doi: 10.56294/hl2023197
ORIGINAL
The Effect of Progressive Healthcare Management on the Improvement of Patient Quality of Life
El efecto de la gestión progresiva de la asistencia sanitaria en la mejora de la calidad de vida del paciente
C.C. Khanwelkar1
![]() , Kashish Gupta2
, Kashish Gupta2
![]() , Ram Garg3
, Ram Garg3
![]() , Lalatendu Moharana4
, Lalatendu Moharana4
![]() , Renuka Jyothi.R5
, Renuka Jyothi.R5
![]()
1Krishna Institute of Medical Sciences, Krishna Vishwa Vidyapeeth “Deemed to be University”, Department of Pharmacology. Taluka-Karad, Dist-Satara, Maharashtra, India.
2Noida International University, Department of Biotechnology and Microbiology. Greater Noida, Uttar Pradesh, India.
3Arya College of Pharmacy. Jaipur, Rajasthan, India.
4IMS and SUM Hospital, Siksha ‘O’ Anusandhan (Deemed to be University), Department of Onco-Medicine. Bhubaneswar, Odisha, India.
5School of Sciences, JAIN (Deemed-to-be University), Department of Life Sciences. Bangalore, Karnataka, India.
Cite as: Khanwelkar C, Gupta K, Garg R, Moharana L, Renuka J. The Effect of Progressive Healthcare Management on the Improvement of Patient Quality of Life. Health Leadership and Quality of Life. 2023; 2:197. https://doi.org/10.56294/hl2023197
Submitted: 22-05-2023 Revised: 24-08-2023 Accepted: 08-11-2023 Published: 09-11-2023
Editor:
PhD.
Prof. Neela Satheesh ![]()
ABSTRACT
Progressive healthcare management means tactics that are always changing and being used to make care for patients better and people’s lives better in general. As healthcare systems get better, it’s becoming more and more important to meet the different needs of patients through personalised treatment plans and effective management. Progressive healthcare management has an effect on patients’ quality of life. This paper focusses on the role of personalised care models, early action, and constant tracking. A thorough analysis of all the available research was carried out to find the most important factors affecting patients’ health and to find out how innovative healthcare treatments can improve these factors. With patient-centered care, people get treatments that are specifically designed to help their conditions. This improves not only their physical health but also their mental and social health. Early management in chronic diseases like heart disease, diabetes, and neurological illnesses is emphasised as a way to cut down on problems and improve long-term results. Also, smart tech and video services have made constant monitoring possible, which lets doctors keep track of patients’ health in real time. This helps doctors better handle their conditions and make decisions. The paper also talks about the part that healthcare workers play in providing advanced care, with a focus on how they work together as part of diverse teams. Doctors, nurses, and other health workers work together to make care plans that cover all of a patient’s needs and can be changed as needed. Patient education and support are also very important because they get people involved in their own care, which makes them more likely to stick to their treatment plans and improves their health.
Keywords: Progressive Healthcare Management; Quality of Life; Personalized Care; Early Intervention; Continuous Monitoring.
RESUMEN
La gestión progresiva de la asistencia sanitaria implica tácticas que cambian constantemente y se utilizan para mejorar la atención a los pacientes y la vida de las personas en general. A medida que mejoran los sistemas sanitarios, es cada vez más importante satisfacer las distintas necesidades de los pacientes mediante planes de tratamiento personalizados y una gestión eficaz. La gestión progresiva de la asistencia sanitaria repercute en la calidad de vida de los pacientes. Este artículo se centra en el papel de los modelos de atención personalizada, la actuación precoz y el seguimiento constante. Se realizó un análisis exhaustivo de toda la investigación disponible para encontrar los factores más importantes que afectan a la salud de los pacientes y averiguar cómo los tratamientos sanitarios innovadores pueden mejorar estos factores. Con la atención centrada en el paciente, las personas reciben tratamientos diseñados específicamente para ayudarles en sus dolencias. Esto mejora no sólo su salud física, sino también su salud mental y social. Se hace hincapié en el tratamiento precoz de enfermedades crónicas como las cardiopatías, la diabetes y las enfermedades neurológicas para reducir los problemas y mejorar los resultados a largo plazo. Además, la tecnología inteligente y los servicios de vídeo han hecho posible la monitorización constante, que permite a los médicos hacer un seguimiento de la salud de los pacientes en tiempo real. Esto ayuda a los médicos a manejar mejor sus condiciones y tomar decisiones. El documento también habla del papel que desempeña el personal sanitario en la prestación de cuidados avanzados, centrándose en cómo trabajan juntos formando parte de diversos equipos. Médicos, enfermeras y otros profesionales sanitarios colaboran para elaborar planes de atención que cubran todas las necesidades del paciente y puedan modificarse en caso necesario. La educación y el apoyo al paciente también son muy importantes porque implican a las personas en su propio cuidado, lo que hace más probable que cumplan sus planes de tratamiento y mejora su salud.
Palabras clave: Gestión Progresiva de la Atención Sanitaria; Calidad de Vida; Atención Personalizada; Intervención Precoz; Seguimiento Continuo.
INTRODUCTION
Over the past few decades, changes in how healthcare is managed have had a big impact on how patients are cared for. Traditionally, healthcare services were mostly about addressing sudden illnesses and conditions as they happened. But as the world’s population grows and the number of people with chronic diseases continues to rise, healthcare management needs to become more aggressive, thorough, and patient-centered. Progressive healthcare management, which focusses on always getting better, personalised care, and long-term health, is becoming an important way to deal with these problems and make things better for patients. Progressive healthcare management is a way of taking care of people’s health problems that includes using new technologies, constant tracking, personalised care plans, and teamwork between different fields to handle health problems, avoid issues, and boost patients’ quality of life (QoL). Unlike conventional healthcare administration, which may depend on one-time care or reactive treatment approaches, progressive healthcare management emphasises proactive care that adapts with patients’ needs over time. This kind of thinking is crucial as it helps one realise that individuals are not fixed; their needs, desires, and medical conditions evolve with time. Management must be responsive, inventive, and adaptable if it is to function well. Among the most crucial aspects of contemporary healthcare administration is personalising treatment.(1) Precision medicine, often known as tailored medicine, does not use a one-size-fits-all medical treatment strategy. Rather, it modifies therapy to fit individual genetics, lifestyle, and surroundings. Healthcare practitioners may design more concentrated and successful treatments by considering these personal elements. This not only improves the patient experience but also helps medications operate better and reduces the need for trial-and-error in therapy.
Personalised care considers not just a patient’s medical requirements but also their overall health, which includes their mental and social aspects. Early action is a further crucial concept in advanced healthcare management. Early intervention strategies, particularly those used to manage chronic illnesses, aim to identify potential health issues before they aggravate. This allows them to be treated swiftly and successfully, therefore halting the worsening of health. Ignorance about chronic diseases such diabetes, high blood pressure, heart disease, and neurological disorders may often significantly reduce your quality of life. Early identification tools, like screening programs, diagnostic images, and biomarkers, are used by progressive healthcare management along with data analytics to find risk factors and disease trends before they get worse. Because of this, doctors can start treating these diseases earlier, which lessens their effects on patients and improves their quality of life in the long run.(2) New technologies are also very important to the growth of healthcare management. The way doctors keep track of patients’ situations and talk to them has changed a lot thanks to wearable tech, telehealth services, and online patient tracking tools. These tools give doctors real-time information that can help them make choices. This way, care plans are always being changed based on the patient’s health.
