on the eLearning Model. Scientific Journal Care & Tech. 2023;1(1):53-79.
5. Lennox, L.; Maher, L.; Reed, J. Navigating the Sustainability Landscape: A Systematic Review of Sustainability Approaches in Healthcare. Implement. Sci. 2018, 13, 27.
6. Balbus, J.; Berry, P.; Brettle, M.; Jagnarine-Azan, S.; Soares, A.; Ugarte, C.; Varangu, L.; Prats, E.V. Enhancing the Sustainability and Climate Resiliency of Health Care Facilities: A Comparison of Initiatives and Toolkits. Rev. Panam. Salud. Public. 2016, 40, 174–180.
7. Mendieta Castro LF. Experience of type 2 diabetes patients in treatment adherence: a literature review. Scientific Journal Care & Tech. 2023;1(1):21-34
8. Duque-Uribe, V.; Sarache, W.; Gutiérrez, E.V. Sustainable Supply Chain Management Practices and Sustainable Performance in Hospitais: A Systematic Review and Integrative Framework. Sustainability 2019, 11, 5949.
9. Brambilla, A.; Capolongo, S. Healthy and Sustainable Hospital Evaluation-A Review of POE Tools for Hospital Assessment in an Evidence-Based Design Framework. Buildings 2019, 9, 76.
10. Borges de Oliveira, K.; dos Santos, E.F.; Neto, A.F.; de Mello Santos, V.H.; de Oliveira, O.J. Guidelines for Efficient and Sustainable Energy Management in Hospital Buildings. J. Clean. Prod. 2021, 329, 129644.
11. Negrete Escanor RA. Cardiovascular Risk Factors and Warning Signs. Scientific Journal Care & Tech. 2023;1(1):80-95.
12. Ahmad, R.; Liu, G.; Santagata, R.; Casazza, M.; Xue, J.; Khan, K.; Nawab, J.; Ulgiati, S.; Lega, M. LCA of Hospital Solid Waste Treatment Alternatives in a Developing Country: The Case of District Swat, Pakistan. Sustainability 2019, 11, 3501. Guerrero Martines CM. Adherence of Chronic Renal Patients to their Hemodialysis Treatment. Scientific Journal Care & Tech. 2023;1(1):35-52.
13. Capolongo, S.; Gola, M.; Di Noia, M.; Nickolova, M.; Nachiero, D.; Rebecchi, A.; Settimo, G.; Vittori, G.; Buffoli, M. Social sustainability in healthcare facilities: A rating tool for analysing and improving social aspects in environments of care. Ann. Ist Super. Sanita 2016, 52, 15–23.
14. Moldavska, A.; Welo, T. The concept of sustainable manufacturing and its definitions: A content-analysis based literature review. J. Clean. Prod. 2017, 166, 744–755.
15. Xia, B.; Olanipekun, A.; Chen, Q.; Xie, L.; Liu, Y. Conceptualising the State of the Art of Corporate Social Responsibility (CSR) in the Construction Industry and Its Nexus to Sustainable Development. J. Clean. Prod. 2018, 195, 340–353.
16. Candia Acosta MD, Jousson Ayala DA, Melgarejo Fretes RD. Epidemiological Characterization of Chikungunya Infection in Pediatric Patients, Pilar 2023. Scientific Journal Care & Tech. 2023; 1(1):9-20
17. Ch.V.L.L.Kusuma Kumari. (2015). Performance Appraisal: Dimensions and Determinants. International Journal on Research and Development - A Management Review, 4(3), 27 - 32.
18. Kompalli Sasi Kumar. (2015). Short Run and Long Run Performance of Indian Initial Public Offerings (IPOs) during 2007-2012. International Journal on Research and Development - A Management Review, 4(3), 33 - 41.
19. Moro Visconti, R.; Morea, D. Big Data for the Sustainability of Healthcare Project Financing. Sustainability 2019, 11, 3748.
FINANCING
None.
CONFLICT OF INTEREST
None.
AUTHORSHIP CONTRIBUTION
Conceptualization: Sangram Keshari Behera, Dhairyasheel D. Patil, Renuka Jyothi.S, Nancy Puri, Ashok Kr Sharma.
Data curation: Sangram Keshari Behera, Dhairyasheel D. Patil, Renuka Jyothi.S, Nancy Puri, Ashok Kr Sharma.
Formal analysis: Sangram Keshari Behera, Dhairyasheel D. Patil, Renuka Jyothi.S, Nancy Puri, Ashok Kr Sharma.
Drafting - original draft: Sangram Keshari Behera, Dhairyasheel D. Patil, Renuka Jyothi.S, Nancy Puri, Ashok Kr Sharma.
Writing - proofreading and editing: Sangram Keshari Behera, Dhairyasheel D. Patil, Renuka Jyothi.S, Nancy Puri, Ashok Kr Sharma.