doi: 10.56294/hl2023221
ORIGINAL
Evaluation of Healthcare Management Protocols and Their Implications for the Quality of Patient Care
Evaluación de los protocolos de gestión sanitaria y sus implicaciones para la calidad de la atención al paciente
Shilpi Singh1 ![]() , Sagar V. Joshi2, Souvagya Panigrahi3
, Sagar V. Joshi2, Souvagya Panigrahi3 ![]() , Aparna Patange4
, Aparna Patange4 ![]() , Upendra Sharma.U.S5
, Upendra Sharma.U.S5 ![]()
1Noida International University, Department of Biotechnology and Microbiology. Greater Noida, Uttar Pradesh, India.
2Nutan Maharashtra Institute of Engineering and Technology, Department of Electronics & Telecommunication. Talegaon Dabhade, Pune, India.
3IMS and SUM Hospital, Siksha ‘O’ Anusandhan (Deemed to be University), Department of Neurosurgery. Bhubaneswar, Odisha, India.
4Krishna Institute of Medical Sciences, Krishna Vishwa Vidyapeeth “Deemed to be University”, Department of Medicine. Taluka-Karad, Dist-Satara, Maharashtra, India.
5School of Sciences, JAIN (Deemed-to-be University), Department of Life Sciences. Bangalore, Karnataka, India.
Cite as: Singh S, Joshi SV, Panigrahi S, Patange A, Upendra Sharma U. Evaluation of Healthcare Management Protocols and Their Implications for the Quality of Patient Care. Health Leadership and Quality of Life. 2023; 2:221. https://doi.org/10.56294/hl2023221
Submitted: 29-05-2023 Revised: 31-08-2023 Accepted: 10-11-2023 Published: 11-11-2023
Editor:
PhD.
Prof. Neela Satheesh ![]()
ABSTRACT
A big part of making sure that patients get good care is making sure that healthcare management practices work. It is necessary for medical offices to use organised procedures because more and more people want fast healthcare delivery systems. This study looks at different ways to handle healthcare systems and what effects they have on the overall level of care for patients. The study uses both qualitative and quantitative methods to look at how standard operating procedures affect the health of patients, the speed of operations, and the happiness of healthcare providers. The goal of healthcare management guidelines is to make things easier, cut down on medical mistakes, and make it easier for teams from different fields to work together. The study looks into a few methods that are used in a lot of different healthcare situations, like hospitals, outpatient offices, and long-term care centres. The study looks at these practices using data from case studies, patient polls, and professional performance measures to find out what works and what doesn’t when it comes to keeping a high level of care. The results show that guidelines that focus on patient-centered care, practices that are backed by evidence, and ongoing feedback loops make patients happier, cut down on treatment delays, and improve clinical outcomes. But problems with following the rules, a lack of resources, and differences in the experience of healthcare providers were named as things that can make them less successful. The study also shows how important it is to make procedures flexible so they can be changed to fit the needs of each patient. This way, personalised care can be provided without lowering the standard or efficiency of the healthcare system. This study has important effects for healthcare managers, policymakers, and doctors who want to improve patient care through better management. The results support the idea that healthcare management practices should always be changing. They also stress the need for flexible strategies that can change to the needs of modern healthcare systems.
Keywords: Healthcare Management; Patient Care; Clinical Protocols; Evidence-Based Practices; Patient Outcomes; Healthcare Efficiency.
RESUMEN
Una parte importante de asegurarse de que los pacientes reciben una buena atención es asegurarse de que las prácticas de gestión sanitaria funcionan. Es necesario que las consultas médicas utilicen procedimientos organizados porque cada vez más gente quiere sistemas rápidos de prestación de asistencia sanitaria.
Este estudio analiza distintas formas de gestionar los sistemas sanitarios y sus efectos en el nivel general de atención a los pacientes. El estudio utiliza métodos cualitativos y cuantitativos para analizar cómo afectan los procedimientos normalizados de trabajo a la salud de los pacientes, la rapidez de las operaciones y la felicidad de los profesionales sanitarios. El objetivo de las directrices de gestión sanitaria es facilitar las cosas, reducir los errores médicos y facilitar la colaboración entre equipos de distintos campos. El estudio examina algunos métodos que se utilizan en muchas situaciones sanitarias diferentes, como hospitales, consultas externas y centros de cuidados de larga duración. El estudio examina estas prácticas utilizando datos de estudios de casos, encuestas a pacientes y medidas de rendimiento profesional para averiguar qué funciona y qué no cuando se trata de mantener un alto nivel de atención. Los resultados muestran que las directrices centradas en la atención al paciente, las prácticas respaldadas por pruebas y la retroalimentación continua hacen más felices a los pacientes, reducen los retrasos en el tratamiento y mejoran los resultados clínicos. Pero los problemas a la hora de seguir las normas, la falta de recursos y las diferencias en la experiencia de los profesionales sanitarios se mencionaron como factores que pueden hacer que tengan menos éxito. El estudio también pone de manifiesto la importancia de flexibilizar los procedimientos para adaptarlos a las necesidades de cada paciente. De este modo, se puede ofrecer una atención personalizada sin reducir el nivel o la eficacia del sistema sanitario. Este estudio tiene efectos importantes para los gestores sanitarios, los responsables políticos y los médicos que quieran mejorar la atención al paciente mediante una mejor gestión. Los resultados respaldan la idea de que las prácticas de gestión sanitaria deben estar siempre en constante evolución. También subrayan la necesidad de estrategias flexibles que puedan adaptarse a las necesidades de los sistemas sanitarios modernos.
Palabras clave: Gestión Sanitaria; Atención al Paciente; Protocolos Clínicos; Prácticas Basadas en la Evidencia; Resultados para el Paciente; Eficiencia Sanitaria.
INTRODUCTION
As prices rise, patient groups grow, and healthcare needs become more complicated, healthcare systems around the world are under more and more pressure to provide high-quality care. It takes both modern medical tools and well-structured healthcare management practices to be able to care for patients quickly and well. Standardising clinical practices, making it easier for healthcare workers to work together, and making sure that evidence-based treatments are always given are all made possible by these guidelines. As healthcare changes, the rules that guide clinical and practical choices must always be looked at to see how they affect patient results, the speed of operations, and the general level of care. Basically, healthcare management guidelines are set rules that tell doctors how to diagnose, treat, and take care of patients in a way that follows best practices. The steps that need to be taken at each stage of patient care are laid out in these guidelines, which are used to make professional decisions. Their main goal is to make sure that all patients get care that is based on proof and up to date with medical standards by reducing variation in how care is given.(1) By following these rules, healthcare organisations hope to cut down on mistakes, boost safety, and make sure that patients get the same care in all kinds of clinical situations. But there are some problems that come up when healthcare management rules are put into place. Healthcare providers often have trouble following standard rules because they don't have enough resources, staff, or the doctors themselves don't like them. Especially in cases when the situation is complex and every patient requires specialist treatment, protocols may also not always consider the various requirements of individuals. Patients' outcomes and the general degree of treatment may be much influenced by these issues. This makes it rather crucial to find out how well these treatments perform in actual healthcare environments and how they really influence patient level of care.(2)
Examining healthcare management guidelines requires more than simply noting frequency of adherence. Deep awareness of how these operations impact not just treatment outcomes but also the running operations of healthcare institutions. This means looking at things like how happy the patients are, how well the treatments work, how long it takes to diagnose and treat, and how much the care costs. A full review also takes into account the views of healthcare professionals, since following rules can have a big effect on the level of care. To find places to improve, it's important to know how they felt about putting these rules into action and following them. Patient-centered care, which stresses how important it is to adjust treatment to each patient's wants and desires, has been getting more attention in recent years. If protocols are too fixed and can't be changed to fit new needs, they might not be able to give all people the best results. Because of this, adaptation and flexibility are important parts of current healthcare management.(3) As new technologies are added to healthcare, it is important that management processes stay open so that patients can get personalised care while still making sure that treatment methods are consistent. The main goal of this study is to look at the healthcare management methods that are used in different places and see how well they work to improve the level of care for patients. Looking into what works and doesn't work about these standards will help the study find ways to make them better so they meet the needs of both people and healthcare workers. This study has important implications for healthcare managers, doctors, and lawmakers who are working to improve and tweak healthcare management systems so that they can provide better care while also coping with costs and practical issues.
