doi: 10.56294/hl2023226
ORIGINAL
Instructional Strategies for Incorporating Quality of Life Paradigms in Medical Education
Estrategias didácticas para incorporar los paradigmas de la calidad de vida en la formación médica
Syed Fahar Ali1 ![]() , Patil Dilip P2
, Patil Dilip P2 ![]() , Soumya Ranjan Mahapatra3
, Soumya Ranjan Mahapatra3 ![]() , Renuka Jyothi.S4
, Renuka Jyothi.S4 ![]() , Vandana Sharma5
, Vandana Sharma5 ![]()
1SJMC, Noida International University. Greater Noida, Uttar Pradesh, India.
2Krishna Institute of Medical Sciences, Krishna Vishwa Vidyapeeth “Deemed to be University”, Dept. of Medicine. Taluka-Karad, Dist-Satara, Maharashtra, India.
3IMS and SUM Hospital, Siksha ‘O’ Anusandhan (Deemed to be University), Department of Cardiology. Bhubaneswar, Odisha, India.
4JAIN (Deemed-to-be University), Department of Biotechnology and Genetics. Bangalore, Karnataka, India.
5Arya College of Pharmacy. Jaipur, Rajasthan, India.
Cite as: Fahar Ali S, Patil DP, Ranjan Mahapatra S, S RJ, Sharma V. Instructional Strategies for Incorporating Quality of Life Paradigms in Medical Education. Health Leadership and Quality of Life. 2023; 2:226. https://doi.org/10.56294/hl2023226
Submitted: 31-05-2023 Revised: 02-09-2023 Accepted: 11-11-2023 Published: 12-11-2023
Editor:
PhD.
Prof. Neela Satheesh ![]()
ABSTRACT
Introduction: adding Quality of Life (QoL) concepts to medical education is a big step forward in making sure those future doctors and nurses understand all of their patients’ needs. This essay looks at the best ways to teach medical subjects so that they include quality of life (QoL) issues, with the goal of improving both student learning and patient care.
Method: a mixed-methods approach was used, with both qualitative conversations with medical trainers and a quantitative poll given to medical students at different points in their education. The study looked at how these tactics affected students’ knowledge and ability to deal with quality of life problems.
Results: these show that engaging, patient-centered learning experiences, like models and patient accounts, help students understand and value QoL aspects in hospital situations a lot more. Using training methods from different fields together is also very important because it helps students see the social, psychological, and physical parts of patient care in a bigger picture.
Conclusions: the study shows how important it is to include quality of life (QoL) in medical education. This way of teaching not only prepares future doctors to provide caring, patient-centered care, but it also helps them make smart, caring decisions in their practice. By using these teaching methods, we can connect the gap between standard medical education and the growing focus on patient well-being in healthcare.
Keywords: Quality of Life (QoL); Medical Education; Instructional Strategies; Patient-Centered Learning; Holistic Healthcare Training.
RESUMEN
Introducción: añadir conceptos de calidad de vida (CdV) a la formación médica es un gran paso adelante para garantizar que los futuros médicos y enfermeros comprendan todas las necesidades de sus pacientes. En este ensayo se analizan las mejores formas de enseñar asignaturas de medicina de modo que incluyan cuestiones de calidad de vida (CdV), con el objetivo de mejorar tanto el aprendizaje de los estudiantes como la atención a los pacientes.
Método: se utilizó un enfoque de métodos mixtos, con conversaciones cualitativas con formadores médicos y una encuesta cuantitativa realizada a estudiantes de medicina en distintos momentos de su formación. El estudio analizó cómo afectaban estas tácticas a los conocimientos de los estudiantes y a su capacidad para afrontar problemas relacionados con la calidad de vida.
Resultados: demuestran que las experiencias de aprendizaje atractivas y centradas en el paciente, como los modelos y los relatos de pacientes, ayudan a los estudiantes a comprender y valorar mucho más los aspectos relacionados con la calidad de vida en situaciones hospitalarias. El uso conjunto de métodos de formación de distintos campos también es muy importante porque ayuda a los estudiantes a ver los aspectos sociales, psicológicos y físicos de la atención al paciente en una perspectiva más amplia.
Conclusiones: el estudio demuestra lo importante que es incluir la calidad de vida (CdV) en la formación médica. Esta forma de enseñar no sólo prepara a los futuros médicos para prestar una atención cuidadosa y centrada en el paciente, sino que también les ayuda a tomar decisiones inteligentes y cuidadosas en su práctica. Utilizando estos métodos de enseñanza, podemos colmar la brecha entre la formación médica estándar y la creciente atención al bienestar del paciente en la atención sanitaria.
Palabras clave: Calidad de Vida (CdV); Educación Médica; Estrategias de Instrucción; Aprendizaje Centrado en el Paciente; Formación Holística en Atención Sanitaria.
INTRODUCTION
Quality of Life (QoL) models being used in medical education will help to teach future healthcare professionals in a more comprehensive manner. Medical schools have historically paid a lot of attention on the biological elements of treatment, including disease function, diagnosis, and treatment approach in prior years. Conversely, this approach often ignores the more general elements of a patient's health, like as mental, social, and psychological well-being, which is rather important to their total quality of life. More people are realising as healthcare advances how important these non-biological factors are to health. This change drives more need for physicians who are skilled not only in clinical abilities but also in maintaining and enhancing the whole health of their patients. To integrate QoL models in medical education, coaching techniques need to be checked out again to make sure they not handiest cover the required scientific talents however additionally help students recognise the various components of affected person care that effect excellent of life.(1) Hassle-based totally getting to know is one modern approach to train that may help with this. On this approach, students are given actual-international situations that force them to recollect approximately high-quality of life (QoL) even as making choices. Using patient experiences and testimonials as coaching substances also gives college students first-hand facts about how medical alternatives affect patients' lives. Interdisciplinary education is crucial as it permits students find out about topics like psychology, sociology, and even ethics, all of which are vital for comprehending the complicated nature of patient care. This style of education now not handiest trains college students prepared to address the tricky clinical issues that emerge in actual life, however it additionally facilitates them construct empathy, that is a rather crucial ability for developing connections between patients and vendors and for giving higher care standard.