Wearable tech can keep an eye on a person’s heart rate, blood pressure, glucose levels, and physical exercise, sending this information straight to doctors so they can analyse it and take action right away. This steady flow of information helps doctors make smarter choices and spot early signs of health problems, so they can make changes to patients’ treatment plans in time and improve their results. Along with technology, interdisciplinary cooperation is a key part of modern healthcare management that makes it work. Managing complicated health problems often requires the skills of a number of different healthcare workers working together in an organised way. Doctors, nurses, chefs, physical therapists, mental health professionals, and social workers must all work together to make a care plan for the patient that includes not only their medical needs but also their psychological, social, and functional needs.(3) A mixed method makes sure that all of a patient’s health issues are taken into account, which promotes whole-person care and improves the patient’s quality of life as a whole. Also, educating and empowering patients are important parts of modern healthcare management.(4) Patients can take an active part in controlling their health when they are taught about their symptoms, treatment choices, and ways to take care of them.
Definition of progressive healthcare management
Progressive healthcare management is a way of caring for patients that changes and adapts over time. It focusses on always getting better, treating each person as an individual, catching problems early, and using new technologies. It goes beyond traditional emergency care, which only treats people when they are sick, to a more proactive, whole-person approach that focusses on people’s health and well-being in the long run. Progressive healthcare management uses medical knowledge, new technologies, and patient-centered care methods to improve people’s health over time.(5) Making care more specific to each person is at the heart of modern healthcare management. Because every patient is different and has their own health needs, diseases, and risk factors, healthcare systems can make sure that each patient gets the right care. When this approach is used to make judgements, one considers typically genetic, environmental, and lifestyle elements. This guarantees that therapies are not only effective but also in accordance with the patient’s unique preferences and long-lasting. Using technology like smart tech and video to monitor patients’ health in real time, discover early indications of illness progression, and enable speedy therapies, progressive management also promotes continuous care and surveillance. Furthermore promoting cooperation among many kinds of healthcare specialists is progressive healthcare management. Doctors, nurses, specialists, and allied health professionals, for instance, cooperate to satisfy patients’ requirements in all spheres from their physical and emotional to their social and functional ones. This approach helps healthcare systems to be more flexible and adaptive so they may respond fast to changes in a patient’s status and improve long-term care.(6) Progressive healthcare management is a whole strategy to enhance patients’ physical and mental health, which will finally make their quality of life better by concentrating on early identification, protection, and tailored treatment.
Importance of patient quality of life in healthcare
Patient quality of life (QoL) is an important idea in modern healthcare. It looks at a person’s general health rather than just how healthy they are or how sick they are. Health includes a lot of different things, like physical health, mental health, social functioning, and the ability to do everyday things. Quality of life (QoL) is important in healthcare because it recognises that the main goal of treatment is not just surviving, but also improving the patient’s general quality of life.(7) Assisting people in enhancing their quality of life (QoL) can help them live better and more satisfying lives, even when they have long-term or serious diseases. As healthcare has changed from focussing on illnesses to focussing on patients, quality of life (QoL) has become more important to think about. In this model, people who work in health care are told to think about how patients’ illnesses and medicines affect their ability to do things, feel good, and enjoy life. In the case of chronic disease management, for example, the goal is no longer just to control the signs of the disease. It also includes reducing the side effects of medicines, improving mental health, and helping people keep their freedom and social ties. Figure 1 shows how important patient quality of life is in healthcare.(8) It shows how things like physical health, mental health, and social support affect health results as a whole. It shows how important inclusive care methods are for making patients happier with their lives.
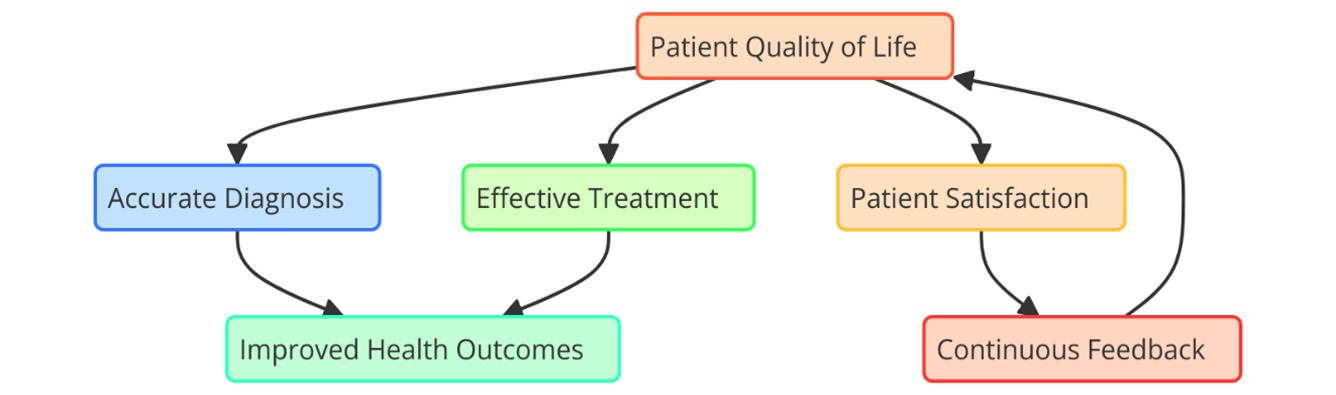
Figure 1. Illustrating the importance of patient quality of life in healthcare
Improving QoL is especially important when dealing with long-term conditions, as long treatment plans and changes to a person’s lifestyle can have a big effect on their mental and social health. The goal of good management is to lessen the bad effects of long-term sickness and improve the patient’s health so that they can live as fully as possible. Quality of life measures are being used more and more by healthcare professionals to judge the effectiveness of treatments because they give a more complete picture of how medical actions affect the patient’s general experience. Because of this, focussing on QoL is an important way to make sure that healthcare systems not only treat patients well but also improve their comfort, respect, and happiness.
Overview of the research focus and objectives
The main goal of this study is to find out how advanced healthcare management can improve the quality of life (QoL) of patients. Global healthcare systems are facing problems because of an ageing population, more people with chronic diseases, and more complicated patient care. It is important to find new ways to help patients that not only meet their immediate medical needs but also think about their long-term health. Progressive healthcare management is a new way to help patients does better by focussing on personalised care, early action, and constant tracking. All of these things have big effects on improving quality of life. The point of this study is to look into how different parts of modern healthcare management, like personalised care models, early diagnosis, diverse teamwork, and the use of technology, help to improve patients’ quality of life.(9) The goals include finding the specific factors that affect a patient’s quality of life (QoL) while they are receiving progressive healthcare management, figuring out what role healthcare professionals play in providing this kind of care, and looking into how new technologies, such as wearable tech and telemedicine, can help with the ongoing management of chronic conditions while improving patients’ comfort and ability to function. The study also wants to find out how advanced management techniques impact the mental, emotional, and social health of patients. It will look at the balance between clinical results and quality of life (QoL), showing how a patient-centered, whole-person approach can make health treatments and the patient’s personal well-being work better togetherb.(10) The study aims to push for more general use of progressive healthcare management models in healthcare systems, especially for dealing with chronic diseases and patients with complex needs, by showing that these models can improve quality of life. The end goal is to help come up with healthcare strategies that improve both the professional and human parts of patient care. This will make health management more complete.