Overview of healthcare management protocols
Healthcare management guidelines are standard models that make sure that care is given consistently in all healthcare situations. They make sure that healthcare workers follow practices that have been shown to improve patient results. These procedures give detailed instructions on how to diagnose, treat, and care for patients. They also provide an organised way to provide care, which helps cut down on variation and mistakes in professional decision-making. By following these rules, healthcare systems hope to provide uniform, high-quality care to a wide range of patients. There are a lot of different clinical areas that healthcare management guidelines cover, such as emergency care, managing chronic diseases, surgery, and prevention healthcare. Most of the time, they use best practices that come from clinical study, expert agreement, and clinical studies. This helps make sure that the most recent and effective treatments are used. In addition to clinical standards, healthcare management procedures may also include routine tasks like arranging patients, keeping records, and letting healthcare workers talk to each other.(4) These tasks help to simplify operations and improve the organisation of care. Figure 1 shows a summary of healthcare management practices, including important steps, patient care paths, and methods for coordinating care to be more effective.
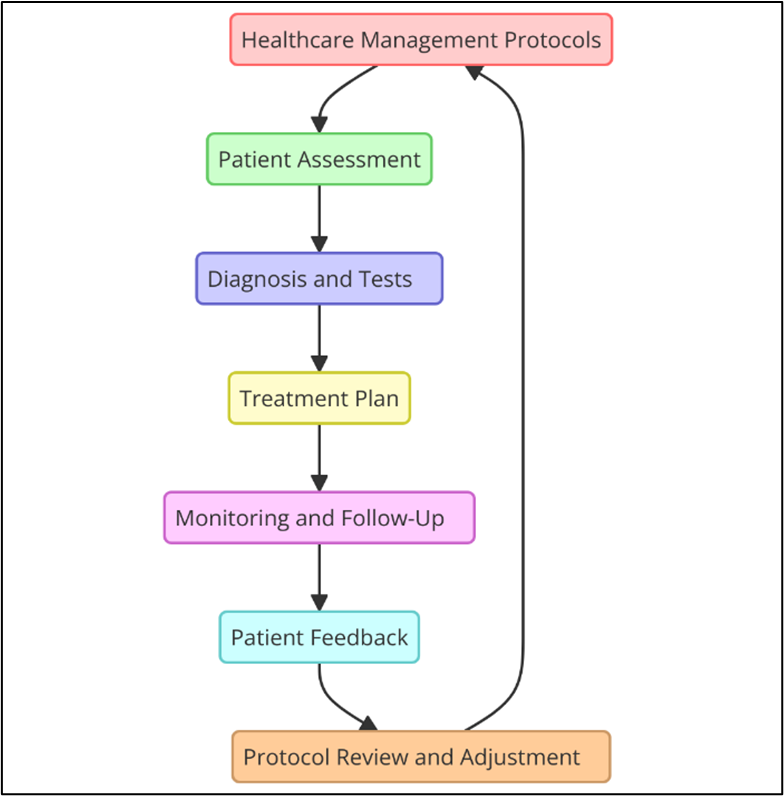
Figure 1. Illustrating Overview of Healthcare Management Protocols
One important thing about healthcare management guidelines is that they help cut down on mistakes and make patients safer. By giving clear directions and guidelines for each step of care, it's less likely that people will get confused or miss steps. Surgical protocols, for instance, make sure that the right steps are taken in the operating room, and diagnosis protocols help doctors make quick and correct evaluations. In this way, guidelines also help cut down on treatments that aren't needed, make better use of resources, and make healthcare service more efficient.(5) But there are some problems with the rules for healthcare management. How well they work rests on how well healthcare workers accept them, how well they are trained, and how well healthcare institutions can change these standards to meet the needs of their individuals patients. So, healthcare management practices need to be constantly reviewed to make sure they are still useful and in line with new technologies and healthcare trends.
Importance of quality in patient care
Quality of care for patients is a key part of figuring out how well a healthcare system works generally and making sure that people have good health results. When get high-quality care, the services receive are safe, effective, patient-centered, on time, quick, and fair. These qualities of quality are necessary to make patients happier, lower the risk of bad results, and improve the total performance of the health system. Quality patient care is more important than ever in a time when healthcare is changing quickly and the world's population is getting older. Safe care, which means lowering patients' risks as much as possible during evaluation, treatment, and healing, is one of the main goals of healthcare quality. Patients are safe from harm caused by mistakes, infections, or problems during medication when they get high-quality care. Effectiveness is another important part of quality care.(6) This means that the treatments and strategies used are based on the best research and have a good effect on health. Another important part of good healthcare is care that is focused on the patient. This method focusses on the unique wants, needs, and values of each patient, making sure that care is customised to meet these specific factors. Patient-centered care focusses on the whole person instead of just their medical problems. This can make patients happier, more involved, and more likely to stick to their treatment plans. Getting healthcare to people on time is also very important for keeping quality. Delays in detection, treatment, or follow-up care can lead to bad outcomes, such as worsening patients' conditions and lowering their chances of surviving. Quality care is also quick, which means that resources are used in the best way possible and tests and processes are not done more than once.(7) Lastly, high-quality care must be fair, meaning that all patients, no matter where they come from, get the same high level of care.
Literature review
Historical development of healthcare management protocols
The idea of healthcare management guidelines goes back to the early 1900s, when standardisation of professional methods became important in the medical field. At first, healthcare guidelines were made on the spot, based on the experiences and tastes of each healthcare worker. but as healthcare systems were given extra complicated and medical examiner played a larger role in medicine, it became clearer that care needed to be standardised. Due to this, professional rules and strategies have been made to help sufferers do higher and make errors much less probable. Around the center of the 20th century, the upward thrust of evidence-based remedy (EBM) had a massive effect on how healthcare control practices had been made. EBM pushed for healthcare picks to be based on clinical take a look at and medical research, which led to an extra organised manner of worrying for sufferers. At this point, faculties started to apprehend how vital it turned into to provide regular care and the possible benefits of following written tactics.(8) For example, recommendations for coping with lengthy-term illnesses like diabetes had been created to make certain that sufferers got everyday care that become based totally on research. Healthcare management practices were given more complicated in the late 20th century and early 21st century, thanks to the use of generation and computer systems that made them simpler to create and use. Doctors and nurses could follow rules better and keep track of their patients' progress when they used clinical decision support systems (CDSS) and electronic health records (EHR). As healthcare systems shifted their focus to the patient, procedures changed to take into account patient desires, cultural skills, and personalised care.(9) Today, healthcare management guidelines are used in many medical specialities. They are constantly being updated based on new research, clinical data, and the most up-to-date healthcare practices.