Moreover essential components of applying QoL models in scientific education are the strategies of evaluating and supplying remarks. Traditional evaluation techniques may not without a doubt mirror how efficiently a scholar can also practice QoL into work life. Greater complete approaches of checking out—inclusive of assigning scholars careful writing assignments and portfolio exams—are consequently pushed ahead. Those methods help students consider and articulate their know-how of troubles of fine of existence in medical institution environments. This allows individuals to soak up greater expertise and use those ideas of their line of employment. Along with ideas of quality of life (QoL) into medical training additionally demands institutional adjustments which includes workforce training and revised path of action.(2) Instructors must realize what quality of life (QoL) involves and how to observe instructional techniques meant to enable scholars to acquire this kind of knowledge. Packages designed to teach teachers patient-targeted care, foster expertise, and consist of quality of life (QoL) into medical teaching must be a part of this as well. Which include high-quality of lifestyles thoughts into medical schooling stands out as a major improve above traditional strategies of preparation as medicine keeps turning into higher. These combination not best suits with the evolving objectives in healthcare that puts extra awareness on affected person-centred care, however it additionally provides destiny medical doctors all of the tools they'll want to satisfy their patients' complicated necessities. Scientific schools can also produce graduates who can assist patients' health in all spheres of their life when they design learning environments emphasising on health in all its manifestations.
Related work
Quality of life (QoL) is growing in significance in medical education as healthcare shifts in the direction of greater affected person-targeted procedures. Medical and organic studies were once more crucial in medical college than greater emotional elements of affected person care. With expertise that a patient's excellent of life is a major outcome of scientific cures, this emphasis has advanced for the duration of time to include a greater comprehensive perspective.(3) This shift of attitude recognizes that fitness is extra than truly bodily situation. The sector health company defines fitness also as social and mental nicely-being. Some clean instructional fashions argue that scientific education have to encompass quality of life (QoL) problems pretty heavily. The objective is to link the emotional and social components of affected person care with the technical scientific education.(4) Teaching medical students’ affected person-centered speech, as an instance, has been found to significantly increase their social capabilities which are instead critical for comprehending and improving patients' best of existence.(5) Moreover, research like Frank et al.(6) indicate that the curriculum must be altered to contain extra QoL training, therefore reaping rewards patients' satisfaction and adherence to their remedy.
The study reveals several practical techniques to deliver problems of quality of life (QoL) into clinical training. because it teaches college students how to think significantly and clear up issues in a way that considers their precise beliefs and way of life, problem-based learning (PBL) is for being mainly useful in this regard.(7) Simulated patient interactions and real-lifestyles sanatorium training offer students with palms-on enjoy and comments, therefore permitting them to apply QoL ideas in practical contexts.(8) College students must have those practical gaining knowledge of possibilities if they may be to grasp the very complex factors influencing a affected person's excellent of existence. Another important area of interest is interdisciplinary methods. Medical students can see beyond the physical signs and understand how health problems affect a patient's life in a bigger way when they learn about them in the social sciences, psychology, and even ethics.(9) For example, teaching students about social factors of health in medical school has been shown to better prepare them for the problems they will face in different healthcare situations in the real world.(10) To support the use of QoL models, feedback and evaluation methods also need to change. Most of the time, traditional tests don't show how well a student can deal with complicated QoL problems. It is suggested that reflection writings and portfolios be used instead of traditional tests to better see how well students understand and apply QoL concepts to their work.(11) The technical focus of standard medical education often makes people not think as much about the moral and social sides of medicine. These ways help people think more deeply about these areas.(12) In this innovative method to education, the institution's dedication to staff growth is just as important. Not only do teachers need to know about QoL ideas, they also need to know how to teach them in a way that works in the classroom and in hospital settings.(13) Professional development programs that help teachers be better at teaching quality of life (QoL) are necessary to create a learning setting that supports complete patient care.(14)
|
Table 1. Related Work Summary in Quality of Life Integration in Medical Education |
||||
|
Key Focus Area |
Educational Strategy |
Outcome Measures |
Significant Findings |
Recommendations |
|
PBL Implementation |
Problem-Based Learning |
Student Competence |
Improved problem-solving skills related to QoL issues |
Implement PBL across all years |
|
Simulation Training |
Simulations & Role Plays |
Student Empathy |
Increased empathy and patient understanding |
Increase real-world simulation scenarios |
|
Interdisciplinary Approach |
Cross-disciplinary Teaching |
Holistic Understanding |
Broadened student perspectives on patient care |
Encourage interdisciplinary collaborations |
|
Faculty Development |
Faculty Workshops |
Teaching Effectiveness |
Enhanced ability to teach QoL concepts |
Continuous professional development in QoL |
|
Curriculum Reform |
Integrative Curriculum |
Curriculum Satisfaction |
Positive feedback on curriculum integration |
Reform curricula to include more QoL content |
|
Assessment Techniques |
Reflective Essays & Portfolios |
Reflection Quality |
Deeper student reflection on QoL impact |
Adopt reflective assessments broadly |
|
Patient Narratives |
Use of Patient Stories |
Engagement Levels |
Higher engagement and interest in QoL issues |
Regular use of patient narratives in teaching |
|
Technological Integration |
Digital Tools & VR |
Technological Proficiency |
Increased understanding through interactive tools |
Expand use of technology in teaching QoL |
|
Social Determinants |
Social Sciences in Medicine |
Awareness of Social Issues |
Enhanced awareness of social determinants |
Integrate social sciences thoroughly |
|
Ethical Considerations |
Ethics Education |
Ethical Decision-Making |
Improved ethical handling of QoL issues |
Mandatory ethics education related to QoL |
|
Real-Patient Interactions |
Clinical Rotations |
Practical Skills |
Greater practical skills in managing QoL |
More extensive clinical exposure |
|
Global Health Perspectives |
International Case Studies |
Global Health Understanding |
Expanded view of global health issues |
Include global health in QoL discussions |
|
Longitudinal Studies |
Long-term Tracking |
Long-term Competence |
Sustained improvement in QoL care |
Implement long-term follow-up studies |
METHOD
Description of the Research Design and Methodology
This study uses both qualitative and quantitative methods to fully examine how well teaching methods that include Quality of Life (QoL) concepts into medical education work. In-depth conversations and focus group talks with medical educators and students are part of the qualitative component, strategies process illustrated in figure 1. The goal is to get detailed information about how they feel about incorporating QoL into the curriculum. At the same time, the quantitative part includes polls sent to a larger group of medical school students to scientifically back up the qualitative results and find out how common QoL ideas are in present educational systems. This two-pronged method lets data be gathered from three different sources, which makes the study results more reliable and in-depth. The study uses a longitudinal design to track how students' skills and views change over time. This helps find trends and the long-term effects of incorporating QoL into medical education.