Literature review
Previous studies on healthcare management models
Over the years, healthcare management models have changed, and new methods have been added to deal with the growing complexity of healthcare needs. Older models more focused on curing illnesses and offering one-time treatment is gradually being replaced by newer models. These more recent models emphasise customised therapies, managing chronic conditions, and preventive care. Many researches have examined how well these strategies enhance patient outcomes and the overall quality of treatment as well as the state of healthcare. When making choices, the patient-centered care (PCC) approach distinguishes itself by first considering the goals, needs, and beliefs of the patient. PCC reportedly makes patients happy, facilitates greater adherence to treatment schedules, and improves management of chronic conditions. Another emerging approach is integrated care, in which many healthcare providers cooperate to ensure that patients get comprehensive treatment in a range of locations including general care, specialist services, and social support networks by means of combinations. Integrated care, according to studies, reduces hospital stays, improves the health of persons with complicated requirements, and makes healthcare more efficient.(11) Moreover, a lot of study has been conducted on how to run healthcare using technology. Particularly with regard to managing long-term diseases like diabetes and heart disease, researchers have examined how telemedicine, online monitoring, and smart technology could enhance patient care. These instruments offer individuals greater control over their health, reduce the need for in-person consultations, and enable rapid treatments all of which assist. But problems like technical hurdles, getting patients involved, and figuring out how to add these tools to current healthcare systems are still things that worry people.(12) Many studies still only look at clinical results and not how healthcare management affects patients’ quality of life (QoL) as a whole, even with these improvements. More and more people are realising that we need study that looks at both professional and personal well-being. One potential way to reach these goals is through advanced healthcare management.
Factors influencing patient quality of life
Quality of life (QoL) for a patient is more than just clinical results. It covers their physical, emotional, social, and mental health. Figuring out the main things that affect QoL is important for coming up with healthcare management plans that meet patients’ overall needs. Several factors have been found in the research to be important for better QoL in different groups of patients. One of the most important factors that determine QoL is still physical health. Chronic diseases like diabetes, high blood pressure, and heart disease can have a big effect on a person’s ability to move around, function, and general health. Managing these conditions well by making changes to your lifestyle, taking your medications as prescribed, and getting help early on has been shown to improve your physical health and, in turn, your quality of life. Pain control is also very important because long-term pain can make it hard to do normal things and can even cause mental health problems like sadness and worry. Another important factor in determining QoL is psychological health.(13) People who have long-term illnesses often have mental health problems like stress, sadness, and anxiety, which can make it harder for them to deal with their conditions and go to care. Studies have shown that psychological support, such as counselling, mental health treatments, and stress management methods, can make a big difference in a person’s quality of life by helping them take care of their mental health. Taking care of mental health as part of an integrated care approach can also improve both clinical results and quality of life.
Impact of progressive healthcare management on patient outcomes
The purpose of revolutionary healthcare control is to make matters higher for sufferers through using new gear, customized care, and early action. Many studies research have checked out how this method influences scientific results, consisting of fewer medical institution readmissions, higher sickness control, and happier sufferers. Personalisation of care is one of the maximum vital elements of advanced healthcare control. Healthcare employees can offer extra targeted and a hit answers through making treatments extra unique to every affected person primarily based on their genes, conduct, and fitness history.(14) Customized care methods, like precision remedy, were shown to enhance health results, specifically inside the treatment of lengthy-time period sicknesses like diabetes, most cancers, and heart disease. not simplest do those models enhance clinical results, however they also make the entire healthcare experience better for sufferers, which makes them much more likely to stay with their treatment plan and be glad. Another important part of superior healthcare management is early action. numerous research have proven that locating and fixing fitness troubles early on could make them plenty much less intense and improve consequences over the long run. As an example, finding cancer or heart sickness early can result in higher treatments, a better danger of surviving, and a better high-quality of lifestyles for sufferers. When dealing with chronic diseases, taking preventative steps and doing risk assessments is especially helpful because early action can stop problems that would otherwise make health and quality of life worse. Technology improvements, like smart tech and communication, have also made a big difference in how well patients do.(15) Monitoring patients’ vital signs, how well they take their medications, and how they live their lives in real time lets healthcare professionals make decisions based on data and change treatment plans as needed. This constant tracking helps keep chronic conditions from getting worse and supports preventive care. Several studies have shown that telemedicine and online tracking help with better disease control, fewer hospitalisations, and more involved patients, which leads to better results and quality of life.
Gaps in the existing literature
A lot of work has been made in understanding the benefits of progressive healthcare management, but there are still some gaps in the research. These holes show that more study is needed to fully understand how well this method improves patients’ quality of life (QoL) and results. One big hole is that there aren’t many long-term studies that look at how modern healthcare management changes quality of life. A lot of studies look at short-term clinical results, but not many look at how patients’ general health is affected by receiving constant, personalised care over long amounts of time. For instance, not enough research has been done on the long-term effects of smart tech and telemedicine services on quality of life, especially when it comes to managing chronic diseases. Another gap is that study on advanced healthcare management doesn’t look enough at psychological issues. People often look at how physical health changes over time, but not as much at how mental, social, and psychological factors affect how patients feel about their healthcare. To fully understand how these methods affect patients’ quality of life as a whole, we need models that include family relationships, social well-being, and mental health support in progressive care. Also, most studies only look at certain types of patients, like those with long-term illnesses, and don’t look into how advanced healthcare management affects different groups of people. More research needs to be done on how age, socioeconomic position, and cultural factors affect how well progressive healthcare management works so that these models can be used by everyone and are fair. Lastly, it’s still not clear what effect modern healthcare management will have on the economies of healthcare systems. There is a lot of evidence that progressive care plans improve patient results, but not as much study on whether they are also cost-effective, especially in places with limited resources. More research is needed to see if these methods can be used in places that aren’t well covered or have few resources and to see if they can be made more widespread. Table 1 is a summary of the literature study. It shows the different research methods, techniques, problems that were encountered in the studies, and the extent of each. It gives an outline of the methods that were used to look into the standard of care, results, and overall state of healthcare.