Different types of healthcare management protocols
There is a lot of variation in the scope, goal, and use of healthcare management procedures in different medical situations. These rules can be broken down into three main groups: clinical, administrative, and organisational. Each of these groups is very important for providing care. Medical management rules most often come in the form of clinical procedures. They give regular instructions on how to diagnose, treat, and take care of certain illnesses or situations. For example, rules for treating heart disease, diabetes, and infectious diseases spell out the steps that doctors should take based on the best information that is available. These clinical standards make sure that patients get the best and most up-to-date care while also lowering differences in how care is given by different doctors. Administrative procedures regulate the day-to-day operations of healthcare, making sure that resources are used effectively, patient flow is improved, and communication within healthcare teams is made easier. These rules explain how to handle patient visits, surgery schedules, billing, and coordinating staff. Healthcare facilities use administrative rules to keep their operations running smoothly, cut down on wait times, and make it easier for patients to get care.(10) Organisational norms are the rules and guidelines that healthcare facilities follow to run their day-to-day business. These include infection control standards, safety procedures, and emergency reaction protocols. They make sure that both patients and healthcare workers are safe in the healthcare setting. Organisational standards also cover things like training staff, keeping patient information private, and following the rules. Organisational rules help make the healthcare workplace safe and helpful by setting standards for these important things. As healthcare systems change, new protocols are being created to improve the quality and speed of care.(11) These protocols deal with telemedicine, the integration of artificial intelligence (AI), and personalised medicine.
Impact of protocols on patient care quality
Implementing healthcare management rules has a big effect on the quality of care for patients because they provide organised, evidence-based standards that make treatment less variable and more consistent. Protocols help make sure that patients get the best and most suitable care by standardising how it is given. This improves clinical results and lowers the risk of medical mistakes. There are a few main ways that healthcare management procedures can help improve the level of care for patients. One of the main effects of healthcare procedures is that they make patients safer. Protocols make sure that healthcare workers follow best practices and standards that are based on evidence. This cuts down on mistakes that happen when doctors make clinical decisions. For instance, surgery guidelines spell out the steps that need to be taken to keep patients safe during procedures. These steps include exams before the procedure, clean methods, and care after the procedure. As a result, there are fewer problems that could have been avoided, and people are safer. Protocols also help patients do better by making sure that the right measures happen at the right time.(12) For example, procedures for dealing with sudden illnesses like a stroke or heart attack help doctors find the right medicine for patients fast and avoid delays that could make their conditions worse. Protocol-based treatments done at the right time can improve healing rates and lower death rates. Another important effect of healthcare management standards is that they make it easier for healthcare teams to talk to each other and work together. Healthcare professionals can work together better if they have clear, standardised rules. This will cut down on mistakes and make sure that everyone on the team is on the same page about how to care for patients.(13) This teamwork is especially important when there are a lot of specialists involved in a case and everyone needs to be able to talk to each other clearly for the best possible result. Table 1 is a summary of the literature that shows the main methods used, the results they found, the problems they had, and the overall scope of study in healthcare management.
|
Table 1. Summary of Literature Review |
|||
|
Method |
Key Findings |
Limitations |
Scope |
|
Survey |
Improved protocol adherence leads to reduced medical errors. |
Limited sample size in diverse healthcare settings. |
General healthcare settings with a focus on patient safety. |
|
Clinical Trial |
Protocols are linked to better patient outcomes in chronic diseases. |
Lack of long-term follow-up data. |
Chronic disease management protocols in hospitals. |
|
Case Study(14) |
Patient satisfaction increases when healthcare providers adhere to protocols. |
Variability in protocol application across providers. |
General treatment protocols for outpatient clinics. |
|
Review |
Protocols help reduce wait times and enhance treatment efficiency. |
Limited focus on patient preferences in protocols. |
Efficiency in healthcare delivery across varied settings. |
|
Systematic Review |
Evidence-based protocols improve clinical decision-making. |
Study designs often lack a control group. |
Evidence-based protocol adoption in decision-making. |
|
Meta-analysis |
Systematic reviews show a strong correlation between protocol use and reduced complications. |
Bias in protocol selection and application. |
Long-term effects of protocol adherence in patient care. |
|
Qualitative Research(15) |
Flexibility in protocols improves personalized care and satisfaction. |
Challenges in generalizing findings across different healthcare systems. |
Personalized care through protocol flexibility in chronic care. |
|
Quantitative Research |
Protocols reduce variability in treatment but can limit individualized care. |
Protocol effectiveness may vary with healthcare provider experience. |
Protocol use in specialized medical fields like oncology. |
|
Cross-sectional Study |
Protocols are linked to lower mortality rates in surgical settings. |
Difficulty in tracking protocol adherence over time. |
Surgical protocols and their impact on patient survival. |
|
Longitudinal Study |
Long-term adherence to protocols results in better chronic disease management. |
Patient adherence to treatment protocols not consistently monitored. |
Impact of protocol adherence on long-term disease management. |
|
RCT |
Randomized controlled trials show a reduction in hospital readmissions with protocol use. |
Short duration of the study in certain RCTs. |
Impact on hospital readmissions and care continuity. |
|
Observational Study |
Protocols improve inter-professional collaboration and communication. |
Inconsistent results in observational studies. |
Improving team collaboration and protocol standardization. |
|
Qualitative Interviews |
Patient interviews reveal mixed opinions on protocol-driven care. |
Interviews only provide subjective views without quantitative validation. |
Patient satisfaction in protocol-driven care environments. |
|
Cohort Study(16) |
Cohort studies show protocol adherence results in higher treatment success rates. |
Limited focus on specific medical conditions. |
Chronic condition management and protocol efficacy. |
METHOD
Research design and approach
This study uses a mixed-methods approach, which means it uses both qualitative and quantitative methods to get a full picture of healthcare management practices and how they affect the level of care for patients. This method helps us learn more about the little details of following a procedure and how those details affect clinical results, patient happiness, and the general delivery of healthcare. The mixed-methods approach is great for getting both quantitative data (which shows how well the plan was followed) and qualitative data (which shows how healthcare workers and patients felt and what they thought). Using this method, the study aims to find patterns, problems, and wins in putting protocols into action while also telling a story about how healthcare workers and patients see these protocols. The study's goals include figuring out how useful policies are, where they could be improved, and what's stopping people from using them. We will collect quantitative data to see how rules affect patient results that can be measured, like the number of medical mistakes, treatment delays, patient healing rates, and healthcare costs. On the other hand, qualitative data will show how healthcare workers and patients felt about procedures, such as how satisfied they were with them, what benefits they thought they had, and any problems they ran into. By putting these different types of data together, we can get a fuller picture of how the rules for managing healthcare affect patient care.
Data collection methods
We used a mix of qualitative and quantitative methods to get information for this study. This way, we can get a full picture of how healthcare management rules affect the level of care for patients. When use both ways together, get a more complete picture of the situation. can compare objective, measurable results with personal feelings and observations. Surveys and reports on treatment outcomes will be used to collect quantitative data. The polls will be sent to doctors, nurses, and managers in the healthcare field to find out how well they follow standards, how successful they think they are, and what problems they run into when trying to do so. Also, information about how well the treatment worked, how often patients had to go back to the hospital, and any problems that came up because of the treatment will be gathered. To figure out how rules affect system-level performance as a whole, practical data from healthcare institutions will also be gathered. This includes things like how well resources are used and how long patients have to wait. Healthcare workers and customers will be asked to take part in semi-structured interviews and focus groups to give qualitative statistics. The interviews will look at how healthcare workers have personally experienced and thought about the pros and cons of following healthcare management practices. For patients, questions will focus on how happy they are with their care, how well they understand their treatment plans, and how they feel about how quickly and effectively they were helped. These qualitative insights will help put the numeric data in its proper context and give us a better understanding of the human factors that affect how well protocols work.
