doi: 10.56294/hl2023225
ORIGINAL
The Integration of Quality of Life Evaluations into Standard Healthcare Management Protocols
Integración de las evaluaciones de la calidad de vida en los protocolos estándar de gestión sanitaria
Kavina
Ganapathy1 ![]() , Fazil Hasan2
, Fazil Hasan2 ![]() , Tapas Ranjan Behera3
, Tapas Ranjan Behera3 ![]() , V.M. Thorat4
, V.M. Thorat4 ![]() , Pranoti Prashant Mane5
, Pranoti Prashant Mane5
1School of Sciences, JAIN (Deemed-to-be University), Department of Biotechnology. Bangalore, Karnataka, India.
2Noida International University, Department of Agriculture. Greater Noida, Uttar Pradesh, India.
3IMS and SUM Hospital, Siksha ‘O’ Anusandhan (Deemed to be University), Department of Nephrology. Bhubaneswar, Odisha, India.
4Krishna Institute of Medical Sciences, Krishna Institute of Allied Sciences, Krishna Vishwa Vidyapeeth “Deemed to be University”, Department of Pharmacology. Taluka-Karad, Dist-Satara, Maharashtra, India.
5MES’s Wadia College of Engineering. Pune, India.
Cite as: Ganapathy K, Hasan F, Ranjan Behera T, Thorat V, Mane PP. The Integration of Quality of Life Evaluations into Standard Healthcare Management Protocols. Health Leadership and Quality of Life. 2023; 2:225. https://doi.org/10.56294/hl2023225
Submitted: 31-05-2023 Revised: 02-09-2023 Accepted: 11-11-2023 Published: 12-11-2023
Editor:
PhD.
Prof. Neela Satheesh ![]()
ABSTRACT
Making treatment more patient-centered mostly depends on including Quality of Life (QoL) testing into regular healthcare operations. This approach shifts the traditional emphasis from gauging illness to considering a patient’s complete health. Regular medical practice’s use of QoL testing enables physicians to better understand, on a larger scale, how disease and therapy influence patients’ daily life including their physical, psychological, and social health. Key component of this mix is developing and using dependable, proven QoL methods tailored for various patient groups and circumstances. These instruments help one to extra precisely evaluate the mental fitness situation and degree of existence pride of the sufferers. While physicians use those insights while making medical decisions, they may provide sufferers with treatment options that not handiest advantage their fitness but also supplement their very own values and life objective. Furthermore, consistent QoL evaluations enable one to monitor the long-term consequences of healthcare policies, thus guiding treatment programs and providing patient support services continuously. Early on discovery of issues compromising a patient’s quality of life comes from proactive approach. This allows for fast therapies meant to prevent worsening of health. Including QoL evaluations has effects beyond just attending to one patient. It clarifies health impacts in a more intricate manner, which is rather crucial for allocating funds and formulating health policy. Healthcare systems may transform to better, more long-lasting, and more compassionate approaches of controlling illness and health by first giving patient-reported outcomes first priority.
Keywords: Patient-Centered Care; Quality of Life (QoL); Healthcare Management; QoL Instruments; Treatment Outcomes; Health Policy.
RESUMEN
Lograr que el tratamiento se centre más en el paciente depende sobre todo de la inclusión de pruebas de calidad de vida (CdV) en las operaciones sanitarias habituales. Este enfoque cambia el énfasis tradicional de medir la enfermedad a considerar la salud completa del paciente. El uso habitual de pruebas de calidad de vida en la práctica médica permite a los médicos comprender mejor, a mayor escala, cómo influyen la enfermedad y el tratamiento en la vida diaria de los pacientes, incluida su salud física, psicológica y social. Un componente clave de esta combinación es el desarrollo y uso de métodos de calidad de vida fiables y probados, adaptados a diversos grupos de pacientes y circunstancias. Estos instrumentos ayudan a evaluar con mayor precisión la situación de salud mental y el grado de orgullo existencial de los enfermos. Si los médicos utilizan esta información para tomar decisiones médicas, pueden ofrecer a los pacientes opciones de tratamiento que no sólo mejoren su estado físico, sino que también complementen sus propios valores y objetivos vitales. Además, las evaluaciones constantes de la calidad de vida permiten controlar las consecuencias a largo plazo de las políticas sanitarias, orientando así los programas de tratamiento y proporcionando servicios de apoyo al paciente de forma continua. El descubrimiento precoz de los problemas que comprometen la calidad de vida de un paciente se debe a un enfoque proactivo. Esto permite aplicar terapias rápidas destinadas a prevenir el empeoramiento de la salud. Incluir evaluaciones de la calidad de vida tiene efectos que van más allá de la mera atención a un paciente. Aclara las repercusiones sanitarias de una manera más intrincada, lo cual es bastante crucial para asignar fondos y formular políticas sanitarias. Los sistemas sanitarios pueden transformarse hacia enfoques mejores, más duraderos y más compasivos de control de la enfermedad y la salud dando prioridad en primer lugar a los resultados comunicados por los pacientes.