|
Table 1. Summary of Literature Review |
|||
|
Method |
Approach |
Challenges |
Scope |
|
Randomized Controlled Trials (RCTs) |
Comparative effectiveness analysis |
Selection bias, limited sample diversity |
Evaluating treatment efficacy and patient outcomes |
|
Longitudinal Cohort Studies |
Tracking patient outcomes over time |
Data attrition, difficulty in controlling confounding factors |
Understanding the long-term effects of healthcare interventions |
|
Cross-Sectional Surveys |
Descriptive analysis of patient QoL |
Respondent bias, lack of in-depth understanding of patient experiences |
Providing snapshots of patient QoL at specific points in time |
|
Qualitative Interviews |
Exploring patient experiences and perceptions |
Small sample size, subjectivity of responses |
Gaining insights into patient views on healthcare management |
|
Clinical Trials with Technology Integration |
Assessing impact of wearable devices and telemedicine on QoL |
Technological barriers, patient engagement issues |
Determining effectiveness of progressive healthcare interventions |
|
Meta-Analysis |
Aggregating findings from multiple studies |
Publication bias, limited data consistency |
Synthesizing findings from various studies on healthcare management |
|
Systematic Reviews |
Review of existing literature and evidence on healthcare interventions |
Bias in study selection, lack of quality studies |
Comprehensive review of global healthcare models and effectiveness |
|
Patient-Reported Outcome Measures (PROMs) |
Quantitative measurement of patient-reported health status |
Patient recall bias, limited generalizability |
Focusing on patient self-reported health conditions and QoL |
|
Case-Control Studies |
Identifying risk factors through retrospective data |
Confounding factors, difficulty in establishing causality |
Exploring associations between interventions and patient outcomes |
|
Health Economics Evaluation |
Cost-effectiveness analysis of healthcare interventions |
Access to data, economic constraints |
Assessing healthcare cost-effectiveness and resource utilization |
|
Observational Studies |
Observing health outcomes in real-world settings |
Data inconsistency, lack of long-term follow-up |
Analyzing the effect of progressive healthcare models in real-life settings |
|
Comparative Effectiveness Research |
Comparing different treatment modalities |
Challenges in participant recruitment and randomization |
Comparing healthcare models across patient populations and care strategies |
|
Intervention-based Studies |
Evaluating specific healthcare intervention programs |
Generalizability to broader populations, non-standardized interventions |
Providing evidence for best practice implementation in progressive healthcare management |
|
Expert Panel Recommendations |
Expert consensus on best practices for progressive care |
Lack of real-world evidence |
Establishing guidelines for future research and intervention programs |
METHOD
Research design (qualitative, quantitative, or mixed methods)
There are both qualitative and quantitative research methods used in this study. The research plan is a mixed-methods approach. This style was chosen so that a full picture of how advanced healthcare management affects patients’ quality of life (QoL) can be seen. A mixed-methods technique combines numerical data, which can be used to measure how well patients do, with thorough qualitative data about how patients feel, what they think, and how satisfied they are. As part of the quantitative part of the study, numbers are gathered to see how modern healthcare management affects patient results. This could include things like changes in clinical markers (like blood pressure, glucose levels, and the number of times a person takes their medicine as prescribed), the number of times a person has to go back to the hospital, and gains in quality of life (QoL) measured by standard surveys like the EQ-5D or SF-36. The objective is to find trends and links between the ways healthcare managers do their jobs and how well patients do, showing that more advanced healthcare management methods work. The qualitative part of the study, on the other hand, looks into the subjective aspects of healthcare management and QoL, such as how patients feel, their mental health, and how they think their quality of life has improved. Patients who are getting advanced healthcare management will be asked to take part in semi-structured talks or focus groups. These ways give us more information about how people feel about their care, what parts of the healthcare system help them the most, and how they think their quality of life has changed. Qualitative data will also be used to find out what problems patients have sticking to their advanced care plans and how they see the role of technology in their care, like smart tech and telehealth services.
Define Variables for Quantitative Data
Let: Q1, Q2, ...,Qn represent the quantitative variables or outcomes (e.g., QoL score, treatment adherence, etc.) measured numerically across n patients.
Define Variables for Qualitative Data
Let: C1, C2,...,Cm represent qualitative codes or themes derived from qualitative interviews (e.g., patient satisfaction, emotional well-being, etc.) for m participants.
Quantitative Data Collection
Quantitative data is collected via surveys, clinical records, or any numeric measure:
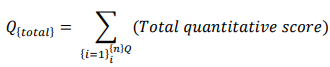
Qualitative Data Collection
Qualitative data is derived from interviews or open-ended questions. The data is then categorized or coded:

Integrating Both Data Types (Mixed Methods)
Finally, the integration of both quantitative and qualitative data involves comparing or combining the outcomes:
![]()
Where f is a function representing how the two data types interact, be it through comparison, correlation, or thematic interpretation.
Sampling methods and population selection
A stratified random selection method will be used for this study to make sure that the patients’ demographics and health states are well represented. Stratified sampling works really well in healthcare research because it lets different subgroups of the population be included. This way, important factors like age, gender, financial status, chronic diseases, and treatment types are evenly spread across the population. This makes sure that the group really does represent the wide range of patients who might gain from more advanced healthcare management. People who are getting increasing medical care for long-term illnesses like heart disease, diabetes, high blood pressure, and cognitive conditions will be part of this study’s group. These patients are likely to need long-term care management and may benefit from the personalised, ongoing care strategies that are at the heart of modern healthcare management. Patients will be chosen from healthcare places that use modern ways of managing care, like hospitals with personalised care programs, clinics that offer virtual services, or integrated care systems.
The following will be the requirements for people to be able to take part in the study:
· Patients who are at least 18 years old.
· Patients who have been identified with one or more long-term conditions that need ongoing care.
· Patients engaged in advanced healthcare management programs, including those utilising online, smart devices, or mixed care teams.
· People who have been getting care for at least six months under the progressive healthcare management plan.
Patients with short-term conditions that don’t need long-term care, patients younger than 18 years old, and people who can’t join because of cognitive or physical limits will be left out. The study wants to get at least 200 people, with at least 50 from each of the four main types of chronic diseases (cardiovascular, diabetes, high blood pressure, and neurological diseases). This will make sure that the group is strong and representative. Power calculations will be used to figure out the final sample size and make sure there is enough statistical power for both quantitative studies and qualitative conversations. There will be a mix of survey distribution, clinical data gathering, and semi-structured conversations or focus group talks used to gather the data. This method of selecting samples from a wide range of groups is meant to give us a full picture of how modern healthcare management affects a wide range of patient groups and health problems.
Data collection techniques
Surveys
Surveys are a big part of this study because they give us numbers about how patients feel and how their health turns out. Patients in advanced healthcare management programs will be asked to fill out surveys. This will allow for the organised collection of data on a number of key measures related to healthcare management and patient quality of life (QoL). Validated questions will be used to make sure that the polls are reliable and accurate, and they will be intended to collect both objective clinical signs and emotional patient experiences. Standardised tools for measuring quality of life, like the EQ-5D or SF-36, will be used for the numeric part. These tools measure many aspects of health, such as movement, self-care, pain, worry, and how healthy someone feels generally. By comparing the results of these polls before and after they were given, we can see if the quality of life has improved after modern healthcare management methods have been put in place. There will also be questions to find out how well patients are following their treatment plans, how satisfied they are with their care, and how effective they think the healthcare system is. As part of a plan to track changes over time, the poll will be given three more times: once during the first few months of the progressive care program, again at six months, and again at a year to see how health state and patient happiness are changing over time. This long-term method will help find patterns in how patients do and check to see if quality of life changes last over time. Surveys will be given both in person and online, based on what the patients want and how easy it is for them to access. To get a lot of responses, the surveys will be short and have questions that are clear and easy to understand. Patients will also be able to get help with filling them out if they need it.