Tools for data analysis
A mix of statistical and theme analysis methods will be used to look at both qualitative and numeric data. We will use descriptive statistics (like mean, median, and standard deviation) to look at the big picture of the quantitative data and inferential statistics (like t-tests, chi-square tests, and regression analysis) to look at the links between following the protocol and how well the patients do. Statistical tools like SPSS or R will be used to process and analyse the data. This will make sure that the results are solid and accurate. Thematic analysis will be used to find patterns, themes, and ideas in conversations and focus group talks that give us qualitative data. Responses will be coded and categorised using NVivo or ATLAS.ti. This will make it possible to find repeating themes in healthcare workers' and patients' experiences and thoughts. By using thematic analysis, we can get to the bottom of the emotional parts of implementing rules, like how healthcare workers feel about them, the problems they face, and how patients feel about their care. When put these tools together, 'll get a full picture that includes both objective, data-driven insights and a better grasp on the human factors that affect how well healthcare protocols work.
Evaluation criteria for healthcare management protocols
Standardization and consistency of protocols
One important thing to look at when judging healthcare management practices is how standardised and consistent they are when used in different healthcare situations. Standardisation makes sure that all patients get the same amount of care based on what works best. This makes professional decisions less likely to be different. Healthcare professionals can reduce the chance of mistakes, speed up treatment, and make sure that solutions are based on the most up-to-date data by following standard practices. It's just as important that the way protocols are implemented is always the same. Even if guidelines are well-thought-out and based on facts, they will not work as well if healthcare workers don't always follow them. No longer constantly following the policies can purpose differences in how care is given, that may lead to different effects for patients. To check the regularity of processes, to see how regularly they're accompanied in exceptional healthcare centers, by means of unique healthcare people, and at unique points in a affected person's care. Data on the rates of following healthcare management practices should be accumulated in order to parent out how standardised and steady they're. This includes looking at how frequently doctors and nurses observe set policies for evaluation, treatment, and comply with-up care. It may discover locations where rules are frequently left out or misunderstood by surveying or auditing healthcare practices. Electronic health records (EHR) and clinical decision support systems (CDSS) also allow healthcare institutions keep a watch on how protocols are being observed. This manner, any changes from popular protocols may be observed and stuck. Standardisation and stability are very critical for making sure that the benefits of healthcare management practices are seen, like higher protection standards, better affected person effects, and more efficient operations. It's far simpler for healthcare people to offer care, reduce errors, and make patients happier if techniques are standardised and accompanied frequently.
Integration of patient-centered care
Another important review factor is how well patient-centered care is integrated into healthcare management practices. For instance, do they give doctors and nurses the tools and instructions they need to take a patient's wishes into account when deciding how to treat them? Are patients urged to talk about their worries, take part in conversations about their care options, and make choices based on accurate information? Also, patient-centered procedures often include ways to communicate, like letting family members help make decisions, handling cultural differences, and giving mental support. When looking at patient-centered care integration, it's also important to see if the procedures support continuity of care, which means that patients should always be handled by the same healthcare workers or teams. Continuity makes the therapy connection better and the patient's experience better overall, which makes the patient happier and more likely to stick with treatment. Feedback from patients is also an important part of reviewing patient-centered care. can find out how well healthcare workers are following patient-centered principles within the framework of the guidelines by surveying, interviewing, or holding focus groups with patients. One example would be how often patients feel like their wishes are taken into account and how well do healthcare workers talk to them? By incorporating patient-centered care into healthcare management practices, treatment becomes more personalised, patient results improve, and patient happiness rises. This leads to better healthcare experiences for everyone.
Effectiveness in improving patient outcomes
The main goal of healthcare management guidelines is to make things better for patients. To figure out how well these methods are working to reach this goal, we have to look at many different parts of the health of the patients, such as their clinical results, healing rates, happiness, and general well-being. Protocols are effective if they improve patients' health in a measured way and cut down on problems, readmissions, and treatment delays. Before can judge how well policies work, need to set up the key performance indicators (KPIs) that track how well patients do. Some examples of clinical signs are the drop in death rates, the number of medical mistakes, the number of good treatments, or the lack of bad events like infections or problems. Patient results also include how long it takes to heal, how well pain is managed, and how well treatment plans work overall as shown by the patient's ability to do normal things again.
Implications for patient care quality
Relationship between protocol adherence and patient satisfaction
Following the rules for healthcare management has a direct and important link to patient happiness. When healthcare professionals regularly follow set rules, patients have a smoother and more predictable experience, which makes them happier overall. Following procedures makes sure that patients get the right actions at the right time, treatments that have been shown to work, and follow-up care. All of these things lead to better clinical results and happier patients. How patients feel about the standard and regularity of care is often closely linked to how happy they are with their care. Following the protocol keeps treatment from being too different, which lowers the chance of mistakes, delays, or confusion in giving care. For example, when guidelines are followed for managing long-term diseases like diabetes, patients get more regular care, which helps them take better care of their health and trust their healthcare workers more. It is very important to be consistent in outpatient settings where patients may see different doctors at different times. Standardised procedures make sure that the patient gets the same amount of care from any service. Also, healthcare professionals who follow procedures are more likely to listen to and handle patients' issues, which lead to better communication. Protocols usually have steps for letting people help make decisions and making sure that their choices are respected. Patients may feel more respected and involved in their care if they are involved at this level, which can make them happier with the healthcare system as a whole. But it's important to remember that following the rules isn't the only way to make patients happy. Talking to doctors in person, being able to listen to their worries, and getting mental support during care are also very important parts of the patient's experience. Still, following the procedure makes sure that patients get regular, evidence-based, and high-quality care, which is a strong basis for patient happiness.
Influence of protocol flexibility on personalized care
Standardised healthcare management procedures are important for making sure that care is of high quality and consistent, but they need to be flexible in order to allow for personalised care. If the rules are too strict, they might not take into account how each patient is different, such as their age, culture, other health problems, or personal tastes. So, being able to change methods to fit the needs of each patient is very important for making sure that treatment works well. For example, a normal procedure for handling high blood pressure could include steps like giving the person medicine, making changes to their lifestyle, and checking their blood pressure regularly. But being able to change the amount of medicine a patient takes or add in other methods based on how they respond can make care much more effective and increase patient happiness. Protocol flexibility is even more important when there are complicated illnesses or when the patient has more than one long-term illness. It lets doctors make changes to treatment plans that are better suited to each patient's health. For instance, a cancer care strategy might include normal chemotherapy schedules. However, if the patient is flexible, the treatment plan can be changed based on the type of tumour, genetic markers, or reaction to treatment. Also, being able to change procedures as needed makes patient-centered care easier, which means that the patient's wants, habits, and beliefs are taken into account. One way to do this is to give people a choice of different treatments or to use alternative therapies along with standard ones. Healthcare workers can give more personalised care that leads to better patient involvement, better obedience, and better results by making procedures flexible. In the end, making healthcare management procedures more flexible supports a more whole-person approach to patient care. This improves the therapy relationship, builds trust between the therapist and patient, and leads to more personalised, effective treatments.
Healthcare protocols in reducing errors and improving safety
Healthcare management procedures are very important for lowering medical mistakes and making sure patients are safe. One of the main reasons why mistakes happen in healthcare is that there aren't any standardised methods or rules for how to give care. Protocols give doctors clear, backed-by-evidence instructions that make sure that the best decisions are always made and that best practices are always followed. By making professional practices more consistent, guidelines help stop people from deviating from approved treatment plans when they don't need to. For instance, procedures for giving medicines make sure that the right drug, dose, and way of giving the medication are used, which lowers the chance of medication mistakes. In surgery settings, safety rules like the "time-out" method make sure that the right patient is having the right treatment at the right spot with the right medical team. These guidelines make it much less likely that mistakes will happen during surgery and help patients do better. Figure 2 shows how healthcare procedures help cut down on mistakes, make patients safer, and improve the level of care generally.