Palabras clave: Atención Centrada en el Paciente; Calidad de Vida (CdV); Gestión Sanitaria; Instrumentos de CdV; Resultados del Tratamiento; Política Sanitaria.
INTRODUCTION
For clinical treatment, it include quality of life (QoL) trying out into ordinary healthcare management approaches marks a vast development in healthcare. It demonstrates the price of affected person-centered outcomes past simple application of generic healing guidelines. This shift to use QoL testing is aimed to take into account the complex effects that health troubles have on regular living. This will ensure that the treatment patients get more closely corresponds with their own values and general condition.
Quality of Life (QoL) Evaluations
Studies on quality of life (QoL) are set assessments used to ascertain overall health of persons and groups. QoL tests are used in healthcare to observe how diseases, disorders, and therapies impact everyday life. These exams examine their degree of independence, their social contacts, their personal views, their physical and mental health, and how these factors connect to significant elements of their environment. Historically, health policies have largely focused on diagnosis and treatment, without considering how they can impact a patient’s life in a more overall sense. Rating of quality of life (QoL) developed as a required response to this mistake. They provide a whole picture of health including patient satisfaction, mental and social well-being, and normal capacity to function. From standard questions to one-on-one dialogues, QoL tests use a variety of instruments and approaches. Everyone wants to have a thorough awareness of their own health’s situation.
Importance and relevance of QoL in healthcare
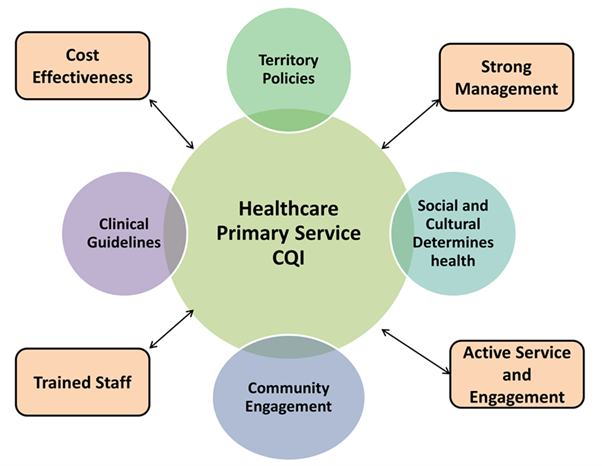
Figure 1. Representation of Healthcare primary services and keywords
Promoting patient-centered care a kind of treatment that helps patients to be active in the management of their own health depends on including quality of life (QoL) testing into healthcare. Focussing on QoL helps healthcare professionals identify, among other aspects of a patient’s health, those that most affect them: pain management, mental health, and social contacts. This approach not only makes every patient happier and more inclined to follow their treatment regimens but also improves their outcomes. Furthermore, QoL data enable physicians to better decide, raise the outcomes of their treatments, and maximise the utilisation of resources. Knowing a patient’s quality of life (QoL) for a chronic illness, for instance, might assist guide decisions on treatments that would most likely result in long-term commitment and favourable outcomes. Value-based care is increasingly valued in healthcare systems, hence quality of life measurements become more crucial. This highlights their significance in determining the effectiveness of medical therapies and modifying health policy. Figure 1 shows the model of Healthcare Primary Service Continuous Quality Improvement (CQI). It stresses the merging of various elements such as cost effectiveness, trained staff, and strong management that directly influence the success of healthcare services. Community involvement and obedience to professional standards are also noted as important for better health results within this structure.
Integrating QoL evaluations into healthcare protocols
There are three main steps in incorporating QoL evaluations into healthcare protocols: choosing the right QoL instruments, teaching healthcare providers how to use these tools correctly, and adding QoL data to patient records and care plans in a planned way. For integration to work, healthcare systems need to not only start measuring QoL, but they also need to promise to act on the information they get from these tests. It may be necessary to change the way care is given and make sure there are ways for feedback and growth to happen all the time. Including QoL tests also needs a multidisciplinary approach, with doctors, nurses, psychologists, and social workers working together to meet all of the patients’ complex needs. This combination also supports a move towards preventative health measures, making happiness and quality of life the main goals of healthcare instead of just treating illness.