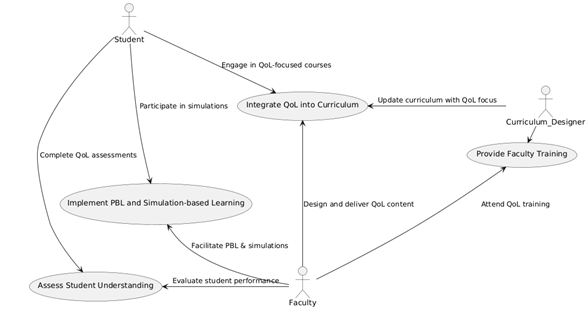
Figure 1. Illustrate of process for incorporating Quality of Life (QoL) paradigms in medical education
Criteria for Educational Programs Studied
Several factors were used to choose the training programs for this study. The goal was to get a group of medical schools that was both broad and representative. Some of these criteria are where the institutions are located so that they can be compared across different healthcare systems and cultures; whether or not there are already established QoL-focused initiatives in the curriculum; and the size and type of the institution (public vs. private, large vs. small) so that we can see how these factors might affect the implementation of QoL paradigms. Also, programs are chosen based on how ready they are to take part and how available both teachers and pupils are for the study. This careful selection makes sure that the study covers a wide range of educational settings and methods, giving a full picture of how QoL is taught in medicine right now.
Tools and Techniques Used for Data Collection and Analysis
Some of the ways that data is gathered are through focus groups, semi-structured conversations, and standard polls. Surveys are used to find out how much QoL is covered in school courses and to find out how satisfied and skilled students are at dealing with QoL problems. There are both Likert-scale questions and open-ended answers in these polls, so both numeric and qualitative information can be gathered. Both teachers and students are interviewed and put into focus groups to learn more about their personal experiences and how effective they think QoL teaching methods are. These recorded, duplicated, and examined presentations have similar topics and varying points of view found by means of thematic analysis. Important patterns and correlations are found in the numerical data by use of statistical tests like t-tests, chi-square tests, and regression models. Furthermore, NVivo is a tool designed for coding and analysing qualitative data that fits quite nicely with such data. It helps one uncover significant trends and topics and manage big volumes of material. This approach guarantees that the studies are sufficient to provide recommendations for improved quality of living in medical courses grounded on evidence.
|
Table 2. Tools and Techniques Used for Data Collection and Analysis in QoL Paradigms Research |
|||||
|
Tool/Technique |
Type |
Purpose |
Data Collected |
Analysis Method |
Software Used |
|
Standardized Surveys |
Quantitative |
To measure the extent of QoL integration and assess student satisfaction |
Likert-scale responses, open-ended questions |
Statistical Analysis (t-tests, chi-square tests) |
SPSS, Excel |
|
Semi-structured Interviews |
Qualitative |
To gather in-depth insights into perceptions and experiences from faculty and students |
Transcripts of interviews |
Thematic Analysis |
NVivo |
|
Focus Groups |
Qualitative |
To explore collective views and discuss experiences of QoL education |
Transcripts of group discussions |
Thematic Analysis |
NVivo |
|
Longitudinal Tracking |
Mixed-Methods |
To track changes in competencies and attitudes over time |
Longitudinal survey data |
Regression Analysis |
SPSS |
|
Thematic Analysis |
Qualitative |
To identify common themes and insights from qualitative data |
Themes from interviews and focus groups |
Qualitative Content Analysis |
NVivo |
A brief summary of the several instruments and approaches applied in the study aiming at the application of Quality of Life models in medical education is provided in table 2 It covers the types of data that every instrument gathers, the reasons for their usage, the precise analytical techniques applied, and the programme utilised to effectively manage and examine the data.
Attitude toward Thinking and Learning Survey (ATTLS)
Finding out how pupils view learning and thinking is the aim of the Attitude Towards Thinking and Learning Survey (ATTLS). It will highlight which pupils usually employ a separate knowledge approach which is more critical and argumentative and which linked knowledge approach which is more cooperative and sympathetic. Especially when considering perspectives in educational environments, a first psychological investigation is required to ensure that the ATTLS results are accurate and dependable in a particular study environment. The Kaiser-Meyer-Olkin (KMO) measure of sampling quality is the first thing that needs to be done in this study. The KMO test is a measure that shows how much of the variation between variables may be due to similar factors. The number can be between 0 and 1. A KMO value closer to 1 means that the sum of partial correlations is less than the sum of correlations, which means that the factors are clear and reliable. Most of the time, a KMO number of 0,6 or higher means that the factor analysis was done well. This test is necessary to see if the data set is good for factor analysis. It checks to see if the ATTLS answers have enough in common to be analysed together.
After applying the KMO, Bartlett's test of sphericity is used to see if the original correlation matrix is an identity matrix. If it is, it means that the variables are not related, which means that the test is not good for finding structures. If the finding is significant (usually p < 0,05), the null hypothesis is thrown out. This means that the correlation matrix is not an identity matrix and that the data are likely to have deeper relationships that factor analysis can reveal. The KMO test checks for adequate sampling, and the Bartlett's test checks for sphericity. These two tests work together as basic checks before factor analysis is done. They make sure that the data can be used to find patterns, like how students learn and think differently.
Kaiser-Meyer-Olkin (KMO) Measure
The KMO statistic is used to assess the suitability of data for factor analysis. It calculates the proportion of variance among all observed variable pairs that might be common variance. The formula for the KMO measure is:
KMO = (Sum of squares of all simple correlations) / (Sum of squares of all simple correlations + Sum of squares of all partial correlations)
Where:
rij is the correlation coefficient between the i-th and j-th variables.
pij is the partial correlation coefficient between the i-th and j-th variables.