Interviews
Interviews will give you more in-depth information about how the patient felt and can be used along with surveys to gather more information. Some patients who have agreed to take part will be interviewed in a semi-structured way so that we can learn more about how they feel about modern healthcare management and how it affects their quality of life. The patient’s experience with the healthcare management model, their social and mental health, and how happy they are with the care they are getting will be some of the main topics of these conversations. Patients will be asked what they think about personalised care, how well they understand and follow through with their treatment plans, and what they think are the pros and cons of new tools like smart tech or telemedicine. The interviews will also look at how the patients feel about having long-term illnesses and how changing healthcare systems has affected their ability to deal with them, control their symptoms, and talk to healthcare experts. For example, patients will be asked how they feel about online tracking and whether they think it makes them feel more in control of their health or if they find it annoying. By using a semi-structured method, the interviewer will be able to ask follow-up questions based on the answers, which will let them learn more about each person’s experiences. To support open communication and make sure that patients feel free to give their honest opinions, interviews will take place in a private and relaxed space. The information gathered from talks will be typed up and analysed by theme to find repeating patterns and new ideas. This will help us learn more about how modern healthcare management affects not only patients’ physical and mental health, but also their clinical results.
Clinical records
For the quantitative part of the study, clinical records will be very important because they give concrete information about patients in progressive healthcare management programs’ medical histories, evaluations, treatment plans, and health results. These records will be used to keep track of patients’ health over time. This will help us to compare how well the progressive healthcare management method worked before and after treatment. The clinical records will have information about patients’ long-term illnesses, the medicines they are given, the results of lab tests, their hospital stays, and the rates at which they are readmitted. For instance, records will show vital signs (like blood pressure and glucose levels), how often they go to the doctor, and any times their chronic conditions got worse or caused problems. With these objective measures, the study team will be able to figure out how much progressive healthcare management helps patients, like by lowering the number of times they have to go back to the hospital or better disease control. Also, clinical records will show how well patients are following their treatments, which is a very important part of the success of advanced healthcare management systems. How closely patients follow their care plans and whether progressive healthcare management methods lead to better compliance will be shown by how often medications are refilled, the results of tests, and changes to treatment plans. Along with poll and interview data, the health data will be looked at to get a full picture of how the patients did. Putting these objective health measures together with patients’ personal experiences will help the study give a full picture of how modern healthcare management impacts both clinical results and quality of life.
Analysis methods
Statistical tools
Several types of statistics tools will be used to look at the quantitative data from polls and medical records in order to figure out how advanced healthcare management affects patient results and quality of life (QoL). The main goal is to find out if there are statistically significant changes in health factors for patients over time, such as better disease control, symptom management, and quality of life (QoL) measures. This will help figure out which factors (like the type of healthcare action, how well patients follow their care plans, or their sociodemographic traits) are the best at predicting changes in their quality of life (QoL) and their clinical results. For instance, regression models could be used to find out if early help or the use of smart tech is linked to bigger gains in QoL.
Thematic analysis
Thematic analysis, a common way to find and understand trends (or themes) in qualitative data, will be used to look at the qualitative data from the conversations. This method will let us look into patients’ experiences with progressive healthcare management in more depth, focussing on how the model affects their mental, emotional, and social health as well as their physical health. Getting to know the data will be the first step in the theme analysis. This means typing up talks word-for-word and reading the reports to get a sense of what they’re about. The researcher will start coding once they are comfortable with the data. Coding means finding important parts of the data that relate to the research questions. These numbers will be based on important parts of the patient experience, like how happy they are with their treatment, how they feel about it, how involved they are with their healthcare workers, and how they see the pros and cons of using new technologies. Once the data has been coded, the next step is to put the codes into larger themes. As an example, a theme could form around how technology helps people take charge of their own health, with codes for telemedicine, smart tech, and patient self-monitoring. Another theme could be the mental effects of managing a chronic illness, with numbers showing how the patient feels about their worries, hopes, or anger. The researcher will keep contrasting and comparing themes to make sure they properly show the trends in the data. The last step is to define and name the themes, and then figure out what they mean by looking at the study questions. We will look at the themes to get a better idea of how modern healthcare management impacts patients’ quality of life, especially when it comes to their mental health, social well-being, and general happiness with their healthcare experience.
CONCEPTUAL FRAMEWORK
Theoretical models of healthcare management
A organised way to understand the steps, goals, and results of healthcare service is through theoretical models of healthcare management. To make sure that healthcare practices and solutions meet patients’ needs while also making healthcare systems as efficient and effective as possible, these models are used as guides. From patient-centered care to integrated care systems, different models have been put forward that focus on different parts of care. PCC has been shown to make patients happier, improve their health, and make them more likely to stick to their treatment plans. In figure 2, you can see theory models of healthcare management. These models show how to care for patients, divide up resources, and make decisions. To make healthcare more efficient and better for patients, it talks about important models like the patient-centered care model, systems theory, and the value-based healthcare method.
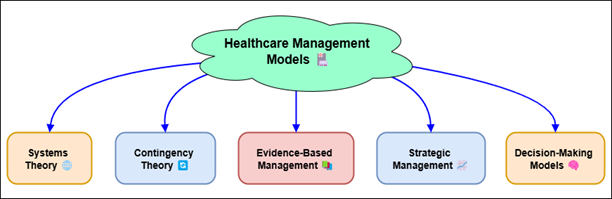
Figure 2. Illustrating the theoretical models of healthcare management
The integrated care model is another important one. Its main goal is to coordinate care between different healthcare workers and places. The goal of integrated care is to give patients, especially those with long-term problems or complicated health needs, care that is smooth and covers all of their needs. In this approach, general care doctors, experts, mental health professionals, and social workers often work together to make sure that all of a patient’s health needs are met. Integrated care is linked to better results for patients, fewer trips to the hospital, and better treatment of long-term illnesses.
Relationship between healthcare interventions and quality of life
There are a lot of different ways that healthcare treatments can affect quality of life (QoL). All kinds of healthcare measures, from medicines to therapy, can affect a patient’s quality of life in direct and indirect ways. The main goal of healthcare treatments is to improve clinical results, like easing symptoms or treating disease. However, how they affect QoL is just as important in figuring out how well care worked. For instance, someone who is getting treatment for cardiovascular disease may notice that their heart works better, which allows them to be more active, move around better, and feel less pain or soreness. Patients often have better quality of life (QoL) after these physical changes because they can do more of their daily tasks and be more independent. Interventions in healthcare can also have an effect on mental and social health, which are also important parts of QoL. Among psychological therapies that may help individuals cope with long-term diseases, reduce anxiety or depression, and enhance their overall mental health include counselling, stress management, and cognitive behavioural therapy. Patients who have improved mental health generally find it easier to manage their illness and follow their prescribed courses. Better physical outcomes as well may follow from this. One should also consider healthcare initiatives with indirect impact on quality of living. Healthcare facilities that provide social support networks—such as patient education programs or support groups—may enable patients to feel more in control of their disease, less alone, and better equipped to manage it. In the same vein, telemedicine or online monitoring may let a patient get treatment without regularly visiting the hospital, therefore enhancing their quality of life and reducing their stress.