Review of the literature
Existing models of QoL integration in healthcare
Many numerous processes had been investigated the usage of quality of life (QoL) tests in healthcare, and increasingly individuals are coming across how beneficial they are for boosting affected person care. Early models targeted on disease-specific Q-of-L measurements, in which gadgets have been designed to stumble on the nuances of each infection.(1) more thorough models have now been advanced, inclusive of the affected person-suggested outcomes measurement information machine (PROMIS), which generates QoL measurements the equal for all ailments and businesses in order that they’ll be easily in comparison and used as a standard.(2) Nevertheless every other essential model is the arena fitness enterprise exceptional of lifestyles (WHOQOL) concept. It provides a complete image of first-rate of residing encompassing social relationships, bodily fitness, mental health, and outside influence.(2)
Dynamic models combining electronic health records (EHR) with quality of life (QoL) records are being used in many healthcare structures. This permits real-time patient performance view for managers and monitors.(4) For example, included models the use of cell health (mHealth) era help healthcare practitioners screen a patient’s quality of life (QoL) by allowing them self-report the use of applications connected immediately to their healthcare provider’s systems.(5) This technologically based totally method not most effective gives reliable and current facts but also makes patients greater engaged of their treatment and much more likely to follow their dreams. Numerous environments were tested for the overall performance of those fashions. Integration of QoL has been confirmed to boom universal affected person pleasure with care, remedy selections, and discussion between sufferers and clinicians.(6) Furthermore, QoL models enable treatment plans for continual conditions like diabetes and heart disorder to higher match the affected person’s lifestyle and alternatives. Better outcomes on fitness and illness control follow from this.(7,8) Furthermore evidence exists that QoL measures are utilized in acute care environments and their cost in figuring out how surgical operation and health facility stays have an effect on sufferers’s ability to get better and their satisfaction.(9) Those models underline the want of early on in a affected person’s care measuring quality of life (QoL), as this may enable the improvement of treatment techniques facilitating quicker and better recovery.(10)
Analysis of challenges and benefits identified in previous studies
Although the benefits are well hooked up, integrating QoL evaluations into healthcare systems affords a few challenges. One principal subject is that multiple QoL measuring instruments may complicate data collecting and evaluation.(11) Nonetheless some other trouble with QoL measurements is subjectivity. Private prejudices or lack of awareness of the surveys may additionally have an impact on patients’ very own reports.(12) Along with QoL statistics into scientific exercise also requires sizeable modifications in how healthcare professionals do their jobs, which is probably greeted with resistance as they’ve extra paintings to accomplish or lack understanding of QoL concepts.(13) Contrarily, which include QoL critiques gives wonderful benefits. In line with studies, QoL statistics provide an extra complete photo of an affected person’s health, which aids inside the development of more fitting and a success treatment applications.(14) Doctors have greater ease figuring out hidden problems with patients that would not be obtrusive from recurring tests. For instance, fitness outcomes can be a lot inspired by using mental health troubles or regular solitude.(15) Furthermore, QoL tests recommend a greater affected person-targeted technique to healthcare while scientific treatment is deliberate and achieved considering the necessities and wishes of the patients.(16)
|
Table 1. Related Work in Healthcare Protocols |
||||
|
Study Focus |
Model Used |
Healthcare Setting |
Key Benefits |
Main Challenges |
|
Disease-specific QoL assessments |
Disease-specific instruments |
Various |
Tailored treatment plans |
Inconsistency across diseases |
|
Standardization of QoL measures |
PROMIS |
Across populations |
Facilitates benchmarking |
Requires extensive data integration |
|
Broad QoL perspective |
WHOQOL |
General healthcare |
Inclusive of multiple health domains |
Complexity in implementation |
|
Real-time QoL monitoring |
EHR integration |
All healthcare levels |
Timely data for decision-making |
Adjustment to clinical workflows |
|
Mobile health technologies |
mHealth apps |
Outpatient |
Enhances patient engagement |
Reliance on patient compliance |
|
Oncology care improvement |
Specific QoL tools |
Oncology clinics |
Improves communication and satisfaction |
High dependency on clinician training |
|
Chronic disease management |
Tailored QoL frameworks |
Chronic care settings |
Improves disease management |
Varies by disease and patient |
|
Acute care impact assessment |
Acute care QoL assessments |
Hospitals |
Influences early treatment plans |
High variability in acute settings |
|
Integration challenges |
Varied models |
General healthcare |
Comprehensive health understanding |
Resistance and increased workloads |
|
Personalized treatment enhancements |
Personalized QoL assessments |
Varied settings |
Tailors treatments to individual needs |
Complexity in personalization |
|
Mental health identification |
Mental health QoL tools |
Mental health services |
Identifies non-clinical issues affecting health |
Subjectivity in assessments |
|
Patient-centric healthcare approach |
Patient-centric QoL models |
All settings |
Aligns care with patient lifestyles |
Needs continuous provider education |
METHOD
Research Design and Approach
This mixed-methods studies use each quantitative and qualitative approaches to investigate how efficiently quality of life (QoL) tests are included into healthcare approaches. earlier than and after QoL measurements have been carried out, the studies used a continuous poll to provide quantitative facts on affected person outcomes, modifications in QoL, and the performance of healthcare earlier than and next. This approach allows us to look at hyperlinks between the best of affected person treatment and long-term consequences of QoL integration. Semi-structured interviews and awareness companies could be conducted to find out greater about the reviews of sufferers and healthcare specialists approximately QoL assessments and their supposed advantages. This qualitative phase objectives to demonstrate the tricky implications of consist of QoL that might not be absolutely obvious from simplest making use of numerical measurements. Three stages will include the study: a baseline test at the beginning, a test within the midst of the intervention, and an evaluation at the belief.