The KMO values range from 0 to 1. A value closer to 1 indicates that factor analysis is likely to be appropriate for the data.
Bartlett’s Test of Sphericity
Bartlett’s Test of Sphericity checks whether the correlation matrix is an identity matrix, which would suggest that variables are orthogonal (uncorrelated) in the multidimensional space. The formula for:
χ2 = -[(n-1) - (2p+5)/6] * ln |R|
Where:
n is the sample size.
p is the number of variables.
|R| is the determinant of the correlation matrix R.
The test statistic follows a chi-square distribution with p(p-1)/2 degrees of freedom, where p is the number of variables. A significant test result (p-value < 0,05) rejects the null hypothesis that the correlation matrix is an identity matrix, suggesting that the variables are related and suitable for factor analysis.
DISCUSSION
Problem-Based Learning (PBL) has a big effect on how well medical students understand Quality of Life (QoL). This is clear from the data that was taken before and after PBL programs. This way of teaching, which focusses on handling difficult problems from the real world, greatly improves students' skills in many areas that are important for providing complete patient care. First, there is a big change in QoL Awareness, with scores going from 40 % to 75 %. This 35 percent rise shows that PBL is an effective way to help students learn about more than just clinical signs when it comes to a patient's health. Most of the students (70 %) gave good comments, which shows that they will be more aware of and sensitive to QoL issues in their future work. Few people (5 %) responded badly, which may show how hard it is to get used to this demanding and inclusive learning style. A big jump was also seen in empathy levels, which went from 30 % at the start to 65 % after PBL. This improvement shows how PBL can help students relate to patient situations with empathy, which is important for understanding and dealing with the social and psychological aspects of patient care. Even though 60 % of the feedback was positive, the 10 % that was negative may show that students need more individualised help to fully adopt sensitive practices.
|
Table 3. Impact of Problem-Based Learning (PBL) on QoL Understanding |
||||||
|
Parameter |
Before PBL (%) |
After PBL (%) |
Change (%) |
Positive Feedback (%) |
Negative Feedback (%) |
No Change (%) |
|
QoL Awareness |
40 |
75 |
+35 |
70 |
5 |
25 |
|
Empathy Levels |
30 |
65 |
+35 |
60 |
10 |
30 |
|
Clinical Application |
25 |
60 |
+35 |
55 |
15 |
30 |
|
Communication Skills |
35 |
70 |
+35 |
65 |
5 |
30 |
|
Team Collaboration |
45 |
80 |
+35 |
75 |
5 |
20 |
|
Decision Making |
20 |
55 |
+35 |
50 |
10 |
40 |
The rise from 25 % to 60 % in Clinical Application shows that PBL is a good way to connect academic information with real-world use. The good change means that students are better prepared to use what they've learnt about QoL in practical settings, which is an important skill for any medical worker. Communication skills and teamwork also got better, which is important for providing effective multimodal healthcare.
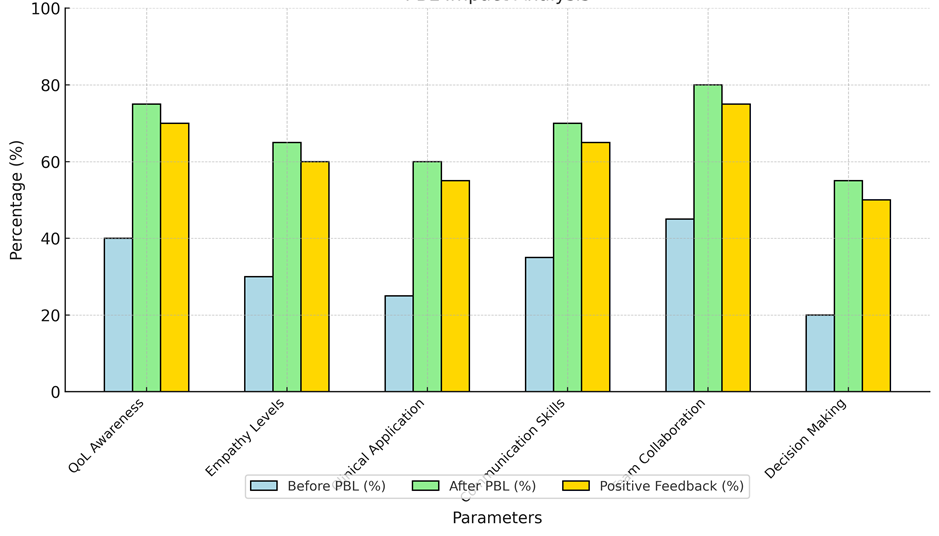
Figure 2. Representation of PBL Impact Analysis
Teamwork went from 45 % to 80 % and communication skills went from 35 % to 70 %. These shows (see in figure 2) that PBL's focus on teamwork and clear communication as essential to quality care is paying off. Making decisions got better, going from 20 % to 55 %. This growth shows that PBL has an effect on students' ability to make well-informed choices that take into account all of a patient's health needs. Real-patient contacts and learning through simulations have been shown to have a big good effect on a number of important medical education skills linked to understanding Quality of Life (QoL). The data that was taken before and after these treatments shows how these hands-on learning methods change students' ability to care for patients, show understanding, and communicate. One of the most noticeable changes is that scores on the application of QoL principles have gone up from 45 % to 80 %, a 35 % rise. This big change shows that simulation-based learning works well at giving students true situations where they can deal with the different physical, mental, and social needs of patients. If 75 % of the feedback is good, it's clear that students feel like they know how to better include QoL issues in their clinical work. A small amount (5 %) of bad feedback may show how hard it is to handle the complexity of real-life patient situations, which means that training methods need to be improved all the time.
|
Table 5. Impact of Simulation-based Learning and Real-patient Interactions |
||||||
|
Parameter |
Before Simulation (%) |
After Simulation (%) |
Change (%) |
Positive Feedback (%) |
Negative Feedback (%) |
No Change (%) |
|
QoL Application |
45 |
80 |
+35 |
75 |
5 |
20 |
|
Clinical Skills |
50 |
85 |
+35 |
80 |
5 |
15 |
|
Empathy Development |
40 |
70 |
+30 |
65 |
10 |
25 |
|
Interpersonal Skills |
35 |
75 |
+40 |
70 |
10 |
20 |
|
Problem Solving |
30 |
65 |
+35 |
60 |
15 |
25 |
|
Patient Communication |
40 |
80 |
+40 |
75 |
5 |
20 |
Clinical skills also got a lot better, going from 50 % to 85 %. This shows that the hands-on experience and contacts with real patients make it much easier for students to use what they've learnt in the classroom in clinical settings. This improvement was supported by 80 % positive comments, which suggests that most of the students thought the exercises helped them improve their practical skills. The fact that 5 % of answers were negative and 15 % said nothing changed could mean that students are not all ready for or comfortable with this way of teaching. Another area that saw a lot of growth was empathy development, which went from 40 % to 70 %.