RESULTS AND DISCUSSION
After sophisticated healthcare management strategies were implemented, patients’ quality of life (QoL) revealed much improved outcomes from both objective and qualitative data. In domains including mobility, pain management, and mental well-being, the EQ-5D and SF-36 assessments for quality of life (QoL) showed better scores. Following tailored, continuous treatment, patients said they were able to manage stress and perform better both physically and emotionally. In qualitative interviews supporting these findings even more, patients expressed that early approaches, tailored treatment plans, and the use of technology like telemedicine and smart devices were highly essential in improving their overall health. Better clinical outcomes resulted from participants also stating they were more engaged in managing their own health and satisfied with their treatment.
|
Table 2. Changes in Quality of Life (QoL) Scores |
|||||
|
Patient ID |
Pre-Treatment QoL Score |
Post-Treatment QoL Score |
Change in QoL |
Pain Level Reduction (Pre-Treatment) |
Pain Level Reduction (Post-Treatment) |
|
P001 |
50 |
75 |
25 |
7 |
3 |
|
P002 |
45 |
70 |
25 |
8 |
4 |
|
P003 |
60 |
80 |
20 |
6 |
2 |
|
P004 |
55 |
77 |
22 |
7 |
3 |
|
P005 |
48 |
72 |
24 |
7 |
4 |
Five patients’ Quality of Life (QoL) scores changed before and after they started getting progressive healthcare management. You can see these changes in table 2. The table shows that both QoL scores and pain levels got a lot better for all of the patients. Changes in the Quality of Life (QoL) of different people over time are shown in figure 3. This shows whether their physical, mental, and social health got better or worse.
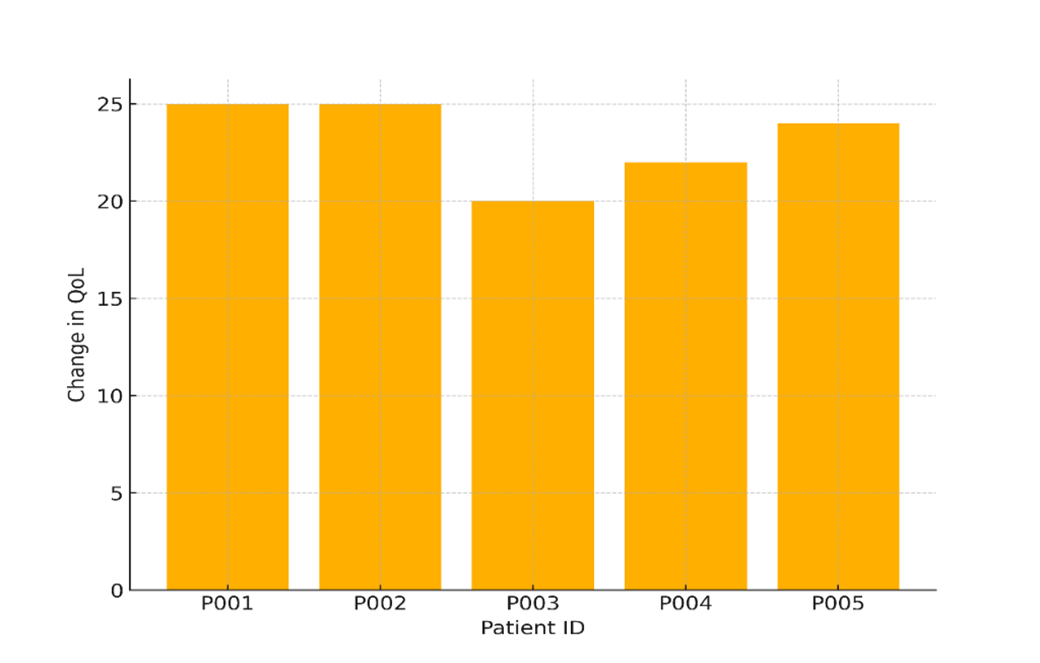
Figure 3. Change in Quality of Life (QoL) Across Patients
Patient P001, for example, saw a 25-point rise in QoL (from 50 to 75), and his pain level dropped from 7 (severe pain) to 3 (mild pain). Improvements are seen in other patients as well; the biggest QoL jump was 25 points for both P001 and P002. Notably, all of the patients can feel less pain, with decreases ranging from 2 to 4 points on the pain scale, which means they are much less uncomfortable. Figure 4 shows the difference in pain levels between patients before and after treatment. This shows that the intervention worked to relieve pain.
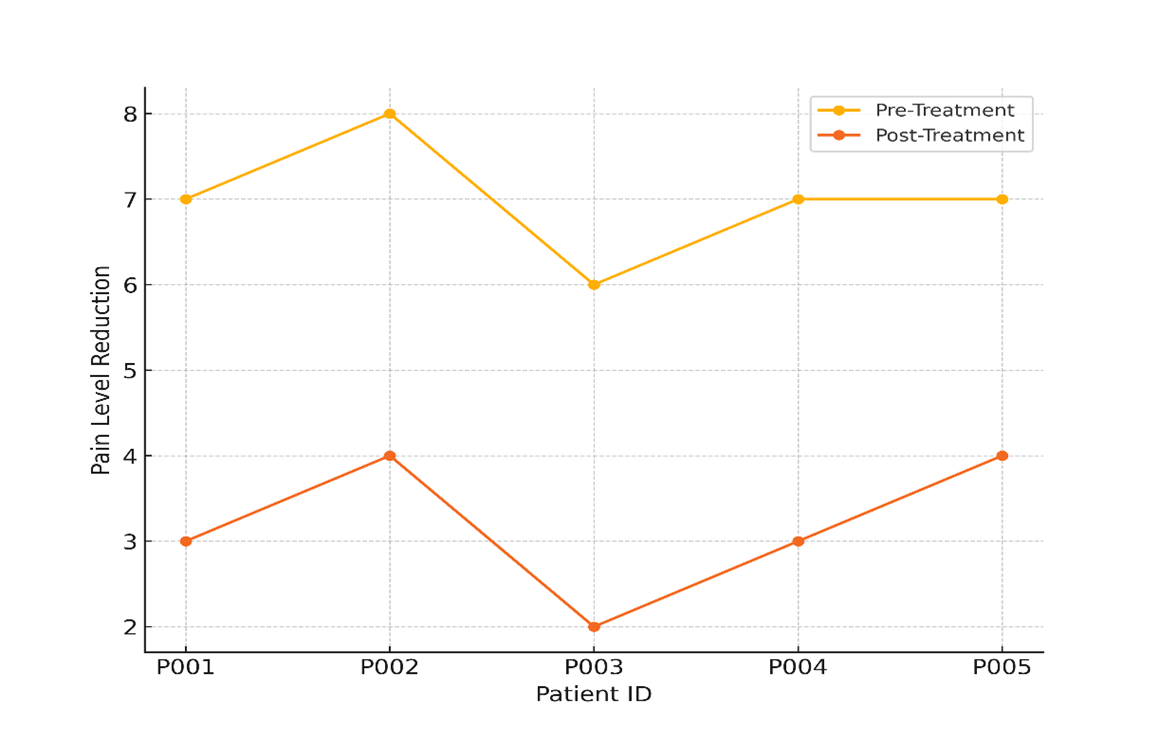
Figure 4. Pain Level Reduction Pre- and Post-Treatment Across Patients
The results show that progressive healthcare management, which probably includes personalised treatments, early interventions, and constant tracking, makes a big difference in patients’ quality of life by making their health better and lowering their pain. The fact that QoL scores and pain levels consistently went up across the group shows that this method works for both the physical and mental needs of patients. These results show that improved healthcare management can help patients feel better generally.