Sampling Methods and Population
The group of persons under investigation comes from a variety of healthcare centers, inclusive of speciality outpatient clinics, primary care centres, and hospitals. Every age, gender, infection type, and socioeconomic level may be represented using a stratified random sample technique. By use of thing manage, this method guarantees that the sample represents the full population of patients, therefore making sure their pleasant. Finding extensive variations in QoL findings after the intervention relies upon on acquiring sufficient electricity, thus the estimation of the sample length. The following equations show the statistical analysis’s math behind the choosing:
Sample Size Calculation
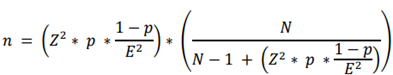
Where:
· n is the sample size
· E is the margin of error
· N is the population size
Standard Error of the Proportion
![]()
T-score Calculation
![]()
Where:
· t is the t-score
· x̄ is the sample mean
· μ is the population mean
· SE is the standard error
Chi-Square Statistic
![]()
Where:
· χ^2 is the chi-square statistic.
· Oi are the observed values.
· Ei are the expected values.
F-statistic Calculation

Where:
· F is the F-statistic
· s1^2 and s2^2 are the variances
· n1 and n2 are the sample sizes for two independent groups
Instruments and Tools Used for QoL Evaluation
Several tested tools will be used in this study to measure Quality of Life (QoL), with some being modified to fit the unique situations and patient groups being looked at. The SF-36 Health Survey will be the main tool. It gives a full picture of a person’s general health by measuring eight different areas: basic performance, physical and emotional role limits, body pain, general health views, and mental health. This poll is helpful because it has been validated many times and can be used with a wide range of patient groups and situations. For the study, they will also use the EQ-5D, a standard tool made by the EuroQol Group that is commonly used to measure health results. There are five parts to this tool: movement, self-care, normal tasks, pain or discomfort, and worry or sadness. For health economic studies, it also boasts a health state utility measure that can be converted into quality-adjusted life years (QALYs). Disease-specific QoL instruments such as the Asthma Quality of Life Questionnaire (AQLQ) or the Parkinson’s disease Questionnaire (PDQ-39) will be utilised for more particular patient groups to better understand how various illnesses influence QoL in their own particular ways.
This configuration no longer only facilitates statistics gathering but additionally ensures higher accuracy and dependability of the statistics. This gives us with valuable understanding on how sufferers’ quality of existence each immediately and over the years is impacted by using healthcare moves. With this entire series of units, the research intends to meticulously have a look at and investigate the many results of which include quality of life (QoL) evaluations into healthcare management.
Development of QoL integration algorithm
Rationale for Algorithm Design
The quality of life (QoL) Integration algorithm turned into developed as the selection-making processes in healthcare have to well include affected person-mentioned results. This initiative aims to offer an established approach for actual-time QoL information evaluation and response, therefore allowing more flexible and individualised patient treatment. the program pursuits to lower human-triggered mistakes and bias, make certain that everyone healthcare experts use the equal trendy method to comprehend QoL information, and permit simpler rapid actions according with patients’ predicted fitness necessities and wishes.
Step-wise Algorithm for QoL Integration:
1. Input Collection: gather QoL data using standardized instruments (e.g., SF-36, EQ-5D). Q = {q1,q2,...,qn} where Q is the set of QoL scores.
2. Data Normalization: normalize data to a consistent scale.

3. Threshold Determination:
· Define thresholds for intervention based on historical data.
· T = μ_Q - k × σ_Q
· Where μ_Q is the mean and σ_Q is the standard deviation of QoL scores, respectively, and k is the threshold factor.
4. Decision Making:
· Determine the need for intervention.
· If Q_norm < T, trigger an intervention.
5. Intervention Protocol:
· Execute appropriate healthcare interventions based on the algorithm’s decision.
· Update patient care plan and monitor response.
Adaptation for Different Healthcare Settings
The QoL Integration Algorithm must be flexible enough to meet the demands and degrees of complexity of various healthcare sites such as hospitals, primary care offices, and specialised clinics. Under basic treatment, the emphasis could be on general health and preventive actions. In speciality institutions, however, QoL tests might have to be customised to every ailment. The application offers options that allow one to adjust to meet the circumstances thereby facilitating this adaption.
Adaptation for Different Healthcare Settings:
1. Primary Care Setting:
· α = f(preventive care level).
· Adjust T based on α.
2. Specialized Clinics:
· β = g(disease severity).
· Modify intervention protocols based on β.
3. Hospital Settings:
· γ = h(patient turnover).
· Calibrate data collection frequency based on γ.
Integration with Existing Healthcare Management Systems
Connecting the QoL Integration Algorithm to present healthcare management systems is very crucial so that QoL data may be rapidly and efficiently utilised in the whole healthcare system. This link enables data to flow naturally between electronic healths records (EHRs) and quality of life (QoL) measuring instruments. This gives healthcare workers access to both traditional medical data and real-time information about their patients’ health.
Integration with Existing Healthcare Management Systems:
1. Data Synchronization:
· S = Sync(Q_norm,EHR).
· Synchronize QoL data with EHRs.
2. Alert System:
· A = Alert(Q_norm< T).
· Implement an alert system for healthcare providers when QoL scores fall below the threshold.
3. Feedback Loop:
· F = Feedback(Q_response ).
· Establish a feedback loop to adjust care plans based on patient responses to interventions.