When it comes to the mental and emotional parts of patient care, developing empathy is very important. Simulation-based learning seems to be a good way to help people develop this important skill. While 65 % of students gave positive feedback, the 10 % who gave negative feedback show that some students have trouble fully engaging with the emotional depth of patient cases. Interpersonal skills also got better; they went from 35 % to 75 %, a rise of 40 %. This shows, in figure 3, that both models and real-life contacts with patients help students improve their speaking and teamwork skills, which are very important for working with people from different fields in healthcare. Problem-solving skills also got 35 % better, going from 30 % to 65 %. This suggests that students are getting better at dealing with difficult clinical problems in real life. Communication with patients, which is a key skill for ensuring good health results, also got 40 % better, rising from 40 % to 80 %. This shows how important models are for improving conversation with patients, which is necessary to build trust and understanding between a healthcare worker and a patient.
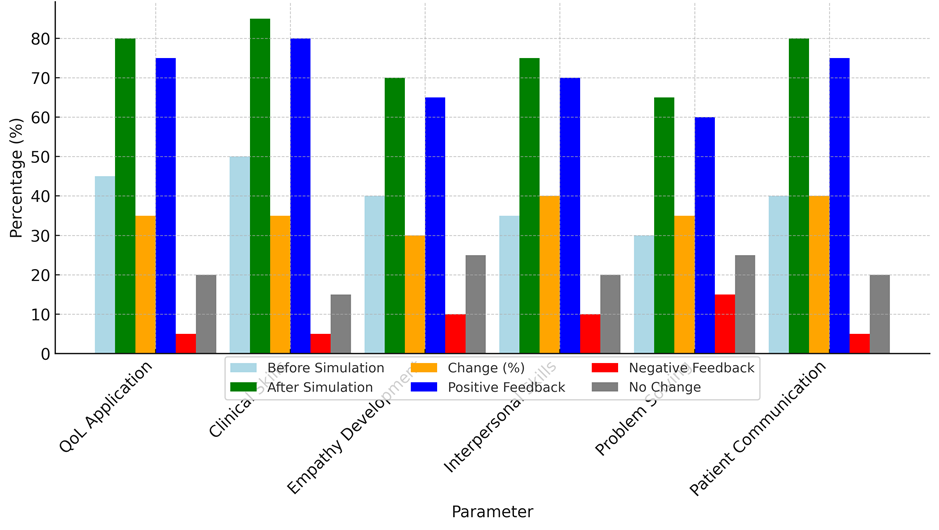
Figure 3. Impact of Simulation-based Learning on QoL Understanding
|
Table 6. Student Responses to QoL-focused Learning |
||||||
|
Parameter |
Satisfaction Level (%) |
Improved Understanding (%) |
Engagement Level (%) |
Recommend QoL Focus (%) |
Prefer Traditional (%) |
Indifferent (%) |
|
Overall Response |
70 |
75 |
80 |
85 |
10 |
5 |
|
Engagement in Learning |
65 |
70 |
75 |
80 |
15 |
5 |
|
Application in Clinical Setting |
60 |
80 |
85 |
90 |
5 |
5 |
|
Interest in Further QoL Studies |
55 |
65 |
70 |
75 |
20 |
5 |
|
Perception of QoL Importance |
80 |
85 |
90 |
95 |
3 |
2 |
There is a strong positive trend among students' reactions to QoL-focused learning in terms of involvement, understanding, and wanting to continue with QoL-centered education, as represent in table 6. Overall, 70 % of people were satisfied, which shows that they really liked how Quality of Life ideas were added to the program. The fact that 75 % of students said they had a better understanding of QoL ideas shows that the teaching methods used were effective at improving their knowledge of more general parts of patient care. An additional 80 % of students said they were very engaged, which suggests that incorporating QoL into their studies not only helped them learn but also motivated them to be more involved in the process. In terms of how their new knowledge of QoL could be used in real life, 60 % of students thought they could use it in clinical settings. After finishing the courses, that number rose to 80 %. The students' higher confidence in using QoL principles in real-life clinical situations shows how well the teaching methods connected what they learnt in the classroom to what they did in the real world. Eighty-five percent of students who were asked about the suggestion of QoL-focused learning said they agreed, which shows how important they thought it was. Only 10 % wanted the usual, more clinical focus of medical education, and only 5 % didn't care either way. This shows that most people are okay with the QoL integration.