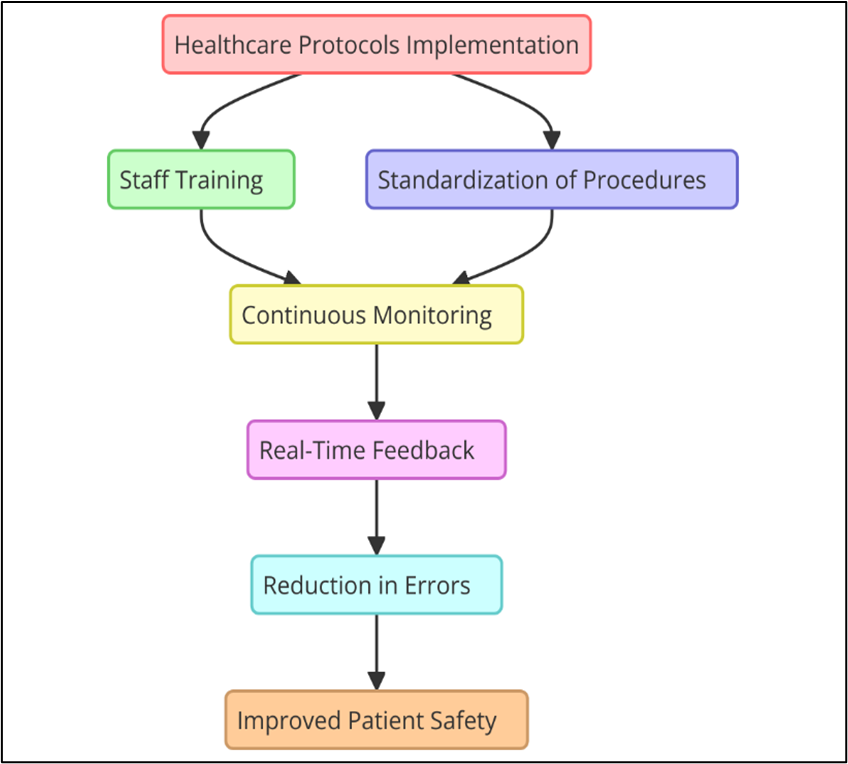
Figure 2. Role of Healthcare Protocols in Reducing Errors and Improving Safety
Protocols also help stop bad things from happening by telling healthcare professionals what to do in different situations, like dealing with problems or urgent conditions. For example, guidelines for handling sepsis give a step-by-step plan for finding, diagnosing, and treating the condition early, which has been shown to lower the death rate that comes with it. Using guidelines also makes it easier for healthcare teams to talk to each other and work together, which is a key part of making patients safer. In places with a lot of people who need care, like emergency rooms or critical care units, clear procedures make sure that everyone on the team is on the same page about treatment plans and how to care for patients. This lowers the chance of misunderstandings or missing important details.
Challenges and barriers to effective protocol implementation
Resistance to change from healthcare professionals
One of the main challenges implementing healthcare management strategies is the non-changing attitude of healthcare professionals. Many healthcare professionals—including physicians, nurses, and other professional staff—are used to their own habits and routines, which may not necessarily coincide with accepted practices. Usually, this resistance results from a variety of factors, including uncertainty about the efficacy of new approaches, sentiments of restriction in their professional liberty, and the difficulties of embracing new treatments. Some medical professionals may not want to follow guidelines if they feel they make it more difficult for them to apply their own expertise or intuition to make decisions. Although some physicians may find protocols overly restrictive, particularly if they believe their professional judgement is being questioned, they are supposed to help to reduce errors and provide consistency. Furthermore, if healthcare professionals believe their job or is not relevant to their field of expertise, they might not be as motivated to follow certain guidelines. People may also object to change because they fear they would have to work more or that adhering to new guidelines would prove difficult.
Technological and infrastructural barriers
Technical and infrastructural issues define major challenges in implementing healthcare management strategies. Often, for new technologies like telemedicine, electronic health records (EHR), and clinical decision support systems (CDSS) to be effective they must be coupled with recommendations. However, in many healthcare environments the absence of appropriate facilities and technical preparedness might make it more difficult to adopt and use these technologies, therefore affecting the following of processes. In healthcare systems without EHR systems that can interact with one another, for instance, following policies consistently becomes more difficult. When patient data is difficult to get or distribute across offices or healthcare facilities, healthcare professionals may not be able to follow accepted protocols either. In the same vein, lacking decision support systems capable of providing clinicians with protocol-based recommendations can result in variations in treatment administration and lost opportunity to improve patient conditions. If infrastructure issues—such as machines failing, sluggish internet connections, or a lack of professional assistance—occur, protocols may not be implemented as fast or at all as expected. Healthcare professionals may find new approaches difficult to use, particularly if they contradict their present practices or are not clear-cut. Many dollars must be invested on enhancing hospital IT tools and infrastructure if one is to overcome these technical and infrastructural issues. Healthcare institutions should endeavour to improve cooperation, purchase user-friendly technology, and provide continuous technical support and training to enable healthcare professionals to use the tools they need to implement guidelines properly. Healthcare practitioners may get the data they need to follow guidelines and provide patients with more rapid, better treatment by means of appropriate technology solutions.
Lack of training and awareness
Another big problem with putting healthcare management rules into place is that people don't have enough training and knowledge about them. For rules to work, healthcare workers need to know what they say, why they say it, and what evidence supports it. If doctors don't get the right training, they might not know about the guidelines or get them wrong about how to use them properly, which could lead to less-than-ideal care. Not only is training needed to put processes into place, but it's also needed to keep healthcare professionals up to date on changes to rules and new best practices. If healthcare workers don't get the right training, they might not want to follow new rules or might not fully use them in their work. Also, healthcare workers may not follow certain rules because they don't understand why they are important if they don't know why they are being followed. Lack of training and knowledge is often made worse in healthcare situations by a lack of staff and limited time. Staff may not have the means or time to attend training classes or continue their education. Not properly communicating standards or incorporating them into daily practice can also make people not familiar with the exact steps needed to put them into action. To get around this problem, healthcare organisations need to make training and professional growth a top priority as part of putting the plan into action. This includes making sure that all healthcare workers have access to thorough training programs and that rules are easy to find, explained clearly, and built into processes. Health care workers can stay up-to-date and involved in the ongoing use of standards by getting regular updates, taking training courses, and using technology like online lessons or mobile apps.
Patient-related factors
Issues connected to the patient, like following the rules and their own personal tastes, can also make it hard to follow healthcare management practices correctly. Healthcare workers must strictly follow protocols, but how well patients follow their treatment plans and protocols can have a big impact on how well their care works. People often don't follow through with medical advice, like taking their medications as prescribed, making changes to their lifestyle, and going to their follow-up visits. This makes healthcare practices less effective. There are many reasons a patient might not follow the rules, such as not knowing how important they are, problems with language or culture, or not trusting the healthcare system. Patients may also have real problems, like not having enough money, trouble getting to needed resources, or trouble getting to where they need to go, that can make it hard for them to fully follow the recommended routines.