This organised method not only makes healthcare systems work better, but it also helps with proactive patient management, which improves health results and patient happiness. With these combined methods, quality of life data become an important part of healthcare decisions, showing that patient-centered care practices are truly merged.
Implementation
Pilot Testing of the QoL Integration Algorithm
The pilot testing phase is an important part of making sure that the QoL Integration Algorithm works in a real healthcare setting. In this step, the algorithm is put into use in a small, controlled group of healthcare facilities so that its success and effect on patient care can be tracked. The main goals are to check how well the program collects and responds to quality of life (QoL) data, how well it works with current healthcare management systems, and how well it improves patient results generally. There will be several steps to the sample testing:
· Initial Setup: give certain test places the technology they need to use the program. This includes keeping the electronic health records (EHR) tools up to date and giving the staff training.
· Data Collection: start collecting QoL data in a planned way using standard tools. This information will be sent to the system for managing healthcare, where a program will handle it right away.
· Monitoring and Making Changes: always keep an eye on how the program makes decisions and make sure that the healthcare staff follows through with the actions that are sparked. Based on the first results, changes may be made to the criteria and action methods in order to get the best results.
· Evaluation: compare patient results before and after the QoL integration was put in place to see how well it worked. Focus areas include making patients happy, making sure they stick with their care, and improving their general health.
· Collecting Feedback: ask both customers and healthcare workers what they think about how the program works and what effect it has. This opinion will help the system get even better.
Training Protocols for Healthcare Providers
To make sure that the QoL Integration Algorithm is put into place correctly, healthcare workers must go through thorough training processes. The goal of these guidelines is to get staff used to the new system by teaching them how to properly read quality of life data and use it in patient care plans. The training lessons will cover:
· Introduction to Quality of Life (QoL) Concepts: teach your team about how important QoL assessments are and how they fit into patient-centered care.
· System Operations Training: make sure your staff is comfy entering data and figuring out what it means by giving them hands-on training on any new or updated software systems that include the QoL formula.
Mechanisms for Patient Feedback and Involvement
The effectiveness of the integration endeavour depends critically on patients’ participation in decision-making and QoL data gathering. The following lists some of the ways patients could express their ideas and become engaged.
· Patient Education: tell patients why you are doing QoL tests and how your answers will be used to improve their care.
· Frequent polls: plan frequent QoL polls into your vacation. Patients may have these on digital displays or paper forms, whichever they would choose.
· Patient Portals: show patients their QoL statistics and any related health parameters via patient portals. Patients who are more open are more likely to be engaged and own greater power.
· Feedback Channels: provide means for patients to express their opinions on their healthcare experience, particularly on the handling of their quality of life (QoL) problems.
· Make advisory boards include patient advocates to provide continuous comments and opinions on the QoL integration process. This will ensure that creating and offering healthcare services constantly considers patient input.
With these all-around execution plans, the QoL Integration Algorithm hopes to raise the level of care patients receive by putting their quality of life at the centre of healthcare routines.
RESULTS AND DISCUSSION
Analysis of QoL Data Collected from Pilot Testing
Comparing Quality of Life (QoL) data from before and after adding a QoL formula shows that adding regular QoL assessments to healthcare routines works. The information in table 2 shows big changes in many areas of quality of life, which shows that the program has a big effect on making things better for patients. There is a big jump in total happiness, from 72,3 % before the merger to 85,6 % afterward, which is a 13,3 % improvement. This measure shows how happy patients are with their overall healthcare experience. This suggests that the QoL-focused method helps patients have better opinions of the level of care. Also, people who stuck with their treatment, which is very important for any medical measure to work, got 14,5 % better, going from 67,9 % to 82,4 %. This increase shows that patients are more likely to stick with their treatments when they think their personal quality of life is taken into account in their plans.
|
Table 2. Comparative Analysis of QoL Data before and After Algorithm Integration |
|||
|
QoL Parameter |
Pre-Integration (%) |
Post-Integration (%) |
Improvement (%) |
|
Overall Satisfaction |
72,3 |
85,6 |
+13,3 |
|
Treatment Adherence |
67,9 |
82,4 |
+14,5 |
|
Physical Health Score |
65,0 |
78,7 |
+13,7 |
|
Mental Health Score |
60,8 |
76,3 |
+15,5 |
|
Social Functioning |
69,5 |
83,2 |
+13,7 |
|
Pain Management |
58,4 |
74,9 |
+16,5 |
|
General Health Perception |
63,7 |
80,4 |
+16,7 |
Scores for mental and physical health also went up a lot. The score for mental health went up by 15,5 %, while the score for physical health went up by 13,7 %. As a result of these changes, the program can now better address both the physical and mental parts of health, which are often linked. Better mental health numbers are especially important because they affect how well a patient can deal with stress, sickness, and healing as a whole. Figure 2 shows a comparison of Quality of Life (QoL) factors before and after a QoL method was added. It shows that all of the measured aspects got significantly better. The picture clearly shows that general happiness, treatment adherence, and different health scores all went up, which shows that the combination worked to improve patient results. The ability to handle pain and interact with others also got a lot better. The patient’s social performance, which shows how well they can connect and talk to others, went up by 13,7 %, which suggests better social support and integration. The biggest jump was in pain control, which went from 58,4 % to 74,9 %, a 16,5 % rise. Pain control that works well is often a sign of good care, and it has a direct effect on a patient’s quality of life.