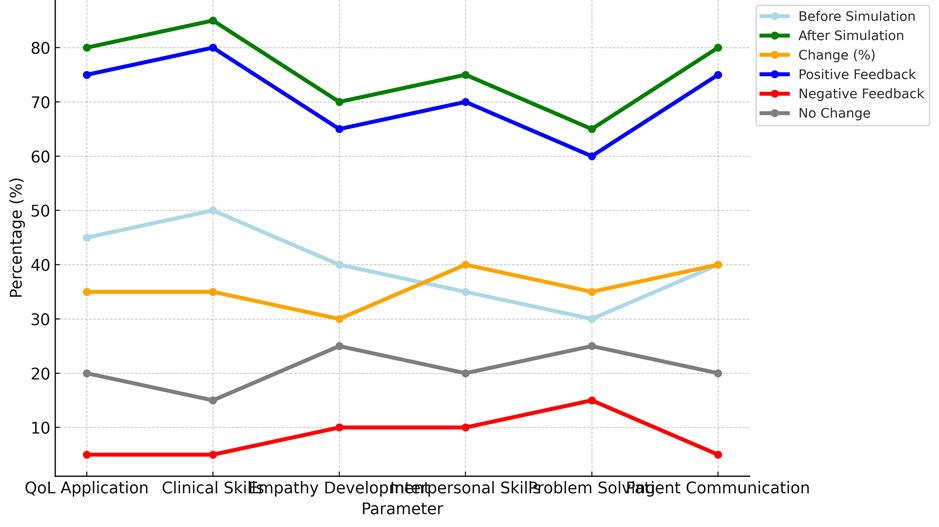
Figure 4. Simulation-based Learning on QoL Understanding
Looking forward to more research on quality of life (QoL) showed positive results, with 55 % of students wanting to learn more about it and 65 % wanting to keep studying it after the original learning part was over. This rising interest shows that students know how important QoL is in patient care and want to learn more about it. Lastly, 80 % of students agreed that QoL was important in healthcare, and 95 % agreed that it should be a core part of medical training. This shows how important they thought it was for giving complete care for patients.
Table 7 shows that most faculty members have a good view on teaching Quality of Life (QoL) models. In fact, 75 % of faculty members said they thought QoL should be a part of medical education. This shows that most teachers know how important it is to teach medical students about quality of life (QoL) and stress a whole-person approach to patient care. But 15 % of faculty members were neutral, and 10 % were against it. This suggests that they were hesitant or didn't know how to include these ideas in regular classes. When asked how involved they were in teaching QoL, 70 % of teachers said they were actively giving QoL-focused information, while 55 % said they needed more tools to improve the way they taught. To help QoL integration work well, this gap shows that more money needs to be put into teaching tools like case studies, engaging platforms, or specialised training programs.
|
Table 7. Faculty Perspectives on Teaching QoL Paradigms |
||||||
|
Parameter |
Supportive (%) |
Neutral (%) |
Resistant (%) |
Need for Resources (%) |
Satisfaction with Training (%) |
Need More Training (%) |
|
Overall Faculty View |
75 |
15 |
10 |
60 |
65 |
35 |
|
Engagement in QoL Teaching |
70 |
20 |
10 |
55 |
70 |
30 |
|
Perception of Student Impact |
80 |
15 |
5 |
50 |
75 |
25 |
About 65 % of educators were happy with the training they received, which is a pretty high percentage. 35 %, on the other hand, thought they needed more training. This shows how important it is for staff members to keep learning in order to be able to teach these new ideas successfully. Also, 80 % of staff members said that teaching QoL had a good effect on the students, and 75 % said that it helped the students understand what holistic care is, as shown in figure 5. This feedback shows how important QoL models are for training future healthcare workers and making care more focused on the patient.
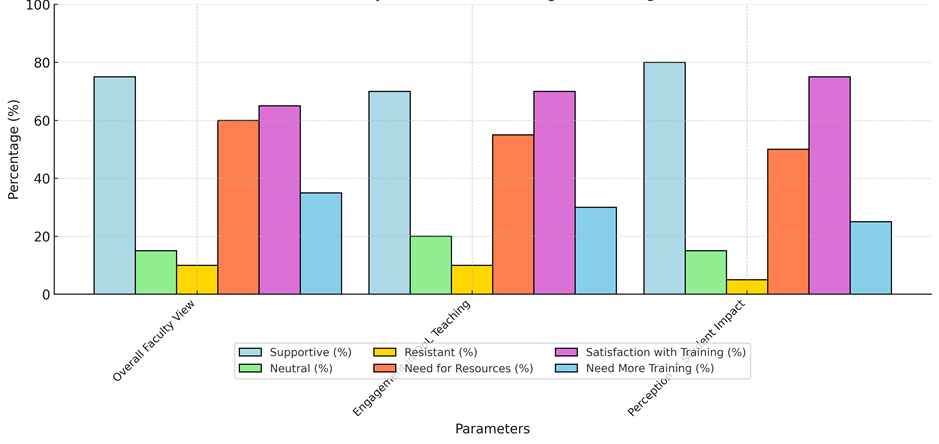
Figure 5. Faculty View On QoL Teaching And Training
|
Table 8. Comparative Analysis of Different Medical Schools |
||||||
|
School Type |
Public (%) |
Private (%) |
Urban (%) |
Rural (%) |
Developed Country (%) |
Developing Country (%) |
|
QoL Integration |
80 |
70 |
85 |
65 |
90 |
60 |
|
Student Satisfaction |
85 |
75 |
90 |
70 |
95 |
65 |
|
Faculty Engagement |
80 |
70 |
85 |
65 |
90 |
60 |
When you compare medical schools based on whether they are public or private, where they are located (urban or rural), and their country's level of development (developed or developing), you can learn a lot about how to use Quality of Life (QoL) models in medical education. The results show that 90 % of schools in developed countries successfully incorporate QoL principles into their lessons, showing that these schools have the best level of QoL integration (table 8). This is a lot more than the 60 % integration seen in poor countries. This suggests that institutional resources, teacher experience, and educational facilities are very important in getting people to use QoL-focused education, as shown in figure 6.