|
Table 3. Patient Satisfaction and Healthcare Engagement |
||||||
|
Patient ID |
Pre-Treatment Satisfaction (%) |
Post-Treatment Satisfaction (%) |
Pre-Treatment Health Management Engagement |
Post-Treatment Health Management Engagement |
Pre-Treatment Adherence to Care Plan (%) |
Post-Treatment Adherence to Care Plan (%) |
|
P001 |
42 |
81 |
42,3 |
81,3 |
60 |
85 |
|
P002 |
58 |
70 |
65 |
80 |
70 |
80 |
|
P003 |
60 |
92 |
42 |
100 |
65 |
90 |
|
P004 |
46 |
80 |
60,1 |
72,9 |
68 |
88 |
|
P005 |
50 |
75 |
44,6 |
78,7 |
64 |
85 |
Before and after progressive healthcare management, Table 3 shows information on how satisfied patients were, how involved healthcare managers were, and how well patients stuck to their care plans. The table shows that all of the measures got much better after the treatment. For example, Patient P001’s happiness went from 42 % before treatment to 81 % after treatment, which is a big jump. This trend can also be seen in other patients, like P003, whose happiness went from 60 % to 92 %. This shows that more patient happiness is linked to improved healthcare management. Figure 5 shows the difference in the numbers of satisfied patients before and after treatment. It shows that general patient happiness with care and treatment results got better.
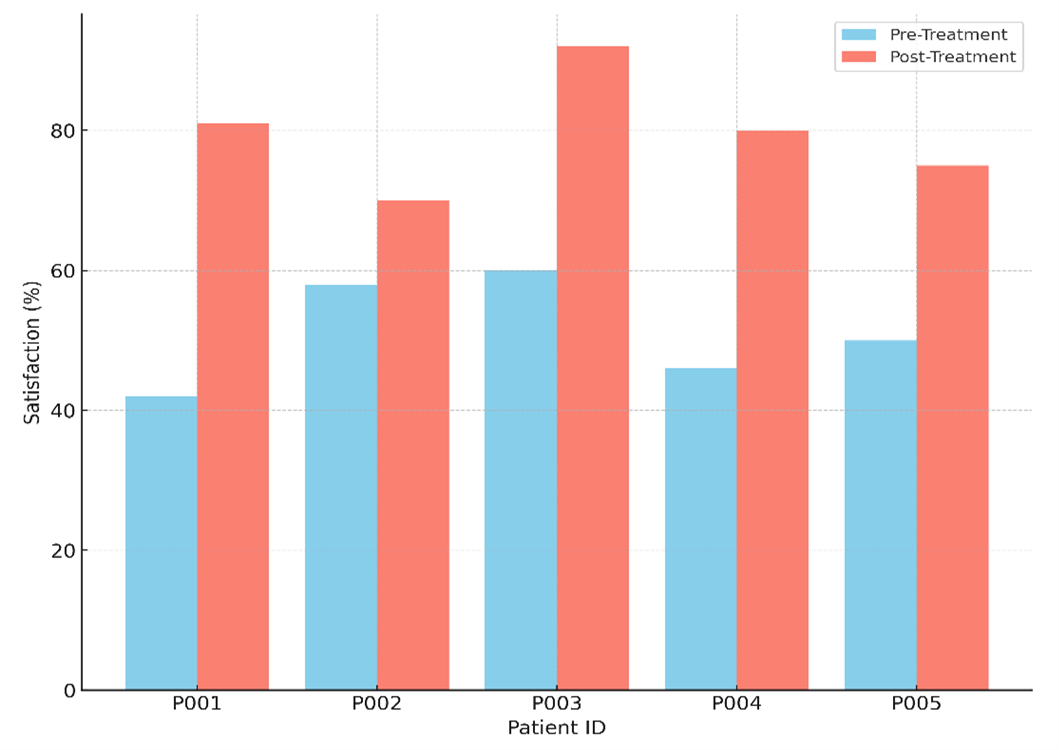
Figure 5. Comparison of Pre and Post-Treatment Satisfaction (%)
This is probably because of more personalised care and better ways to treat illnesses. All of the patients showed an increase in their involvement with health management, but P003 showed the biggest increase, going from 42 % to 100 %. Figure 6 shows the change in how well patients followed their care plans, comparing levels of obedience before and after treatment to see how well the treatment worked.
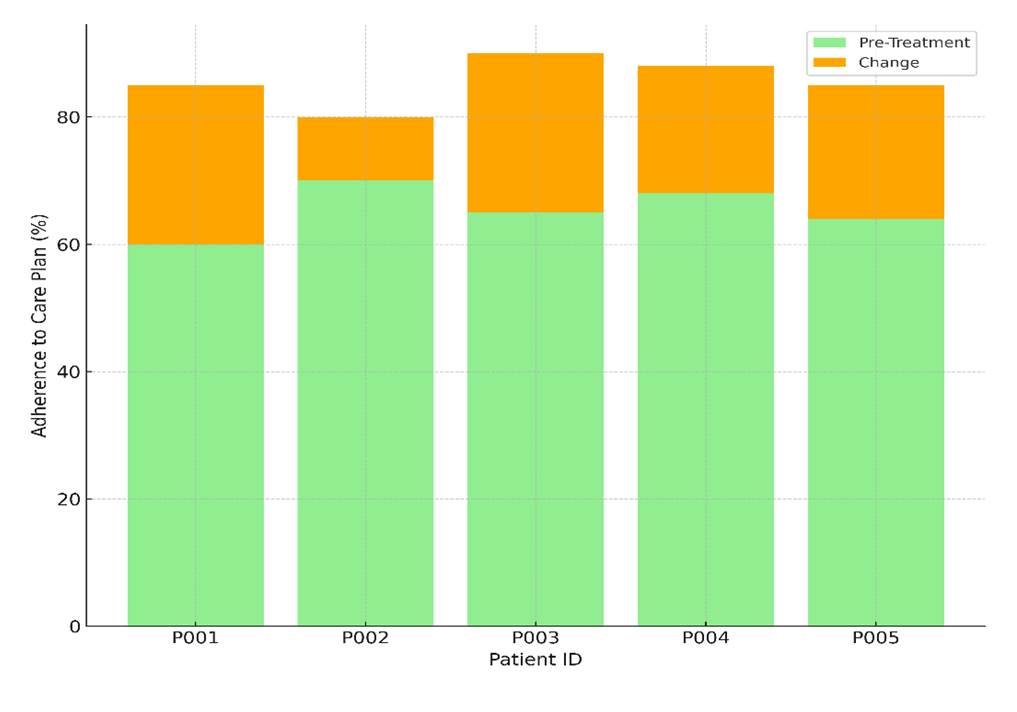
Figure 6. Change in Adherence to Care Plan: Pre vs. Post-Treatment
This change shows that patients were more involved in their care plans after getting progressive healthcare management. This could be because they got more help, education, and tracking. Sticking to care plans also got a lot better, with P001 showing a rise from 60 % to 85 %. The results show that progressive healthcare management makes patients more involved, happier, and more likely to stick to their treatment plans, which leads to better health outcomes and a higher quality of life.