RESULT AND DISCUSSION
The review of healthcare management standards showed that they had a big effect on the quality of care for patients, leading to clear changes in results, safety, and regularity. It was found that following standard procedures led to happier patients, fewer medical mistakes, and more efficient operations. Following protocols on a regular basis led to fewer problems, faster diagnoses, and more rapid treatments, all of which led to better results for patients in both short-term and long-term care. However, problems were seen with putting the plan into action, mainly because healthcare professionals were unwilling to follow it, there wasn't enough technology available, and there were training holes. Standardised procedures provided a basic level of care, but their rigidity sometimes made it harder to tailor treatment to each person. Because the procedure was designed to be flexible, it was possible to make changes based on what the patient wanted and small clinical details. This led to more engaged and happy patients.
|
Table 2. Protocol Adherence and Patient Satisfaction |
|||
|
Healthcare Setting |
Protocol Adherence (%) |
Patient Satisfaction (%) |
Medical Errors Reduced (%) |
|
Hospital A |
85 |
88 |
15 |
|
Hospital B |
78 |
84 |
12 |
|
Clinic A |
92 |
91 |
18 |
|
Clinic B |
89 |
86 |
16 |
In four different healthcare settings (Hospital A, Hospital B, Clinic A, and Clinic B), table 2 shows the link between following the rules, making patients happy, and lowering medical mistakes. Overall, Hospital A and Clinic A have the best rates of following the rules, at 85 % and 92 %, respectively. Figure 3 shows a comparison of following protocols, patient happiness, and fewer medical mistakes. This shows that following protocols is linked to better healthcare.
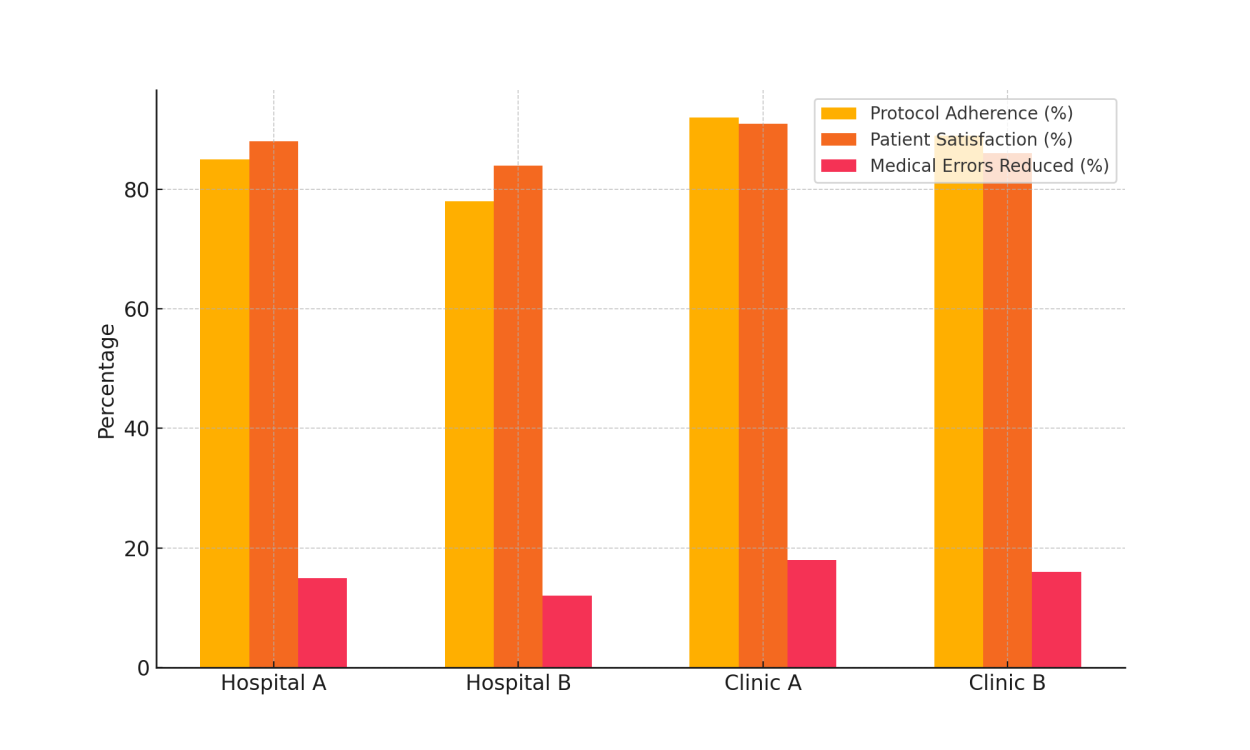
Figure 3. Comparison of Protocol Adherence, Patient Satisfaction, and Medical Error Reduction in Healthcare Settings
Clinic A also has the best rates of customer happiness, at 91 %. Also, the number of medical mistakes has gone down pretty significantly at these institutions, with Clinic A showing the biggest drop (18 %). This shows that following rules more closely is linked to better results, both in terms of patient happiness and safety. Figure 4 shows changes over time in following protocols, keeping patients happy, and lowering medical mistakes, showing how things have gotten better in a variety of healthcare situations.
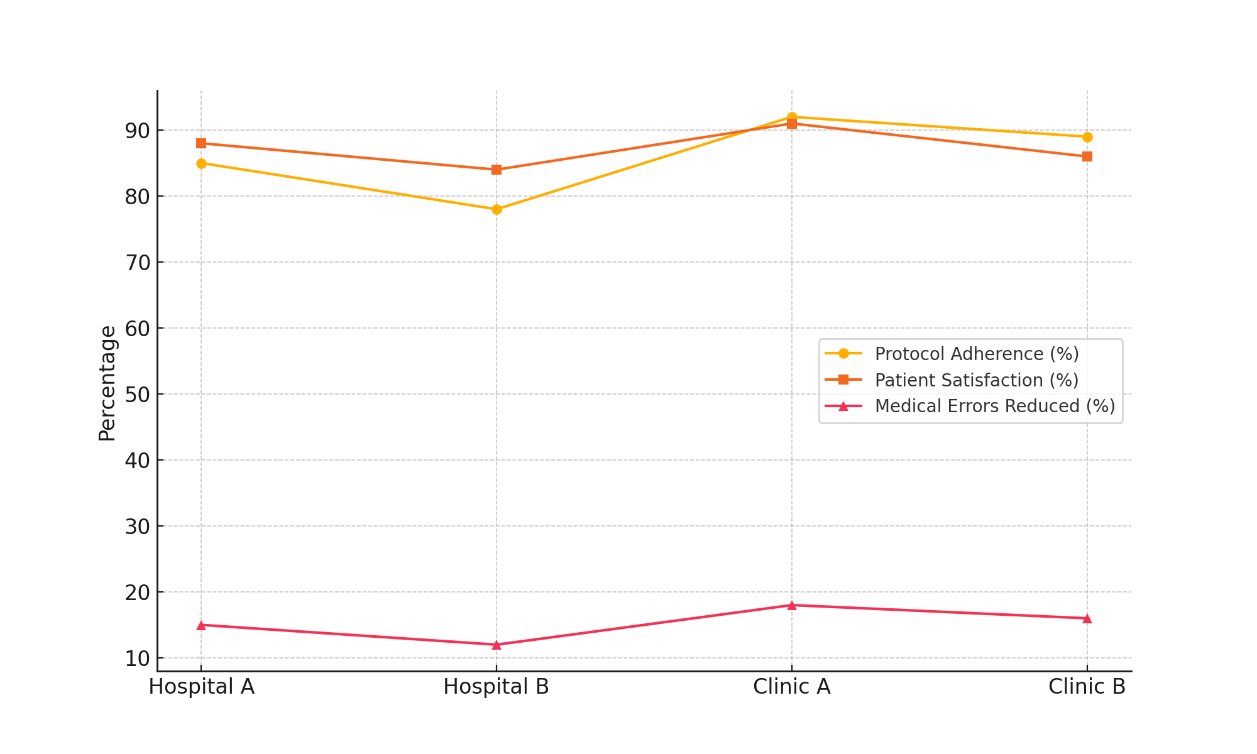
Figure 4. Trends in Protocol Adherence, Patient Satisfaction, and Medical Error Reduction Across Healthcare Settings
In contrast, Hospital B has the lowest patient satisfaction (84 %), which is related to its lowest protocol obedience (78 %). This shows that lower patient satisfaction can be caused by poor protocol adherence. It's also only a 12 % drop in medical mistakes in Hospital B, which supports the idea that procedures are very important for making sure patients are safe and happy.