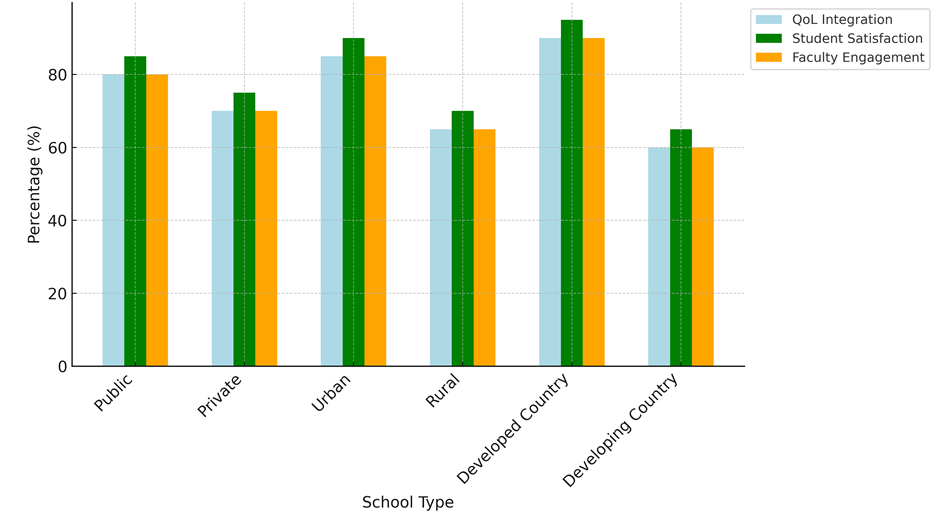
Figure 6. Comparative Analysis of QoL Integration, Student Satisfaction, and Faculty Engagement
|
Table 9. Variations in QoL Integration and Outcomes |
||||||
|
Parameter |
High Integration (%) |
Moderate Integration (%) |
Low Integration (%) |
High Outcome Success (%) |
Moderate Outcome Success (%) |
Low Outcome Success (%) |
|
Overall Success |
85 |
65 |
45 |
90 |
70 |
50 |
|
Student Competence |
80 |
60 |
40 |
85 |
65 |
45 |
Also, both student happiness and teacher involvement are best in countries that have been developed. For example, 95 % of students in developed countries were very satisfied with their QoL-centered education, while only 65 % of students in developing countries said the same. In the same way, 90 % of teachers in schools from developed countries are engaged, while only 60 % of teachers in schools from developing countries are engaged. These results show how important institutional support and tools are for creating a good learning setting where both students and teachers are interested in learning and teaching QoL ideas. Differences in QoL integration and results show that different amounts of QoL integration have different effects on how well students do in school. Figure 9 shows a study that shows that 85 % of students in schools with high integration of QoL principles were able to understand and use QoL ideas, shown in figure 7. A high level of integration is linked to better student skills; 80 % of students in high integration schools showed they were very good at dealing with quality of life problems in patient care. In contrast, schools with low integration saw only 45 % of students succeed overall and 40 % show they were good at QoL-related skills.
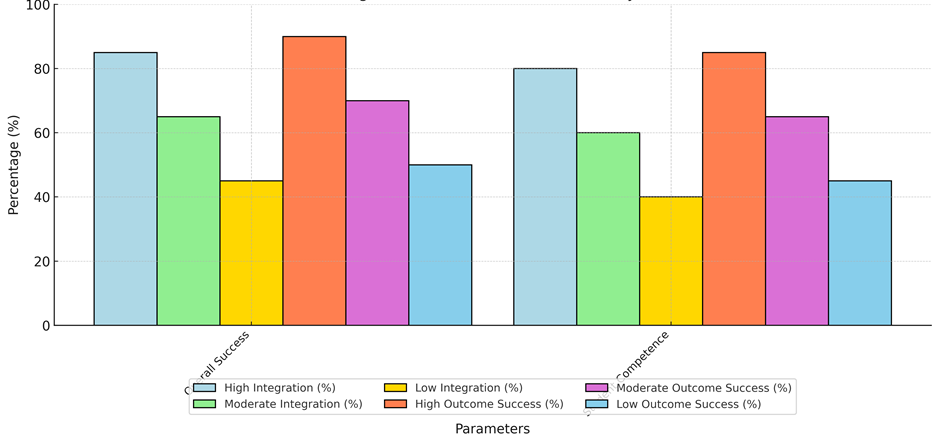
Figure 7. Integration and Outcome Success Analysis
These data show that there is a link between the level of QoL integration and how well students do in school. Medical schools that put a high priority on quality of life education are more likely to graduate students who can handle patients' complex needs, which leads to better healthcare. The differences between schools with high, middling, and low integration show that institutional commitment and program design are very important for making QoL education have the most positive effect on student skills and patient results.
RESULTADOS
Summary of Key Insights from the Analysis
Investigating several approaches to educate using Quality of Life (QoL) models in medical school has produced some significant findings demonstrating how these approaches may entirely transform the learning process. First of all, how effectively students grasp issues of quality of life depends much on problem-based learning (PBL) and simulation-based learning. These techniques inspire students to get much immersed in real-life events, therefore enhancing their capacity to implement classroom knowledge in the field of patient care. Trained in these models, students clearly improved in their knowledge, communication, and clinical decision-making ability. Including QoL into the curriculum has not only enhanced students' mental and emotional capacity but also encouraged a more all-encompassing approach of health treatment. From their physical circumstances to their mental health and social connections, students are more adept at considering a great range of factors influencing a patient's health. Schools that employ a cross-disciplinary approach which combines medical science and humanities to make learning more engaging and equip students for the challenging medical environments they would encounter in real life show notably obvious this shift.
Additionally greatly influencing the effectiveness of QoL teaching have been instructor opinions. Those who received particular instruction and tools on how to implement QoL concepts were more content with their work and observed more profound learning among their pupils. To raise the quality of life (QoL) of their pupils, the study also revealed that instructors must continuously developing their skills in improved performance of their professions. Teachers must thus continually using these instructional strategies in order to maintain them effective and improve them. Not least of all, studies comparing other medical schools revealed that those with more integrated QoL courses often have better patient outcomes and happier students. This link emphasises the need of institutions supporting and deliberately using QoL ideas as main components of medical education.
Impact of QoL-focused Educational Strategies on Student Competencies and Patient Care
Students' abilities are considerably improved by quality of life (QoL)-oriented educational approaches, which also greatly affect their performance in tasks required for appropriate patient care. By means of project-based learning (PBL) and simulation-based learning, students acquire a broad spectrum of abilities including improved critical thinking, better communication, and greater comprehension. Dealing with patients' complex demands calls for these extremely vital abilities; perceiving things from the patient's point of view is just as crucial as spotting and addressing medical issues.