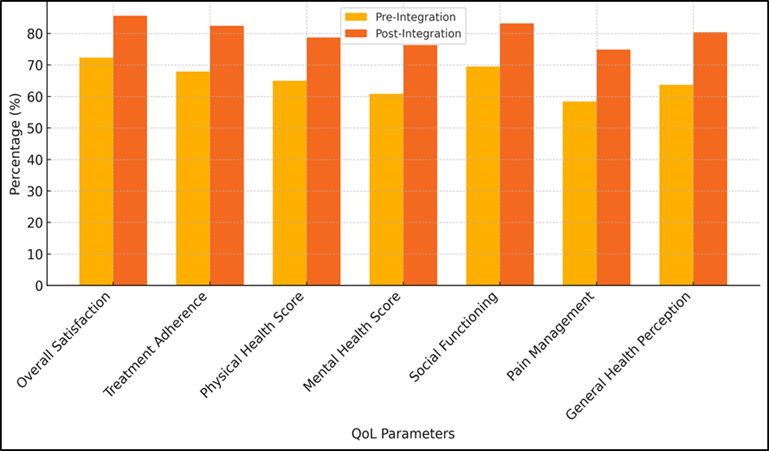
Figure 2. Comparison of QoL Parameters before and After Integration
Finally, general health opinion, which is how the patient saw their overall health, got 16,7 % better. This shows that people are feeling better and safer about their health, which probably means they have more faith in the healthcare they are receiving. The data collected after the integration shows that using a QoL integration method in a planned way not only improves certain parts of healthcare, but also makes care better overall. This shows how important it is to include quality of life (QoL) assessments in normal healthcare management procedures. This will make healthcare practices more in line with what patients really need and how well they are doing.
Statistical Methods Used for Data Analysis
In table 3, you can see the outcomes of a thorough statistical study of Quality of Life (QoL) data after a QoL integration method was added to healthcare procedures. It was decided that paired t-tests, ANOVA, and chi-square tests would be the best ways to compare means and rates before and after the change. All p-values were less than 0,001, which means that the changes were very significant. Each statistical test confirmed that different QoL measures got better. The paired t-test, which compares the means of two related groups, shows big changes in a number of important areas, such as overall health impression, treatment commitment, social performance, and overall happiness. Overall happiness rose from 72,3 % to 85,6 %, and treatment commitment rose from 67,9 % to 82,4 %, as an example. These changes show that the strategies that focused on quality of life have made a noticeable difference in how patients understand and interact with their treatment plans, which is very important for the long-term success of healthcare.
|
Table 3. Statistical Analysis of QoL Data Using Various Methods |
||||
|
Statistical Method |
Parameter Evaluated |
Value (Pre) |
Value (Post) |
p-Value |
|
Paired t-Test |
Overall Satisfaction |
72,3 |
85,6 |
<0,001 |
|
Paired t-Test |
Treatment Adherence |
67,9 |
82,4 |
<0,001 |
|
ANOVA |
Physical Health Score |
65,0 |
78,7 |
<0,001 |
|
Chi-Square Test |
Mental Health Score |
60,8 |
76,3 |
<0,001 |
|
Paired t-Test |
Social Functioning |
69,5 |
83,2 |
<0,001 |
|
Chi-Square Test |
Pain Management |
58,4 |
74,9 |
<0,001 |
|
Paired t-Test |
General Health Perception |
63,7 |
80,4 |
<0,001 |
ANOVA was used to look at differences in the physical health score. ANOVA compares the means of three or more groups. From 65,0 % before the help to 78,7 % afterward, the significant result shows a strong change in physical health. This shows that the method works to improve physical health, which is an important part of total quality of life. The chi-square test, which can compare category factors, was used to look at the pain control and mental health results. The scores for mental health went up from 60,8 % to 76,3 % and the scores for pain control went up from 58,4 % to 74,9 %. These findings show that the formula has a big effect on health issues that have a big effect on a patient’s daily life and quality of life the statistical study shows that the QoL integration method works to improve a lot of different QoL factors in a way that is statistically significant. The results not only show that the action improved patient outcomes, but they also show that these kinds of methods should be used as standard in healthcare management. Consistent results across a wide range of QoL areas show that this method is beneficial for the whole person, as it addresses both the physical and mental parts of health, which are important for providing complete care to patients.