|
Table 3. Patient Outcomes and Healthcare Efficiency |
||||
|
Healthcare Setting |
Readmission Rate (%) |
Treatment Success Rate (%) |
Average Waiting Time (min) |
Cost Reduction (%) |
|
Hospital A |
5 |
95 |
25 |
10 |
|
Hospital B |
7 |
92 |
30 |
8 |
|
Clinic A |
3 |
97 |
20 |
12 |
|
Clinic B |
6 |
94 |
22 |
9 |
The information in table 3 shows how well patients did and how efficiently healthcare was used in four different settings: Hospital A, Hospital B, Clinic A, and Clinic B. The table shows important numbers like the number of readmissions, the number of successful treatments, the average length of wait times, and the amount of money saved. These numbers show how well and efficiently care is delivered. Clinic A is unique because it has the lowest rate of return (3 %), and the treatment works 97 % of the time. Figure 5 shows an overall look at some important measures, including how well patients do, how often mistakes happen, and how well healthcare places follow their own protocols.
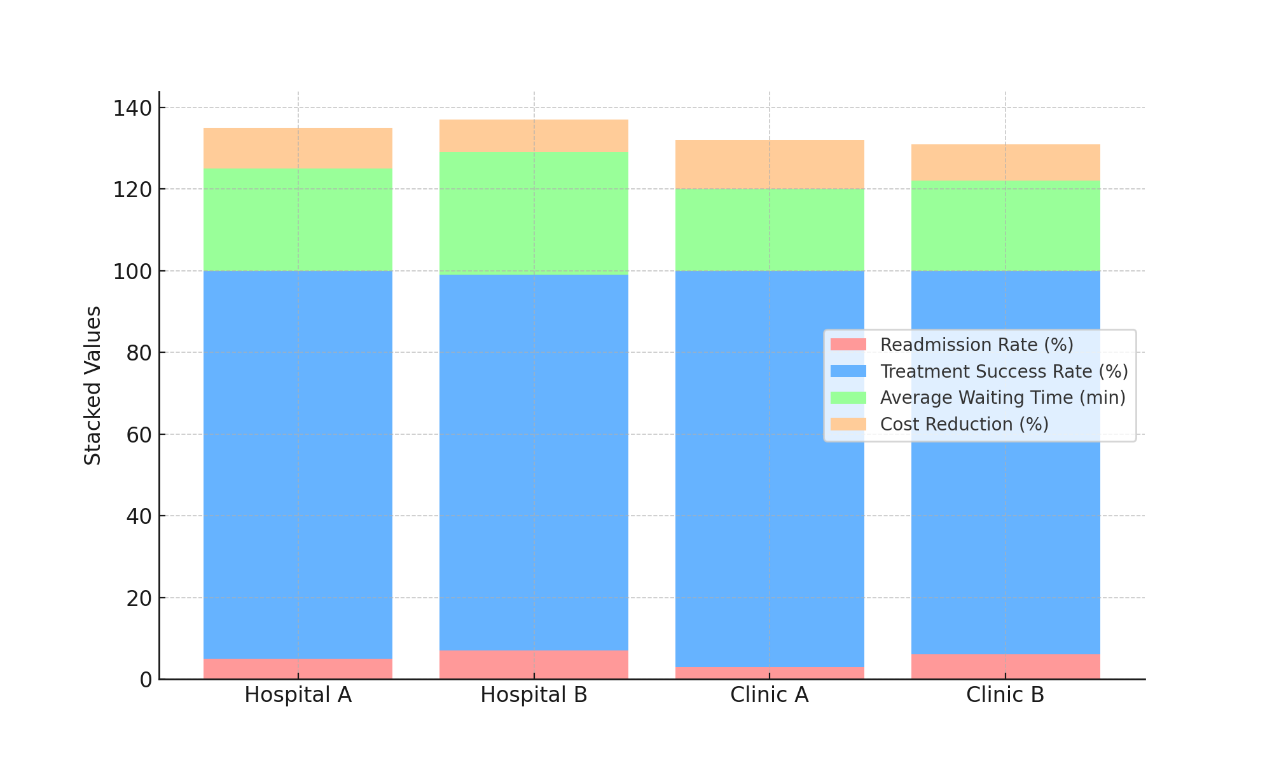
Figure 5. Cumulative Comparison of Key Metrics in Healthcare Settings
This shows that the rules that Clinic A follows are very good at taking care of patients' situations and making sure they have good results. Clinic A also has the fastest average wait time, at just 20 minutes. Figure 6 shows how different measures, such as quality of care for patients, fewer mistakes, and following protocols, add up over time in healthcare situations.
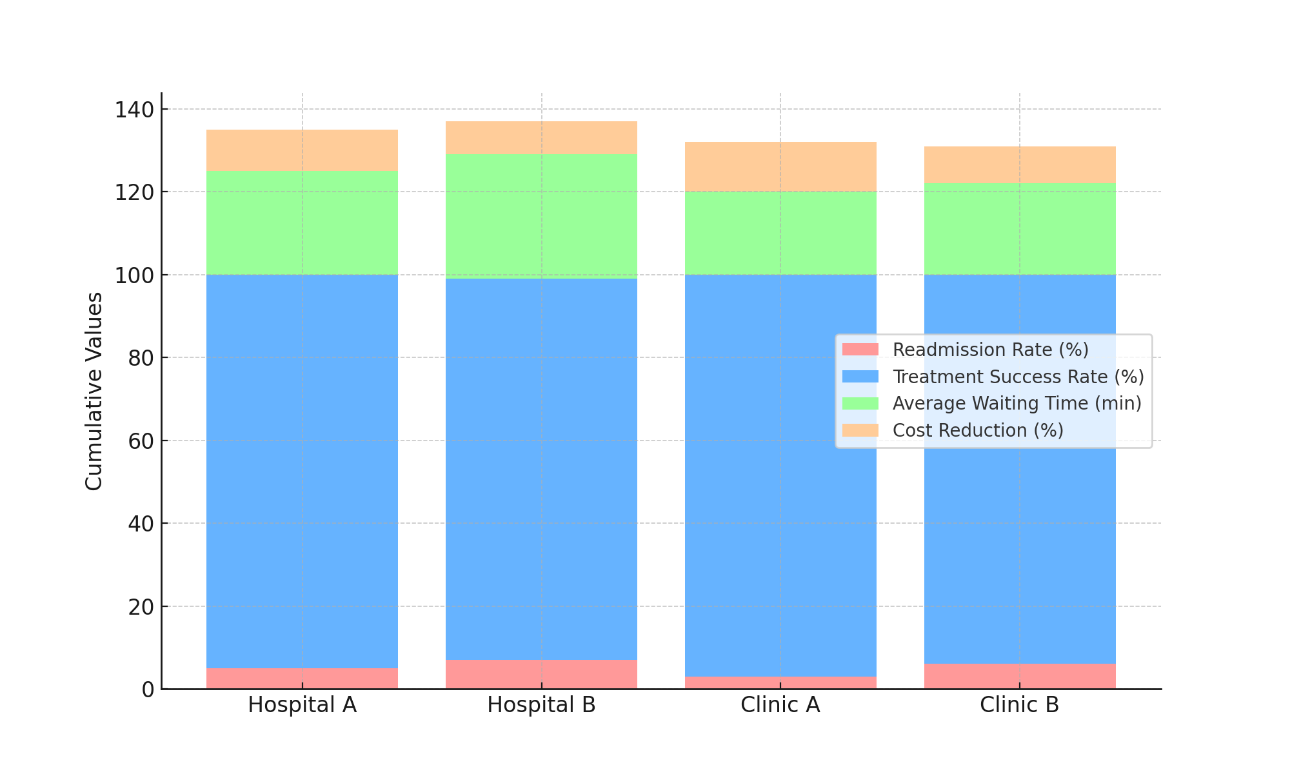
Figure 6. Incremental Contribution of Metrics Across Healthcare Settings
This shows that the healthcare system works well, which makes the customer experience better. The 12 % drop in costs at Clinic A is also noteworthy, and shows that providing better care can also lower healthcare costs. Hospital B, on the other hand, has the highest rate of readmissions (7 %) and the lowest rate of cost reduction (8 %). This suggests that while it may offer effective treatments, it could do a better job of controlling its resources and stopping readmissions. Hospital A has an average wait time of 22 minutes, and Clinic B has an average wait time of 22 minutes. Hospital A has a relatively low return rate of 5 %.