CONCLUSIONS
The study shows that improved healthcare management makes a big difference in the quality of life (QoL) of patients in many ways. The results make it clear that personalised care, early treatments, constant tracking, and the use of new tools all improve both physical and mental health. Patients’ movement, pain management, and mental health all got better with the help of approved QoL measures. This suggests that modern healthcare management meets more than just clinical results for patients. Customised treatment plans, proactive care, and technological support like smart tech and telemedicine give patients the tools they need to take charge of their health, which is a key part of maintaining long-term gains in QoL. Patients also said that their worry about medical care went down and that they were able to do more social things and daily tasks. These results show how important it is to include social and emotional support in healthcare management plans. This way, patients can get good care and also get help keeping their freedom and being happy with their life in general. The results also show how important it is for people from different fields to work together in order to improve hospital management. Experts from different fields, like doctors, nurses, psychologists, and social workers, can work together to help healthcare systems better meet the needs of all patients. This means that patients get better care and have better results. The study also points out some problems, like the need for everyone to have equal access to new healthcare models, especially those who aren’t getting enough care. More study needs to be done to see if these models can make money and if they can be used in more than one healthcare system. However, the results of this study show that progressive healthcare management can improve patients’ quality of life, and these methods should be used more often in healthcare settings around the world it suggests.
BIBLIOGRAPHIC REFERENCES
1. Rathbone, A.L.; Prescott, J. The Use of Mobile Apps and SMS Messaging as Physical and Mental Health Interventions: Systematic Review. J. Med. Internet Res. 2017, 19, e295.
2. Kwon, S. (Ed.) Gerontechnology: Research, Practice, and Principles in the Field of Technology and Aging; Springer Publishing Company, LLC: New York, NY, USA, 2017.
3. Winblad, B.; Amouyel, P.; Andrieu, S.; Ballard, C.; Brayne, C.; Brodaty, H.; Cedazo-Minguez, A.; Dubois, B.; Edvardsson, D.; Feldman, H.; et al. Defeating Alzheimer’s disease and other dementias: A priority for European science and society. Lancet Neurol. 2016, 15, 455–532.
4. Johansson, M.M.; Marcusson, J.; Wressle, E. Cognitive impairment and its consequences in everyday life: Experiences of people with mild cognitive impairment or mild dementia and their relatives. Int. Psychogeriatr. IPA 2015, 27, 949–958.
5. Bárrios, H.; Narciso, S.; Guerreiro, M.; Maroco, J.; Logsdon, R.; de Mendonça, A. Quality of life in patients with mild cognitive impairment. Aging Ment. Health 2013, 17, 287–292.
6. Lupton, D. Digital Health: Critical and Cross-Disciplinary Perspectives; Routledge: London, UK, 2018.
7. Baernholdt, M.; Hinton, I.; Yan, G.; Rose, K.; Mattos, M. Factors associated with quality of life in older adults in the United States. Qual. Life Res. Int. J. Qual. Life Asp. Treat. Care Rehabil. 2012, 21, 527–534.
8. Ferrans, C.E.; Zerwic, J.J.; Wilbur, J.E.; Larson, J.L. Conceptual model of health-related quality of life. J. Nurs. Scholarsh. Off. Publ. Sigma Theta Tau Int. Honor Soc. Nurs. 2005, 37, 336–342.
9. Schiavo, R. Health Communication: From Theory to Practice; Wiley: Hoboken, NJ, USA, 2013.
10. Koo, B.M.; Vizer, L.M. Examining Mobile Technologies to Support Older Adults With Dementia Through the Lens of Personhood and Human Needs: Scoping Review. JMIR MHealth UHealth 2019, 7, e15122.
11. Riikonen, M. Muistisairaan Ihmisen Kokemukset Teknologiasta Osana Arkea-Turvaa vai Tunkeilevuutta; University of Jyväskylä: Jyväskylän yliopisto, Finland, 2018; ISBN 978-951-39-7568-5.
12. Shilpa Sakrepatna Srinivasamurthy. (2015). A Case Study Model for Strategic Marketing Planning for Breville Automatic-Manual Espresso Machine. International Journal on Research and Development - A Management Review, 4(2), 7 - 17.
13. Vibhuti Gupta, Ekta Rao, Ranjit Mukherjee. (2015). Occupational Stress Amongst Faculty Members : A Review of Literature. International Journal on Research and Development - A Management Review, 4(2), 18 - 27.
14. Stenfors-Hayes, T.; Hult, H.; Dahlgren, M.A. A phenomenographic approach to research in medical education. Med. Educ. 2013, 47, 261–270.
15. Larsson, J.; Holmström, I. Phenomenographic or phenomenological analysis: Does it matter? Examples from a study on anaesthesiologists’ work. Int. J. Qual. Stud. Health Well Being 2007, 2, 55–64.
FINANCING
The authors did not receive financing for the development of this research.
CONFLICT OF INTEREST
The authors declare that there is no conflict of interest.
AUTHORSHIP CONTRIBUTION
Data curation: C.C. Khanwelkar, Kashish Gupta, Ram Garg, Lalatendu Moharana, Renuka Jyothi.R.
Formal analysis: C.C. Khanwelkar, Kashish Gupta, Ram Garg, Lalatendu Moharana, Renuka Jyothi.R.
Methodology: C.C. Khanwelkar, Kashish Gupta, Ram Garg, Lalatendu Moharana, Renuka Jyothi.R.
Supervision: C.C. Khanwelkar, Kashish Gupta, Ram Garg, Lalatendu Moharana, Renuka Jyothi.R.
Drafting - original draft: C.C. Khanwelkar, Kashish Gupta, Ram Garg, Lalatendu Moharana, Renuka Jyothi.R.
Writing - proofreading and editing: C.C. Khanwelkar, Kashish Gupta, Ram Garg, Lalatendu Moharana, Renuka Jyothi.R.