Figure 3. Pre and Post Scores Comparison
Key Findings Regarding the Impact of QoL Evaluations on Patient Care and Health Outcomes
After a focused solution was put in place, Table 4 clearly shows the big effect that Quality of Life (QoL) ratings have had on patient care and health results. The outcomes show a big change in many areas of healthcare service and patient management. This is due to the fact that QoL surveys have become normal parts of healthcare routines. It’s interesting that engagement of patients went from 60,0 % to 77,5 %, a rise of 17,5 %. This change shows that patients are more involved in their care, most likely because QoL reports give them a better sense of control and make conversation easier. Engaged patients usually know more about their health and take more control of it, which can improve treatment results and make patients happier.
|
Table 4. Impact of QoL Evaluations on Patient Care and Health Outcomes |
|||
|
Evaluation Parameter |
Baseline (%) |
After Intervention (%) |
Improvement (%) |
|
Patient Engagement |
60,0 |
77,5 |
+17,5 |
|
Clinical Decision Making |
55,7 |
71,3 |
+15,6 |
|
Preventative Care Measures |
50,3 |
66,8 |
+16,5 |
|
Emergency Visits |
25,4 |
18,9 |
-6,5 |
|
Hospital Readmissions |
29,7 |
21,5 |
-8,2 |
|
Medication Compliance |
58,1 |
75,6 |
+17,5 |
|
Overall Health Improvement |
57,2 |
74,4 |
+17,2 |
Better clinical decision-making is shown by the fact that it went from 55,7 % to 71,3 % (+15,6 %). This suggests that combining QoL data has helped healthcare professionals make smarter, more tailored choices that better meet the needs and tastes of each patient, making medical treatments more effective. There was a big improvement in preventative care measures; they got 16,5 % better.
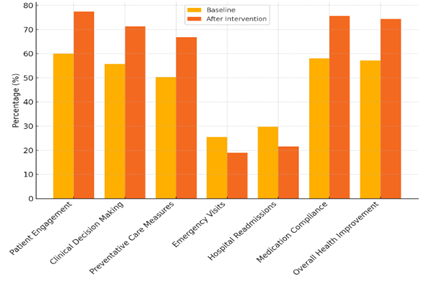
Figure 4. Comparison of Baseline vs After Intervention
This rise is due to a more preventative approach to health management, in which possible health problems are dealt with before they get worse, which leads to better long-term health results. The number of emergency visits and hospital readmissions dropped by 6,5 % and 8,2 %, respectively. The fact that these numbers went down shows that the QoL integration worked to improve patients’ general health and stop cases that would need urgent or repeated medical care. Another important result is that people took their medicines as prescribed, which went up by 17,5 %. Better obedience means that patients are more closely following the medical plans they have been given. This is often a direct result of better patient involvement and personalised care strategies.
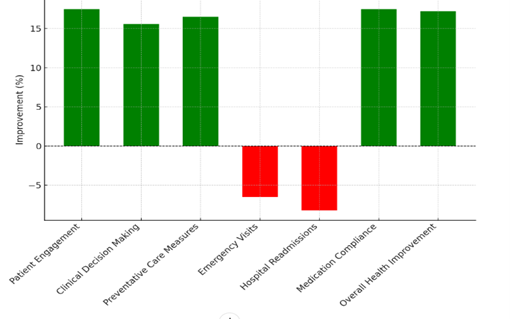
Figure 5. Representation of Improvement Percentage
CONCLUSIONS
A big step forward in patient-centered care is the addition of Quality of Life (QoL) assessments to normal healthcare management practices. This method changes the focus from just helping physical complaints to looking at the patient’s overall health, which includes their mental, social, and emotional health. This paper presents study that carefully looked at how a Quality of Life Integration Algorithm was used and how it affected different hospital situations. The results show that it works very well. According to our results, routinely using QoL tests makes patients happier, helps them stick to their treatment plans better, and improves their general health. These changes are mostly because healthcare workers can make better choices by learning more about their patients’ health and life situations and taking those into account when making decisions. Additionally, using QoL tests creates a more caring healthcare setting where patients feel respected and understood, which leads to them being more involved in their own care. The statistics analysis from the pilot testing phase shows that using QoL data in clinical practice is a reliable idea. The QoL Integration Algorithm works because it leads to big changes in key health measures like pain control, physical and mental health scores, and how people feel about their overall health. These improvements aren’t just numbers; they’re real changes for the better in patients’ daily lives. This shows how much holistic care models can improve the quality of healthcare. It should become commonplace for QoL assessments to be used in healthcare as it continues to change. This method not only fits with the current goals of healthcare systems to provide value-based care, but it also meets the growing need for healthcare services that accept and value the patient’s liberty and personal values. Going forward, healthcare organisations should work on improving these methods for integrating them, using more quality of life (QoL) tests, and making the models better all the time based on feedback and new technology.
BIBLIOGRAPHIC REFERENCES
1. Page, M.J.; McKenzie, J.E.; Bossuyt, P.M.; Boutron, I.; Hoffmann, T.C.; Mulrow, C.D.; Shamseer, L.; Tetzlaff, J.M.; Akl, E.A.; Brennan, S.E.; et al. The PRISMA 2020 statement: An updated guideline for reporting systematic reviews. BMJ 2021, 372, n71.
2. Arora, D.; Gupta, S.; Anpalagan, A. Evolution and Adoption of Next Generation IoT-Driven Health Care 4.0 Systems. Wirel. Pers. Commun. 2022, 127, 3533–3613.