CONCLUSIONS
Healthcare management rules are very important for making sure that patients always get good care. The study showed that standard practices make healthcare processes much more efficient, protect patients more, and cut down on mistakes. Following these guidelines lowers variation in care, making sure that patients get quick treatments that are based on research. In turn, this leads to better clinical outcomes, happier patients, and more efficient healthcare generally. But beating a number of obstacles is necessary for operations to go well. Healthcare workers' worries about liberty and stress can make it hard to follow the plan. It is very important for healthcare organisations to create an atmosphere that supports following guidelines, including doctors in their growth and making sure they have the right training and support. Getting rid of technology and infrastructure problems, like making sure that systems can talk to each other and giving them the tools they need, is essential for putting protocols into action correctly. The study also stressed how important it is for guidelines to be flexible. Standardisation is important for uniformity, but being able to change methods to meet the needs of each patient is more important for patient-centered care. Protocols shouldn't be too strict; they should be able to be changed based on what the patient wants and the specifics of the case. This method makes patients more involved and improves the general quality of care. Even with these problems, the results support the idea that healthcare management procedures are an important part of making healthcare better. They make care more consistent, help patients do better, and make things safer, but to work best, they need to be constantly reviewed, improved, and changed. To make sure that procedures improve both the professional and patient situations as much as they can, they need to have good training, equipment, and patient-centered methods. A healthcare system that is more efficient, safer, and focused on patients is the result of following procedures correctly. It also meets the needs of a wide range of patients better.
BIBLIOGRAPHIC REFERENCES
1. Lamothe, M.; Boujut, E.; Zenasni, F.; Sultan, S. To be or not to be empathic: The combined role of empathic concern and perspective taking in understanding burnout in general practice. BMC Fam. Pract. 2014, 15, 15.
2. Adamson, K.; Loomis, C.; Cadell, S.; Verweel, L.C. Interprofessional empathy: A four-stage model for a new understanding of teamwork. J. Interprof. Care 2018, 32, 752–761.
3. Derksen, F.; Bensing, J.; Lagro-Janssen, A. Effectiveness of empathy in general practice: A systematic review. Br. J. Gen. Pract. 2013, 63, e76–e84.
4. Flickinger, T.E.; Saha, S.; Roter, D.; Korthuis, P.; Sharp, V.; Cohn, J.; Eggly, S.; Moore, R.D.; Beach, M.C. Clinician empathy is associated with differences in patient–clinician communication behaviors and higher medication self-efficacy in HIV care. Patient Educ. Couns. 2016, 99, 220–226.
5. Roter, D.L.; Frankel, R.M.; Hall, J.A.; Sluyter, D. The expression of emotion through nonverbal behavior in medical visits. Mechanisms and outcomes. J. Gen. Intern. Med. 2006, 21 (Suppl. S1), S28–S34.
6. Hojat, M.; Louis, D.Z.; Markham, F.W.; Wender, R.; Rabinowitz, C.; Gonnella, J.S. Physicians’ Empathy and Clinical Outcomes for Diabetic Patients. Acad. Med. 2011, 86, 359–364.
7. Rakel, D.; Barrett, B.; Zhang, Z.; Hoeft, T.; Chewning, B.; Marchand, L.; Scheder, J. Perception of empathy in the therapeutic encounter: Effects on the common cold. Patient Educ. Couns. 2011, 85, 390–397.
8. Lown, B.A.; Dunne, H.; Muncer, S.J.; Chadwick, R. How important is compassionate healthcare to ? A comparison of the perceptions of people in the United States and Ireland. J. Res. Nurs. 2017, 22, 60–69.
9. Vedsted, P.; Heje, H.N. Association between patients’ recommendation of their GP and their evaluation of the GP. Scand. J. Prim. Health Care 2008, 26, 228–234.
10. Doohan, I.; Saveman, B.-I. Need for compassion in prehospital and emergency care: A qualitative study on bus crash survivors’ experiences. Int. Emerg. Nurs. 2015, 23, 115–119.
11. Sashikanta Khuntia, Subhodip Adhikary. (2015). Research Article On “A Study on Job Satisfaction and Performance of Management Guru’s of Management Colleges-with Reference to Odisha”. International Journal on Research and Development - A Management Review, 4(1), 94 - 100.
12. Debasmita Tripathy. (2015). Work Life Balance and the Gender Agenda in Facilitating Performance. International Journal on Research and Development - A Management Review, 4(1), 101 - 106.
13. Dilalla, L.F.; Hull, S.K.; Dorsey, J.K. Effect of gender, age, and relevant course work on attitudes toward empathy, patient spirituality, and physician wellness. Teach. Learn. Med. 2004, 16, 165–170.
14. Singer, T.; Klimecki, O.M. Empathy and compassion. Curr. Biol. 2014, 24, R875–R878.
15. Teding van Berkhout, E.; Malouff, J.M. Link to external site this link will open in a new window. The efficacy of empathy training: A meta-analysis of randomized controlled trials. J. Couns. Psychol. 2016, 63, 32–41.
16. Riess, H.; Kelley, J.M.; Bailey, R.W.; Dunn, E.J.; Phillips, M. Empathy training for resident physicians: A randomized controlled trial of a neuroscience-informed curriculum. J. Gen. Intern. Med. 2012, 27, 1280–1286.
FINANCING
The authors did not receive financing for the development of this research.
CONFLICT OF INTEREST
The authors declare that there is no conflict of interest.
AUTHORSHIP CONTRIBUTION
Data curation: Shilpi Singh, Sagar V. Joshi, Souvagya Panigrahi, Aparna Patange, Upendra Sharma.U.S.
Formal analysis: Shilpi Singh, Sagar V. Joshi, Souvagya Panigrahi, Aparna Patange, Upendra Sharma.U.S.
Methodology: Shilpi Singh, Sagar V. Joshi, Souvagya Panigrahi, Aparna Patange, Upendra Sharma.U.S.
Supervision: Shilpi Singh, Sagar V. Joshi, Souvagya Panigrahi, Aparna Patange, Upendra Sharma.U.S.
Drafting - original draft: Shilpi Singh, Sagar V. Joshi, Souvagya Panigrahi, Aparna Patange, Upendra Sharma.U.S.
Writing - proofreading and editing: Shilpi Singh, Sagar V. Joshi, Souvagya Panigrahi, Aparna Patange, Upendra Sharma.U.S.