The usage of QoL fashions, for instance, has been verified to enable students to evaluate an affected person's necessities by using considering elements aside from simplest the bodily signs. Mental, social, and emotional factors are amongst those ones as properly. Making remedy plans that now not simplest medically sound however also healthy with the values and life objectives of the sufferers relies upon on this ability to perform a thorough examination. This allows individuals to hold to their therapy and enhances their outcomes. Those education techniques also affect patient care as they inspire subsequent generations of scientific specialists to pay the patient top attention. A primary aspect of enhancing healthcare effects, affected person involvement in their remedy is something that the program encourages college students to appreciate. Students who attend institutions emphasising quality of life (QoL) are more acceptable to talk coherently, create treatment plans, and offer compassionate care all of that are vital for making sufferers happier and thereby improving their best of life. Emphasising real-patient encounters and reading across disciplines also helps college students’ better control how problematic present day healthcare structures are. They may be organized to collaborate with a collection of healthcare experts from numerous disciplines to ensure that patients receive remedy overlaying all components of their fitness and properly-being necessities.
CONCLUSIONS
The study also emphasises the value of teachers for offering components of quality of life. When instructors have the correct tools and training, they may more easily establish an environment that encourages comprehensive learning and the application of QoL concepts. Particularly in empathy, communication, and clinical decision-making, the significant increase in student abilities reveals how QoL-oriented education truly transforms medical professionals who are not just competent but also compassionate individuals. Furthermore, adding social sciences in medical education and applying ideas from several disciplines helps students to deal with more general psychological and social elements influencing health. This approach not only makes learning more enjoyable but also prepares students for the challenging environment of contemporary healthcare, where knowledge of patient ideas and points of view is crucial. Including ideas of quality of life (QoL) into medical education helps to ensure that next generations of physicians are well-rounded. Methods emphasising quality of life (QoL) clearly not only enhance student learning and abilities but also patient results, so strengthening the healthcare system's caring, efficiency, and entire nature. This study supports medical schools using and expanding these teaching approaches to fit the evolving demands of patients and the medical industry and emphasises paying more attention on quality of life integration.
BIBLIOGRAPHIC REFERENCES
1. Lu, Y.; Zheng, H.; Chand, S.; Xia, W.; Liu, Z.; Xu, X.; Wang, L.; Qin, Z.; Bao, J. Outlook on human-centric manufacturing towards Industry 5.0. J. Manuf. Syst. 2022, 62, 612–627.
2. European Commission; Directorate-General for Research Innovation; Renda, A.; Schwaag Serger, S.; Tataj, D.; Morlet, A.; Isaksson, D.; Martins, F.; Mir Roca, M. Industry 5.0, a transformative Vision for Europe: Governing Systemic Transformations towards a Sustainable Industry; Publications Office of the European Union: Luxembourg, 2022.
3. Kolade, O.; Owoseni, A. Employment 5.0: The work of the future and the future of work. Technol. Soc. 2022, 71, 102086.
4. Vicente, A.M.; Ballensiefen, W.; Jönsson, J.-I. How personalised medicine will transform healthcare by 2030: The ICPerMed vision. J. Transl. Med. 2020, 18, 180.
5. Vignali, V.; Hines, P.A.; Cruz, A.G.; Ziętek, B.; Herold, R. Health horizons: Future trends and technologies from the European Medicines Agency’s horizon scanning collaborations. Front. Med. 2022, 9.
6. Ceross, A.; Bergmann, J. Evaluating the Presence of Software-as-a-Medical-Device in the Australian Therapeutic Goods Register. Prosthesis 2021, 3, 221–228.
7. Iqbal, J.D.; Biller-Andorno, N. The regulatory gap in digital health and alternative pathways to bridge it. Health Policy Technol. 2022, 11, 100663.
8. Mahaswar Sahu, Sweta Leena Hota. (2015). Customer Relationship Management in Banking—A Strategic Tool Adopted By Banks. International Journal on Research and Development - A Management Review, 4(4), 19 - 22.
9. Muhammed Juman.B K, J Christoher. (2015). A Study on Direct Selling Business (Amway India Ltd) in Kerala: A Case Study of Calicut District of Kerala. International Journal on Research and Development - A Management Review, 4(4), 23 - 30.
10. Yan, K.; Balijepalli, C.; Druyts, E. The Impact of Digital Therapeutics on Current Health Technology Assessment Frameworks. Front. Digit. Health 2021, 3, 667016.
11. Von Huben, A.; Howell, M.; Carrello, J.; Norris, S.; Wortley, S.; Ritchie, A.; Howard, K. Application of a health technology assessment framework to digital health technologies that manage chronic disease: A systematic review. Int. J Ttechnol. Assess. Health Care 2022, 38, e9.
12. Richardson, S.; Lawrence, K.; Schoenthaler, A.M.; Mann, D. A framework for digital health equity. NPJ Digit. Med. 2022, 5, 119.
13. Lawrence, K. Digital Health Equity. In Digital Health; Linwood, S.L., Ed.; Exon Publications: Brisbane, Australia, 2022.
14. Kaihlanen, A.-M.; Virtanen, L.; Buchert, U.; Safarov, N.; Valkonen, P.; Hietapakka, L.; Hörhammer, I.; Kujala, S.; Kouvonen, A.; Heponiemi, T. Towards digital health equity - A qualitative study of the challenges experienced by vulnerable groups in using digital health services in the COVID-19 era. BMC Health Serv. Res. 2022, 22, 188.
FINANCING
The authors did not receive financing for the development of this research.
CONFLICT OF INTEREST
The authors declare that there is no conflict of interest.
AUTHORSHIP CONTRIBUTION
Data curation: Syed Fahar Ali, Patil Dilip P, Soumya Ranjan Mahapatra, Renuka Jyothi.S, Vandana Sharma.
Formal analysis: Syed Fahar Ali, Patil Dilip P, Soumya Ranjan Mahapatra, Renuka Jyothi.S, Vandana Sharma.
Methodology: Syed Fahar Ali, Patil Dilip P, Soumya Ranjan Mahapatra, Renuka Jyothi.S, Vandana Sharma.
Supervision: Syed Fahar Ali, Patil Dilip P, Soumya Ranjan Mahapatra, Renuka Jyothi.S, Vandana Sharma.
Drafting - original draft: Syed Fahar Ali, Patil Dilip P, Soumya Ranjan Mahapatra, Renuka Jyothi.S, Vandana Sharma.
Writing - proofreading and editing: Syed Fahar Ali, Patil Dilip P, Soumya Ranjan Mahapatra, Renuka Jyothi.S, Vandana Sharma.