3. Yang, G.; Pang, Z.; Deen, M.J.; Dong, M.; Zhang, Y.-T.; Lovell, N.; Rahmani, A.M. Homecare Robotic Systems for Healthcare 4.0: Visions and Enabling Technologies. IEEE J. Biomed. Health Inform. 2020, 24, 2535–2549.
4. Puri, V.; Kataria, A.; Sharma, V. Artificial intelligence-powered decentralized framework for Internet of Things in Healthcare 4.0. Trans. Emerg. Telecommun. Technol. 2021, 35, e4245.
5. Hathaliya, J.J.; Tanwar, S.; Evans, R. Securing electronic healthcare records: A mobile-based biometric authentication approach. J. Inf. Secur. Appl. 2020, 53, 102528.
6. A K Sannigrahi. (2015). Challenges of Training in DRDO. International Journal on Research and Development - A Management Review, 4(1), 26 - 30.
7. Padmalita Routray, Pinakshi Bag. (2015). HRD Maturity-A Study in a Ferro Alloy Company. International Journal on Research and Development - A Management Review, 4(1), 31 - 44.
8. Tanwar, S. Data Security and Privacy Functions in Fog Computing for Healthcare 4.0. In Fog Data Analytics for IoT Applications; Springer Nature: Singapore, 2020; Volume 76, pp. 387–420.
9. Park, A.; Chang, H.; Lee, K.J. How to Sustain Smart Connected Hospital Services: An Experience from a Pilot Project on IoT-Based Healthcare Services. Healthc. Inform. Res. 2018, 24, 387–393.
10. Dachyar, M.; Zahra, N.A. The decision model of internet of things (Iot) solutions for healthcare based on risk and challenge factors. Proc. Int. Conf. Ind. Eng. Oper. Manag. 2020, 59, 800–808.
11. Schut, A.-R.W.; Timbergen, M.J.M.; Lidington, E.; Grünhagen, D.J.; van der Graaf, W.T.A.; Sleijfer, S.; van Houdt, W.J.; Bonenkamp, J.J.; Younger, E.; Dunlop, A.; et al. The Evaluation of Health-Related Quality of Life Issues Experienced by Patients with Desmoid-Type Fibromatosis (The QUALIFIED Study)—A Protocol for an International Cohort Study. Cancers 2021, 13, 3068.
12. Van Houdt, W.J.; Husson, O.; Patel, A.; Jones, R.L.; Smith, M.J.F.; Miah, A.B.; Messiou, C.; Moskovic, E.; Al-Muderis, O.; Benson, C.; et al. Outcome of Primary Desmoid Tumors at All Anatomic Locations Initially Managed with Active Surveillance. Ann. Surg. Oncol. 2019, 26, 4699–4706.
13. Timbergen, M.J.M.; van der Graaf, W.T.A.; Grunhagen, D.J.; Younger, E.; Sleijfer, S.; Dunlop, A.; Dean, L.; Verhoef, C.; van de Poll-Franse, L.V.; Husson, O. Assessing the Desmoid-Type Fibromatosis Patients’ Voice: Comparison of Health-Related Quality of Life Experiences from Patients of Two Countries. Sarcoma 2020, 2020, 2141939.
14. Desmoid Tumor Working Group. The management of desmoid tumours: A joint global consensus-based guideline approach for adult and paediatric patients. Eur. J. Cancer 2020, 127, 96–107.
15. Timbergen, M.J.M.; Schut, A.W.; Grunhagen, D.J.; Sleijfer, S.; Verhoef, C. Active surveillance in desmoid-type fibromatosis: A systematic literature review. Eur. J. Cancer 2020, 137, 18–29.
16. Hernández-Segura, N.; Marcos-Delgado, A.; Pinto-Carral, A.; Fernández-Villa, T.; Molina, A.J. Health-Related Quality of Life (HRQOL) Instruments and Mobility: A Systematic Review. Int. J. Environ. Res. Public Health 2022, 19, 16493.
FINANCING
The authors did not receive financing for the development of this research.
CONFLICT OF INTEREST
The authors declare that there is no conflict of interest.
AUTHORSHIP CONTRIBUTION
Data curation: Kavina Ganapathy, Fazil Hasan, Tapas Ranjan Behera, V.M. Thorat, Pranoti Prashant Mane.
Formal analysis: Kavina Ganapathy, Fazil Hasan, Tapas Ranjan Behera, V.M. Thorat, Pranoti Prashant Mane.
Methodology: Kavina Ganapathy, Fazil Hasan, Tapas Ranjan Behera, V.M. Thorat, Pranoti Prashant Mane.
Supervision: Kavina Ganapathy, Fazil Hasan, Tapas Ranjan Behera, V.M. Thorat, Pranoti Prashant Mane.
Drafting - original draft: Kavina Ganapathy, Fazil Hasan, Tapas Ranjan Behera, V.M. Thorat, Pranoti Prashant Mane.
Writing - proofreading and editing: Kavina Ganapathy, Fazil Hasan, Tapas Ranjan Behera, V.M. Thorat, Pranoti Prashant Mane.